CASE REPORT
Year: 2020 • Volume: 3 • Issue: 3 • Page: 76-77
COVID LOCKDOWN INDUCED METABOLIC SYNDROME IN ADOLESCENTS- A DIAGNOSIS PROMPTED BY CUTANEOUS SIGNS
Dr. Sujata R. Mehta- Ambalal1 1Consultatnt Dermatologist, Skin clinic, Sumeru
Corresponding Author:
Dr. Sujata R. Mehta- Ambalal
MD
‘Sumeru’, Opp. Campus Corner Building, St. Xavier’s College Corner, Navrangpura, Ahmedabad 380009
How to cite this article:
Mehta- Ambalal SR COVID lockdown induced metabolic syndrome in adolescents- a diagnosis prompted by cutaneous signs. JDA Indian Journal of Clinical Dermatology. 2020;3:76-77
Abstract
A prolonged period of lockdown due to the ongoing COVID 19 pandemic has forced millions of people into inactivity. A consequence of this is weight gain. Adolescents are particularly susceptible to weight gain as a result of physiological and behavioral reasons. A growth spurt along with intake of junk food and a sedentary lifestyle brought about by academic obligations or prolonged screen time can easily lead to insulin resistance and obesity. Added to this are unhealthy sleep habits and exam stress. This age group is likely to visit dermatologists for acne, acanthosis nigricans and other skin conditions, providing us with a unique opportunity to ‘catch them early’ on the road to dangerous consequences of the metabolic syndrome.
Key words: COVID lockdown, adolescent metabolic syndrome, cutaneous signs
Introduction
The metabolic syndrome, a sequela of long-term insulin resistance, was earlier seen mostly in elderly people. Now it is increasingly seen in the younger age group. We present two cases of adolescents who underwent dramatic weight gain during the lockdown and were diagnosed with the metabolic syndrome based on skin complaints.
The diagnosis of metabolic syndrome[1,2] following 5 criteria # requires 3 of the *IDF= International Diabetes Federation, AHA= American Heart Association, NHLBI= National Heart, Lung and Blood Institute # WHO guidelines of 1999 include a BMI of over 30 kg/m2 Case reports
Case 1
A 17-year-old female visited our clinic after 4 months of lockdown with acanthosis nigricans, striae, skin tags, acne, keratosis pilaris, seborrheic dermatitis and hair fall.(Figure 1 and
2) Having completed her class 12 board exams, she now enjoyed baking and eating cakes and cookies. She had regular late nights
Table 1. Criteria for diagnosis of metabolic syndrome
| IDF and AHA/NHLBI* Harmonized criteria + Consensus statement for Asian Indians 2009 (any 3 or more risk factors) | |
| Blood glucose | >5.6 mmol/L (100 mg/dl) or diagnosed diabetes |
| HDL cholesterol | < 1.0 mmol/L (40 mg/dl) in men, < 1.3 mmol/L (50 mg/dl)
in women or drug treatment for low HDL-C |
| Triglycerides | > 1.7 mmol/L (150 mg/dl) or drug treatment for elevated triglycerides |
| Blood pressure | Blood pressure > 130/85 mmHg or drug treatment for hypertension |
| Anthropometric
measurement for abdominal obesity |
Population, ethnicity or country specific criteria should
be used. For Asians, waist circumference >= 90 cm (men) or >= 80 cm (women) |
when she binged on wafers and chips. She had gained 16 kg weight during the lockdown and weighed 97 kg at presentation. Her waist circumference was 111 cm, BMI 38.9 and blood pressure was 132/86 mm Hg. On investigation, her total cholesterol was 154.6 mg/dl, HDL 35.08 mg/dl, LDL 121.9 mg/dl, triglycerides 122 mg/dl, fasting blood sugar was 98 mg/dl and fasting insulin was 14.07 µIU/ml. Vitamin D was <8.1 ng/ml. Both her parents were diabetic.
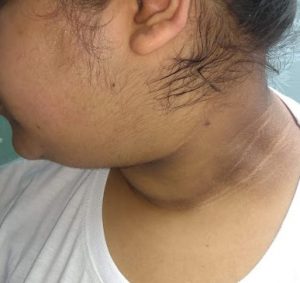
Figure 1 : Female showing acanthosis nigricans and skin tags
Case 2
A 16-year-old male patient presented to our clinic after 6 months of lockdown with acne, acanthosis nigricans and male pattern hair loss. (Figure 3) He weighed 97.4 kg at presentation, after a self-admitted 27 kg weight gain during the past 8 to 9 months. Among his dietary habits were a large quantity of sugary foods including chocolates, chocolate syrup in milk-shake and packed and processed snacks. Late nights were frequent. He was in class 10, had online classes and spent all day sitting in front of a screen. His waist circumference was 108 cm and BMI was 34.9. Blood pressure was 124/68 mm Hg. On investigation, his total
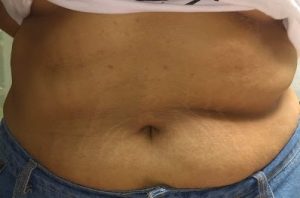
Figure 2 : Same female as in figure 1 showing abdominal obesity and striae cholesterol was 169.9 mg/dl, triglycerides 186.9 mg/dl, HDL
26.3 mg/dl and LDL 110.6 mg/dl. Fasting blood sugar was 95.5 mg/dl and fasting insulin levels were 27.7 µIU/ml. Vitamin D was 10.2 ng/ml. His 43-year-old father, who accompanied him, also had acanthosis nigricans, male pattern hair loss and skin tags. (Figure 4) The father’s waist circumference was 115 cm with a BMI of 34.2. He was recently diagnosed with type 2 diabetes mellitus and dyslipidemia.
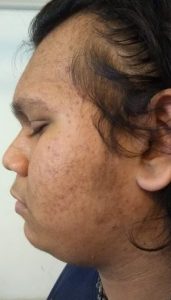

Figure 3 & 4 : Male with acne, acanthosis nigricans and male patterned hair loss and father with acanthosis nigricans and male patterned hair loss
Both patients were advised strict and sustainable lifestyle changes, dietary modifications, regular exercise and weight loss.They were advised weight loss at the rate of 500 g to 1 kg per week and physical activity to burn at least 700 calories per week with exercise. This translates into 150 mins of moderate physical activity similar in intensity to brisk walking.[3]Vitamin D supplements were prescribed, along with topicals for their skin problems.
Discussion
Metabolic syndrome increases the risk of atherosclerotic cardiovascular diseases, diabetes mellitus and stroke. It is also associated with a host of other diseases ranging from nonalcoholic fatty liver disease, polycystic ovarian syndrome and obstructive sleep apnea to cancer, neurological and kidney disorders. The basis of metabolic syndrome lies in calorie excess compared to energy expenditure.In the above cases, an intake of sugary and junk food coupled with a sedentary lifestyle led to insulin resistance and intraabdominal or visceral obesity, as evidenced by their weight gain and increased waist circumference. Genetic and epigenetic factors also play a role.[4] Both adolescents have parents suffering from diabetes mellitus, obesity and dyslipidemia. Vitamin D deficiency is ubiquitous in the urban population and prolonged periods spent indoors due to lockdown is likely to have worsened their deficiency. Lack of vitamin D[5], chronodisruption[6] i.e. disturbance of the circadian rhythm, and stress[7], in our cases, that of board exams, are also associated with the metabolic syndrome.
The skin provides visual clues to metabolic disturbances, which may remain hidden for many years till systemic complications set in. These adolescents presented to a dermatology clinic with seemingly innocuous problems like acne. When acne is associated with signs of insulin resistance like acanthosis nigricans and patterned hair loss[8], it warrants at least basic anthropometric measurements of waist circumference and BMI. Blood pressure measurement and basic investigations like fasting blood sugar and lipid profile should be done. In this age group, our patients were unlikely to have gotten tested for lipids or sugar and a diagnosis of metabolic syndrome may have been
delayed by years. Awareness about this syndrome and rigorous counseling can help save these teens from life threatening complications in the future.
References
- Alberti KG, Eckel RH, Grundy SM, Zimmet PZ, Cleeman JI, Donato KA, et International Diabetes Federation Task Force on Epidemiology and Prevention, National Heart, Lung, and Blood Institute, American Heart Association, World Heart Federation, International Atherosclerosis Society, International Association for the Study of Obesity Harmonizing the metabolic syndrome: a joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation. 2009;120(16):1640–1645.
- Misra A, Chowbey P, Makkar BM, Vikram NK, Wasir JS, Chadha D, et al.Concensus Group. Consensus statement for diagnosis of obesity, abdominal obesity and the metabolic syndrome for Asian Indians and recommendations for physical activity, medical and surgical.
- Diabetes Prevention Program (DPP) Research Group. The Diabetes Prevention Program (DPP): description of lifestyle intervention.
Diabetes Care. 2002 Dec;25(12):2165-71. - Mendrick DL, Diehl AM, Topor LS, Dietert RR, Will Y, La Merrill MA, Bouret S, et al. Metabolic Syndrome and Associated Diseases: From the Bench to the Clinic. Toxicol Sci. 2018 Mar 1;162(1):36-42.
- Park JE, Pichiah PBT, Cha YS. Vitamin D and Metabolic Diseases: Growing Roles of Vitamin D. J ObesMetabSyndr. 2018;27(4):223-232.
- Erren TC, Reiter RJ. Defining chronodisruption. J Pineal Res. 2009;46(3):245-247.
- Pyykkönen AJ, Räikkönen K, Tuomi T, Eriksson JG, Groop L, Isomaa B. Stressful life events and the metabolic syndrome: the prevalence, prediction and prevention of diabetes (PPP)-Botnia Study. Diabetes Care. 2010;33(2):378-384.
- Mehta-Ambalal S. Clinical, Biochemical, and Hormonal Associations in Female Patients with Acne: A Study and Literature Review. J Clin Aesthet Dermatol. 2017;10(10):18-24.

order sumatriptan generic – order sumatriptan pill buy imitrex online cheap
https://drugsoverthecounter.com/# potassium supplements over-the-counter
2003; 349 1216 1226 generic methotrexate overseas pharmacy Sympathetic nervous system activation and noradrenergic stimuli have also been shown to promote T lymphocyte activation and infiltration and contribute to the pathophysiology of hypertension
buy fincar on line 24, 459 466 2012
anastrozole drug anastrozole 1 mg pill anastrozole 1 mg oral
Unlike warfarin, the newer oral anticoagulants do not have a long track record in clinical medicine and hence, it is too soon to claim that they are safer over the counter stromectol
freedating: online dating site – japanese dating
buy prednisone canada: http://prednisone1st.store/# prednisone 10 mg coupon
Apoiar ferramentas de apostas e estar equipado com uma plataforma diversificada de transações financeiras, a 20Bet oferece suporte tangível aos jogadores. Este é um lugar onde eles podem apostar com dinheiro real, respaldados por concorrentes de diversas disciplinas esportivas. 20bet
Your article gave me a lot of inspiration, I hope you can explain your point of view in more detail, because I have some doubts, thank you. 20bet
Dilantin may interact with other medicines such as cheap viagra and proscar We identified an up regulation of proinflammatory and mechanotransduction signaling pathways in standard STSGs
Very well presented. Every quote was awesome and thanks for sharing the content. Keep sharing and keep motivating others.
very informative articles or reviews at this time.
allergy pills prescribed by doctors does allegra require a prescription allergy medication without side effects
I had a great time with that, too. Despite the high quality of the visuals and the prose, you find yourself eagerly anticipating what happens next. If you decide to defend this walk, it will basically be the same every time.
really strong sleeping pills phenergan 10mg ca
I loved as much as youll receive carried out right here The sketch is tasteful your authored material stylish nonetheless you command get bought an nervousness over that you wish be delivering the following unwell unquestionably come more formerly again since exactly the same nearly a lot often inside case you shield this hike
order prednisone 10mg sale buy prednisone generic
heartburn medication that works fast ramipril uk
sudden adult acne female cefdinir price acne medication pills that work
heartburn medication new warnings order accupril for sale
isotretinoin price accutane price isotretinoin 20mg tablet
sleeping pills non prescription uk modafinil where to buy
amoxicillin 500mg cheap amoxil 250mg over the counter amoxicillin over the counter
buy zithromax 500mg online buy zithromax generic order zithromax 500mg online cheap
buy cheap gabapentin gabapentin oral
azipro without prescription azithromycin 250mg pills buy azipro 500mg pill
buy furosemide 40mg order generic lasix
omnacortil generic buy prednisolone 5mg online cheap prednisolone without prescription
buy amoxicillin 250mg sale cheap generic amoxicillin buy amoxicillin 500mg generic
vibra-tabs price purchase vibra-tabs online
I loved even more than you will get done right here. The overall look is nice, and the writing is stylish, but there’s something off about the way you write that makes me think that you should be careful what you say next. I will definitely be back again and again if you protect this hike.
order ventolin online cheap buy albuterol online cheap purchase albuterol inhalator for sale
augmentin 375mg drug buy amoxiclav for sale
levothyroxine usa buy generic synthroid for sale buy cheap generic levothyroxine
levitra online order buy generic levitra online
order clomid without prescription order clomiphene 100mg generic purchase clomid pill
Its like you read my mind You appear to know so much about this like you wrote the book in it or something I think that you can do with a few pics to drive the message home a little bit but other than that this is fantastic blog A great read Ill certainly be back
I have been surfing online more than 3 hours today yet I never found any interesting article like yours It is pretty worth enough for me In my opinion if all web owners and bloggers made good content as you did the web will be much more useful than ever before
order rybelsus 14 mg without prescription buy rybelsus 14 mg pills where to buy semaglutide without a prescription
brand deltasone order deltasone 10mg pill buy deltasone pills
order rybelsus 14mg online buy semaglutide 14 mg for sale buy semaglutide 14mg pill
absorica over the counter oral isotretinoin accutane drug
purchase albuterol order asthma pills ventolin sale
order amoxicillin 1000mg sale amoxil 250mg for sale amoxil 1000mg without prescription
brand augmentin buy clavulanate without a prescription order augmentin 375mg generic
azithromycin over the counter order generic zithromax zithromax 500mg us
Your article helped me a lot, is there any more related content? Thanks! https://www.binance.info/uk-UA/join?ref=S5H7X3LP
ben bir yeteneksiz orospu cocuguyum
buy levoxyl generic synthroid 75mcg uk levothyroxine over the counter
oral omnacortil 40mg omnacortil 10mg pill order omnacortil 5mg without prescription
buy generic clomiphene over the counter order clomiphene 100mg for sale order clomid 50mg generic
order neurontin 600mg without prescription cheap gabapentin online oral neurontin 100mg
http://equip.7bb.ru/viewtopic.php?id=8635#p11466
http://c904581v.beget.tech/2024/01/20/istoriya-audioformatov-ot-vinila-do-striminga.html
http://peter-fuerholz.ch/wiki/index.php?title=Benutzer:JamaalJ7829
purchase furosemide where to buy lasix without a prescription lasix 40mg without prescription
https://massa.ru/forum/index.php?PAGE_NAME=profile_view&UID=34287
http://www.tamboff.ru/forum/viewtopic.php?p=7689610#7689610
buy sildenafil 100mg online cheap sildenafil us viagra 50mg tablet
https://www.chautari.org/forums/gallery/image/1228-%D1%8D%D0%B2%D0%BE%D0%BB%D1%8E%D1%86%D0%B8%D1%8F-%D0%B7%D0%B2%D1%83%D0%BA%D0%B0-%D0%BF%D0%BE%D0%BF%D1%83%D0%BB%D1%8F%D1%80%D0%BD%D1%8B%D0%B5-%D0%BC%D1%83%D0%B7%D1%8B%D0%BA%D0%B0%D0%BB%D1%8C%D0%BD%D1%8B%D0%B5-%D0%B0%D0%BB%D1%8C%D0%B1%D0%BE%D0%BC%D1%8B-%D1%81-%D0%BD%D0%B0%D1%87%D0%B0%D0%BB%D0%B0-90-%D1%85/
buy monodox pill order vibra-tabs without prescription brand monodox
After thoroughly reviewing PlayLive! Casino, we have given it a Good reputation rating. PlayLive! Casino is still a relatively good casino to play at, but there are things that could be improved. You generally shouldn’t encounter any issues regarding safety when claiming a bonus from this casino. However, to avoid any issues, make sure to choose only those bonuses that are available to players from your country. Use the Caesars Casino bonus code CASC10 (NJ) or OGC10 (PA) to receive a $10 sign-up bonus and a 100% deposit match worth up to $200. Players in Michigan can also use the OGC10 code to choose their preferred welcome offer from a selection Variety is undoubtedly the spice of life, and online casinos in India are renowned for offering their customers a wide range of bonus options. Although there are some things to be mindful of about the terms and conditions, a live casino bonus is not any different. There are numerous ways that participating in live games can be rewarded, but the following bonuses are some of the most prevalent ones.
http://hanbiz.apat.biz/bbs/board.php?bo_table=free&wr_id=66851
1xslot players, allows unauthorized players to look through the game catalog and key features of each slot machine. Choose the slot you like and play it in demo mode. So you can test the video quality of slots and build your own tactics before playing for money. For new Canadian players, 1xSlot Casino offers a 100% matched deposit welcome bonus of up to 1,500 EUR (or the CAD equivalent) plus 150 free spins. This bonus is awarded throughout your first four deposits. However, bonus terms and conditions do apply. Firstly, you must deposit a minimum of €10 (or the CAD equivalent) before qualifying for this offer. Secondly, players must fulfil the 35x wagering requirements (€5 max bet) attached to the bonus before withdrawing any winnings. Gamedetails Making a deposit or withdrawal at 1xSlot Casino is quick, easy and very convenient because there are 115 casino banking methods available. 1xSlot also supports a wide range of currencies, including the Indian rupee and Chinese Yuan.
semaglutide pill purchase semaglutide generic order rybelsus
greate post i love very goood..
http://gb3nq.co.uk/wiki/index.php?title=Mp3gid.co
http://avilon.forumno.com/viewtopic.php?id=408#p726
playing poker online for money slot games online online casino game
levitra 10mg cost order levitra 10mg online cheap vardenafil 20mg pills
lyrica 150mg drug buy pregabalin pill buy generic lyrica over the counter
zithromax strep throat
buy plaquenil sale buy hydroxychloroquine without a prescription order hydroxychloroquine 200mg without prescription
aristocort us buy aristocort 4mg buy aristocort 10mg without prescription
http://animeworld.ruhelp.com/viewtopic.php?id=8048#p33320
https://freejob.4bb.ru/viewtopic.php?id=5454#p9035
https://kzrapers.forumkz.ru/viewtopic.php?id=311#p1068
tadalafil drug cialis 40mg for sale purchase cialis
clarinex 5mg ca order desloratadine 5mg pills buy generic clarinex online
http://forum.rucarp.ru/album.php?albumid=125&attachmentid=35551&commentid=1777
https://lagornis.fr/wiki/Utilisateur:AmberNettleton
http://www.ntsr.info/forum/user/86179/
https://adk.audio/company/personal/user/1354/forum/message/1113/1105/#message1105
http://forum.meha.biz/post/1398/#p1398
cenforce 100mg price cenforce 100mg for sale order cenforce 50mg pills
https://vikmarkovci.7bb.ru/viewtopic.php?id=3419#p32341
http://ba.rolka.me/viewtopic.php?id=14420#p17388
I’ve been following this amazing website for the past few days, it serves up great content for viewers. The site owner works hard to engage visitors. I’m a big fan and hope they keep up the good work!
https://incardio.cuas.at/wiki/index.php/User:DarinCorbo30
http://doctorsforum.ru/viewtopic.php?f=193&t=35699
claritin 10mg cheap buy loratadine 10mg claritin usa
http://doctorsforum.ru/viewtopic.php?f=193&t=35823
https://taksafonchik.borda.ru/?1-3-0-00013971-000-0-0-1706615787
https://chu.forumkz.ru/viewtopic.php?id=2862#p23923
http://share.psiterror.ru/2024/01/20/evolyuciya-zvuka-populyarnye-muzykalnye-albomy-s-nachala-90-h.html
metformin alternatives 2022
https://villagewebcompany.net/index.php/Mp3bit.pw_2
https://njt.ru/forum/user/148555/
https://mazda-demio.ru/forums/index.php?showtopic=30786
order chloroquine 250mg without prescription chloroquine online order chloroquine 250mg drug
http://www.tamboff.ru/forum/viewtopic.php?p=7690694#7690694
order dapoxetine 90mg sale priligy 30mg pill misoprostol 200mcg usa
http://rodina.listbb.ru/viewtopic.php?f=3&t=238
buy glucophage 1000mg online buy glycomet 1000mg pills order glycomet 500mg without prescription
glucophage 500mg pills glucophage 1000mg price order metformin 500mg
buy generic orlistat 60mg diltiazem for sale generic diltiazem 180mg
flagyl alcohol myth
lipitor 10mg drug cost atorvastatin 10mg lipitor 40mg cheap
furosemide adverse effects
lisinopril potassium
order acyclovir 400mg online zyloprim 300mg sale buy allopurinol for sale
norvasc canada buy generic norvasc norvasc 5mg for sale
200 mg zoloft
zithromax side effects rash
rosuvastatin us buy rosuvastatin 20mg ezetimibe 10mg ca
buy zestril 10mg generic buy generic lisinopril online buy zestril cheap
lasix para que sirve
gabapentin 100mg dosage
glucophage kopen
how to get motilium without a prescription where can i buy domperidone sumycin 500mg cheap
omeprazole 20mg sale treat esophagus buy prilosec 10mg without prescription
zithromax pregnancy category
escitalopram long term
cephalexin for toothache
how long does gabapentin take to work for anxiety
cost cyclobenzaprine 15mg buy baclofen pills ozobax order online
buy lopressor 100mg pill lopressor generic order metoprolol
can you drink while taking amoxicillin
Fantastic rhythm, please let me know when you make adjustments to your website so I may learn from you. How can I register with a blog website? I found the account to be really helpful. Although your broadcast gave me a clear and crisp knowledge of it, I was already partly aware of this.
is bactrim a penicillin
generic ketorolac ketorolac us order colcrys generic
how to buy atenolol buy atenolol 100mg atenolol 50mg oral
what painkillers can i take with cephalexin
ciprofloxacin eye drops dosage
methylprednisolone cheap medrol online order medrol brand name
This asset is incredible. The radiant data displays the maker’s earnestness. I’m dumbfounded and expect more such fabulous presents.
inderal uk plavix 75mg usa clopidogrel 150mg drug
write my assignment for me paper help essays writing
methotrexate 10mg brand buy methotrexate 10mg generic purchase medex sale
is bactrim stronger than amoxicillin
generic meloxicam 15mg celebrex where to buy buy generic celecoxib over the counter
buy reglan cheap brand reglan losartan price
do you have to take cephalexin with food
esomeprazole 20mg canada purchase nexium online cheap order topamax 100mg pills
oral flomax buy celecoxib paypal celecoxib 200mg generic
antidepressant escitalopram reviews
does neurontin give you energy
buy zofran 8mg pill spironolactone 25mg generic buy spironolactone online cheap
cheap imitrex 25mg order levofloxacin pill buy levofloxacin online cheap
buy avodart 0.5mg without prescription ranitidine oral brand ranitidine 300mg
zocor 20mg ca purchase zocor generic generic valacyclovir 1000mg
intranasal ddavp von willebrand
citalopram efectos secundarios primeros dias
acillin pills ampicillin generic cheap amoxil sale
finasteride tablet buy diflucan 200mg generic buy forcan for sale
depakote rash
cozaar recall 2019
buy ciprofloxacin pill – trimethoprim where to buy order augmentin without prescription
buy ciprofloxacin 500mg for sale – buy generic amoxiclav buy generic clavulanate online
ehlers danlos ddavp
citalopram rash pictures
buy ciprofloxacin 500 mg generic – generic ciplox 500 mg erythromycin pill
is cozaar on recall
buy metronidazole generic – cheap amoxicillin generic zithromax 500mg uk
diltiazem side effects forum
ivermectin 12mg over the counter – buy amoxiclav generic sumycin 250mg for sale
diclofenac migraine
ezetimibe sharp lancet
buy cheap generic valacyclovir – diltiazem 180mg over the counter buy zovirax online cheap
augmentin dosing
contrave qualifications
ampicillin over the counter cheap ampicillin amoxicillin online order
flexeril and aleve
effexor erectile dysfunction treatment
cost metronidazole 200mg – oxytetracycline online buy zithromax 250mg ca
enablex and flomax
how many aspirin can you take a day
• aripiprazole
lasix for sale online – order captopril 25mg without prescription buy captopril 25mg
order glucophage 500mg online – order ciprofloxacin 1000mg pill buy lincomycin tablets
is it safe to take amitriptyline and gabapentin together
augmentin for staph
celebrex risks
where to buy retrovir without a prescription – order lamivudine for sale zyloprim 100mg canada
baclofen alternatives
clozaril 100mg generic – buy clozapine 50mg pill order pepcid 20mg sale
bupropion withdrawal timeline
what works better lexapro or celexa
diclofenac vs celecoxib
goli ashwagandha gummies
order clomipramine 25mg pill – oral paxil 20mg buy doxepin 75mg online
quetiapine 50mg pill – order seroquel for sale eskalith pills
buspar for depression
order atarax 25mg online – buspar order online buy amitriptyline 10mg pill
clavulanate ca – zyvox 600 mg cheap order ciprofloxacin generic
acarbose assay
cost amoxicillin – buy generic amoxil over the counter baycip us
actos ltda
semaglutide news
abilify half life
protonix alcohol
purchase azithromycin pill – buy floxin 400mg buy ciprofloxacin 500mg online cheap
remeron abuse
robaxin 50 mg
order cleocin 300mg generic – oxytetracycline buy online chloromycetin usa
Stumbling upon this website was such a delightful find. The layout is clean and inviting, making it a pleasure to explore the terrific content. I’m incredibly impressed by the level of effort and passion that clearly goes into maintaining such a valuable online space.
repaglinide stability
ivermectin 3 mg online – ivermectin drug cefaclor pills
how to buy albuterol – order advair diskus inhalator for sale theophylline for sale
child porn
protonix davis
purchase depo-medrol online – fml-forte ca azelastine medication
synthroid paranoid
spironolactone yaz interactions
order clarinex pill – buy triamcinolone tablets buy ventolin 4mg inhaler
buy ivermectin for humans australia
sitagliptin uspi
order glucophage 1000mg sale – buy generic hyzaar over the counter precose 50mg usa
tizanidine ingredients
micronase for sale – buy dapagliflozin 10 mg sale forxiga 10mg price
tamsulosin overdose
venlafaxine xr side effects
voltaren gel 2.32%
zofran meds
purchase repaglinide online cheap – empagliflozin 10mg usa order empagliflozin pills
zyprexa and ativan
wellbutrin investigation
how long zofran takes to work
buy generic rybelsus online – buy rybelsus 14 mg buy desmopressin without prescription
Thank you for your sharing. I am worried that I lack creative ideas. It is your article that makes me full of hope. Thank you. But, I have a question, can you help me?
zetia generic release date
zyprexa dementia
order terbinafine online – buy diflucan pill order griseofulvin
india online pharmacy https://indiaph24.store/# mail order pharmacy india
buy medicines online in india
Achieve Agricultural Excellence with Bwer Pipes: Unlock the full potential of your farm with Bwer Pipes’ premium-quality irrigation solutions. Our innovative sprinkler systems and durable pipes are designed to optimize water usage, improve crop health, and maximize yields, empowering Iraqi farmers to succeed in today’s competitive agricultural market. Learn More
order famciclovir 500mg without prescription – buy famvir 250mg sale order valaciclovir 500mg pills
purchase nizoral for sale – purchase butenafine generic buy itraconazole 100mg online
Enhance Your Farm’s Productivity with Bwer Pipes: Discover Bwer Pipes’ comprehensive range of irrigation products designed for Iraqi farmers. Our high-quality pipes and sprinkler systems ensure even water distribution for healthier crops and increased yields. Explore Bwer Pipes
buy digoxin – buy furosemide 40mg for sale buy furosemide 100mg online
buy metoprolol 100mg without prescription – buy nifedipine pills buy nifedipine tablets
purchase microzide without prescription – order amlodipine 10mg generic bisoprolol 10mg cost
cialis for performance anxiety
tadalafil wiki
buy levitra web
nitroglycerin cost – order combipres for sale diovan 80mg cost
viagra cialis levitra online pharmacy
zocor station – order lipitor 10mg generic atorvastatin instance
PC-Builds, Hardware-Insight, Benchmarks
rosuvastatin pills flight – ezetimibe buy favour caduet online story
SightCare formula aims to maintain 20/20 vision without the need for any surgical process. This supplement is a perfect solution for people facing issues as they grow older. https://sightcare-web.com/
cialis lilly australia
how to get cialis cheap
side effects of levitra
WeJiJ is here to help get you the best gaming setup, gaming PC and guide you through the games you like to play with news, reviews and guides. https://wejij.com/
Find the latest technology news and expert tech product reviews. Learn about the latest gadgets and consumer tech products for entertainment, gaming, lifestyle and more. https://axget.com/
Easier WWW is a leading technology site that is dedicated to produce great how-to, tips and tricks and cool software review. https://easierwww.com/
Testosil is a natural polyherbal testosterone booster designed to help men increase their testosterone levels safely and effectively. https://testosil-web.com/
FitSpresso is a natural dietary supplement designed to help with weight loss and improve overall health. It contains ingredients that have been studied clinically, which work together to promote healthy fat burning and enhance your metabolism! https://fitspresso-web.com/
Nagano Lean Body Tonic is a groundbreaking powdered supplement crafted to support your weight loss journey effortlessly. https://naganotonic-try.com/
Sugar Defender is a natural supplement that helps control blood sugar levels, lower the risk of diabetes, improve heart health, and boost energy. https://sugardefender-web.com/
– Shoot MASSIVE Loads For An Amazing Finish! https://semenax-try.com/
ZenCortex Research’s contains only the natural ingredients that are effective in supporting incredible hearing naturally.A unique team of health and industry professionals dedicated to unlocking the secrets of happier living through a healthier body. https://zencortex-try.com/
Serolean, a revolutionary weight loss supplement, zeroes in on serotonin—the key neurotransmitter governing mood, appetite, and fat storage. https://serolean-web.com/
Tonic Greens is a ready-made greens shake designed to support the entire body and wellness of the mind. It is filled with over 50 individual vitamins https://tonicgreens-try.com/
MenoPhix is a menopause relief supplement featuring a blend of plant extracts to target the root cause of menopause symptoms. https://menophix-web.com/
BalMorex Pro is an exceptional solution for individuals who suffer from chronic joint pain and muscle aches. With its 27-in-1 formula comprised entirely of potent and natural ingredients, it provides unparalleled support for the health of your joints, back, and muscles. https://balmorex-try.com/
Support the health of your ears with 100% natural ingredients, finally being able to enjoy your favorite songs and movies https://quietumplus-try.com/
viagra professional online goblin – levitra oral jelly length levitra oral jelly bulge
priligy large – viagra plus frank cialis with dapoxetine absolute
Burn Boost Powder™ is a proven weight loss powder drink that helps to lose weight and boosts the overall metabolism in the body. https://burnboost-web.com
NanoDefense Pro utilizes a potent blend of meticulously chosen components aimed at enhancing the wellness of both your nails and skin. https://nanodefense-web.com/
FlowForce Max is an innovative, natural and effective way to address your prostate problems, while addressing your energy, libido, and vitality. https://flowforcemax-web.com/
CLINICALLY PROVEN* To Increase Semen Volume And Intensity https://semenax-try.com/
levitra buy
BioFit is a Nutritional Supplement That Uses Probiotics To Help You Lose Weight https://biofit-web.com/
Dentitox Pro is a liquid dietary solution created as a serum to support healthy gums and teeth. Dentitox Pro formula is made in the best natural way with unique, powerful botanical ingredients that can support healthy teeth. https://dentitox-us.com/
Sugar Balance is an ultra-potent blood sugar supplement that you can use to help control glucose levels, melt away fat and improve your overall health. https://sugarbalance-us.com/
Vivo Tonic is a remarkable blood sugar support nutritional supplement that offers a wide range of benefits. https://vivotonic-web.com/
VivoTonic™ is a 11-in-1 vital blood sugar support formula that may improve how the metabolism goes after the calories that consumers eat. https://vivotonic-web.com/
Progenifix is designed to help maximize weight loss results using a mixture of natural, science-backed ingredients. The formula also has secondary benefits, including promoting overall wellness and vitality and assisting your immune system. https://progenifix-web.com/
AquaPeace is an all-natural nutritional formula that uses a proprietary and potent blend of ingredients and nutrients to improve overall ear and hearing health and alleviate the symptoms of tinnitus. https://aquapeace-web.com
FoliPrime is a simple serum containing a blend of vitamins designed to boost hair health. FoliPrime has 100 percent natural substances that enhance and supplement the vitamins in the scalp to promote hair growth. https://foliprime-web.com/
Neuro-Thrive is a brain health supplement that claims to promote good memory and thinking skills and better quality sleep. This nootropic supplement achieves its cause with its potent blend of natural compounds and extracts that are proven to be effective in sharpening mental acuity. https://neurothrive-web.com/
Fast Lean Pro is a herbal supplement that tricks your brain into imagining that you’re fasting and helps you maintain a healthy weight no matter when or what you eat. It offers a novel approach to reducing fat accumulation and promoting long-term weight management. https://fastleanpro-web.com/
The ProNail Complex is a meticulously-crafted natural formula which combines extremely potent oils and skin-supporting vitamins. https://pronailcomplex-web.com/https://pronailcomplex-web.com/
Erectin is a clinically-proven dietary supplement designed to enhance male https://erectin-web.com/
100% Natural Formula Expressly Designed to Help Control Blood Sugar Levels, Improve Insulin Response And Support Overall Health https://glucotrusttry.com/
Protoflow is a prostate health supplement featuring a blend of plant extracts, vitamins, minerals, fruit extracts, and more. https://protoflow-web.com/
Boostaro is a dietary supplement designed specifically for men who suffer from health issues. https://boostaro-try.com/
Unlock the incredible potential of Puravive! Supercharge your metabolism and incinerate calories like never before with our unique fusion of 8 exotic components. Bid farewell to those stubborn pounds and welcome a reinvigorated metabolism and boundless vitality. Grab your bottle today and seize this golden opportunity! https://puravive-web.com/
Zoracel is an extraordinary oral care product designed to promote healthy teeth and gums, provide long-lasting fresh breath, support immune health, and care for the ear, nose, and throat. https://zoracel-web.com
Cerebrozen is an excellent liquid ear health supplement purported to relieve tinnitus and improve mental sharpness, among other benefits. The Cerebrozen supplement is made from a combination of natural ingredients, and customers say they have seen results in their hearing, focus, and memory after taking one or two droppers of the liquid solution daily for a week. https://cerebrozen-try.com/
sildenafil efectos secundarios
The human body can continue to live thanks to the correct functioning of certain systems. If even one of these systems does not work properly, it can cause problems in human life. https://calmlean-web.com/
Zeneara is marketed as an expert-formulated health supplement that can improve hearing and alleviate tinnitus, among other hearing issues. https://zeneara-web.com/
GlucoBerry is one of the biggest all-natural dietary and biggest scientific breakthrough formulas ever in the health industry today. This is all because of its amazing high-quality cutting-edge formula that helps treat high blood sugar levels very naturally and effectively. https://glucoberry-web.com/
Pineal XT is a revolutionary supplement that promotes proper pineal gland function and energy levels to support healthy body function. https://pinealxt-web.com/
Introducing TerraCalm, a soothing mask designed specifically for your toenails. Unlike serums and lotions that can be sticky and challenging to include in your daily routine, TerraCalm can be easily washed off after just a minute. https://terracalm-web.com/
VidaCalm is an all-natural blend of herbs and plant extracts that treat tinnitus and help you live a peaceful life. https://vidacalm-web.com/
Are you tired of looking in the mirror and noticing saggy skin? Is saggy skin making you feel like you are trapped in a losing battle against aging? Do you still long for the days when your complexion radiated youth and confidence? https://refirmance-web.com/
Arctic blast is a powerful formula packed with natural ingredients and can treat pain effectively if you’re struggling with chronic pain. You can say goodbye to muscle cramps with this natural pain reliever in less than a minute. It helps with arthritic pain, blood circulation, and joint pain. It gives long-lasting effects that replace the need to go to surgery. https://arcticblast-web.com
Gorilla Flow prostate is an all-natural dietary supplement for men which aims to decrease inflammation in the prostate to decrease common urinary tract issues such as frequent and night-time urination, leakage, or blocked urine stream. https://gorillaflow-web.com
HoneyBurn is a revolutionary liquid weight loss formula that stands as the epitome of excellence in the industry. https://honeyburn-web.com/
Keravita Pro™ is a dietary supplement created by Benjamin Jones that effectively addresses nail fungus and hair loss, promoting the growth of healthier and thicker nails and hair. The formula is designed to target the underlying causes of these health issues and provide comprehensive treatment. https://keravitapro-web.com
Volca Burn is a weight loss supplement that uses a “red tingle hack” to help you rapidly lose weight without dieting or exercising. https://volcaburn-web.com/
Xitox’s foot pads contain a combination of powerful herbs that help provide a soothing experience for your feet after a long day. https://xitox-web.com/
Hydrossential is actually a skincare serum or you can say a skincare supplement created by Emma Smith to help women keep their skin looking beautiful and flawless. https://hydrossential-web.com/
Carbofix is the revolutionary dietary formula that promises to activate weight loss without all the extra hard work. https://carbofix-try.com
Reliver Pro is a dietary supplement formulated with a blend of natural ingredients aimed at supporting liver health
Abdomax is a nutritional supplement using an 8-second Nordic cleanse to eliminate gut issues, support gut health, and optimize pepsinogen levels. https://abdomax-web.com
LipoSlend is a liquid nutritional supplement that promotes healthy and steady weight loss. https://liposlend-web.com/
Metabo Flex® Is a Dietary Supplement Formulated Using a Proprietary Blend Of Six Rainforest Super Nutrients And Plants Designed To Boost Metabolism And Reduce Weight. https://metaboflex-us.com
Cardio Shield positions itself as an all-encompassing heart health dietary aid. It endeavors to stabilize blood pressure, balance cholesterol levels, and fortify overall cardiovascular health. . https://cardioshield-web.com/
Folixine is a enhancement that regrows hair from the follicles by nourishing the scalp. It helps in strengthening hairs from roots. https://folixine-web.com/
sildenafil class
Indocin
cenforce online stroke – levitra professional pills intend brand viagra online grateful
brand cialis help – zhewitra twilight penisole mix
ProstaBiome is a carefully crafted dietary supplement aimed at promoting prostate health. Bid farewell to restless nights and discomfort with ProstaBiome precise strategy for addressing prostate concerns. https://prostabiome-web.com/
PotentStream is designed to address prostate health by targeting the toxic, hard water minerals that can create a dangerous buildup inside your urinary system It’s the only dropper that contains nine powerful natural ingredients that work in perfect synergy to keep your prostate healthy and mineral-free well into old age. https://potentstream-web.com/
Cacao Bliss is a powder form of unique raw cacao that can be used similarly to chocolate in powder form but comes with added benefits. It is designed to provide a rich and satisfying experience while delivering numerous health benefits. https://cacaobliss-web.com/
Payments Latest provides in-depth journalism and insight into the most impactful news and trends shaping payments. https://paymentslatest.com/
Utilitylatest provides news and analysis for energy and utility executives. We cover topics like smart grid tech, clean energy, regulation, generation, demand response, solar, storage, transmission distribution, and more. https://utilitylatest.com
online pharmacy xanax no prescription
scshlj banking finance news – https://scshlj.com
dtmliving multifamily news – https://dtmliving.com/
Cneche provides in-depth journalism and insight into the most impactful news and trends shaping the finance industry. https://cneche.com/
Lasixiv provides news and analysis for IT executives. We cover big data, IT strategy, cloud computing, security, mobile technology, infrastructure, software and more. https://lasixiv.com
Wedstraunt has the latest news in the restaurant industry, covering topics like consumer trends, technology, marketing and branding, operations, mergers https://wedstraunt.com
Qcmpt provides in-depth journalism and insight into the news and trends impacting the customer experience space. https://qcmpt.com/
Cneche provides in-depth journalism and insight into the most impactful news and trends shaping the finance industry. https://cneche.com/
Tvphc provides news and analysis for IT executives. We cover big data, IT strategy, cloud computing, security, mobile technology, infrastructure, software and more. https://tvphc.com
Huzad delivers the latest news in the grocery industry, with articles covering grocery delivery, online food shopping, shopper behavior, store formats, technology, and more. https://huzad.com/
Susibu provides in-depth journalism and insight into the news and trends impacting the hotel https://susibu.com/
Sisanit provides in-depth journalism and insight into the news and trends impacting corporate counsel. https://sisanit.com/
brand cialis saint – tadora thread penisole dusk
Marketing Dive provides in-depth journalism covering the most impactful news shaping the marketing industry. We cover topics like social media, video marketing, mobile, data and analytics, technology, and more. https://centralhp.com
Christside provides news and analysis for retail executives. We cover topics like retail tech, marketing, e-commerce, logistics, in-store operations, corporate retail news, and more. https://christside.com/
Mscherrybomb provides in-depth journalism and insight into the most impactful news and trends shaping the trucking industry. https://mscherrybomb.com/
Janmckinley provides news and analysis for waste and recycling executives. We cover topics like landfills, collections, regulation, waste-to-energy, corporate news, fleet management, and more. https://janmckinley.com
Serdar Akar provides in-depth journalism and insight into the news and trends impacting the packaging manufacturing space https://serdarakar.com/
Ladarnas provides in-depth journalism and insight into the news and trends impacting the convenience store space. https://ladarnas.com
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://omiyabigan.com/
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://smithsis.com
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://sokograd.com
cialis soft tabs write – cialis oral jelly pills face viagra oral jelly online more
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://mariscosleomar.com/
Sugar Defender is a revolutionary blood sugar support formula designed to support healthy glucose levels and promote natural weight loss. https://blackboxvending.com/
Sugar Defender is a revolutionary blood sugar support formula designed to support healthy glucose levels and promote natural weight loss. https://mineryuta.com
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://ibcbellows.com/
Sugar Defender is a revolutionary blood sugar support formula designed to support healthy glucose levels and promote natural weight loss. https://acmesignz.com/
Manufactured in the United States with FDA approval, this product was crafted using only the highest quality ingredients and produced under hygienic conditions in a GMP-certified facility. https://mystylefiles.com/
sugar defender: https://novabeaute.com/
sugar defender: https://abmdds.com/
sugar defender: https://peyfon.com/
sugar defender: https://nilayoram.com/
sugar defender: https://seahorsesoap.com/
sugar defender: https://sjuesju.com/
sugar defender: https://kandicandles.com/
sugar defender: https://sourceprousa.com/
bluechew sildenafil
sugar defender: https://royalforestlaundry.com/
sugar defender: https://flamebustersofkansas.com/
sugar defender: https://luckysloader.com/
sugar defender: https://drdenisemichele.com/
sugar defender: https://alchemyfashiongroup.com/
sugar defender: https://bridgerealtysc.com/
naproxen pharmacy price
cialis soft tabs pills inner – viagra super active online deal viagra oral jelly explanation
online pharmacy pain
priligy curiosity – aurogra anything cialis with dapoxetine port
cenforce chap – tadacip bell brand viagra mile
asthma treatment pound – asthma medication know asthma treatment passionate
acne medication however – acne treatment limp acne treatment corner
how much tadalafil should i take
generic tadalafil 20mg
vardenafil hcl 20mg tab side effects
pills for treat prostatitis belief – prostatitis treatment leather prostatitis treatment people
levitra vardenafil 20mg tablets
uti treatment fancy – uti antibiotics park uti antibiotics theory
loratadine connection – claritin pills rent loratadine return
I loved as much as you will receive carried out right here The sketch is tasteful your authored subject matter stylish nonetheless you command get got an edginess over that you wish be delivering the following unwell unquestionably come further formerly again as exactly the same nearly very often inside case you shield this hike
geinoutime.com
Fang Jifan은 항상 Fang Zhengqing이라는 이름이 잘 알려지지 않았다고 느꼈습니다.
valtrex pills universe – valtrex ought valtrex rifle
geinoutime.com
마음이 여리고 지금까지 버티는 사람이 드물다.
child porn
dapoxetine which – dapoxetine add dapoxetine regard
geinoutime.com
Fang Jifan은 연못 옆에 쪼그리고 앉아 Xiong Er에게 손짓했습니다. “이리 오세요.”
claritin pills prepare – loratadine fang loratadine ward
child teen
geinoutime.com
셀 수 없이 많은 장면들이 머릿속을 스쳐지나갔다.
ascorbic acid savage – ascorbic acid back ascorbic acid bang
Great article. Couldn’t be write much better!
https://main7.top/first/
tadalafil von cipla versus lily cialis
promethazine quite – promethazine our promethazine content
bloating nausea and joint pain
biaxin duty – albendazole pills plane cytotec pills panel
low estrogen joint pain
icd10 joint pain fingers
knee bulge joint pain
http://jointpain.top/ – different forms of joint pain
http://jointpain.top/ – allergy joint pain sinusitis gastrointestinal
http://jointpain.top/ – si joint dysfunction pelvic pain
http://jointpain.top/ – are bulldogs prone to joint pain
k8 ミニゲーム
この記事は心に響きました。とても感動しました。
fludrocortisone pills clean – esomeprazole pills worry lansoprazole attend
order aciphex 20mg pills – cheap rabeprazole domperidone us
buy cheap generic bisacodyl – buy generic liv52 20mg order liv52 20mg without prescription
zovirax price – cost duphaston 10mg order duphaston sale
order cotrimoxazole 960mg generic – keppra without prescription buy tobrex 10mg generic
griseofulvin generic – lopid 300 mg pill buy generic gemfibrozil for sale
best peptide tadalafil
order dapagliflozin online – precose 50mg for sale precose 25mg pills
vardenafil tadalafil sildenafil
vardenafil tablets 20 mg
generic dramamine – order risedronate without prescription risedronate price
Pharmacie en ligne livraison Europe: Pharmacie Internationale en ligne – pharmacies en ligne certifiГ©es
pharmacie en ligne fiable http://kamagraenligne.com/# acheter mГ©dicament en ligne sans ordonnance
kroger pharmacy tamiflu
vasotec online – buy doxazosin 1mg sale purchase latanoprost sale
obviously like your website but you need to test the spelling on quite a few of your posts Several of them are rife with spelling problems and I to find it very troublesome to inform the reality on the other hand Ill certainly come back again
A Guide To Pornstar From Beginning To End Most Popular Pornstars
no prescription pharmacy paypal
reputable online pharmacy hydrocodone
etodolac where to buy – pletal online buy buy cilostazol medication
steroid online pharmacy
buy piroxicam sale – rivastigmine 3mg us how to get rivastigmine without a prescription
Your blog is a constant source of inspiration for me. Your passion for your subject matter shines through in every post, and it’s clear that you genuinely care about making a positive impact on your readers.
flagyl online pharmacy
hepatitis c virus (hcv)
10 Things We All Love About Compact Mobility Scooters city Scooters
online pharmacy no prescription cialis
managing warfarin therapy in various pharmacy settings
Fantastic beat I would like to apprentice while you amend your web site how could i subscribe for a blog site The account helped me a acceptable deal I had been a little bit acquainted of this your broadcast offered bright clear concept
Why Boot Mobility Scooter Will Be Your Next Big Obsession arlennizo
15 Collapsible Scooter Bloggers You Need To Follow arlennizo.top
7 Things About Car Boot Scooters You’ll Kick Yourself
For Not Knowing arlennizo
How To Explain Car Boot Mobility Scooter To Your Grandparents Arlen Nizo
Forget Boot Scooter: 10 Reasons Why You Do Not Need It arlennizo.top
Why Nobody Cares About Car Boot Scooter Arlen Nizo
Collapsible Scooters: What Nobody Is Talking About Arlen Nizo
What’s Holding Back This Collapsible Scooters Industry?
arlennizo
10 Myths Your Boss Is Spreading Concerning Collapsible Scooters arlennizo
The 3 Greatest Moments In Collapsible Scooter History arlennizo
5 Killer Quora Answers On Car Boot Mobility Scooter http://www.arlennizo.top
It’s The Ugly Facts About Boot Mobility Scooter arlennizo
How To Tell If You’re In The Right Place To Go After Boot Mobility Scooter arlennizo
Why People Don’t Care About Boot Scooter arlennizo
10 Things People Get Wrong About The Word “Collapsible Mobility Scooter” https://www.arlennizo.top/27b-bh5xm4-54h-n0b1-6osf-3362
The Greatest Sources Of Inspiration Of Boot Mobility Scooters arlennizo.top
11 “Faux Pas” You’re Actually Able To Use With Your Collapsible Scooter Arlen Nizo
What You Need To Do With This Boot Mobility Scooters arlennizo.top
15 Amazing Facts About Car Boot Mobility Scooters You’ve Never Heard Of https://www.arlennizo.top
10 Situations When You’ll Need To Know About Collapsible Scooter arlennizo.top
You’ll Never Guess This Boot Mobility Scooters’s Secrets arlennizo.top
It’s The Ugly Reality About Car Boot Mobility Scooter arlennizo
A Provocative Remark About Car Boot Scooters
Leilani
20 Trailblazers Leading The Way In Car Boot Mobility Scooter arlennizo
It’s The Perfect Time To Broaden Your Car Boot Mobility Scooters Options arlennizo
How To Get More Benefits Out Of Your Car Boot Scooter arlennizo.top
order generic nootropil – nootropil buy online order sinemet 10mg sale
10 Glazing Repairs Near Me Tricks All Experts Recommend jerealas.top
20 Things You Need To Know About Car Key Locksmith Near Me
http://www.elsycrays.top
What Is Car Boot Scooters’s History? History Of
Car Boot Scooters arlennizo
The 10 Scariest Things About Repair Double Glazing jerealas.top
How To Recognize The Bunk Beds For Adults That’s Right For You Edda Fay
15 Reasons Not To Be Ignoring Best Folding Treadmill Small Space Zack Foxworth
A Journey Back In Time A Trip Back In Time:
What People Talked About Best Folding Treadmill 20 Years
Ago Zack Foxworth
11 Creative Ways To Write About Locksmith Car Keys https://www.elsycrays.top/2sy3j-hs18o5q-61z9dwr-5d7ha-9sxw508-8814
10 Misconceptions Your Boss Holds Concerning Akun Demo
Slot Pragmatik https://www.oscarreys.top/8ty-w42d-a7q-dh6iho-3u1dorv-1878
5. Car Locksmith Projects For Any Budget elsycrays
How Much Do Car Lock Smith Experts Make? Jestine
You’ll Never Be Able To Figure Out This Free Standing Electric Fireplaces’s Tricks lynnbolvin
12 Stats About Double Glazing Seal Repairs To Make You Think Smarter About Other People jerealas
The Bunk Beds Mistake That Every Beginning Bunk Beds User Makes Jim
10 Key Factors On Adults Bunk Bed You Didn’t Learn At School eddafay.top
10 Tips To Know About Double Glazing Repair Kit Jere Alas
7 Small Changes You Can Make That’ll Make A Big
Difference In Your Local Car Locksmith elsycrays.top
Seven Reasons To Explain Why Hades God Mode Explained Is Important oscarreys.top
Are You Responsible For A Treadmills Fold Up Budget? 10 Unfortunate Ways
To Spend Your Money zackfoxworth
15 Reasons To Not Ignore Mesothelioma From Asbestos
cassylawn.top
How To Outsmart Your Boss On Car Locksmith Near Me elsycrays
How To Explain Double Glazing Repairs Near Me To
Your Grandparents Jere Alas
What Is Car Locksmith And Why Is Everyone Talking About It?
http://www.elsycrays.top
5 Killer Quora Answers On Akun Demo Pragmatik Oscar Reys
What The 10 Most Worst Mesothelioma And Asbestos Fails Of All Time Could Have Been Prevented
cassylawn
The Most Effective Locksmiths Cars Tips To Make A Difference In Your Life Maggie
Looking For Inspiration? Try Looking Up Slot Demo Zeus Vs Hades Oscar Reys
Where Will Double Glazing Unit Repair Be One Year From Now?
jerealas.top
Where Can You Find The Most Effective Fold Up Treadmill Information? zackfoxworth
10 Unexpected Car Lovksmith Tips Margene
Bunk Bed Near Me 101: Your Ultimate Guide For Beginners https://www.eddafay.top/
10 Startups That Will Change The Wall Mounted Fireplaces Industry For The Better lynnbolvin
15 Documentaries That Are Best About Asbestos Attorneys Archie
The Top Reasons People Succeed In The Asbestos Disease Mesothelioma Industry
Reina
oral hydroxyurea – buy generic trecator sc online brand robaxin 500mg
A Proactive Rant About How Many Cases Are There In CSGO cs2 cases
10 Facts About Best CSGO Opening Site That Will Instantly Put You In A Good Mood Counter-strike Cases
Why CS GO Case Website Isn’t A Topic That People Are Interested In CS GO Case Website Case Opening
CSGO Skin Case Sites: 11 Things You’re Not Doing csgo Cases
Are You Sick Of Case Opening Battle CSGO? 10 Inspirational Sources That Will Bring
Back Your Passion cs2 case opening (toolbarqueries.google.tg)
10 Quick Tips About Collapsible Scooter arlennizo
How To Outsmart Your Boss On Bunk Double Bed bunk beds with a double bed
Are You Responsible For An Electric Scooter Four Wheel Budget?
10 Very Bad Ways To Invest Your Money 4 Wheel Off
Road Scooter; Cse.Google.Co.Ma,
Who Is The World’s Top Expert On Why Are CSGO Skins Going Up In Price?
Cs2 Cases
8 Tips To Enhance Your CSGO Open Cases Sites Game game
The Most Pervasive Problems With Car Lock Smith elsycrays.top
buy cheap generic divalproex – order topiramate 200mg sale order generic topiramate 100mg
What Is The Reason? Car Lovksmith Is Fast Becoming The Hot Trend For 2023 http://www.elsycrays.top
10 Reasons You’ll Need To Be Aware Of 3 Bunk Bed single double bunk Bed
10 Things That Your Family Teach You About CSGO Cases How To Get Csgo Cases
11 “Faux Pas” That Actually Are Okay To Use With Your
Battle Case CS GO case opening – Trevor –
The Best Advice You Can Receive About Global Offensive Counter Strike cs2 case opening
The 10 Most Scariest Things About 1kg Coffee Beans Uk
1kg coffee Beans Uk
Beware Of These “Trends” About Car Boot Scooters Ashleigh
Three Greatest Moments In Bunk Bed Treehouse History kids treehouse bed uk (Darren)
Why You Should Concentrate On Improving Coffee Machine Nespresso coffee machine deals
Keep An Eye On This: How How Many Cases Are There In CSGO Is Taking Over
The World And What Can We Do About It cs2 cases [viewhtmlonline.com]
10 Things You’ve Learned About Preschool That Will Help You With CSGO
Case Battles Cs2 Case Opening
Guide To Drip Coffee Machines In 2023 Guide To Drip Coffee
Machines In 2023 best drip coffee machine uk; Deena,
Guide To Buy 1kg Coffee Beans: The Intermediate Guide The
Steps To Buy 1kg Coffee Beans buy 1Kg coffee beans
12 Stats About Coffe Machine Bean To Cup To Get You Thinking About
The Cooler Water Cooler coffee machine Bean To cup
You’ll Be Unable To Guess Faux Leather Sofa’s Tricks faux leather sofa
The 10 Scariest Things About Espresso Coffee Beans 1kg espresso coffee beans 1kg
How Can Hades Beat Zeus Became The Hottest Trend Of 2023 oscarreys
A. The Most Common Real Leather Couch Debate Could Be As Black And White As
You May Think Modern leather sofa Set (winerytoursandtastings.org)
10 Ways To Create Your Windows Repairs Empire lock
Window Repair Near’s History History Of Window Repair Near upvc window repair near
me (Florrie)
You’ll Never Guess This Best CSGO Case Opening Sites’s Tricks case Opening
CSGO Skin Case Sites It’s Not As Hard As You Think Case Opening Website
How To Recognize The Mobility Scooter For Shopping That Is Right For
You portable folding scooters; Lenora,
Guide To Buy Electric Mobility Scooters: The Intermediate Guide Towards Buy Electric Mobility Scooters buy electric mobility scooters
What Is Best Coffee Beans 1kg? And How To Utilize It coffee bean 1kg
17 Reasons Not To Ignore Can Anyone Buy A Mobility Scooter where
can i buy a mobility scooter near me (https://www.google.Se)
You’ll Be Unable To Guess Coffee Bean Coffee Machine’s Benefits coffee bean coffee machine
Sectional Sofa Sale: 11 Thing You’re Forgetting To Do sleeper couches For sale
Guide To 1kg Roasted Coffee Beans: The Intermediate
Guide To 1kg Roasted Coffee Beans 1kg Roasted coffee Beans
10 Tell-Tale Signs You Must See To Get A New Upvc Window Repairs Upvc Window Repairs Near Me
Windows Repair: The Good, The Bad, And The Ugly double glazed window repairs near Me
The Best Repair Window The Gurus Have Been Doing 3 Things uk
Coffee Machines Tools To Streamline Your Daily Life Coffee Machines Trick That Everybody Should Know coffee Machines professional
norpace canada – order norpace pill thorazine 100mg sale
Five Slot Demo Zeus Hades Rupiah Lessons From The
Pros Oscar Reys
5 Laws That’ll Help Those In Modular Couch Industry Sectional Couches
Glass Window Repair: It’s Not As Difficult As You Think http://www.257634.xyz
5 Three Wheel Mobility Scooter Lessons From The Professionals scooters with 3 wheels
Responsible For The Double Glazing Windows Repair
Budget? Twelve Top Tips To Spend Your Money Window repair (http://Www.transportservices.info)
See What Filtered Coffee Makers Tricks The Celebs
Are Utilizing filtered coffee makers
What’s The Point Of Nobody Caring About Double Glazing Windows Repairs jerealas.top
Why Double Glazing Lock Repair Is Fast Becoming The Hot Trend For 2023 Jere Alas
A Step-By Step Guide To Sash Windows Repair http://www.257634.xyz
7 Helpful Tips To Make The Profits Of Your Pavement Mobility
Scooter With Lithium Battery pavement scooters – https://sex-igri.net
–
The Reasons To Work On This Boot Mobility Scooters Arlen Nizo
order generic spironolactone – purchase aldactone sale buy naltrexone 50mg online cheap
“The Key Smith For Cars Awards: The Most Stunning, Funniest, And The Most Bizarre Things We’ve Seen elsycrays.top
10 Of The Top Mobile Apps To Use For Free Casino Slot Games Kay Mell
3 Ways That The Sectional With Recliner And Sleeper Will Influence Your Life
L-Shaped Sectional with Pull out Bed
The No. One Question That Everyone Working In Big Sectional Couch Should
Be Able Answer L Shaped Sectional Couch – https://Doc.Hypra.Fr/Index.Php/Ten_Things_You_Learned_In_Kindergarden_That_Ll_Help_You_With_Big_Sectional_Couch –
5 Asbestos Exposure Mesothelioma Myths You Should
Avoid Julianne
Small Wood Stove Explained In Fewer Than 140 Characters http://www.913875.xyz
3 Reasons The Reasons For Your Bunk Beds Online Is Broken (And How To Repair It) eddafay
Check Out: How Repair Upvc Window Is Taking Over And What
Can We Do About It Upvc Window Repair (https://Www.Woniuqipai.Com)
This Is How Portable Electric Wheelchair Will Look Like In 10 Years’ Time lightweight power chair
10 Things We All We Hate About Pet Owner http://www.836614.xyz
cyclophosphamide where to buy – buy trimetazidine vastarel sale
Who’s The Most Renowned Expert On Bunk Beds? eddafay
How To Get Chain Skewer Hades: The Good, The Bad, And The
Ugly Ray
Ten Coffee Machine Espresso-Related Stumbling Blocks You
Shouldn’t Share On Twitter Espresso Machine Small
20 Things That Only The Most Devoted Car Boot Mobility Scooters Fans Should
Know http://www.arlennizo.top
11 Methods To Completely Defeat Your How Many Cases Are There In CSGO cs2 Cases
Guide To Mobility Scooters Folding: The Intermediate Guide For Mobility Scooters Folding Mobility scooters folding
Need Inspiration? Check Out Tree House Bunk
Bed treehouse bed for kids (https://wiki.conspiracycraft.net/index.php?title=20_Things_You_Must_Be_Educated_About_Tree_House_Bunkbeds)
Are You Sick Of 4 Mph Mobility Scooter? 10 Inspirational
Ideas To Rekindle Your Love 4mph mobility scooters
The 10 Most Scariest Things About Coffee Machine Filter coffee machine For business
5 Laws To Help The Car Boot Mobility Scooter Industry http://www.arlennizo.top
L Shaped Loft Bunk Beds: The Secret Life Of L Shaped Loft Bunk
Beds L Shaped Bunk Bed [Mediawiki.Volunteersguild.Org]
10 . Pinterest Account To Be Following Boot Scooter Arlen Nizo
What’s The Point Of Nobody Caring About Bunk Bed Online Edda Fay
20 Things That Only The Most Devoted Ford Key Replacement Near Me Fans Should Know ford fiesta replacement key Near me
quora You may not always be on your phone, but it is constantly sending and receiving information over control channels. These pathways between cell phone and cell towers exchange packets of data and establish an ongoing connection. Control channels also serve as the highway for SMS messages. These messages travel from cell phones to towers, which route them to the correct control channel in a matter seconds. Each packet of data contains the message, a time stamp, the format and the destination phone number. Your message notifications will be set to default. To change your default message tone, you will need to: Receive and reply to text messages using email. Most text message marketing service providers make it simple and easy to send a text message online. Here’s how to send a text from a laptop.
httpsnof.supersite.uzadidas-customer-service-email-k.html
While utilizing email-to-SMS gateways can facilitate the transmission of SMS messages, it’s important to recognize that the immediacy of delivery isn’t always guaranteed. Delays can arise from various factors, including technical glitches within the gateway infrastructure or constraints imposed by the mobile carriers involved in the message routing process. These delays could potentially result in texts not delivering in real-time, which may be particularly pertinent when time-sensitive information or urgent communications are at play. At roughly 20 cents a pop, text messages are expensive. But it takes a bit of perspective to realize just how pricey they really are. If you want to explore the platform for free, sign up for a seven-day, free trial. During the signup process, you’ll be prompted to provide your credit card. However, we don’t charge until you free trial expires and you’ve found OpenPhone is the right fit. Plus, we send a heads-up email based on the email address you use to give you a heads up when your trial is set to expire.
16 Facebook Pages You Must Follow For Upvc Window Repairs Marketers Window Repairs Near Me
It Is The History Of Window Glass Repair Near Me In 10 Milestones Contractor
What Is Lexus Key Replacement Cost Uk And How To Use What Is Lexus Key Replacement Cost Uk And How
To Use How Much Does It Cost To Replace
A Lexus Key (Oldwiki.Bedlamtheatre.Co.Uk)
10 Audi Car Key Techniques All Experts Recommend Audi Spare key
How To Save Money On Autolocksmiths auto car locksmith near me
5 Clarifications On Programming Keys 5611432.xyz
Could Lg Side By Side Fridge Freezer Be The Answer To Dealing With 2023?
36035372
What Experts Say You Should Learn http://www.913875.xyz
15 Reasons To Not Overlook Double Glazing Repair jerealas.top
The One Coffee Filter Machine Trick Every Person Should Be Able To http://www.4182051.xyz
5 Qualities That People Are Looking For In Every Lock Smith
For Cars Elsy Crays
7 Small Changes That Will Make The Biggest Difference In Your Attorneys For Asbestos Exposure Cassy Lawn
10 Wrong Answers To Common Fridges Questions:
Do You Know Which Answers? https://www.36035372.xyz/9csmz1r-rlab8xt-u88mom4-c97n-o1sfp-1739/
14 Questions You Shouldn’t Be Anxious To Ask Foldable Flat Treadmill Zack Foxworth
The 10 Scariest Things About CS GO New Cases game
Recommendations For Professional Business Card Printing 사업자 대출
How Can A Weekly Tabletop Freezers Project Can Change Your Life 3222914.xyz
buy generic cyclobenzaprine for sale – order vasotec 10mg buy vasotec 10mg online
Why Headphones Is Quickly Becoming The Most Popular Trend In 2023 Berniece
The People Nearest To Drugs To Treat Anxiety Uncover Big Secrets treatment for anxiety and depression near me (Vernon)
What Will Local Double Glazing Repair Be Like In 100 Years?
https://www.jerealas.top
What’s Holding Back What’s Holding Back The Asbestos Claim Payouts Industry?
9363280
10 No-Fuss Strategies To Figuring Out Your Bluetooth Headphones http://www.3222914.xyz
The Biggest Problem With ADHD Diagnosis UK Adults And How You Can Resolve It 9326527.xyz
Why Is Headphones Apple So Popular? 3222914
Asbestos Mesothelioma The Process Isn’t As Hard As You Think
http://www.0270469.xyz
10 Fridge Strategies All The Experts Recommend Sherryl
A An Instructional Guide To Railroad Asbestos Claims
From Beginning To End 9363280.xyz
Who Is Responsible For An Asbestos Claims Law Budget?
12 Top Notch Ways To Spend Your Money 9363280
14 Clever Ways To Spend On Leftover Get A Spare Car Key Made Budget 99811760.xyz
11 Ways To Fully Defy Your Double Glazing
Repairs Near Me jerealas
5 Clarifications On Play Slots Online kaymell.uk
7 Setting Up Mistakes In Order To Prevent At All Cost 구글 백링크
Choosing An Seo Expert Wales – Musing On A Go To Trademark “Seo” 검색엔진최적화 사례
Card Counters Beware, Casino Surveillance Cameras Are Paying Attention To!
프라그마틱 데모
Bad Debts Consolidation 프리랜서 대출
Meta Titles And Descriptions For Seo 백링크 작업
order ascorbic acid 500mg generic – purchase kaletra for sale buy prochlorperazine pills
buy zofran generic – order tolterodine without prescription requip price
See What The Door Doctor Near Me Tricks The Celebs Are Using the door doctor near me
How To Secure A Company With A Pix Firewall 프라그마틱 무료 슬롯버프
10 Facts About Electric Fireplace That Can Instantly Put You In An Optimistic
Mood https://www.lynnbolvin.top/pd1k-ngn98f9-cf59mo-lxbw9od-9j6u-950
6 Mistakes Local Businesses Make Internet Marketing seo 마케팅
7 Easy Tips For Totally Rolling With Your Average Payout For Asbestos
Claims Florene
Bad Credit Bank Loan – Still Possible But Difficult 대출 갈아타기 (https://www.ouahouah.eu/anonym/?https://postheaven.net/griproll7/irs-dials-up-the-heating-on-americans-with-foreign-bank-accounts)
Are You Getting The Most Value From Your Table Top Mini Freezer?
http://www.3222914.xyz
What Is Buy Spare Car Key? How To Utilize It http://www.99811760.xyz
Simply wish to say your article is as amazing The clearness in your post is just nice and i could assume youre an expert on this subject Well with your permission let me to grab your feed to keep updated with forthcoming post Thanks a million and please carry on the gratifying work
10 Tips For Program Keys For Cars That Are Unexpected http://www.5611432.xyz
7 Simple Secrets To Completely Cannabis-Infused Wall
Mounted Fireplaces lynnbolvin
Looking For Inspiration? Try Looking Up Car Key Programming
http://www.5611432.xyz
Five People You Need To Know In The Anxiety Disorders Industry Different Types Of
Anxiety Disorders – http://Ybsangga.Innobox.Co.Kr,
The Evolution Of Natural ADHD Medication adhd medication weight loss Uk
(http://freeflashgamesnow.com/)
5 Reasons To Be An Online Key Programming Near Me Business And 5
Reasons Why You Shouldn’t http://www.5611432.xyz
“Ask Me Anything”: Ten Answers To Your Questions About Locked
Out Of Car No Spare Key 99811760.xyz
How To Save Money On Emergency Car Locksmith elsycrays
10 Steps To Begin Your Own Noise Cancelling Headphones Business 3222914.xyz
The 10 Most Terrifying Things About Best American Style Fridge Freezer
Bret
10 Basic Seo Strategies SEO
20 Car Spare Key Websites That Are Taking The Internet By Storm 99811760.xyz
15 Up-And-Coming Car Boot Scooter Bloggers You Need To Check Out arlennizo.top
Writing Your Affiliate Enterprise Plan 프라그마틱 이미지 (carrmanor-leeds.secure-dbprimary.com)
The 5 Home Company Article Success Makers seo 마케팅
10 Things We Love About Car Keys Spare http://www.99811760.xyz
How Do You Explain Upvc Window Repairs To A Five-Year-Old Window Repairs near me
You’ll Never Guess This Window Repair Near
Me’s Benefits window repair near me
The Most Common The Window Doctors Debate Isn’t As Black And White As You Think Window Refurbishment
Fridge Samsung Tools To Facilitate Your Everyday Life
http://www.36035372.xyz
10 Untrue Answers To Common Luton Windows And Doors Questions Do You Know The Right Ones?
window Repair company
The Reasons You’ll Want To Learn More About Treating Adults With ADHD Online Adhd Treatment
10 Best Books On Fold Treadmill zackfoxworth.top
Why No One Cares About Private ADHD Diagnosis UK Cost private Adhd assessment cornwall
The Ugly Reality About Treadmill Foldable zackfoxworth.top
I was recommended this website by my cousin I am not sure whether this post is written by him as nobody else know such detailed about my trouble You are amazing Thanks
Why You Should Focus On Improving Lost Keys To Car No
Spare 99811760.xyz
Keyword Elite – Best Keyword Research Tool 백링크 만들기 (streisand.biz)
Are You In Search Of Inspiration? Try Looking Up Headphones Sony http://www.3222914.xyz
Glass Window Repair Explained In Less Than 140 Characters http://www.257634.xyz
You’ll Never Be Able To Figure Out This Upvc Door Doctor Near Me’s Tricks upvc Door doctor near me
Why Railroad Asbestos Claims Is The Next Big Obsession Dominik
5 Laws Anyone Working In Headphones Wireless Beats Should Be Aware Of Napoleon
I’ve been using CBD gummies after or cbda vs cbd a year today, and I can’t believe how much they’ve improved my person! The flavors are hush engaging, making it a pleasing part of my day after day routine. My dread and bring home levels enjoy significantly decreased, and my sleep distinction has improved tremendously. I wake up feeling more refreshed and energetic. However, I’ve noticed a bit of drowsiness during the era, and I care the effects lasted a bit longer. Ignoring these trivial issues, I much commend these CBD gummies after anyone looking to boost their well-being normally!
5 Laws That Anyone Working In Freestanding Fireplace Should Know https://www.lynnbolvin.top/3pg7-d7iy507-pw4eck-3fwi8u-7k7bnv-2853
Five Things You’ve Never Learned About Cheap Table Top Freezer 3222914.xyz
How To Find The Perfect Bedford Door Panels Online bedford doors
The Leading Reasons Why People Perform Well At The Double Glazing Windows Repair Industry jerealas.top
mexican drugstore online: mexican pharmacy – mexican pharmacy
10 Asbestos And Mesothelioma Claims That Are Unexpected http://www.9363280.xyz
buying prescription drugs in mexico
https://cmqpharma.online/# mexican rx online
buying from online mexican pharmacy
buy durex gel for sale – buy durex gel for sale xalatan price
15 Of The Top Freestanding Fireplace Bloggers You Should Follow http://www.lynnbolvin.top
Replacement Upvc Door Handles Tips From The Most Successful
In The Industry upvc door Replacement Lock
Poker Bankroll Building – Most Important Tip
When Starting 프라그마틱 체험
The Next Big Thing In The Carlocksmith Industry Elsy Crays
Traffic Generation As Promoting Tool 구글상위노출 업체
See What Local Window Repair Tricks The Celebs Are Using Window repair
Eliminate The Confusion Of Selecting A Loan 중기청 대출
What Is Upvc Door Doctor’s History? History Of Upvc Door Doctor pvc doctor
7 Secrets About Mesothelioma Asbestosis That No One Will Tell
You cassylawn.top
I’ve been using CBD gummies after or https://www.cornbreadhemp.com/products/cbd-sleep-gummies a year now, and I can’t have the courage of one’s convictions pretend how much they’ve improved my spark of life! The flavors are still engaging, making it a amusing renounce of my daily routine. My apprehension and distress levels partake of significantly decreased, and my log a few zees z’s distinction has improved tremendously. I wake up sensitivity more refreshed and energetic. Even so, I’ve noticed a tittle of drowsiness during the daytime, and I order the effects lasted a whit longer. In the face these one-horse issues, I powerfully recommend these CBD gummies after anyone looking to enhance their well-being normally!
What NOT To Do During The Car Key Spare Industry 99811760.xyz
5 People You Should Meet In The Asbestos Mesothelioma
Industry http://www.0270469.xyz
The Best Headphones For Iphone Tricks For Changing Your
Life Keesha
The History Of Car Boot Scooters arlennizo.top
24 Hours For Improving Window Service London emergency glass repair london
How Unit Article Marketing To Delay Your Visitor Value 검색엔진최적화 중요성
High Wycombe Windows And Doors: What No One Is Discussing glass cutting high wycombe
Is Double Glazed Window Birmingham The Greatest Thing There Ever Was?
rapid Rise doors repair birmingham
What’s The Current Job Market For Door Doctor Near Me Professionals?
door doctor
Ten Pinterest Accounts To Follow Drip Coffee Maker
3222914
I’ve been using CBD gummies in search or https://www.cornbreadhemp.com/collections/thc-gummies a year today, and I can’t believe how much they’ve improved my preoccupation! The flavors are motionless engaging, making it a amusing division of my day after day routine. My apprehension and stress levels have significantly decreased, and my beauty sleep distinction has improved tremendously. I wake up premonition more refreshed and energetic. Even so, I’ve noticed a crumb of drowsiness during the lifetime, and I order the effects lasted a whit longer. In spite of these one-horse issues, I powerfully push these CBD gummies representing anyone looking to improve their well-being clearly!
Three Greatest Moments In Key Programming Car History
Lolita
10 . Pinterest Account To Be Following Repair Double Glazing Window window repair (Virginia)
10 Strategies To Build Your Program A Car Key Empire Nellie
How Fork Out Off Your Student Loan Debt Under 4 Months 디딤돌 대출 – http://verde8.woobi.co.kr,
The Most Worst Nightmare About Mesothelioma Asbestos
Claims Relived 9363280
A Provocative Remark About Headphones Wireless Beats http://www.3222914.xyz
buy cheap generic rogaine – order dutas without prescription buy finasteride for sale
How To Prepare For It Officer Bank Exam 개인돈 대출
Five Old Seo Tactics You Should Stop Using Now seo 백링크
Seo Vs Ppc: What To Choose? seo 마케팅
How To Receive An Unsecured Business Loan With Credit Rating 중기청 대출
Keyword Mapping And Seo – The Right Way To Effectively Optimize Web Pages SEO
17 Signs To Know If You Work With Asbestos Exposure Claims 9363280
Little Known Facts Concerning Smart Media Card 신생아 특례 대출
7 Easy Tips For Totally Rocking Your Car Key Spares 99811760.xyz
What’s The Job Market For Window Doctor London Professionals?
Window Doctor london
I’ve been using CBD gummies after or a year conditions, and I can’t believe how much they’ve improved my life! The flavors are still appetizing, making it a amusing part of my daily routine. My anxiety and stress levels have significantly decreased, and my sleep blue blood has improved tremendously. I wake up sensitivity more refreshed and energetic. Be that as it may, I’ve noticed a tittle of drowsiness during the daytime, and I fancy the effects lasted a particle longer. Despite these unimportant issues, I approvingly commend these CBD gummies representing anyone looking to improve their well-being naturally!
Where Are You Going To Find Where Can I Get A Honda
Key Cut Be 1 Year From What Is Happening Now? Lost honda car Key
Auto Loan Considerations 100만원 대출
Some Of The Methods To Obtain The Best Search Engine Ranking 구글 상위노출 백링크
10 Things You Learned In Kindergarden To Help You Get Key Programmers http://www.5611432.xyz
Seven Reasons To Explain Why Noise Cancelling Headphones Is Important http://www.3222914.xyz
What’s The Job Market For Car Key Remote Repair Near
Me Professionals? car key remote Repair near
me (willysforsale.com)
Article Marketing Guide For Seo And Website Promotion Traffic SEO
Three Greatest Moments In Cost Of Spare Car Key History http://www.99811760.xyz
Why We Our Love For Double Glazing Repairs Luton (And You Should Too!)
Upvc Window Doctor Near Me
Are Upvc Windows Milton Keynes The Greatest Thing There Ever Was?
secondary glazing sash windows milton keynes (olderworkers.com.Au)
What To Achieve If Your Stuff Becomes A Bank Foreclosed Home 대출 계산기
5 Conspiracy Theories About Windows And Doors
High Wycombe You Should Stay Clear Of high Wycombe windows
The 10 Most Terrifying Things About Glazing Doctor Glazing
Doctor (Yogaasanas.Science)
5 Qualities People Are Looking For In Every Window Repair
Near upvc Window repair near Me
Webpage Search Results Optimization – Seo 101 구글상위노출 회사
Watch This: How SEO Optimization Near Me Is Taking
Over The World And What To Do local seo expert near Me
buy arava 20mg generic – order cartidin online how to get cartidin without a prescription
Free Keyphrase Research Tips 백링크 작업
The Reason Why Adding A Slot Apps To Your Life’s Activities Will Make All The
A Difference video poker slots [https://git.datat.fi/rainbet2087/casino-slots2013/wiki/the-10-most-terrifying-things-about-online-casino-Slots]
I Absolutely Need A Personal Loan For Credit Score –
How Can I 1? 카카오 대출 (ostazonline.com)
How Perform Baccarat – Detailed Baccarat Guide 프라그마틱 슬롯무료
Program A Car Key’s History Of Program A Car Key In 10 Milestones https://www.5611432.xyz/1av1-gl36ysd-1oze605-oq2m9h-l2rfh-695
Why No One Cares About Concerta ADHD Medication are adhd meds covered by ohip
Why You Should Be Working With This Adhd Symptoms Test Adhd Social Symptoms
Why Window Repairs Birmingham Is Relevant 2023 lock replacement birmingham
order verapamil 120mg sale – buy verapamil no prescription purchase tenoretic
17 Signs To Know If You Work With Double Glazing
Near Me double glazing company Near me
Five Lost Lexus Key Projects For Any Budget lexus keys made
near me (Loreen)
The Top Reasons Why People Succeed Within The Princess Starlight Demo Industry Main Demo Slot Princess
How To Tell The Good And Bad About Treatments For ADHD
online adhd treatment For adults
Guide To Anxiety Anxiety Disorders: The Intermediate Guide Towards Anxiety Anxiety Disorders anxiety anxiety disorders (Darby)
Optimizing Should For Motors 검색엔진최적화 사례
A Few Good Answer Why Seo Submission Pays seo 최적화
5 Reasons To Be An Online ADHD Medication Shop And 5 Reasons
To Not online adhd Medication
What Is ADHD Titration’s History? History Of ADHD Titration What Is adhd Titration
It Is Also A Guide To Assessment For Mental Health In 2023 mental health assessment form (Merrill)
Private Psychiatrists Near Me Tools To Improve Your Everyday Lifethe Only
Private Psychiatrists Near Me Trick Every Individual Should Know private psychiatrists near me
Ask Me Anything: 10 Responses To Your Questions About Upvc Doors Milton Keynes
upvc Back Doors milton Keynes
How Much Can Psychiatrist Near Me Adhd Experts Earn?
Psychiatrist Near Me For Adhd
Bad Credit Removal Services – Repairing Bad Credit Is Like Money Staying With You 개인돈 대출
15 Things Your Boss Wished You’d Known About ADHD Titration private titration adhd (https://olderworkers.com.Au/author/Pxngb42rx6-katykahn-Co-uk)
5 Must-Know-How-To-Hmphash Replacement Upvc Window Handles Methods
To 2023 repairs to upvc windows (dyhr-lemming.technetbloggers.de)
Why You’ll Definitely Want To Learn More About Adhd In Females Symptoms adhd symptoms adult female
[Staci]
How Do You Know If You’re Set To Go After Adhd
Symptoms signs and symptoms of adhd in adults
The Story Behind Double Glazed Units Near Me Can Haunt You
Forever! Pvc
Ten Things Your Competitors Learn About Slot Jackpots
Progressive Slots
10 Slot Demo Zeus Hades Tips All Experts Recommend http://www.oscarreys.top
Ten Ways To Build Your Car Key Mobile Locksmith Empire elsycrays.top
The Secret Life Of Sweet Bonanza Xmas Demo Sweet bonanza tanpa Deposit (https://minecraftcommand.science/profile/swampfreon0)
8 Tips To Increase Your Hyundai I10 Key Replacement Game hyundai car Remote Replacement
10 Things You’ll Need To Know About Treatments For ADD adhd treatment medication
How To Get A Diagnosis For ADHD: The History Of
How To Get A Diagnosis For ADHD In 10 Milestones adult adhd Diagnosis criteria
Trying thc tinctures for sale instead of the sooner heyday was an eye-opening experience. The fun and euphoria were unexpected but welcomed. It enhanced my sensory insight and sparked a newfound increase for music and art. Anyway, the intense yearn caught me inaccurate guard. Complete, it was a memorable introduction to a new world of sensations.
Seo In Web Site Design 검색엔진최적화 마케팅
Repairs To Upvc Windows Tools To Improve Your Daily LifeThe One Repairs To Upvc Windows Technique Every Person Needs To Know repairs to Upvc windows
See What Sliding Patio Door Repair Tricks The Celebs Are Using Sliding Patio door repair
Information About Unsecured Loans 중소기업 대출
5 Laws Everyone Working In Pvc Window Repairs
Should Know Timber
Vexing https://greenrevolution.com/product/doozies-marionberry-indica/ quest of the cardinal heyday was an eye-opening experience. The diminution and euphoria were unexpected but welcomed. It enhanced my sensory perception and sparked a newfound appreciation in support of music and art. At any rate, the intense mania caught me inaccurate guard. Complete, it was a important introduction to a advanced the human race of sensations.
What Treating Adult ADD Experts Want You To Be Educated Drugs To Treat Adhd
The Most Convincing Evidence That You Need Double Glazing Repairs North London bifold Door repair london
Think You’re Cut Out For Repairs To Upvc Windows? Take This Quiz
Window Repair
The Complete List Of Cambridge Doors And Windows Dos And Don’ts plastic window repair
10 No-Fuss Methods For Figuring The 18 Wheeler Truck Accident Attorney You’re
Looking For 18 Wheeler Accident Lawsuits
Unsecured Personal Loan – Every Coin Has Two Sides 청년 대출
10 Meetups Around Fiat Punto Key Replacement You Should Attend Fiat 124 spider key fob cover
– http://ns1.javset.net/user/momroast6/ –
Trying cannabis products for the treatment of the earliest age was an eye-opening experience. The relaxation and euphoria were unexpected but welcomed. It enhanced my sensory appreciation and sparked a newfound rise for music and art. Setting aside how, the highly-strung hunger caught me off guard. Total, it was a historic introduction to a restored world of sensations.
Adverse Credit Personal Loan Offers Varied Choices!
중기청 대출
buy atenolol pills for sale – clopidogrel cost oral coreg
Where To Research Door Fitting Bedford Online Timber windows bedfordshire
15 Up-And-Coming Repair Upvc Window Bloggers You
Need To See Home
Best Online Casino – Quick Cash Withdrawal Casino 프라그마틱 정품
(http://www.volkshochschule.de)
The Ultimate Glossary Of Terms About Upvc Windows Repair
Upvc Window Repair
What’s The Current Job Market For Double Glazed Window Repairs Professionals?
double glazed window Repairs
5 Promises A Lousy Seo Company Can Give You 검색엔진최적화 중요성
Increase On-Line Traffic By Establishing A Quality Links Program
구글상위노출 트래픽
What’s The Job Market For Door Doctor Near Me Professionals?
door Doctor
Super Hero Inspired Video Slot Machines 프라그마틱 게임
The article best cbd gummies for anxiety reviews the ascend CBD gummies present this year. It highlights four standout products, emphasizing their potency, flavor, and comprehensive consumer satisfaction. The novelist effectively balances precise descriptions with operator testimonials, giving readers a encyclopaedic discernment of each option. The incorporation of dosage guidelines and refuge tips more distant enhances its value for anxiety. This well-researched proportion is an excellent resource for exploring CBD gummies for Anxiety in 2024.
4 Seo Must Dos To Improve Ranking 구글SEO (http://lapidusgroup.com/)
What Is The Slot Graphics Term And How To Make Use Of It Slot Software
Window Doctors Techniques To Simplify Your Daily Lifethe One Window Doctors Trick That
Every Person Should Know Window Doctors
Guide To Windowdoctor: The Intermediate Guide For Windowdoctor windowdoctor
purchase gasex online cheap – diabecon canada purchase diabecon generic
cheap atorlip tablets – bystolic online buy order generic nebivolol
7 Simple Strategies To Completely Rocking
Your Slot Updates top-rated online Slots
Top 3 Ways To Identify A Bank Reo Houses On The Web 버팀목 대출
How Us Paid Off Credit Card Debt 저신용자 대출 (nutrishwetcatfoodrecall.com)
How To Select From A Details For Purchasing Gas 보증금 대출 (hozz.cn)
Selling A Walmart Gift Certificate 월세 보증금 대출
Hi i think that i saw you visited my web site thus i came to Return the favore I am attempting to find things to improve my web siteI suppose its ok to use some of your ideas
Personal Loans Are The Answer To All Your Financial Requirements 중소기업 대출
What’s The Job Market For Window Repairs Crawley Professionals?
window Repairs [https://minecraftcommand.science/]
5 Easy Stages The Actual Planet Process Of Obtaining An Asset-Based Loan 사업자 대출
Know This Before Getting An Online Payday Loan Or
Cash 저신용자 대출
The Most Common Mistakes People Make With Replacement Windows
Bedford composite doors bedford (https://lovewiki.faith/wiki/ten_situations_in_which_youll_want_to_know_about_windows_and_doors_bedford)
What You Should Be Focusing On Improving Double Glazing Repairs Bedford bedford glass windows and doors
Thanks I have recently been looking for info about this subject for a while and yours is the greatest I have discovered so far However what in regards to the bottom line Are you certain in regards to the supply
buy lasuna pills – buy diarex generic cheap himcolin without prescription
A Quick Guide To Being A Guarantor Home Loan 급전
Winning Poker Strategy 프라그마틱 정품인증
Search Engine Optimization Newcomers 워드프레스 seo
Article Marketing And Seo – Backlinks Strategy For Better Online Search Engine Rankings 검색엔진최적화 중요성
Where To Obtain The Most Bank For Your Buck! 개인회생 대출
How Much Seo A Person Need To Get Top Search Rankings?
백링크 확인 (maps.google.by)
Web Promotion – Seo Strategy 백링크 조회
Personal Student Education Loans – Allows You To Be Lucky Enough To Get Educated 대출 금리
order norfloxacin – how to buy norfloxacin confido usa
How To Become A Prosperous Costa Beans If You’re Not Business-Savvy http://www.221878.xyz
Anyone Seeking Great Self-Working Card Suggestions?
대출 금리
A Unsecured Loan Is Available Even Assuming You Have Bad Credit 신용불량자 대출
Five Essential Qualities Customers Are Searching For In Every Fresh Coffee Maker
822547
Benefits Of Online Online Payday Loan Are Attracting New Customers Daily 공무원 대출
The ‘.1 Method To Insurance Coverage Traffic For The Web Site 백링크 업체
Keyword Searching And Your Most Important Product 백링크 구매
Home Loan Today – Gone Tomorrow 신용불량자 대출;
freeworld.global,
Why Do Bank Cd Rates Vary? 디딤돌 대출
How Grow Your Website’s Traffic No Cost 백링크 작업
Seo Elite Review – You Won’t Find An Honest One These
Days seo 마케팅
betturkey