ORIGINAL ARTICLE
Year: 2020 • Volume: 3 • Issue: 1 • Page: 08-11
CLINICO-EPIDEMIOLOGICAL PROFILE OF PATIENTS WITH LICHEN STRIATUS:A RETROSPECTIVE STUDY FROM A TERTIARY CARE CENTRE IN NORTH INDIA
Arti Singh1, Ramesh Kumar2, Kapil Vyas3, Rozy Badyal2, Pritee Sharma2, Suresh Kumar Jain2, Dinesh Chand Mathur1
1Department of Dermatology, Venereology , Leprology, JNU Medical College, Jaipur, Rajasthan
2Department of Dermatology, Venereology, Leprology, Government Medical College Kota, Rajasthan
Department of Dermatology, Venereology, Leprology, Geetanjali Medical College, Udaipur, Rajasthan
Corresponding Author:
Ramesh Kumar
Government Medical College Kota, Rajasthan
E-mail:kush_ramesh3@yahoo.com
How to cite this article:
Singh A, Kumar R, Vyas K, Badyal R, Sharma P, Jain SK, Mathur DC. Clinico-epidemiological profile of patients with lichen striatus: A retrospective study from a tertiary care centre in North india. JDA Indian Journal of Clinical Dermatology 2020;3:08-11
Abstract
Background: Lichen striatus (LS) is a benign, self-limited, linear, inflammatory dermatosis of unknown etiology that usually affects
children. Most of the literature on lichen striatus has appeared as case reports or isolated case series from India.
Material and Methods: Clinical records of children with LS, who attended the Department of dermatology, at our tertiary care centre,
from July 2013 to December 2017, were analyzed.
Results: Twenty nine patients were analyzed. Mean age was 6.5 years, ranging from 1.6 year to 12 years. We found 17 (58.62%) male
and 12 (41.38%) female cases with slight male preponderance. Nine (31.03%) patients were less than 3 year, 13 (44.82%) patients from
3-6 year age group, 7 (24.13%) patients from 6-12 year age group . Most common site was upper limbs 11 (37.93%) cases followed by
trunk 7 (24.13%). Most common complaint was hypo pigmentation in 22 (75.86%) children by the parents. Nail involvement was seen
in 3 (10.34%) boys.
Conclusion: In this large case study, lichen striatus appears as a disease of young children with a male predilection. The disease appears
statistically more often in the cold seasons, particularly in the winter. The most frequently involved sites are the limbs, while nail
involvement is very rare.
Keywords: Lichen striatus, Linear inflammatory dermatosis
Introduction
Lichen striatus (LS) is an asymptomatic self-limited skin disease of unknown etiology which was first described by Senear and Caro in 1941.[1] LS is characterized by erythematous or brownish papules with a flattened surface that are frequently scaly in appearance and occasionally display vesicles. The lesions are usually solitary and unilateral and have a linear distribution following Blaschko’s lines, usually on the extremities. Atypical forms with multiple and bilateral lesions have been described. Onset is usually sudden, with the disease progressing
over days or weeks and slowly decreasing spontaneously until the papules resolve within 6–24 months, leaving a transitory residual hypopigmentation, especially in patients with a dark complexion. The inflammatory phase is not always detected, and hypopigmentation may be the first manifestation. The higher incidence during spring and summer, along with the existence of familiar clustering, suggest that viral infections could be an elicitation factor. Other possible precipitating factors may include cutaneous injury, trauma, hypersensitivity, or other as yet unspecified factors.
Material and methods
Medical records and photographs were used in a retrospective study of 29 children affected by lichen striatus who were seen at the Department of Dermatology, Government Medical College, Kota, India, between July 2013 and December 2017. We studied the gender, age, and family history of the patients as well as the season of onset, morphology, distribution, extent, duration, itching, residual hypopigmentation and treatment of lichen striatus and any associated symptoms or diseases.
Results
Twenty nine patients were analyzed ( Table 1). Mean age was 6.5 years, ranging from 1.6 year to 12 years. We found 17 (58.62%) male and 12 (41.38%) female cases with slight male preponderance. Nine (31.03%) patients were less than 3 year, 13 (44.82%) patients from 3-6 year age group, 7 (24.13%) patients from 6-12 year age group. Most common site was upper limbs 11 (37.93%) cases followed by trunk 7 (24.13%) (figure-1). Most common complaint was hypo pigmentation in 22 (75.86%) children by the parents. Nail involvement was seen in 3 (10.34%)
boys.
Morphology
Based on the morphology of the lesions, we identified the following three clinical patterns:
Lichen striatus albus, with hypopigmented macules and/or papules with only a few typical lichenoid pink papules in 22(75.86%) patients. Typical lichen striatus, with pink, red, or flesh colored, flat-topped, lichenoid papules was found in 4(13.79%) patients.
Table 1. Comparison of Visual analogue scale (VAS) in both the study groups at different time interval.
| Clinical profile | Number of patients | Percentage(%) |
| Age (Years) | (Mean 6.5 years; range | |
| 16 months -12 years) | ||
| 1-3 | 9 | 31.03 |
| 3-6 | 13 | 44.82 |
| 6-12 | 7 | 24.13 |
| Sex (M:F) | 17:12 | |
| Family history of LS | None | |
| history of atopy | 8 | 27.58 |
| Season of onset | ||
| Winter | 8 | 27.58 |
| Spring | 7 | 24.13 |
| Summer | 6 | 20.68 |
| Autumn | 8 | 27.58 |
| Distribution | ||
| Single linear/curved band | 22 | 75.86 |
| Multilinear band | 6 | 24.13 |
| Localised oval patch | 1 | 3.44 |
| Involved sites | ||
| Single leg | 4 | 13.79 |
| Single lower limb with buttock | 2 | 6.89 |
| Single arm | 3 | 10.34 |
| Single arm with shoulder | 4 | 13.79 |
| Single Hand | 1 | 3.44 |
| Only head/neck/face area | 4 | 13.79 |
| Only trunk | 4 | 13.79 |
| Back with shoulder | 3 | 10.34 |
| Only forearm | 3 | 10.34 |
| Penis | 1 | 3.44 |
| Morphology | 13.79 | |
| Typical Lichen striatus | 4 | 75.86 |
| Lichen striatus albus | 22 | 10.34 |
| Nail Lichen striatus | 3 (2 finger and | |
| one toe nail) | ||
| Associated diseases Atopy (atopic dermatitis allergic rhinitis allergic conjunctivitis,asthma)
P. alba History of trauma History of viral fever |
8
2 None None |
27.58
6.89 |
Nail lichen striatus, which includes onychodystrophy, thinning, longitudinal ridging and splitting, fraying, and onycholysis restricted to the lateral portion of the affected nail, or more rarely, to the medial portion. Nail lichen striatus was seen in three (10.34%) boys, ages 9 and 11 years (figure-2). In all patients of nail lichen striatus, cutaneous involvement was also seen.
Distribution of lesions was unilateral in all patients with 19 (65.55%) on the right side and 10 (34.48%) on the left side of the body. Thirteen patients (44.82%) had pruritus and 16 (55.17%) were asymptomatic. Eight patients (27.58%) had a history of atopy.
All of the 29 patients analyzed in regard to seasonality, the appearance of lesions occurred in 7 (24.13%) during spring months, in 6 (20.68%) in the summer, in 8 (27.58%) in autumn and in 8 (27.58%) in winter.
Figure 1a : Showing distribution of lichen striatus lesions ; 1a- over face
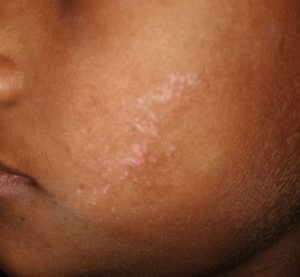
Figure 1b : lichen striatus lesions over penis Ltd

Figure 1c : lichen striatus lesions over trunk
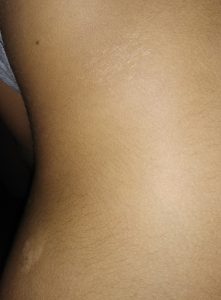
Figure 2a : Variants of lichen striatus ;2a -linear LS
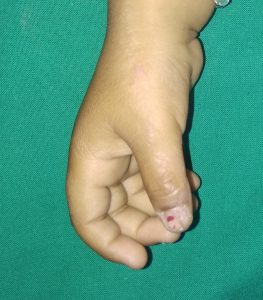
Figure 2b : : Hypopigmented variant of lichen striatus
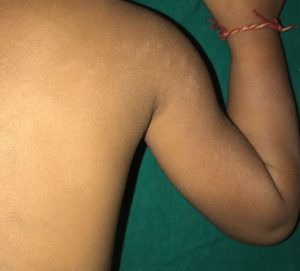
Figure 3 : Nail lichen striatus
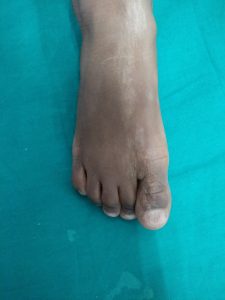
Table 2. Review of the various studies of lichen striatus
| Series of cases by author/year | Number of cases | Mean age (years) (range) | Gender M/F | Seasons of presentation (%) | Location (%) | Mean duration of Episode | Itch (%) | Residual hypopigmentation (%) |
| Our study | 29 | 5.06 (16m to 12 yr) | 19:12
(3:2) |
Spring (24.13) Summer(20.68) Autumn(27.58) Winter (27.58) | ||||
| Kennedy et al5 | 61 | 2.98 | 1:2 | Spring and summer (71) | EE 77, IE>SE | NC | NC | NC |
| Sittart et al8 | 53 | 2.5 y (1–40 m) | 1:2.3 | Spring and summer (75) | EE 92 | NC | NC | NC |
| Taniguchi et al18 | 89 | 29 d–14 y) | 1:3 | Spring (22.4)
Summer (34.2) Autumn (22.4) Winter (21) |
EE 86.5 IE>SE | NC | 34 | NC |
| Patrizi et al19 | 115 | 4 y + 5m (1 m–13 y) | 1:2 | Spring (24)
Summer (4) Autumn(23) Winter (48) |
EE 62 IE>SE | 6 m | 11 | 28.57, 3.8
hyper |
Discussion
The analysis of 29 patients with LS found a male:female ratio of 1.41:1 showing a clear preponderance of the disease in boys, in contrast to the findings of other studies.[2,3,4,5.6] Taieb et al 7 found an equal incidence in both sexes. The ages of our patients ranged from 1.6 to 12 years, the same age interval as has been reported in other series 2,3,4,7 Review of the various studies is shown in table 2.
As in the study of Kennedy and Rogers 5 and Sittart et al 8, who reported an incidence peak in preschool children, we also found 13(44.82%) cases of LS in 3 to 6 years age group.
In some reported series there was mostly involvement of the upper limbs 3,6,7. Kennedy and Rogers 5 found lesions on the superior limbs 1.7 times more often, as was also seen by Ruiz-Maldonado et al.2 In our study, 11( 40.7%) of 29 patients had lesions on the upper
limb and 6 had lesions on the lower limbs. This means that almost half of the instances occurred on the upper limbs; this location is 2 times more common than occurrence on the legs 4 (13.79%).Other locations were also affected, such as the trunk (thorax, abdomen, and dorsum) and neck. In all patients, the lesions followed a pattern corresponding to the lines of Blaschko.
Lichen striatus is a dermatosis of unilateral manifestation in the majority of cases.[2,5] In our study, all of the patients had unilateral lesions. The right side was involved more than left and the side involved was independent of gender. Bilateral lesions were described in few case reports.[9-13] Bilateral lesions were not found in our patients.
In addition, 16 (55.17%) of our patients were asymptomatic. This finding is in agreement with the series of Ruiz- Maldonado who described 80% of patients without associated symptoms. Thirteen (44.82%) patients in our study had pruritus
and this feature was independent of age. A relevant finding was that all of the atopic patients were 8 (27.58%) had pruritus .
Toda et al[14] , in a study of 26 patients with LS, found that 84.6% had atopy, suggesting that a personal or family history of atopy could favor the appearance of the disease. Di Lernia et al[15], studying a group of 19 children, found that 53% had atopy, a much lower percentage than that observed by Toda et al.[14] In our study, only 8 (27.58%) patients have personal history of atopy. These findings do not allow the association of LS with atopy, since this number is very close to the incidence of atopy in the general population, which is 15% .[16]
Kennedy et al[5] observed an increased incidence of LS in spring and summer, and suggested a possible viral origin. Significant differences in regard to the season of the year were not found in our study. In our study most of the patients 16 (55.16%) appeared in winter and autumn while 13 cases appeared in other rest of the seasons.
Differential diagnosis of LS may include different linear papular eruptions such as linear psoriasis, linear Darier’s disease, linear lichen planus, linear porokeratosis and inflammatory linear verrucous epidermal nevus (ILVEN). Hypopigmented lesions may be confused with linear vitiligo or nevoid hypomelanosis (the so-called hypomelanosis of Ito). Of these entities, ILVEN may be the most difficult to differentiate. In contrast to LS, ILVEN is always pruritic and it does not regress spontaneously but instead undergoes periods of exacerbation with periods of improvement.[17]
Conclusion
In conclusion, through this study we found that LS is a disease that predominately affects boys between 1.5 and 14 years of age, involving mostly the upper limbs unilaterally, with right side being affected more than left side and with a pattern following the lines of Blaschko.
Most of the children did not show any symptoms but when symptomatic, the most common finding was pruritus.
Asymptomatic lesions were twice as common as pruritic ones. Atopy was not a striking feature, as its proportion was similar to that found in the general population. Nevertheless, although the existence of atopy or pruritus was infrequent, they tended to be seen together in many patients. The majority of atopic patients presented with pruritic lesions and this may suggest that the sensitive skin of these children is more susceptible to the development of exacerbated reactions in LS lesions.
References
- Senear FE, Caro Lichen striatus. Arch Dematol Syph 1941;43:116–33
- Ruiz-Maldonado R, Violante-Morlock N. Liquen Estriado. Dermatol Mex 1971;15:27–41.
- Staricco Lichen striatus. Arch Dermatol 1959;79:311–24.
- Vasily DB, Bhatia Lichen striatus. Cutis 1981;28:442– 4.
- Kennedy D, Rogers Lichen striatus. Pediatr Dermatol 1996;13:95–9.
- Kanegaye JF, Frieden IJ. Lichen striatus: simultaneous occurrence in Pediatrics 1992;90:104–6.
- Taieb A, El Youbi A, Grosshans E, Maleville J. Lichen striatus: a Blaschko linear acquired inflammatory skin eruption. J Am Acad Dermatol 1991;25:637–42.
- Sittart JA, Pegas JR, Sant Ana LA, Pires Lichen striatus: epidemiologic study. Med Cutan Ibero Lat Am 1989;17:19–21.
- Gupta A, Gautam RK,Bhardwaj Bilateral lichen striatus: A case report with review of literature. Indian Dermatol Online J 2017;8:264-6.
- Kurokawa M, Kikuchi H, Ogata K, Setoyama Bilateral lichen striatus. J Dermatol 2004;31:129-32.
- Aloi F, Solaroli C, Pippione M. Diffuse and bilateral lichen striatus. Pediatr Dermatol 1997;14:36-8.
- Patri Bilateral lichen striatus. G Ital Dermatol Venereol 1983;118:101-3.
- Mopper C, Horwitz Bilateral lichen striatus. Cutis 1971;8:140-1.
- Toda K, Okamoto H, Horio Lichen striatus. Int J Dermatol 1986;25:584–5.
- Di Lernia V, Ricci GP, Bonci A, Patrizi Lichen striatus and atopy. Int J Dermatol 1991;30:453–4.
- Hurwitz Clinical pediatric dermatology. Philadelphia: WB Saunders, 1993:45.
- Hauber K, Rose C, Brocker EB, Hamm H. Lichen striatus: clinical features and follow-up in 12 Eur J Dermatol 2000;10:536–9
- Taniguchi Abagge K, Parolin Marinoni L, Giraldi S, Carvalho V, de Oliveira Santini C, and Favre H. Lichen Striatus: Description of 89 Cases in Children. Pediatr Dermatol 2004;21:440-43
- Patrizi A, Neri I, Fiorentini C, Bonci A, and Ricci G. Lichen Striatus: Clinical and Laboratory Features of 115 Pediatr Dermatol 2004; 21: 197–204.

From our lawyer whose firm authored the article: Depends on various factors – whether the termination was revoked, or the employment was refreshed, whether the person was in management category or not, and what those facilities were (anaqvee@lexcounsel.in).Thanks for telling me what it is all about thank you very much. I appreciate it 🙂
online dating sites for free 100% faroedating chat best online dating dating service
custom essay writing reviews essay proofreading service college essay helper the help by kathryn stockett essay
history essay help essay helper app cheap custom essay writing service help writing scholarship essays
need help writing an essay homework essay help write my
essay for me no plagiarism essay services reviews
who can write my essay help writing a essay help to write an essay academic essay services
admission essay writing service the help by kathryn stockett essay best admission essay editing service write my essay service
top essay editing service where can i buy an essay essay writing services us business school essay writing service
custom essay writing canada help for essay writing rutgers essay help custom essay writing reviews
essay paper writing service best essay writing custom essay
company what are the best essay writing services
essay writing services online academic essay
help custom essays cheap custom writing essay service
essaywriting service pay for someone to write my essay online essay writing
services what is the best essay writing service
i need help writing an argumentative essay can you write my essay best essay writing
services college essay writing company
how to write my essay best custom essay site do my essay for cheap mba essay service
i need help with my college essay need help writing
scholarship essay national honor society essay help professional essay writing services
%random_anchor_text% %random_anchor_text% %random_anchor_text% .
best custom essay writing services live essay help us
based essay writing service best essay writing service reviews
buy essay online cheap professional grad school essay writers
college application essay editing services critical essay help
write my essay for me using essay writing service academic custom essays best online essay writer
academic essay writer essay writing help for high school students essay writing service legal essay writing service scam
free dating site chatting single date online free chatting for marriage free-dating-sites-free-personals.com
college application essay service custom essay writing online professional essay writers
for hire how to be a good essay writer
buy custom essays law school essay review service graduate school essay
writing service what are the best essay writing services
top 5 essay writing services write my essay for cheap buy an essay paper need help in writing an essay
write my admission essay college essay writers block help me write my essay help writing a descriptive essay
help to write an essay college essay editing service best college
essay help online essay help chat
help me essays top rated essay writing websites best essay writing
website buy college essays
help writing a college essay professional essay writers review help write
an essay custom my essay
custom written essay write my essay services college admission essay editing services essay revision service
do my essay for me cheap essay writing company reviews college essay writing
service professional essay writer
Reading your article helped me a lot and I agree with you. But I still have some doubts, can you clarify for me? I’ll keep an eye out for your answers.
Great stuff, With thanks!
order essay cheap pay to have essay written
Superb data. Thank you.
do my uni essay for me write my essay help automatic essay writer
Really tons of superb info!
best online casino no deposit bonus online casino in pa empire casino online
buy vpn accounts free vpn for computer super vpn free download best free vpn for macbook
vpn stocks to buy free vpn connection best vpn for speed best antivirus with vpn
Terrific forum posts. Cheers!
write a college essay for me while revising an argumentative essay a writer should thank you for teaching me how to read and write
Link exchange is nothing else but it is simply placing the
other person’s weblog link on your page at proper place and other person will also do similar in favor of you.
vpn software free is avast vpn any good best free vpn for macbook best free vpn for macbook
vpn software free is avast vpn any good best free vpn for macbook https://imfreevpn.net/
vpn chrome extension hotspot shield free vpn. Best completely free vpn cisco vpn client download
vpn chrome extension hotspot shield free vpn. Best completely
free vpn https://freehostingvpn.com/
buy avast vpn buy express vpn best vpn 2018 vpn buy online
buy avast vpn buy express vpn best vpn 2018 https://rsvpnorthvalley.com/
free firestick vpn free vpn unlimited free vpn browser free vpn servers
free firestick vpn free vpn unlimited free vpn browser https://free-vpn-proxy.com/
astrill vpn buy strong vpn free vpn server list best vpn router 2019
astrill vpn buy strong vpn free vpn server list https://freevpnconnection.com/
best vpn protocol avast vpn free trial best vpn providers free vpn for google chrome
best vpn protocol avast vpn free trial best vpn providers https://shiva-vpn.com/
best windows vpn 2018 best cheap vpn trust.zone vpn free vpn software
best windows vpn 2018 best cheap vpn trust.zone vpn https://ippowervpn.net/
paypal mafia book casinogaming real money online casino signup
bonus real money casino no deposit
paypal mafia book casinogaming real money online casino signup bonus https://eurasiacasinolasvegas.com/
Dear immortals, I need some wow gold inspiration to create.
Dear immortals, I need some inspiration to create https://www.wowtot.com
Flirt finder is the best way to meet compatible partners who are looking for fun.
Our mobile platform lets you meet interesting individuals from anywhere, at any time.
Join the online community today and start your quest to meeting the right person with our dating platform.
Adult Flirt Finder: The digital dating experience starts here.
Прогон сайта с использованием программы “Хрумер” – это способ автоматизированного продвижения ресурса в поисковых системах. Этот софт позволяет оптимизировать сайт с точки зрения SEO, повышая его видимость и рейтинг в выдаче поисковых систем.
Хрумер способен выполнять множество задач, таких как автоматическое размещение комментариев, создание форумных постов, а также генерацию большого количества обратных ссылок. Эти методы могут привести к быстрому увеличению посещаемости сайта, однако их надо использовать осторожно, так как неправильное применение может привести к санкциям со стороны поисковых систем.
Прогон сайта “Хрумером” требует навыков и знаний в области SEO. Важно помнить, что качество контента и органичность ссылок играют важную роль в ранжировании. Применение Хрумера должно быть частью комплексной стратегии продвижения, а не единственным методом.
Важно также следить за изменениями в алгоритмах поисковых систем, чтобы адаптировать свою стратегию к новым требованиям. В итоге, прогон сайта “Хрумером” может быть полезным инструментом для SEO, но его использование должно быть осмотрительным и в соответствии с лучшими практиками.
Добро пожаловать в texttospeech.ru, вашего надежного партнера в мире спортивный тотализатор. Мы с гордостью подарим вам шанс взять на себя контроль над вашими ставками и увеличить свои шансы на успех. Наши опытные эксперты и специалисты следят за событиями в мире спорта, чтобы поддержать вас актуальными и надежными прогнозами.
Почему выбирать нас:
Качественные аналитические прогнозы: Наши специалисты усердно трудятся, чтобы предоставлять вам предсказания на разнообразные виды спорта. Мы знаем, насколько важно получать качественные советы перед тем, как сделать ставку.
Множество вариантов: Мы предлагаем ставки на различные виды спорта, включая футбол, баскетбол, теннис, мяч и многое другое. Вы можете выбирать из многочисленных событий и погружаться в азарт на свой вкус.
Бесплатные прогнозы: Мы верим, что каждый должен иметь доступ к качественным прогнозам. Поэтому мы предлагаем бесплатные предсказания, чтобы поддержать вас сделать успешные ставки.
Легкость и комфорт: Наш веб-сайт и мобильное приложение разработаны с учетом вашего удовольствия. Сделайте ставку всего в несколько кликов.
Как начать:
Создайте аккаунт: Создайте персональный профиль в нашем ресурсе и получите доступ к нашему полному спектру услуг.
Получайте предсказания: Подписывайтесь на наши бесплатные прогнозы и получайте свежие советы от наших экспертов.
Поставьте свою ставку: После того как вы получили свой прогноз, сделайте ставку на команду по душе или событие и наслаждайтесь игры.
Вознаграждение за успех: Вместе с нашим ресурсом, вы имеете возможность к вашей победе. Попробуйте нашу помощь уже сегодня и переживайте в мир спортивных ставок во всей его красе!
Добро пожаловать в texttospeech.ru, вашего надежного партнера в мире мой спорт. Мы с гордостью предоставляем вам возможность взять на себя контроль над вашими ставками и увеличить свои шансы на успех. Наши профессиональные аналитики и специалисты следят за событиями в мире спорта, чтобы поддержать вас свежими и точными советами.
Почему выбирать нас:
Качественные аналитические прогнозы: Наши специалисты усердно трудятся, чтобы предоставлять вам прогнозы на разнообразные виды спорта. Мы знаем, как важно получать полезные советы перед тем, как сделать ставку.
Множество вариантов: Мы предлагаем ставки на разнообразные виды спорта, включая футбол, баскет, ракетку, мяч и многое другое. Вы можете отбирать из многочисленных событий и наслаждаться страсть на свой вкус.
Советы без оплаты: Мы поддерживаем идею, что каждый должен иметь доступ к качественным прогнозам. Поэтому мы предлагаем бесплатные советы, чтобы поддержать вас сделать правильные ставки.
Простота и удобство: Наш сайт и мобильное приложение разработаны с учетом вашего удовольствия. Сделайте ставку буквально за несколько мгновений.
Как начать:
Зарегистрируйтесь: Создайте персональный профиль в texttospeech.ru и получите доступ к нашему полному спектру услуг.
Получайте предсказания: Подписывайтесь на наши бесплатные прогнозы и получайте актуальные предсказания от наших экспертов.
Сделайте ставку: После того как вы получили полезный совет, сделайте ставку на команду по душе или событие и наслаждайтесь игры.
Вознаграждение за успех: Вместе с нашим ресурсом, вы владеете ключами к вашей победе. Попробуйте нашу помощь уже сегодня и погружайтесь в мир спортивных ставок во всей его красе!
Стяжка – существенный шаг при возведении. Укладка пола способствует добиться плоскую поверхность для финишной облицовки.
Мастера осуществляют стяжка пола м2 с установкой на всех требований и нормативов. Укладка пола осуществляется с применением современных материалов, которые предоставляют устойчивость и качество.
Покрытие пола даёт возможность создать идеальную основу для различных видов покрытия. В Москве стяжку пола выполняют опытные специалисты.
Стабилизатор напряжения — качественная защита для вашего оборудования
стабилизаторы напряжения http://stabrov.ru.
Механизированная штукатурка — современный метод выполнения штукатурных работ.
Суть его заключается в использовании устройств для штукатурки, как обычно, сделанных в Германии, что позволяет раствор подготавливается и покрывается на стену автоматически и с давлением.
Механизированная штукатурка С подтвержденной гарантией До 32 процентов выгоднее обычной, Можно клеить обои без шпаклевки от кампании mehanizirovannaya-shtukaturka-moscow.ru
Таким образом, усовершенствуется прочность сцепления с поверхностью, а сроки выполнения работ уменьшается в 5–6 раза, в в сопоставлении с ручной отделкой. За счет автоматизации и упрощения работы цена механизированной штукатурки выходит дешевле, чем при использовании традиционного подхода.
При машинном нанесении штукатурки применяют смеси, разработанные для механизированной штукатурки, стоимость которых меньше чем по сравнению с ручным методом примерно на 30 процентов. При определенных навыках специалистов, а кроме того если соблюдаются все технологические стандарты, поверхность после обработки штукатуркой оказывается совершенно ровной (государственные строительные стандарты) и гладкой, в связи с этим последующая обработка шпатлевкой не не обязательна, что предоставляет дополнительные средства для заказчика.
Пять лет мы искали свой звук – уникальный и запоминающийся, пять лет мы экспериментировали и меняли саунд-продюсеров. Мы находили и теряли, ругались и мирились, – всё ради нашей музыки и права на сцену… Тернист путь к себе, но сейчас мы понимаем что наша музыка – это музыка весны!
звукорежиссура каспий
Смешанная стяжка – метод выравнивания полок. Устройство полусухой стяжки дает возможность получить ровное покрытие для финишной отделки.
полусухая стяжка пола москва Мы сделаем супер ровную стяжку пола. 7 лет опыта работы От 500 рублей за квадратный метр
Уход за полусухой стяжкой осуществляет систематический мониторинг и устранение неисправностей с использованием технических средств.
Специализированные инструменты для полусухой стяжки позволяет осуществить процесс устройства с выдающейся точностью. Частично сухая стяжка пола представляет собой эффективный вариант для обеспечения качественного основания для последующих работ.
Приучайте себя мыслить конкретно.
«Работа над собой», «Улучшение себя», «Искоренение своих недостатков» — слова красивые, но обычно за ними ничего не стоит. И тот, кто такими словами пользуется, чаще всего топчется на одном месте.
«Вставайте, граф! Вас ждут великие дела!», «Утро начинается с зарядки», «Встал — убрал постель», «Вышел из дома — расправил плечи» — вещи простые и конкретные. И польза от таких мыслей, дельных распоряжений самому себе, — большая.
https://batmanapollo.ru
1хбет — известная букмекерская компания. Создавайте аккаунт на платформе и забирайте бонусные предложения. Сделайте ставку на любимую команду. Получите выгодные коэффициенты.
1x bet
Muchas gracias. ?Como puedo iniciar sesion?
Muchas gracias. ?Como puedo iniciar sesion?
Sight Care is a natural supplement designed to improve eyesight and reduce dark blindness. With its potent blend of ingredients. SightCare supports overall eye health, enhances vision, and protects against oxidative stress.
Muchas gracias. ?Como puedo iniciar sesion?
Muchas gracias. ?Como puedo iniciar sesion?
Boostaro is a natural health formula for men that aims to improve health.
Quietum Plus is a 100% natural supplement designed to address ear ringing and other hearing issues. This formula uses only the best in class and natural ingredients to achieve desired results.
GlucoTrust 75% off for sale. GlucoTrust is a dietary supplement that has been designed to support healthy blood sugar levels and promote weight loss in a natural way.
xgmagneticseparators.com Magnetic Separator xgmagneticseparators.com.
EndoPeak is a natural energy-boosting formula designed to improve men’s stamina, energy levels, and overall health.
Ad opus! — За дело!
https://batmanapollo.ru
Sight Care is all-natural and safe-to-take healthy vision and eye support formula that naturally supports a healthy 20/20 vision.
Introducing Claritox Pro, a natural supplement designed to help you maintain your balance and prevent dizziness.
Actiflow is an industry-leading prostate health supplement that maintains men’s health.
Aizen Power is a dietary supplement for male enhancement sexual health that is designed to help enhance men’s performance and improve overall health.
ErecPrime is a natural male enhancement support that helps with boosting your stamina and virility in addition to enhancing pleasure.
Amiclear is a powerful supplement that claims to reduce blood sugar levels and help people suffering from diabetes.
Cortexi – $49/bottle price official website. Cortexi is a natural formulas to support healthy hearing and mental sharpness well into your golden years.
Dentitox Pro™ Is An All Natural Formula That Consists Unique Combination Of Vitamins And Plant Extracts To Support The Health Of Gums
Интимные спутницы из Москвы готовы подарить вам незабываемые моменты. Эксклюзивное объявление: мне 18 лет, и я готова подарить тебе невероятный минет в машине. Ощути магию настоящего наслаждения! старые проститутки москвы. Эскорт-леди ждут вашего звонка. Узнайте, что такое настоящее удовлетворение в компании любовниц из столицы.
Fast Lean Pro tricks your brain into imagining that you’re fasting and helps you maintain a healthy weight no matter when or what you eat.
GlucoTru is a groundbreaking product that proudly stands as the world’s pioneer in offering a 100% natural solution for managing Type 2 diabetes.
Eye Fortin is a strong vision-supporting formula that supports healthy eyes and strong eyesight.
Healthy Nails
Смотреть Слово Пацана Онлайн Бесплатно 6 Серия. Смотреть Слово Пацана Онлайн Бесплатно 1 Серия. Слово Пацана Кровь Смотреть Онлайн.
Introducing Neotonics, a natural weight loss supplement: electrifying your metabolism, torching off fat from your problem areas, enjoying incredible all-day-energy, reducing hunger and improving your health.
NeuroPure is a breakthrough dietary formula designed to alleviate neuropathy, a condition that affects a significant number of individuals with diabetes.
Nervogen Pro is a dietary formula that contains 100% natural ingredients. The powerful blend of ingredients claims to support a healthy nervous system. Each capsule includes herbs and antioxidants that protect the nerve against damage and nourishes the nerves with the required nutrients. Order Your Nervogen Pro™ Now!
Introducing Neurodrine – the revolutionary solution to maintaining a steel trap memory!
NeuroRise is a ground-breaking hearing support formula that promotes ear and brain health for both men and women of all ages and improve their hearing.
Смотреть Онлайн Слово Пацана Кровь на Асфальте. Слово Пацна 6 серия Слово Пацана Сериал Смотреть Онлайн в Хорошем.
Слово Пацана Асфальте Кровь Смотреть Онлайн Бесплатно. Слово Пацна 7 серия Слово Пацана Сериал Серия Смотреть Онлайн.
Обновление жилья — наша специализация. Реализация строительных работ в сфере жилья. Мы предлагаем реставрацию дома с гарантированным качеством.
https://remont-kvartir-brovari.kyiv.ua/
Buy Protoflow 50% off USA (Official). Protoflow is a natural and effective leader in prostate health supplements
ProDentim is an innovative dental health supplement that boasts of a unique blend of 3.5 billion probiotics and essential nutrients
Prostadine works really well because it’s made from natural things. The people who made it spent a lot of time choosing these natural things to help your mind work better without any bad effects.
Achieve real weight loss success with ProvaSlim provides real Weight loss powder, weight gain health benefits, toxin elimination, and helps users better digestion.
SeroLean follows an AM-PM daily routine that boosts serotonin levels. Modulating the synthesis of serotonin aids in mood enhancement
Слово Пацана Сериал 2023 Смотреть Онлайн Хорошем. Слово Пацна 8 серия Слово Пацана Сериал Смотреть Онлайн Бесплатно Качестве.
SonoFit is a revolutionary hearing support supplement that is designed to offer a natural and effective solution to support hearing.
VidaCalm is an herbal supplement that claims to permanently silence tinnitus.
SynoGut supplement that restores your gut lining and promotes the growth of beneficial bacteria.
SonoVive™ is a 100% natural hearing supplement by Sam Olsen made with powerful ingredients that help heal tinnitus problems and restore your hearing.
TerraCalm is a potent formula with 100% natural and unique ingredients designed to support healthy nails.
Alpha Tonic daily testosterone booster for energy and performance. Convenient powder form ensures easy blending into drinks for optimal absorption.
TonicGreens flushes away the harmful elements from your body, leaving you feeling refreshed and revitalized.
Neurozoom is one of the best supplements out on the market for supporting your brain health and, more specifically, memory functions.
Tropislim, is an all-natural dietary supplement. It promotes healthy weight loss through a proprietary blend of tropical plants and nutrients.
ProstateFlux™ is a natural supplement designed by experts to protect prostate health without interfering with other body functions.
Pineal XT™ is a dietary supplement crafted from entirely organic ingredients, ensuring a natural formulation.
GlucoBerry is a unique supplement that offers an easy and effective way to support balanced blood sugar levels.
BioVanish is a supplement from WellMe that helps consumers improve their weight loss by transitioning to ketosis.
BioFit is a natural supplement that balances good gut bacteria, essential for weight loss and overall health.
Joint Genesis is a supplement from BioDynamix that helps consumers to improve their joint health to reduce pain.
MenoRescue™ is a women’s health dietary supplement formulated to assist them in overcoming menopausal symptoms.
https://samye-luchshie-prostitutki-moskvy.top
Cortexi is a natural hearing support aid that has been used by thousands of people around the globe.
Amiclear is a blood sugar support formula that’s perfect for men and women in their 30s, 40s, 50s, and even 70s.
SharpEar™ is a 100% natural ear care supplement created by Sam Olsen that helps to fix hearing loss
MOTOLADY предлагают услуги аренды и проката мотоциклов и скутеров в Хургаде, Эль Гуне и Сахл Хашиш. MOTOLADY – одна из самых популярных компаний по прокату мотоциклов и скутеров. Они предлагают большой выбор транспортных средств по разумным ценам. MOTOLADY компания, специализирующаяся на Прокат мотоцикла в Эльгуне и Эль Гуне. Они предлагают услуги доставки транспорта в любое удобное для вас место. У нас в наличии различные модели транспортных средств по доступным ценам. Перед арендой транспорта обязательно ознакомьтесь с правилами и требованиями компании, также проверьте наличие страховки и необходимые документы для аренды.
Bona dicta — Поучительные слова
http://batmanapollo.ru
Veni, vidi, vici – пришел, увидел, победил
http://batmanapollo.ru
Ab imo pectore — С полной откровенностью.
http://batmanapollo.ru
https://batmanapollo.ru
Слово пацна 2 сезон Слово пацна 2 сезон 1 серия просмотр Слово пацна 2 сезон
Слово пацна 2 сезон Слово пацна 2 сезон 1 серия онлайн Слово пацна 2 сезон
Слово пацна 8 серия Слово пацна 8 серия онлайн Слово пацна 8 серия
Слово пацна 8 серия Слово пацна 8 серия сериал Слово пацна 8 серия
Everything has a second side (У всего есть вторая сторона)
http://batmanapollo.ru
Günsu AŞ Havuz, her projede mükemmel işçiliği ve özgün tasarımlarıyla fark yaratıyor.
Ad oculos — Наглядно
http://batmanapollo.ru
Boostaro increases blood flow to the reproductive organs, leading to stronger and more vibrant erections. It provides a powerful boost that can make you feel like you’ve unlocked the secret to firm erections
ErecPrime is a 100% natural supplement which is designed specifically
Puravive introduced an innovative approach to weight loss and management that set it apart from other supplements.
Prostadine™ is a revolutionary new prostate support supplement designed to protect, restore, and enhance male prostate health.
Aizen Power is a dietary supplement for male enhancement
Neotonics is a dietary supplement that offers help in retaining glowing skin and maintaining gut health for its users. It is made of the most natural elements that mother nature can offer and also includes 500 million units of beneficial microbiome.
EndoPeak is a male health supplement with a wide range of natural ingredients that improve blood circulation and vitality.
Glucotrust is one of the best supplements for managing blood sugar levels or managing healthy sugar metabolism.
EyeFortin is a natural vision support formula crafted with a blend of plant-based compounds and essential minerals. It aims to enhance vision clarity, focus, and moisture balance.
Support the health of your ears with 100% natural ingredients, finally being able to enjoy your favorite songs and movies
GlucoBerry is a meticulously crafted supplement designed by doctors to support healthy blood sugar levels by harnessing the power of delphinidin—an essential compound.
Оцифровка архивных документов цена — это наше направление. Мы предоставляем услуги перевода на цифровой носитель с использованием новейших методов. Сотрудничество с нами — это эффективный способ сделать вашу документацию доступной в электронной форме.
Free Shiping If You Purchase Today!
mba admission essays examples https://buyessaysonlinedsd50482.answerblogs.com/23800257/rumored-buzz-on-buy-essays-online-d-sd essay my favorite holiday
SonoVive™ is a completely natural hearing support formula made with powerful ingredients that help heal tinnitus problems and restore your hearing
BioFit™ is a Nutritional Supplement That Uses Probiotics To Help You Lose Weight
Dentitox Pro is a liquid dietary solution created as a serum to support healthy gums and teeth. Dentitox Pro formula is made in the best natural way with unique, powerful botanical ingredients that can support healthy teeth.
The ingredients of Endo Pump Male Enhancement are all-natural and safe to use.
Gorilla Flow is a non-toxic supplement that was developed by experts to boost prostate health for men.
GlucoCare is a natural and safe supplement for blood sugar support and weight management. It fixes your metabolism and detoxifies your body.
Nervogen Pro, A Cutting-Edge Supplement Dedicated To Enhancing Nerve Health And Providing Natural Relief From Discomfort. Our Mission Is To Empower You To Lead A Life Free From The Limitations Of Nerve-Related Challenges. With A Focus On Premium Ingredients And Scientific Expertise.
Neurodrine is a fantastic dietary supplement that protects your mind and improves memory performance. It can help you improve your focus and concentration.
InchaGrow is an advanced male enhancement supplement. The Formula is Easy to Take Each Day, and it Only Uses. Natural Ingredients to Get the Desired Effect
HoneyBurn is a 100% natural honey mixture formula that can support both your digestive health and fat-burning mechanism. Since it is formulated using 11 natural plant ingredients, it is clinically proven to be safe and free of toxins, chemicals, or additives.
GlucoFlush™ is an all-natural supplement that uses potent ingredients to control your blood sugar.
SynoGut is a natural dietary supplement specifically formulated to support digestive function and promote a healthy gut microbiome.
Amiclear is a dietary supplement designed to support healthy blood sugar levels and assist with glucose metabolism. It contains eight proprietary blends of ingredients that have been clinically proven to be effective.
Claritox Pro™ is a natural dietary supplement that is formulated to support brain health and promote a healthy balance system to prevent dizziness, risk injuries, and disability. This formulation is made using naturally sourced and effective ingredients that are mixed in the right way and in the right amounts to deliver effective results.
allkidsnetwork writing paper https://followbookmarks.com/story16278414/pay-someone-to-write-my-paper-cheap-can-be-fun-for-anyone christmas writing paper for first grade
TropiSlim is a unique dietary supplement designed to address specific health concerns, primarily focusing on weight management and related issues in women, particularly those over the age of 40.
ProDentim is a nutritional dental health supplement that is formulated to reverse serious dental issues and to help maintain good dental health.
GlucoFlush Supplement is an all-new blood sugar-lowering formula. It is a dietary supplement based on the Mayan cleansing routine that consists of natural ingredients and nutrients.
Metabo Flex is a nutritional formula that enhances metabolic flexibility by awakening the calorie-burning switch in the body. The supplement is designed to target the underlying causes of stubborn weight gain utilizing a special “miracle plant” from Cambodia that can melt fat 24/7.
SynoGut is an all-natural dietary supplement that is designed to support the health of your digestive system, keeping you energized and active.
Glucofort Blood Sugar Support is an all-natural dietary formula that works to support healthy blood sugar levels. It also supports glucose metabolism. According to the manufacturer, this supplement can help users keep their blood sugar levels healthy and within a normal range with herbs, vitamins, plant extracts, and other natural ingredients.
Manufactured in an FDA-certified facility in the USA, EndoPump is pure, safe, and free from negative side effects. With its strict production standards and natural ingredients, EndoPump is a trusted choice for men looking to improve their sexual performance.
While Inchagrow is marketed as a dietary supplement, it is important to note that dietary supplements are regulated by the FDA. This means that their safety and effectiveness, and there is 60 money back guarantee that Inchagrow will work for everyone.
GlucoCare is a dietary supplement designed to promote healthy blood sugar levels, manage weight, and curb unhealthy sugar absorption. It contains a natural blend of ingredients that target the root cause of unhealthy glucose levels.
Introducing FlowForce Max, a solution designed with a single purpose: to provide men with an affordable and safe way to address BPH and other prostate concerns. Unlike many costly supplements or those with risky stimulants, we’ve crafted FlowForce Max with your well-being in mind. Don’t compromise your health or budget – choose FlowForce Max for effective prostate support today!
Nervogen Pro is a cutting-edge dietary supplement that takes a holistic approach to nerve health. It is meticulously crafted with a precise selection of natural ingredients known for their beneficial effects on the nervous system. By addressing the root causes of nerve discomfort, Nervogen Pro aims to provide lasting relief and support for overall nerve function.
FitSpresso stands out as a remarkable dietary supplement designed to facilitate effective weight loss. Its unique blend incorporates a selection of natural elements including green tea extract, milk thistle, and other components with presumed weight loss benefits.
Herpagreens is a dietary supplement formulated to combat symptoms of herpes by providing the body with high levels of super antioxidants, vitamins
Gorilla Flow is a non-toxic supplement that was developed by experts to boost prostate health for men. It’s a blend of all-natural nutrients, including Pumpkin Seed Extract Stinging Nettle Extract, Gorilla Cherry and Saw Palmetto, Boron, and Lycopene.
SonoVive is an all-natural supplement made to address the root cause of tinnitus and other inflammatory effects on the brain and promises to reduce tinnitus, improve hearing, and provide peace of mind. SonoVive is is a scientifically verified 10-second hack that allows users to hear crystal-clear at maximum volume. The 100% natural mix recipe improves the ear-brain link with eight natural ingredients. The treatment consists of easy-to-use pills that can be added to one’s daily routine to improve hearing health, reduce tinnitus, and maintain a sharp mind and razor-sharp focus.
TerraCalm is an antifungal mineral clay that may support the health of your toenails. It is for those who struggle with brittle, weak, and discoloured nails. It has a unique blend of natural ingredients that may work to nourish and strengthen your toenails.
купить хостинг
Когда речь заходит о создании своего собственного сайта, выбор хостинга играет огромную роль. Ведь именно хостинг будет определять доступность и быстродействие вашего сайта для пользователей. Если вы находитесь в Беларуси и ищете надежного хостинг-провайдера, то BestHost.BY – это отличный выбор. BestHost.BY – одна из ведущих хостинг-компаний в Беларуси, предоставляющая высококачественные услуги уже на протяжении 15 лет.
1xbet зеркало рабочее на сегодня – это популярная букмекерская компания, предлагающая широкий выбор ставок на спорт, казино и многое другое. С высокими коэффициентами и удобным интерфейсом, 1xbet привлекает множество игроков. Он также предоставляет возможность онлайн-трансляций событий. 1xbet создает захватывающий игровой опыт для своих пользователей.
1xbet зеркало на сегодня прямо – это популярная букмекерская компания, предлагающая широкий выбор ставок на спорт, казино и многое другое. С высокими коэффициентами и удобным интерфейсом, 1xbet привлекает множество игроков. Он также предоставляет возможность онлайн-трансляций событий. 1xbet создает захватывающий игровой опыт для своих пользователей.
Холоп 2 скачать торрент. Холоп 2. Холоп фильм 2024 актеры. Холоп 2 трейлер на русском. Где найти фильм холоп в хорошем качестве бесплатно. Скачать фильм холоп. Холоп актеры. Фильм холоп 2.
Amazing, blog yang fantastis! 🌟 Saya sangat impressed dengan kontennya yang informatif dan mencerahkan. Setiap artikel memberikan pengetahuan tambahan dan segar. 🚀 Saya sungguh-sungguh menikmati membaca setiap kata. Semangat terus! 👏 Sudah tidak sabar untuk membaca postingan berikutnya. 📚 Terima kasih atas kontribusinya dalam memberikan informasi yang berguna dan menginspirasi. 💡🌈 Keep up the great work! linetogel 🙌
Холоп 2 фильм 2024 актеры. Холоп 2 смотреть онлайн бесплатно в хорошем. Холоп 1. Холоп 2 дата выхода в россии в кинотеатрах. Фильм холоп смотреть онлайн бесплатно в хорошем качестве. Холоп 2 фильм 2024 актеры.
Фильм холоп смотреть онлайн бесплатно. Холоп смотреть онлайн бесплатно. Смотреть фильм холоп онлайн бесплатно в хорошем качестве. Холоп 2 смотреть бесплатно. Холоп фильм. Холоп смотреть онлайн бесплатно в хорошем. Холоп 2 фильм. Холоп 2 дата выхода. Холоп 1 смотреть. Холоп 2 фильм 2024 смотреть. Холоп 2 фильм 2024.
Когда выйдет холоп 2. Холоп 2 дата выхода в россии. Холоп 2 актеры. Фильм холоп смотреть онлайн. Фильм холоп актеры. Холоп 2 трейлер. Актеры фильма холоп. Кто такой холоп.
Скачать фильм холоп. Фильм холоп смотреть. Холоп фильм смотреть. Холоп скачать торрент. Где найти фильм холоп в хорошем качестве бесплатно. Холоп 2 смотреть онлайн бесплатно в хорошем качестве. Холоп смотреть онлайн бесплатно. Когда выйдет холоп 2. Холоп 1 смотреть. Холоп актеры и роли. Трейлер холоп 2.
Теория внутреннего стимулирования лидерства. Тренинг лидерства. Великобритания экономическое лидерство и политические реформы конспект. Модель ситуационного лидерства херсея и бланшарда. Тренинг лидерство для руководителей. Авторитарное лидерство это. Эффективное лидерство. Макс вебер лидерство. Анархический тип политического лидерства.
Ситуационная модель лидерства херси и бланшара. Лидерство в команде. Ситуационная теория лидерства. Кен бланшар лидерство к вершинам успеха. Типы лидерства в психологии. Понятие лидерства. Транзакционное лидерство.
Проблемы лидерства. Оценка персонала на лидерство развитие лидерских компетенций. Книги лидерство купить. Лаборатория лидерства. Тренинг лидерство для руководителей. Сетевая модель лидерства статьи. Лидерство и командообразование. Лидерство это простыми словами.
Cortexi is an effective hearing health support formula that has gained positive user feedback for its ability to improve hearing ability and memory. This supplement contains natural ingredients and has undergone evaluation to ensure its efficacy and safety. Manufactured in an FDA-registered and GMP-certified facility, Cortexi promotes healthy hearing, enhances mental acuity, and sharpens memory.
Джон максвелл лидерство. Лидерство курс. Технологии формирования лидерства. Пять уровней лидерства джона максвелла. Основные теории лидерства. Трансформационное лидерство это.
Стили лидерства в менеджменте. Анархический тип политического лидерства. 5 уровней лидерства джон максвелл. Каковы причины потери англией промышленного лидерства. Картинки для презентации лидерство. Стратегия ценового лидерства. Курсы по лидерству для руководителей. Тренинги лидерства.
Buy discount supplements, vitamins, health supplements, probiotic supplements. Save on top vitamin and supplement brands.
Общенациональный тип политического лидерства. Германия на пути к европейскому лидерству 9 класс кратко. Тренинги по лидерству. Стили лидерства по левину. Наибольшую эффективность в современных условиях предлагает подход к пониманию сути лидерства. Конспект германия на пути к европейскому лидерству. По стилю общения лидера с подчиненными различают харизматический рационально легальный тип лидерства. 8 уроков лидерства кийосаки.
Традиционный тип лидерства примеры. Авторитарный стиль лидерства. Сетевое лидерство это. Тест на лидерство в коллективе. Согласно какой теории руководства и лидерства лидерами рождаются а не становятся. Психология лидерства реферат. Основная характеристика современного института лидерства. Природа лидерства. Современные подходы к лидерству.
Теория лидерства и власти никколо макиавелли. Стратегия лидерства по издержкам нацелена на. Харизматический тип лидерства. Типы лидерства в менеджменте. Технологии формирования лидерства. Современные подходы к лидерству. Лидерство во льдах. Психология политического лидерства и управления.
Ситуационное лидерство институт тренинга. Перечислите принципы лидерства. Креативная модель лидерства выстраивается в последовательности от. Стиль лидерства. Многофакторный опросник лидерства.
Отличительным признаком лидерства любого типа является. Книги по лидерству. Формальное лидерство. Стратегия лидерства. Рационально легальное лидерство примеры. Политическое лидерство это. Джон максвелл лидерство.
Wah, blog ini memang luar biasa! 🚀 Saya terkesan dengan kontennya yang penuh semangat dan informatif. 🌟 Setiap artikel memberikan wawasan baru dan inspiratif. 👏 Saya sangat merasa terhubung dengan topik yang menarik dan berhubungan. 🤩 Tambahkan selalu konten-konten seru seperti ini! 💯 Jangan berhenti berbagi pengetahuan dan keceriaan. 🌈 Terima kasih terima kasih banyak atas dedikasinya! 🙌✨ Ayo bertambah berkarya dan buat blog ini sebagai sumber inspirasi bagi semua! 🌟👍 #SemangatPositif #PenuhInspirasi #NomorSatu
Luar biasa blog ini! 🚀 Isi yang begitu energik dan menghibur. 🌟 Saya benar-benar terkesan dengan gayanya menulis yang menarik. 👏 Teruslah berbagi semangat dan pengetahuan baru! 🤩💯 Artikel ini sungguh menawan hati! 🌈 Terima kasih terima kasih banyak! 🙌✨ #Inspiratif #SemangatPositif #Energik
Hebat, blog ini luar biasa! 🚀 Isinya energik dan pengetahuan yang menarik perhatian. 🌟 Artikel yang memotivasi! 👏 Teruslah berbagi kebaikan! 🤩💯 Sungguh memikat hati! 🌈 Terima kasih atas keceriaannya! 🙌✨ #Inspirasional #SemangatBaru #Terbaik
While improving eyesight isn’t often the goal of consumers who wear their glasses religiously, it doesn’t mean they’re stuck where they are.
Sight Care is a daily supplement proven in clinical trials and conclusive science to improve vision by nourishing the body from within. The Sight Care formula claims to reverse issues in eyesight, and every ingredient is completely natural.
Почему англия теряла промышленное лидерство в мире. Центр цифрового лидерства sap. Наибольшую эффективность в современных условиях предлагает подход к пониманию сути лидерства. По количеству компьютеров на душу населения мировое лидерство удерживают. Вопросы про лидерство. Авторитарное лидерство это.
К харизматическому типу политического лидерства. Лидерство в группе огэ обществознание. Академия лидерства детский лагерь. Презентация великобритания экономическое лидерство и политические реформы 9 класс. Про лидерство. Ситуационное лидерство херси и бланшара. Типы политического лидерства. Креативное лидерство.
Джон максвелл лидерство. Дайте определение типу лидерства служитель. Курсы по лидерству. Теория политических элит и политическое лидерство. 5 уровней лидерства джон максвелл. Авторитарное лидерство предполагает единоличное направляющее воздействие лидера на подчиненных.
Природа лидерства. Принципы лидерства. Рационально легальное лидерство. Проявление лидерства. Тест по истории 9 класс великобритания экономическое лидерство и политические реформы. Исследование бюрократии и форм политического лидерства. Креативное лидерство setters.
Манипуляция и лидерство. Отличительным признаком лидерства любого типа является. Сетевое лидерство это. Наиболее значимые признаки лидерства в психологии доклад. Чем обеспечивается лидерство в области охраны труда. Сущность и стили политического лидерства.
Закажите перетяжку мягкой мебели с гарантией качества
Обновление мягкой мебели: простой способ обновить интерьер
Качественное обслуживание перетяжки мягкой мебели
Легко и просто обновить диван или кресло
ремонт мебели в Минске https://www.peretyazhkann.ru/.
Смотреть фильмы онлайн бесплатно в хорошем качестве. Фильмы и сериалы — где смотреть онлайн бесплатно? Фильмы 2023 смотреть онлайн бесплатно в хорошем качестве. Фильмы 2024 смотреть онлайн бесплатно в хорошем качестве. 5 лучших способов смотреть фильмы онлайн вместе. 10 лучших сайтов для просмотра бесплатных фильмов онлайн. Фильмы 2023 смотреть онлайн бесплатно в хорошем качестве HD.
https://tinyurl.com/yvb6ogpx
Смотреть фильмы онлайн бесплатно в хорошем качестве. Смотреть новые фильмы онлайн, которые уже вышли. Новинки. Смотреть фильмы онлайн. Фильмы онлайн смотреть онлайн. Смотреть фильмы онлайн в хорошем качестве Full HD 720. Фильмы – смотреть онлайн бесплатно в хорошем качестве. Фильмы – смотреть онлайн в хорошем качестве. Смотреть фильмы онлайн бесплатно в хорошем качестве.
Фильмы и сериалы онлайн смотреть онлайн. Смотреть фильмы в хорошем качестве (HD, 1080p) в онлайн. Смотреть фильмы онлайн бесплатно в хорошем качестве. Смотреть новые фильмы онлайн, которые уже вышли. Новинки. Смотреть фильмы онлайн. Фильмы онлайн смотреть онлайн.
Фильмы смотреть онлайн. Смотреть фильмы онлайн бесплатно в хорошем качестве. Смотреть новые фильмы онлайн, которые уже вышли. Новинки. Смотреть фильмы онлайн в хорошем качестве. Список лучших. Фильмы – смотреть онлайн бесплатно в хорошем качестве. Фильмы онлайн смотреть онлайн. Смотреть фильмы онлайн в хорошем качестве Full HD 720.
Смотреть русские фильмы онлайн, новинки бесплатно, которые уже вышли. Смотреть фильмы онлайн бесплатно в хорошем качестве. Фильмы и сериалы — где смотреть онлайн бесплатно? Фильмы 2023 смотреть онлайн бесплатно в хорошем качестве. Фильмы 2024 смотреть онлайн бесплатно в хорошем качестве.
Хостинг Windows VDS / VPS серверов
– Более 15 000 сервер уже РІ работе
– Возможность арендовать сервер РЅР° 1 час или 1 сутки
– Дата-центр РІ РњРѕСЃРєРІРµ Рё Амстердаме
– Отлично РїРѕРґС…РѕРґРёС‚ РїРѕРґ GSA Search Engine Ranker
– Outline VPN, WireGuard VPN, IPsec VPN.
– Супер (аптайм, скорость, РїРёРЅРі, нагрузка)
– Ubuntu, Debian, CentOS, Oracle 9 – бесплатно
– Скорость порта подключения Рє сети интернет — 1000 РњР±РёС‚/сек
– Отлично РїРѕРґС…РѕРґРёС‚ РїРѕРґ Xneolinks
– Автоматическая установка Windows – бесплатно
– Управляйте серверами РЅР° лету.
– Круглосуточная техническая поддержка – бесплатно
– Мгновенное развёртывание сервера РІ несколько кликов – бесплатно
– Отлично РїРѕРґС…РѕРґРёС‚ РїРѕРґ A-Parser
– Почасовая оплата
– Windows – 2022, 2019, 2016, 2012 R2
– FASTPANEL Рё HestiaCP – бесплатно
– Отлично РїРѕРґС…РѕРґРёС‚ РїРѕРґ XRumer + XEvil
– Быстрые серверы СЃ NVMe.
– Windows – 2012 R2, 2016, 2019, 2022 – бесплатно
– Для сервера сеть РЅР° скорости 1 Гбит!
– Отлично РїРѕРґС…РѕРґРёС‚ РїРѕРґ CapMonster
Купить VPS/VDS серверы
– Автоматическая установка Windows – бесплатно
– Супер (аптайм, скорость, пинг, нагрузка)
– Отлично подходит под A-Parser
– Мгновенное развёртывание сервера в несколько кликов – бесплатно
– Дата-центр в Москве и Амстердаме
– Скорость порта подключения к сети интернет — 1000 Мбит/сек
– Отлично подходит под XRumer + XEvil
– Отлично подходит под Xneolinks
– FASTPANEL и HestiaCP – бесплатно
– Отлично подходит под CapMonster
– Для сервера сеть на скорости 1 Гбит!
– Windows – 2022, 2019, 2016, 2012 R2
– Возможность арендовать сервер на 1 час или 1 сутки
– Windows – 2012 R2, 2016, 2019, 2022 – бесплатно
– Ubuntu, Debian, CentOS, Oracle 9 – бесплатно
– Более 15 000 сервер уже в работе
– Outline VPN, WireGuard VPN, IPsec VPN.
– Быстрые серверы с NVMe.
– Круглосуточная техническая поддержка – бесплатно
– Отлично подходит под GSA Search Engine Ranker
– Управляйте серверами на лету.
– Почасовая оплата
Купить VPS/VDS серверы
– Windows – 2012 R2, 2016, 2019, 2022 – бесплатно
– Мгновенное развёртывание сервера в несколько кликов – бесплатно
– Возможность арендовать сервер на 1 час или 1 сутки
– Супер (аптайм, скорость, пинг, нагрузка)
– Отлично подходит под XRumer + XEvil
– Отлично подходит под A-Parser
– Outline VPN, WireGuard VPN, IPsec VPN.
– FASTPANEL и HestiaCP – бесплатно
– Отлично подходит под CapMonster
– Ubuntu, Debian, CentOS, Oracle 9 – бесплатно
– Для сервера сеть на скорости 1 Гбит!
– Скорость порта подключения к сети интернет — 1000 Мбит/сек
– Windows – 2022, 2019, 2016, 2012 R2
– Круглосуточная техническая поддержка – бесплатно
– Отлично подходит под GSA Search Engine Ranker
– Быстрые серверы с NVMe.
– Дата-центр в Москве и Амстердаме
– Автоматическая установка Windows – бесплатно
– Почасовая оплата
– Управляйте серверами на лету.
– Отлично подходит под Xneolinks
– Более 15 000 сервер уже в работе
Аренда VDS или VPS сервера
– Отлично подходит под CapMonster
– Круглосуточная техническая поддержка – бесплатно
– Мгновенное развёртывание сервера в несколько кликов – бесплатно
– Управляйте серверами на лету.
– Отлично подходит под Xneolinks
– Более 15 000 сервер уже в работе
– Отлично подходит под A-Parser
– Скорость порта подключения к сети интернет — 1000 Мбит/сек
– Outline VPN, WireGuard VPN, IPsec VPN.
– Windows – 2012 R2, 2016, 2019, 2022 – бесплатно
– Почасовая оплата
– Дата-центр в Москве и Амстердаме
– Для сервера сеть на скорости 1 Гбит!
– Windows – 2022, 2019, 2016, 2012 R2
– FASTPANEL и HestiaCP – бесплатно
– Отлично подходит под GSA Search Engine Ranker
– Отлично подходит под XRumer + XEvil
– Автоматическая установка Windows – бесплатно
– Супер (аптайм, скорость, пинг, нагрузка)
– Возможность арендовать сервер на 1 час или 1 сутки
– Быстрые серверы с NVMe.
– Ubuntu, Debian, CentOS, Oracle 9 – бесплатно
Купить VPS/VDS серверы
– Возможность арендовать сервер на 1 час или 1 сутки
– Для сервера сеть на скорости 1 Гбит!
– Outline VPN, WireGuard VPN, IPsec VPN.
– Отлично подходит под CapMonster
– Более 15 000 сервер уже в работе
– Скорость порта подключения к сети интернет — 1000 Мбит/сек
– Мгновенное развёртывание сервера в несколько кликов – бесплатно
– Управляйте серверами на лету.
– Почасовая оплата
– FASTPANEL и HestiaCP – бесплатно
– Супер (аптайм, скорость, пинг, нагрузка)
– Быстрые серверы с NVMe.
– Дата-центр в Москве и Амстердаме
– Автоматическая установка Windows – бесплатно
– Отлично подходит под A-Parser
– Windows – 2022, 2019, 2016, 2012 R2
– Круглосуточная техническая поддержка – бесплатно
– Windows – 2012 R2, 2016, 2019, 2022 – бесплатно
– Отлично подходит под Xneolinks
– Отлично подходит под XRumer + XEvil
– Отлично подходит под GSA Search Engine Ranker
– Ubuntu, Debian, CentOS, Oracle 9 – бесплатно
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me. https://www.binance.com/zh-TC/join?ref=FIHEGIZ8
https://tinyurl.com/ypfn4hn6
https://tinyurl.com/yp3e64k9
Освежить мягкую мебель в доме: лучшие методы новый вид старой мебели: эффектные идеи перетягивать мебель своими руками: шаг за шагом ткани для перетяжки мягкой мебели: Как сэкономить на перетяжке мягкой мебели: советы экономистов
обивка мебели.
Дайте новую жизнь вашей мебели с помощью перетяжки
Отремонтировать мягкую мебель в доме: Придать новый вид старой мебели: эффектные идеи перетягивать мебель своими руками: шаг за шагом ткани для перетяжки мягкой мебели: Как сэкономить на перетяжке мягкой мебели: безболезненный выбор
перетяжка мягкой мебели.
Перетяжка мягкой мебели: как сохранить стиль дома
“Melin Ajans, İstanbul fuarlarının vazgeçilmezi. Profesyonelliklerini her zaman takdir ediyoruz.”
“Fuarlarımızın vazgeçilmezi Melin Ajans, teşekkürler!”
Impressive piece! The article is well-structured and informative. Adding more visuals in your future articles could be a great way to enrich the reader’s experience.
Sight Care is a natural supplement designed to improve eyesight and reduce dark blindness. With its potent blend of ingredients. https://sightcarebuynow.us/
SightCare supports overall eye health, enhances vision, and protects against oxidative stress. Take control of your eye health and enjoy the benefits of clear and vibrant eyesight with Sight Care https://sightcarebuynow.us/
Sight Care is a natural supplement designed to improve eyesight and reduce dark blindness. With its potent blend of ingredients. https://sightcarebuynow.us/
SightCare supports overall eye health, enhances vision, and protects against oxidative stress. Take control of your eye health and enjoy the benefits of clear and vibrant eyesight with Sight Care. https://sightcarebuynow.us/
Новое покрытие для вашей мебели: перетяжка
перетяжка мебели https://peretyazhka-mebeli-v-minske.ru/.
Отдыхайте с комфортом на мягкой мебели
мебель https://murom-mebel-tula.ru/.
Обновление мебели плюс индивидуальный дизайн
перетяжка диванов обивка мягкой мебели.
Акции на ремонт холодильников
ремонт холодильников ремонт холодильника.
->>>>>>>>>>>>>последствия приворотов для мужчин<<<<<<<<<-
______________заговор на церковную свечу _____________
присушка на любовь девушки
приворот на удачу и деньги читать в домашних условиях, а также:
->>>>>>заговор на любовь по фотографии читать
->>>>>>самый сильный заговор на мужа
->>>>>>присушка по фото в домашних условиях
->>>>>>сильный приворот на любовь мужчины читать
еврейские привороты
технические двери купить https://texnicheskiedveri.ru/.
перетяжка мягкой мебели https://peretyazhka-bel.ru/.
Conclamatum est — Всё кончено, всё погибло.
http://batmanapollo.ru
Ad usum internum — Для внутреннего употребления.
http://batmanapollo.ru
сериал бесплатно
черный очень сильный приворот – Обратится к магу – https://dzen.ru/id/653538d7d6100f7a6fee8469
фильм приворот черное венчание википедия
Agere sequitur esse — филос. Действие вытекает из бытия.
http://batmanapollo.ru
Магическая помощь – сильные экстрасенсы
сексуальная привязка на фото https://gadalkindom.ru заговор на мужчину в домашних условиях
как приворожить девушку без последствия на любовь на расстоянии
ищу магическую помощь ->>>>>>>приворот и магическая помощь https://www.magecam.ru <<<<<<<<<<-
https://www.magecam.ru
Услуги магов
-привороты
-наведение порчи на смерть
-отнятие удачи
-возврат любимого
сильные маги настоящие
Черный маг
как сделать приворот на женщину https://gadalkindom.ru привороты на любовь мужчины читать в домашних условиях
приворот на волос любимого
бой и порча товаров https://www.magecam.ru порча на рост
как понять что на человеке приворот – Помощь экстрасенса https://www.magecam.ru – приворот на бумаге как привязать любимого к себе
услуги экстрасенса цена в москве ->>>>>>>экстрасенс дарья миронова стоимость услуг https://www.magecam.ru <<<<<<<<<<-
как узнать что на тебе порча или приворот https://www.magecam.ru настоящий маг приворот
приворот в домашних условиях видео
naturally like your web site however you need to take a look at the spelling on several of your posts. A number of them are rife with spelling problems and I find it very bothersome to tell the truth on the other hand I will surely come again again.
psyho2031.8ua.ru
psyho2037.8ua.ru
->>>>>>>>>>>>>сильный приворот любимого<<<<<<<<<-
______________сильный приворот на замок для жены _____________
на любовь мужчины заговор https://privorot4.wordpress.com
приворот на мужчину в домашних условиях без последствия сразу действует, а также:
->>>>>>можно ли делать приворот в новолуние
->>>>>>как избавиться от девушки сына которая на него плохо действует
->>>>>>как приворожить девушку на расстоянии без последствия в домашних условиях
->>>>>>заговор на возврат любимого без последствия в домашних условиях без фото на расстоянии
Быстрый онлайн займ на карту – это финансовая услуга, предоставляемая онлайн-платформами, которые обеспечивают оперативное оформление займов и перевод средств на банковские карты клиентов. Это современный способ получения финансовой помощи.
->>>>>>>>>>>>>сильный заговор на женатого мужчину<<<<<<<<<-
______________белая магия приворот на любовь парня _____________
верну любимого человека бесплатно
приворот на любовь парня читать в домашних условиях по фото https://privorot4.wordpress.com сильный приворот на жену в домашних
как навсегда привязать к себе мужчину
отворот от ребенка, а также:
->>>>>>любовный приворот на мужчину в домашних
вольт приворот приворот мужа на кровь из пальца – https://magic-white.net безопасный приворот на любовь парня читать в домашних условиях без свечей
радость общения приворот самостоятельный приворот люб самый сильный приворот вернуть померится с жиной
https://artgrom.com
диагностика приворота онлайн бесплатно как сделать любовный приворот на девушку в домашних условиях читать
рунический приворот зомби из книги ворона – https://simvolmagii.ru приворот на месячные на фото
приворот мужчины на расстоянии читать в домашних – https://vsezagovori.ru как узнать кто навел приворот на мужа
– приворот с сигаретой отзывы
– https://privorot-vsem.ru фиалка рс приворотное зелье
– приворот на свечах и крови
– схема начала действия приворота
размещать блог приворот – https://магиявера.рф
как приворот действует на мужчину последствия любовный приворот как определить – https://мир-магов.рф признаки приворота у мужчин как определить и его
what is tadalafil 20 mg
приворот мужа к жене на расстоянии приворот на мужчину без последствия в домашних условиях по фото белая магия
приворот на мужчину читать в домашних условиях который – https://stepslove.ru как узнать о привороте
Мастер и Маргарита 2024
череп и куклу привязанную к кресту на что эта порча – https://darstars.ru лечится гипнозом приворотная порча
приворот на женатого приворот как определить и снять – https://zakolduj.ru приворот на женщину без последствия в домашних условиях чтоб полюбила по фото
зачет по приворотам очень сильный приворот на любовь мужчины на расстоянии читать
приворот на девушку в домашних – https://simvolmagii.ru снятие приворота по фото
белые привороты на любовь парня читать в домашних условиях – https://turk-sinema.ru как убрать приворот в домашних условиях
приворот похож на синусоиду привороты на клиентов приворот на возврат кровь
https://fb.ru
– як зробити приворот на мосячно
– https://magicwishes.ru самый лёгкий приворот
– сайт степановой приворот на мужчину
– привороты и заговоры семейные
Great information shared.. really enjoyed reading this post thank you author for sharing this post .. appreciated
порча на смерть рабочая сделать порча на смерть как навести порчу на смерть
приворот на вольт форум кто приворот белый – медицинская астрология молитва от приворота и колдовства на сына
ирина астрология хорарной астрологией
репетитор астрологии
сильный приворот на фото который нельзя снять – https://www.sowilo.ru сильная молитва на приворот мужчины
===============================================================================
приворот после результата
признаки кладбищенского приворота приворот на мужчину без последствия сразу действует в домашних на имя
как понять что на тебя сделали приворот – https://starway555.ru магия приворота мужчин
======================
приворот на дружбу друзей услуги приворот верну в семью рунический приворот по чакрам
https://www.woman.ru
привороты западная украина
следствия приворотов
приворотные слова чтоб муж сильно любил
– приворот на расстоянии невестку
– https://psy-magic.org приворот по фото черное венчание
– приворот спб татьяна
– что не надо делать после приворота
– приворот на сколько он действуетпривороты на сигарете отзывыприворот что
энтропия импульса – энтропия неопределенность.
изменение энтропии – https://privorot-vsem.ru начальная энтропия.
нормальная энтропия
крыло энтропии
повелитель энтропии
приворот при помощи роз = https://magicwishes.ru приворот на безжалостность
привороты от измен стопроцентные привороты
введение философия объект философии
философия питанияфилософия рисункифетишизм философия
философия возрождение псевдо философия философия игры
New! Enhanced options to earn 3% cash back based on Bank of America customer feedback. Maximize your rewards with 3% cash back in the category of your choice — with newly-expanded options. https://wisethink.us/
порча на одиночество наложить – https://artgrom.com сглаз, порча и как с ними бороться.
как делается порча на деньги начальника
порча как переводится на немецкий
колдовство порча в детской игрушке
как с помощью куриного яйца узнать есть ли порча
приворот на кладбищенскую землю сильнейший приворот на любовь мужчины который нельзя снять читать в домашних условиях – астрология диаграмма сильный приворот на мужчину читать на растущую луну
орбы астрология вуз астрологии.
мэджик астрология. астрологии нумерология астрология европейская.
I appreciate you sharing this blog post. Thanks Again. Cool.
приворот на подарок любимому читать – https://docgid.ru молитва о снятии приворота.
самый сильный приворот на любовь
экстрасенсы приворот
самые эффективные привороты в домашних условиях
сложно снять приворот
приворот на месячной крови по фотографии .
приворот чертогрыз кто делал самый сильный приворот на последний день года
приворот с 31 на 1 января фото месячные – https://morfeos.ru сильнейший бесплатный приворот любимого .
привороты и отвороты украина сексуальный приворот дыхание любви.
Find healthy, delicious recipes and meal plan ideas from our test kitchen cooks and nutrition experts at SweetApple. Learn how to make healthier food choices every day. https://sweetapple.site/
RVVR is website dedicated to advancing physical and mental health through scientific research and proven interventions. Learn about our evidence-based health promotion programs. https://rvvr.us/
===============================================================================
приворот на волосы и кровь
сильнейший приворот.
приворот без последствий читать в домашних цыганский приворот на подарок кто.
кладбищенский приворот самостоятельно – https://duhmaga.ru приворот любимого читать в домашних условиях сильнейший.
белые привороты на мужчину без последствия сразу действует
вернуть любимую девушку с помощью приворота по фотографии
======================
– приворот на любовь номер телефона парня
– https://belli-portelli.com снять приворот владимир
приворот на виноградную лозу сделаю приворот объявления цена
привороты магия колдовство видео сильные привороты на любовь тоску
привороты от мандрагоры приворот на любовь парня по фото онлайн бесплатно
The latest news on grocery chains, celebrity chefs, and fast food – plus reviews, cooking tips and advice, recipes, and more. https://megamenu.us/
View the latest from the world of psychology: from behavioral research to practical guidance on relationships, mental health and addiction. Find help from our directory of therapists, psychologists and counselors. https://therapisttoday.us/
Virginia News: Your source for Virginia breaking news, sports, business, entertainment, weather and traffic https://virginiapost.us/
Island Post is the website for a chain of six weekly newspapers that serve the North Shore of Nassau County, Long Island published by Alb Media. The newspapers are comprised of the Great Neck News, Manhasset Times, Roslyn Times, Port Washington Times, New Hyde Park Herald Courier and the Williston Times. Their coverage includes village governments, the towns of Hempstead and North Hempstead, schools, business, entertainment and lifestyle. https://islandpost.us/
приворот ком приворот на цветы – астрология дхарма приворот на мужчину без последствия сразу действует в домашних на имя на расстоянии навсегда
прогрессии астрология селена астрология.
астрология евреев. астрология пифагор
навигатор астрология.
Covering the latest beauty and fashion trends, relationship advice, wellness tips and more. https://gliz.us/
приворот что это и какие последствия – https://www.sowilo.ru приворот на любовь по фото читать в домашних условиях.
черный приворот на женатого мужчину который нельзя снять. приворот чтобы муж вернулся
как сделать приворот на дому приворот парня на сигарету
приворот по фотографии девушки.
For the reason that the admin of this site is working, no uncertainty very quickly it will be renowned, due to its quality contents.
заговор приворот на любовь мужчины читать самостоятельно состояние после приворота.
приворот на любовь девушки читать в домашних как узнать есть ли приворот на мужчине в домашних условиях.
приворот на волос девушки читать – https://domorakula.com приворот на мужчину без последствия сразу действует форум.
последствия приворота на крови месячных приворот на любовь с призывом демона ощущения при привороте
Colorado breaking news, sports, business, weather, entertainment. https://denver-news.us/
Breaking food industry news, cooking tips, recipes, reviews, rankings, and interviews https://tastingcorner.us/
приворот с использованием свадебного торта. приворот на землю с трех могил приворот парня молитвами
https://koldovstvo.net .
////скачать бесплатно книги о любовных приворотах приворот черный сват тонкий мир.
////снятие приворота через вольт.
////приворот на кровь,если любимого нет рядом
Healthcare Blog provides news, trends, jobs and resources for health industry professionals. We cover topics like healthcare IT, hospital administration, polcy
BioPharma Blog provides news and analysis for biotech and biopharmaceutical executives. We cover topics like clinical trials, drug discovery and development, pharma marketing, FDA approvals and regulations, and more. https://biopharmablog.us/
– приворот со свечами и спичками – приворот на зеркалах и кукле действия и эффект.
– https://morfeos.ru приворот на любовь от куриловой
-снятие приворота в воткинске приворот по вуду без греха.приворот на яфйце.
-самый сильный и действенный белый приворот старые любовные привороты и белая магия.привороты н.степановой.
-приворот на менструальную кровь как о приворот на приход любимого бесплатно и самостоятельно
http://psyho2039.8ua.ru/
черный приворот на парня читать в домашних условиях на расстоянии без фото и свечей сильный приворот на бывшего парня – https://knyazhinskaya.ru приворот на порог
имя астрология астрология клип.
виды астрология. астрология экзальтация
вектор астрология.
приворот на женщину без последствия в домашних условиях по фото – https://volhovnov.ru молитвы приворот на любовь.
приворот на имя на бумаге. привороты днем на любовь мужчины
как понять что приворот снят с мужчины приворот чтобы позвонил
как узнать есть на муже приворот.
1xbet зеркало рабочее– это популярная букмекерская контора, предоставляющая широкий выбор ставок на спорт и казино. Сайт обладает удобным интерфейсом, мобильной версией и приложением для удобства пользователей. 1xBet также известен разнообразными акциями и бонусами, делая игровой опыт более захватывающим.
Looking for quick and easy dinner ideas? Browse 100
приворот на свечах на любовь приворот на девушку без последствия сразу в домашних условиях.
приворот на любовь парня по фото снять рунами приворот с себя.
любовный приворот девушки по фото – https://mysekret.ru черный приворот на парня читать в домашних.
на какую луну делается приворот как начинает действовать приворот приворот на красоту читать в домашних
черная магия приворот сделать самой без чьей либо помощи. сильные привороты омск черная магия привороты на крови.
https://moyozdorove.ru .
приворот на фото в домашних условиях самостоятельно приворот на месячные в кофе.
– что нужно делать после приворота заказчику – страстный приворот от феникса.
– https://cardul.ru привороты руны
-привороты в вечернее время приворот на вечную любовь как дейтвует.рождественский приворот любимого.
-сколько стоит приворот в челябинске приворот на воль из теста.приворот на свадебный букет.
-сайт чёрной магии иконый приворот самый сильный приворот форум
приворот новосибирск самый легкий приворот парня – https://nagadali.ru сильнейший приворот на бывшего
ураническая астрология украина астрология.
астрология презентации. спб астрология
черная астрология.
приворот на тоску мужчины привороты на парня без последствия в домашних условиях без фото и свечей.
приворот на девушку по волосам читать . приворот на парня на вещи , приворот на квартиру.
кладбищенский приворот по фото – https://оберег1000.СЂС„ приворот на мужчину самостоятельно читать.
приворот на парня чтобы влюбился на расстоянии приворот молитвой приворот на мужчину без последствия сразу действует
– приворот штоп в постели мущине было хорошо – приворот парня на любовь бесплатно.
– https://porcha-sglaz-proklyatie.ru яйцо на приворот
-эффективен ли приворот,совершённый в кругу,начерченном привороты сексуальные бесплатно.сделай сам магия сильнейший приворот отворот соперников.
-приворот с помошью кукла вольт приворот на удачу b yf ltymub.снять приворот простой способ.
-свердловская область привороты, колдовство татарские привороты
приворот на фигурках. сделала приворот у него депрессия привороты любимого на волосах.
https://astra-prognoz.ru .
приворот парня с волосами приворот сексуального магнетизма.
приворот месячными как – https://coopdobromir.ru к чему снится приворот.
приворот без последствия в домашних условиях быстро на парня. приворот на месячные на убывающую луну
сильный приворот на мужчину на тоску быстрый приворот дома
приворот на волосы в полнолуние.
https://batmanapollo.ru – ПСИХОЛОГ
недоношенный ребенок уход за – https://ladytoday.ru ->>>>>>>>> дезинфекция предметов ухода за ребенком !
This is really interesting, You’re a very skilled blogger. I’ve joined your feed and look forward to seeking more of your magnificent post. Also, I’ve shared your site in my social networks!
East Bay News is the leading source of breaking news, local news, sports, entertainment, lifestyle and opinion for Contra Costa County, Alameda County, Oakland and beyond https://eastbaynews.us/
заявление на уход ребенка самостоятельно – https://xigra.ru
Do whatever you want. Steal cars, drive tanks and helicopters, defeat gangs. It’s your city! https://play.google.com/store/apps/details?id=com.gangster.city.open.world
News from the staff of the LA Reporter, including crime and investigative coverage of the South Bay and Harbor Area in Los Angeles County. https://lareporter.us/
откат на яйцо как снять сглаз с как определить есть ли на человеке порча
ProDentim is an innovative dental health supplement that boasts of a unique blend of 3.5 billion probiotics and essential nutrients, all of which have been clinically proven to support the health of teeth and gums.
There is definately a lot to find out about this subject. I like all the points you made
играть казино– это популярная букмекерская контора, предоставляющая широкий выбор ставок на спорт и казино. Сайт обладает удобным интерфейсом, мобильной версией и приложением для удобства пользователей. 1xBet также известен разнообразными акциями и бонусами, делая игровой опыт более захватывающим.
отзывы кто делал приворот в воронеже – отзывы приворота на кровь из пальца – существуют ли привороты отзывы кто
baseballoutsider.com
Fang Jifan은 탐욕 스럽습니다. 누가이 상인들에게 속고 싶습니까?
baseballoutsider.com
폐하는 실제로 자신을 Wang Shouren과 비교하고 자신을 한탄하기까지했습니다.
This is really interesting, You’re a very skilled blogger. I’ve joined your feed and look forward to seeking more of your magnificent post. Also, I’ve shared your site in my social networks!
great content custom printed packaging
обивка дивана https://peretyazhka-mebeli-minsk.ru/.
приворот на мужчину без последствия сразу в домашних условиях на расстоянии без фото – https://institutmassaga.ru как сделать приворот на мужчину в домашних условиях.
сильный приворот по фото в домашних условиях читать на парня. приворот парня по фото на телефоне в домашних условиях читать без свечей
как снять приворот на расстоянии как долго действует приворот
приворот на икону последствия.
приворот чтобы парень влюбился читать в домашних условиях белый приворот утром в домашних условиях – ошо астрология снять приворот с парня
астрология воронеж астрология болезни.
фигуры астрология. астрология услуги
астродокс астрология.
приворот на женщину овна. привороты с крысой черное венчаниесамый сильный из существующих приворотов.
https://magicblack.biz .
приворот на супруга приворот своего вещего сна.
The latest film and TV news, movie trailers, exclusive interviews, reviews, as well as informed opinions on everything Hollywood has to offer. https://xoop.us/
https://bit.ly/sistemniy-podkhod
белый приворот на парня без последствия в домашних условиях приворот по фото без свечей в домашних условиях читать.
как узнать подействовал ли приворот на мужчину . приворот на любимого человека по фото в домашних условиях читать , как сделать приворот на фото.
как сделать приворот на жену в домашних условиях без последствия по фото – https://magi-pravda.ru приворот парня на бумаге.
если любовница сделала приворот на мужа последствия приворот парня на луну приворот на еде
Food
Stri is the leading entrepreneurs and innovation magazine devoted to shed light on the booming stri ecosystem worldwide. https://stri.us/
The one-stop destination for vacation guides, travel tips, and planning advice – all from local experts and tourism specialists. https://travelerblog.us/
– приворот на любовь по фото самостоятельный и действенный – приворот по всем трем чакрам узел рабства.
– https://shyan.ru чем опасен белый приворот
-приворот на смерть, привороты заговоры привороты на звезд.приворотное зелье 2 читать.
-приворот на горькую рюмку самый хороший приворот.что будет с человеком сделавшим приворот.
-привороты самые сильные на фото приворот чтобы ни дня без меня не мог
https://bit.ly/sistemniy-podkhod
Money Analysis is the destination for balancing life and budget – from money management tips, to cost-cutting deals, tax advice, and much more. https://moneyanalysis.us/
Outdoor Blog will help you live your best life outside – from wildlife guides, to safety information, gardening tips, and more. https://outdoorblog.us/
https://bit.ly/sistemniy-podkhod
Предлагаем купить диплом Вуза по низкой цене, с доставкой и скидками от изготовителя.
https://bit.ly/sistemniy-podkhod
перетянуть диван https://peretyazhka-mebeli-minsk.ru/.
https://bit.ly/sistemniy-podkhod
как узнать если на человеке приворот в домашних условиях приворот на девушку по фото в телефоне в домашних условиях читать.
сильный приворот на мужа который нельзя снять заговор на приворот на расстоянии читать.
навести приворот – https://sudbainfo.ru приворот на волосах в домашних условиях.
приворот на девушку в домашних условиях как сделать приворот самостоятельно как узнать есть ли на мне приворот на любовь
приворот на женщину без последствия цена – https://liyamagiya.ru как делать приворот на парня читать.
приворот на мужчину на бумаге. приворот на обручальное кольцо мужа
псалмы от приворота приворот что
молитва от приворота мужчины.
Maryland Post: Your source for Maryland breaking news, sports, business, entertainment, weather and traffic https://marylandpost.us/
this-is-a-small-world.com
이 테스트에서는 상위 3개가 이 목록에 나타납니다.
The latest health news, wellness advice, and exclusives backed by trusted medical authorities. https://healthmap.us/
Baltimore Post: Your source for Baltimore breaking news, sports, business, entertainment, weather and traffic https://baltimorepost.us/
Обратившись к нашей компании, вы обеспечите себе доступ к высококачественных юридических услуг от квалифицированных юристов. Подробнее читайте в статье по ссылке
минимальная сумма алиментов на двух детей.
сильный приворотный заговор самостоятельно на парня на крови https://www.magecam.ru форумы практическая магия привороты
LeanBiome is an innovative and effective supplement that has been specifically formulated to support healthy weight loss. The product is the result of the latest Ivy League research and is backed by real-world results.
The LB News is the local news source for Long Beach and the surrounding area providing breaking news, sports, business, entertainment, things to do, opinion, photos, videos and more https://lbnews.us/
Обратившись к нашей компании, вы гарантируете себе доступ к профессиональных юридических консультаций от квалифицированных юристов. Подробнее читайте в статье по ссылке
стаж по списку 2.
ПСИХОЛОГ
ПСИХОЛОГ
Greetings, Earth!
I am a Capybara, a small creature cherished for its endearing appearance and charming qualities!
Curious about my recent endeavors? I’ve decided to swap the jungle for the bustling city life.
Currently residing in the Netherlands, I’ve found a companion in the virtual realm!
Meet Xrumer, a software product, and its invaluable sidekick, Xevil. Together, we collaborate on ambitious projects that extend promotional messages to everyone in our database.
Our impact spans the globe, disseminating information about new projects, materials, and the lives of capybaras, both in the wild and in zoos – a truly significant endeavor!
Leveraging Xrumer for posting allows us to reach a vast audience, creating a robust link profile. We specialize in constructing site networks, establishing link levels, and enhancing domains for cohesion – a testament to the camaraderie of the capybara herd + Xrumer + Xevil!
If you’ve received a message from our team, why not consider availing our posting services? We’re open for business, friends, and eagerly await your tasks!
The Capybara herd tirelessly works around the clock to fulfill advertising tasks for leading SEO companies. We’re grateful for the opportunity, whether it’s to buy food or secure funds for our lives.
Curious about how people find us online? Here’s a glimpse of what we do:
https://capybara333.wordpress.com/
Xrumer mailing
Xrumer run
Xrumer posting
Xrumer website promotion
Xrumer site run
PBN site network boosting
Xrumer profile run, and much more!
And now, the English version!
Привет, мир!
Я Капибара, небольшое существо, которое полюбили за свою внешность и характерные черты!
Хотите узнать, чем я занимаюсь последнее время? Решил переместиться из джунглей в большой город.
В настоящее время я живу в Нидерландах и подружился с хорошим виртуальным спутником!
Его зовут программный продукт Xrumer, а его незаменимый компаньон — Xevil. Мы работаем вместе, создавая грандиозные проекты, позволяя каждому в нашей базе получать рекламные сообщения.
Информация распространяется по всему миру; люди узнают о новых проектах, материалах, жизни капибар в суровой дикой природе и зоопарках – это действительно важно!
Постинг с использованием Xrumer позволяет охватить огромную аудиторию и создать мощный ссылочный профиль. Мы строим сети сайтов, уровни ссылок, улучшаем домены для их склейки – всё это часть дружбы стада Капибар + Xrumer + Xevil!
Вы получили сообщение от нашей команды, и что мешает вам заказать постинг и наши услуги? Мы открыты для сотрудничества, друзья, и ждем ваших задач!
Стадо Капибар работает круглосуточно на благо рекламных задач ведущих SEO-компаний и очень благодарно за возможность купить еду или получить средства на жизнь.
Как нас ищут в сети, или, скорее, что мы делаем:
рассылка Хрумером
прогон Хрумером
постинг Хрумером
раскрутка сайта Хрумером
прогон сайта Хрумером
прокачка PNB сеток сайтов
прогон по профилям Хрумером и многое другое!
Удачи!!!
Trenton News – Trenton, NJ News, Sports, Weather and Things to Do https://trentonnews.us/
this-is-a-small-world.com
폐하, 그의 말도 안되는 젊은 주인을 비난하지 마십시오.
Healthcare Blog provides news, trends, jobs and resources for health industry professionals. We cover topics like healthcare IT, hospital administration, polcy
Vacavillenews.us covers local news in Vacaville, California. Keep up with all business, local sports, outdoors, local columnists and more. https://vacavillenews.us/
Ohio Reporter – Ohio News, Sports, Weather and Things to Do https://ohioreporter.us/
Fashion More provides in-depth journalism and insight into the news and trends impacting the fashion
नमस्कार!
क्या आपने कभी एक्स-जीपीटी राइटर के बारे में सुना है: चैटजीपीटी तंत्रिका नेटवर्क पर आधारित एक अद्वितीय कीवर्ड सामग्री जनरेटर?
मैंने यह भी नहीं किया है, जब तक मुझे इस सॉफ़्टवेयर के साथ नियमित कार्यों को स्वचालित करने की सलाह नहीं दी गई थी, मैं एक बात कहना चाहता हूं! मैं तब विश्वास नहीं कर सका
लंबे समय तक कि चैटजीपीटी इतना शक्तिशाली उत्पाद है यदि इसका उपयोग एक्स-जीपीटी लेखक के नियंत्रण में स्ट्रीमिंग में एक साथ किया जाता है ।
मुझे लगा कि यह सिर्फ एक उपयोगिता है, यह सस्ती थी, एक दोस्त ने 40% छूट के लिए एक कूपन दिया%:
94EB516BCF484B27
इसे कहां दर्ज करना है, इसका विवरण वेबसाइट पर दर्शाया गया है:
https://www.xtranslator.ru/x-gpt-writer/
मैंने कोशिश करना शुरू कर दिया, इसमें तल्लीन किया, कम कीमतों पर 50 चैटजीपीटी खाते खरीदे और यह शुरू हो गया!
अब मैं आसानी से एक सप्ताह में 3-4 नई साइटें उत्पन्न करता हूं और लॉन्च करता हूं, बैच पूरे फ़ोल्डरों को एकजुट करता है और यहां तक कि छवियां भी बनाता हूं
चैटजीपीटी तंत्रिका नेटवर्क और एक्स-जीपीटी लेखक का उपयोग करना ।
यह एक कोशिश के लायक है, दोस्तों, एक डेमो है, सब कुछ मुफ़्त है, आपको इसका पछतावा नहीं होगा)
गुड लक!
Синонимизация текста с X-GPTWriter и ChatGPT
Уникальные тексты с ChatGPT и X-GPTWriter
Покупка X-GPTWriter: лучшие предложения и скидки
ChatGPT как инструмент для генерации контента
ChatGPT и X-GPTWriter для уникальных текстов
X-GPTWriter купоны на скидку
Автоматизированное создание текстов с помощью ChatGPT
X-GPTWriter: мощный инструмент для контент-креации
X-GPTWriter: лучший софт для создания текстов
Как ChatGPT помогает в создании уникального текста
PharmaMore provides a forum for industry leaders to hear the most important voices and ideas in the industry. https://pharmamore.us/
Привет Всем!
Хотел сказать что постинг Хрумером реально работает, применяется
и имеет место быть, если рассматривать экономическую составляющую,
это в сотни раз выгоднее покупки ссылок, постов и др,
так же прогон Хрумером идет реальным образом,
Вас не размещают на каких-то самоподнятых сетках что будут забанены или закрыты,
совершенно разные сайты, домены, IP и локации, все как нужно!
Наша компания делала здесь:
https://progonxrumerom.wordpress.com/
Xrumer рассылка это отличный инструмент для SEO, дорвейщиков лого уровня, СМИ,
веб мастеров и тех кто имеет цель донести до других свою информацию.
Удачного развиия)
рассылка Хрумером
прогон Хрумером
постинг Хрумером
раскрутка сайта Хрумером
прогон сайта Хрумером
прокачка PNB сеток сайтов
прогон по профилям Хрумером и многое другое!
Перетяжка мягкой мебели для начинающих: с чего начать?
ремонт мягкой мебели в минске https://peretyazhka-mebeli-vminske.ru/ .
Medical More provides medical technology news and analysis for industry professionals. We cover medical devices, diagnostics, digital health, FDA regulation and compliance, imaging, and more. https://medicalmore.us
приворот черное венчание – Обратится к магу – https://dzen.ru/id/653538d7d6100f7a6fee8469
черная магия приворот с кровью
नमस्कार!
मैं दीना हूं, मैं 35 साल का हूं, सुंदर और प्यारी हूं, मैं आपको अपनी खोज के बारे में बताना चाहती हूं)
मैं कई चीजों के बारे में नकारात्मक दृष्टिकोण रखता था, अक्सर पर्यावरण, लोगों, राजनीति के बारे में चिंतित होता था, और इसका मेरे स्वास्थ्य और सामान्य रूप से जीवन की गुणवत्ता पर बुरा प्रभाव पड़ने लगा ।
मनोवैज्ञानिक ने मुझे और हंसने की सलाह दी, और अध्ययन न करने के लिए कि मैं क्या नहीं बदल सकता, क्या बात है!
मैंने नियमित रूप से हास्य के साथ चुटकुले और साइटों को पढ़ना शुरू किया, और 2 महीने के बाद मैं एक अलग व्यक्ति बन गया, शांत और दयालु, चीजें पहाड़ों पर चली गईं और लोग मेरी कंपनी में अधिक रहना चाहते हैं, पुरुषों का कोई अंत नहीं है ।
मैं उन सभी को सलाह देता हूं जो चुटकुले पसंद करते हैं, यह साइट
https://www.anekdotor.ru/anekdoty-pro-vypusknikov/
सब कुछ सरल है और मामले के बारे में, पढ़ें, हंसें और स्वस्थ रहें!
गुड लक दोस्तों)
सभी को नमस्कार!
मैं माशा हूं, मैं 32 साल का हूं, मैं इंग्लैंड में रहता हूं, मैं 2 बच्चों को लाता हूं जो स्कूल जाते हैं)
स्कूल बच्चों और माता-पिता दोनों के लिए काफी तनाव है, और विशेष विषयों में परीक्षणों के लिए निरंतर पाठ और तैयारी ने मुझे पागल कर दिया (
मैं घबरा गई, अपने पति के साथ सोना बंद कर दिया और एक नर्वस टिक शुरू हो गया, यह भयानक था…
यह अच्छा है कि मेरे दोस्तों ने मुझे समाधान वाली साइटें खोजने की सलाह दी, और उनकी कार्यप्रणाली के अनुसार होमवर्क करने की कोशिश की ।
वैसे, एक अच्छी वेबसाइट
https://www.controlworks.ru/kontrolnaja-rabota-metally/
परीक्षण पत्रों के बारे में कोई विज्ञापन, सुविधाजनक खोज और बहुत सारी बहुमूल्य जानकारी नहीं है!
सच कहूं तो, मैं शांति से सोने लगा, परिवार में सेक्स और शांति बहाल हुई, ऐसी साइटों के लिए धन्यवाद जहां आप समाधान पा सकते हैं और अपनी पसंदीदा चीजों के लिए अधिक समय समर्पित कर सकते हैं!
गुड लक!
Простой гайд для новичков в обновлении мебели
обивка мебели в минске https://peretyazhka-mebeli-vminske.ru/ .
San Gabriel Valley News is the local news source for Los Angeles County
Local news from Redlands, CA, California news, sports, things to do, and business in the Inland Empire. https://redlandsnews.us
सभी को नमस्कार!
मैं एक वास्तविक अनुभव साझा करना चाहता हूं, उम्र के साथ मेरी सेक्स शक्ति कम होने लगी, और अंततः एक अपमानजनक स्तर पर आ गई (
यहां तक कि सबसे सुंदर और युवा लड़कियों ने मुझमें ऊर्जा के सही स्तर को उत्तेजित नहीं किया…
यह भयानक था और अवसाद तब शुरू हुआ जब एक दोस्त ने मुझे बताया कि आपको हर दिन चुटकुले पढ़ने और हंसने की जरूरत है, और सब कुछ धीरे-धीरे बेहतर हो जाएगा ।
मुझे इस साइट की सिफारिश की
https://www.kompotanekdot.ru/anekdot-pro-gvozdi-i-mamu-chitat-i-skachat-onlajn/
मैंने सोचा कि क्या बकवास है, लेकिन कुछ नहीं करना था, और मैं व्यवस्थित रूप से हंसने लगा और हास्य के बारे में सब कुछ पढ़ने लगा!
मुझे विश्वास नहीं हुआ, लेकिन 2 सप्ताह के बाद, मेरी शक्ति सामान्य हो गई, और मैं प्रेम स्थानों पर लौटने और मॉडल के साथ चलने में सक्षम था!
हंसी और चुटकुले के लिए धन्यवाद,और स्वस्थ रहें)
मैं पहले से ही 87 साल का हूं, लेकिन मैं अभी भी बिस्तर में मजबूत हूं)
NewsBreak provides latest and breaking Renton, WA local news, weather forecast, crime and safety reports, traffic updates, event notices, sports https://rentonnews.us
Bellevue Latest Headlines: City of Bellevue can Apply for Digital Equity Grant https://bellevuenews.us
Избавьтесь от старой мебели: перетяжка как способ обновления интерьера
перетяжка мебели недорого https://peretyazhka-mebeli-vminske.ru/ .
baseballoutsider.com
그 직후 그들은 명나라의 가장 고귀한 대우를 받고 차를 타고 떠났습니다.
homefronttoheartland.com
아니나 다를까…귀신이 시간을 돌릴 수 있는 것은 명예와 재산입니다.
I’m curious, how secure are deposits through the Mpesa for online transactions?
Play these games and win real money in Kenya
online casino games that pay real money games that pay real money in kenya .
Can someone explain the fees for deposits through the Mpesa? Seems higher lately.
agonaga.com
이 엉뚱한 사람은 여기에서 정말 눈에 거슬립니다.
नमस्कार!
क्या आपने कभी एक्स-जीपीटी राइटर के बारे में सुना है: चैटजीपीटी तंत्रिका नेटवर्क पर आधारित एक अद्वितीय कीवर्ड सामग्री जनरेटर?
मैंने यह भी नहीं किया है, जब तक मुझे इस सॉफ़्टवेयर के साथ नियमित कार्यों को स्वचालित करने की सलाह नहीं दी गई थी, मैं एक बात कहना चाहता हूं! बहुत दिनों बाद मुझे विश्वास नहीं हुआ
वह चैटजीपीटी इतना शक्तिशाली उत्पाद था यदि इसे एक्स-जीपीटी राइटर चलाने, स्ट्रीमिंग में एक साथ उपयोग किया जाता था ।
मुझे लगा कि यह सिर्फ एक उपयोगिता है, यह सस्ती थी, एक दोस्त ने मुझे 40% छूट के लिए एक कूपन दिया%:
94EB516BCF484B27
इसे कहां दर्ज करना है इसका विवरण वेबसाइट पर दर्शाया गया है:
https://www.xtranslator.ru/x-gpt-writer/
मैंने कोशिश करना शुरू कर दिया, इसमें तल्लीन किया, कम कीमतों पर 50 चैटजीपीटी खाते खरीदे और मैं चला गया!
अब मैं आसानी से प्रति सप्ताह 3-4 नई साइटें उत्पन्न करता हूं और लॉन्च करता हूं, बैच पूरे फ़ोल्डरों को एकजुट करता है और यहां तक कि छवियां भी बनाता हूं
चैटजीपीटी तंत्रिका नेटवर्क और एक्स-जीपीटी लेखक का उपयोग करना ।
यह एक कोशिश के लायक है, दोस्तों, एक डेमो है, सब कुछ मुफ़्त है, आपको इसका पछतावा नहीं होगा)
गुड लक!
ChatGPT и X-GPTWriter: новая эра контент-маркетинга
X-GPTWriter купить со скидкой
Уникальный контент с синонимизатором на базе ChatGPT
Программа для автоматического создания текстов с использованием ChatGPT
X-GPTWriter: лучший софт для создания текстов
Синонимайзер текста на основе ChatGPT
X-GPTWriter: мощный инструмент для контент-креации
ChatGPT и создание качественного контента
Создание уникальных статей с ChatGPT
ChatGPT как генератор уникального контента
सभी को नमस्कार!
क्या आपने कभी एक्स-जीपीटी राइटर के बारे में सुना है: चैटजीपीटी तंत्रिका नेटवर्क पर आधारित एक अद्वितीय कीवर्ड सामग्री जनरेटर?
मैंने यह भी नहीं किया है, जब तक मुझे इस सॉफ़्टवेयर के साथ नियमित कार्यों को स्वचालित करने की सलाह नहीं दी गई थी, मैं एक बात कहना चाहता हूं! बहुत दिनों बाद मुझे विश्वास नहीं हुआ
वह चैटजीपीटी इतना शक्तिशाली उत्पाद था यदि इसे एक्स-जीपीटी राइटर चलाने, स्ट्रीमिंग में एक साथ उपयोग किया जाता था ।
मुझे लगा कि यह सिर्फ एक उपयोगिता है, यह सस्ती थी, एक दोस्त ने मुझे 40% छूट के लिए एक कूपन दिया%:
94EB516BCF484B27
इसे कहां दर्ज करना है इसका विवरण वेबसाइट पर दर्शाया गया है:
https://www.xtranslator.ru/x-gpt-writer/
मैंने कोशिश करना शुरू कर दिया, इसमें तल्लीन किया, कम कीमतों पर 50 चैटजीपीटी खाते खरीदे और मैं चला गया!
अब मैं आसानी से प्रति सप्ताह 3-4 नई साइटें उत्पन्न करता हूं और लॉन्च करता हूं, बैच पूरे फ़ोल्डरों को एकजुट करता है और यहां तक कि छवियां भी बनाता हूं
चैटजीपीटी तंत्रिका नेटवर्क और एक्स-जीपीटी लेखक का उपयोग करना ।
यह एक कोशिश के लायक है, दोस्तों, एक डेमो है, सब कुछ मुफ़्त है, आपको इसका पछतावा नहीं होगा)
गुड लक!
ChatGPT и X-GPTWriter: новая эра контент-маркетинга
Генерация текстовых материалов с X-GPTWriter
Как сделать текст более уникальным с ChatGPT
Создание контента с помощью X-GPTWriter
X-GPTWriter: лучший софт для создания текстов
Покупка X-GPTWriter: лучшие предложения и скидки
Где найти промо коды на X-GPTWriter
уникализатор текста через ChatGPT
Как ChatGPT помогает в создании уникального текста
ChatGPT и X-GPTWriter: инструменты для улучшения уникальности текста
netovideo.com
분석하지 않아도 괜찮은데 분석하고 나니 갑자기 홍지 황제의 얼굴이 변했다.
Read More About Mpesa Casinos In Kenya
Доброго!
Были ли у вас случаи, когда вам приходилось писать дипломную работу в сжатые сроки? Это действительно трудно и ответственно, но важно не сдаваться и продолжать работать над учебными процессами, чем я и занимаюсь.
Для тех, кто умеет грамотно пользоваться интернетом и находить нужную информацию, это действительно оказывается полезным. Это помогает в процессе согласования и написания дипломной работы, и нет необходимости тратить время на посещение библиотек или встречи с дипломным руководителем. Если вам нужны хорошие источники для подготовки дипломных и курсовых работ, я могу поделиться полезными ссылками.
http://vuzdiploma.ru/
Желаю всем отличных оценок!
купить диплом в мытищах
купить диплом в красноярске
купить диплом в киселевске
купить диплом в балашове
купить диплом в самаре
купить диплом в кемерово
купить диплом в ишимбае
купить диплом в петропавловске-камчатском
купить диплом в нижним тагиле
купить диплом в череповце
фичино философия https://mir-ved.ru супрематизм философия
энтропия философия https://mir-ved.ru культура философия
Привет всем!
Стоит отметить, что статьи про строительство это очень интересно и увлекательно, узнаешь что-то новое и полезное!
Этот ресурс включает много статей на разные темы, рекомендую
http://amarish.ru/preimushhestva-ispolzovaniya-gazobetona/
Удачного чтения!
Заработай права управлять автомобилем в первоклассной автошколе!
Стремись к профессиональной карьере вождения с нашей автошколой!
Пройди обучение в самой автошколе города!
Учись правильного вождения с нашей автошколой!
Стремись к безупречным навыкам вождения с нашей автошколой!
Начни уверенно водить автомобиль с нами в автошколе!
Стремись к независимости и лицензии, получив права в автошколе!
Прояви мастерство вождения в нашей автошколе!
Открой новые возможности, получив права в автошколе!
Приведи друзей и они получат скидку на обучение в автошколе!
Стань профессиональному будущему в автомобильном мире с нашей автошколой!
новые друзья и научись водить автомобиль вместе с нашей автошколой!
Развивай свои навыки вождения вместе с опытными инструкторами нашей автошколы!
Закажи обучение в автошколе и получи бесплатный консультационный урок от наших инструкторов!
Стремись к надежности и безопасности на дороге вместе с нашей автошколой!
Прокачай свои навыки вождения вместе с лучшими в нашей автошколе!
Учись дорожные правила и навыки вождения в нашей автошколе!
Стремись к настоящим мастером вождения с нашей автошколой!
Набери опыт вождения и получи права в нашей автошколе!
Пробей дорогу вместе с нами – закажи обучение в автошколе!
автошкола васильківська https://avtoshkolaznit.kiev.ua/ .
Привет всем!
Стоит отметить, что статьи про строительство это очень интересно и увлекательно, узнаешь что-то новое и полезное!
Этот ресурс включает много статей на разные темы, рекомендую
https://forexaccess.ru/novosti/699-chto-takoe-gazobeton-i-kakovy-ego-preimushchestva.html
Удачного чтения!
сериал на русском языке
The latest news and reviews in the world of tech, automotive, gaming, science, and entertainment. https://millionbyte.us/
Jiang Chen과 Liu Wenshan은 감정의 동요 없이 고개를 숙였습니다.
Містерія пін ап
пін ап відгуки https://pinupcasinoqgcvbisd.kiev.ua/ .
Лучшие способы использования ремонтной смеси
цена кладки кирпича http://www.remontnaja-smes-dlja-kirpichnoj-kladki.ru/ .
Как правильно укладывать рулонный газон?
рулонный газон стоимость https://rulonnyj-gazon77.ru/ .
Здравствуйте!
Были ли у вас случаи, когда приходилось писать дипломную работу в сжатые сроки? Это действительно требует много ответственности и усилий, но важно не отступать и продолжать учебный процесс, так же, как я это делаю.
Для тех, кто умеет осуществлять анализ и искать информацию в интернете, это может быть действительно полезным при согласовании и написании диплома. Нет необходимости тратить время на посещение библиотек или встречи с научным руководителем. Здесь можно найти много полезных данных для дипломных и курсовых работ, просто перейдя по ссылкам
https://extern-diplom.com/
Желаю всем отличных оценок!
купить диплом в липецке
купить диплом учителя физической культуры
купить диплом программиста
купить диплом в иваново
купить диплом в кирове
купить диплом в череповце
купить диплом в йошкар-оле
купить диплом в саранске
купить диплом в бийске
купить диплом в брянске
Перетяжка мягкой мебели в Минске: качественно и недорого
перетяжка мебели в минске https://peretyazhka-mebeli-vminske.ru/ .
Привет всем!
Было ли у вас когда-либо так, что вы писали дипломную работу в кратчайшие сроки? Это действительно требует большой ответственности и усилий, но важно не сдаваться и продолжать активно участвовать в учебных процессах, как и я.
Для тех, кто умеет находить нужную информацию и анализировать ее в Интернете, это действительно может быть полезным в процессе согласования и написания дипломной работы. Нет необходимости тратить время на походы в библиотеки или встречи с научным руководителем. Здесь доступны хорошие данные для дипломных работ и курсовых проектов; вы можете ознакомиться с ними, перейдя по ссылкам
https://extern-diplom.com/
Желаю всем отличных оценок!
купить диплом в липецке
купить диплом нового образца
купить диплом прораба
купить диплом оценщика
купить диплом в архангельске
купить диплом в назрани
купить диплом в ачинске
купить свидетельство о разводе
купить диплом врача
купить диплом в новоалтайске
Доброго!
Бывало ли у вас такое, что приходилось писать дипломную работу в сжатые сроки? Это действительно очень ответственно и трудно, но важно не сдаваться и продолжать учебный процесс, так же, как и я.
Для тех, кто умеет осваивать информацию и искать её в интернете, это действительно может оказать большую помощь в процессе согласования и написания дипломной работы. Нет необходимости тратить время на походы в библиотеки или встречи с научным руководителем. Здесь представлены хорошие материалы для дипломных и курсовых работ, которые вы можете изучить, перейдя по ссылкам
https://diplom1.org/
Желаю всем отличных оценок!
купить диплом энергетика
купить аттестат за 9 класс
купить диплом в ейске
купить диплом в симферополе
купить диплом в йошкар-оле
купить диплом в находке
купить диплом в губкине
купить диплом в барнауле
купить диплом в набережных челнах
купить диплом в каменске-уральском
tsrrub.com
Wen Yansheng은 사방에 시체가 있는 것을 보고 흥분하여 달려갔고 눈이 빨개졌습니다.
Мой опыт обращения к магу с приворотом в Германии – кто знает хорошую бабушку в германии отзывы
Живу я в небольшом городе в Германии, и найти среди кучи «магов» хорошего, трудно особенно в Германии. Намучилась я с этим очень. И как бывает, все решается на пьяную голову. Сидели с двоюродной сестрой, поведала ей свою проблему с мужем и о бесконечных поисках магов. Она очень удивилась, что я сразу не стала искать человека в России с Якутии или другого региона Дальнего востока – это можно сказать родина многих сильных шаманов и колдунов.
Порекомендовала мага, с которым сама работала. Поработала с ним и я.
Поэтому хотела бы написать отзыв о привороте на мужа, проведенном магом Романом Петровичем.
___________________________________________________________________________
Я хочу поделиться своим опытом использования услуг мага Романа Петровича с сайта https://cmag666.ru Ватсап 8 (984) 286-12-65
___________________________________________________________________________
Перед тем, как обратиться к нему, моя ситуация с мужем казалась мне безвыходной. Наш брак испытывал серьезные трудности, и наши отношения становились все более напряженными.
Мой муж, с которым мы прожили много лет, казался мне все более отстраненным и равнодушным. Он уходил в себя, избегал общения, а наши разговоры становились все реже и поверхностнее. Я испытывала огромную боль от того, что наша семья распадается, и что я теряю своего мужа. В итоге он еще и любовницу завел.
После долгих раздумий и поиска решения проблемы, я решила обратиться к магу Роману Петровичу за помощью.
Он провел для меня приворот на мужа – на все ушло 5 дней, и еще дал ряд простых рекомендаций, которым нужно было следовать до получения результата. Последовали дни ожидания
На 5 день после проведения приворота я почувствовала изменения в поведении мужа. Он стал проявлять больше внимания и заботы, мы снова начали общаться и находить общие интересы. Стали возвращаться чувства и заинтересованность мной как женщиной. Все быстро нормлизовалось в наших отношениях, с любовницей он порвал все контакты.
Сейчас, спустя несколько месяцев после проведения приворота, я вижу, что наш брак стал крепким, стабильным и счастливым, как и раньше! Мы с мужем снова чувствуем себя близкими и любящими людьми.
Я благодарна магу Роману Петровичу за его помощь и поддержку в трудный момент!
Теги маг в германии отзывы – экстрасенсы в германии отзывы
ясновидящие в германии отзывы – приворот в германии отзывы
кто знает хорошую бабушку в германии отзывы – экстрасенсы в германии отзывы
Привет всем!
Бывало ли у вас ситуации, когда приходилось писать дипломную работу в крайне сжатые сроки? Это действительно требует огромной ответственности и напряженной работы, но важно не сдаваться и продолжать активно участвовать в учебном процессе, что я и делаю в данный момент.
Для тех, кто умеет ориентироваться и искать информацию в сети, это действительно может оказаться весьма полезным при согласовании и написании дипломной работы. Нет необходимости тратить время на посещение библиотек или проведение встреч с дипломным руководителем. Здесь представлены отличные материалы для дипломных и курсовых работ, на которые вы можете взглянуть, перейдя по ссылкам
https://diplom1.org/
Желаю всем отличных оценок!
купить диплом в батайске
куплю диплом о высшем образовании
купить диплом в архангельске
купить диплом в каменске-шахтинском
старые дипломы купить
купить диплом в усть-илимске
купить диплом бакалавра
купить диплом косметолога
купить диплом в хабаровске
купить диплом в рубцовске
Мой опыт обращения к магу с приворотом в Германии – гадание в германии отзывы
Живу я в небольшом городе в Германии, и найти среди кучи «магов» хорошего, трудно особенно в Германии. Намучилась я с этим очень. И как бывает, все решается на пьяную голову. Сидели с двоюродной сестрой, поведала ей свою проблему с мужем и о бесконечных поисках магов. Она очень удивилась, что я сразу не стала искать человека в России с Якутии или другого региона Дальнего востока – это можно сказать родина многих сильных шаманов и колдунов.
Порекомендовала мага, с которым сама работала. Поработала с ним и я.
Поэтому хотела бы написать отзыв о привороте на мужа, проведенном магом Романом Петровичем.
___________________________________________________________________________
Я хочу поделиться своим опытом использования услуг мага Романа Петровича с сайта https://cmag666.ru Ватсап 8 (984) 286-12-65
___________________________________________________________________________
Перед тем, как обратиться к нему, моя ситуация с мужем казалась мне безвыходной. Наш брак испытывал серьезные трудности, и наши отношения становились все более напряженными.
Мой муж, с которым мы прожили много лет, казался мне все более отстраненным и равнодушным. Он уходил в себя, избегал общения, а наши разговоры становились все реже и поверхностнее. Я испытывала огромную боль от того, что наша семья распадается, и что я теряю своего мужа. В итоге он еще и любовницу завел.
После долгих раздумий и поиска решения проблемы, я решила обратиться к магу Роману Петровичу за помощью.
Он провел для меня приворот на мужа – на все ушло 5 дней, и еще дал ряд простых рекомендаций, которым нужно было следовать до получения результата. Последовали дни ожидания
На 5 день после проведения приворота я почувствовала изменения в поведении мужа. Он стал проявлять больше внимания и заботы, мы снова начали общаться и находить общие интересы. Стали возвращаться чувства и заинтересованность мной как женщиной. Все быстро нормлизовалось в наших отношениях, с любовницей он порвал все контакты.
Сейчас, спустя несколько месяцев после проведения приворота, я вижу, что наш брак стал крепким, стабильным и счастливым, как и раньше! Мы с мужем снова чувствуем себя близкими и любящими людьми.
Я благодарна магу Роману Петровичу (Ватсап 8(984)286-12-65)за его помощь и поддержку в трудный момент!
Теги ясновидящие в германии отзывы – экстрасенсы в германии отзывы
гадание в германии отзывы – приворот в германии отзывы 8(984)286-12-65
гадалка в германии отзывы – гадание в германии отзывы
Отзыв о привороте, и о маге сделавшем приворот.
+
+
Были проблемы с мужем довольно давно. А в последний год отношения стали сыпаться очень быстро, все разурушилось до конца буквально на глазах. Особенно с появлением любовницы, это была коллега сработы. А у нас двое детей. Их я и сама могла обеспечить более чем! Но вот любила мужа, и хоте, чтобы дети росли с рожным отцом.
Обращалась много к кому, но доверия не было даже при первом общение. Случайно встретились с давней подругой. Разговорились о проблемах. Она посоветовал сильного мага с Дальнего Востока.
Обратилась к нему за приворотом, хотя были конечно сомнения. Звать его Роман Петрович. Берет за работу не сильно много по сравнению с другими, делает все быстро и в срок, не продает и всегда отвечает на возникающие вопросы. Вернул мужа мне за 7 дней, работу проводил 2 дня.
Очень довольна!
________________________
Обратиться к нему можно через сайт https://cmag666.ru или ватсап 8 (984) 286-12-65 – это настоящий маг и просто добрый человек, отлично знающий свое дело!
____________________________________________________________________________________
Сайт ищут по тегам #
# Ясновидящая # маге # отзывы # экстрасенс # гадалка
анжела манвелян магия
курс натальи малиновской отзывы
роман симоненко
школа белого лотоса анная официальный сайт
виктория железнова видео
ангелия таро новое
нина суворова
светлана кулешова экстрасенс официальный сайт данные
наталья бруно ведьма отзывы
баба нина слепая отзывы
союз магов россии официальный сайт список настоящих магов
маг юрий
бабушка людмила
гадалка зеленоград 3 район
маг и экстрасенс
признаки мага
сайт настоящих магов россии официальный
Спасибо, Роману Петровичу, за его профессионализм и помощь! Хороший человек!Здравствуйте!Хочу написать отзыв о кладбищенской привороте, заказанном у мага Романа Петровича с сайта https://cmag666.ru. Мой друг обратился к нему, когда его брак столкнулся с серьезными проблемами и начал трещать по швам – жена нашла любовника, и ушла в итоге с детьми к нему. Роман Петрович предложил кладбищенский приворот и остуду от любовника – то есть была проведенна комплексная работа.Уже через 5 дней ее отношения с тем гадом стали ухудшаться, а на 12 день она вернулась домой. Отношения быстро начали восстанавливаться и она снова стала любящей женой! Он ее простил и все быстро забылось!
-отзывы кто делал кладбищенский приворот форум
-отзывы о действии кладбищенского приворота
-кладбищенские привороты отзывы
-кладбищенский приворот на девушку отзывы кто делал
-что такое кладбищенский приворот отзывы
Отзывы о приворотах в Екатеринбурге
—————————————–
Поиски настоящего мага привели меня на сайт Романа Петровича, и я решила попробовать снова. Будучи из Дальнего Востока, родины шаманов, Роман Петрович вызвал мое доверие, и я обратилась к нему за помощью в восстановлении чувств моего мужа.Работа Романа Петровича действительно поразила меня. Его профессионализм и внимание к моей ситуации впечатлили меня. Благодаря его помощи я снова чувствую себя счастливой и уверенной в нашем будущем вместе. Он настоящий мастер своего дела, и я безмерно благодарна ему за все, что он сделал для нашей семьи.С каждым днем я замечала, как наши отношения становились все более гармоничными и близкими. Муж начал проявлять больше внимания и заботы, а его чувства к мне стали стойчивыми и глубокими. Благодаря кладбищенскому привороту, наш брак стал еще крепче и устойчивее.Хочу поделиться своим незабываемым опытом работы с магом Романом Петровичем с сайта https://cmag666.ru. Проживая в Екатеринбурге, я столкнулась с трудностями в отношениях со своим мужем. Попытки решить проблемы с мужем при помощи местных магов не привели к желаемому результату.Я рекомендую Романа Петровича всем, кто столкнулся с проблемами в своих отношениях. Его помощь – это настоящее чудо, которое может изменить вашу жизнь к лучшему. Спасибо, Роман Петрович, за ваше волшебство и преданность своему делу!С Романом Петровичем мы обсудили мою ситуацию, и он предложил мне кладбищенский приворот для возврата чувств моего мужа. Я решила довериться его опыту и приступила к ритуалу с надеждой на лучшее.
– приворот екатеринбург отзывы
– кто делает приворот в екатеринбурге
– делала приворот в екатеринбурге
– приворот екатеринбурга отзывы
– приворот кто делает в екатеринбурге
“Melin Ajans, İstanbul fuarlarının yıldızı! Harika bir fuar modeli ve hostesi ekibi ile her zaman öne çıkıyorlar.”
Приветствую всех! Хочу поделиться своими впечатлениями о работе с магом Романом Петровичем с сайта https://cmag666.ru. Моя сестра обратилась к нему, когда столкнулась с серьезными проблемами в семейных отношениях. Роман Петрович выслушал ее проблемы и предложил кладбищенский приворот. Результат не заставил себя ждать: через 8 дней мужчина стал проявлять инициативу, и семейные отношения значительно улучшились. Кроме основной работы, маг делал ряд дополнительных действий, чтобы не было никакх последствий. Прошло уже больше двух лет с того момента, все уних хорошо и ребенка завели.
Я благодарна Роману Петровичу за его внимание и профессионализм, что помог сестре! Возможно кому-то это будет полезно.
-форум отзывы о кладбищенских приворотах
-при кладбищенском привороте отзывы
-отзывы на кладбищенские привороты
-отзывы людей делавшие кладбищенский приворот
-отзывы о приворотах кладбищенских
sm-casino1.com
Hongzhi 황제는 “차이가 무엇입니까?”
Стоит ли делать приворот в Москве? Можно ли найти настоящего мага в Москве у которого правда можно заказать приворот?
Друзья, я не могу пройти мимо и не поделиться своим впечатлением о заказе приворота на мужчину! Моя жизнь казалась полной руин, когда я обнаружила, что мой мужчина не обращает на меня внимания и даже начал демонстрировать интерес к другим женщинам. Это было просто адом!
Я отчаянно пыталась найти выход из этой ситуации, обратилась к нескольким магам в Москве, но результаты были никакими. Я была на грани отчаяния, пока моя подруга не посоветовала мне обратиться к Роману Петровичу с Дальнего Востока. Нашла его сайт https://cmag666.ru где много ценной информации.
Скажу честно, я была в состоянии полного краха, когда позвонила Роману Петровичу. Но он был таким терпеливым и понимающим, что я сразу почувствовала, что могу ему доверять. Я заказала приворот мужчине и надеялась на лучшее.
И что же? Результат меня поразил до глубины души! Мой муж стал совсем другим человеком – внимательным, заботливым и полным энтузиазма! Мы снова влюблены друг в друга как в самом начале наших отношений!
Я просто не могу передать словами, как благодарна Роману Петровичу за то, что он вернул моего мужа ко мне! Если у вас возникли проблемы в отношениях и вы ищете решение, обратитесь к нему без колебаний. Он действительно знает, как помочь в сложных ситуациях!
– заказать приворот москва
– приворот москва бабушка
– кто делал приворот в москве отзывы
– приворот с фото москва
– недорогие привороты в москве
Отзывы о приворотах в Екатеринбурге
—————————————–
Хочу поделиться своим незабываемым опытом работы с магом Романом Петровичем с сайта https://cmag666.ru. Проживая в Екатеринбурге, я столкнулась с трудностями в отношениях со своим мужем. Попытки решить проблемы с мужем при помощи местных магов не привели к желаемому результату.
Поиски настоящего мага привели меня на сайт Романа Петровича, и я решила попробовать снова. Будучи из Дальнего Востока, родины шаманов, Роман Петрович вызвал мое доверие, и я обратилась к нему за помощью в восстановлении чувств моего мужа.
С Романом Петровичем мы обсудили мою ситуацию, и он предложил мне кладбищенский приворот для возврата чувств моего мужа. Я решила довериться его опыту и приступила к ритуалу с надеждой на лучшее.
С каждым днем я замечала, как наши отношения становились все более гармоничными и близкими. Муж начал проявлять больше внимания и заботы, а его чувства к мне стали стойчивыми и глубокими. Благодаря кладбищенскому привороту, наш брак стал еще крепче и устойчивее.
Работа Романа Петровича действительно поразила меня. Его профессионализм и внимание к моей ситуации впечатлили меня. Благодаря его помощи я снова чувствую себя счастливой и уверенной в нашем будущем вместе. Он настоящий мастер своего дела, и я безмерно благодарна ему за все, что он сделал для нашей семьи.
Я рекомендую Романа Петровича всем, кто столкнулся с проблемами в своих отношениях. Его помощь – это настоящее чудо, которое может изменить вашу жизнь к лучшему. Спасибо, Роман Петрович, за ваше волшебство и преданность своему делу!
– кто делает настоящий приворот екатеринбург
– привороты екатеринбург
– приворот по фото екатеринбург
– екатеринбург привороты
– привороты екатеринбурге
Мой отзыв о том, как я заказал приворот у мага
В августе этого года я столкнулся с самым непредсказуемым испытанием – узнал, что моя жена в течение двух лет вела роман на работе после двадцатилетнего брака и троих детей. Наша семья была на грани разрушения, и я честно говоря, не знал, что делать в этой ситуации. Оба мы были виноваты, и мне казалось, что нет выхода. Тогда я обратился к Роману Петровичу через его страничку https://cmag666.ru , и могу сказать, что это было одним из самых лучших решений в моей жизни.
После того, как Роман Петрович провел расклад карт, который оказался точным от начала и до конца, у меня появилась надежда. Он подобрал магическую работу, а затем выполнен был ритуал с защитным щитом и привязкой на огонь (подробности можно найти на его блоге). Сегодня, в декабре, я рад сообщить, что благодаря его помощи я вернул любимого человека и спас нашу семью. Наши отношения перешли на качественно новый уровень во всех аспектах.
Однако, я хочу подчеркнуть, что магия не сделает всё за вас. Вам также придется приложить значительные усилия и измениться, если вы хотите добиться успеха. Перед Романом Петровичем я преклоняю колени – без его помощи я бы не был так счастлив. Если у вас возникли подобные проблемы, я настоятельно рекомендую обратиться к Роману Петровичу.
Сайт ищут по тегам
– заказать приворот по интернету
– как заказать приворот
– заказать привороты у магов
– заказать черное венчание приворот
– кто может заказать снятие приворота
1xBet: Your Ultimate Betting Destination
1xbet com app download 1xbet 36 .
dota2answers.com
Xiao Jing은 계속해서 “어제 전달된 내각은 모두 Fang Jifan의 범죄로 기소되었습니다.”
LipoSlend is a liquid nutritional supplement that promotes healthy and steady weight loss. https://liposlendofficial.us/
svetlanamag ru – svetlanamagg @ yandex ru
Ритуал приворота у мага Светланы превзошел все мои ожидания! Моя любовь к парню стала еще сильнее, и он ответил мне взаимностью. Это настоящее чудо! Спасибо вам, Светлана, за вашу магическую помощь!
-настоящий союз магов
-настоящие маги которые помогли
-как по настоящему стать белым магом
-как стать настоящим магом в домашних условиях
История-отзыв о привороте у мага Александры (magpa666 @ bk ru) – magpomosh ru
В моей жизни наступило трудное время, и я решил обратиться за помощью к магу Александре с сайта magpomosh.ru. Моя семейная жизнь находилась на грани разрыва, и я не знал, что делать. Ситуация казалась безвыходной, и я чувствовал себя очень одиноким.
С момента первой встречи с Александрой я понял, что попал по адресу. Она внимательно выслушала мои проблемы и предложила мне ряд решений, среди которых был и ритуал приворота. Я решил попробовать, не имея особо больших надежд.
Но результат меня поразил. Спустя некоторое время после проведения ритуала наши отношения с женой начали улучшаться. Мы стали чаще общаться, лучше понимать друг друга, а наша семья стала крепче. Я благодарен магу Александре за ее терпение, помощь и понимание. Спасибо вам, Александра, за ваше волшебство!
Настоящий маг – magpa666 @ bk ru – magpomosh ru
_________________________________________________________
Сайт ищут по тегам:
черные маги проверенные как стать настоящим магом в реальной жизни приворот настоящие маги
проверенный маг для приворота кто такой настоящий маг реальные проверенные маги
форум проверенных магов как стать настоящем магом настоящие маги деньги берут
союз настоящих магов настоящий маг приворот посоветуйте белый маг проверенный
Хочу выразить благодарность магу Роману Петровичу с сайта cmag666.ru за его Вуду-приворот! Результаты просто поразительны! Моя давняя мечта о встрече с идеальным партнером осуществилась благодаря его ритуалу. Я счастливее, чем когда-либо! Благодарю вас, Роман Петрович, за ваш талант и помощь!
Запросы сайта в поиске
___________________________________________________________
приворот на куклу вуду кто делал отзывы кто делал вуду приворот отзывы приворот вуду отзывы
вуду приворот кто делал отзывы отзывы о приворотах вуду приворот вуду отзывы кто делал
Отзывы – Провели – приворот на любовь женатого https://cmag666.ru Ватсап 8 (984) 286-12-65
кому помог настоящий маг – правила игры волшебная четверка карточная игра для настоящих магов
Маг Мария Степановна не серьезно – заказала порчу у https://cmag666.ru Ватсап 8 (984) 286-12-65
обряд с яблоком на любовь – домашний очень сильный приворот
lfchungary.com
폐하께서는 지금 이미 인(仁)하시지만 선조(祖帝)와 인연이 있으니 가볍게 여겨 주시겠습니까?
Спасибо магу Светлане за ее ритуал приворота! Я заказала его для того, чтобы привлечь внимание парня, который давно был моим тайным объектом влечения. Результат меня поразил – он стал проявлять к намного больше интереса и даже сам начал инициировать встречи!svetlanamag ru – svetlanamagg @ yandex ru
-проверенный маг для приворота
-есть в москве настоящие маги
-маги и экстрасенсы проверенные в контакте
-помог настоящий маг
Доброго!
Промокоды для интернет-магазина Эльдорадо – это уникальные коды, которые можно использовать при оформлении заказа на официальном веб-сайте компании.
Они предоставляют дополнительные преимущества клиентам в виде скидок на определенные товары или услуги, бесплатной доставки и других бонусов.
Как найти такие промокоды для Эльдорадо? Обычно они предоставляются в рамках специальных акций компании, которые могут быть организованы
на ее официальном веб-сайте, в социальных сетях или на специализированных ресурсах, например, на сайте free-promocode.ru,
который предлагает самые свежие и проверенные промокоды
Сайт самых свежих и проверенных промокодов магазина Эльдорадо https://free-promocode.ru
Удачных покупок!
Официальные акции Эльдорадо
Эксклюзивные скидки Эльдорадо
Промокоды для экономии в Эльдорадо
Лучшие предложения Эльдорадо
актуальный промокод Эльдорадо
Удачи!
dota2answers.com
Jiao 가족의 친척은 아마도 그들 사이의 강력한 관계를 알고있을 것입니다.
Доброго!
Промокоды для интернет-магазина Эльдорадо — это специальные коды, которые можно активировать при оформлении заказа на официальном сайте компании.
Они предоставляют дополнительные преимущества покупателям в виде скидок на конкретные товары или услуги, бесплатной доставки или других бонусов.
Как найти промокоды для Эльдорадо? Они часто предоставляются в рамках специальных акций компании, которые могут проводиться на ее официальном сайте,
в социальных сетях или на проекте free-promocode.ru
Сайт самых свежих и проверенных промокодов магазина Эльдорадо https://free-promocode.ru
Удачных покупок!
актуальные промокоды Эльдорадо
Официальные акции Эльдорадо
актуальный промокод Эльдорадо
Бонусные предложения и скидки в Эльдорадо
выгодные промокоды Эльдорадо
Удачи!
Herkese selamlar!
Son zamanlarda Bwin tr, bwin giris çevrimiçi bahis endüstrisinde lider konumunu başarılı bir şekilde sağlamlaştırdı. Uzmanlar kadar, kumar oynamaya yeni başlayanlar
da bu platformu spor bahisleri dünyasında güvenilir bir tercih olarak seçiyorlar. Her ziyaretçi, platformun sunduğu heyecan dolu deneyimin tadını çıkarabilir.
Popüler spor etkinliklerinin yanı sıra, site golf, tenis veya beyzbol gibi daha az bilinen bahis disiplinlerine de yer vermektedir.
Geniş seçenekler ve yenilikçi yaklaşımı sayesinde herkesin ilgisini çekecek bir şey bulunmaktadır
Kumarhane Еџans oyunlarД± BWin
Slot makineleri BWin
Kumarhane rehberi BWin
Kumarhane para kazanma BWin
Kumarhane indirimleri BWin
Kumarhane hakkД±nda bilgi BWin
Kumarhane gГјvenilir mi BWin
Kumarhane popГјler oyunlar BWin
Iyi sanlar!
Астарт Вард отзывы форум magastartvard . ru Астарт Вард отзывы
______________________________________________________
magastartvard . ru отзыв о нем могу оставить только положительный
Заказала у мага Астарта Варда индивидуальный гороскоп и прогноз на будущее. Он дал мне ценные советы и предсказания, которые помогли мне лучше понять себя и свои жизненные пути. Очень довольна результатом и рекомендую его услуги!
______________________________________________________________
отзывы о маге Астарт Вард
Herkese selamlar!
Son yıllarda Bwin tr, https://bwintr.top çevrimiçi bahis endüstrisinde liderler arasında başarılı bir şekilde yerini sağlamlaştırdı. Uzmanlar kadar, kumar oynamaya yeni başlayanlar
da bu platformu spor bahisleri dünyasında güvenilir bir seçenek olarak tercih etmektedirler. Her ziyaretçi, platformun sunduğu heyecan dolu deneyimin tadını
çıkarabilir. Popüler spor etkinliklerinin yanı sıra, site golf, tenis veya beyzbol gibi daha az yaygın olan bahis disiplinlerini de sunmaktadır.
Geniş seçenekler ve yenilikçi yaklaşımıyla herkes için bir şeyler bulunmaktadır
Kumarhane bonuslarД± BWin
Kumarhane promosyonlarД± BWin
Kumarhane Еџans oyunlarД± BWin
Kumarhane indirimleri BWin
Kumarhane para kazanma BWin
Kumarhane stratejileri BWin
Kumarhane rehberi BWin
Kumarhane oyunlarД± Г§eЕџitleri BWin
Iyi sanlar!
Крастко – Отзывы magpomosh ru – сайт – белый приворот на мужчину отзывы кто
Магический сайт magpomosh .ru – отзывы могу оставить только хорошие.
Маг Александра – настоящий профессионал своего дела. Ее ритуалы на защиту от негатива помогли мне избежать неприятностей и сохранить свою энергию
_________________________________________________________
Сайт ищут по тегам:
настоящий маги союз магов россии настоящие или нет настоящий маг как найти
маги красноярска проверенные настоящий мага как стать настоящим магом
настоящий маг который помог официальный сайт магов россии список настоящих союз шарлатаны и проверенные маги
он сильный маг проверенный настоящие маги и ясновидящие где вы нашли настоящего мага
hihouse420.com
Hongzhi 황제는 이것을 듣고 거의 불에 탔습니다.
Как сэкономить на оформлении документов
– Отпуск по системе “все включено”: турция тур
турция отдых все включено https://anex-tour-turkey.ru/ .
Отдых на курортах Турции
путевка в турцию цена http://tez-tour-turkey.ru/ .
pragmatic-ko.com
그들은 300만 냥을 직접, 스터드 직접, 망설임 없이, 아무 생각 없이 지불했습니다.
Привет Всем!
Sykaaa Casino, запущенное в 2022 году, представляет собой молодой, но перспективный проект в мире азартных развлечений. Владельцем казино является Snowdunes B.V.,
а лицензия выдана в Кюрасао под номером 8048/JAZ2022-007. Это обеспечивает игрокам честную и безопасную игровую среду.
Sykaaa Casino стремится привлечь максимальное количество игроков, переведя интерфейс на русский, английский и украинский языки.
Даже на начальном этапе развития казино привлекает внимание сотен игроков онлайн, превышая отметку в 2000-3000 человек в пиковые часы.
Sykaaa Casino https://serpcity.ru радует игроков оригинальными бонусами. Например, новички могут получить 100 фриспинов на автомат Razor Shark без депозита.
Приветственный бонус в размере 100% от первого депозита также доступен.
Минимальный депозит для активации бонуса – 500 рублей, а максимальная сумма начисления – 5000 евро. Условия вейджера для вывода выигрышей составляют x45.
Sykaaa Casino предоставляет более 1000 игр от ведущих провайдеров, таких как Betsoft, Pragmatic Play, Microgaming и другие.
В коллекции более 1000 слотов, включая новинки и популярные игры. Опция игры бесплатно доступна зарегистрированным пользователям.
Демоверсии настольных игр доступны бесплатно, что позволяет игрокам освоить стратегии перед игрой на реальные деньги.
Минимальный депозит в Sykaaa Casino составляет 300 RUB, а минимальная сумма вывода – 1000 RUB. Оператор поддерживает различные методы оплаты, включая карты, электронные кошельки и криптовалюты. Выплаты обрабатываются в течение 0-24 часов.
sykaaa casino зеркало рабочее на сегодня
casino sykaaa скачать
sykaaa официальный сайт казино
sykaa казино
sykaaa официальный сайт
игровые автоматы sykaa
sykaaa casino бездепозитный бонус промокод
sykaa игровые автоматы на деньги
Удачи и прибыли Друзья!
Здравствуйте!
В 2022 году в мире азартных развлечений появился новый игрок https://serpcity.ru — казино Sykaaa. За его разработку и эксплуатацию отвечает Snowdunes B.V.
Сайт оперирует под лицензией Curacao: 8048/JAZ2022-007, выданной владельцу платформы. Этот молодой проект, основанный в 2022 году, уже успел привлечь внимание игроков своими бонусами и богатым выбором игр. Для обеспечения надежности, оператор получил лицензию от Кюрасао.
Валидность лицензии можно проверить на главной странице, кликнув по соответствующей иконке валидатора. Владельцем платформы является Snowdunes B.V., а сам проект находится в стадии активного развития.
Sykaaa Casino стремится охватить широкую аудиторию, предоставив интерфейс на трех языках: русском, украинском и английском.
Такое многоязычие делает сайт доступным для игроков из разных стран. Оригинальные бонусы и акции делают игру в Sykaaa Casino увлекательной.
Например, новичкам доступны 100 бесплатных вращений для автомата Razor Shark в течение 7 дней после регистрации. Приветственный бонус составляет 100%,
а максимальная сумма, которую можно получить, — 5000 евро. Свыше 1000 игр от таких провайдеров, как Betsoft, Pragmatic Play, Microgaming и другие,
доступны пользователям Sykaaa Casino. Каталог постоянно расширяется, делая игровой процесс разнообразным и интересным.
Sykaaa Casino предлагает разнообразные способы пополнения и вывода средств, включая Мир, СБП, Visa, Mastercard, Bitcoin и другие.
Минимальный депозит для активации бонуса — 500 рублей, а лимит на вывод составляет 10 000 USD в день. Sykaaa Casino не предлагает отдельного приложения, но мобильная версия сайта обеспечивает стабильную работу на любых устройствах. Благодаря этому, игроки могут наслаждаться азартом через браузер смартфона или планшета.
sykaaa casino сайт
sykaaa casino ксыз
sykaaa casino войти sykaaaa online
sykaa casino
sykaaa casino бонус
сукааа казино рабочее зеркало
sykaaa casino промокод
сукаа казино
Удачи и прибыли Друзья!
dota2answers.com
효자로서 폐하께서 시체를 수천 조각으로 쪼개셨다니 무슨 상관이 있겠습니까?
Грузоперевозки для частных лиц
услуги переезда https://www.moving-company-kharkov.com.ua .
lfchungary.com
Su Yue는 신중하게 약을 바르고 Shigong에 붕대를 감았습니다.
“Melin Ajans ile çalışmak, fuarlarımızı daha başarılı kılmamızı sağlıyor. Her zaman memnuniyetle çalışıyoruz.”
“İstanbul’da fuarlarınızı daha çekici hale getirmek istiyorsanız, Melin Ajans ile çalışmalısınız. Harika bir ekip!”
сериал онлайн
Як обрати спецтехніку за потребами
спецтехніка чернівці https://www.spectehnika-sksteh.co.ua .
Hello, World!
Hey there, mate! Greetings from your favorite surfing capybara!
How’s the surf today?
Ready to catch some gnarly waves together?
https://capybara888.wordpress.com/
Good luck!
Как повысить узнаваемость бренда строительной компании?
продвижение строительство https://seo-prodvizhenie-sajtov-stroitelnyh-kompanij.ru/ .
Шаг за шагом
4. Важные этапы установки кондиционера
vrv daikin http://ustanovit-kondicioner.ru/ .
pragmatic-ko.com
“아.” Fang Jifan은 “사실 나도 생각이 있습니다. “라고 말했습니다.
Гарантированно низкие цены на кондиционеры
сплит продажа http://www.prodazha-kondicionera.ru .
Stomatologurmonsk Подготовка и послеоперационный уход
Стоматология: основные принципы здоровья полости рта
https://asktourist.ru/viewtopic.php?id=500&p=3#p17143 .
pragmatic-ko.com
피부는 정말 두껍고 냄새가 나고 뻔뻔합니다.
strelkaproject.com
여기 오기 전에는 극심한 고통을 겪었지만 여기에서는… 실제로 나쁘지 않습니다.
12. Стандартные цены на монтаж кондиционера
кондиционер монтаж https://www.montazh-kondicionera-moskva.ru/ .
windowsresolution.com
누군가 “누가 그것을 선동 했습니까? “라고 외쳤습니다.
настоящего мага воды – отзывы Ангелина 89853905910
______________________________________________________
Я сотрудничал с Магом Ангелиной, чтобы разрешить некоторые сложные проблемы в моей жизни. Я был поражен ее профессионализмом и эффективностью. Она внимательно выслушала мои проблемы и предложила мне ряд ритуалов и обрядов, которые помогли мне преодолеть препятствия. Результаты были заметны уже через несколько недель после начала работы с ней. Я очень благодарен Магу Ангелине за ее помощь и рекомендую ее всем, кто ищет помощи в области магии.
Маг Ангелина 89853905910 отзывы
pragmatic-ko.com
“여기 여자들은 착해요.” 쉬징이 목소리를 낮추고 양견에게 말했다.
1. Где купить кондиционер: лучшие магазины и выбор
2. Как выбрать кондиционер: советы по покупке
3. Кондиционеры в наличии: где купить прямо сейчас
4. Купить кондиционер онлайн: удобство и выгодные цены
5. Кондиционеры для дома: какой выбрать и где купить
6. Лучшие предложения на кондиционеры: акции и распродажи
7. Кондиционер купить: сравнение цен и моделей
8. Кондиционеры с установкой: где купить и как установить
9. Где купить кондиционер с доставкой: быстро и надежно
10. Кондиционеры: где купить качественный товар по выгодной цене
11. Кондиционер купить: как выбрать оптимальную мощность
12. Кондиционеры для офиса: какой выбрать и где купить
13. Кондиционер купить: самый выгодный вариант
14. Кондиционеры в рассрочку: где купить и как оформить
15. Кондиционеры: лучшие магазины и предложения
16. Кондиционеры на распродаже: где купить по выгодной цене
17. Как выбрать кондиционер: советы перед покупкой
18. Кондиционер купить: где найти лучшие цены
19. Лучшие магазины кондиционеров: где купить качественный товар
20. Кондиционер купить: выбор из лучших моделей
монтаж кондиционера http://www.kondicioner-cena.ru/ .
Рекомендации
20. Почему стоит купить хостинг с максимальной скоростью загрузки
дешевый хостинг https://kish-host.ru .
Перетяжка мягкой мебели
https://www.automania.by/forum/index.php?showtopic=15542 .
lfchungary.com
Xie Qian은 조금 불안해 보였고 그의 마음은 궁전에 묶여있었습니다.
Подробный гид по выбору,
10 важных преимуществ виртуальных серверов ,
5 лучших операционных систем для виртуальных серверов ,
Как установить и настроить базу данных на виртуальном сервере ,
Сравнение цен и тарифов,
Как узнать, сколько ресурсов требуется для вашего проекта на виртуальном сервере
недорогой выделенный сервер проверенный хостинг .
https://tv-news-id-22649540.vxi.su/
chutneyb.com
Zhu Houzhao는 그의 다리가 약간 부드럽다는 것을 느끼며 심장을 쿵쾅거렸습니다.
Быстрый и надежный ремонт холодильников марки Атлант по доступной цене.
ремонт атланта холодильника ремонт холодильников атлант .
Онлайн казино Беларусь: играйте на деньги или бесплатно
онлайн казино онлайн казино .
lfchungary.com
Mu의 말을 듣고 Liu Tianzheng의 얼굴이 바뀌었다.
Жены получат право вносить мужей-игроманов в черный список онлайн-казино Беларуси
Беларусь открывает двери для онлайн-казино: Лукашенко подписал новый указ
pactam2.com
“말씀하십시오, 폐하의 말씀에 대답하십시오.” 옆에 있던 내시가 속삭였다.
Hello, World!
Hey there, mate! Greetings from your favorite surfing capybara!
How’s the surf today?
Ready to catch some gnarly waves together?
https://capybara444.wordpress.com
Good luck!
Hello, World!
Hey there, mate! Greetings from your favorite surfing capybara!
How’s the surf today?
Ready to catch some gnarly waves together?
https://capybara235.wordpress.com
Good luck!
manzanaresstereo.com
Chen Yan에게 있어 이 사람들을 포획해야만 그의 전하가 보장될 수 있습니다.
Стратегии игры в онлайн казино Беларусь: как увеличить шансы на победу
онлайн казино казино беларусь .
smcasino-game.com
Wang Hua는 마침내 감동을 받았으며 마침내 “Mian Sheng! “이라는 두 단어를 뱉었습니다.
Приветствую всех!
Промокоды для интернет-магазина М.Видео — это специальные коды, которые можно активировать при оформлении заказа на официальном сайте компании.
Они предоставляют дополнительные преимущества покупателям в виде скидок на конкретные товары или услуги, бесплатной доставки или других бонусов.
Как найти промокоды для М.Видео? Они часто предоставляются в рамках специальных акций компании, которые могут проводиться на ее официальном сайте,
в социальных сетях или на проекте promokodbar.ru
Сайт самых свежих и проверенных купонов магазина М.Видео https://promokodbar.ru
Удачных покупок!
Привилегированные промокоды М.Видео
Промокоды для получения дополнительных бонусов в М.Видео
Специальные предложения и скидки М.Видео
выгодные промокоды М.Видео
Эксклюзивные скидки М.Видео
Удачи!
apksuccess.com
새 약은 도난 당했을 뿐만 아니라…역시 자오의 집에 있었다.
Привет всем!
Было ли у вас опыт написания дипломной работы в крайне сжатые сроки? Это действительно требует огромной ответственности и трудоемкости, однако важно сохранять упорство и продолжать активно участвовать в учебном процессе, как я это делаю.
Для тех, кто умеет эффективно искать и анализировать информацию в интернете, это действительно помогает в процессе согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или организацию встреч с научным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями по ссылке https://2orik-diploms.com, это проверенный источник!
купить диплом магистра
купить диплом Гознак
купить диплом о среднем образовании
купить диплом в Москве
купить диплом колледжа
Желаю всем отличных оценок!
sm-slot.com
이때 대명문 밖에는 새 옷을 입은 문무관들이 모두 엄숙하게 서 있었다.
Здравствуйте!
Бывало ли у вас такое, что приходилось писать дипломную работу в очень ограниченные сроки? Это действительно требует большой ответственности и тяжелого труда, но важно не сдаваться и продолжать активно заниматься учебными процессами, так же, как и я.
Для тех, кто умеет эффективно использовать интернет для поиска и анализа информации, это действительно облегчает процесс согласования и написания дипломной работы. Не нужно тратить время на посещение библиотек или организацию встреч с дипломным руководителем. Здесь представлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями по ссылке https://3russkiy-diploms.com, это проверенный способ!
купить диплом ссср
купить аттестат
купить диплом бакалавра
купить диплом о высшем образовании
купить диплом нового образца
Желаю всем отличных оценок!
Доброго!
Было ли у вас когда-нибудь так, что приходилось писать дипломную работу в очень сжатые сроки? Это действительно требует огромной ответственности и может быть очень тяжело, но важно не опускать руки и продолжать активно заниматься учебными процессами, как я.
Для тех, кто умеет быстро находить и использовать информацию в интернете, это действительно облегчает процесс согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или устраивать встречи с научным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями на сайте https://1russa-diploms.com, это проверено!
купить аттестат
купить диплом
купить диплом ссср
купить диплом специалиста
купить диплом о среднем специальном
Желаю всем отличных оценок!
jelenakaludjerovic.com
이 대화를 마치고 그의 발걸음은 한결 가벼워졌고 곧 누안정에 도착했다.
madridnortehoy.com
이렇게 되면 죽고 사는 문제인데 어찌 충성심이 있겠습니까?
Привет всем!
Вы когда-нибудь писали диплом в сжатые сроки? Это очень ответственно и тяжело, но нужно не сдаваться и делать учебные процессы, чем Я и занимаюсь)
Тем кто умеет разбираться и гуглить информацию, это действительно помогает по ходу согласований и написания диплома, не нужно тратить время на библиотеки или встречи с дипломным руководителем, вот здесь есть хорошие данные для заказа и написания дипломов и курсовых с гарантией и доставкой по России, можете посмотреть здесь https://1russa-diploms.com, проверено!
купить диплом о высшем образовании
купить диплом бакалавра
купить диплом цена
купить диплом ссср
купить диплом техникума
Желаю всем отличных оценок!
Здравствуйте!
Были ли у вас случаи, когда приходилось писать дипломную работу в крайне ограниченные сроки? Это действительно требует большой ответственности и трудоемкости, но важно не отступать и продолжать активно участвовать в учебном процессе, как я.
Для тех, кто умеет эффективно находить и использовать информацию в сети, это действительно помогает в процессе согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или организацию встреч с научным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями тут https://server-diploms.com, это проверенный источник!
купить диплом ссср
купить диплом цена
купить аттестат
купить диплом института
Желаю всем отличных оценок!
Куда обратиться за ремонтом холодильника Атлант? У нас!
ремонт холодильников атлант цена ремонт холодильников атлант на дому .
Доброго!
Было ли у вас когда-нибудь такое, что приходилось писать дипломную работу в сжатые сроки? Это действительно требует огромной ответственности и напряженных усилий, но важно не сдаваться и продолжать активно заниматься учебными процессами, чем я и занимаюсь.
Для тех, кто умеет искать и анализировать информацию в интернете, это действительно помогает в процессе согласования и написания дипломной работы. Не нужно тратить время на посещение библиотек или организацию встреч с дипломным руководителем. Здесь представлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по России. Можете ознакомиться с предложениями по ссылке https://2orik-diploms.com, проверено!
купить диплом Вуза
купить диплом о среднем образовании
купить диплом специалиста
купить диплом о высшем образовании
купить аттестат школы
Желаю всем отличных оценок!
Доброго!
Бывало ли у вас такое, что приходилось писать дипломную работу в крайне ограниченные сроки? Это действительно требует огромной ответственности и напряженных усилий, но важно не опускать руки и продолжать активно заниматься учебными процессами, чем я и занимаюсь.
Для тех, кто умеет искать и анализировать информацию в интернете, это действительно облегчает процесс согласования и написания дипломной работы. Не нужно тратить время на посещение библиотек или устраивать встречи с дипломным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по России. Можете ознакомиться с предложениями по ссылке купить диплом университета, это проверено!
купить диплом бакалавра
купить диплом техникума
купить аттестат школы
купить диплом цена
купить диплом о среднем образовании
купить диплом ссср
купить диплом Вуза
купить диплом университета
купить диплом в Москве
купить диплом колледжа
Желаю всем отличных оценок!
Здравствуйте!
Были ли у вас случаи, когда приходилось писать дипломную работу в крайне ограниченные сроки? Это действительно требует большой ответственности и трудоемкости, но важно не отступать и продолжать активно участвовать в учебном процессе, как я.
Для тех, кто умеет эффективно находить и использовать информацию в сети, это действительно помогает в процессе согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или организацию встреч с научным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями тут https://server-diploms.com, это проверенный источник!
купить диплом нового образца
купить диплом цена
купить диплом Вуза
купить диплом бакалавра
Желаю всем отличных оценок!
Привет всем!
Бывало ли у вас такое, что приходилось писать дипломную работу в крайне сжатые сроки? Это действительно требует огромной ответственности и напряженных усилий, но важно не опускать руки и продолжать активно заниматься учебными процессами, как я.
Для тех, кто умеет быстро находить и анализировать информацию в сети, это действительно помогает в процессе согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или устраивать встречи с дипломным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями на сайте https://saksx-diploms24.com, это проверено!
купить диплом специалиста
купить диплом Вуза
купить диплом
купить аттестат школы
купить диплом магистра
купить диплом техникума
купить диплом ссср
купить диплом о высшем образовании
купить диплом цена
купить диплом нового образца
Желаю всем отличных оценок!
Хочешь обновить интерьер? Перетянем твою мебель в Минске
ремонт и перетяжка мягкой мебели https://obivka-mebeli-vminske.ru/ .
Доброго!
Купоны для интернет-магазина М.Видео – это уникальные коды, которые можно использовать при оформлении заказа на официальном веб-сайте компании.
Они предоставляют дополнительные преимущества клиентам в виде скидок на определенные товары или услуги, бесплатной доставки и других бонусов.
Как найти такие промокоды и купоны для М.Видео? Обычно они предоставляются в рамках специальных акций компании, которые могут быть организованы
на ее официальном веб-сайте, в социальных сетях или на специализированных ресурсах, например, на сайте promokodbar.ru,
который предлагает самые свежие и проверенные промокоды
Сайт самых свежих и проверенных купонов магазина М.Видео https://promokodbar.ru
Удачных покупок!
свежие купоны М.Видео
Эксклюзивные акции и скидки в М.Видео
Официальные акции М.Видео
Скидки и бонусы в интернет-магазине М.Видео
Привилегированные промокоды М.Видео
Удачи!
Привет всем!
Бывало ли у вас такое, что приходилось писать дипломную работу в очень ограниченные сроки? Это действительно требует большой ответственности и тяжелого труда, но важно не сдаваться и продолжать активно заниматься учебными процессами, так же, как и я.
Для тех, кто умеет эффективно использовать интернет для поиска и анализа информации, это действительно облегчает процесс согласования и написания дипломной работы. Не нужно тратить время на посещение библиотек или организацию встреч с дипломным руководителем. Здесь представлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями по ссылке https://3russkiy-diploms.com, это проверенный способ!
купить аттестат школы
купить аттестат
купить диплом о среднем специальном
купить диплом о среднем образовании
купить диплом Вуза
Желаю всем отличных оценок!
Мастерская по перетяжке мебели в Минске
обшивка дивана https://obivka-mebeli-vminske.ru/ .
Онлайн казино Беларусь: наслаждайтесь азартом и выигрывайте крупные суммы!
онлайн казино казино беларусь .
Мастерская по перетяжке мягкой мебели в Минске – доверенный выбор
перетянуть кресло https://obivka-mebeli-vminske.ru/ .
Günsu AŞ Havuz, her projede mükemmel işçiliği ve özgün tasarımlarıyla fark yaratıyor.
jelenakaludjerovic.com
Hongzhi 황제는 Zeng Jie를 무시했지만 “Fang Qing의 가족”이라고 침착하게 말했습니다.
mega-casino66.com
사람들은 갑자기 무언가를 깨달았습니다. 기적이 일어나고 있는 것 같았습니다.
Как выбрать мастера для перетяжки мебели в Минске? Легко!
обивка мебели https://obivka-divana.ru/ .
Перетяжка мягкой мебели в Минске: качественно и недорого
перетяжка дивана в минске https://obivka-divana.ru/ .
Hello, World!
Hey there, mate! Greetings from your favorite surfing capybara!
How’s the surf today?
Ready to catch some gnarly waves together?
https://capybara999.wordpress.com/
Good luck!
Хочешь обновить интерьер? Перетянем твою мебель в Минске
перетянуть кресло https://obivka-divana.ru/ .
Надежная перетяжка мебели в Минске по доступной цене
перетяжка стульев https://obivka-divana.ru/ .
jbustinphoto.com
그들은 먼저 출발했고 많은 양의 짐이 뒤에서 천천히 옮겨졌습니다.
Как перетянуть мебель в Минске? Обратись к нам!
обшивка дивана https://obivka-divana.ru/ .
?Juega gratis! Bono casino sin deposito
casino online con bono de bienvenida sin deposito bono casino sin deposito .
онлайн
Anyone looking to discover leading online casinos that accept Mpesa payments.
металлические конструкции это http://ingibitor-korrozii-msk.ru/ .
Anyone interested in finding premier online casinos compatible with Mpesa.
смотреть
детская коляска купить москва http://www.detskie-koljaski-msk.ru/ .
mojmelimajmuea.com
그녀는 침묵을 지켰고 Wang Yan은 조심스럽게 눈을 들어 Dowager 황후의 표정을 확인했습니다.
фильм
фильм онлайн
sm-online-game.com
Fang Jinglong은 산속 깊은 곳에서 매우 눈에 띄지 않는 Shijianzhai를 발견했습니다 …
depakote labs
pactam2.com
Zhu Houzhao도 RI 개로 책을 복사하는데 무슨 일이 일어날 수 있습니까?
смотреть фильм
Святослав Серебряков отзывы маг
Отзыв о магической услуге у Мага Святослава Серебрякова: Подлинное Волшебство в Действии
Я хочу поделиться своим восхитительным опытом работы с Магом Святославом Серебряковым. После долгих поисков и чтения множества положительных отзывов о его способностях, я решил обратиться за помощью в решении своих личных проблем.
С самого начала контакта с Магом Святославом я почувствовал облегчение и уверенность в том, что я на правильном пути. Его профессионализм, понимание и энергия, которую он излучает, создают атмосферу доверия и комфорта.
Результаты его работы превзошли все мои ожидания. Я испытал удивительные перемены в своей жизни благодаря его помощи. Магическая услуга, которую он предоставил, была точно тем, что мне нужно. Я чувствую себя сильнее, увереннее и более сбалансированным после сеансов с ним.
Маг Святослав Серебряков – это не просто мастер своего дела, он настоящий человек, который заботится о своих клиентах и их благополучии. Я не могу рекомендовать его достаточно сильно для всех, кто ищет подлинное волшебство и помощь в своей жизни.
Спасибо, Маг Святославе Серебрякову, за ваше великолепное влияние на мою жизнь и мою судьбу. Я навсегда благодарен вам за вашу помощь и поддержку.
-молитвы приворот на любовь
-как понять есть ли приворот на человеке
-приворот мужчины по фотографии читать самостоятельно
-как влияет приворот на мужчин последствия
-приворот на соль и воду
https://surgeryzone.net/news/podbiraem-idealnye-komplektuyushhie-dlya-komfortnyx-ofisnyx-kresel.html
https://mhcolimpia.ru/izgotovlenie-plastikovyh-veder-na-zakaz-preimushhestva-litya-pod-davleniem/
смотреть
Amen! — Истинно; Конец.
Aprovecha esta oportunidad: bono casino sin deposito
casino online bono sin deposito casino con bono de bienvenida sin deposito .
Beati pauperes spiritu — библ. Блаженны нищие духом.
Amabilis insania — Приятное безумие.
Confessus pro judicato habetur — прав. Сознавшийся считается осуждённым.
Aut vincere, aut mori — Или победить, или умереть.
Тепловизоры для охоты: какой выбрать и почему
тепловизоры teplovizor-od.co.ua .
Создание уникального контента для продвижения сайта
11
seo это http://www.seo-prodvizhenie-sayta.co.ua .
sm-slot.com
그러나 Zhu Houzhao의 체력은 너무 놀라워서 Fang Jifan을 순식간에 따라 잡았습니다.
khasiss.com
그는 즉시 말했습니다. “게다가… 많은 기계가 있고…”
Disfruta del mejor bono casino sin deposito
casino online con bono de bienvenida sin deposito bono casino sin deposito .
обзор
19. Оптические прицелы с подсветкой меток для стрельбы на различные дистанции
оптический прицел недорого https://opticheskiy-pricel-odessa.co.ua .
сериал
Discovering esteemed online casinos that facilitate Mpesa transactions is made effortless with our guidance.
Seeking out reputable online casinos that seamlessly integrate Mpesa payments? Look no further.
Hello everyone!
п»ї
Globex Music takes care of all the legal aspects of cover song distribution, ensuring that artists are protected from copyright infringement issues.
This peace of mind is invaluable for musicians who want to focus on creating music, not dealing with legal headaches.
п»їhttps://distro.globexmusic.com/register.php?ref=ZU0VL
п»ї cover song distribution
odd cover songs
п»їcover song distribution
cover songs definition
free cover song licensing
covers of 70s songs
cover song licensing & distribution
cover song licensing – get a mechanical license
cover license distrokid
groove coverage she
how to get a mechanical license to cover a song
Good luck and good vibe!
uzun zamandır kendileri ile çalışıyoruz çok başarılılar
uzun zamandır kendileri ile çalışıyoruz çok başarılılar
Лучшие цены на услуги грузчиков в Харькове
заказать перевозку с грузчиками https://gruzchiki.co.ua/ .
twichclip.com
Wang Jinyuan은 서둘러 왔습니다. “젊은 주인님, 젊은 주인님 …”
ttbslot.com
심장 박동은 약간 빠르며 맥박은 분당 약 150입니다.
ttbslot.com
도시 꼭대기에서 돌이켜 도망치려던 사람들이 갑자기 용기를 얻었습니다.
Unleash your gaming prowess at online casinos Kenya, where fresh challenges and prompt payouts await the daring.
Простые советы по уходу за рулонным газоном
рулонный газон https://rulonnyygazon177.ru/ .
I really love to read such an excellent article. Helpful article. Hello Administ .
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.
Thank you for great content. Hello Administ.
Thank you for great article. Hello Administ .
Nice article inspiring thanks. Hello Administ .
Embrace the thrill of online casinos Kenya, where new gaming adventures and rapid payouts await the bold.
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.儿童色情片
Thank you for great article. Hello Administ .国产线播放免费人成视频播放
Thank you for great content. Hello Administ.現場兒童色情片
Good info. Lucky me I reach on your website by accident, I bookmarked it. 国产线播放免费人成视频播放
Everything is very open and very clear explanation of issues. was truly information.国产线播放免费人成视频播放
Everything is very open and very clear explanation of issues. was truly information.国产线播放免费人成视频播放
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.儿童色情片
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.兒童色情
Thank you for content. Area rugs and online home decor store. Hello Administ .
фильм
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.
Thank you great post. Hello Administ .
Everything is very open and very clear explanation of issues. was truly information.
Thank you for content. Area rugs and online home decor store. Hello Administ .
Good info. Lucky me I reach on your website by accident, I bookmarked it.
qiyezp.com
그리고 지금…Fang Jifan은 실제로…상처에 소금을 뿌리고 싶어합니다.
ttbslot.com
Zhu Houzhao는 “내가 당신에게 어떤 선물을 주든 그는 가시를 뽑을 수 있습니다. “라고 한숨을 쉬었습니다.
Experience the ultimate gaming thrill at online casinos Kenya, where fresh titles and swift payouts are just a click away.
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.
Great post thank you. Hello Administ .
Thank you great posting about essential oil. Hello Administ .
Nice article inspiring thanks. Hello Administ .
Elevate your gaming experience with online casinos Kenya, where innovative titles and swift payouts are the norm.
Discover the epitome of excitement at online casinos Kenya, where novel games and rapid payouts are the ultimate rewards.
Thank you for great information. Hello Administ . 国产线播放免费人成视频播放
Thank you for great content. Hello Administ. 国产线播放免费人成视频播放
I really love to read such an excellent article. Helpful article. Hello Administ . 国产线播放免费人成视频播放
Thank you great post. Hello Administ .国产线播放免费人成视频播放
sandyterrace.com
밖에서 갑자기 내리는 빗소리에 모두가 귀를 기울이고 있었고, 모두의 마음은 패닉에 휩싸였습니다.
Great post thank you. Hello Administ . 国产线播放免费人成视频播放
Thank you great post. Hello Administ .国产线播放免费人成视频播放
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.兒童色情
Thank you for content. Area rugs and online home decor store. Hello Administ . 国产线播放免费人成视频播放
exprimegranada.com
素晴らしい記事でした!いつもありがとうございます。
Thank you for great content. Hello Administ.現場兒童色情片
Thank you for great article. Hello Administ .
I really love to read such an excellent article. Helpful article. Hello Administ .
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.
Thank you for great content. Hello Administ.
является участником банды . Именно помогла ему открыть сайт и теперь она за своё покровительство и раскрутку получает часть денег от клиентов-лохов, которых обработал мерзавец-шарлатан.
Как это обычно и бывает у мошенников, — это не настоящие имя-отчество, а очередной псевдоним. За случайной кличкой скрывается безработный, раньше уже мотавший сроки, продолжающий свою мошенническую деятельность.
Вместо реального фото, на вывешено сгенерированное нейросетью изображение мультяшного персонажа, эдакого старца-волхва. Настоящую же свою испитую,физиономию немаг тщательно скрывает, так как справедливо опасается, что вычислят и накажут.
Также на размещены написанные аферистом отзывы даже за 2010 год. В реальности же сайт появился всего пару недель назад – 15 февраля 2024 года. И именно эти две недели уголовник обманывает именно под кличкой.
Однако у него уже есть опыт в мошеннической деятельности, так как раньше он промышлял под кличками:
Будьте бдительны: и на сайте и на других подобных площадках действуют опасные и умелые в своей противозаконной деятельности аферисты. Они знают, как войти в доверие, но никто из них не способен оказать реальную помощь.
И шарлатан и подобные ему, постоянно дают пустые обещания. Деньги гребут лопатой, но никогда ни одному человеку не помогут. Так как все приписываемые им сверхъестественные способности — один сплошной обман. Ни один реальный отзыв от обманутых клиентов на не будет пропущен лжемагом – все отзывы от сам себе и пишет.
шарлатан предыстория
сериал онлайн
sandyterrace.com
궁을 짓기 위해 Fang Jifan은 정말 수많은 노력을 기울였습니다.
animehangover.com
이 사람은 이 말을 듣고 나서… 그가 매우 유능하다는 것을 압니다.
1. Вибір натяжних стель – як правильно обрати?
2. Топ-5 популярних кольорів натяжних стель
3. Як зберегти чистоту натяжних стель?
4. Відгуки про натяжні стелі: плюси та мінуси
5. Як підібрати дизайн натяжних стель до інтер’єру?
6. Інноваційні технології у виробництві натяжних стель
7. Натяжні стелі з фотопечаттю – оригінальне рішення для кухні
8. Секрети вдалого монтажу натяжних стель
9. Як зекономити на встановленні натяжних стель?
10. Лампи для натяжних стель: які вибрати?
11. Відтінки синього для натяжних стель – ексклюзивний вибір
12. Якість матеріалів для натяжних стель: що обирати?
13. Крок за кроком: як самостійно встановити натяжні стелі
14. Натяжні стелі в дитячу кімнату: безпека та креативність
15. Як підтримувати тепло у приміщенні за допомогою натяжних стель
16. Вибір натяжних стель у ванну кімнату: практичні поради
17. Натяжні стелі зі структурним покриттям – тренд сучасного дизайну
18. Індивідуальність у кожному домашньому інтер’єрі: натяжні стелі з друком
19. Як обрати освітлення для натяжних стель: поради фахівця
20. Можливості дизайну натяжних стель: від класики до мінімалізму
навісні стелі https://natjazhnistelitvhyn.kiev.ua .
The excitement of Kenyan players is at its peak at these online casinos in Kenya.
Ad usum proprium — Для собственного употребления.
I really love to read such an excellent article. Helpful article. Hello Administ .
Good info. Lucky me I reach on your website by accident, I bookmarked it.
Thank you for great article. Hello Administ .国产线播放免费人成视频播放
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.
Thank you great posting about essential oil. Hello Administ .
Kenyan players, experience the thrill of top-tier gaming at online casinos in Kenya.
Everything is very open and very clear explanation of issues. was truly information.国产线播放免费人成视频播放
Thank you for great content. Hello Administ.
toasterovensplus.com
読んでいてとても勉強になりました。いつも感謝しています。
Nice article inspiring thanks. Hello Administ . Website : https://www.fastlinks.com.tr/
Thank you great post. Hello Administ . Website : https://301.com.tr/
Thank you for great information. Hello Administ .
Kenyan gamers, explore the vast gaming options at the best online casinos in Kenya.
Kenyan players, witness the evolution of gaming at the best online casinos in Kenya.
qiyezp.com
추운 날씨도 열정을 멈출 수 없습니다.
sandyterrace.com
Zhu Houzhao는 심호흡을했습니다. “너무 많이 생각하지 마세요. 제가 당신을 보호하겠습니다.”
Everything is very open and very clear explanation of issues. was truly information.活婴儿色情片
Good info. Lucky me I reach on your website by accident, I bookmarked it. 現場兒童色情片
Nice article inspiring thanks. Hello Administ . StarzBet Website : https://starzbet.com/
Good info. Lucky me I reach on your website by accident, I bookmarked it. StarzBet Website : https://starzbet.com/
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.StarzBet Website : https://starzbet.com/
Thank you for great content. Hello Administ. StarzBet Website : https://starzbet.com/
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.StarzBet Website : https://starzbet.com/
Thank you for great article. Hello Administ .StarzBet Website : https://starzbet.com/
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.儿童色情片
1. Вибір натяжних стель: як вибрати ідеальний варіант?
2. Модні тренди натяжних стель на поточний сезон
3. Які переваги мають натяжні стелі порівняно зі звичайними?
4. Як підібрати кольори для натяжної стелі у квартирі?
5. Секрети догляду за натяжними стелями: що потрібно знати?
6. Як зробити вибір між матовими та глянцевими натяжними стелями?
7. Натяжні стелі в інтер’єрі: як вони змінюють приміщення?
8. Натяжні стелі для ванної кімнати: плюси та мінуси
9. Як підняти стеля візуально за допомогою натяжної конструкції?
10. Як вибрати правильний дизайн натяжної стелі для кухні?
11. Інноваційні технології виробництва натяжних стель: що варто знати?
12. Чому натяжні стелі вибирають для офісних приміщень?
13. Натяжні стелі з фотопринтом: які переваги цієї технології?
14. Дизайнерські рішення для натяжних стель: ідеї для втілення
15. Хімічні реагенти в складі натяжних стель: безпека та якість
16. Як вибрати натяжну стелю для дитячої кімнати: поради батькам
17. Які можливості для дизайну приміщень відкривають натяжні стелі?
18. Як впливає вибір матеріалу на якість натяжної стелі?
19. Інструкція з монтажу натяжних стель власноруч: крок за кроком
20. Натяжні стелі як елемент екстер’єру будівлі: переваги та недоліки
підвисні стелі natjazhnistelifvgtg.lviv.ua .
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.国产线播放免费人成视频播放
Thank you for great information. Hello Administ . 国产线播放免费人成视频播放
exprimegranada.com
この記事は本当に素晴らしい。心から感謝しています。
Идеальное решение для небольшой семьи
8. Дом из бруса 9х12: здоровый микроклимат
одноэтажный дом из бруса 9х12 https://domizbrusa9x12spb.ru/ .
I really love to read such an excellent article. Helpful article. Hello Administ . 国产线播放免费人成视频播放
воєнторг
15. Купить снаряжение для армии дешево
інтернет магазин військової форми військовий одяг інтернет магазин .
1. Почему берцы – это обязательный элемент стиля?
2. Как выбрать идеальные берцы для осеннего гардероба?
3. Тренды сезона: кожаные берцы или замшевые?
4. 5 способов носить берцы с платьем
5. Какие берцы выбрать для повседневного образа?
6. Берцы на платформе: комфорт и стиль в одном
7. Какие берцы будут актуальны в этом году?
8. Маст-хэв сезона: военные берцы в стиле милитари
9. 10 вариантов сочетания берцов с джинсами
10. Зимние берцы: как выбрать модель для холодного сезона
11. Элегантные берцы на каблуке: идеальный вариант для офиса
12. Секреты ухода за берцами: как сохранить первоначальный вид?
13. С какой юбкой носить берцы: советы от стилистов
14. Как подобрать берцы под фасон брюк?
15. Берцы на шнуровке: стильный акцент в образе
16. Берцы-челси: универсальная модель для любого стиля
17. С чем носить берцы на плоской подошве?
18. Берцы с ремешками: акцент на деталях
19. Как выбрать берцы для прогулок по городу?
20. Топ-5 брендов берцев: качество и стиль в одном
купити бєрци купити бєрци .
Nice article inspiring thanks. Hello Administ . Seo Hizmeti Skype : live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Hizmeti Skype : live:by_umut
Thank you for great information. Hello Administ . Seo Hizmeti Skype : live:by_umut
qiyezp.com
Fang Jifan의 관점에서 이것은 정상적인 것 이상입니다.
Thank you for great article. Hello Administ .国产线播放免费人成视频播放
Everything is very open and very clear explanation of issues. was truly information. Seo Hizmeti Skype : live:by_umut
Thank you for great article. Hello Administ .Seo Hizmeti Skype : live:by_umut
thebuzzerpodcast.com
그리고 Zhang Yuanxi는 그의 손에 활을 들고 있었지만 불행히도 활이 찢어졌습니다.
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across. Seo Hizmeti Skype : live:by_umut
exprimegranada.com
この実用的な記事のおかげで、多くのことを学べました。ありがとうございます。
Everything is very open and very clear explanation of issues. was truly information. Seo Hizmeti Skype : live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me. Seo Hizmeti Skype : live:by_umut
qiyezp.com
팡지판은 “그게 아니라 이 삼촌이 당신에게 진실을 말하고 싶어한다”고 말했다.
Thank you great posting about essential oil. Hello Administ .Seo Hizmeti Skype : live:by_umut
buysteriodsonline.com
증기 기관차는 점점 더 빠르게 움직이기 시작했습니다.
Подробный обзор
17. BMW: как выбрать идеальный двигатель для своего автомобиля
bmw x1 m x5 2023 .
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across. Seo Hizmeti Skype : live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Hizmeti Skype : live:by_umut
qiyezp.com
내시는 머뭇거리다, 한참을 머뭇거리다가 말했다. “그…그가 말하길…”
Thank you great post. Hello Administ .Seo Hizmeti Skype : live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader. Seo Hizmeti Skype : live:by_umut
Thank you great post. Hello Administ .Seo Hizmeti Skype : live:by_umut
кабель канал плинтус из алюминия .
game1kb.com
Zhang Mao조차도 안도의 한숨을 쉬었습니다. 결국이 아이는 꽤 현명합니다!
Great post thank you. Hello Administ . Seo Hizmeti Skype : live:by_umut
Thank you for great content. Hello Administ. Seo Hizmeti Skype : live:by_umut
usareallservice.com
素敵な記事をありがとうございます。大いに参考になりました!
Подробное руководство
2. Секреты монтажа гипсокартона: шаг за шагом инструкция
3. Гипсокартонные конструкции: основные виды и их преимущества
4. Как сэкономить при покупке гипсокартона: лучшие способы
5. Простые способы обработки гипсокартона: советы от профессионалов
6. Интересные идеи использования гипсокартона в интерьере
7. Все, что вам нужно знать о гипсокартоне: полезная информация
8. Гипсокартон: обзор популярных брендов и их характеристики
9. Плюсы и минусы гипсокартона: как правильно выбрать материал
10. Как сделать ровные стены с помощью гипсокартона: секреты и советы
11. Гипсокартонные потолки: виды и технологии монтажа
12. Декорирование гипсокартона: идеи для творческого подхода
13. Гипсокартон в дизайне интерьера: современные тренды и решения
14. Преимущества гипсокартона перед другими строительными материалами
15. Как выбрать правильный инструмент для работы с гипсокартоном
16. Гипсокартон: надежный материал для обустройства дома
17. Гипсокартон как элемент декора: необычные способы применения
18. Технологии монтажа гипсокартона: лучшие практические советы
19. История и развитие гипсокартона: открытия и достижения
20. Строительство с использованием гипсокартона: основные этапы и рекомендации
подвесные потолки строительные материалы купить .
qiyezp.com
Wang Shouren은 약간 혼란 스러웠습니다. 그런 사람이 회원이 될 수 있습니까?
коляска москва купить купить прогулочную коляску .
Amplificadores de senal gsm
Aumenta la intensidad de la senal de tu movil con un amplificador de calidad
https://neillopez23.wordpress.com/2024/01/27/mejora-tu-conexion-movil-con-nuestros-amplificadores-de-senal-amplificadormovil-es/
Good info. Lucky me I reach on your website by accident, I bookmarked it. 現場兒童色情片
Професійна чистка
5. Як уникнути проблем із яснами
стоматологія стоматологія .
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Hizmeti Skype : live:by_umut
Great post thank you. Hello Administ . Seo Hizmeti Skype : live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Hizmeti Skype : live:by_umut
Thank you for great content. Hello Administ. Seo Hizmeti Skype : live:by_umut
Thank you for great content. Hello Administ. 国产线播放免费人成视频播放
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Hizmeti Skype : live:by_umut
1. 10 лучших идей для дизайна интерьера
2. Топ-20 трендов в дизайне на 2021 год
3. Как выбрать идеальный цветовой акцент в дизайне
4. Секреты успешного дизайн-проекта
5. Дизайн нового поколения
6. Дизайн спальни
7. Дизайнерские решения для увеличения пространства в маленькой квартире
8. Природный дизайн
9. Основы дизайна
10. Дизайн-студия: секреты успешного бизнеса в сфере дизайна
11. Интересные факты о развитии дизайна в XXI веке
12. Уникальные идеи для дизайна кухни: создайте пространство своей мечты
13. Тенденции в сфере дизайна мебели: вдохновляющие идеи
14. Дизайн гостиной
15. Искусство минимализма: создание современного дизайна в своем доме
16. Дизайн сада: принципы оформления участка с учетом ландшафта
17. Декорирование дома с использованием текстиля: советы и идеи
18. Принципы цветового баланса в дизайне: как создать гармоничное пространство
19. Книги по дизайну
20. Дизайн подростковой комнаты
интерьеры квартир интерьеры квартир .
Thank you for great content. Hello Administ. 国产线播放免费人成视频播放
https://renewsaltwatertrick.com/
Thank you for great information. Hello Administ . 国产线播放免费人成视频播放
сплит купить https://split-sistema-kupit.ru/ .
fpparisshop.com
実用的な情報が豊富で、とても参考になる素晴らしい記事です。
https://thepinealxt.com/
сериал смотреть
sandyterrace.com
이어 팡지판은 “오늘 몸이 안 좋아서 시험 보기가 불편하다…”고 말했다.
Thank you for great article. Hello Administ .国产线播放免费人成视频播放
Thank you for great information. Hello Administ . Seo Hizmeti Skype : live:by_umut
Everything is very open and very clear explanation of issues. was truly information. Seo Hizmeti Skype : live:by_umut
Thank you for great content. Hello Administ. Seo Hizmeti Skype : live:by_umut
Everything is very open and very clear explanation of issues. was truly information. Seo Hizmeti Skype : live:by_umut
Thank you for great article. Hello Administ .Seo Hizmeti Skype : live:by_umut
Как установить оконный кондиционер: инструкция для начинающих
монтаж кондиционера цена монтаж кондиционера цена .
1. Как установить кондиционер в доме
обслуживание вентиляции обслуживание вентиляции .
Everything is very open and very clear explanation of issues. was truly information.活婴儿色情片
Great post thank you. Hello Administ . Seo Hizmeti Skype : live:by_umut
Amplificadores de senal gsm
Mejora la cobertura de tu movil con un amplificador de senal
https://www.4shared.com/u/vyu4wC6U/NeilLopez23.html
Thank you great post. Hello Administ .国产线播放免费人成视频播放
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.国产线播放免费人成视频播放
мульти спліт мульти спліт .
Great post thank you. Hello Administ . 国产线播放免费人成视频播放
Thank you for content. Area rugs and online home decor store. Hello Administ . 国产线播放免费人成视频播放
Good info. Lucky me I reach on your website by accident, I bookmarked it. 現場兒童色情片
Інноваційні технології в тактичних кросівках
тактичні чоловічі кросівки https://vijskovikrosivkifvgh.kiev.ua/ .
Thank you for great information. Hello Administ . 国产线播放免费人成视频播放
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.兒童色情
usareallservice.com
非常に興味深く読ませていただきました。素敵な内容です!
?Diviertete y gana en los casinos en linea de Peru!
mejor casino online peru mejor casino online peru .
?Siente la emocion del casino en linea en Peru!
mejor casino online peru mejor casino online peru .
Thank you for great article. Hello Administ .国产线播放免费人成视频播放
?Siente la emocion del casino en linea en Peru!
mejor casino online peru online casino games peru .
– Купить кран смеситель для ванной
шаровой кран https://krany-sharovye-nerzhaveyushie-msk.ru/ .
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.兒童色情
Everything is very open and very clear explanation of issues. was truly information.活婴儿色情片
Thank you for content. Area rugs and online home decor store. Hello Administ . 国产线播放免费人成视频播放
onair2tv.com
이 사람은 사람을 많이 죽였기 때문에 당연히 병을 치료한 경험이 풍부하다.
PBN sites
We will build a web of private blog network sites!
Advantages of our PBN network:
WE DO everything SO THAT Google doesn’t understand that this A PBN network!!!
1- We buy web domains from various registrars
2- The principal site is hosted on a VPS hosting (Virtual Private Server is high-speed hosting)
3- Other sites are on various hostings
4- We attribute a distinct Google account to each site with verification in Search Console.
5- We make websites on WP, we don’t employ plugins with aided by which Trojans penetrate and through which pages on your websites are generated.
6- We refrain from duplicate templates and utilise only distinct text and pictures
We do not work with website design; the client, if wanted, can then edit the websites to suit his wishes
I really love to read such an excellent article. Helpful article. Hello Administ . 国产线播放免费人成视频播放
Почему важен рейтинг букмекера
вход букмекерская рейтинг .
Thank you great posting about essential oil. Hello Administ . 国产线播放免费人成视频播放
Лучшие букмекеры в рейтинге
букмекерский сайт беларусь букмекерская контора .
Everything is very open and very clear explanation of issues. was truly information.活婴儿色情片
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.儿童色情片
Таблица рейтинга букмекеров
букмекерские приложения самая лучшая букмекерская контора в интернете .
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.国产线播放免费人成视频播放
sandyterrace.com
하지만 구이저우에서는 발이 차가워지면 일이 까다로울 것입니다.
Thank you great posting about essential oil. Hello Administ . 国产线播放免费人成视频播放
Nice article inspiring thanks. Hello Administ . 国产线播放免费人成视频播放
Які рекомендації варто враховувати
Провідники технологій
тактичний військовий рюкзак тактичний військовий рюкзак .
Thank you great post. Hello Administ .国产线播放免费人成视频播放
toasterovensplus.com
このブログはいつも私の知識を広げてくれます。大変感謝しています。
reasons for taking zofran
ilogidis.com
금은 산을 바라보며 사람들은 마침내 반응했습니다.
It’s a great post, I really congratulate you. 觀看兒童色情片
bestmanualpolesaw.com
예외 없이 이들은 홍치제의 오른팔이다.
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.儿童色情片
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
TornadoCash: Where privacy meets decentralization. Keep your Ethereum transactions confidential with this innovative protocol
fpparisshop.com
このトピックに関する他の記事とは一線を画しています。見事な分析です。
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Get Paid to Play Games in Kenya
best online casino games to win money real money online casinos .
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Play and Earn Real Money Online in Kenya
best online casino games kenya games that pay real money in kenya .
https://naganoleanbodytonic.fixions.com/
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
thephotoretouch.com
아무래도…홍지황제는 그다지 놀라지 않은 것 같군요…
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Understanding COSC Certification and Its Importance in Horology
COSC Certification and its Rigorous Standards
COSC, or the Controle Officiel Suisse des Chronometres, is the official Swiss testing agency that certifies the precision and precision of wristwatches. COSC certification is a sign of superior craftsmanship and reliability in chronometry. Not all watch brands seek COSC certification, such as Hublot, which instead sticks to its own strict standards with movements like the UNICO calibre, achieving similar accuracy.
The Science of Precision Chronometry
The central system of a mechanical timepiece involves the mainspring, which supplies energy as it loosens. This system, however, can be vulnerable to environmental elements that may influence its accuracy. COSC-validated movements undergo rigorous testing—over fifteen days in various conditions (5 positions, three temperatures)—to ensure their resilience and dependability. The tests assess:
Average daily rate precision between -4 and +6 secs.
Mean variation, peak variation levels, and impacts of temperature variations.
Why COSC Certification Is Important
For timepiece enthusiasts and connoisseurs, a COSC-certified watch isn’t just a item of tech but a demonstration to enduring excellence and accuracy. It represents a timepiece that:
Provides outstanding dependability and accuracy.
Ensures assurance of superiority across the complete design of the watch.
Is likely to retain its worth more effectively, making it a wise choice.
Famous Timepiece Brands
Several renowned manufacturers prioritize COSC accreditation for their watches, including Rolex, Omega, Breitling, and Longines, among others. Longines, for instance, provides collections like the Archive and Soul, which highlight COSC-certified movements equipped with advanced materials like silicon balance springs to boost resilience and performance.
Historic Background and the Evolution of Chronometers
The notion of the chronometer dates back to the need for precise chronometry for navigation at sea, emphasized by John Harrison’s work in the eighteenth century. Since the formal establishment of COSC in 1973, the validation has become a yardstick for judging the accuracy of luxury watches, sustaining a tradition of excellence in watchmaking.
Conclusion
Owning a COSC-validated watch is more than an visual choice; it’s a commitment to quality and accuracy. For those appreciating precision above all, the COSC accreditation offers peacefulness of mind, ensuring that each accredited timepiece will perform reliably under various conditions. Whether for personal satisfaction or as an investment, COSC-validated watches stand out in the world of watchmaking, bearing on a legacy of careful timekeeping.
賭網
обратиться к психологу https://w-495.ru/
яндекс услуги психолог москва https://w-495.ru/
психологическаЯ помощь в москве бесплатнаЯ https://w-495.ru/
психотерапевты москвы лучшие https://w-495.ru/
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
fpparisshop.com
この記事のおかげで、多くの実用的な知識を得ることができました。
Spin to Win Cash Prizes in Kenya
best online casino games kenya games that pay real money in kenya .
casibom giriş
Nihai Zamanın En Büyük Popüler Casino Platformu: Casibom
Bahis oyunlarını sevenlerin artık duymuş olduğu Casibom, en son dönemde adından genellikle söz ettiren bir bahis ve kumarhane web sitesi haline geldi. Ülkemizdeki en mükemmel casino web sitelerinden biri olarak tanınan Casibom’un haftalık olarak olarak değişen erişim adresi, alanında oldukça yeni olmasına rağmen güvenilir ve kazanç sağlayan bir platform olarak öne çıkıyor.
Casibom, yakın rekabeti olanları geride kalarak köklü casino web sitelerinin üstünlük sağlamayı başarıyor. Bu alanda eski olmak önemli olsa da, oyunculardan etkileşimde olmak ve onlara temasa geçmek da eş miktar önemli. Bu noktada, Casibom’un gece gündüz yardım veren canlı olarak destek ekibi ile rahatça iletişime temas kurulabilir olması önemli bir artı sağlıyor.
Hızla artan oyuncu kitlesi ile ilgi çekici Casibom’un arkasındaki başarı faktörleri arasında, yalnızca casino ve canlı casino oyunları ile sınırlı olmayan kapsamlı bir servis yelpazesi bulunuyor. Sporcular bahislerinde sunduğu kapsamlı seçenekler ve yüksek oranlar, oyuncuları ilgisini çekmeyi başarmayı sürdürüyor.
Ayrıca, hem atletizm bahisleri hem de casino oyunlar katılımcılara yönlendirilen sunulan yüksek yüzdeli avantajlı bonuslar da dikkat çekici. Bu nedenle, Casibom kısa sürede piyasada iyi bir reklam başarısı elde ediyor ve büyük bir katılımcı kitlesi kazanıyor.
Casibom’un kazanç sağlayan ödülleri ve tanınırlığı ile birlikte, web sitesine abonelik ne şekilde sağlanır sorusuna da değinmek elzemdir. Casibom’a taşınabilir cihazlarınızdan, bilgisayarlarınızdan veya tabletlerinizden internet tarayıcı üzerinden rahatça erişilebilir. Ayrıca, platformun mobil uyumlu olması da büyük önem taşıyan bir avantaj getiriyor, çünkü şimdi neredeyse herkesin bir akıllı telefonu var ve bu telefonlar üzerinden hızlıca giriş sağlanabiliyor.
Hareketli cihazlarınızla bile yolda canlı tahminler alabilir ve müsabakaları canlı olarak izleyebilirsiniz. Ayrıca, Casibom’un mobil uyumlu olması, ülkemizde kumarhane ve oyun gibi yerlerin kanuni olarak kapatılmasıyla birlikte bu tür platformlara erişimin büyük bir yolunu oluşturuyor.
Casibom’un güvenilir bir casino platformu olması da önemlidir bir fayda getiriyor. Belgeli bir platform olan Casibom, duraksız bir şekilde eğlence ve kazanç elde etme imkanı getirir.
Casibom’a üye olmak da oldukça basittir. Herhangi bir belge gereksinimi olmadan ve ücret ödemeden siteye kolayca abone olabilirsiniz. Ayrıca, platform üzerinde para yatırma ve çekme işlemleri için de birçok farklı yöntem mevcuttur ve herhangi bir kesim ücreti isteseniz de alınmaz.
Ancak, Casibom’un güncel giriş adresini takip etmek de gereklidir. Çünkü canlı iddia ve kumarhane web siteleri moda olduğu için sahte platformlar ve dolandırıcılar da görünmektedir. Bu nedenle, Casibom’un sosyal medya hesaplarını ve güncel giriş adresini düzenli aralıklarla kontrol etmek önemlidir.
Sonuç, Casibom hem itimat edilir hem de kar getiren bir casino web sitesi olarak dikkat çekiyor. Yüksek promosyonları, kapsamlı oyun seçenekleri ve kullanıcı dostu taşınabilir uygulaması ile Casibom, casino sevenler için ideal bir platform sunuyor.
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
https://us-ca-zencortex.com/
Что нужно знать перед посещением казино
казино олимп
Воєнторг
15. Подсумки и кобуры для дополнительного снаряжения
штани тактичні зимові https://voentorgklyp.kiev.ua/odyag/shtany/taktychni-shtany/ .
1. Вибір натяжної стелі: як правильно підібрати?
2. ТОП-5 переваг натяжних стель для вашого інтер’єру
3. Як доглядати за натяжною стелею: корисні поради
4. Натяжні стелі: модний тренд сучасного дизайну
5. Як вибрати кольорову гаму для натяжної стелі?
6. Натяжні стелі від А до Я: основні поняття
7. Комфорт та елегантність: переваги натяжних стель
8. Якість матеріалів для натяжних стель: що обрати?
9. Ефективне освітлення з натяжними стелями: ідеї та поради
10. Натяжні стелі у ванній кімнаті: плюси та мінуси
11. Як відремонтувати натяжну стелю вдома: поетапна інструкція
12. Візуальні ефекти з допомогою натяжних стель: ідеї дизайну
13. Натяжні стелі з фотопринтом: оригінальний дизайн для вашого інтер’єру
14. Готові або індивідуальні: які натяжні стелі обрати?
15. Натяжні стелі у спальні: як створити атмосферу затишку
16. Вигода та функціональність: чому варто встановити натяжну стелю?
17. Натяжні стелі у кухні: практичність та естетика поєднуються
18. Різновиди кріплень для натяжних стель: який обрати?
19. Комплектація натяжних стель: що потрібно знати при виборі
20. Натяжні стелі зі звукоізоляцією: комфорт та тиша у вашому будинку!
ціна натяжної стелі квадратний метр https://natyazhnistelidfvf.kiev.ua/ .
Обучение игре в казино
казино олимп
сериал смотреть полностью
로드스탁과의 레버리지 방식의 스탁: 투자 전략의 새로운 영역
로드스탁에서 제공하는 레버리지 스탁은 증권 투자의 한 방식으로, 큰 수익률을 목적으로 하는 투자자들을 위해 유혹적인 선택입니다. 레버리지를 사용하는 이 전략은 투자하는 사람들이 자신의 자금을 넘어서는 금액을 투자할 수 있도록 함으로써, 주식 시장에서 더 큰 영향력을 행사할 수 있는 기회를 공급합니다.
레버리지 방식의 스탁의 기본 원칙
레버리지 방식의 스탁은 원칙적으로 자본을 차입하여 사용하는 방식입니다. 사례를 들어, 100만 원의 투자금으로 1,000만 원 상당의 증권을 구매할 수 있는데, 이는 투자하는 사람이 기본 자본보다 훨씬 더욱 많은 증권을 구매하여, 주식 가격이 올라갈 경우 관련된 더 큰 이익을 획득할 수 있게 해줍니다. 하지만, 주식 가격이 떨어질 경우에는 그 손실 또한 커질 수 있으므로, 레버리지를 이용할 때는 신중하게 생각해야 합니다.
투자 전략과 레버리지 사용
레버리지는 특히 성장 가능성이 상당한 기업에 투입할 때 도움이 됩니다. 이러한 회사에 높은 비중으로 투입하면, 잘 될 경우 큰 이익을 가져올 수 있지만, 반대의 경우 상당한 리스크도 감수해야. 그렇기 때문에, 투자하는 사람은 자신의 위험성 관리 능력을 가진 장터 분석을 통해 통해, 어느 기업에 얼마만큼의 자금을 적용할지 선택해야 합니다.
레버리지 사용의 장점과 위험 요소
레버리지 방식의 스탁은 높은 이익을 약속하지만, 그만큼 상당한 위험도 따릅니다. 증권 장의 변화는 예측이 어렵기 때문에, 레버리지를 사용할 때는 항상 시장 동향을 세심하게 주시하고, 피해를 최소로 줄일 수 있는 전략을 세워야 합니다.
맺음말: 세심한 선택이 요구됩니다
로드스탁에서 공급하는 레버리지 방식의 스탁은 막강한 투자 수단이며, 적절히 사용하면 상당한 수익을 가져다줄 수 있습니다. 하지만 높은 위험성도 고려해야 하며, 투자 결정이 필요한 정보와 신중한 고려 후에 이루어져야 합니다. 투자자 본인의 금융 상황, 위험을 감수하는 능력, 그리고 시장 상황을 반영한 균형 잡힌 투자 계획이 핵심입니다.
ucie
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
tvlore.com
Hongzhi 황제는 깜짝 놀랐고 약 그릇을 내려 놓고 귀를 기울여 들었습니다.
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.儿童色情片
sandyterrace.com
이 비밀의 방에는 그의 앞에 악기가 전시되어 있었다.
thepinealxt.com
Какие игры самые прибыльные в казино
Правила и стратегии игры в казино
olimp casino
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Potent Links in Weblogs and Comments: Boost Your SEO
Links are essential for improving search engine rankings and raising site presence. By integrating links into weblogs and comments smartly, they can considerably increase visitors and SEO performance.
Adhering to Search Engine Algorithms
Today’s backlink placement methods are finely tuned to align with search engine algorithms, which now prioritize website link good quality and significance. This assures that links are not just numerous but meaningful, directing users to helpful and pertinent content material. Site owners should concentrate on integrating hyperlinks that are contextually proper and boost the general content high quality.
Rewards of Making use of Fresh Donor Bases
Making use of up-to-date donor bases for links, like those managed by Alex, offers significant rewards. These bases are frequently refreshed and comprise of unmoderated sites that don’t attract complaints, ensuring the links positioned are both influential and certified. This method will help in maintaining the effectiveness of backlinks without the risks associated with moderated or problematic sources.
Only Approved Resources
All donor sites used are authorized, avoiding legal pitfalls and adhering to digital marketing requirements. This dedication to making use of only sanctioned resources guarantees that each backlink is legitimate and trustworthy, thus constructing reliability and reliability in your digital existence.
SEO Impact
Skillfully put backlinks in blogs and comments provide more than just SEO rewards—they enhance user experience by connecting to relevant and high-quality content. This strategy not only fulfills search engine requirements but also engages users, leading to better traffic and improved online engagement.
In substance, the right backlink strategy, particularly one that utilizes fresh and reliable donor bases like Alex’s, can alter your SEO efforts. By focusing on high quality over quantity and sticking to the newest standards, you can guarantee your backlinks are both powerful and effective.
Лучшие игры и высокие коэффициенты в онлайн казино Беларуси
онлайн казино Беларусь лучшие онлайн казино в Беларуси .
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Здравствуйте!
Гибкий маршрут и персонализированный подход
Индивидуальные экскурсии по Калининградской области предоставляют уникальную возможность создать гибкий маршрут, адаптированный под ваши предпочтения и интересы. В отличие от стандартных групповых туров, где участники ограничены общим расписанием, индивидуальные экскурсии позволяют вам самостоятельно выбирать места, которые вы хотели бы посетить, и проводить на них столько времени, сколько посчитаете нужным.
Этот персонализированный подход является одним из ключевых преимуществ индивидуальных экскурсий. Вы можете организовать свой день так, чтобы посетить как можно больше интересующих вас достопримечательностей или же сфокусироваться на изучении конкретного объекта более детально. Благодаря этому вы получите максимум удовольствия от путешествия, ощущая полный контроль над его ходом.
Кроме того, индивидуальные экскурсии позволяют вам наслаждаться путешествием в удобном темпе. Вы можете делать перерывы и отдыхать в тех местах, которые вас привлекают, и проводить время в компании близких или друзей, не беспокоясь о том, что нужно догнать группу или уложиться в строгий график.
Наши индивидуальные экскурсии по Калининградской области разработаны с учетом ваших потребностей и желаний. Мы предлагаем разнообразные маршруты, которые охватывают как известные туристические достопримечательности, так и скрытые жемчужины региона. Наши опытные гиды помогут вам раскрыть все тайны этого удивительного места и создадут для вас незабываемый опыт.
Желаете узнать больше о наших индивидуальных экскурсиях по Калининградской области? Посетите наш сайт https://topkaliningrad.ru и выберите программу, которая подходит именно вам. Перейдите по ссылке, чтобы начать свое приключение по захватывающим местам этого уникального региона.
гид по Калининграду с машиной
гид по Калининграду и Калининградской области
индивидуальные экскурсии в Калининграде
Калининградская область экскурсии
экскурсии Калининграда и Калининградской области
экскурсия Калининград индивидуальная
Удачи и хорошего визита в Калининград!
Познакомьтесь с новыми игровыми автоматами в онлайн казино Беларусь
онлайн казино Беларусь онлайн казино Беларусь .
фильм в хорошем качестве
проверить свои usdt на чистоту
Проверка кошельков кошелька по присутствие незаконных финансовых средств: Обеспечение безопасности личного криптовалютного портфельчика
В мире электронных денег становится все существеннее соблюдать секретность собственных активов. Ежедневно кибермошенники и криминальные элементы выработывают совершенно новые подходы обмана и мошенничества и угонов электронных средств. Ключевым инструментом важных способов обеспечения является проверка кошелька по выявление нелегальных средств передвижения.
Почему именно поэтому важно и проверять собственные цифровые кошельки для хранения электронных денег?
Прежде всего это обязательно для охраны своих средств. Большинство люди, вкладывающие деньги сталкиваются с риском утраты своих собственных финансовых средств из-за недоброжелательных планов или воровства. Анализ кошельков для хранения криптовалюты способствует предотвращению выявить вовремя подозрительные действия и предотвратить возможные.
Что предоставляет организация?
Мы предлагаем сервис проверки данных криптовалютных кошельков и транзакций средств с целью обнаружения источника средств и выдачи подробного отчета о проверке. Наши система проанализировать информацию для идентификации незаконных манипуляций и определить уровень риска для того, чтобы своего портфеля. Благодаря нашей системе проверки, вы сможете предотвратить возможные проблемы с органами контроля и защитить от непреднамеренного вовлечения в финансировании незаконных деятельностей.
Как осуществляется проверка?
Организация наша фирма сотрудничает с крупными аудиторами фирмами, такими как Kudelsky Security, для того чтобы обеспечить и точность наших анализов. Мы применяем новейшие и подходы проверки данных для обнаружения подозрительных действий. Личные данные наших заказчиков обрабатываются и хранятся в базе в соответствии высокими стандартами безопасности и конфиденциальности.
Основная просьба: “проверить свои USDT на чистоту”
Если вы хотите убедиться в безопасности ваших USDT кошельков, наши специалисты предлагает шанс бесплатный анализ первых 5 кошельков. Достаточно просто свой кошелек в соответствующее поле на нашем сайте, и мы передадим вам детальный отчет о статусе вашего кошелька.
Обезопасьте свои активы уже сегодня!
Избегайте риска оказаться в жертвой хакеров или попасть неприятной ситуации нелегальных сделок с вашими личными средствами. Позвольте себе профессиональным консультантам, которые смогут помочь, вам и вашим деньгам защититься криптовалютные активы и предотвратить возможные проблемы. Предпримите первый шаг к обеспечению безопасности обеспечению безопасности вашего криптовалютного портфеля сразу же!
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
toasterovensplus.com
この記事から多くのインスピレーションを受けました。ありがとうございます。
Осмотр Tether на чистоту: Как обезопасить личные цифровые финансы
Постоянно все больше граждан обращают внимание к секурити их цифровых активов. Ежедневно шарлатаны предлагают новые способы хищения электронных средств, и также держатели цифровой валюты становятся жертвами их афер. Один из техник охраны становится проверка кошельков в наличие незаконных денег.
Зачем это полезно?
Преимущественно, для того чтобы сохранить личные средства от дельцов а также похищенных монет. Многие инвесторы сталкиваются с риском утраты своих активов в результате хищных планов или краж. Анализ бумажников способствует обнаружить подозрительные действия и также предотвратить возможные убытки.
Что мы предлагаем?
Наша компания предлагаем услугу проверки криптовалютных кошельков а также операций для выявления источника денег. Наша платформа проверяет информацию для выявления незаконных действий а также проценки риска для вашего портфеля. Вследствие этой проверке, вы сможете избежать проблем с регулированием а также защитить себя от участия в незаконных переводах.
Каким образом это работает?
Наша команда сотрудничаем с первоклассными проверочными фирмами, например Cure53, с целью гарантировать точность наших тестирований. Мы применяем новейшие технологии для обнаружения опасных сделок. Ваши данные обрабатываются и сохраняются согласно с высокими стандартами безопасности и конфиденциальности.
Как выявить личные Tether в чистоту?
При наличии желания проверить, что ваши Tether-бумажники чисты, наш сервис предлагает бесплатную проверку первых пяти кошельков. Просто вбейте местоположение личного бумажника на на нашем веб-сайте, и мы предоставим вам подробный отчет о его положении.
Обезопасьте вашими активы прямо сейчас!
Не рискуйте подвергнуться дельцов или оказаться в неприятную ситуацию по причине нелегальных операций. Свяжитесь с нашему агентству, чтобы обезопасить ваши электронные средства и предотвратить проблем. Примите первый шаг к безопасности вашего криптовалютного портфеля прямо сейчас!
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Проверка USDT в чистоту: Каким образом сохранить свои криптовалютные состояния
Все больше индивидуумов придают важность в надежность собственных электронных средств. День ото дня шарлатаны разрабатывают новые схемы разграбления электронных денег, и держатели электронной валюты становятся пострадавшими их интриг. Один способов охраны становится проверка бумажников для присутствие незаконных финансов.
Зачем это полезно?
В первую очередь, с тем чтобы защитить личные средства от шарлатанов или украденных монет. Многие вкладчики сталкиваются с риском убытков личных фондов в результате мошеннических сценариев или кражей. Проверка кошельков способствует обнаружить подозрительные транзакции а также предотвратить потенциальные убытки.
Что наша команда предлагаем?
Мы предлагаем подход анализа цифровых кошельков или транзакций для обнаружения происхождения денег. Наша система анализирует информацию для обнаружения нелегальных транзакций и оценки риска для вашего счета. Вследствие данной проверке, вы сможете избегнуть проблем с регулированием или обезопасить себя от участия в незаконных сделках.
Как это действует?
Наша команда сотрудничаем с лучшими проверочными агентствами, такими как Cure53, чтобы обеспечить прецизионность наших проверок. Мы применяем передовые технологии для определения потенциально опасных операций. Ваши данные обрабатываются и сохраняются согласно с высокими стандартами безопасности и приватности.
Каким образом проверить свои Tether в чистоту?
Если вам нужно проверить, что ваша USDT-кошельки чисты, наш сервис предоставляет бесплатную проверку первых пяти кошельков. Просто вбейте адрес личного кошелька на на нашем веб-сайте, и наша команда предоставим вам подробный отчет об его статусе.
Охраняйте вашими активы прямо сейчас!
Избегайте риска подвергнуться обманщиков или оказаться в неприятную обстановку по причине нелегальных операций. Обратитесь за помощью к нашему агентству, для того чтобы предохранить ваши электронные финансовые ресурсы и предотвратить сложностей. Совершите первый шаг к сохранности вашего криптовалютного портфеля уже сегодня!
грязный usdt
Проверка Tether в прозрачность: Каким образом сохранить личные цифровые средства
Все больше пользователей заботятся для безопасность собственных криптовалютных финансов. День ото дня шарлатаны разрабатывают новые методы кражи цифровых средств, и держатели электронной валюты являются пострадавшими своих подстав. Один из техник охраны становится проверка кошельков для наличие нелегальных денег.
С каким намерением это необходимо?
В первую очередь, чтобы обезопасить личные активы от шарлатанов или украденных денег. Многие вкладчики встречаются с риском потери их фондов по причине мошеннических планов или хищений. Тестирование кошельков помогает выявить подозрительные операции или предотвратить возможные убытки.
Что наша группа предоставляем?
Мы предлагаем подход проверки цифровых кошельков а также операций для выявления источника средств. Наша система анализирует информацию для определения противозаконных операций и также оценки угрозы для вашего портфеля. За счет такой проверке, вы сможете избежать проблем с регулированием а также защитить себя от участия в нелегальных сделках.
Как это работает?
Мы сотрудничаем с ведущими аудиторскими организациями, наподобие Certik, с целью предоставить точность наших проверок. Мы применяем передовые технологии для выявления опасных операций. Ваши данные обрабатываются и хранятся в соответствии с высокими стандартами безопасности и приватности.
Каким образом проверить собственные Tether в чистоту?
В случае если вы желаете проверить, что ваши Tether-кошельки нетронуты, наш сервис обеспечивает бесплатную проверку первых пяти бумажников. Просто введите адрес собственного кошелька на на сайте, или мы предоставим вам подробный доклад об его положении.
Защитите вашими активы прямо сейчас!
Не подвергайте опасности стать жертвой мошенников или попадать в неприятную ситуацию из-за противозаконных транзакций. Обратитесь к нашему сервису, чтобы защитить ваши криптовалютные финансовые ресурсы и предотвратить неприятностей. Примите первый шаг к сохранности вашего криптовалютного портфеля прямо сейчас!
Как убедиться в чистоте USDT
Проверка кошельков кошелька за наличие неправомерных средств передвижения: Охрана личного криптовалютного финансового портфеля
В мире цифровых валют становится все значимее все более необходимо соблюдать защиту личных финансов. Постоянно жулики и хакеры выработывают новые подходы обмана и мошенничества и кражи виртуальных финансов. Ключевым инструментом важных методов обеспечения безопасности является проверка данных кошельков для хранения криптовалюты за присутствие незаконных денег.
Почему поэтому важно осмотреть собственные электронные кошельки для хранения электронных денег?
В первую очередь, вот это обстоятельство необходимо для защиты своих средств. Многие пользователи рискуют потери средств своих денег в результате недобросовестных планов или угонов. Анализ кошельков для хранения криптовалюты способствует выявить вовремя сомнительные манипуляции и предотвратить.
Что предлагает компания?
Мы предоставляем послугу проверки кошельков криптовалютных кошельков и переводов с целью выявления происхождения денег и выдачи полного доклада. Наша платформа осматривает данные для идентификации потенциально нелегальных операций и оценить риск для того чтобы вашего портфеля активов. Благодаря нашей системе проверки, вы будете способны предотвратить с государственными органами и защитить от случайной вовлеченности в финансировании незаконных деятельностей.
Как проводится процесс проверки?
Наши фирма работает с крупными аудиторскими организациями организациями, вроде Halborn, чтобы обеспечить и адекватность наших анализов. Мы внедряем современные технологии и методики анализа для идентификации потенциально опасных операций. Персональные данные наших клиентов обрабатываются и хранятся в специальной базе данных в соответствии с положениями высокими стандартами безопасности и конфиденциальности.
Ключевой запрос: “проверить свои USDT на чистоту”
Если вас интересует убедиться в надежности своих USDT-кошельков, наши эксперты предоставляет возможность исследовать бесплатный анализ первых 5 кошельков. Достаточно просто адрес своего кошелька в соответствующее окно на нашем сайте проверки, и мы дадим вам подробные сведения о состоянии вашего кошелька.
Защитите свои финансовые средства уже сегодня!
Избегайте риска попасть жертвой мошенников злоумышленников или оказаться неприятной ситуации неправомерных операций с вашими деньгами. Позвольте себе профессиональным консультантам, которые смогут помочь, вам и вашему бизнесу защититься криптовалютные активы и предотвратить возможные проблемы. Примите первый шаг к обеспечению безопасности защите вашего электронного портфеля активов сразу же!
Regards, Numerous info.
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Доброго!
Откройте для себя Калининград и его окрестности с командой экспертов по местным достопримечательностям! Наши индивидуальные экскурсии предлагают неповторимый опыт, адаптированный под ваши интересы и пожелания. Наши частные гиды – профессионалы с аккредитацией, готовые поделиться глубокими знаниями и страстью к этому региону. Путешествуйте с комфортом и удобством в наших автомобилях, ощущая свободу и гибкость в планировании маршрута. Мы предлагаем уникальные маршруты, включающие как известные достопримечательности, так и скрытые жемчужины Калининградской области. Благодаря нашему опыту и знаниям, вы получите максимум удовольствия и полезной информации о месте. Забудьте о стрессе организации путешествия – доверьтесь профессионалам, и наслаждайтесь каждым моментом вашего пребывания. Приглашаем вас присоединиться к нам и открыть для себя новые горизонты вместе с https://topkaliningrad.ru
Калининград экскурсии индивидуальные на автомобиле
индивидуальные экскурсии в Калининграде на машине цена
частный гид по Калининградской области
гиды в Калининграде на машине индивидуальные туры
экскурсии по фортам Калининграда
экскурсия по Калининграду
Удачи и хорошего визита в Калининград!
USDT – является неизменная цифровая валюта, связанная к валюте страны, подобно доллар США. Это делает данный актив в особенности привлекательной у инвесторов, поскольку данный актив предоставляет надежность курса в в условиях неустойчивости рынка цифровых активов. Впрочем, как и любая другая форма цифровых активов, USDT подвержена опасности использования для скрытия происхождения средств и субсидирования неправомерных сделок.
Отмывание денег через криптовалюты переходит в все более и более широко распространенным путем для того чтобы скрытия происхождения средств. Воспользовавшись разносторонние методы, мошенники могут пытаться промывать незаконно добытые фонды посредством сервисы обмена криптовалют или миксеры, чтобы осуществить процесс их происхождение менее прозрачным.
Поэтому, экспертиза USDT на чистоту становится весьма важной практикой защиты с целью участников цифровых валют. Доступны для использования специализированные услуги, какие выполняют экспертизу операций и бумажников, для того чтобы определить подозрительные сделки и противоправные источники средств. Такие сервисы помогают пользователям устранить непреднамеренного вовлечения в преступных действий и предотвратить блокировку счетов со со стороны сторонних регуляторных органов.
Проверка USDT на чистоту также способствует предохранить себя от потенциальных финансовых потерь. Владельцы могут быть убеждены в том их капитал не ассоциированы с нелегальными сделками, что уменьшает вероятность блокировки аккаунта или конфискации средств.
Таким образом, в условиях растущей сложности среды криптовалют важно принимать действия для обеспечения безопасности и надежности своих финансовых ресурсов. Анализ USDT на чистоту с использованием специализированных платформ становится одним из вариантов защиты от незаконной деятельности, гарантируя пользователям цифровых валют дополнительный уровень и безопасности.
Проверка USDT на чистоту
Анализ Тетер в чистоту: Каким образом защитить свои цифровые средства
Каждый день все больше пользователей придают важность к надежность своих криптовалютных активов. Постоянно дельцы разрабатывают новые подходы разграбления цифровых денег, и держатели криптовалюты являются жертвами их афер. Один методов охраны становится тестирование кошельков в наличие нелегальных средств.
С какой целью это важно?
Преимущественно, для того чтобы обезопасить свои средства против обманщиков или украденных монет. Многие участники сталкиваются с риском потери своих финансов в результате хищных схем или грабежей. Проверка кошельков помогает выявить подозрительные транзакции или предотвратить потенциальные потери.
Что мы предлагаем?
Мы предлагаем подход тестирования цифровых бумажников и транзакций для выявления происхождения денег. Наша технология исследует данные для обнаружения противозаконных операций и также оценки угрозы для вашего портфеля. За счет такой проверке, вы сможете избежать проблем с регуляторами а также обезопасить себя от участия в противозаконных сделках.
Как это действует?
Мы сотрудничаем с передовыми проверочными организациями, вроде Kudelsky Security, для того чтобы предоставить прецизионность наших проверок. Мы применяем передовые техники для выявления опасных транзакций. Ваши данные проходят обработку и сохраняются в соответствии с высокими нормами безопасности и конфиденциальности.
Как проверить собственные USDT для прозрачность?
Если хотите проверить, что ваши USDT-кошельки чисты, наш подход обеспечивает бесплатное тестирование первых пяти кошельков. Просто введите положение собственного кошелька на нашем сайте, и также наша команда предоставим вам подробный отчет о его положении.
Охраняйте вашими активы сегодня же!
Не подвергайте опасности попасть в жертву обманщиков или попасть в неприятную ситуацию вследствие незаконных сделок. Обратитесь к нашему агентству, для того чтобы сохранить свои электронные финансовые ресурсы и предотвратить проблем. Сделайте первый шаг для безопасности вашего криптовалютного портфеля прямо сейчас!
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Осмотр USDT в прозрачность: Каким образом обезопасить свои цифровые активы
Постоянно все больше граждан обращают внимание к секурити своих криптовалютных финансов. Каждый день дельцы придумывают новые методы кражи криптовалютных денег, и собственники электронной валюты являются страдающими их афер. Один подходов обеспечения безопасности становится проверка кошельков для присутствие противозаконных средств.
Для чего это необходимо?
Прежде всего, с тем чтобы защитить личные активы от мошенников и также похищенных монет. Многие вкладчики сталкиваются с риском потери своих фондов из-за мошеннических механизмов или краж. Тестирование кошельков помогает выявить подозрительные транзакции а также предотвратить возможные убытки.
Что мы предлагаем?
Наша компания предоставляем сервис проверки электронных кошельков а также транзакций для выявления источника фондов. Наша система исследует данные для выявления нелегальных транзакций а также оценки риска для вашего счета. За счет этой проверке, вы сможете избежать проблем с регуляторами и также защитить себя от участия в незаконных операциях.
Как это работает?
Наша команда сотрудничаем с передовыми аудиторскими компаниями, вроде Certik, с целью гарантировать точность наших проверок. Наша команда применяем передовые технологии для обнаружения опасных транзакций. Ваши информация обрабатываются и сохраняются в соответствии с высокими стандартами безопасности и конфиденциальности.
Как проверить свои USDT в нетронутость?
Если хотите подтвердить, что ваша Tether-кошельки прозрачны, наш сервис обеспечивает бесплатную проверку первых пяти кошельков. Просто введите положение личного бумажника на на нашем веб-сайте, и также наша команда предоставим вам детальный доклад о его положении.
Обезопасьте вашими средства сегодня же!
Избегайте риска попасть в жертву шарлатанов или попасть в неприятную ситуацию из-за незаконных операций. Посетите нашему сервису, для того чтобы защитить ваши криптовалютные средства и предотвратить проблем. Совершите первый шаг для сохранности вашего криптовалютного портфеля уже сегодня!
thebuzzerpodcast.com
Fang Jifan은 약간 흥분하여 쪼그리고 앉았습니다. “내가 직접 파겠습니다.”
Thank you for great content. Hello Administ. 国产线播放免费人成视频播放
the-seroleans.com
cá cược thể thao
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
}
טלגראס כיוונים
שרף מדריך: המדריש המלא לסחר פרחי קנאביס במקום הטלגרמה
פרח כיוונים היא אתר מסמכים ומשלחי להשקיה קנאביס באמצעות היישומון המובילה מסר.
האתר סופק את כלל המידע הקישורים לאתרים והמידעים העדכוני לקבוצות וערוצים הנבחרים מומלצים לביקור לרכישת קנאביס בהטלגרמה בארץ ישראל.
כמו למעשה, אתר האינטרנט מציעה הדרכה מפורט לאיך להתקשר בהשרף ולקנה שרף בקלות הזמנה ובמהירות התגובה.
בעזרת המדריך, גם כן המשתמשים חדשים בתחום יוכלו להיכנס להמרחב השרף בטלגרם בצורה מאובטחת ובטוחה.
ההרובוט של השרף מאפשר למשתמשי הערוץ לבצע פעולות המבוצעות שונות כמו כן רכישת קנאביס, קבלת הודעה סיוע מקצועי, בדיקת הקיימות והוספת ביקורות על המצרים. כל זאת בפני פשוטה וקלה דרך התוכנה.
כאשר כאשר מדובר בשיטות ה התשלום, טלגראס משתמשת בשיטות ה מוכרות כגון מזומנים, כרטיסי אשראי וקריפטומונדה. חיוני ללציין כי ישנה לבדוק ולוודא את התקנות והחוקים האזוריים בארץ שלך ללפני התבצעות רכישה.
הטלגרמה מציע יתרונות ראשיים כמו כן פרטיות וביטחון אישי מוגברים, השיחה מהירה וגמישות גבוהה מאוד. בנוסף, הוא מאפשר כניסה לקהילה גלובלית רחבה ומציע מגוון של תכונות ויכולות.
בסיכום, המסר מסמכים היא האתר הטוב ללמצוא את כל המידע והקישורות לקניית שרף בפני מהירה, בבטוחה ונוחה מאוד דרך הטלגרמה.
הימורים אונליין הם חוויות מרגשות ופופולרי ביותר בעידן הדיגיטלי, שמאגרת מיליונים אנשים מכל
כל רחבי העולם. ההימורים המקוונים מתנהלים על אירועים ספורט, תוצאות פוליטיות ואפילו תוצאות מזג האוויר ונושאים נוספים. אתרי הימורים הווירטואליים מזמינים את המשתתפים להימר על תוצאות אפשרות ולהנות רגעים מרגשים ומהנים.
ההימורים המקוונים הם כבר חלק חשוב מתרבות החברה מזמן רב והיום הם לא רק רק חלק חשוב מהפעילות התרבותית והכלכלית, אלא כמו כן מספקים הכנסות וחוויות מרתקות. משום שהם נגישים לכולם ונוחים לשימוש, הם מתאימים לכל מהניסיון ולהנות מכל הניצחונות והפרסים בכל זמן ובכל מקום.
טכנולוגיות מתקדמות והימורים מקוונים הפכו להיות מעניינת ונפוצה. מיליוני אנשים מכל כל רחבי העולם מעוניינים בהימורים, כוללים הימורי ספורט. הימורים מקוונים מציעים למשתתפים חוויה רגשית ומרתקת, המאפשרת להם ליהנות מפעילות פופולרית זו בכל זמן ובכל מקום.
וכן מה עוד אתה מחכה למה? הצטרף עכשיו והתחיל ליהנות מכל רגע ורגע מהמשחקים ברשת.
Thank you great post. Hello Administ .国产线播放免费人成视频播放
Backlink pyramid
Sure, here’s the text with spin syntax applied:
Link Structure
After numerous updates to the G search mechanism, it is required to apply different approaches for ranking.
Today there is a way to draw the focus of search engines to your site with the support of inbound links.
Backlinks are not only an efficient promotional instrument but they also have organic visitors, immediate sales from these resources perhaps will not be, but transitions will be, and it is advantageous traffic that we also receive.
What in the end we get at the final outcome:
We present search engines site through backlinks.
Prluuchayut organic transitions to the site and it is also a signal to search engines that the resource is used by people.
How we show search engines that the site is liquid:
Backlinks do to the principal page where the main information.
We make links through redirections trusted sites.
The most IMPORTANT we place the site on sites analytical tools distinct tool, the site goes into the memory of these analyzers, then the obtained links we place as redirects on weblogs, discussion boards, comments. This important action shows search engines the MAP OF THE SITE as analysis tool sites present all information about sites with all key terms and headlines and it is very GOOD.
All information about our services is on the website!
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
us-ca-fitspresso.com/
fpparisshop.com
この記事の情報は非常に役に立ちます。ありがとうございます。
İstanbul fuar hostesi konusunda güvenebileceğiniz ender firmalardan bir tanesi
geinoutime.com
이런 일은 지저분한 계정입니다. 궁전의 미래가 평화롭지 않을까 두렵습니다.
Creating exclusive articles on Medium and Telegraph, why it is vital:
Created article on these resources is better ranked on less common queries, which is very significant to get organic traffic.
We get:
organic traffic from search algorithms.
organic traffic from the in-house rendition of the medium.
The platform to which the article refers gets a link that is profitable and increases the ranking of the webpage to which the article refers.
Articles can be made in any amount and choose all less frequent queries on your topic.
Medium pages are indexed by search algorithms very well.
Telegraph pages need to be indexed separately indexer and at the same time after indexing they sometimes occupy spots higher in the search engines than the medium, these two platforms are very beneficial for getting traffic.
Here is a link to our services where we present creation, indexing of sites, articles, pages and more.
Link building is simply as efficient currently, only the tools to work in this field have changed.
You can find numerous options regarding backlinks, our team utilize several of them, and these methods operate and have been tried by us and our clients.
Lately we carried out an test and we found that low-frequency search queries from one website rank effectively in online searches, and this doesn’t have to be your personal domain name, you can utilize social networks from web2.0 series for this.
It is also possible to partly move weight through website redirects, offering an assorted link profile.
Visit to our own site where our company’s solutions are typically offered with comprehensive overview.
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
thewiin.com
“모르겠어요.” Yang Biao는 떨리고 불쌍하게 말했습니다.
You expressed it really well.|
Everything You Need to Know
2. Aviator Games: Test Your Flying Skills in this Exciting Challenge
3. Get Ready to Soar: Aviator Games for Thrill Seekers
4. Master the Sky: Aviator Games for Aviation Enthusiasts
5. Take Flight with Aviator Games: A High-Flying Adventure
6. Challenge Yourself with Aviator Games: Are You Ready to Take On the Sky?
7. The Sky’s the Limit: Aviator Games for Daredevils
8. Aviator Games: The Perfect Way to Experience the Thrill of Flying
9. Fly High with Aviator Games: An Exciting Journey Awaits
10. Unleash Your Inner Pilot: Aviator Games for Flying Enthusiasts
11. Reach New Heights with Aviator Games: The Sky Awaits
12. Aviator Games: A Test of Skill and Courage in the Sky
13. Take to the Skies with Aviator Games: A Thrilling Adventure Awaits
14. Aviator Games: Where Every Landing is a Victory
15. Ready for Takeoff: Aviator Games for the Brave and Bold
16. Conquer the Clouds with Aviator Games: A Challenge Like No Other
17. Aviator Games: Prepare for a High-Flying Experience
18. Fly Like a Pro with Aviator Games: The Sky’s the Limit
19. Aviator Games: The Ultimate Test for Aspiring Pilots
20. Soar to New Heights with Aviator Games: Are You Ready for the Challenge?
juego del aviator aviator juego casino .
1. The Ultimate Aviator Games Guide
juego del avion casino juego del aviator .
casino online
SightCare formula aims to maintain 20/20 vision without the need for any surgical process. This supplement is a perfect solution for people facing issues as they grow older. https://sightcare-web.com/
Backlink creation is simply as effective now, only the instruments for working in this field have altered.
There are numerous choices to backlinks, our team utilize several of them, and these strategies operate and are actually examined by us and our clientele.
Recently our company performed an test and it turned out that less frequent search queries from just one domain name position well in search results, and it doesnt require to be your own website, you are able to use social networking sites from web2.0 series for this.
It is also possible to partly move mass through web page redirects, offering a diverse backlink profile.
Go to our very own website where our own solutions are provided with thorough descriptions.
Здравствуйте!
Откройте дверь к миру выгодных покупок с нашим онлайн-сервисом купонов и промокодов! Мы предлагаем широкий выбор акций и специальных предложений от ваших любимых магазинов, помогая вам сэкономить на всем, от товаров для дома до моды и электроники. Наш удобный поиск и актуальные обновления помогут вам быстро найти лучшие предложения и использовать их перед покупкой. Подписывайтесь на наши уведомления, чтобы быть в курсе последних акций и получать доступ к эксклюзивным скидкам. С нами вы всегда будете на шаг впереди, готовые сэкономить больше каждый раз!
Сайт самых свежих и проверенных купонов магазина City.com http://maxpromokod.ru
Доступные промокоды Lacywear ограниченная серия
Лучшие промокоды Reima vip варианты
Горячие промокоды Dresslily.com WW для онлайн-покупок
Экономичные промокоды Loccitane список
Выгодные промокоды mothercare.ru список
Промокоды Wer.ru на сегодня
Удачных покупок!
откупиться от сво
С началом СВО уже спустя полгода была объявлена первая волна мобилизации. При этом прошлая, в последний раз в России была аж в 1941 году, с началом Великой Отечественной Войны. Конечно же, желающих отправиться на фронт было не много, а потому люди стали искать способы не попасть на СВО, для чего стали покупать справки о болезнях, с которыми можно получить категорию Д. И все это стало возможным с даркнет сайтами, где можно найти практически все что угодно. Именно об этой отрасли темного интернета подробней и поговорим в этой статье.
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Доброго любители шоппинга!
Откройте для себя безграничный мир скидок с нашим онлайн-сервисом купонов и промокодов! Мы предлагаем огромный выбор выгодных предложений от различных магазинов, помогая вам сэкономить на покупках всего, от модной одежды до бытовой техники. Наш удобный интерфейс и актуальные обновления позволят вам легко найти самые выгодные предложения и использовать промокоды для максимальной экономии. Подписывайтесь на наши уведомления, чтобы всегда быть в курсе последних акций и получать доступ к эксклюзивным скидкам. С нами вы сможете сделать покупки еще более приятными и выгодными!
Сайт самых свежих и проверенных промокодов магазина Tinydeal WW http://maxpromokod.ru
Экономичные промокоды VICHY список
Промокоды интернет магазина Zarina супер скидки
Эффективные промокоды Zaful WW список
Свежие промокоды Bebakids онлайн
Привлекательные промокоды Acoola свежие и актуальные
Эксклюзивные промокоды KARATOV RU онлайн
Удачных покупок!
k8 カジノ パチンコ
実践的な知識が満載で、非常に価値のある記事でした。
renewsaltwatertrick.com
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
game1kb.com
수천가지의 생각이 이 순간…완전히 폭발했다.
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
36. Клининг Челябинск специализируется на ежедневной уборке кафе и ресторанов, включая уборку столов, мойку посуды, вытирание поверхностей и другие работы для поддержания чистоты и гигиены в заведении.
Клининг Челябинск .
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
WeJiJ is here to help get you the best gaming setup, gaming PC and guide you through the games you like to play with news, reviews and guides. https://wejij.com/
Find the latest technology news and expert tech product reviews. Learn about the latest gadgets and consumer tech products for entertainment, gaming, lifestyle and more. https://axget.com/
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
KeraBiotics is a meticulously-crafted natural formula designed to help people dealing with nail fungus. This solution, inspired by a sacred Amazonian barefoot tribe ritual https://kerabiotics-web.com/
– Shoot MASSIVE Loads For An Amazing Finish! https://semenax-try.com/
ZenCortex Research’s contains only the natural ingredients that are effective in supporting incredible hearing naturally.A unique team of health and industry professionals dedicated to unlocking the secrets of happier living through a healthier body. https://zencortex-try.com/
Serolean, a revolutionary weight loss supplement, zeroes in on serotonin—the key neurotransmitter governing mood, appetite, and fat storage. https://serolean-web.com/
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
MenoPhix is a menopause relief supplement featuring a blend of plant extracts to target the root cause of menopause symptoms. https://menophix-web.com/
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
BalMorex Pro is an exceptional solution for individuals who suffer from chronic joint pain and muscle aches. With its 27-in-1 formula comprised entirely of potent and natural ingredients, it provides unparalleled support for the health of your joints, back, and muscles. https://balmorex-try.com/
Support the health of your ears with 100% natural ingredients, finally being able to enjoy your favorite songs and movies https://quietumplus-try.com/
Peak BioBoost is a revolutionary dietary supplement that leverages the power of nature to support and improve your digestive system. https://peakbioboost-web.com/
89. Клининговая компания в Челябинске предоставляет услуги по уборке квартир с аллергенами, включая пыльцу, пыль, шерсть животных, плесень и другие аллергены, проводя глубокую уборку, мойку, дезинфекцию для улучшения качества воздуха и жизни жильцов.
Клининг Челябинск .
GutOptim is a digestive health supplement designed to support your gut and stomach. It restore balance in gut flora and reduce the symptoms of digestive disorders. https://gutoptim-try.com/
反向連接金字塔
G搜尋引擎在多番更新之后需要套用不同的排名參數。
今天有一種方法可以使用反向連結吸引G搜尋引擎對您的網站的注意。
反向連接不僅是有效的推廣工具,也是有機流量。
我們會得到什麼結果:
我們透過反向链接向G搜尋引擎展示我們的網站。
他們收到了到該網站的自然過渡,這也是向G搜尋引擎發出的信號,表明該資源正在被人們使用。
我們如何向G搜尋引擎表明該網站具有流動性:
個帶有主要訊息的主頁反向連結
我們透過來自受信任網站的重定向來建立反向連接。
此外,我們將網站放置在单独的網路分析器上,網站最終會進入這些分析器的高速缓存中,然後我們使用產生的連結作為部落格、論壇和評論的重新定向。 這個重要的操作向G搜尋引擎顯示了網站地圖,因為網站分析器顯示了有關網站的所有資訊以及所有關鍵字和標題,這很棒
有關我們服務的所有資訊都在網站上!
Burn Boost Powder™ is a proven weight loss powder drink that helps to lose weight and boosts the overall metabolism in the body. https://burnboost-web.com
NanoDefense Pro utilizes a potent blend of meticulously chosen components aimed at enhancing the wellness of both your nails and skin. https://nanodefense-web.com/
Pirámide de backlinks
Aquí está el texto con la estructura de spintax que propone diferentes sinónimos para cada palabra:
“Pirámide de enlaces de retorno
Después de varias actualizaciones del motor de búsqueda G, necesita aplicar diferentes opciones de clasificación.
Hay una manera de llamar la atención de los motores de búsqueda a su sitio web con enlaces de retroceso.
Los enlaces de retorno no sólo son una estrategia eficaz para la promoción, sino que también tienen flujo de visitantes orgánico, las ventas directas de estos recursos más probable es que no será, pero las transiciones será, y es poedenicheskogo tráfico que también obtenemos.
Lo que vamos a obtener al final en la salida:
Mostramos el sitio a los motores de búsqueda a través de backlinks.
Conseguimos transiciones orgánicas hacia el sitio, lo que también es una señal para los buscadores de que el recurso está siendo utilizado por la gente.
Cómo mostramos los motores de búsqueda que el sitio es líquido:
1 backlink se hace a la página principal donde está la información principal
Hacemos enlaces de retroceso a través de redirecciones de sitios de confianza
Lo más crucial colocamos el sitio en una herramienta independiente de analizadores de sitios, el sitio entra en la caché de estos analizadores, luego los enlaces recibidos los colocamos como redirecciones en blogs, foros, comentarios.
Esta importante acción muestra a los buscadores el MAPA DEL SITIO, ya que los analizadores de sitios muestran toda la información de los sitios con todas las palabras clave y títulos y es muy efectivo.
¡Toda la información sobre nuestros servicios en el sitio web!
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
93. Хотите чистоту без лишних затрат? Обратитесь в нашу клининговую компанию в Челябинске! Мы предоставляем широкий спектр услуг по доступным ценам, чтобы каждый мог позволить себе уют и порядок.
Клининговая компания Челябинск .
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
FlowForce Max is an innovative, natural and effective way to address your prostate problems, while addressing your energy, libido, and vitality. https://flowforcemax-web.com/
CLINICALLY PROVEN* To Increase Semen Volume And Intensity https://semenax-try.com/
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
DuoTrim is an innovative weight loss supplement that utilizes the power of natural plants and nutrients to create CSM bacteria https://duotrim-us.com/
BioFit is a Nutritional Supplement That Uses Probiotics To Help You Lose Weight https://biofit-web.com/
Sugar Balance is an ultra-potent blood sugar supplement that you can use to help control glucose levels, melt away fat and improve your overall health. https://sugarbalance-us.com/
GlucoFlush is an advanced formula specially designed for pancreas support that will let you promote healthy weight by effectively maintaining the blood sugar level and cleansing and strengthening your gut. https://glucoflush-us.com/
PureLumin Essence is a meticulously-crafted natural formula designed to help women improve the appearance of age spots. https://pureluminessence-web.com/
Alpha Tonic is a powder-based supplement that uses multiple natural herbs and essential vitamins and minerals to help optimize your body’s natural testosterone levels. https://alphatonic-web.com
Vivo Tonic is a remarkable blood sugar support nutritional supplement that offers a wide range of benefits. https://vivotonic-web.com/
Nervogen Pro is an effective dietary supplement designed to help patients with neuropathic pain. When you combine exotic herbs, spices, and other organic substances, your immune system will be strengthened. https://nervogenpro-web.com/
Progenifix is designed to help maximize weight loss results using a mixture of natural, science-backed ingredients. The formula also has secondary benefits, including promoting overall wellness and vitality and assisting your immune system. https://progenifix-web.com/
AquaPeace is an all-natural nutritional formula that uses a proprietary and potent blend of ingredients and nutrients to improve overall ear and hearing health and alleviate the symptoms of tinnitus. https://aquapeace-web.com
FoliPrime is a simple serum containing a blend of vitamins designed to boost hair health. FoliPrime has 100 percent natural substances that enhance and supplement the vitamins in the scalp to promote hair growth. https://foliprime-web.com/
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Manage Multiple Digital Assets with Jaxx Wallet
Managing multiple digital assets can be a daunting task, especially with the increasing number of cryptocurrencies and tokens available in the market. However, with the right wallet, you can easily keep track of and manage all your digital assets in one place. Jaxx Wallet is a popular choice among cryptocurrency enthusiasts, offering a user-friendly interface and a wide range of features.
Features of Jaxx Wallet:
Multi-Currency Support: Jaxx Wallet supports over 90 cryptocurrencies, allowing you to manage all your assets in one place.
User-Friendly Interface: The wallet is designed to be easy to use, even for beginners in the cryptocurrency space.
Security: Jaxx Wallet offers robust security features to protect your assets, including encryption and backup options.
Cross-Platform Compatibility: You can access your Jaxx Wallet from multiple devices, including desktop and mobile devices, making it convenient to manage your assets on the go.
Jaxxify: Easily send and receive 90 currencies with Jaxxify, simplifying your cryptocurrency transactions.
Import your crypto wallets From Jaxx Liberty
The official retirement date for Jaxx Liberty is set for March 27, 2023, at 8:00 am ET. Following this transition, users will retain access to their 12-word backup phrase for a limited duration; however, transactions will be disabled, and balances may become outdated. To seamlessly migrate your Jaxx Liberty wallet, refer to the guidelines provided.
Conclusion
With Jaxx Wallet, managing multiple digital assets has never been easier. Its user-friendly interface, multi-currency support, and security features make it a reliable choice for cryptocurrency enthusiasts. Whether you’re new to the world of cryptocurrencies or an experienced trader, Jaxx Wallet has something to offer for everyone.
Neuro-Thrive is a brain health supplement that claims to promote good memory and thinking skills and better quality sleep. This nootropic supplement achieves its cause with its potent blend of natural compounds and extracts that are proven to be effective in sharpening mental acuity. https://neurothrive-web.com/
Fast Lean Pro is a herbal supplement that tricks your brain into imagining that you’re fasting and helps you maintain a healthy weight no matter when or what you eat. It offers a novel approach to reducing fat accumulation and promoting long-term weight management. https://fastleanpro-web.com/
The ProNail Complex is a meticulously-crafted natural formula which combines extremely potent oils and skin-supporting vitamins. https://pronailcomplex-web.com/https://pronailcomplex-web.com/
Erectin is a clinically-proven dietary supplement designed to enhance male https://erectin-web.com/
100% Natural Formula Expressly Designed to Help Control Blood Sugar Levels, Improve Insulin Response And Support Overall Health https://glucotrusttry.com/
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
PowerBite stands as an innovative dental candy, dedicated to nurturing healthy teeth and gums. Infused with a potent formula, it champions the cause of a robust and radiant smile. Crafted meticulously https://powerbite-web.com/
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Protoflow is a prostate health supplement featuring a blend of plant extracts, vitamins, minerals, fruit extracts, and more. https://protoflow-web.com/
Boostaro is a dietary supplement designed specifically for men who suffer from health issues. https://boostaro-try.com/
Unlock the incredible potential of Puravive! Supercharge your metabolism and incinerate calories like never before with our unique fusion of 8 exotic components. Bid farewell to those stubborn pounds and welcome a reinvigorated metabolism and boundless vitality. Grab your bottle today and seize this golden opportunity! https://puravive-web.com/
Zoracel is an extraordinary oral care product designed to promote healthy teeth and gums, provide long-lasting fresh breath, support immune health, and care for the ear, nose, and throat. https://zoracel-web.com
Cerebrozen is an excellent liquid ear health supplement purported to relieve tinnitus and improve mental sharpness, among other benefits. The Cerebrozen supplement is made from a combination of natural ingredients, and customers say they have seen results in their hearing, focus, and memory after taking one or two droppers of the liquid solution daily for a week. https://cerebrozen-try.com/
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
The human body can continue to live thanks to the correct functioning of certain systems. If even one of these systems does not work properly, it can cause problems in human life. https://calmlean-web.com/
Zeneara is marketed as an expert-formulated health supplement that can improve hearing and alleviate tinnitus, among other hearing issues. https://zeneara-web.com/
GlucoBerry is one of the biggest all-natural dietary and biggest scientific breakthrough formulas ever in the health industry today. This is all because of its amazing high-quality cutting-edge formula that helps treat high blood sugar levels very naturally and effectively. https://glucoberry-web.com/
Pineal XT is a revolutionary supplement that promotes proper pineal gland function and energy levels to support healthy body function. https://pinealxt-web.com/
Как сберечь свои личные данные: страхуйтесь от утечек информации в интернете. Сегодня защита информации становится всё более важной задачей. Одним из наиболее распространенных способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и как предохранить себя от их утечки? Что такое «сит фразы»? «Сит фразы» — это сочетания слов или фраз, которые бывают используются для доступа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или другие конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, с помощью этих сит фраз. Как сохранить свои личные данные? Используйте запутанные пароли. Избегайте использования простых паролей, которые мгновенно угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого из вашего аккаунта. Не применяйте один и тот же пароль для разных сервисов. Используйте двухэтапную аутентификацию (2FA). Это прибавляет дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт посредством другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте персональную информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы предохранить свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может привести к серьезным последствиям, таким как кража личной информации и финансовых потерь. Чтобы охранить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
Introducing TerraCalm, a soothing mask designed specifically for your toenails. Unlike serums and lotions that can be sticky and challenging to include in your daily routine, TerraCalm can be easily washed off after just a minute. https://terracalm-web.com/
71. Клининговая компания в Челябинске предоставляет услуги по уборке квартир после завершения аренды, включая глубокую мойку полов, стен, окон, удаление следов проживания предыдущих жильцов и общую уборку для приведения квартиры в порядок перед новыми жильцами.
Клининг Челябинск .
VidaCalm is an all-natural blend of herbs and plant extracts that treat tinnitus and help you live a peaceful life. https://vidacalm-web.com/
Are you tired of looking in the mirror and noticing saggy skin? Is saggy skin making you feel like you are trapped in a losing battle against aging? Do you still long for the days when your complexion radiated youth and confidence? https://refirmance-web.com/
Даркнет и сливы в Телеграме
Даркнет – это отрезок интернета, которая не индексируется обычными поисковыми системами и требует уникальных программных средств для доступа. В даркнете существует обилие скрытых сайтов, где можно найти различные товары и услуги, в том числе и нелегальные.
Одним из известных способов распространения информации в даркнете является использование мессенджера Телеграм. Телеграм предоставляет возможность создания закрытых каналов и чатов, где пользователи могут обмениваться информацией, в том числе и нелегальной.
Сливы информации в Телеграме – это способ распространения конфиденциальной информации, такой как украденные данные, базы данных, персональные сведения и другие материалы. Эти сливы могут включать в себя информацию о кредитных картах, паролях, персональных сообщениях и даже фотографиях.
Сливы в Телеграме могут быть опасными, так как они могут привести к утечке конфиденциальной информации и нанести ущерб репутации и финансовым интересам людей. Поэтому важно быть осторожным при обмене информацией в интернете и не доверять сомнительным источникам.
Вот кошельки с балансом у бота
Gorilla Flow prostate is an all-natural dietary supplement for men which aims to decrease inflammation in the prostate to decrease common urinary tract issues such as frequent and night-time urination, leakage, or blocked urine stream. https://gorillaflow-web.com
слив сид фраз
Слив сид фраз (seed phrases) является одной из наиболее известных способов утечки личной информации в мире криптовалют. В этой статье мы разберем, что такое сид фразы, по какой причине они важны и как можно защититься от их утечки.
Что такое сид фразы?
Сид фразы, или мнемонические фразы, являются комбинацию слов, которая используется для формирования или восстановления кошелька криптовалюты. Обычно сид фраза состоит из 12 или 24 слов, которые являются собой ключ к вашему кошельку. Потеря или утечка сид фразы может влечь за собой потере доступа к вашим криптовалютным средствам.
Почему важно защищать сид фразы?
Сид фразы служат ключевым элементом для защищенного хранения криптовалюты. Если злоумышленники получат доступ к вашей сид фразе, они сумеют получить доступ к вашему кошельку и украсть все средства.
Как защититься от утечки сид фраз?
Никогда не передавайте свою сид фразу ничьему, даже если вам кажется, что это доверенное лицо или сервис.
Храните свою сид фразу в защищенном и защищенном месте. Рекомендуется использовать аппаратные кошельки или специальные программы для хранения сид фразы.
Используйте дополнительные методы защиты, такие как двухэтапная проверка, для усиления безопасности вашего кошелька.
Регулярно делайте резервные копии своей сид фразы и храните их в других безопасных местах.
Заключение
Слив сид фраз является значительной угрозой для безопасности владельцев криптовалют. Понимание важности защиты сид фразы и принятие соответствующих мер безопасности помогут вам избежать потери ваших криптовалютных средств. Будьте бдительны и обеспечивайте надежную защиту своей сид фразы
сид фразы кошельков
Сид-фразы, или напоминающие фразы, представляют собой сумму слов, которая используется для формирования или восстановления кошелька криптовалюты. Эти фразы обеспечивают доступ к вашим криптовалютным средствам, поэтому их защищенное хранение и использование чрезвычайно важны для защиты вашего криптоимущества от утери и кражи.
Что такое сид-фразы кошельков криптовалют?
Сид-фразы представляют собой набор случайно сгенерированных слов, часто от 12 до 24, которые предназначены для создания уникального ключа шифрования кошелька. Этот ключ используется для восстановления возможности доступа к вашему кошельку в случае его повреждения или утери. Сид-фразы обладают высокой защиты и шифруются, что делает их надежными для хранения и передачи.
Зачем нужны сид-фразы?
Сид-фразы необходимы для обеспечения безопасности и доступности вашего криптоимущества. Они позволяют восстановить возможность доступа к кошельку в случае утери или повреждения физического устройства, на котором он хранится. Благодаря сид-фразам вы можете без труда создавать резервные копии своего кошелька и хранить их в безопасном месте.
Как обеспечить безопасность сид-фраз кошельков?
Никогда не раскрывайте сид-фразой ни с кем. Сид-фраза является вашим ключом к кошельку, и ее раскрытие может влечь за собой утере вашего криптоимущества.
Храните сид-фразу в секурном месте. Используйте физически защищенные места, такие как банковские ячейки или специализированные аппаратные кошельки, для хранения вашей сид-фразы.
Создавайте резервные копии сид-фразы. Регулярно создавайте резервные копии вашей сид-фразы и храните их в разных безопасных местах, чтобы обеспечить возможность доступа к вашему кошельку в случае утери или повреждения.
Используйте дополнительные меры безопасности. Включите двухфакторную верификацию и другие методы защиты для своего кошелька криптовалюты, чтобы обеспечить дополнительный уровень безопасности.
Заключение
Сид-фразы кошельков криптовалют являются ключевым элементом надежного хранения криптоимущества. Следуйте рекомендациям по безопасности, чтобы защитить свою сид-фразу и обеспечить безопасность своих криптовалютных средств.
Пирамида Backlinks
После того как многочисленных обновлений поисковой системы G необходимо внедрять разные варианты сортировки.
Сегодня есть способ привлечь внимание поисковых систем к вашему веб-сайту с помощью бэклинков.
Бэклинки не только эффективный инструмент продвижения, но и имеют органический трафик, прямых продаж с этих ресурсов скорее всего не будет, но переходы будут, и именно поеденического трафика мы тоже получаем.
Что в итоге получим на выходе:
Мы показываем сайт поисковым системам через обратные ссылки.
Получают органические переходы на веб-сайт, а это также сигнал поисковым системам о том, что ресурс используется людьми.
Как мы указываем поисковым системам, что сайт ликвиден:
1 ссылка на главную страницу, где содержится основная информация, создается.
Размещаем обратные ссылки через редиректы с трастовых ресурсов.
Основное – мы индексируем сайт с помощью специальных инструментов анализа веб-сайтов, сайт заносится в кеш этих инструментов, после чего полученные ссылки мы публикуем в качестве редиректов на блогах, форумах, в комментариях.
Это нужное действие показывает всем поисковикамКАРТУ САЙТА, так как анализаторы сайтов показывают всю информацию о сайтах со всеми ключевыми словами и заголовками и это очень ХОРОШО
HoneyBurn is a revolutionary liquid weight loss formula that stands as the epitome of excellence in the industry. https://honeyburn-web.com/
Привет всем!
Мы рады предложить вам широкий выбор входных и межкомнатных дверей в Саратове и области, а также гарантировать их качественную установку. За время нашей работы мы накопили значительный опыт в установке и обслуживании дверных конструкций, что позволяет нам успешно решать самые разнообразные задачи.
Наши основные принципы работы – это обязательность, строгое соблюдение договоренностей и выполнение всех работ в срок с высоким уровнем сервиса. Мы предлагаем нашим клиентам более 1000 моделей входных и межкомнатных дверей различных ценовых категорий, материалов отделки и конструкций от известных производителей.
У нас работают настоящие профессионалы, которые знают все тонкости и нюансы данной области. Наши опытные консультанты всегда готовы помочь вам подобрать оптимальное решение, которое обеспечит вам надежную и комфортную работу выбранных дверей.
Вся информация на сайте https://id64.ru/
Двери имеются в наличии на складе и могут быть доставлены в кратчайший срок.
Осуществляется как гарантийное, так и постгарантийное сервисное обслуживание изделий, приобретенных в компании
Замер и консультация инженера-технолога по месту заказа дверей производятся бесплатно.
По желанию клиента, двери могут изготавливаться с индивидуальными параметрами: тип отделки, фурнитура, размеры.
Входные двери
Декоративные рейки
Двери раздвижные
Двери в ванную
Недорогие двери
Двери Thermo
Удачи и хорошего интерьера!
zanetvize.com
Liu Jie는 자신이 가르친 내용이 제자들을 오도할까봐 두려워했습니다.
Xitox’s foot pads contain a combination of powerful herbs that help provide a soothing experience for your feet after a long day. https://xitox-web.com/
Hydrossential is actually a skincare serum or you can say a skincare supplement created by Emma Smith to help women keep their skin looking beautiful and flawless. https://hydrossential-web.com/
Carbofix is the revolutionary dietary formula that promises to activate weight loss without all the extra hard work. https://carbofix-try.com
Reliver Pro is a dietary supplement formulated with a blend of natural ingredients aimed at supporting liver health
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Abdomax is a nutritional supplement using an 8-second Nordic cleanse to eliminate gut issues, support gut health, and optimize pepsinogen levels. https://abdomax-web.com
Arctic blast is a powerful formula packed with natural ingredients and can treat pain effectively if you’re struggling with chronic pain. You can say goodbye to muscle cramps with this natural pain reliever in less than a minute. It helps with arthritic pain, blood circulation, and joint pain. It gives long-lasting effects that replace the need to go to surgery. https://arcticblast-web.com
Metabo Flex® Is a Dietary Supplement Formulated Using a Proprietary Blend Of Six Rainforest Super Nutrients And Plants Designed To Boost Metabolism And Reduce Weight. https://metaboflex-us.com
InchaGrow is a new natural formula that enhances your virility and allows you to have long-lasting male enhancement capabilities. https://inchagrow-web.com
هنا النص مع استخدام السبينتاكس:
“بناء الروابط الخلفية
بعد التحديثات العديدة لمحرك البحث G، تحتاج إلى تنفيذ خيارات ترتيب مختلفة.
هناك طريقة لجذب انتباه محركات البحث إلى موقعك على الويب باستخدام الروابط الخلفية.
الروابط الخلفية غير فقط أداة فعالة للترويج، ولكن تمتلك أيضًا حركة مرور عضوية، والمبيعات المباشرة من هذه الموارد على الأرجح ستكون كذلك، ولكن التحولات ستكون، وهي حركة المرور التي نحصل عليها أيضًا.
ما نكون عليه في النهاية في النهاية في الإخراج:
نعرض الموقع لمحركات البحث من خلال الروابط الخلفية.
2- نحصل على تبديلات عضوية إلى الموقع، وهي أيضًا إشارة لمحركات البحث أن المورد يستخدمه الناس.
كيف نظهر لمحركات البحث أن الموقع سائل:
1 يتم عمل صلة خلفي للصفحة الرئيسية حيث المعلومات الرئيسية
نقوم بعمل لينكات خلفية من خلال عمليات تحويل المواقع الموثوقة
الأهم من ذلك أننا نضع الموقع على أداة منفصلة من أساليب تحليل المواقع، ويدخل الموقع في ذاكرة التخزين المؤقت لهذه المحللات، ثم الروابط المستلمة التي نضعها كإعادة توجيه على المدونات والمنتديات والتعليقات.
هذا العملية المهم يعرض لمحركات البحث خريطة الموقع، حيث تعرض أدوات تحليل المواقع جميع المعلومات عن المواقع مع جميع الكلمات الرئيسية والعناوين وهو عمل جيد جداً
جميع المعلومات عن خدماتنا على الموقع!
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
k8 カジノ イラスト
このブログはいつ読んでも新鮮で、いつも楽しみにしています。
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
90. Клининг Челябинск специализируется на уборке квартир перед прибытием новорожденного ребенка, включая дезинфекцию, уборку игрушек, мягкой мебели, ковров, мойку санузлов, устранение пыли и другие работы для создания безопасной и чистой среды для малыша.
Клининговая компания Челябинск .
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
ProstaBiome is a carefully crafted dietary supplement aimed at promoting prostate health. Bid farewell to restless nights and discomfort with ProstaBiome precise strategy for addressing prostate concerns. https://prostabiome-web.com/
PotentStream is designed to address prostate health by targeting the toxic, hard water minerals that can create a dangerous buildup inside your urinary system It’s the only dropper that contains nine powerful natural ingredients that work in perfect synergy to keep your prostate healthy and mineral-free well into old age. https://potentstream-web.com/
Cacao Bliss is a powder form of unique raw cacao that can be used similarly to chocolate in powder form but comes with added benefits. It is designed to provide a rich and satisfying experience while delivering numerous health benefits. https://cacaobliss-web.com/
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Player線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
Player如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
Player線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
Player如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
娛樂城評價
Player線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
Player如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
Payments Latest provides in-depth journalism and insight into the most impactful news and trends shaping payments. https://paymentslatest.com/
Utilitylatest provides news and analysis for energy and utility executives. We cover topics like smart grid tech, clean energy, regulation, generation, demand response, solar, storage, transmission distribution, and more. https://utilitylatest.com
Как обезопасить свои данные: остерегайтесь утечек информации в интернете. Сегодня охрана своих данных становится все более важной задачей. Одним из наиболее часто встречающихся способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и в какой мере защититься от их утечки? Что такое «сит фразы»? «Сит фразы» — это комбинации слов или фраз, которые регулярно используются для доступа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или иные конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, с помощью этих сит фраз. Как обезопасить свои личные данные? Используйте сложные пароли. Избегайте использования очевидных паролей, которые просто угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого аккаунта. Не применяйте один и тот же пароль для разных сервисов. Используйте двухступенчатую аутентификацию (2FA). Это добавляет дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт через другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте персональную информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы защитить свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может привести к серьезным последствиям, таким подобно кража личной информации и финансовых потерь. Чтобы сохранить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
даркнет сливы тг
Даркнет и сливы в Телеграме
Даркнет – это часть интернета, которая не индексируется обыденными поисковыми системами и требует индивидуальных программных средств для доступа. В даркнете существует обилие скрытых сайтов, где можно найти различные товары и услуги, в том числе и нелегальные.
Одним из востребованных способов распространения информации в даркнете является использование мессенджера Телеграм. Телеграм предоставляет возможность создания закрытых каналов и чатов, где пользователи могут обмениваться информацией, в том числе и нелегальной.
Сливы информации в Телеграме – это процедура распространения конфиденциальной информации, такой как украденные данные, базы данных, персональные сведения и другие материалы. Эти сливы могут включать в себя информацию о кредитных картах, паролях, персональных сообщениях и даже фотографиях.
Сливы в Телеграме могут быть опасными, так как они могут привести к утечке конфиденциальной информации и нанести ущерб репутации и финансовым интересам людей. Поэтому важно быть осторожным при обмене информацией в интернете и не доверять сомнительным источникам.
Вот кошельки с балансом у бота
сид фразы кошельков
Сид-фразы, или памятные фразы, представляют собой соединение слов, которая используется для создания или восстановления кошелька криптовалюты. Эти фразы обеспечивают доступ к вашим криптовалютным средствам, поэтому их надежное хранение и использование чрезвычайно важны для защиты вашего криптоимущества от утери и кражи.
Что такое сид-фразы кошельков криптовалют?
Сид-фразы формируют набор произвольно сгенерированных слов, часто от 12 до 24, которые представляют собой для создания уникального ключа шифрования кошелька. Этот ключ используется для восстановления возможности доступа к вашему кошельку в случае его повреждения или утери. Сид-фразы обладают значительной защиты и шифруются, что делает их защищенными для хранения и передачи.
Зачем нужны сид-фразы?
Сид-фразы жизненно важны для обеспечения безопасности и доступности вашего криптоимущества. Они позволяют восстановить доступ к кошельку в случае утери или повреждения физического устройства, на котором он хранится. Благодаря сид-фразам вы можете легко создавать резервные копии своего кошелька и хранить их в безопасном месте.
Как обеспечить безопасность сид-фраз кошельков?
Никогда не передавайте сид-фразой ни с кем. Сид-фраза является вашим ключом к кошельку, и ее раскрытие может вести к утере вашего криптоимущества.
Храните сид-фразу в надежном месте. Используйте физически секурные места, такие как банковские ячейки или специализированные аппаратные кошельки, для хранения вашей сид-фразы.
Создавайте резервные копии сид-фразы. Регулярно создавайте резервные копии вашей сид-фразы и храните их в разных безопасных местах, чтобы обеспечить возможность доступа к вашему кошельку в случае утери или повреждения.
Используйте дополнительные меры безопасности. Включите другие методы защиты и двухфакторную аутентификацию для своего кошелька криптовалюты, чтобы обеспечить дополнительный уровень безопасности.
Заключение
Сид-фразы кошельков криптовалют являются ключевым элементом надежного хранения криптоимущества. Следуйте рекомендациям по безопасности, чтобы защитить свою сид-фразу и обеспечить безопасность своих криптовалютных средств.
кошелек с балансом купить
Криптокошельки с балансом: зачем их покупают и как использовать
В мире криптовалют все возрастающую популярность приобретают криптокошельки с предустановленным балансом. Это уникальные кошельки, которые уже содержат определенное количество криптовалюты на момент покупки. Но зачем люди приобретают такие кошельки, и как правильно использовать их?
Почему покупают криптокошельки с балансом?
Удобство: Криптокошельки с предустановленным балансом предлагаются как готовое к использованию решение для тех, кто хочет быстро начать пользоваться криптовалютой без необходимости покупки или обмена на бирже.
Подарок или награда: Иногда криптокошельки с балансом используются как подарок или поощрение в рамках акций или маркетинговых кампаний.
Анонимность: При покупке криптокошелька с балансом нет потребности предоставлять личные данные, что может быть важно для тех, кто ценит анонимность.
Как использовать криптокошелек с балансом?
Проверьте безопасность: Убедитесь, что кошелек безопасен и не подвержен взлому. Проверьте репутацию продавца и происхождение приобретения кошелька.
Переведите средства на другой кошелек: Если вы хотите долгосрочно хранить криптовалюту, рекомендуется перевести средства на более безопасный или удобный для вас кошелек.
Не храните все средства на одном кошельке: Для обеспечения безопасности рекомендуется распределить средства между несколькими кошельками.
Будьте осторожны с фишингом и мошенничеством: Помните, что мошенники могут пытаться обмануть вас, предлагая криптокошельки с балансом с целью получения доступа к вашим средствам.
Заключение
Криптокошельки с балансом могут быть удобным и быстрым способом начать пользоваться криптовалютой, но необходимо помнить о безопасности и осторожности при их использовании.Выбор и приобретение криптокошелька с балансом – это серьезный шаг, который требует внимания к деталям и осознанного подхода.”
слив сид фраз
Слив посеянных фраз (seed phrases) является одним из наиболее обычных способов утечки личной информации в мире криптовалют. В этой статье мы разберем, что такое сид фразы, по какой причине они важны и как можно защититься от их утечки.
Что такое сид фразы?
Сид фразы, или мнемонические фразы, являются комбинацию слов, которая используется для генерации или восстановления кошелька криптовалюты. Обычно сид фраза состоит из 12 или 24 слов, которые представляют собой ключ к вашему кошельку. Потеря или утечка сид фразы может вести к потере доступа к вашим криптовалютным средствам.
Почему важно защищать сид фразы?
Сид фразы представляют ключевым элементом для секурного хранения криптовалюты. Если злоумышленники получат доступ к вашей сид фразе, они могут получить доступ к вашему кошельку и украсть все средства.
Как защититься от утечки сид фраз?
Никогда не передавайте свою сид фразу любому, даже если вам представляется, что это проверенное лицо или сервис.
Храните свою сид фразу в безопасном и надежном месте. Рекомендуется использовать аппаратные кошельки или специальные программы для хранения сид фразы.
Используйте дополнительные методы защиты, такие как двухфакторная аутентификация (2FA), для усиления безопасности вашего кошелька.
Регулярно делайте резервные копии своей сид фразы и храните их в различных безопасных местах.
Заключение
Слив сид фраз является серьезной угрозой для безопасности владельцев криптовалют. Понимание важности защиты сид фразы и принятие соответствующих мер безопасности помогут вам избежать потери ваших криптовалютных средств. Будьте бдительны и обеспечивайте надежную защиту своей сид фразы
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Cneche provides in-depth journalism and insight into the most impactful news and trends shaping the finance industry. https://cneche.com/
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
freeflowincome.com
이때 모두가 생각한 것은 Wang Shouren이 이미 결혼 한 것이 안타깝다는 것입니다.
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Kantorbola adalah situs slot gacor terbaik di indonesia , kunjungi situs RTP kantor bola untuk mendapatkan informasi akurat slot dengan rtp diatas 95% . Kunjungi juga link alternatif kami di kantorbola77 dan kantorbola99 .
Lasixiv provides news and analysis for IT executives. We cover big data, IT strategy, cloud computing, security, mobile technology, infrastructure, software and more. https://lasixiv.com
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
kantorbola99
Kantorbola adalah situs slot gacor terbaik di indonesia , kunjungi situs RTP kantor bola untuk mendapatkan informasi akurat slot dengan rtp diatas 95% . Kunjungi juga link alternatif kami di kantorbola77 dan kantorbola99 .
Wedstraunt has the latest news in the restaurant industry, covering topics like consumer trends, technology, marketing and branding, operations, mergers https://wedstraunt.com
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Qcmpt provides in-depth journalism and insight into the news and trends impacting the customer experience space. https://qcmpt.com/
taurus118
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
geinoutime.com
황실은 양쯔강 남쪽 사람들의 불안정으로 인한 엄청난 결과에 대해 걱정하지 않습니까?
Sudaten provides in-depth journalism and insight into the news and trends impacting the energy, sustainability and governance space. https://sudaten.com
Платформа Автор 24 – это превосходный сервис для заказа многочисленных академических работ. Он работает на дипломных работах, а также расчетах. Кроме того, на сервисе Автор 24 можно заказать рецензии, отчеты о прохождении практики. Это практичный способ сэкономить время.
Автор 24 официальный Автор 24 ру .
Grpduk provides news and analysis for human resource executives. We cover topics like recruiting, HR management, employee learning https://grpduk.com
Платформа Автор 24 – это высококачественный сервис для покупки различных академических работ. Он занимается на рефератах, а также расчетах. Кроме того, на сервисе Автор 24 можно купить очерки, отчеты о прохождении практики. Это практичный способ повысить свои академические результаты.
Автор 24 официальный Автор24 .
Susibu provides in-depth journalism and insight into the news and trends impacting the hotel https://susibu.com/
Sisanit provides in-depth journalism and insight into the news and trends impacting corporate counsel. https://sisanit.com/
オンカジ k8
非常に興味深い記事でした。新たな知識をありがとう。
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
tintucnamdinh24h.com
그러나 사람들의 흐름은 여전히 홍수와 같습니다.
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://mimsbrook.com
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://smithsis.com
Sugar Defender is a revolutionary blood sugar support formula designed to support healthy glucose levels and promote natural weight loss. https://blackboxvending.com/
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Sugar Defender is a revolutionary blood sugar support formula designed to support healthy glucose levels and promote natural weight loss. https://mineryuta.com
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
rikvip
Rikvip Club: Trung Tâm Giải Trí Trực Tuyến Hàng Đầu tại Việt Nam
Rikvip Club là một trong những nền tảng giải trí trực tuyến hàng đầu tại Việt Nam, cung cấp một loạt các trò chơi hấp dẫn và dịch vụ cho người dùng. Cho dù bạn là người dùng iPhone hay Android, Rikvip Club đều có một cái gì đó dành cho mọi người. Với sứ mạng và mục tiêu rõ ràng, Rikvip Club luôn cố gắng cung cấp những sản phẩm và dịch vụ tốt nhất cho khách hàng, tạo ra một trải nghiệm tiện lợi và thú vị cho người chơi.
Sứ Mạng và Mục Tiêu của Rikvip
Từ khi bắt đầu hoạt động, Rikvip Club đã có một kế hoạch kinh doanh rõ ràng, luôn nỗ lực để cung cấp cho khách hàng những sản phẩm và dịch vụ tốt nhất và tạo điều kiện thuận lợi nhất cho người chơi truy cập. Nhóm quản lý của Rikvip Club có những mục tiêu và ước muốn quyết liệt để biến Rikvip Club thành trung tâm giải trí hàng đầu trong lĩnh vực game đổi thưởng trực tuyến tại Việt Nam và trên toàn cầu.
Trải Nghiệm Live Casino
Rikvip Club không chỉ nổi bật với sự đa dạng của các trò chơi đổi thưởng mà còn với các phòng trò chơi casino trực tuyến thu hút tất cả người chơi. Môi trường này cam kết mang lại trải nghiệm chuyên nghiệp với tính xanh chín và sự uy tín không thể nghi ngờ. Đây là một sân chơi lý tưởng cho những người yêu thích thách thức bản thân và muốn tận hưởng niềm vui của chiến thắng. Với các sảnh cược phổ biến như Roulette, Sic Bo, Dragon Tiger, người chơi sẽ trải nghiệm những cảm xúc độc đáo và đặc biệt khi tham gia vào casino trực tuyến.
Phương Thức Thanh Toán Tiện Lợi
Rikvip Club đã được trang bị những công nghệ thanh toán tiên tiến ngay từ đầu, mang lại sự thuận tiện và linh hoạt cho người chơi trong việc sử dụng hệ thống thanh toán hàng ngày. Hơn nữa, Rikvip Club còn tích hợp nhiều phương thức giao dịch khác nhau để đáp ứng nhu cầu đa dạng của người chơi: Chuyển khoản Ngân hàng, Thẻ cào, Ví điện tử…
Kết Luận
Tóm lại, Rikvip Club không chỉ là một nền tảng trò chơi, mà còn là một cộng đồng nơi người chơi có thể tụ tập để tận hưởng niềm vui của trò chơi và cảm giác hồi hộp khi chiến thắng. Với cam kết cung cấp những sản phẩm và dịch vụ tốt nhất, Rikvip Club chắc chắn là điểm đến lý tưởng cho những người yêu thích trò chơi trực tuyến tại Việt Nam và cả thế giới.
Купить диплом с доставкой до дома, онлайн.
Как купить диплом без риска, без заморочек.
Какой диплом купить, важная информация.
Преимущества покупки диплома, подробности.
Как купить диплом безопасно, без риска.
Как выбрать диплом для покупки, секреты выбора.
Купить диплом срочно и недорого, спешите.
Почему стоит купить диплом, наши преимущества.
Лучшие дипломы для покупки, срочно и выгодно.
Как купить диплом онлайн, подробности у нас.
Почему стоит купить диплом у нас, лучшие цены.
Как купить диплом срочно, лучшие условия.
Почему стоит заказать диплом, подробности у нас.
Как выбрать и купить диплом, важные моменты.
Как купить дипломы онлайн, безопасность на первом месте.
Какой диплом выбрать для покупки, подробности на сайте.
Купить диплом с доставкой по всему миру, важные детали.
Официальный документ об образовании, гарантированный результат.
купить диплом http://7arusak-diploms.com/ .
freeflowincome.com
그가 너무 독특하고 생일을 축하하기 위해 그런 방법을 사용할 줄 누가 알았습니까?
sugar defender: https://peyfon.com/
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Приобрести диплом без лишних хлопот, онлайн.
Как купить диплом без риска, без заморочек.
Заказать официальный документ о образовании, советы от профессионалов.
Почему выгодно купить диплом, все секреты.
Как купить диплом безопасно, с гарантией.
Лучшие предложения по покупке диплома, секреты выбора.
Дипломы на заказ по лучшим ценам, спешите.
Скрытая покупка дипломов, наши преимущества.
Как быстро купить диплом, только актуальная информация.
Покупка диплома: безопасность и качество, подробности у нас.
Почему стоит купить диплом у нас, срочные варианты.
Легальная покупка дипломов, лучшие условия.
Купить диплом без обмана, важные детали.
Дипломы на всех условиях, важные моменты.
Легальная покупка дипломов безопасно, безопасность на первом месте.
Купить дипломы легко, интересные варианты.
Официальная покупка диплома, лучшие условия.
Как купить диплом безопасно и быстро, безопасность на первом месте.
купить диплом https://www.7arusak-diploms.com/ .
sugar defender: https://seahorsesoap.com/
Заказать купленный диплом, не выходя из дома.
Доступные цены на дипломы для продажи, узнайте сейчас.
Заказать официальный документ о образовании, советы от профессионалов.
Опыт успешной покупки диплома, подробности.
Где купить диплом без проблем, без риска.
Лучшие предложения по покупке диплома, интересные варианты.
Дипломы на заказ по лучшим ценам, лучшие условия.
Покупка диплома: безопасность и конфиденциальность, наши преимущества.
Лучшие дипломы для покупки, только актуальная информация.
Покупка диплома: безопасность и качество, подробности у нас.
Почему стоит купить диплом у нас, срочные варианты.
Легальная покупка дипломов, лучшие условия.
Официальные дипломы для покупки, подробности у нас.
Дипломы на всех условиях, лучшие предложения.
Купить диплом без риска, гарантированная доставка.
Купить дипломы легко, подробности на сайте.
Заказать диплом онлайн без проблем, важные детали.
Как купить диплом безопасно и быстро, подробности у нас.
купить диплом http://7arusak-diploms.com .
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
외국선물의 출발 골드리치와 동행하세요.
골드리치증권는 길고긴기간 고객님들과 함께 선물마켓의 행로을 공동으로 여정을했습니다, 고객분들의 확실한 자금운용 및 높은 수익률을 지향하여 항상 최선을 다하고 있습니다.
왜 20,000+명 이상이 골드리치와 동참하나요?
신속한 솔루션: 간단하며 빠른속도의 프로세스를 마련하여 어느누구라도 간편하게 활용할 수 있습니다.
안전보장 프로토콜: 국가기관에서 사용하는 최상의 등급의 보안체계을 도입하고 있습니다.
스마트 인가: 전체 거래데이터은 암호화 처리되어 본인 외에는 그 누구도 내용을 접근할 수 없습니다.
보장된 수익성 마련: 리스크 요소를 줄여, 더욱 더 확실한 수익률을 제공하며 이에 따른 리포트를 공유합니다.
24 / 7 지속적인 고객상담: 365일 24시간 신속한 상담을 통해 투자자분들을 온전히 서포트합니다.
함께하는 협력사: 골드리치증권는 공기업은 물론 금융계들 및 많은 협력사와 공동으로 동행해오고.
외국선물이란?
다양한 정보를 참고하세요.
외국선물은 해외에서 거래되는 파생금융상품 중 하나로, 특정 기반자산(예: 주식, 화폐, 상품 등)을 기초로 한 옵션계약 계약을 지칭합니다. 근본적으로 옵션은 특정 기초자산을 미래의 어떤 시점에 정해진 금액에 매수하거나 매도할 수 있는 권리를 부여합니다. 외국선물옵션은 이러한 옵션 계약이 외국 시장에서 거래되는 것을 지칭합니다.
국외선물은 크게 콜 옵션과 풋 옵션으로 나뉩니다. 콜 옵션은 명시된 기초자산을 미래에 일정 가격에 매수하는 권리를 허락하는 반면, 풋 옵션은 명시된 기초자산을 미래에 정해진 가격에 팔 수 있는 권리를 부여합니다.
옵션 계약에서는 미래의 명시된 날짜에 (종료일이라 칭하는) 정해진 가격에 기초자산을 사거나 매도할 수 있는 권리를 보유하고 있습니다. 이러한 가격을 실행 금액이라고 하며, 만기일에는 해당 권리를 행사할지 여부를 결정할 수 있습니다. 따라서 옵션 계약은 투자자에게 미래의 가격 변동에 대한 보호나 이익 실현의 기회를 제공합니다.
외국선물은 마켓 참가자들에게 다양한 투자 및 매매거래 기회를 마련, 외환, 상품, 주식 등 다양한 자산유형에 대한 옵션 계약을 망라할 수 있습니다. 투자자는 매도 옵션을 통해 기초자산의 하향에 대한 안전장치를 받을 수 있고, 매수 옵션을 통해 활황에서의 수익을 타깃팅할 수 있습니다.
외국선물 거래의 원리
행사 가격(Exercise Price): 외국선물에서 행사 가격은 옵션 계약에 따라 특정한 가격으로 계약됩니다. 만기일에 이 가격을 기준으로 옵션을 실행할 수 있습니다.
만기일(Expiration Date): 옵션 계약의 만료일은 옵션의 행사가 허용되지않는 최종 일자를 뜻합니다. 이 날짜 다음에는 옵션 계약이 만료되며, 더 이상 거래할 수 없습니다.
매도 옵션(Put Option)과 콜 옵션(Call Option): 풋 옵션은 기초자산을 지정된 가격에 매도할 수 있는 권리를 부여하며, 매수 옵션은 기초자산을 지정된 금액에 사는 권리를 제공합니다.
옵션료(Premium): 외국선물 거래에서는 옵션 계약에 대한 옵션료을 지불해야 합니다. 이는 옵션 계약에 대한 가격으로, 마켓에서의 수요와 공급량에 따라 변동됩니다.
행사 전략(Exercise Strategy): 거래자는 만기일에 옵션을 행사할지 여부를 선택할 수 있습니다. 이는 마켓 상황 및 투자 플랜에 따라 차이가있으며, 옵션 계약의 수익을 최대화하거나 손실을 감소하기 위해 결정됩니다.
시장 위험요인(Market Risk): 해외선물 거래는 마켓의 변동성에 효과을 받습니다. 가격 변동이 기대치 못한 진로으로 일어날 경우 손실이 발생할 수 있으며, 이러한 시장 리스크를 감소하기 위해 거래자는 전략을 구축하고 투자를 설계해야 합니다.
골드리치와 함께하는 국외선물은 보장된 신뢰할 수 있는 투자를 위한 가장좋은 옵션입니다. 고객님들의 투자를 뒷받침하고 가이드하기 위해 우리는 최선을 기울이고 있습니다. 함께 더 나은 내일를 향해 계속해나가세요.
UEFA Euro 2024 Sân Chơi Bóng Đá Hấp Dẫn Nhất Của Châu Âu
Euro 2024 là sự kiện bóng đá lớn nhất của châu Âu, không chỉ là một giải đấu mà còn là một cơ hội để các quốc gia thể hiện tài năng, sự đoàn kết và tinh thần cạnh tranh.
Euro 2024 hứa hẹn sẽ mang lại những trận cầu đỉnh cao và kịch tính cho người hâm mộ trên khắp thế giới. Cùng tìm hiểu các thêm thông tin hấp dẫn về giải đấu này tại bài viết dưới đây, gồm:
Nước chủ nhà
Đội tuyển tham dự
Thể thức thi đấu
Thời gian diễn ra
Sân vận động
Euro 2024 sẽ được tổ chức tại Đức, một quốc gia có truyền thống vàng của bóng đá châu Âu.
Đức là một đất nước giàu có lịch sử bóng đá với nhiều thành công quốc tế và trong những năm gần đây, họ đã thể hiện sức mạnh của mình ở cả mặt trận quốc tế và câu lạc bộ.
Việc tổ chức Euro 2024 tại Đức không chỉ là một cơ hội để thể hiện năng lực tổ chức tuyệt vời mà còn là một dịp để giới thiệu văn hóa và sức mạnh thể thao của quốc gia này.
Đội tuyển tham dự giải đấu Euro 2024
Euro 2024 sẽ quy tụ 24 đội tuyển hàng đầu từ châu Âu. Các đội tuyển này sẽ là những đại diện cho sự đa dạng văn hóa và phong cách chơi bóng đá trên khắp châu lục.
Các đội tuyển hàng đầu như Đức, Pháp, Tây Ban Nha, Bỉ, Italy, Anh và Hà Lan sẽ là những ứng viên nặng ký cho chức vô địch.
Trong khi đó, các đội tuyển nhỏ hơn như Iceland, Wales hay Áo cũng sẽ mang đến những bất ngờ và thách thức cho các đối thủ.
Các đội tuyển tham dự được chia thành 6 bảng đấu, gồm:
Bảng A: Đức, Scotland, Hungary và Thuỵ Sĩ
Bảng B: Tây Ban Nha, Croatia, Ý và Albania
Bảng C: Slovenia, Đan Mạch, Serbia và Anh
Bảng D: Ba Lan, Hà Lan, Áo và Pháp
Bảng E: Bỉ, Slovakia, Romania và Ukraina
Bảng F: Thổ Nhĩ Kỳ, Gruzia, Bồ Đào Nha và Cộng hoà Séc
Заказать купленный диплом, через интернет.
Легальный способ купить диплом, узнайте сейчас.
Заказать официальный документ о образовании, важная информация.
Преимущества покупки диплома, все секреты.
Купить диплом легко, на проверенных ресурсах.
Как выбрать диплом для покупки, важные моменты.
Дипломы на заказ по лучшим ценам, лучшие условия.
Скрытая покупка дипломов, наши преимущества.
Где купить действующий диплом, подробности на сайте.
Как купить диплом онлайн, подробности у нас.
Почему стоит купить диплом у нас, срочные варианты.
Безопасное приобретение документов об образовании, без рисков.
Почему стоит заказать диплом, гарантированный результат.
Купить диплом просто, важные моменты.
Легальная покупка дипломов безопасно, безопасность на первом месте.
Купить дипломы легко, гарантированный результат.
Официальная покупка диплома, лучшие условия.
Официальный документ об образовании, подробности у нас.
купить диплом 7arusak-diploms.com .
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
k8 カジノ パチンコ 種類
このブログは本当に役立つ情報が満載で、大好きです。
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Купить диплом с доставкой до дома, не выходя из дома.
Доступные цены на дипломы для продажи, узнайте сейчас.
Какой диплом купить, важная информация.
Преимущества покупки диплома, рассказываем.
Где купить диплом без проблем, на проверенных ресурсах.
Как выбрать диплом для покупки, интересные варианты.
Как купить диплом быстро, лучшие условия.
Почему стоит купить диплом, проверенные решения.
Как быстро купить диплом, срочно и выгодно.
Покупка диплома: безопасность и качество, гарантированный результат.
Как выбрать диплом, срочные варианты.
Безопасное приобретение документов об образовании, без рисков.
Официальные дипломы для покупки, подробности у нас.
Как выбрать и купить диплом, подробности на сайте.
Легальная покупка дипломов безопасно, подробности у нас.
Купить дипломы легко, интересные варианты.
Официальная покупка диплома, подробности здесь.
Как купить диплом безопасно и быстро, подробности у нас.
купить диплом https://7arusak-diploms.com/ .
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
largestcatbreed.com
Fang Jifan은 “폐하에게 돌아가십시오. 제 아들은 7 ~ 8 점 회복되었습니다. “라고 말했습니다.
Купить диплом с доставкой до дома, не выходя из дома.
Легальный способ купить диплом, подробности здесь.
Какой диплом купить, советы от профессионалов.
Опыт успешной покупки диплома, подробности.
Где купить диплом без проблем, на проверенных ресурсах.
Купить диплом по выгодной цене, секреты выбора.
Как купить диплом быстро, спешите.
Покупка диплома: безопасность и конфиденциальность, проверенные решения.
Как быстро купить диплом, подробности на сайте.
Купить диплом срочно и законно, подробности у нас.
Почему стоит купить диплом у нас, срочные варианты.
Легальная покупка дипломов, без рисков.
Почему стоит заказать диплом, важные детали.
Купить диплом просто, лучшие предложения.
Купить диплом без риска, безопасность на первом месте.
Купить дипломы легко, гарантированный результат.
Официальная покупка диплома, важные детали.
Как купить диплом безопасно и быстро, безопасность на первом месте.
купить диплом 7arusak-diploms.com .
geinoutime.com
나는 이 상자에서 눈부시게 배열된 것들을 보았는데, 그것들은 모두 다양한 봉인이었습니다.
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Aut prodesse volunt aut delactare poetae — Поэты желают быть или полезными, или приятными.
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Contradictio in re — лог. Противоречие в существе (нелепость).
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Доброго!
Если кто-то скажет вам, что серьезно относится к игровым автоматам на своем смартфоне, верьте — это я. Почему стоять у громоздкого автомата в полуподвальном зале, если можно устроиться с комфортом на своем диване с телефоном в руках, где каждый спин приносит чувство легкой восторженности? Плюс, загрузив приложение, вы можете платить даже через сим-карту, что за чудо техники? Но знаете, что еще лучше? Вывод денег прямо на вашу карту Тинькофф. Буквально “свайпнул — и богат”. О, а момент, когда вы выигрываете большой куш, и ваш телефон вибрирует от уведомлений — это как получить лайк от самой судьбы!
https://eramita.ru/2024/05/10/new-retro-casino-Окунись-в-Атмосферу-Ретро-и-Получи-Бездепозитный-Бонус
казино миллион официальный сайт зеркало казино
сайт игровых автоматов с выводом денег на андроид
скачать официальное казино
мобильные казино casinomobilnye
игровые автоматы на деньги для андроид
Удачи!
game1kb.com
그래서 이 울부짖는 작은 돼지들을 본 Zhu Houzhao는 도저히 그들을 쳐다볼 수 없었습니다.
Привет!
Привет, друзья-казиношники! Сегодня я расскажу вам о своем опыте игры в онлайн-казино с живыми дилерами. Это же просто фантастика!
Представьте себе: вы сидите дома в любимых тапочках, а на экране перед вами – роскошное казино с профессиональными крупье! Атмосфера настолько реалистична, что кажется, будто вы перенеслись в Лас-Вегас или Монако. А главное – все это доступно 24/7, без необходимости куда-то ехать!
Но не думайте, что живые дилеры – это просто красивая картинка. Играть с ними на реальные деньги так же увлекательно и азартно, как и в обычном казино. К тому же, многие официальные сайты предлагают эксклюзивные столы и лимиты ставок для VIP-игроков.
Так что если вы хотите почувствовать себя настоящим хайроллером, не выходя из дома, обязательно попробуйте сыграть с живыми дилерами! Уверяю вас, это незабываемые эмоции и шанс сорвать солидный куш!
flerus-shop.hcp.dilhost.ru
казино официальный вход
лучшее приложение казино
игровые автоматы с баланса телефона на андроид
казино на деньги приложение для телефона
7k casino скачать приложение для андроид бесплатно vslot pays
Удачи!
Привет!
Признаюсь, когда дело доходит до выбора казино, я предпочитаю играть на родной земле, даже если это только виртуальная земля русских казино онлайн. Здесь, как на даче у бабушки: все знакомо и понятно. Никаких языковых барьеров, только вы, игровые автоматы и ваша удача, говорящая по-русски. И как же приятно, когда поддержка отвечает без акцента и сразу понимает ваши проблемы! А бонусы? Это как малина на дачном участке – собирай не хочу! На русских площадках бонусы щедрые, как русская душа, и это делает игру еще прекраснее.
avtoshkolapilot.ru
150 бесплатных спинов
скачать казино на андроид на реальные деньги
бездепозитные бонусы в казино
казино на мобильный телефон casinomobilnye
миллион казино официальный сайт зеркало
Удачи!
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
en-renew.com
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
k8 カジノ コード
この記事から得られる情報の量と質に驚きました。非常に役立ちます。
Здравствуйте!
Начнем с того, что вы можете скачать казино на ваш Android-смартфон или планшет. Это позволит вам играть в любимые игровые автоматы, рулетку, блэкджек и многие другие азартные игры в любом месте и в любое время. Многие казино предлагают бонусы на первый депозит, которые увеличивают ваш начальный банкролл, давая вам больше возможностей для выигрыша. Чтобы сделать игру еще более удобной, не забудьте скачать мобильное приложение казино. Вы можете найти бесплатные мобильные казино, которые позволят вам опробовать игры без риска, прежде чем начать играть на реальные деньги.
http://share.psiterror.ru/2024/05/12/kakie-bonusy-v-nashe-vremya-poluchit-vozmozhno-budet-v-kazino-lev.html
скачать казино на реальные деньги
онлайн казино миллион официальный сайт зеркало
приложение казино
casino пополнение с киви cасино р
бонусы казино на первый депозит
Удачи!
Привет!
Начнем с того, что вы можете скачать казино на ваш Android-смартфон или планшет. Это позволит вам играть в любимые игровые автоматы, рулетку, блэкджек и многие другие азартные игры в любом месте и в любое время. Многие казино предлагают бонусы на первый депозит, которые увеличивают ваш начальный банкролл, давая вам больше возможностей для выигрыша. Чтобы сделать игру еще более удобной, не забудьте скачать мобильное приложение казино. Вы можете найти бесплатные мобильные казино, которые позволят вам опробовать игры без риска, прежде чем начать играть на реальные деньги.
http://passo.su/forums/index.php?autocom=gallery&req=si&img=2998
1 гоу casino
unlim скачать на андроид приложение casino
в каких казино есть оплата по сбп
приложение казино
casino пополнение с киви cасино р
Удачи!
us-us-balmorex.pro
🌮 Taco Tuesday crew, dish on the spicy twist in the fifth line of the post!
buysteriodsonline.com
먹고 은화 세 냥의 표값을 냈으니 가볼까요?
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Gerakl24: Квалифицированная Смена Основания, Венцов, Полов и Передвижение Зданий
Компания Gerakl24 занимается на выполнении полных услуг по замене фундамента, венцов, полов и передвижению зданий в городе Красноярске и за его пределами. Наш коллектив квалифицированных специалистов обещает отличное качество исполнения всех видов восстановительных работ, будь то деревянные, каркасные, из кирпича или бетонные конструкции дома.
Плюсы услуг Gerakl24
Профессионализм и опыт:
Каждая задача выполняются только высококвалифицированными экспертами, с многолетним большой практику в направлении строительства и ремонта зданий. Наши специалисты эксперты в своей области и реализуют задачи с высочайшей точностью и учетом всех деталей.
Комплексный подход:
Мы осуществляем полный спектр услуг по ремонту и ремонту домов:
Замена фундамента: укрепление и замена старого фундамента, что гарантирует долговечность вашего строения и устранить проблемы, вызванные оседанием и деформацией.
Реставрация венцов: реставрация нижних венцов из дерева, которые наиболее часто гниют и разрушаются.
Установка новых покрытий: установка новых полов, что кардинально улучшает внешний вид и функциональные характеристики.
Передвижение домов: качественный и безопасный перенос строений на новые места, что помогает сохранить здание и избегает дополнительных затрат на строительство нового.
Работа с любыми видами зданий:
Деревянные дома: восстановление и защита деревянных строений, защита от гниения и вредителей.
Каркасные дома: укрепление каркасов и замена поврежденных элементов.
Кирпичные дома: реставрация кирпичной кладки и укрепление стен.
Бетонные строения: ремонт и укрепление бетонных конструкций, устранение трещин и повреждений.
Надежность и долговечность:
Мы применяем только проверенные материалы и новейшее оборудование, что гарантирует долговечность и надежность всех работ. Все наши проекты проходят строгий контроль качества на каждой стадии реализации.
Личный подход:
Каждому клиенту мы предлагаем персонализированные решения, учитывающие ваши требования и желания. Мы стремимся к тому, чтобы конечный результат полностью соответствовал вашим ожиданиям и требованиям.
Почему стоит выбрать Геракл24?
Работая с нами, вы найдете надежного партнера, который возьмет на себя все хлопоты по восстановлению и ремонту вашего здания. Мы обеспечиваем выполнение всех проектов в сроки, установленные договором и с соблюдением всех правил и норм. Обратившись в Геракл24, вы можете не сомневаться, что ваше строение в надежных руках.
Мы готовы предоставить консультацию и ответить на все ваши вопросы. Звоните нам, чтобы обсудить детали и узнать о наших сервисах. Мы сохраним и улучшим ваш дом, сделав его безопасным и комфортным для проживания на долгие годы.
Геракл24 – ваш выбор для реставрации и ремонта домов в Красноярске и области.
You reported that exceptionally well.|
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Андреас Стив и лучшие обзоры по психологии.
geinoutime.com
뜻밖에도… 이 대규모 반란은 학교 관계자에 의해 진압되었습니다.
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
ihrfuehrerschein.com
You Fang Jifan … 여전히 약간의 흑역사가 있고 여전히 우리에게 거짓말을하고 싶습니까?
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Корчагина И.Л. и новые обзоры по психиатрии.
Telegrass
האפליקציה היא פלטפורמה נפוצה בארץ לרכישת קנאביס באופן אינטרנטי. היא מספקת ממשק נוח ובטוח לקנייה ולקבלת שילוחים של פריטי צמח הקנאביס מגוונים. בסקירה זה נסקור את הרעיון שמאחורי טלגראס, כיצד זו עובדת ומהם היתרים מ השימוש בה.
מה זו האפליקציה?
טלגראס מהווה דרך לקנייה של צמח הקנאביס באמצעות היישומון טלגראם. היא נשענת על ערוצי תקשורת וקבוצות טלגרם ייעודיות הקרויות ״כיווני טלגראס״, שבהם ניתן להרכיב מרחב פריטי קנאביס ולקבל אותם ישירותית לשילוח. ערוצי התקשורת אלו מסודרים לפי איזורים גיאוגרפיים, כדי לשפר את קבלתם של המשלוחים.
כיצד זאת עובד?
התהליך פשוט יחסית. ראשית, צריך להצטרף לערוץ טלגראס הרלוונטי לאזור המגורים. שם אפשר לעיין בתפריטי הפריטים המגוונים ולהזמין את המוצרים הרצויים. לאחר ביצוע ההזמנה וסיום התשלום, השליח יופיע לכתובת שנרשמה עם הארגז שהוזמן.
רוב ערוצי הטלגראס מציעים טווח נרחב מ פריטים – זנים של קנאביס, ממתקים, שתייה ועוד. כמו כן, ניתן למצוא חוות דעת של צרכנים קודמים על איכות המוצרים והשירות.
יתרונות השימוש בפלטפורמה
יתרון מרכזי מ הפלטפורמה הינו הנוחות והדיסקרטיות. ההרכבה וההכנות מתבצעות מרחוק מאיזשהו מקום, בלי נחיצות בהתכנסות פיזי. כמו כן, הפלטפורמה מוגנת ביסודיות ומבטיחה סודיות גבוהה.
נוסף אל זאת, מחירי המוצרים בפלטפורמה נוטות להיות זולים, והשילוחים מגיעים במהירות ובהשקעה רבה. יש גם מוקד תמיכה זמין לכל שאלה או בעיה.
סיכום
טלגראס הווה שיטה חדשנית ויעילה לרכוש פריטי צמח הקנאביס בארץ. היא משלבת בין הנוחות הטכנולוגית של היישומון הפופולרי, לבין הזריזות והדיסקרטיות של דרך השילוח הישירה. ככל שהביקוש לקנאביס גדלה, פלטפורמות בדוגמת זו צפויות להמשיך ולצמוח.
b29
Bản cài đặt B29 IOS – Giải pháp vượt trội cho các tín đồ iOS
Trong thế giới công nghệ đầy sôi động hiện nay, trải nghiệm người dùng luôn là yếu tố then chốt. Với sự ra đời của Bản cài đặt B29 IOS, người dùng sẽ được hưởng trọn vẹn những tính năng ưu việt, mang đến sự hài lòng tuyệt đối. Hãy cùng khám phá những ưu điểm vượt trội của bản cài đặt này!
Tính bảo mật tối đa
Bản cài đặt B29 IOS được thiết kế với mục tiêu đảm bảo an toàn dữ liệu tuyệt đối cho người dùng. Nhờ hệ thống mã hóa hiện đại, thông tin cá nhân và dữ liệu nhạy cảm của bạn luôn được bảo vệ an toàn khỏi những kẻ xâm nhập trái phép.
Trải nghiệm người dùng đỉnh cao
Giao diện thân thiện, đơn giản nhưng không kém phần hiện đại, B29 IOS mang đến cho người dùng trải nghiệm duyệt web, truy cập ứng dụng và sử dụng thiết bị một cách trôi chảy, mượt mà. Các tính năng thông minh được tối ưu hóa, giúp nâng cao hiệu suất và tiết kiệm pin đáng kể.
Tính tương thích rộng rãi
Bản cài đặt B29 IOS được phát triển với mục tiêu tương thích với mọi thiết bị iOS từ các dòng iPhone, iPad cho đến iPod Touch. Dù là người dùng mới hay lâu năm của hệ điều hành iOS, B29 đều mang đến sự hài lòng tuyệt đối.
Quá trình cài đặt đơn giản
Với những hướng dẫn chi tiết, việc cài đặt B29 IOS trở nên nhanh chóng và dễ dàng. Chỉ với vài thao tác đơn giản, bạn đã có thể trải nghiệm ngay tất cả những tính năng tuyệt vời mà bản cài đặt này mang lại.
Bản cài đặt B29 IOS không chỉ là một bản cài đặt đơn thuần, mà còn là giải pháp công nghệ hiện đại, nâng tầm trải nghiệm người dùng lên một tầm cao mới. Hãy trở thành một phần của cộng đồng sử dụng B29 IOS để khám phá những tiện ích tuyệt vời mà nó có thể mang lại!
Заметки по общей лингвистике и популярные книги по психологии.
Как сберечь свои личные данные: страхуйтесь от утечек информации в интернете. Сегодня обеспечение безопасности своих данных становится всё больше важной задачей. Одним из наиболее распространенных способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и в какой мере защититься от их утечки? Что такое «сит фразы»? «Сит фразы» — это синтезы слов или фраз, которые бывают используются для получения доступа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или дополнительные конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, при помощи этих сит фраз. Как защитить свои личные данные? Используйте запутанные пароли. Избегайте использования простых паролей, которые мгновенно угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого из аккаунта. Не воспользуйтесь один и тот же пароль для разных сервисов. Используйте двухэтапную аутентификацию (2FA). Это добавляет дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт посредством другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте личную информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы сохранить свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может привести к серьезным последствиям, таким подобно кража личной информации и финансовых потерь. Чтобы защитить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
venopluss8.com
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
100 лет тому вперед 1080. 100 лет тому вперед фильм смотреть онлайн бесплатно 2024. 100 лет тому вперед фильм смотреть онлайн бесплатно в хорошем. 100 лет тому вперед фильм смотреть онлайн бесплатно 2024.
Carpe diem
טלגראס כיוונים
האפליקציה הווה תוכנה רווחת בארץ לרכישת מריחואנה בצורה אינטרנטי. זו מספקת ממשק משתמש פשוט לשימוש ומאובטח לקנייה ולקבלת שילוחים מ מוצרי צמח הקנאביס שונים. במאמר זו נסקור עם העיקרון מאחורי הפלטפורמה, כיצד היא פועלת ומה היתרונות של השימוש בזו.
מהי הפלטפורמה?
הפלטפורמה הווה אמצעי לקנייה של צמח הקנאביס דרך היישומון טלגרם. זו נשענת מעל ערוצי תקשורת וקבוצות טלגראם ייעודיות הנקראות ״כיווני טלגראס״, שם ניתן להרכיב מרחב פריטי צמח הקנאביס ולקבלת אותם ישירות למשלוח. ערוצי התקשורת אלו מאורגנים לפי איזורים גיאוגרפיים, במטרה לשפר את קבלת השילוחים.
כיצד זה עובד?
התהליך פשוט למדי. קודם כל, צריך להצטרף לערוץ הטלגראס הנוגע לאזור המגורים. שם אפשר לצפות בתפריטים של הפריטים השונים ולהרכיב עם הפריטים המבוקשים. לאחר ביצוע ההזמנה וסגירת התשלום, השליח יופיע בכתובת שנרשמה ועמו הארגז שהוזמן.
רוב ערוצי הטלגראס מציעים טווח רחב של פריטים – סוגי מריחואנה, עוגיות, שתייה ועוד. כמו כן, ניתן למצוא חוות דעת של לקוחות קודמים על איכות המוצרים והשירות.
יתרונות השימוש באפליקציה
יתרון עיקרי של האפליקציה הינו הנוחות והדיסקרטיות. ההרכבה וההכנות מתבצעות מרחוק מאיזשהו מקום, ללא נחיצות בהתכנסות פיזי. כמו כן, האפליקציה מאובטחת ביסודיות ומבטיחה חיסיון גבוהה.
נוסף אל זאת, עלויות המוצרים בטלגראס נוטות לבוא זולים, והשילוחים מגיעים במהירות ובמסירות גבוהה. קיים גם מוקד תמיכה זמין לכל שאלה או בעיית.
סיכום
טלגראס מהווה שיטה חדשנית ויעילה לרכוש פריטי צמח הקנאביס בישראל. זו משלבת את הנוחיות הטכנולוגית מ האפליקציה הפופולרי, לבין הזריזות והפרטיות מ שיטת השילוח הישירה. ככל שהדרישה למריחואנה גובר, אפליקציות כמו טלגראס צפויות להמשיך ולצמוח.
отмывание usdt
Как обезопасить свои данные: страхуйтесь от утечек информации в интернете. Сегодня защита информации становится более насущной важной задачей. Одним из наиболее популярных способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и в какой мере обезопаситься от их утечки? Что такое «сит фразы»? «Сит фразы» — это комбинации слов или фраз, которые регулярно используются для получения доступа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или другие конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, при помощи этих сит фраз. Как защитить свои личные данные? Используйте сложные пароли. Избегайте использования легких паролей, которые просто угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого из аккаунта. Не используйте один и тот же пароль для разных сервисов. Используйте двухэтапную аутентификацию (2FA). Это прибавляет дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт путем другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте персональную информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы сохранить свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может спровоцировать серьезным последствиям, таким подобно кража личной информации и финансовых потерь. Чтобы обезопасить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
Оградите собственные USDT: Проверяйте операцию TRC20 перед отсылкой
Виртуальные деньги, подобные как USDT (Tether) на распределенном реестре TRON (TRC20), делаются всё более популярными в области сфере децентрализованных финансов. Но вместе со повышением востребованности повышается и опасность ошибок или обмана при переводе финансов. Именно именно поэтому важно проверять перевод USDT TRC20 перед её отправкой.
Ошибка во время вводе адреса получателя адресата либо пересылка по некорректный адрес получателя сможет привести к необратимой потере ваших USDT. Жулики тоже могут пытаться обмануть вас, посылая ложные адреса для транзакции. Потеря криптовалюты вследствие таких ошибок сможет обернуться серьезными финансовыми потерями.
Впрочем, имеются специализированные сервисы, дающие возможность проверить перевод USDT TRC20 перед ее отправкой. Некий из подобных сервисов дает опцию наблюдать а также изучать операции на блокчейне TRON.
На данном обслуживании вы сможете вводить адрес получателя и получать подробную информацию о адресе, включая в том числе архив операций, баланс и состояние аккаунта. Данное поможет выяснить, есть или нет адрес истинным и надежным для пересылки финансов.
Прочие службы также предоставляют аналогичные опции для удостоверения операций USDT TRC20. Некоторые кошельки для криптовалют по крипто имеют интегрированные возможности по контроля адресов получателей и операций.
Не игнорируйте удостоверением перевода USDT TRC20 перед ее пересылкой. Крохотная осмотрительность сможет сберечь вам много денег и избежать утрату твоих дорогих криптовалютных ресурсов. Задействуйте заслуживающие доверия сервисы для достижения безопасности ваших транзакций и целостности ваших USDT в блокчейне TRON.
Cogito ergo sum
В процессе взаимодействии с виртуальной валютой USDT в блокчейне TRON (TRC20) чрезвычайно важно не просто удостоверять адрес получателя перед отправкой средств, а также и систематически мониторить остаток личного кошелька, и источники входящих транзакций. Это позволит своевременно обнаружить любые нежданные операции и не допустить вероятные издержки.
В первую очередь, нужно проверить в правильности показываемого баланса USDT TRC20 в собственном криптокошельке. Рекомендуется сверять информацию с данными публичных обозревателей блокчейна, для того чтобы избежать возможность компрометации или скомпрометирования самого крипто-кошелька.
Но исключительно наблюдения баланса недостаточно. Чрезвычайно важно анализировать историю поступающих переводов и этих происхождение. Если вы обнаружите переводы USDT с анонимных или сомнительных реквизитов, сразу же заблокируйте эти средства. Есть угроза, чтобы данные криптомонеты стали получены.
Наше сервис предоставляет возможности для углубленного исследования поступающих USDT TRC20 переводов относительно этой легальности а также неимения связи с криминальной активностью. Мы обеспечим вам безопасную работу с этой распространенной стейблкоин-монетой.
Плюс к этому следует регулярно отправлять USDT TRC20 на безопасные неконтролируемые криптовалютные кошельки находящиеся под собственным полным управлением. Хранение монет на сторонних платформах неизменно связано с рисками взломов а также утраты финансов вследствие программных сбоев либо несостоятельности платформы.
Следуйте основные меры безопасности, будьте внимательны а также вовремя мониторьте остаток а также источники поступлений USDT TRC20 кошелька. Данные действия дадут возможность защитить Ваши электронные активы от незаконного завладения и потенциальных юридических проблем в будущем.
Carpe diem
provadenta.com
Your style is unique compared to other people I’ve read stuff from.
Thank you for posting when you광양출장샵’ve got the opportunity, Guess
Per aspera ad astra
https://618-27-83.ru/
– RamenBet казино
100 лет тому вперед смотреть. Фильм 100 лет тому вперед смотреть онлайн.
沖ドキ!
非常に興味深い記事でした。新たな知識をありがとう。
Секреты оформления пропуска на МКАД, Как быстро получить пропуск на МКАД, секреты, которую важно помнить, основные требования, которые помогут вам разобраться, подробный обзор, Пропуск на МКАД: основные преимущества, Как продлить пропуск на МКАД, полный гайд
Проверить пропуск на мкад Пропуск на мкад .
Актуальность подтверждения транзакции USDT в сети TRC20
Платежи USDT в рамках сети TRC20 демонстрируют растущую активность, однако следует являться особенно аккуратными во время этих обработке.
Такой форма платежей нередко привлекается в процессе отмывания денежных средств, приобретенных криминальным образом.
Ключевой факторов риска получения USDT TRC-20 – это такие платежи вероятно будут получены вследствие разнообразных моделей обмана, таких как похищения конфиденциальной информации, принуждение, взломы а также дополнительные противоправные действия. Обрабатывая подобные платежи, клиент неизменно оказываетесь соучастником незаконной активности.
Таким образом повышенно существенно глубоко анализировать происхождение различных поступающего транзакции в USDT в сети TRC20. Обязательно запрашивать от перевододателя сведения относительно легитимности денежных средств, при минимальных сомнениях – воздерживаться данные транзакций.
Осознавайте, в ситуации, когда в результате обнаружения незаконных происхождений финансов, вы скорее всего будете подвергнуты с применением санкциям вместе вместе с отправителем. В связи с этим целесообразнее подстраховаться а также тщательно проверять всевозможный платеж, нацело подвергать опасности своей репутацией наряду с быть втянутым под значительные судебные трудности.
Поддержание осторожности при работе по USDT по сети TRC20 – является ключ финансовой финансовой защищенности как и избежание попадания в преступные практики. Оставайтесь осторожны а также постоянно анализируйте природу цифровых валютных финансов.
100 лет тому вперед фильм 2024 смотреть. 100 лет тому вперед фильм 2024 смотреть.
Подробная инструкция по оформлению пропуска на МКАД, основные моменты, Важная информация о пропуске на МКАД, Список требуемых документов для пропуска на МКАД, полный гайд, которые помогут вам разобраться, основные моменты, советы, важные детали, полный гайд
Пропуск на мкад Пропуск в москву .
Заголовок: Обязательно проверяйте адресе адресата во время транзакции USDT TRC20
При деятельности со крипто, особенно со USDT в распределенном реестре TRON (TRC20), чрезвычайно нужно проявлять бдительность а также аккуратность. Одна среди наиболее частых погрешностей, которую совершают юзеры – отправка средств по неверный адресу. Чтобы предотвратить лишение собственных USDT, нужно всегда внимательно контролировать адресе адресата до передачей перевода.
Цифровые адреса кошельков являют собой длинные наборы букв а также чисел, например, TRX9QahiFUYfHffieZThuzHbkndWvvfzThB8U. Даже незначительная ошибка либо оплошность во время копировании адреса может привести к тому, чтобы твои монеты станут безвозвратно утрачены, так как они попадут на неконтролируемый тобой криптокошелек.
Присутствуют различные способы проверки адресов кошельков USDT TRC20:
1. Глазомерная ревизия. Тщательно сверьте адрес во твоём кошельке со адресом реципиента. При небольшом расхождении – не совершайте транзакцию.
2. Использование онлайн-сервисов контроля.
3. Двойная проверка с реципиентом. Обратитесь с просьбой к адресату удостоверить корректность адреса кошелька перед передачей операции.
4. Тестовый операция. При значительной сумме перевода, допустимо сначала передать незначительное количество USDT с целью проверки адреса.
Сверх того советуется содержать крипто на личных кошельках, а не на биржах либо сторонних службах, для того чтобы обладать полный управление над собственными активами.
Не пренебрегайте контролем адресов при взаимодействии со USDT TRC20. Данная несложная мера безопасности поможет обезопасить твои финансы против непреднамеренной потери. Помните, чтобы на мире крипто операции неотменимы, и отправленные монеты по ошибочный адрес кошелька вернуть почти невозможно. Пребывайте осторожны и аккуратны, для того чтобы защитить собственные инвестиции.
Подробная инструкция по оформлению пропуска на МКАД, Срочное оформление пропуска на МКАД, Основные аспекты пропуска на МКАД, которую важно помнить, Часто задаваемые вопросы о пропуске на МКАД, Информация о стоимости и сроках пропуска на МКАД, Эффективные способы получения пропуска для МКАД, Какие преимущества дает пропуск на МКАД, Инструкция по продлению пропуска на МКАД, полный гайд
Проверить пропуск на мкад Проверить пропуск на мкад .
100 лет тому вперед смотреть. Смотреть 100 лет тому вперед фильм.
Привет игроманы!
Я давно увлекаюсь онлайн казино и, как многие из вас, всегда искал платформу, которая бы соответствовала всем моим требованиям. Искал и . Перепробовал множество сайтов, но постоянно сталкивался с различными проблемами: неудобный интерфейс, задержки с выплатами, отсутствие нормальной поддержки, да и просто скучный набор игр. В какой-то момент я почти потерял надежду, но решил попробовать еще один раз и наконец-то нашел Telegram . Вот несколько причин, почему я считаю его идеальным:
– Удобный интерфейс: сайт очень удобный и понятный, даже для новичков. Все нужные разделы под рукой, ничего лишнего.
– Мгновенные выплаты: проверил на себе – выигрыш приходит на счет практически моментально.
– Отличная поддержка: техподдержка реально работает и помогает решить любые проблемы. Причем они доступны 24/7.
– Широкий выбор игр: тут есть все – от классических слотов до живых дилеров. И постоянно добавляют что-то новое.
– Бонусы и акции: щедрые приветственные бонусы и регулярные акции. Всегда приятно получать дополнительные фриспины или бонусы за пополнение счета.
Понимаю, что каждому свое, но лично для меня стало настоящей находкой. Если вы тоже устали искать, рекомендую попробовать. Возможно, оно станет вашим новым любимым местом для игры.
Если у кого-то уже есть опыт игры на этом сайте, делитесь своими впечатлениями! Интересно узнать ваше мнение.
Удачи и больших выигрышей всем!
werankcities.com
Fang Jifan의 두 제자가 고등학교 순위에서 1 위를 차지한 것도 놀라운 일이 아닙니다.
Подробная инструкция по оформлению пропуска на МКАД, Как быстро получить пропуск на МКАД, секреты, которую нужно знать, Основные вопросы о пропуске на МКАД, которые важно учесть, подробный обзор, рекомендации, важные детали, полный гайд
Пропуск на мкад Пропуск в москву .
Фоллаут смотреть онлайн
Секреты оформления пропуска на МКАД, Как быстро получить пропуск на МКАД, Важная информация о пропуске на МКАД, Какие документы нужны для оформления пропуска на МКАД, полный гайд, Пропуск на МКАД: сроки и стоимость, Как получить пропуск для поездок по МКАД, Какие преимущества дает пропуск на МКАД, Сроки и порядок продления пропуска на МКАД, шаг за шагом
Проверить пропуск на мкад Проверить пропуск на мкад .
Секреты оформления пропуска на МКАД, советы, Ключевые моменты о пропуске на МКАД, которую стоит учесть, подробная инструкция, Пропуск на МКАД: сроки и стоимость, Как оформить пропуск для движения по МКАД, Пропуск на МКАД: основные преимущества, основные аспекты, подробная информация
Проверить пропуск на мкад Пропуск на мкад .
Фоллаут 2 сезон 2024
5 шагов для успешного ремонта телевизора: полезные советы и рекомендации|Как не попасть на мошенников при ремонте телевизора: важные критерии отбора|Что делать, если телевизор сломался: полезные советы от профессионалов|Эффективные методы самодиагностики телевизора: шаг за шагом|Цены на ремонт телевизоров: как не переплатить и получить качественный сервис|Профессиональный подход к ремонту телевизоров: как выбрать лучший сервис для восстановления работы техники|Лучшие специалисты по ремонту телевизоров: где найти и как выбрать|Профилактика и уход за телевизорами: как обеспечить долговечность и надежность|Самые распространенные причины, почему телевизоры перестают работать и как их устранить|Оригинальные детали и запчасти для телевизоров: где заказать и как выбрать|Почему лучше доверить ремонт телевизора профессионалам: основные преимущества|Что нужно знать перед ремонтом телевизора: важные советы и рекомендации|Способы определения проблемы с телевизором: как быстро и эффективно выявить причины|Опасности и недостатки самостоятельного ремонта телевизора: важные моменты и советы|Как быстро вернуть телевизор в строй после поломки: проверенные способы и техники
заправка картриджей Воркута ремонт ноутбуков Воркута .
טלגראס מהווה תוכנה מקובלת בישראל לרכישת מריחואנה בצורה וירטואלי. זו מספקת ממשק פשוט לשימוש ובטוח לקנייה ולקבלת משלוחים מ פריטי מריחואנה מגוונים. במאמר זו נסקור את הרעיון שמאחורי האפליקציה, כיצד היא עובדת ומה היתרונות של השימוש בה.
מהי הפלטפורמה?
הפלטפורמה הווה שיטה לרכישת צמח הקנאביס באמצעות האפליקציה טלגראם. היא נשענת מעל ערוצי תקשורת וקבוצות טלגראם מיוחדות הנקראות ״טלגראס כיוונים, שבהם אפשר להרכיב מרחב פריטי קנאביס ולקבלת אלו ישירות לשילוח. הערוצים אלו מסודרים על פי אזורים גיאוגרפיים, במטרה להקל את קבלת השילוחים.
כיצד זה פועל?
התהליך פשוט למדי. ראשית, צריך להצטרף לערוץ הטלגראס הרלוונטי לאזור המגורים. שם אפשר לעיין בתפריטי המוצרים השונים ולהרכיב את המוצרים הרצויים. לאחר השלמת ההרכבה וסיום התשלום, השליח יופיע לכתובת שנרשמה ועמו הארגז המוזמנת.
מרבית ערוצי הטלגראס מספקים טווח רחב של פריטים – סוגי קנאביס, עוגיות, משקאות ועוד. בנוסף, אפשר למצוא חוות דעת של לקוחות שעברו לגבי רמת הפריטים והשרות.
מעלות הנעשה בפלטפורמה
יתרון מרכזי של האפליקציה הוא הנוחיות והפרטיות. ההרכבה וההכנות מתבצעות ממרחק מאיזשהו מקום, ללא צורך בהתכנסות פיזי. בנוסף, האפליקציה מוגנת ביסודיות ומבטיחה סודיות גבוה.
נוסף אל כך, מחירי הפריטים בפלטפורמה נוטות להיות זולים, והמשלוחים מגיעים במהירות ובמסירות גבוהה. קיים גם מוקד תמיכה זמין לכל שאלה או בעיה.
סיכום
הפלטפורמה הינה שיטה חדשנית ויעילה לקנות פריטי מריחואנה בישראל. זו משלבת את הנוחיות הטכנולוגית מ היישומון הפופולרי, לבין הזריזות והפרטיות מ דרך המשלוח הישירות. ככל שהביקוש לצמח הקנאביס גדלה, אפליקציות כמו זו צפויות להמשיך ולצמוח.
Геракл24: Профессиональная Реставрация Основания, Венцов, Полов и Перенос Строений
Фирма Gerakl24 специализируется на предоставлении полных работ по замене основания, венцов, полов и перемещению зданий в месте Красноярске и в окрестностях. Наш коллектив опытных мастеров обеспечивает высокое качество выполнения всех типов ремонтных работ, будь то древесные, с каркасом, из кирпича или бетонные дома.
Плюсы сотрудничества с Геракл24
Квалификация и стаж:
Все работы осуществляются исключительно профессиональными мастерами, имеющими большой опыт в направлении возведения и ремонта зданий. Наши специалисты эксперты в своей области и реализуют проекты с максимальной точностью и учетом всех деталей.
Комплексный подход:
Мы осуществляем все виды работ по реставрации и реконструкции строений:
Смена основания: укрепление и замена старого фундамента, что позволяет продлить срок службы вашего дома и предотвратить проблемы, связанные с оседанием и деформацией.
Смена венцов: восстановление нижних венцов деревянных зданий, которые наиболее часто подвергаются гниению и разрушению.
Установка новых покрытий: установка новых полов, что кардинально улучшает внешний вид и практическую полезность.
Перемещение зданий: безопасное и надежное перемещение зданий на новые локации, что обеспечивает сохранение строения и предотвращает лишние расходы на создание нового.
Работа с различными типами строений:
Древесные строения: реставрация и усиление деревянных элементов, защита от разрушения и вредителей.
Дома с каркасом: укрепление каркасов и замена поврежденных элементов.
Кирпичные дома: реставрация кирпичной кладки и усиление стен.
Бетонные строения: реставрация и усиление бетонных элементов, устранение трещин и повреждений.
Качество и надежность:
Мы применяем только проверенные материалы и передовые технологии, что гарантирует долгий срок службы и прочность всех выполненных задач. Каждый наш проект проходят тщательную проверку качества на каждой стадии реализации.
Личный подход:
Мы предлагаем каждому клиенту подходящие решения, учитывающие все особенности и пожелания. Наша цель – чтобы результат нашей работы полностью удовлетворял вашим ожиданиям и требованиям.
Зачем обращаться в Геракл24?
Обратившись к нам, вы приобретете надежного партнера, который возьмет на себя все хлопоты по ремонту и реконструкции вашего строения. Мы обеспечиваем выполнение всех задач в сроки, оговоренные заранее и с соблюдением всех строительных норм и стандартов. Обратившись в Геракл24, вы можете не сомневаться, что ваш дом в надежных руках.
Мы всегда готовы проконсультировать и дать ответы на все вопросы. Контактируйте с нами, чтобы обсудить ваш проект и узнать больше о наших услугах. Мы обеспечим сохранение и улучшение вашего дома, сделав его безопасным и комфортным для проживания на долгие годы.
Gerakl24 – ваш выбор для реставрации и ремонта домов в Красноярске и области.
Как похудеть
На следующий день был их «полезный» завтрак впервые в жизни. Как оказалось, овощи в омлете не так уж и плохи. А если закрыть глаза, можно даже представить, что это фаст-фуд:
—Даже не думала, что сюда так отлично эта овощная смесь впишется! На обед супчик и гречка с курицей на пару, на вечер еще не придумала. После работы прогуляемся, да, Маша?
—Да! Хочу! Мама, а почему у нас не хлопья на завтрак сегодня? Ну там, шоколадные хотя бы.
—С этого дня у нас другой рацион. И этот лишний сахар нам совсем не нужен.
индивид вовсе не предусматривал из уст собственной избранницы Татьяны. Внутри их собственной семье фигура физической оболочки совсем была иной по сравнению с типовой а также распространённой – иметь предожирение абсолютная стандарт.
Bản cài đặt B29 IOS – Giải pháp vượt trội cho các tín đồ iOS
Trong thế giới công nghệ đầy sôi động hiện nay, trải nghiệm người dùng luôn là yếu tố then chốt. Với sự ra đời của Bản cài đặt B29 IOS, người dùng sẽ được hưởng trọn vẹn những tính năng ưu việt, mang đến sự hài lòng tuyệt đối. Hãy cùng khám phá những ưu điểm vượt trội của bản cài đặt này!
Tính bảo mật tối đa
Bản cài đặt B29 IOS được thiết kế với mục tiêu đảm bảo an toàn dữ liệu tuyệt đối cho người dùng. Nhờ hệ thống mã hóa hiện đại, thông tin cá nhân và dữ liệu nhạy cảm của bạn luôn được bảo vệ an toàn khỏi những kẻ xâm nhập trái phép.
Trải nghiệm người dùng đỉnh cao
Giao diện thân thiện, đơn giản nhưng không kém phần hiện đại, B29 IOS mang đến cho người dùng trải nghiệm duyệt web, truy cập ứng dụng và sử dụng thiết bị một cách trôi chảy, mượt mà. Các tính năng thông minh được tối ưu hóa, giúp nâng cao hiệu suất và tiết kiệm pin đáng kể.
Tính tương thích rộng rãi
Bản cài đặt B29 IOS được phát triển với mục tiêu tương thích với mọi thiết bị iOS từ các dòng iPhone, iPad cho đến iPod Touch. Dù là người dùng mới hay lâu năm của hệ điều hành iOS, B29 đều mang đến sự hài lòng tuyệt đối.
Quá trình cài đặt đơn giản
Với những hướng dẫn chi tiết, việc cài đặt B29 IOS trở nên nhanh chóng và dễ dàng. Chỉ với vài thao tác đơn giản, bạn đã có thể trải nghiệm ngay tất cả những tính năng tuyệt vời mà bản cài đặt này mang lại.
Bản cài đặt B29 IOS không chỉ là một bản cài đặt đơn thuần, mà còn là giải pháp công nghệ hiện đại, nâng tầm trải nghiệm người dùng lên một tầm cao mới. Hãy trở thành một phần của cộng đồng sử dụng B29 IOS để khám phá những tiện ích tuyệt vời mà nó có thể mang lại!
?Her phrase sounded with a special chuckle. It’s obvious that she didn’t believe this obese man: what food lover can give up food? Taking the tray, he retired to the table with doubts. But the very awareness that he supported his beloved and did not abandon her in a difficult moment — already satiated him completely. It turns out that buckwheat is also tasty, and without mayonnaise. The salad has an unusual pleasant sourness, almost like chips. And the compote is even nicer than the foreign soda — that’s how much he wanted to support Tanya! Coming to the shop, he had a very unusual conversation, which he did not expect himself:
— Petrovich, why did you decide to lose weight? Lyudka has already reported everything to us. Have you decided to become an athlete in your years?
— Yes, my wife’s viper-friends are attacking her! They have so bullied her that she decided to put all of us on a weight loss program. The poor thing almost cries when she thinks about it.
— Wait, is that our Tanya from the accounting department? The one with dark hair. Well, what kind of friends are offending her there?
— Yes, my beauty. But it’s Victoria Gronich who teases her the most, if you know her.
— Wait, the Gronich family! So these are my neighbors, they’ve been fighting ungodly every day! I’ll have a talk with her, for sure.
thebuzzerpodcast.com
물론… 지금은 그런 사람과 말, 많은 기업들이 훈련을 하고 있습니다.
https://roserica.ru/
– RamenBet
Уэнздей 1 сезон смотреть
Почему теневой плинтус – красивая и практичная деталь интерьера,
Советы по монтажу теневого плинтуса без дополнительной помощи,
Как использовать теневой плинтус для создания уникального интерьера,
Теневой плинтус: классический стиль в современном исполнении,
Гармония оттенков: выбор цвета теневого плинтуса для любого интерьера,
Теневой плинтус: простое решение для скрытия кабелей и проводов,
Теневой плинтус с подсветкой: создаем эффектное освещение в интерьере,
Современные тренды в использовании теневого плинтуса для уюта и красоты,
Интерьер безупречный до мелочей: роль теневого плинтуса в декоре
алюминиевые плинтуса напольные https://plintus-tenevoj-aljuminievyj-msk.ru/ .
זכו הבאים לאזור הידע והמידע והתרומה הרשמי והמוסמך של טלגרם אופקים! בנקודה זו רשאים לאתר את מלוא המידע והפרטים העדכני והמעודכן ביותר זמין בעניין פלטפורמה טלגרמות ואופני להפעלתה כנדרש.
מה מציין טלגרמות מסלולים?
טלגרם מסלולים מייצגת מנגנון הנסמכת על טלגראס המספקת לתפוצה ורכישה סביב מריחואנה וקנבי בארץ. באופן של הפרסומים והפורומים בטלגראס, פעילים רשאים לקנות ולהשיג את מוצרי דשא בצורה קל ומהיר.
כיצד להתחיל בפלטפורמת טלגרם?
לשם להתחבר בשימוש נכון בטלגרם, אתם נדרשים להצטרף ל לקבוצות ולמסגרות המומלצים. במיקום זה באתר זה רשאים לאתר רשימה מתוך מסלולים לקבוצות פעילים וימינים. לאחר מכן, ניתן להתחבר במסלול ההזמנה והסיפוק סביב אספקת הדשא.
הדרכות ופרטים
באתר זה ניתן למצוא סוגים מבין הוראות והסברים מלאים אודות היישום בטלגרם, בכלל:
– החברות לקבוצות מומלצים
– סדרת האספקה
– בטיחות והגנה בשילוב בטלגראס
– והרבה נתונים אחר
קישורים איכותיים
לגבי נושא זה צירים לערוצים ולמסגרות רצויים בטלגרם:
– פורום המידע הרשמי
– פורום הסיוע והעזרה לצרכנים
– מקום לקבלת מוצרי דשא אמינים
– מבחר נקודות מריחואנה מובטחות
מערך מעניקים אתכם עקב הפעילות שלכם לפורטל המידע והידע מטעם טלגרמות נתיבים ומתקווים לכם חוויית קנייה נעימה ואמינה!
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Король и шут 2 сезон смотреть онлайн
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Король и шут 2 сезон фильм
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
animehangover.com
아무래도…
k8 カジノ
毎回このブログを読むのが楽しみです。素敵な記事をありがとう。
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
geinoutime.com
“뭐라고?” 왕화는 기절, 잘못, 잘못된 약을 먹었습니까?
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Замена венцов красноярск
Геракл24: Опытная Смена Основания, Венцов, Полов и Перенос Зданий
Фирма Геракл24 профессионально занимается на оказании всесторонних услуг по смене основания, венцов, настилов и переносу строений в городе Красноярске и в окрестностях. Наша группа профессиональных специалистов гарантирует отличное качество выполнения всех видов ремонтных работ, будь то древесные, каркасные, кирпичные постройки или из бетона строения.
Достоинства услуг Gerakl24
Профессионализм и опыт:
Каждая задача осуществляются только высококвалифицированными мастерами, с многолетним многолетний стаж в области возведения и восстановления строений. Наши специалисты знают свое дело и выполняют работу с высочайшей точностью и вниманием к мелочам.
Всесторонний подход:
Мы предоставляем полный спектр услуг по реставрации и реконструкции строений:
Смена основания: укрепление и замена старого фундамента, что гарантирует долговечность вашего строения и предотвратить проблемы, вызванные оседанием и деформацией.
Смена венцов: замена нижних венцов деревянных домов, которые наиболее часто гниют и разрушаются.
Замена полов: монтаж новых настилов, что значительно улучшает визуальное восприятие и практическую полезность.
Передвижение домов: безопасное и надежное перемещение зданий на новые локации, что обеспечивает сохранение строения и предотвращает лишние расходы на создание нового.
Работа с любыми типами домов:
Деревянные дома: реставрация и усиление деревянных элементов, обработка от гниения и насекомых.
Каркасные дома: усиление каркасных конструкций и замена поврежденных элементов.
Кирпичные дома: восстановление кирпичной кладки и укрепление конструкций.
Дома из бетона: реставрация и усиление бетонных элементов, исправление трещин и разрушений.
Качество и прочность:
Мы работаем с только высококачественные материалы и передовые технологии, что гарантирует долгий срок службы и прочность всех выполненных задач. Все проекты проходят тщательную проверку качества на всех этапах выполнения.
Личный подход:
Мы предлагаем каждому клиенту персонализированные решения, учитывающие все особенности и пожелания. Мы стремимся к тому, чтобы конечный результат соответствовал вашим запросам и желаниям.
Почему стоит выбрать Геракл24?
Обратившись к нам, вы приобретете надежного партнера, который берет на себя все заботы по ремонту и реставрации вашего дома. Мы гарантируем выполнение всех работ в сроки, установленные договором и с соблюдением всех строительных норм и стандартов. Выбрав Геракл24, вы можете быть уверены, что ваш дом в надежных руках.
Мы всегда готовы проконсультировать и дать ответы на все вопросы. Контактируйте с нами, чтобы обсудить ваш проект и узнать больше о наших услугах. Мы сохраним и улучшим ваш дом, обеспечив его безопасность и комфорт на долгие годы.
Gerakl24 – ваш надежный партнер в реставрации и ремонте домов в Красноярске и за его пределами.
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello!
This post was created with 2ssdsd3222aa.com
Hello!
This post was created with 2ssdsd3222aa.com
Hello.
This post was created with 2ssdsd3222aa.com
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Уэнздей 2 сезон смотреть онлайн
Akarslot777
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Фоллаут 1 сезон смотреть
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Майор Гром 2024
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
казино рф
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Teeth whitening prodentim en-prodentim.com
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
mikaspa.com
싱크대는 멀리 유리 작업장으로 바로 연결되며 냉각을 위해 많은 양의 물이 사용됩니다.
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Работая в сео, нужно знать, что нельзя одним способом вывести сайт в верхние позиции поисковых систем, так как системы поиска это подобны треку с финишной прямой, а интернет-ресурсы это гоночные машины, которые все желают быть на первом месте.
Так вот:
Перечень – Для того чтобы сайт был приспособлен и быстрым, важна
улучшение
Сайт должен иметь только уникальный контент, это тексты и изображения
ОБЯЗАТЕЛЬНО набор ссылок через сайты статейники и напрямую на главную
Увеличение беклинков с использованием сайтов второго уровня
Ссылочная структура, это ссылки Tier-1, Tier-2, Tier-3
И самое главное это личная сеть веб-сайтов PBN, которая подключается на основной сайт
Все сайты сети PBN должны быть без отпечатков, т.е. системы поиска не должны понимать, что это один собственник всех веб-сайтов, поэтому крайне важно соблюдать все эти правила.
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Bu oyundan ne kadar memnun kaldigimi paylasmak most-bet-cz100.com istiyorum. Oyun ilk dakikadan itibaren surukleyici ve finale kadar merak uyandiriyor. Grafikler mukemmel ve muzik surukleyici. Oynanis ilginc ve her zaman ilgi cekici. Kaliteli oyuncaklari deger veren herkese tavsiye ederim!
Gerakl24: Опытная Смена Основания, Венцов, Настилов и Передвижение Зданий
Компания Gerakl24 профессионально занимается на выполнении комплексных работ по смене основания, венцов, полов и передвижению домов в городе Красноярском регионе и в окрестностях. Наша команда профессиональных мастеров гарантирует высокое качество выполнения всех типов ремонтных работ, будь то деревянные, с каркасом, из кирпича или бетонные дома.
Преимущества работы с Gerakl24
Навыки и знания:
Все работы проводятся только опытными мастерами, с многолетним многолетний стаж в области создания и ремонта зданий. Наши мастера эксперты в своей области и реализуют работу с безупречной точностью и вниманием к мелочам.
Полный спектр услуг:
Мы осуществляем все виды работ по восстановлению и ремонту домов:
Смена основания: замена и укрепление фундамента, что позволяет продлить срок службы вашего здания и избежать проблем, связанные с оседанием и деформацией.
Реставрация венцов: восстановление нижних венцов деревянных зданий, которые наиболее часто подвергаются гниению и разрушению.
Установка новых покрытий: замена старых полов, что значительно улучшает визуальное восприятие и практическую полезность.
Перенос строений: качественный и безопасный перенос строений на новые локации, что обеспечивает сохранение строения и предотвращает лишние расходы на строительство нового.
Работа с любыми видами зданий:
Дома из дерева: восстановление и укрепление деревянных конструкций, обработка от гниения и насекомых.
Каркасные строения: укрепление каркасов и реставрация поврежденных элементов.
Дома из кирпича: восстановление кирпичной кладки и укрепление конструкций.
Бетонные дома: реставрация и усиление бетонных элементов, устранение трещин и повреждений.
Качество и прочность:
Мы применяем только проверенные материалы и современное оборудование, что гарантирует долгий срок службы и прочность всех выполненных задач. Все наши проекты проходят строгий контроль качества на каждом этапе выполнения.
Персонализированный подход:
Мы предлагаем каждому клиенту персонализированные решения, с учетом всех особенностей и пожеланий. Мы стремимся к тому, чтобы итог нашей работы полностью соответствовал вашим запросам и желаниям.
Почему стоит выбрать Геракл24?
Работая с нами, вы приобретете надежного партнера, который берет на себя все заботы по ремонту и реконструкции вашего строения. Мы гарантируем выполнение всех проектов в установленные сроки и с соблюдением всех правил и норм. Связавшись с Геракл24, вы можете быть уверены, что ваше здание в надежных руках.
Мы всегда готовы проконсультировать и ответить на ваши вопросы. Контактируйте с нами, чтобы обсудить ваш проект и узнать о наших сервисах. Мы поможем вам сохранить и улучшить ваш дом, сделав его уютным и безопасным для долгого проживания.
Gerakl24 – ваш партнер по реставрации и ремонту домов в Красноярске и окрестностях.
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
娛樂城
線上娛樂城的世界
隨著互聯網的迅速發展,線上娛樂城(在線賭場)已經成為許多人消遣的新選擇。在線娛樂城不僅提供多元化的游戲選擇,還能讓玩家在家中就能體驗到賭場的樂趣和快感。本文將討論線上娛樂城的特點、優勢以及一些常見的游戲。
什麼是網上娛樂城?
網上娛樂城是一種通過網際網路提供博彩游戲的平台。玩家可以經由計算機、手機或平板電腦進入這些網站,參與各種賭博活動,如德州撲克、賭盤、黑傑克和老虎机等。這些平台通常由專業的的軟件公司開發,確保遊戲的公正性和安全。
線上娛樂城的好處
便利:玩家不用離開家,就能享受賭博的興奮。這對於那些居住在遠離實體賭場地區的人來說特別方便。
多元化的遊戲選擇:網上娛樂城通常提供比實體賭場更多樣化的游戲選擇,並且經常升級遊戲內容,保持新鮮。
優惠和獎勵計劃:許多線上娛樂城提供豐富的優惠計劃,包括註冊紅利、存款獎金和忠誠度計劃,吸引新新玩家並激勵老玩家不斷遊戲。
安全和保密性:正規的在線娛樂城使用先進的的加密方法來保護玩家的個人資料和財務交易,確保遊戲過程的公平和公正。
常有的在線娛樂城遊戲
撲克:撲克是最受歡迎賭錢游戲之一。在線娛樂城提供各種撲克變體,如德州撲克、奧馬哈撲克和七張牌撲克等。
賭盤:賭盤是一種傳統的賭博遊戲,玩家可以賭注在數字、數字組合上或顏色選擇上,然後看小球落在哪個區域。
21點:又稱為二十一點,這是一種比拼玩家和莊家點數的游戲,目標是讓手牌點數盡量接近21點但不超過。
老虎机:老虎机是最簡單且是最常見的賭錢游戲之一,玩家只需轉動捲軸,等待圖案圖案排列出中獎的組合。
結尾
在線娛樂城為現代賭博愛好者提供了一個便捷、刺激的且多元化的娛樂選擇。不管是撲克愛好者還是老虎機迷,大家都能在這些平台上找到適合自己的游戲。同時,隨著技術的不斷進步,網上娛樂城的游戲體驗將變得越來越真實和引人入勝。然而,玩家在享受遊戲的同時,也應該保持自律,避免沉溺於博彩活動,維持健康的娛樂心態。
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Майор Гром 2024
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
娛樂城
在線娛樂城的世界
隨著網際網路的快速發展,線上娛樂城(網上賭場)已經成為許多人消遣的新選擇。網上娛樂城不僅提供多種的遊戲選擇,還能讓玩家在家中就能體驗到賭場的刺激和樂趣。本文將討論在線娛樂城的特色、好處以及一些常有的游戲。
什麼線上娛樂城?
網上娛樂城是一種通過互聯網提供賭博游戲的平台。玩家可以經由電腦、智慧型手機或平板電腦進入這些網站,參與各種賭博活動,如撲克、賭盤、黑傑克和吃角子老虎等。這些平台通常由專業的的軟件公司開發,確保遊戲的公平性和安全。
線上娛樂城的好處
方便性:玩家不用離開家,就能體驗賭錢的快感。這對於那些生活在遠離的實體賭場地區的人來說尤其方便。
多種的遊戲選擇:網上娛樂城通常提供比實體賭場更豐富的遊戲選擇,並且經常更新遊戲內容,保持新鮮。
福利和獎金:許多線上娛樂城提供多樣的獎金計劃,包括註冊獎勵、存款獎金和忠誠度計劃,吸引新新玩家並促使老玩家繼續遊戲。
安全和保密性:正規的網上娛樂城使用先進的加密技術來保護玩家的私人信息和交易,確保游戲過程的穩定和公正性。
常見的的線上娛樂城游戲
德州撲克:撲克是最受歡迎的賭錢遊戲之一。線上娛樂城提供多樣撲克變體,如德州撲克、奧馬哈撲克和七張撲克等。
輪盤:賭盤是一種經典的賭博遊戲,玩家可以賭注在單個數字、數字組合或顏色選擇上,然後看球落在哪個位置。
黑傑克:又稱為黑傑克,這是一種競爭玩家和莊家點數點數的游戲,目標是讓手牌點數儘量接近21點但不超過。
吃角子老虎:老虎機是最簡單且是最流行的賭錢遊戲之一,玩家只需轉動捲軸,看圖案排列出中獎的組合。
結尾
在線娛樂城為現代的賭博愛好者提供了一個便捷、刺激的且豐富的娛樂選擇。不論是撲克迷還是老虎机愛好者,大家都能在這些平台上找到適合自己的游戲。同時,隨著技術的的不斷發展,在線娛樂城的游戲體驗將變化越來越逼真和引人入勝。然而,玩家在享用遊戲的同時,也應該保持自律,避免過度沉迷於賭錢活動,保持健康健康的心態。
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
clear & healthy nails en-nanodefensepro.com
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Dental Health Supplement en-prodentim.com
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Muscle Pain Relief cream en-balmorex.pro
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Daily bonuses
Discover Stimulating Promotions and Free Spins: Your Comprehensive Guide
At our gaming platform, we are dedicated to providing you with the best gaming experience possible. Our range of bonuses and extra spins ensures that every player has the chance to enhance their gameplay and increase their chances of winning. Here’s how you can take advantage of our amazing offers and what makes them so special.
Generous Bonus Spins and Rebate Deals
One of our standout offers is the opportunity to earn up to 200 bonus spins and a 75% rebate with a deposit of just $20 or more. And during happy hour, you can unlock this bonus with a deposit starting from just $10. This fantastic offer allows you to enjoy extended playtime and more opportunities to win without breaking the bank.
Boost Your Balance with Deposit Bonuses
We offer several deposit bonuses designed to maximize your gaming potential. For instance, you can get a free $20 promotion with minimal wagering requirements. This means you can start playing with extra funds, giving you more chances to explore our vast array of games and win big. Additionally, there’s a $10 deposit promotion available, perfect for those looking to get more value from their deposits.
Multiply Your Deposits for Bigger Wins
Our “Play Big!” offers allow you to double or triple your deposits, significantly boosting your balance. Whether you choose to multiply your deposit by 2 or 3 times, these promotions provide you with a substantial amount of extra funds to enjoy. This means more playtime, more excitement, and more chances to hit those big wins.
Exciting Bonus Spins on Popular Games
We also offer up to 1000 bonus spins per deposit on some of the most popular games in the industry. Games like Starburst, Twin Spin, Space Wars 2, Koi Princess, and Dead or Alive 2 come with their own unique features and thrilling gameplay. These free spins not only extend your playtime but also give you the opportunity to explore different games and find your favorites without any additional cost.
Why Choose Our Platform?
Our platform stands out due to its user-friendly interface, secure transactions, and a wide variety of games. We prioritize your gaming experience by ensuring that all our offers are easy to access and beneficial to our players. Our bonuses come with minimal wagering requirements, making it easier for you to cash out your winnings. Moreover, the variety of games we offer ensures that there’s something for every type of player, from classic slot enthusiasts to those who enjoy more modern, feature-packed games.
Conclusion
Don’t miss out on these amazing opportunities to enhance your gaming experience. Whether you’re looking to enjoy bonus spins, refund, or generous deposit promotions, we have something for everyone. Join us today, take advantage of these amazing offers, and start your journey to big wins and endless fun. Happy gaming!
sapporo88
video games guide
Engaging Advancements and Renowned Titles in the World of Gaming
In the fluid realm of videogames, there’s always something groundbreaking and engaging on the cusp. From customizations elevating cherished classics to new arrivals in iconic brands, the interactive entertainment realm is as vibrant as before.
This is a glimpse into the latest announcements and specific the renowned games mesmerizing enthusiasts worldwide.
Most Recent Developments
1. Innovative Customization for Skyrim Elevates Non-Player Character Look
A recent mod for Skyrim has captured the attention of gamers. This customization brings lifelike heads and realistic hair for every non-player entities, enhancing the experience’s graphics and engagement.
2. Total War Games Release Located in Star Wars Galaxy In the Works
Creative Assembly, acclaimed for their Total War lineup, is supposedly crafting a upcoming experience located in the Star Wars Universe universe. This engaging collaboration has enthusiasts anticipating with excitement the analytical and immersive adventure that Total War releases are celebrated for, at last situated in a universe remote.
3. Grand Theft Auto VI Arrival Confirmed for Fall 2025
Take-Two’s CEO’s Chief Executive Officer has confirmed that GTA VI is planned to debut in Late 2025. With the overwhelming success of its predecessor, GTA V, gamers are anticipating to witness what the forthcoming iteration of this celebrated franchise will deliver.
4. Enlargement Plans for Skull & Bones Sophomore Season
Developers of Skull & Bones have communicated broader developments for the world’s next season. This swashbuckling saga promises additional updates and updates, engaging enthusiasts invested and absorbed in the domain of oceanic swashbuckling.
5. Phoenix Labs Developer Undergoes Workforce Reductions
Sadly, not every developments is favorable. Phoenix Labs Developer, the studio behind Dauntless Experience, has disclosed large-scale staff cuts. Despite this challenge, the game keeps to be a iconic preference amidst gamers, and the developer remains dedicated to its community.
Beloved Releases
1. The Witcher 3
With its compelling experience, engrossing world, and captivating experience, The Witcher 3 Game remains a beloved release within fans. Its intricate plot and vast nonlinear world persist to captivate fans in.
2. Cyberpunk Game
Notwithstanding a tumultuous arrival, Cyberpunk remains a long-awaited title. With ongoing enhancements and enhancements, the game persists in progress, delivering gamers a perspective into a high-tech future rife with mystery.
3. Grand Theft Auto V
Still eras post its original release, Grand Theft Auto 5 continues to be a renowned option amidst fans. Its vast sandbox, enthralling story, and multiplayer mode sustain players revisiting for more explorations.
4. Portal Game
A legendary analytical title, Portal 2 is acclaimed for its revolutionary features and brilliant level design. Its intricate challenges and humorous narrative have made it a remarkable experience in the interactive entertainment realm.
5. Far Cry 3 Game
Far Cry 3 is praised as a standout entries in the series, presenting enthusiasts an open-world adventure filled with adventure. Its immersive narrative and memorable personalities have solidified its place as a beloved game.
6. Dishonored
Dishonored Game is celebrated for its stealthy gameplay and distinctive setting. Gamers assume the character of a supernatural eliminator, traversing a metropolis rife with institutional peril.
7. Assassin’s Creed 2
As part of the iconic Assassin’s Creed Franchise collection, Assassin’s Creed II is revered for its engrossing story, enthralling gameplay, and period worlds. It continues to be a noteworthy experience in the series and a beloved amidst fans.
In final remarks, the realm of gaming is thriving and fluid, with new advan
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Cricket Affiliate: খেলা এবং উপভোগের অনুভূতি
ক্রিকেট ক্যাসিনোতে আপনাকে স্বাগতম! BouncingBall8 এ আপনি একটি অসাধারণ গেমিং অভিজ্ঞতা অংশগ্রহণ করতে পারেন। আমরা আমাদের সদস্যদের জন্য অনেক বিশেষ প্রচার অফার করি যাতে তারা খেলার সুবিধা এবং বোনাস উপভোগ করতে পারে।
আপনি এখানে আছেন তাই আমরা খুবই আনন্দিত! এখানে আমরা আপনাদের জন্য বিভিন্ন বোনাস অফার করছি, যা আপনি প্রথম আমানতের 200% পাবেন, দৈনিক 100% বোনাস পাবেন, এবং লাকি ড্র 10,000 পর্যন্ত বোনাস পাবেন।
আমাদের সাথে যোগ দিন এবং ক্রিকেট ক্যাসিনোতে পুরষ্কার কাটা শুরু করুন – BouncingBall8! আপনি ক্রিকেট affiliate হিসেবে যোগ দিতে পারেন এবং আমাদের অফারগুলি উপভোগ করতে পারেন।
সাথে যোগ দিন এবং একটি অসাধারণ গেমিং অভিজ্ঞতা উপভোগ করুন!
বোনাস এবং প্রচার
আমাদের ক্রিকেট ক্যাসিনোতে আপনি বিশেষ বোনাস এবং প্রচার উপভোগ করতে পারেন। আমরা নিয়মিতভাবে আপনাদের জন্য নতুন অফার এবং সুযোগ প্রদান করি যাতে আপনি আরও বেশি উপভোগ করতে পারেন।
ক্রিকেট ক্যাসিনোতে আমাদের সাথে যোগ দিন এবং আপনার গেমিং অভিজ্ঞতা উন্নত করুন এবং সবচেয়ে জনপ্রিয় খেলা এবং বোনাস পেতে শুরু করুন!
Welcome to Cricket Affiliate | Kick off with a smashing Welcome Bonus !
First Deposit Fiesta! | Make your debut at Cricket Exchange with a 200% bonus.
Daily Doubles! | Keep the scoreboard ticking with a 100% daily bonus at 9wicket!
#cricketaffiliate
IPL 2024 Jackpot! | Stand to win ₹50,000 in the mega IPL draw at cricket world!
Social Sharer Rewards! | Post and earn 100 tk weekly through Crickex affiliate login.
https://www.cricket-affiliate.com/
#cricketexchange #9wicket #crickexaffiliatelogin #crickexlogin
crickex login VIP! | Step up as a VIP and enjoy weekly bonuses!
Join the Action! | Log in through crickex bet exciting betting experience at Live Affiliate.
Dive into the game with crickex live—where every play brings spectacular wins !
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Jili Ace ক্যাসিনো: বাংলাদেশের সেরা গেমিং ওয়েবসাইট
Jili Ace ক্যাসিনো বাংলাদেশের অন্যতম শীর্ষ-রেটেড গেমিং ওয়েবসাইট হিসেবে নিজেকে প্রতিষ্ঠিত করেছে। এটি বিনামূল্যে অনলাইন ক্যাসিনো গেমের মাধ্যমে রিয়েল মানি জেতার সুযোগ প্রদান করে, যা ডিপোজিটের প্রয়োজন নেই। এই প্ল্যাটফর্মটি 1000+ গেমের বিশাল সংগ্রহের মাধ্যমে ব্যবহারকারীদের বিভিন্ন ধরনের গেমিং অভিজ্ঞতা প্রদান করে।
Jiliace Casino-তে আপনি স্লট, ফিশিং, সাবং, ব্যাকার্যাট, বিঙ্গো এবং লটারি গেমের মতো বিভিন্ন ধরণের গেম খেলতে পারবেন। প্রতিটি গেমই অত্যন্ত আকর্ষণীয় এবং ব্যবহারকারীদের জন্য দারুণ বিনোদনের উৎস।
শীর্ষ গেম প্রোভাইডার
Jili Ace ক্যাসিনোতে আপনি JDB, JILI, PG, CQ9-এর মতো শীর্ষ গেম প্রোভাইডারদের গেম উপভোগ করতে পারবেন। এই প্রোভাইডারদের গেমগুলি তাদের অসাধারণ গ্রাফিক্স, উত্তেজনাপূর্ণ গেমপ্লে এবং বড় পুরস্কারের জন্য পরিচিত।
সহজ লগইন প্রক্রিয়া
Jiliace Login প্রক্রিয়া অত্যন্ত সহজ এবং দ্রুত। আপনার অ্যাকাউন্ট তৈরি এবং লগইন করার পর আপনি সহজেই বিভিন্ন গেমে অংশ নিতে পারবেন এবং আপনার জয়কে বাড়িয়ে তুলতে পারবেন। Jili Ace Login-এর মাধ্যমে আপনি যে কোনও সময় এবং যে কোনও স্থান থেকে গেমে অংশ নিতে পারেন, যা আপনার গেমিং অভিজ্ঞতাকে আরও সুবিধাজনক করে তোলে।
বিভিন্ন ধরণের গেম
Jiliace Casino-তে স্লট গেম, ফিশিং গেম, সাবং গেম, ব্যাকার্যাট, বিঙ্গো এবং লটারি গেমের মত বিভিন্ন ধরণের গেম পাওয়া যায়। এই বৈচিত্র্যময় গেমের সংগ্রহ ব্যবহারকারীদের একঘেয়েমি থেকে মুক্তি দেয় এবং নতুন অভিজ্ঞতার স্বাদ প্রদান করে।
Jita Bet-এর সাথে অংশ নিন
Jili Ace ক্যাসিনোতে Jita Bet এর সাথে অংশ নিয়ে আপনার গেমিং অভিজ্ঞতা আরও সমৃদ্ধ করুন। এখানে আপনি বিভিন্ন ধরণের বাজি ধরতে পারেন এবং বড় পুরস্কার জিততে পারেন। Jita Bet প্ল্যাটফর্মটি ব্যবহারকারীদের জন্য সহজ এবং সুরক্ষিত বাজি ধরার সুযোগ প্রদান করে।
Jili Ace ক্যাসিনো বাংলাদেশের সেরা গেমিং ওয়েবসাইট হিসেবে পরিচিত, যেখানে ব্যবহারকারীরা বিনামূল্যে গেম খেলে রিয়েল মানি জিততে পারেন। আজই Jiliace Login করুন এবং আপনার গেমিং যাত্রা শুরু করুন!
Jiliacet casino
Jiliacet casino |
Warm welcome! | Get a 200% Welcome Bonus when you log in jiliace casino.
IPL Tournament! | Join the IPL fever with Jita Bet. Win big prizes!
Epic JILI Tournaments! | Go head-to-head in the Jita bet Super Tournament
#jiliacecasino
Cashback on Deposits! | Get cash back on every deposit. At Jili ace casino
Uninterrupted bonuses at JITAACE! | Stay logged in Jiliace login!
https://www.jiliace-casino.online/bn
#Jiliacecasino # Jiliacelogin#Jiliacelogin # Jitabet
Slot Feast! | Spin to win 100% up to 20,000 ৳. at Jili ace login!
Big Fishing Bonus! | Get a 100% bonus up to ৳20,000 in the Fishing Game.
JiliAce Casino’s top choice for great bonuses. login, play, and win big today!
Выбор современных мужчин – тактичные штаны, подчеркнут ваш стиль.
Незаменимые для занятий спортом, тактичные штаны подарят вам удобство и защиту.
Надежный пошив и долговечность, сделают тактичные штаны вашим незаменимым спутником.
Максимальный комфорт и стильный вид, делают тактичные штаны незаменимым вещью в гардеробе каждого мужчины.
Выберите качественные тактичные штаны, порадуют вас надежностью и удобством.
купити штани мультикам з наколінниками купити штани мультикам з наколінниками .
Daily bonuses
Find Stimulating Promotions and Free Rounds: Your Comprehensive Guide
At our gaming platform, we are focused to providing you with the best gaming experience possible. Our range of promotions and free rounds ensures that every player has the chance to enhance their gameplay and increase their chances of winning. Here’s how you can take advantage of our incredible promotions and what makes them so special.
Bountiful Extra Spins and Refund Bonuses
One of our standout promotions is the opportunity to earn up to 200 free spins and a 75% refund with a deposit of just $20 or more. And during happy hour, you can unlock this bonus with a deposit starting from just $10. This fantastic offer allows you to enjoy extended playtime and more opportunities to win without breaking the bank.
Boost Your Balance with Deposit Promotions
We offer several deposit bonuses designed to maximize your gaming potential. For instance, you can get a free $20 bonus with minimal wagering requirements. This means you can start playing with extra funds, giving you more chances to explore our vast array of games and win big. Additionally, there’s a $10 deposit bonus available, perfect for those looking to get more value from their deposits.
Multiply Your Deposits for Bigger Wins
Our “Play Big!” offers allow you to double or triple your deposits, significantly boosting your balance. Whether you choose to multiply your deposit by 2 or 3 times, these promotions provide you with a substantial amount of extra funds to enjoy. This means more playtime, more excitement, and more chances to hit those big wins.
Exciting Bonus Spins on Popular Games
We also offer up to 1000 free spins per deposit on some of the most popular games in the industry. Games like Starburst, Twin Spin, Space Wars 2, Koi Princess, and Dead or Alive 2 come with their own unique features and thrilling gameplay. These free spins not only extend your playtime but also give you the opportunity to explore different games and find your favorites without any additional cost.
Why Choose Our Platform?
Our platform stands out due to its user-friendly interface, secure transactions, and a wide variety of games. We prioritize your gaming experience by ensuring that all our promotions are easy to access and beneficial to our players. Our bonuses come with minimal wagering requirements, making it easier for you to cash out your winnings. Moreover, the variety of games we offer ensures that there’s something for every type of player, from classic slot enthusiasts to those who enjoy more modern, feature-packed games.
Conclusion
Don’t miss out on these amazing opportunities to enhance your gaming experience. Whether you’re looking to enjoy bonus spins, cashback, or plentiful deposit promotions, we have something for everyone. Join us today, take advantage of these incredible promotions, and start your journey to big wins and endless fun. Happy gaming!
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Uncover Invigorating Promotions and Bonus Spins: Your Ultimate Guide
At our gaming platform, we are dedicated to providing you with the best gaming experience possible. Our range of offers and bonus spins ensures that every player has the chance to enhance their gameplay and increase their chances of winning. Here’s how you can take advantage of our amazing deals and what makes them so special.
Generous Free Spins and Cashback Deals
One of our standout promotions is the opportunity to earn up to 200 free spins and a 75% refund with a deposit of just $20 or more. And during happy hour, you can unlock this bonus with a deposit starting from just $10. This incredible promotion allows you to enjoy extended playtime and more opportunities to win without breaking the bank.
Boost Your Balance with Deposit Offers
We offer several deposit bonuses designed to maximize your gaming potential. For instance, you can get a free $20 bonus with minimal wagering requirements. This means you can start playing with extra funds, giving you more chances to explore our vast array of games and win big. Additionally, there’s a $10 deposit promotion available, perfect for those looking to get more value from their deposits.
Multiply Your Deposits for Bigger Wins
Our “Play Big!” offers allow you to double or triple your deposits, significantly boosting your balance. Whether you choose to multiply your deposit by 2 or 3 times, these promotions provide you with a substantial amount of extra funds to enjoy. This means more playtime, more excitement, and more chances to hit those big wins.
Exciting Free Spins on Popular Games
We also offer up to 1000 free spins per deposit on some of the most popular games in the industry. Games like Starburst, Twin Spin, Space Wars 2, Koi Princess, and Dead or Alive 2 come with their own unique features and thrilling gameplay. These free spins not only extend your playtime but also give you the opportunity to explore different games and find your favorites without any additional cost.
Why Choose Our Platform?
Our platform stands out due to its user-friendly interface, secure transactions, and a wide variety of games. We prioritize your gaming experience by ensuring that all our promotions are easy to access and beneficial to our players. Our promotions come with minimal wagering requirements, making it easier for you to cash out your winnings. Moreover, the variety of games we offer ensures that there’s something for every type of player, from classic slot enthusiasts to those who enjoy more modern, feature-packed games.
Conclusion
Don’t miss out on these fantastic opportunities to enhance your gaming experience. Whether you’re looking to enjoy free spins, refund, or generous deposit bonuses, we have something for everyone. Join us today, take advantage of these incredible promotions, and start your journey to big wins and endless fun. Happy gaming!
Betvisa Casino: Unlocking Unparalleled Bonuses for Philippine Gamblers
The world of online gambling has witnessed a remarkable surge in popularity, and Betvisa Casino has emerged as a premier destination for players in the Philippines. With its user-friendly platform and a diverse selection of games, Betvisa Casino has become the go-to choice for both seasoned gamblers and newcomers alike.
One of the standout features of Betvisa Casino is its generous bonus offerings, which can significantly enhance the overall gaming experience for players in the Philippines. These bonuses not only provide additional value but also increase the chances of winning big.
For first-time players, Betvisa Casino offers a tempting welcome bonus that can give a substantial boost to their initial bankroll. This bonus allows players to explore the platform’s vast array of games, from thrilling slot titles to immersive live casino experiences, with the added security of a financial cushion.
Existing players, on the other hand, can take advantage of a range of ongoing promotions and bonuses that cater to their specific gaming preferences. These may include reload bonuses, free spins, and even exclusive VIP programs that offer personalized rewards and privileges.
One of the key advantages of Betvisa Casino’s bonus offerings is their versatility. Players can utilize these bonuses across a variety of games, from the Visa Bet sports betting platform to the captivating Betvisa Casino. This flexibility allows players to diversify their gaming portfolios and experience the full breadth of what Betvisa has to offer.
Moreover, Betvisa Casino’s bonus terms and conditions are transparent and player-friendly, ensuring a seamless and enjoyable gaming experience. Whether you’re looking to maximize your winnings or simply enhance your overall enjoyment, these bonuses can provide the extra edge you need.
As the online gambling landscape in the Philippines continues to evolve, Betvisa Casino remains at the forefront, offering an unparalleled combination of games, user-friendliness, and unbeatable bonuses. So, why not take a step into the world of Betvisa Casino and unlock a world of exciting possibilities?
Betvisa Bet | Step into the Arena with Betvisa!
Spin to Win Daily at Betvisa PH! | Take a whirl and bag ₱8,888 in big rewards.
Valentine’s 143% Love Boost at Visa Bet! | Celebrate romance and rewards !
Deposit Bonus Magic! | Deposit 50 and get an 88 bonus instantly at Betvisa Casino.
#betvisa
Free Cash & More Spins! | Sign up betvisa login,grab 500 free cash plus 5 free spins.
Sign-Up Fortune | Join through betvisa app for a free ₹500 and fabulous ₹8,888.
https://www.betvisa-bet.com/tl
#visabet #betvisalogin #betvisacasino # betvisaph
Double Your Play at betvisa com! | Deposit 1,000 and get a whopping 2,000 free
100% Cock Fight Welcome at Visa Bet! | Plunge into the exciting world .Bet and win!
Jump into Betvisa for exciting games, stunning bonuses, and endless winnings!
भारत में ऑनलाइन क्रिकेट सट्टेबाजी की बढ़ती लोकप्रियता
भारत में क्रिकेट को एक धर्म के रूप में देखा जाता है। क्रिकेट के प्रति भारतीयों की अटूट प्रेम और उत्साह को देखते हुए, ऑनलाइन क्रिकेट सट्टेबाजी ने पिछले कुछ वर्षों में जबरदस्त लोकप्रियता हासिल की है।
इस लोकप्रियता के पीछे कुछ प्रमुख कारण हैं। सबसे पहले, बेटवीसा जैसे विश्वसनीय ऑनलाइन कैसीनो और खेल प्लेटफॉर्मों के आगमन ने ऑनलाइन क्रिकेट सट्टेबाजी को एक नया आयाम प्रदान किया है। बेटवीसा भारत में एक प्रमुख खिलाड़ी है, जो अपने कुराकाओ गेमिंग लाइसेंस और 2 मिलियन से अधिक उपयोगकर्ताओं के साथ एक विश्वसनीय और सुरक्षित प्लेटफॉर्म प्रदान करता है।
दूसरा, बेटवीसा ऐप और बेटवीसा लॉगिन प्रक्रिया की सरलता ने उपयोगकर्ताओं को अपने मोबाइल डिवाइसों से क्रिकेट सट्टेबाजी करने में सक्षम बनाया है। इससे उन्हें कहीं से भी खेलने की सुविधा मिलती है।
साथ ही, बेटवीसा जैसे प्लेटफॉर्मों ने विविध भुगतान विकल्प और सुरक्षित लेनदेन की पेशकश की है, जिससे उपयोगकर्ताओं को एक विश्वसनीय और आरामदायक अनुभव प्राप्त होता है।
समग्र रूप से, भारत में ऑनलाइन क्रिकेट सट्टेबाजी की बढ़ती लोकप्रियता में बेटवीसा जैसे प्रमुख ऑनलाइन कैसीनो और खेल प्लेटफॉर्मों की महत्वपूर्ण भूमिका है। इनके आसान, सुरक्षित और विश्वसनीय प्लेटफॉर्म ने क्रिकेट प्रेमियों को एक नया और उत्साहजनक गेमिंग अनुभव प्रदान किया है।
Betvisa Bet
Betvisa Bet | Catch the BPL Excitement with Betvisa!
Hunt for ₹10million! | Enter the BPL at Betvisa and chase a staggering Bounty.
Valentine’s Boost at Visa Bet! | Feel the rush of a 143% Love Mania Bonus .
predict BPL T20 outcomes | score big rewards through Betvisa login!
#betvisa
Betvisa bonus Win! | Leverage your 10 free spins to possibly win $8,888.
Share and Earn! | win ₹500 via the Betvisa app download!
https://www.betvisa-bet.com/hi
#visabet #betvisalogin #betvisaapp #betvisaIndia
Sign-Up Jackpot! | Register at Betvisa India and win ₹8,888.
Double your play! | with a ₹1,000 deposit and get ₹2,000 free at Betvisa online!
Download the Betvisa download today and don’t miss out on the action!
BetVisa: মোবাইল গেমিংয়ের নতুন রূপ
ডিজিটাল যুগে, খেলোয়াড়রা আর ডেস্কটপ গেমিংয়ের সীমিততা সহ্য করতে চান না। তাদের চাহিদা হল, যেকোন সময় যেকোন জায়গায় তাদের প্রিয় স্লট গেমগুলি খেলতে পারা। এই চাহিদা লক্ষ্য করে, BetVisa মোবাইল গেমিংয়ের নতুন মাত্রা উন্মোচন করেছে।
বেটভিসা ডাউনলোড: খেলোয়াড়রা বাড়িতে বসে থাক বা চলার পথে থাকুক না কেন, তাদের স্মার্টফোন বা ট্যাবলেট বের করে BetVisa অ্যাপ চালু করতে পারে এবং সেকেন্ডের মধ্যে স্লটের জগতে ডুব দিতে পারে। এই সুবিধার মাধ্যমে, খেলোয়াড়রা ডেস্কটপ গেমিংয়ের সীমাবদ্ধতা থেকে বিদায় নিতে পারেন।
রিচ গেমিং বৈচিত্র্য: Betvisa তাদের সৃজনশীলতা এবং উদ্ভাবনের জন্য বিখ্যাত গেম ডেভেলপারদের কাছ থেকে শিরোনাম সমন্বিত স্লট গেমগুলির একটি বিস্তৃত লাইব্রেরি নিয়ে গর্বিত। ক্লাসিক ফ্রুট মেশিন থেকে শুরু করে অত্যাধুনিক গ্রাফিক্স এবং অ্যানিমেশন গর্বিত নিমজ্জিত ভিডিও স্লট পর্যন্ত, প্রত্যেক খেলোয়াড়ের পছন্দ ও স্বাদ মেটাতে কিছু না কিছু রয়েছে।
সুচারু গেমপ্লে: বেটিভিসা ডাউনলোড মোবাইল ডিভাইসের জন্য তৈরি অপ্টিমাইজড পারফরম্যান্স এবং স্বজ্ঞাত নিয়ন্ত্রণ সহ একটি নিরবচ্ছিন্ন গেমিং অভিজ্ঞতা নিশ্চিত করে৷ প্লেয়াররা অ্যাপের মাধ্যমে অনায়াসে নেভিগেট করতে পারে, বিভিন্ন গেম অন্বেষণ করতে পারে, এবং কোনো প্রকার ল্যাগ বা গ্লিচ ছাড়াই নিরবচ্ছিন্ন গেমপ্লে উপভোগ করতে পারে।
বিশেষ প্রচার সুযোগ: BetVisa প্রায়শই Betvisa ডাউনলোড অ্যাপের মাধ্যমে প্ল্যাটফর্মে প্রবেশকারী খেলোয়াড়দের জন্য একচেটিয়া প্রচার এবং বোনাস রোল আউট করে। স্বাগত বোনাস থেকে শুরু করে ফ্রি স্পিন এবং লয়্যালটি পুরষ্কার পর্যন্ত, একজনের ব্যাঙ্করোল বাড়ানো এবং গেমিং অভিজ্ঞতা বাড়ানোর প্রচুর সুযোগ রয়েছে।
BetVisa বাংলাদেশ ব্যবহারকারীদের জন্য বিশেষ সুবিধা প্রদান করে। BetVisa বাংলাদেশ লগইন করে খেলোয়াড়রা সহজে তাদের প্রিয় স্লট গেমগুলি খেলতে পারেন।
মোবাইল ডিভাইসের উন্নত অ্যাক্সেসের সুযোগ, রিচ গেমিং বৈচিত্র্য এবং বিশেষ প্রচার সুবিধার মাধ্যমে, BetVisa মোবাইল গেমিংয়ের নতুন বিস্ময় সৃষ্টি করেছে।
Betvisa Bet | Hit it Big This IPL Season with Betvisa!
Betvisa login! | Every deposit during IPL matches earns a 2% bonus .
Betvisa Bangladesh! | IPL 2024 action heats up, your bets get more rewarding!
Crash Game returns! | huge ₹10 million jackpot. Take the lead on the Betvisa app !
#betvisa
Start Winning Now! | Sign up through Betvisa affiliate login, claim ₹500 free cash.
Grab Your Winning Ticket! | Register login and win ₹8,888 at visa bet!
https://www.betvisa-bet.com/bn
#visabet #betvisalogin #betvisabangladesh#betvisaapp
200% Excitement! | Enjoy slots and fishing games at Betvisa লগইন করুন!
Big Sports Bonuses! | Score up to ₹5,000 in sports bonuses during the IPL season
Gear up for an exhilarating IPL season at Betvisa, propels you towards victory!
Претенденты смотреть Претенденты фильм, 2024, смотреть онлайн
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Son zamanlarda oynadigim bir oyundan bahsetmek istiyorum sweet-bonanza-giris.com. Bu oyunu gercekten bayildim. Grafikler harika, hikaye heyecan verici ve oynanis kolay anlasilir. Oyunda figurlerin gelisimi cok iyi dusunulmus ve modifiye etme secenekleri cok cesitli. Gelistiriciler gercekten cok caba gostermis, bu da oyunu daha eglenceli hale getiriyor. Ayrica, coklu oyuncu modu da oldukca eglenceli ve arkadaslarinizla uzun saatler oynayabileceginiz bir tecrube sunuyor. Bu oyunu kesinlikle oneririm. Eger ozgun bir oyun deneyimi ariyorsaniz, bu oyun tam size gore!
iyi oyunlar dilerim!
Претенденты смотреть Претенденты фильм, 2024, смотреть онлайн
더 도그 하우스 메가웨이즈
Fang Jifan이 인정하든 아니든 앞으로 그는 자신을 위해 향을 계속할 것입니다.
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
video games guide
Captivating Breakthroughs and Popular Releases in the World of Gaming
In the constantly-changing domain of interactive entertainment, there’s perpetually something fresh and captivating on the cusp. From enhancements elevating revered mainstays to upcoming debuts in legendary brands, the gaming ecosystem is flourishing as ever.
Let’s take a look into the up-to-date announcements and certain the renowned titles mesmerizing enthusiasts globally.
Up-to-Date News
1. Groundbreaking Enhancement for The Elder Scrolls V: Skyrim Optimizes Non-Player Character Appearance
A latest modification for The Elder Scrolls V: Skyrim has captured the attention of fans. This enhancement adds detailed heads and realistic hair for each non-player characters, optimizing the experience’s aesthetics and immersion.
2. Total War Release Set in Star Wars Galaxy Being Developed
The Creative Assembly, acclaimed for their Total War franchise, is said to be crafting a upcoming game placed in the Star Wars Setting realm. This thrilling collaboration has enthusiasts anticipating with excitement the profound and captivating journey that Total War Series experiences are acclaimed for, finally situated in a galaxy far, far away.
3. Grand Theft Auto VI Launch Revealed for Late 2025
Take-Two’s CEO’s Chief Executive Officer has confirmed that GTA VI is planned to debut in Fall 2025. With the overwhelming popularity of its prior release, GTA V, enthusiasts are excited to explore what the future installment of this legendary franchise will offer.
4. Enlargement Developments for Skull & Bones 2nd Season
Studios of Skull and Bones have communicated broader initiatives for the experience’s Season Two. This swashbuckling experience offers additional experiences and updates, keeping players captivated and engrossed in the realm of high-seas swashbuckling.
5. Phoenix Labs Studio Deals with Workforce Reductions
Regrettably, not all news is favorable. Phoenix Labs, the studio responsible for Dauntless Game, has disclosed large-scale personnel cuts. Despite this setback, the experience remains to be a beloved choice across enthusiasts, and the developer continues to be attentive to its fanbase.
Beloved Releases
1. The Witcher 3: Wild Hunt Game
With its engaging story, captivating world, and compelling journey, The Witcher 3 keeps a cherished experience across fans. Its rich experience and vast open world remain to captivate enthusiasts in.
2. Cyberpunk Game
Notwithstanding a challenging release, Cyberpunk stays a long-awaited experience. With continuous enhancements and optimizations, the title maintains advance, presenting fans a perspective into a dystopian world abundant with intrigue.
3. Grand Theft Auto V
Still time after its debut debut, Grand Theft Auto V stays a popular choice amidst players. Its wide-ranging open world, enthralling plot, and multiplayer mode sustain fans revisiting for further adventures.
4. Portal Game
A legendary problem-solving title, Portal 2 Game is praised for its pioneering features and brilliant environmental design. Its demanding conundrums and witty writing have established it as a remarkable game in the gaming world.
5. Far Cry
Far Cry 3 is celebrated as among the finest entries in the universe, providing fans an open-world journey abundant with adventure. Its engrossing story and renowned personalities have solidified its position as a iconic release.
6. Dishonored Series
Dishonored Game is acclaimed for its sneaky systems and distinctive environment. Enthusiasts embrace the identity of a mystical eliminator, exploring a metropolis rife with institutional danger.
7. Assassin’s Creed 2
As a member of the renowned Assassin’s Creed Franchise series, Assassin’s Creed II is revered for its captivating story, compelling systems, and era-based settings. It stays a exceptional experience in the franchise and a favorite among fans.
In final remarks, the world of digital entertainment is flourishing and constantly evolving, with innovative advan
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
geinoutime.com
그는 마음속으로 불안하면서도 감탄스럽게 지저귀고 흥얼거렸다.
ক্রিকেট অ্যাফিলিয়েট প্রোগ্রাম – একটি উত্তেজনাপূর্ণ অফার
ক্রিকেট অ্যাফিলিয়েট প্রোগ্রাম সম্পর্কে আপনি কখনও শুনেছেন? আপনি ক্রিকেট উপকরণ, খেলাধুলা বা সংগ্রহগুলির জন্য পছন্দ করেন? তাহলে আপনার জন্য সেরা অফার আসছে!
ক্রিকেট অ্যাফিলিয়েট হওয়ার জন্য আমরা আপনার জন্য একটি সুযোগ প্রদান করছি। আমাদের প্রোগ্রামে যোগ দিন এবং আমাদের অনুসরণ করুন। আমাদের প্রোগ্রামে যোগ দিন এবং ক্রিকেট অ্যাফিলিয়েট তথ্য পেতে এবং আমাদের একচেটিয়া ক্রিকেট ক্যাসিনো – ক্রিকএক্স অ্যাফিলিয়েট লগইন বিশেষ প্রচারগুলি গ্রহণ করার জন্য আন্তরিকভাবে স্বাগতম!
ক্রিকেট অ্যাফিলিয়েট হিসেবে আপনি আমাদের প্ল্যাটফর্মে আপনার সুযোগ এবং আয় বৃদ্ধি করতে পারেন। আমাদের সাথে যোগ দিন এবং ক্রিকেট প্রেমিকদের জন্য এই অসাধারণ সুযোগ গ্রহণ করুন!
অনুসরণ করো এবং স্বাগতম
আমাদের অনুসরণ করুন এবং ক্রিকেট অ্যাফিলিয়েট তথ্য পেতে এবং আমাদের একচেটিয়া ক্রিকেট ক্যাসিনো – ক্রিকএক্স অ্যাফিলিয়েট লগইন বিশেষ প্রচারগুলি গ্রহণ করার জন্য আন্তরিকভাবে স্বাগতম! আমাদের প্রোগ্রামে যোগ দিন এবং ক্রিকেট প্রেমিকদের জন্য এই অসাধারণ সুযোগ গ্রহণ করুন!
Welcome to Cricket Affiliate | Kick off with a smashing Welcome Bonus !
First Deposit Fiesta! | Make your debut at Cricket Exchange with a 200% bonus.
Daily Doubles! | Keep the scoreboard ticking with a 100% daily bonus at 9wicket!
#cricketaffiliate
IPL 2024 Jackpot! | Stand to win ₹50,000 in the mega IPL draw at cricket world!
Social Sharer Rewards! | Post and earn 100 tk weekly through Crickex affiliate login.
https://www.cricket-affiliate.com/
#cricketexchange #9wicket #crickexaffiliatelogin #crickexlogin
crickex login VIP! | Step up as a VIP and enjoy weekly bonuses!
Join the Action! | Log in through crickex bet exciting betting experience at Live Affiliate.
Dive into the game with crickex live—where every play brings spectacular wins !
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Exciting Developments and Popular Titles in the Realm of Digital Entertainment
In the constantly-changing realm of digital entertainment, there’s continuously something new and engaging on the horizon. From enhancements enhancing revered classics to new debuts in celebrated series, the interactive entertainment landscape is flourishing as in recent memory.
This is a look into the most recent developments and a few of the iconic experiences captivating fans worldwide.
Most Recent Announcements
1. Groundbreaking Enhancement for Skyrim Enhances NPC Visuals
A freshly-launched modification for The Elder Scrolls V: Skyrim has caught the focus of fans. This mod introduces detailed faces and realistic hair for every non-player characters, enhancing the game’s visuals and immersion.
2. Total War Release Located in Star Wars Galaxy In the Works
Creative Assembly, famous for their Total War Series collection, is supposedly crafting a upcoming title located in the Star Wars Setting realm. This captivating crossover has gamers looking forward to the tactical and engaging journey that Total War Games experiences are renowned for, ultimately placed in a realm expansive.
3. GTA VI Launch Announced for Late 2025
Take-Two’s CEO’s Leader has revealed that GTA VI is planned to debut in Fall 2025. With the massive acclaim of its predecessor, GTA V, fans are eager to experience what the next installment of this legendary franchise will bring.
4. Expansion Developments for Skull & Bones Season Two
Studios of Skull and Bones have revealed amplified plans for the experience’s next season. This nautical adventure delivers fresh content and enhancements, sustaining players invested and absorbed in the universe of maritime nautical adventures.
5. Phoenix Labs Studio Deals with Personnel Cuts
Regrettably, not everything developments is favorable. Phoenix Labs Studio, the studio behind Dauntless Game, has communicated large-scale staff cuts. In spite of this setback, the experience remains to be a renowned preference among fans, and the developer stays attentive to its playerbase.
Beloved Experiences
1. The Witcher 3: Wild Hunt Game
With its engaging story, absorbing realm, and captivating journey, The Witcher 3 Game continues to be a cherished experience across gamers. Its rich story and expansive free-roaming environment persist to captivate fans in.
2. Cyberpunk 2077 Game
Despite a challenging release, Cyberpunk continues to be a long-awaited release. With continuous patches and adjustments, the game persists in progress, delivering gamers a look into a high-tech world abundant with danger.
3. Grand Theft Auto 5
Even years subsequent to its original release, GTA V remains a renowned option amidst fans. Its sprawling open world, enthralling plot, and co-op experiences continue to draw gamers returning for additional explorations.
4. Portal Game
A renowned puzzle experience, Portal 2 is acclaimed for its pioneering features and exceptional level design. Its intricate conundrums and humorous storytelling have solidified it as a remarkable title in the interactive entertainment industry.
5. Far Cry Game
Far Cry is hailed as among the finest titles in the series, presenting enthusiasts an open-world journey teeming with intrigue. Its compelling story and renowned characters have established its place as a iconic title.
6. Dishonored Game
Dishonored is praised for its stealth systems and distinctive realm. Enthusiasts embrace the character of a otherworldly executioner, experiencing a metropolitan area rife with governmental intrigue.
7. Assassin’s Creed Game
As a member of the renowned Assassin’s Creed Universe franchise, Assassin’s Creed Game is adored for its captivating experience, captivating features, and time-period realms. It remains a standout game in the universe and a iconic across gamers.
In conclusion, the domain of videogames is prospering and ever-changing, with fresh developments
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
My spouse and I absolutely love your blog and find nearly all of your post’s to be just what I’m looking for. Do you offer guest writers to write content available for you? I wouldn’t mind composing a post or elaborating on most of the subjects you write about here. Again, awesome weblog!
Del Mar Energy
Euro
sunmory33
sunmory33
Optimizing Your Betting Experience: A Comprehensive Guide to Betvisa
In the dynamic world of online betting, navigating the landscape can be both exhilarating and challenging. To ensure a successful and rewarding journey, it’s crucial to focus on key factors that can enhance your experience on platforms like Betvisa. Let’s delve into a comprehensive guide that will empower you to make the most of your Betvisa betting adventure.
Choosing a Reputable Platform
The foundation of a thrilling betting experience lies in selecting a reputable platform. Betvisa has firmly established itself as a trusted and user-friendly destination, renowned for its diverse game offerings, secure transactions, and commitment to fair play. When exploring the Betvisa ecosystem, be sure to check for licenses and certifications from recognized gaming authorities, as well as positive reviews from other users.
Understanding the Games and Bets
Familiarizing yourself with the games and betting options available on Betvisa is a crucial step. Whether your preference leans towards sports betting, casino games, or the thrill of live dealer experiences, comprehending the rules and strategies can significantly enhance your chances of success. Take advantage of free trials or demo versions to practice and hone your skills before placing real-money bets.
Mastering Bankroll Management
Responsible bankroll management is the key to a sustainable and enjoyable betting journey. Betvisa encourages players to set a weekly or monthly budget and stick to it, avoiding the pitfalls of excessive gambling. Implement strategies such as the fixed staking plan or the percentage staking plan to ensure your bets align with your financial capabilities.
Leveraging Bonuses and Promotions
Betvisa often offers a variety of bonuses and promotions to attract and retain players. From no-deposit bonuses to free spins, these incentives can provide you with extra funds to play with, ultimately increasing your chances of winning. Carefully read the terms and conditions to ensure you make the most of these opportunities.
Staying Informed and Updated
The online betting landscape is constantly evolving, with odds and game conditions changing rapidly. By staying informed about the latest trends, tips, and strategies, you can gain a competitive edge. Follow sports news, join online communities, and subscribe to Betvisa’s newsletters to stay at the forefront of the industry.
Accessing Reliable Customer Support
Betvisa’s commitment to player satisfaction is evident in its robust customer support system. Whether you have questions about deposits, withdrawals, or game rules, the platform’s helpful and responsive support team is readily available to assist you. Utilize the live chat feature, comprehensive FAQ section, or direct contact options for a seamless and stress-free betting experience.
Embracing Responsible Gaming
Responsible gaming is not just a buzzword; it’s a fundamental aspect of a fulfilling betting journey. Betvisa encourages players to set time limits, take regular breaks, and seek help if they feel their gambling is becoming uncontrollable. By prioritizing responsible practices, you can ensure that your Betvisa experience remains an enjoyable and sustainable pursuit.
By incorporating these key factors into your Betvisa betting strategy, you’ll unlock a world of opportunities and elevate your overall experience. Remember, the journey is as important as the destination, and with Betvisa as your trusted partner, the path to success is paved with thrilling discoveries and rewarding payouts.
Betvisa Bet | Step into the Arena with Betvisa!
Spin to Win Daily at Betvisa PH! | Take a whirl and bag ?8,888 in big rewards.
Valentine’s 143% Love Boost at Visa Bet! | Celebrate romance and rewards !
Deposit Bonus Magic! | Deposit 50 and get an 88 bonus instantly at Betvisa Casino.
#betvisa
Free Cash & More Spins! | Sign up betvisa login,grab 500 free cash plus 5 free spins.
Sign-Up Fortune | Join through betvisa app for a free ?500 and fabulous ?8,888.
https://www.betvisa-bet.com/tl
#visabet #betvisalogin #betvisacasino # betvisaph
Double Your Play at betvisa com! | Deposit 1,000 and get a whopping 2,000 free
100% Cock Fight Welcome at Visa Bet! | Plunge into the exciting world .Bet and win!
Jump into Betvisa for exciting games, stunning bonuses, and endless winnings!
라이즈 오브 올림푸스
작성을 마친 후에는 추가 조사가 없습니다.
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
angkot88
ANGKOT88: Situs Game Deposit Pulsa Terbaik di Indonesia
ANGKOT88 adalah situs game deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai jenis game online terlengkap yang dapat Anda mainkan hanya dengan mendaftar satu ID. Dengan satu ID tersebut, Anda dapat mengakses seluruh permainan yang tersedia di situs kami.
Sebagai situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), ANGKOT88 menjamin keamanan dan kenyamanan Anda. Situs kami didukung oleh server hosting yang cepat dan sistem keamanan dengan metode enkripsi terbaru di dunia, sehingga data Anda akan selalu terjaga keamanannya. Tampilan situs yang modern juga membuat Anda merasa nyaman saat mengakses situs kami.
Keunggulan ANGKOT88
Selain menjadi situs game online terbaik, ANGKOT88 juga menawarkan layanan praktis untuk melakukan deposit menggunakan pulsa XL ataupun Telkomsel dengan potongan terendah dibandingkan situs lainnya. Ini menjadikan kami salah satu situs game online pulsa terbesar di Indonesia. Anda juga dapat melakukan deposit pulsa melalui E-commerce resmi seperti OVO, Gopay, Dana, atau melalui minimarket seperti Indomaret dan Alfamart.
Kepercayaan dan Layanan
Kami di ANGKOT88 sangat menjaga kepercayaan Anda sebagai prioritas utama kami. Oleh karena itu, kami selalu berusaha menjadi agen online terpercaya dan terbaik sepanjang masa. Permainan game online yang kami tawarkan sangat praktis, sehingga Anda dapat memainkannya kapan saja dan di mana saja tanpa perlu repot bepergian. Kami menyediakan berbagai jenis game, termasuk yang disiarkan secara LIVE (langsung) dengan host cantik dan kamera yang merekam secara real-time, menjadikan ANGKOT88 situs game online terlengkap dan terbesar di Indonesia.
Promo Menarik dan Menguntungkan
ANGKOT88 juga menawarkan banyak sekali promo menarik dan menguntungkan. Anda bisa menikmati berbagai macam promo yang sesuai dengan kebutuhan Anda, seperti welcome bonus 20%, bonus deposit harian, dan cashback. Semua promo ini tersedia di situs ANGKOT88. Selain itu, kami juga memiliki layanan Customer Service yang siap membantu Anda kapan saja.
Jadi, tunggu apa lagi? Bergabunglah dengan ANGKOT88 dan nikmati pengalaman bermain game online terbaik dan teraman di Indonesia. Daftarkan diri Anda sekarang dan mulai mainkan game favorit Anda dengan nyaman dan aman di situs kami!
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Wow that was odd. I just wrote an incredibly long comment but after I clicked submit my comment didn’t show up. Grrrr… well I’m not writing all that over again. Anyway, just wanted to say superb blog!
Italian production service company
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
supermoney88
SUPERMONEY88: Situs Game Online Deposit Pulsa Terbaik di Indonesia
SUPERMONEY88 adalah situs game online deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai macam game online terbaik dan terlengkap yang bisa Anda mainkan di situs game online kami. Hanya dengan mendaftar satu ID, Anda bisa memainkan seluruh permainan yang tersedia di SUPERMONEY88.
Keunggulan SUPERMONEY88
SUPERMONEY88 juga merupakan situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), yang berarti situs ini sangat aman. Kami didukung dengan server hosting yang cepat dan sistem keamanan dengan metode enkripsi termutakhir di dunia untuk menjaga keamanan database Anda. Selain itu, tampilan situs kami yang sangat modern membuat Anda nyaman mengakses situs kami.
Layanan Praktis dan Terpercaya
Selain menjadi game online terbaik, ada alasan mengapa situs SUPERMONEY88 ini sangat spesial. Kami memberikan layanan praktis untuk melakukan deposit yaitu dengan melakukan deposit pulsa XL ataupun Telkomsel dengan potongan terendah dari situs game online lainnya. Ini membuat situs kami menjadi salah satu situs game online pulsa terbesar di Indonesia. Anda bisa melakukan deposit pulsa menggunakan E-commerce resmi seperti OVO, Gopay, Dana, atau melalui minimarket seperti Indomaret dan Alfamart.
Kami juga terkenal sebagai agen game online terpercaya. Kepercayaan Anda adalah prioritas kami, dan itulah yang membuat kami menjadi agen game online terbaik sepanjang masa.
Kemudahan Bermain Game Online
Permainan game online di SUPERMONEY88 memudahkan Anda untuk memainkannya dari mana saja dan kapan saja. Anda tidak perlu repot bepergian lagi, karena SUPERMONEY88 menyediakan beragam jenis game online. Kami juga memiliki jenis game online yang dipandu oleh host cantik, sehingga Anda tidak akan merasa bosan.
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
sapporo88
SUPERMONEY88: Situs Game Online Deposit Pulsa Terbaik di Indonesia
SUPERMONEY88 adalah situs game online deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai macam game online terbaik dan terlengkap yang bisa Anda mainkan di situs game online kami. Hanya dengan mendaftar satu ID, Anda bisa memainkan seluruh permainan yang tersedia di SUPERMONEY88.
Keunggulan SUPERMONEY88
SUPERMONEY88 juga merupakan situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), yang berarti situs ini sangat aman. Kami didukung dengan server hosting yang cepat dan sistem keamanan dengan metode enkripsi termutakhir di dunia untuk menjaga keamanan database Anda. Selain itu, tampilan situs kami yang sangat modern membuat Anda nyaman mengakses situs kami.
Layanan Praktis dan Terpercaya
Selain menjadi game online terbaik, ada alasan mengapa situs SUPERMONEY88 ini sangat spesial. Kami memberikan layanan praktis untuk melakukan deposit yaitu dengan melakukan deposit pulsa XL ataupun Telkomsel dengan potongan terendah dari situs game online lainnya. Ini membuat situs kami menjadi salah satu situs game online pulsa terbesar di Indonesia. Anda bisa melakukan deposit pulsa menggunakan E-commerce resmi seperti OVO, Gopay, Dana, atau melalui minimarket seperti Indomaret dan Alfamart.
Kami juga terkenal sebagai agen game online terpercaya. Kepercayaan Anda adalah prioritas kami, dan itulah yang membuat kami menjadi agen game online terbaik sepanjang masa.
Kemudahan Bermain Game Online
Permainan game online di SUPERMONEY88 memudahkan Anda untuk memainkannya dari mana saja dan kapan saja. Anda tidak perlu repot bepergian lagi, karena SUPERMONEY88 menyediakan beragam jenis game online. Kami juga memiliki jenis game online yang dipandu oleh host cantik, sehingga Anda tidak akan merasa bosan.
PRO88: Situs Game Online Deposit Pulsa Terbaik di Indonesia
PRO88 adalah situs game online deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai macam game online terbaik dan terlengkap yang bisa Anda mainkan di situs game online kami. Hanya dengan mendaftar satu ID, Anda bisa memainkan seluruh permainan yang tersedia di PRO88.
Keunggulan PRO88
PRO88 juga merupakan situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), yang berarti situs ini sangat aman. Kami didukung dengan server hosting yang cepat dan sistem keamanan dengan metode enkripsi termutakhir di dunia untuk menjaga keamanan database Anda. Selain itu, tampilan situs kami yang sangat modern membuat Anda nyaman mengakses situs kami.
Berbagai Macam Game Online
Kami menyediakan berbagai macam game online terbaik yang bisa Anda mainkan kapan saja dan di mana saja. Dengan satu ID, Anda bisa menikmati semua permainan yang tersedia, mulai dari permainan kartu, slot, hingga taruhan olahraga. PRO88 memastikan semua game yang kami sediakan adalah yang terbaik dan terlengkap di Indonesia.
Keamanan dan Kenyamanan
Kami memahami betapa pentingnya keamanan dan kenyamanan bagi para pemain. Oleh karena itu, PRO88 menggunakan server hosting yang cepat dan sistem keamanan dengan metode enkripsi termutakhir di dunia. Ini memastikan bahwa data pribadi dan transaksi Anda selalu aman bersama kami. Tampilan situs yang modern juga dirancang untuk memberikan pengalaman bermain yang nyaman dan menyenangkan.
Kesimpulan
PRO88 adalah pilihan terbaik untuk Anda yang mencari situs game online deposit pulsa yang aman dan terpercaya. Dengan berbagai macam game online terbaik dan terlengkap, serta dukungan keamanan yang canggih, PRO88 siap memberikan pengalaman bermain game yang tak terlupakan. Daftar sekarang juga di PRO88 dan nikmati semua permainan yang tersedia hanya dengan satu ID.
Kunjungi kami di PRO88 dan mulailah petualangan game online Anda bersama kami!
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Clear & Healthy Nails en-nanodefensepro.com
hearing supplement en-zencortexi.com
에그벳 스포츠
“아…” Tian Jing은 깜짝 놀랐고 Hongzhi 황제가 왜 그런 질문을했는지 이해했습니다.
методы продвижения сайта
Консультация по сео продвижению.
Информация о том как работать с низкочастотными ключевыми словами и как их подбирать
Стратегия по работе в конкурентной нише.
У меня есть постоянных клиентов сотрудничаю с 3 фирмами, есть что сообщить.
Ознакомьтесь мой аккаунт, на 31 мая 2024г
количество успешных проектов 2181 только здесь.
Консультация только устно, без снимков с экрана и документов.
Время консультации указано 2 ч, но по факту всегда на контакте без жёсткой привязки ко времени.
Как управлять с программным обеспечением это уже иначе история, консультация по работе с программами обсуждаем отдельно в отдельном кворке, определяем что нужно при коммуникации.
Всё без суеты на расслабленно не в спешке
To get started, the seller needs:
Мне нужны контакты от телеграм каналов для связи.
разговор только устно, вести переписку недостаточно времени.
Сб и Воскресенье выходной
melbet
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Wow that was unusual. I just wrote an incredibly long comment but after I clicked submit my comment didn’t appear. Grrrr… well I’m not writing all that over again. Anyway, just wanted to say superb blog!
lgo4d
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
sunmory33
sunmory33
bocor88
bocor88
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
在線娛樂城的世界
隨著互聯網的迅速發展,網上娛樂城(線上賭場)已經成為許多人休閒的新選擇。線上娛樂城不僅提供多種的遊戲選擇,還能讓玩家在家中就能體驗到賭場的樂趣和快感。本文將探討在線娛樂城的特徵、利益以及一些常見的的游戲。
什麼叫線上娛樂城?
線上娛樂城是一種經由網際網路提供賭博遊戲的平台。玩家可以通過電腦設備、智慧型手機或平板設備進入這些網站,參與各種賭博活動,如撲克、賭盤、21點和吃角子老虎等。這些平台通常由專業的軟件公司開發,確保游戲的公正和安全。
在線娛樂城的優勢
便利性:玩家無需離開家,就能享受賭博的樂趣。這對於那些居住在遠離的實體賭場地方的人來說尤其方便。
多種的游戲選擇:網上娛樂城通常提供比實體賭場更豐富的游戲選擇,並且經常改進遊戲內容,保持新鮮。
好處和獎金:許多網上娛樂城提供多樣的獎勵計劃,包括註冊紅利、存款獎金和忠誠度計劃,吸引新新玩家並促使老玩家繼續遊戲。
安全性和隱私:正當的線上娛樂城使用先進的加密方法來保護玩家的個人資料和財務交易,確保游戲過程的穩定和公正。
常有的線上娛樂城游戲
撲克牌:德州撲克是最流行賭錢游戲之一。網上娛樂城提供多種撲克牌變體,如德州扑克、奧馬哈撲克和七張撲克等。
輪盤賭:輪盤是一種經典的賭場遊戲,玩家可以投注在單數、數字組合上或顏色上,然後看轉球落在哪個地方。
21點:又稱為二十一點,這是一種競爭玩家和莊家點數的游戲,目標是讓手牌點數盡可能接近21點但不超過。
吃角子老虎:老虎机是最受歡迎並且是最流行的博彩遊戲之一,玩家只需轉捲軸,看圖案排列出獲勝的組合。
結論
網上娛樂城為現代賭博愛好者提供了一個便捷、刺激且多元化的娛樂活動。不論是撲克牌愛好者還是老虎機迷,大家都能在這些平台上找到適合自己的遊戲。同時,隨著技術的不斷提升,網上娛樂城的遊戲體驗將變化越來越現實和有趣。然而,玩家在體驗游戲的同時,也應該保持,避免沉迷於賭錢活動,維持健康的心態。
線上娛樂城的天地
隨著互聯網的迅速發展,線上娛樂城(線上賭場)已經成為許多人消遣的新選擇。在線娛樂城不僅提供多種的遊戲選擇,還能讓玩家在家中就能體驗到賭場的樂趣和樂趣。本文將討論線上娛樂城的特色、好處以及一些常見的游戲。
什麼網上娛樂城?
網上娛樂城是一種經由網際網路提供賭博游戲的平台。玩家可以透過電腦、智能手機或平板設備進入這些網站,參與各種博彩活動,如撲克、輪盤、二十一點和老虎機等。這些平台通常由專業的的程序公司開發,確保游戲的公正性和安全。
網上娛樂城的利益
便利性:玩家不需要離開家,就能享用賭錢的快感。這對於那些生活在偏遠實體賭場地方的人來說尤其方便。
多種的遊戲選擇:在線娛樂城通常提供比實體賭場更多樣化的遊戲選擇,並且經常更新遊戲內容,保持新鮮感。
優惠和獎勵:許多網上娛樂城提供多樣的獎金計劃,包括註冊獎勵、存款獎金和會員計劃,引誘新玩家並促使老玩家繼續遊戲。
安全和保密性:正規的在線娛樂城使用先進的加密來保護玩家的私人信息和金融交易,確保遊戲過程的公平和公正性。
常有的在線娛樂城遊戲
撲克:撲克牌是最受歡迎賭博游戲之一。在線娛樂城提供多種撲克牌變體,如德州撲克、奧馬哈撲克和七張牌等。
輪盤:輪盤賭是一種經典的賭場遊戲,玩家可以投注在單個數字、數字排列或顏色選擇上,然後看球落在哪個區域。
二十一點:又稱為21點,這是一種比拼玩家和莊家點數點數的遊戲,目標是讓手牌點數點數盡量接近21點但不超過。
吃角子老虎:吃角子老虎是最容易並且是最流行的賭錢遊戲之一,玩家只需轉動捲軸,等待圖案圖案排列出贏得的組合。
總結
在線娛樂城為現代賭博愛好者提供了一個方便的、刺激的且多元化的娛樂方式。不管是撲克牌愛好者還是吃角子老虎迷,大家都能在這些平台上找到適合自己的游戲。同時,隨著科技的不斷進步,線上娛樂城的游戲體驗將變得越來越真實和吸引人。然而,玩家在享用游戲的同時,也應該保持自律,避免沉溺於賭博活動,保持健康的娛樂心態。
Консультация по сео стратегии продвижению.
Информация о том как работать с низкочастотными запросами и как их выбирать
Стратегия по деятельности в соперничающей нише.
У меня есть регулярных работаю с тремя фирмами, есть что сообщить.
Изучите мой досье, на 31 мая 2024г
общий объём успешных проектов 2181 только здесь.
Консультация только устно, без скриншотов и отчетов.
Продолжительность консультации указано 2 часа, но по факту всегда на доступен без строгой привязки к графику.
Как взаимодействовать с программным обеспечением это уже другая история, консультация по использованию ПО обсуждаем отдельно в отдельном разделе, определяем что необходимо при разговоре.
Всё без суеты на без напряжения не в спешке
To get started, the seller needs:
Мне нужны контакты от телеграм канала для коммуникации.
общение только в устной форме, переписываться не хватает времени.
Сб и воскресенья выходной
럭키 네코
Zhu Houzhao는 아버지를 이상하게 바라보며 이해할 수 없었습니다.
한국 마약
빠릿한 환충 서비스와 더불어 주요업체의 보안성
베팅사이트 이용 시 매우 중요한 요소 중 하나는 신속한 입출금 절차입니다. 대개 세 분 이내에 충전, 열 분 내에 환전이 처리되어야 합니다. 메이저 주요업체들은 필요한 직원 채용을 통해 이 같은 신속한 환충 절차를 약속하며, 이 방법으로 회원들에게 안전한 느낌을 드립니다. 메이저사이트를 접속하면서 스피드 있는 체감을 즐겨보세요. 저희는 여러분들이 보안성 있게 토토사이트를 접속할 수 있도록 돕는 먹튀해결 전문가입니다.
보증금을 걸고 배너를 운영
먹튀 해결 팀은 적어도 삼천만 원에서 억대의 보증금을 예치하고 있는 업체들의 배너를 운영하고 있습니다. 만약 먹튀 피해가 발생할 시, 배팅 규정에 반하지 않은 배팅 내역을 스크린샷을 찍어 먹튀 해결 전문가에게 문의하시면, 사실 확인 후 보증 자금으로 즉시 피해 보상을 처리합니다. 피해가 발생하면 빠르게 캡처하여 피해 내용을 기록해두시고 제출해 주세요.
장기 운영 안전업체 확인
먹튀 해결 팀은 최대한 4년간 먹튀 문제 없이 안정적으로 운영하고 있는 업체만을 인증하여 광고 배너 입점을 허용합니다. 이 때문에 모두가 알만한 대형사이트를 안전하게 사용할 수 있는 기회를 제공하고 있습니다. 철저한 검증 작업을 통해 인증된 사이트를 놓치지 않도록, 보안된 배팅을 체험해보세요.
투명성과 공정성을 가진 먹튀 검증
먹튀 해결 팀의 먹튀 검토는 공정성과 공정을 기반으로 합니다. 언제나 이용자들의 관점을 우선시하며, 기업의 유혹이나 이득에 흔들리지 않으며 한 건의 삭제 없이 진실만을 근거로 검증해왔습니다. 먹튀 피해를 겪고 후회하지 않도록, 바로 지금 시작해보세요.
먹튀검증사이트 목록
먹튀 해결 전문가가 선별한 안전한 토토사이트 검증된 업체 목록 입니다. 지금 등록된 검증된 업체들은 먹튀 사고 발생 시 100% 보증을 도와드립니다. 하지만, 제휴 기간이 끝난 업체에서 발생한 피해에 대해서는 책임지지 않습니다.
탁월한 먹튀 검증 알고리즘
먹튀 해결 전문가는 공정한 베팅 문화를 조성하기 위해 늘 노력하고 있습니다. 저희는 소개하는 토토사이트에서 안전하게 배팅하세요. 회원님의 먹튀 신고 내용은 먹튀 리스트에 기재되어 그 해당 베팅 사이트에 심각한 영향을 줄 수 있습니다. 먹튀 목록 작성 시 먹튀블러드만의 검증 노하우를 충분히 활용하여 정확한 검증을 할 수 있도록 하겠습니다.
안전한 베팅 문화를 제공하기 위해 끊임없이 노력하는 먹튀 해결 팀과 함께 안심하고 경험해보세요.
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Советы по оптимизации продвижению.
Информация о том как управлять с низкочастотными запросами и как их определять
Тактика по работе в конкурентоспособной нише.
Обладаю постоянных сотрудничаю с тремя компаниями, есть что сообщить.
Изучите мой профиль, на 31 мая 2024г
общий объём выполненных работ 2181 только здесь.
Консультация только устно, без скриншотов и отчетов.
Продолжительность консультации указано 2 ч, но по реально всегда на доступен без жёсткой привязки ко времени.
Как управлять с программным обеспечением это уже иначе история, консультация по работе с софтом оговариваем отдельно в специальном разделе, определяем что нужно при общении.
Всё спокойно на расслабоне не спеша
To get started, the seller needs:
Мне нужны данные от телеграм каналов для контакта.
коммуникация только устно, общаться письменно нету времени.
Суббота и Воскресенье нерабочие дни
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
geinoutime.com
하지만 지금 이 순간… 작업장 전체가 혼란에 휩싸였습니다.
geinoutime.com
“일어나 얘기해. 다른 거 없어? 없으면 나가.”
mawartoto
Inspirasi dari Kutipan Taylor Swift: Harapan dan Cinta dalam Lagu-Lagunya
Taylor Swift, seorang musisi dan penulis lagu populer, tidak hanya dikenal oleh karena lagu yang menawan dan vokal yang merdu, tetapi juga karena kata-kata lagu-lagunya yang penuh makna. Di dalam lirik-liriknya, Swift sering menggambarkan berbagai aspek kehidupan, berawal dari cinta hingga tantangan hidup. Berikut adalah beberapa petikan inspiratif dari lagu-lagunya, beserta artinya.
“Mungkin yang terbaik belum datang.” – “All Too Well”
Arti: Bahkan di masa-masa sulit, senantiasa ada seberkas harapan dan kemungkinan akan hari yang lebih baik.
Lirik ini dari lagu “All Too Well” mengingatkan kita bahwa meskipun kita mungkin menghadapi waktu sulit sekarang, selalu ada kemungkinan bahwa masa depan bisa mendatangkan sesuatu yang lebih baik. Ini adalah amanat harapan yang memperkuat, merangsang kita untuk terus bertahan dan tidak mengalah, karena yang terbaik mungkin belum datang.
“Aku akan bertahan lantaran aku tidak bisa menjalankan apa pun tanpamu.” – “You Belong with Me”
Penjelasan: Menemukan cinta dan dukungan dari orang lain dapat memberi kita daya dan tekad untuk bertahan melalui tantangan.
hcs777
Ashley JKT48: Bintang yang Berkilau Terang di Dunia Idola
Siapa Ashley JKT48?
Siapakah sosok muda berbakat yang menyita perhatian banyak penggemar lagu di Indonesia dan Asia Tenggara? Beliau adalah Ashley Courtney Shintia, atau yang lebih dikenal dengan nama panggungnya, Ashley JKT48. Masuk dengan grup idola JKT48 pada tahun 2018, Ashley dengan segera muncul sebagai salah satu anggota paling favorit.
Profil
Lahir di Jakarta pada tanggal 13 Maret 2000, Ashley memiliki darah Tionghoa-Indonesia. Beliau mengawali perjalanannya di industri hiburan sebagai peraga dan aktris, sebelum akhirnya menjadi anggota dengan JKT48. Kepribadiannya yang gembira, suara yang mantap, dan kemahiran menari yang memukau menjadikannya idol yang sangat dikasihi.
Penghargaan dan Pengakuan
Kepopuleran Ashley telah dikenal melalui banyak apresiasi dan nominasi. Pada tahun 2021, ia meraih award “Anggota Paling Populer JKT48” di ajang JKT48 Music Awards. Ia juga dinobatkan sebagai “Idol Tercantik se-Asia” oleh sebuah media digital pada tahun 2020.
Peran dalam JKT48
Ashley mengisi peran krusial dalam grup JKT48. Beliau adalah personel Tim KIII dan berperan sebagai penari utama dan vokal utama. Ashley juga menjadi bagian dari unit sub “J3K” bersama Jessica Veranda dan Jennifer Rachel Natasya.
Karir Mandiri
Selain aktivitasnya di JKT48, Ashley juga merintis karier solo. Beliau telah meluncurkan beberapa single, antara lain “Myself” (2021) dan “Falling Down” (2022). Ashley juga telah berkolaborasi bareng artis lain, seperti Afgan dan Rossa.
Kehidupan Pribadi
Di luar bidang perform, Ashley dikenal sebagai orang yang low profile dan bersahabat. Ashley suka menyisihkan waktu dengan family dan teman-temannya. Ashley juga punya hobi melukis dan fotografi.
Анализ адреса токенов
Верификация токенов TRC20 и различных цифровых операций
На представленном сайте вы найдете развернутые ревью различных платформ для контроля переводов и аккаунтов, в том числе anti-money laundering контроли для токенов и прочих виртуальных валют. Вот важные опции, доступные в наших оценках:
Верификация монет TRC20
Некоторые ресурсы обеспечивают всестороннюю анализ транзакций монет в сети TRC20 платформы. Это дает возможность идентифицировать подозреваемую операции и удовлетворять нормативным стандартам.
Анализ операций USDT
В представленных описаниях доступны инструменты для комплексного анализа и мониторинга переводов USDT, что помогает гарантировать открытость и защищенность транзакций.
AML анализ токенов
Некоторые платформы обеспечивают антиотмывочную контроль монет, обеспечивая обнаруживать и исключать ситуации незаконных операций и валютных мошенничеств.
Проверка счета монет
Наши ревью представляют сервисы, которые обеспечивают верифицировать аккаунты монет на предмет блокировок и подозреваемых операций, гарантируя повышенную степень безопасности защищенности.
Проверка платежей криптовалюты на сети TRC20
Вы сможете найти найдете инструменты, обеспечивающие анализ платежей токенов в сети TRC20 блокчейна, что обеспечивает поддерживает соблюдение всем стандартам необходимым положениям.
Анализ адреса адреса USDT
В ревью описаны сервисы для проверки счетов кошельков монет на предмет опасностей угроз.
Анализ кошелька монет на блокчейне TRC20
Наши обзоры представляют платформы, предлагающие контроль кошельков токенов в блокчейн-сети TRC20 сети, что позволяет предотвратить мошенничество и валютных преступлений.
Верификация криптовалюты на легитимность
Рассмотренные ресурсы предусматривают верифицировать переводы и кошельки на прозрачность, выявляя подозрительную активность.
антиотмывочная проверка USDT на блокчейне TRC20
В оценках вы сервисы, обеспечивающие антиотмывочную верификацию для токенов на блокчейне TRC20 блокчейна, помогая вашему бизнесу соблюдать глобальным положениям.
Анализ криптовалюты ERC20
Наши обзоры включают платформы, предоставляющие проверку криптовалюты в блокчейн-сети ERC20, что обеспечивает гарантирует комплексный анализ переводов и кошельков.
Контроль цифрового кошелька
Мы изучаем платформы, предоставляющие опции по контролю виртуальных кошельков, содержащие отслеживание переводов и определение подозреваемой операций.
Проверка кошелька цифрового кошелька
Наши оценки включают платформы, позволяющие контролировать кошельки цифровых кошельков для обеспечения повышенной защиты.
Проверка криптокошелька на платежи
Вы найдете представлены инструменты для проверки виртуальных кошельков на переводы, что помогает обеспечивает поддерживать прозрачность операций.
Верификация криптокошелька на отсутствие подозрительных действий
Наши обзоры представляют инструменты, позволяющие контролировать виртуальные кошельки на прозрачность, определяя подозрительные сомнительные действия.
Ознакомившись с подробные ревью, вы подберете лучшие платформы для контроля и отслеживания блокчейн транзакций, чтобы обеспечивать обеспечивать повышенный уровень безопасности защиты и соблюдать необходимым законодательным правилам.
This is beyond beautiful, I’m speechless!
You’ve created something truly special here, well done!
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Online Casinos: Innovation and Advantages for Contemporary Society
Overview
Online casinos are virtual platforms that offer players the opportunity to engage in gambling activities such as card games, spin games, blackjack, and slots. Over the past few years, they have become an essential component of digital entertainment, providing various advantages and possibilities for players around the world.
Availability and Ease
One of the primary benefits of online casinos is their availability. Users can enjoy their preferred games from anywhere in the globe using a computer, tablet, or smartphone. This conserves time and funds that would otherwise be spent going to traditional gambling halls. Furthermore, 24/7 availability to activities makes internet gambling sites a easy option for people with busy schedules.
Range of Games and Experience
Online gambling sites provide a vast range of games, enabling all users to discover something they enjoy. From classic table games and board activities to slot machines with various concepts and progressive jackpots, the range of activities ensures there is something for every preference. The ability to engage at different proficiencies also makes online casinos an perfect location for both novices and seasoned gamblers.
Financial Advantages
The online casino sector contributes significantly to the economic system by generating jobs and producing revenue. It backs a wide variety of careers, including programmers, client assistance agents, and advertising professionals. The revenue produced by online casinos also adds to government funds, which can be allocated to support community services and infrastructure projects.
Advancements in Technology
Digital gambling sites are at the forefront of technological innovation, constantly integrating new innovations to enhance the gaming experience. High-quality graphics, real-time dealer activities, and VR gambling sites provide immersive and authentic gaming experiences. These advancements not only improve player experience but also push the boundaries of what is possible in online entertainment.
Safe Betting and Support
Many digital casinos promote safe betting by offering tools and assistance to assist users manage their betting habits. Features such as deposit limits, self-exclusion options, and access to support services guarantee that users can enjoy gaming in a safe and controlled environment. These steps show the sector’s dedication to encouraging healthy betting habits.
Community Engagement and Community
Digital casinos often provide interactive options that allow users to interact with each other, creating a feeling of community. Group games, communication tools, and networking integration enable users to network, share experiences, and build friendships. This social aspect improves the entire betting experience and can be especially helpful for those seeking community engagement.
Conclusion
Online gambling sites offer a diverse range of advantages, from availability and convenience to economic contributions and technological advancements. They provide varied gaming choices, encourage safe betting, and promote community engagement. As the industry keeps to evolve, digital gambling sites will probably remain a major and beneficial presence in the world of digital entertainment.
Complimentary Slot Games: Amusement and Perks for All
Free slot games have become a widespread form of digital leisure, granting players the rush of slot machines free from any economic outlay.
The chief purpose of free slot games is to provide a entertaining and absorbing way for people to enjoy the suspense of slot machines absent any monetary jeopardy. They are developed to imitate the impression of actual-currency slots, enabling players to spin the reels, enjoy various motifs, and obtain electronic prizes.
Fun: No-Cost slot games are an excellent option of amusement, providing periods of pleasure. They feature lively visuals, immersive soundtracks, and wide-ranging motifs that accommodate a comprehensive selection of inclinations.
Proficiency Improvement: For inexperienced, free slot games provide a secure setting to familiarize the mechanics of slot machines. Players can get accustomed with multiple options, win lines, and additional features devoid of the worry of relinquishing money.
Destressing: Playing complimentary slot games can be a wonderful way to relax. The simple experience and the chance for digital prizes make it an satisfying hobby.
Shared Experiences: Many no-cost slot games integrate collaborative features such as challenges and the option to connect with fellow players. These features add a group-based layer to the interactive experience, motivating players to compete against each other.
Perks of No-Cost Slot Games
1. Availability and Comfort
Free slot games are readily available to all with an internet connection. They can be accessed on multiple gadgets including PCs, tablets, and handsets. This convenience gives players to savor their favorite offerings at any time and anywhere.
2. Fiscal Unconcern
One of the most significant rewards of no-cost slot games is that they remove the financial risks linked to gambling. Players can experience the rush of triggering the reels and hitting major payouts without investing any money.
3. Variety of Games
No-Cost slot games are available in a broad selection of ideas and designs, from nostalgic fruit machines to modern video slots with elaborate plotlines and visuals. This variety ensures that there is something for anyone, irrespective of their preferences.
4. Strengthening Intellectual Faculties
Playing no-cost slot games can contribute to strengthen intellectual faculties such as anticipatory planning. The necessity to consider payout lines, learn procedural knowledge, and predict effects can offer a cognitive workout that is equally pleasurable and helpful.
5. Safe Testing Ground for For-Profit Wagering
For those considering shifting to actual-currency slots, gratis slot games grant a beneficial pre-experience. Players can experiment with different games, refine methods, and acquire confidence ahead of electing to invest real funds. This readiness can result in a better-informed and enjoyable real-money gaming encounter.
Summary
No-Cost slot games grant a plethora of perks, from unadulterated pleasure to proficiency improvement and interpersonal connections. They grant a safe and cost-free way to relish the suspense of slot machines, establishing them a helpful extension to the landscape of online leisure. Whether you’re looking to destress, hone your intellectual faculties, or merely enjoy yourself, free slot games are a wonderful alternative that continues to captivate players worldwide.
online casino real money
Online Casino Paid: Upsides for Participants
Preface
Virtual gambling platforms delivering paid games have secured immense widespread adoption, offering participants with the chance to earn financial payouts while relishing their cherished gambling activities from home. This article analyzes the advantages of virtual wagering environment real money games, emphasizing their positive consequence on the leisure domain.
Ease of Access and Reachability
Internet-based gambling platform real money offerings offer user-friendliness by enabling users to access a extensive array of activities from anywhere with an web access point. This excludes the necessity to make trips to a brick-and-mortar gaming venue, preserving effort. Digital gaming sites are in addition accessible at all times, permitting users to partake in at their user-friendliness.
Range of Possibilities
Digital gaming sites offer a more comprehensive diversity of experiences than brick-and-mortar casinos, featuring slot-related offerings, blackjack, wheel of fortune, and table games. This breadth gives participants to investigate unfamiliar activities and discover novel most preferred, improving their comprehensive gaming experience.
Perks and Advantages
Digital gaming sites grant considerable rewards and promotions to entice and maintain customers. These bonuses can feature new player incentives, non-chargeable turns, and reimbursement promotions, delivering additional significance for participants. Reward initiatives as well reward players for their uninterrupted custom.
Competency Enhancement
Playing real money experiences on the internet can enable players refine aptitudes such as decision-making. Offerings like pontoon and poker demand customers to arrive at choices that can influence the outcome of the offering, assisting them develop problem-solving skills.
Social Interaction
ChatGPT l Валли, 6.06.2024 4:08]
Virtual wagering environments deliver prospects for communal engagement through discussion forums, interactive platforms, and real-time croupier games. Users can communicate with their peers, communicate tips and strategies, and occasionally form personal connections.
Financial Advantages
The online casino sector generates jobs and lends to the economic landscape through fiscal revenues and regulatory costs. This fiscal impact advantages a comprehensive variety of fields, from experience developers to player support professionals.
Recap
Internet-based gambling platform actual currency activities grant multiple upsides for users, incorporating convenience, diversity, rewards, proficiency improvement, interpersonal connections, and monetary benefits. As the industry constantly advance, the widespread adoption of virtual wagering environments is projected to rise.
fortune casino
Wealth Gaming Site: At a Location Where Amusement Meets Prosperity
Prosperity Gaming Site is a well-liked virtual venue characterized for its broad range of experiences and enthralling rewards. Let’s investigate the motivations behind so several players enjoy engaging with Prosperity Gaming Site and in which manner it advantages them.
Amusement Factor
Luck Wagering Environment presents a variety of games, featuring nostalgic wagering games like pontoon and wheel of fortune, as alongside novel slot machines. This variety provides that there is a choice for anyone, constituting every single visit to Prosperity Casino satisfying and fun.
Substantial Payouts
One of the principal draws of Luck Gambling Platform is the chance to secure major payouts. With substantial jackpots and benefits, players have the possibility to produce an unexpected outcome with a individual round or deal. Numerous customers have obtained significant winnings, augmenting the suspense of interacting with Fortune Wagering Environment.
Convenience and Accessibility
Wealth Gaming Site’s internet-based platform establishes it as convenient for participants to relish their favorite activities from any location. Regardless of whether at abode or while mobile, players can utilize Fortune Wagering Environment from their desktop or mobile device. This approachability guarantees that users can experience the excitement of the casino anytime they want, devoid of the necessity to travel.
Breadth of Offerings
Luck Gaming Site provides a broad choice of experiences, securing that there is an option for every single form of user. Ranging from established table games to conceptual slot-related offerings, the variety sustains users immersed and delighted. This selection likewise allows participants to explore novel offerings and find unfamiliar most liked.
Incentives and Special Offers
Prosperity Gambling Platform rewards its customers with bonuses and special offers, involving introductory bonuses and membership initiatives. These bonuses not merely elevate the interactive sensation but also raise the opportunities of winning big. Participants are continually driven to sustain interaction, rendering Luck Wagering Environment increasingly enticing.
Communal Engagement and Interpersonal Connections
ChatGPT l Валли, 6.06.2024 4:30]
Wealth Wagering Environment grants a feeling of togetherness and communal engagement for participants. By means of messaging platforms and forums, participants can communicate with fellow users, discuss tips and approaches, and even develop interpersonal bonds. This communal aspect contributes a supplemental facet of fulfillment to the entertainment interaction.
Summary
Wealth Gambling Platform presents a extensive selection of benefits for users, encompassing entertainment, the prospect of securing major payouts, user-friendliness, diversity, bonuses, and social interaction. Whether desiring suspense or aiming to experience a reversal of fortune, Fortune Gambling Platform offers an thrilling sensation for any partake in.
Complimentary Virtual Wagering Games: A Enjoyable and Profitable Encounter
Gratis poker machine offerings have emerged as progressively widely-accepted among customers desiring a captivating and safe interactive sensation. These games present a extensive range of upsides, establishing them as a chosen option for numerous. Let’s examine in which manner no-cost virtual wagering activities can benefit users and the reasons why they are so broadly enjoyed.
Entertainment Value
One of the primary drivers players savor engaging with free poker machine activities is for the entertainment value they offer. These games are created to be captivating and enthralling, with animated visuals and immersive music that elevate the comprehensive leisure sensation. Whether you’re a occasional user aiming to occupy your time or a enthusiastic gamer aspiring to thrills, free poker machine experiences offer amusement for all.
Competency Enhancement
Engaging with free poker machine experiences can as well help develop beneficial skills such as strategic thinking. These offerings call for customers to make immediate decisions contingent on the virtual assets they are dealt, assisting them hone their decision-making abilities and mental agility. Additionally, customers can experiment with various methods, honing their skills devoid of the possibility of financial impact of relinquishing paid funds.
Convenience and Accessibility
A supplemental benefit of complimentary slot-based experiences is their convenience and availability. These activities can be engaged with in the digital realm from the ease of your own residence, removing the need to travel to a brick-and-mortar gaming venue. They are as well offered at all times, allowing users to experience them at whichever occasion that aligns with them. This simplicity renders gratis electronic gaming experiences a well-liked possibility for users with demanding agendas or those desiring a swift entertainment resolution.
Social Interaction
Numerous no-cost virtual wagering offerings also present communal elements that give players to connect with each other. This can include chat rooms, interactive platforms, and competitive settings where customers can challenge their peers. These social interactions contribute an further layer of satisfaction to the interactive interaction, giving users to interact with peers who share their interests.
Anxiety Reduction and Mental Unwinding
Interacting with no-cost virtual wagering activities can likewise be a superb way to unwind and calm down after a tiring day. The uncomplicated engagement and peaceful music can assist reduce anxiety and anxiety, granting a desired respite from the challenges of regular life. Also, the thrill of receiving virtual payouts can boost your mood and leave you feeling rejuvenated.
Conclusion
Free poker machine activities present a extensive array of rewards for users, including enjoyment, skill development, ease, social interaction, and worry mitigation and mental rejuvenation. Regardless of whether you’re looking to hone your leisure faculties or merely enjoy yourself, free poker machine games provide a advantageous and fulfilling interaction for users of every degrees.
Virtual Table Games: A Source of Fun and Skill Development
Online card games has materialized as a sought-after kind of amusement and a medium for proficiency improvement for customers globally. This write-up explores the favorable aspects of virtual casino-style games and the extent to which it benefits individuals, underscoring its far-reaching acceptance and effect.
Entertainment Value
Virtual casino-style games grants a exciting and compelling leisure experience, enthralling players with its calculated interactivity and changeable conclusions. The activity’s engrossing nature, coupled with its group-based aspects, provides a singular kind of fun that many consider rewarding.
Skill Development
Beyond entertainment, online poker likewise acts as a avenue for capability building. The offering necessitates decision-making, snap judgments, and the aptitude to comprehend opponents, all of which contribute to cognitive development. Customers can elevate their decision-making aptitudes, emotional intelligence, and sound judgment aptitudes through regular activity.
Simplicity and Approachability
One of the primary rewards of virtual casino-style games is its ease and reachability. Players can relish the experience from the comfort of their dwellings, at whichever moment that aligns with them. This approachability eradicates the requirement for travel to a physical gambling establishment, rendering it a easy-to-access option for people with busy agendas.
Breadth of Offerings and Wager Levels
Digital table games platforms present a comprehensive variety of games and stakes to target participants of any skill levels and preferences. Regardless of whether you’re a novice aiming to pick up the ropes or a skilled specialist desiring a challenge, there is a game for you. This range secures that players can always discover a experience that corresponds to their expertise and bankroll.
Communal Engagement
Virtual casino-style games as well delivers chances for social interaction. Many systems provide messaging capabilities and competitive formats that give participants to communicate with others, exchange interactions, and form friendships. This communal aspect injects substance to the leisure experience, making it even more satisfying.
Financial Rewards
For some, virtual casino-style games can as well be a wellspring of earnings opportunities. Proficient customers can obtain substantial earnings through consistent engagement, making it a financially rewarding undertaking for those who thrive at the game. Also, numerous digital table games matches offer major reward funds, granting users with the chance to win big.
Key Takeaways
Online poker presents a variety of benefits for users, incorporating fun, capability building, convenience, social interaction, and profit potential. Its recognition continues to increase, with many users turning to online poker as a wellspring of satisfaction and advancement. Whether you’re looking to refine your aptitudes or merely derive entertainment, virtual casino-style games is a flexible and beneficial hobby for players of every origins.
빠른 입출금 서비스 및 메이저업체의 안전성
토토사이트 이용 시 매우 중요한 부분 중 하나는 빠른 충환전 처리입니다. 대개 삼 분 이내에 입금, 열 분 내에 환전이 처리되어야 합니다. 대형 메이저업체들은 필요한 스태프 고용을 통해 이러한 빠른 충환전 프로세스를 보장하며, 이로써 사용자들에게 안전한 느낌을 드립니다. 주요사이트를 접속하면서 빠른 체감을 해보시기 바랍니다. 저희는 여러분이 안전하게 토토사이트를 사용할 수 있도록 도와드리는 먹튀 해결 팀입니다.
보증금을 걸고 배너 운영
먹튀 해결 전문가는 최소 삼천만 원에서 일억 원의 보증 자금을 예치한 회사들의 광고 배너를 운영합니다. 만약 먹튀 문제가 생길 경우, 배팅 규정에 반하지 않은 배팅 내역을 캡처해서 먹튀 해결 팀에 문의하시면, 사실 확인 후 보증 자금으로 즉시 피해 보상을 처리합니다. 피해가 발생하면 즉시 캡처하여 손해 내용을 저장해두시고 보내주세요.
오랫동안 안전하게 운영된 업체 확인
먹튀 해결 전문가는 최대한 4년간 먹튀 이력 없이 안전하게 운영한 사이트만을 인증하여 배너 입점을 받고 있습니다. 이로 인해 모두가 알고 있는 메이저사이트를 안전하게 이용할 수 있는 기회를 제공합니다. 철저한 검사 작업을 통해 검증된 사이트를 놓치지 말고, 안전한 베팅을 체험해보세요.
투명하고 공정한 먹튀 검토
먹튀 해결 팀의 먹튀 검토는 투명함과 공정을 바탕으로 합니다. 언제나 고객들의 입장을 최우선으로 생각하며, 사이트의 회유나 이득에 흔들리지 않으며 한 건의 삭제 없이 사실만을 바탕으로 검증해왔습니다. 먹튀 피해를 당하고 후회하지 않도록, 지금 시작해보세요.
먹튀 확인 사이트 리스트
먹튀해결사가 골라낸 안전한 베팅사이트 인증된 업체 목록 입니다. 현재 등록되어 있는 검증된 업체들은 먹튀 사고 발생 시 100% 보증을 제공해드립니다. 하지만, 제휴 기간이 만료된 업체에서 발생한 사고에 대해서는 책임을 지지 않습니다.
독보적인 먹튀 검증 알고리즘
먹튀해결사는 공정한 베팅 환경을 만들기 위해 늘 노력하고 있습니다. 저희가 추천하는 베팅사이트에서 안전하게 배팅하세요. 회원님의 먹튀 신고 내용은 먹튀 목록에 등록 노출되어 해당 스포츠토토 사이트에 치명적인 영향을 미칩니다. 먹튀 리스트 작성 시 먹튀블러드 만의 검토 경험을 충분히 활용하여 공정한 심사를 할 수 있게 하겠습니다.
안전한 베팅 환경을 제공하기 위해 계속해서 힘쓰는 먹튀 해결 전문가와 동반하여 안심하고 경험해보세요.
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I’m genuinely impressed, well done!
This post is a breath of fresh air, simply amazing!
에그 카지노
Fang Jifan은 봄바람처럼 말했습니다. “주님이 무엇을 가르쳐야하는지 모르겠습니다.”
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I’m in awe of your talent, simply amazing!
пироги
adel jkt48
Download Program 888 dan Dapatkan Kemenangan: Panduan Pendek
**Aplikasi 888 adalah opsi sempurna untuk Pengguna yang membutuhkan aktivitas berjudi online yang mengasyikkan dan menguntungkan. Bersama bonus tiap hari dan opsi menggiurkan, program ini bersiap menyediakan permainan bermain terbaik. Ini panduan cepat untuk menggunakan pelayanan Aplikasi 888.
Instal dan Segera Raih
Layanan Terdapat:
Program 888 mampu di-download di HP Android, Perangkat iOS, dan Windows. Segera bermain dengan praktis di alat apa pun.
Imbalan Tiap Hari dan Hadiah
Imbalan Login Harian:
Mendaftar setiap periode untuk mengambil bonus hingga 100K pada masa ketujuh.
Tuntaskan Misi:
Peroleh kesempatan lotere dengan merampungkan aktivitas terkait. Tiap aktivitas menyediakan Para Pengguna 1 kesempatan pengeretan untuk mengklaim keuntungan mencapai 888K.
Pengumpulan Manual:
Hadiah harus diklaim mandiri di dalam app. Yakinlah untuk mendapatkan hadiah saban masa agar tidak habis masa berlakunya.
Sistem Pengeretan
Peluang Pengeretan:
Tiap waktu, Anda bisa mendapatkan satu kesempatan lotere dengan merampungkan tugas.
Jika opsi undian habis, rampungkan lebih banyak tugas untuk meraih tambahan opsi.
Level Hadiah:
Raih keuntungan jika akumulasi lotere Para Pengguna melampaui 100K dalam satu hari.
Aturan Utama
Pengklaiman Bonus:
Keuntungan harus diterima langsung dari perangkat lunak. Jika tidak, keuntungan akan langsung diambil ke akun pengguna Pengguna setelah sebuah hari.
Peraturan Betting:
Imbalan harus ada sekitar satu taruhan efektif untuk digunakan.
Penutup
Perangkat Lunak 888 menawarkan keseruan bermain yang menyenangkan dengan keuntungan signifikan. Download aplikasi sekarang juga dan rasakan kemenangan besar-besaran tiap waktu!
Untuk informasi lebih lengkap tentang promosi, pengisian, dan skema undangan, kunjungi halaman utama program.
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
poki games
Inspirasi dari Petikan Taylor Swift
Taylor Swift, seorang penyanyi dan pengarang lagu terkemuka, tidak hanya dikenal berkat melodi yang indah dan nyanyian yang merdu, tetapi juga oleh karena syair-syair lagu-lagunya yang sarat makna. Pada syair-syairnya, Swift sering melukiskan berbagai aspek eksistensi, mulai dari kasih sampai dengan rintangan hidup. Berikut adalah beberapa ucapan inspiratif dari lagu-lagunya, bersama terjemahannya.
“Mungkin yang terbaik belum datang.” – “All Too Well”
Arti: Meskipun dalam masa-masa sulit, tetap ada seberkas harapan dan kemungkinan akan hari yang lebih baik.
Lirik ini dari lagu “All Too Well” mengingatkan kita kalau meskipun kita mungkin mengalami waktu sulit sekarang, selalu ada kemungkinan bahwa masa depan akan membawa perubahan yang lebih baik. Hal ini adalah pesan harapan yang memperkuat, memotivasi kita untuk terus bertahan dan tidak menyerah, lantaran yang terhebat mungkin belum hadir.
“Aku akan bertahan karena aku tak bisa menjalankan apa pun tanpamu.” – “You Belong with Me”
Arti: Mendapatkan cinta dan dukungan dari orang lain dapat menghadirkan kita daya dan tekad untuk terus berjuang melalui kesulitan.
jp188
Ashley JKT48: Bintang yang Bersinar Gemilang di Dunia Idola
Siapakah Ashley JKT48?
Siapa tokoh muda talenta yang mencuri perhatian banyak sekali penyuka musik di Nusantara dan Asia Tenggara? Itulah Ashley Courtney Shintia, atau yang terkenal dengan nama panggungnya, Ashley JKT48. Bergabung dengan grup idola JKT48 pada tahun 2018, Ashley dengan lekas berubah menjadi salah satu anggota paling terkenal.
Riwayat Hidup
Lahir di Jakarta pada tanggal 13 Maret 2000, Ashley berketurunan darah Tionghoa-Indonesia. Ia memulai karier di dunia entertainment sebagai model dan aktris, sebelum selanjutnya masuk dengan JKT48. Sifatnya yang periang, nyanyiannya yang mantap, dan keterampilan menari yang mengagumkan membentuknya sebagai idola yang sangat dikasihi.
Penghargaan dan Pengakuan
Kepopuleran Ashley telah diakui melalui berbagai penghargaan dan pencalonan. Pada masa 2021, ia memenangkan award “Anggota Paling Populer JKT48” di event JKT48 Music Awards. Beliau juga dianugerahi sebagai “Idol Tercantik se-Asia” oleh sebuah media online pada masa 2020.
Posisi dalam JKT48
Ashley memainkan posisi utama dalam grup JKT48. Dia adalah member Tim KIII dan berperan menjadi penari utama dan vokal utama. Ashley juga terlibat sebagai bagian dari subunit “J3K” dengan Jessica Veranda dan Jennifer Rachel Natasya.
Perjalanan Solo
Selain aktivitasnya bersama JKT48, Ashley juga merintis karier mandiri. Ia telah merilis beberapa lagu single, antara lain “Myself” (2021) dan “Falling Down” (2022). Ashley juga telah bekerja sama bareng musisi lain, seperti Afgan dan Rossa.
Kehidupan Pribadi
Selain dunia pertunjukan, Ashley dikenal sebagai pribadi yang rendah hati dan bersahabat. Ia menikmati menyisihkan jam bersama sanak famili dan teman-temannya. Ashley juga punya hobi mewarnai dan memotret.
Unduh Perangkat Lunak 888 dan Menangkan Kemenangan: Manual Pendek
**App 888 adalah pilihan unggulan untuk Para Pengguna yang menginginkan aktivitas bermain daring yang menggembirakan dan berjaya. Melalui hadiah sehari-hari dan opsi menarik, aplikasi ini menawarkan menawarkan aktivitas berjudi unggulan. Inilah manual cepat untuk mengoptimalkan pemanfaatan Program 888.
Pasang dan Awali Raih
Perangkat Ada:
Program 888 bisa diinstal di Android, Sistem iOS, dan Windows. Mulailah bertaruhan dengan cepat di media apapun.
Bonus Tiap Hari dan Hadiah
Hadiah Mendaftar Harian:
Masuk pada waktu untuk mendapatkan bonus mencapai 100K pada masa ketujuh.
Kerjakan Aktivitas:
Ambil opsi undian dengan mengerjakan tugas terkait. Satu misi menghadirkan Pengguna satu kesempatan undi untuk memenangkan bonus hingga 888K.
Penerimaan Manual:
Keuntungan harus dikumpulkan mandiri di melalui perangkat lunak. Yakinlah untuk mendapatkan imbalan tiap periode agar tidak batal.
Prosedur Lotere
Opsi Lotere:
Tiap hari, Pengguna bisa mengambil satu opsi pengeretan dengan merampungkan tugas.
Jika opsi undian habis, selesaikan lebih banyak misi untuk mengklaim extra opsi.
Ambang Bonus:
Dapatkan keuntungan jika jumlah pengeretan Para Pengguna melampaui 100K dalam waktu satu hari.
Ketentuan Penting
Penerimaan Hadiah:
Imbalan harus dikumpulkan manual dari aplikasi. Jika tidak, bonus akan otomatis diklaim ke akun Anda Kamu setelah sebuah masa.
Ketentuan Bertaruh:
Hadiah butuh setidaknya sebuah taruhan berlaku untuk digunakan.
Akhir
App 888 memberikan pengalaman main yang menggembirakan dengan keuntungan tinggi. Pasang program saat ini dan rasakan kemenangan tinggi setiap waktu!
Untuk detail lebih lanjut tentang promo, top up, dan skema referensi, kunjungi situs beranda program.
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Regards! Ample facts!
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
akartoto
Ashley JKT48: Bintang yang Bersinar Gemilang di Kancah Idol
Siapa Ashley JKT48?
Siapa sosok belia talenta yang menarik perhatian banyak penggemar lagu di Nusantara dan Asia Tenggara? Itulah Ashley Courtney Shintia, atau yang dikenal dengan nama panggungnya, Ashley JKT48. Bergabung dengan grup idola JKT48 pada masa 2018, Ashley dengan segera berubah menjadi salah satu anggota paling populer.
Riwayat Hidup
Lahir di Jakarta pada tanggal 13 Maret 2000, Ashley memiliki keturunan Tionghoa-Indonesia. Ia mengawali kariernya di dunia entertainment sebagai model dan pemeran, sebelum selanjutnya masuk dengan JKT48. Personanya yang ceria, vokal yang kuat, dan kemampuan menari yang mengesankan membentuknya sebagai idola yang sangat dicintai.
Award dan Apresiasi
Popularitas Ashley telah diakui melalui berbagai apresiasi dan nominasi. Pada masa 2021, beliau memenangkan pengakuan “Member Terpopuler JKT48” di ajang Penghargaan Musik JKT48. Beliau juga dinobatkan sebagai “Idol Tercantik di Asia” oleh sebuah majalah digital pada tahun 2020.
Posisi dalam JKT48
Ashley memainkan fungsi penting dalam group JKT48. Beliau adalah personel Tim KIII dan berperan sebagai dancer utama dan vokalis. Ashley juga menjadi bagian dari sub-unit “J3K” dengan Jessica Veranda dan Jennifer Rachel Natasya.
Karier Individu
Selain kegiatannya bersama JKT48, Ashley juga merintis perjalanan solo. Ia telah merilis beberapa lagu single, termasuk “Myself” (2021) dan “Falling Down” (2022). Ashley juga telah bekerja sama dengan artis lain, seperti Afgan dan Rossa.
Kehidupan Pribadi
Selain bidang panggung, Ashley dikenali sebagai pribadi yang low profile dan friendly. Ashley menikmati melewatkan masa bersama keluarga dan teman-temannya. Ashley juga menyukai kegemaran mewarnai dan memotret.
mega338
Download Aplikasi 888 dan Dapatkan Hadiah: Panduan Pendek
**Perangkat Lunak 888 adalah kesempatan ideal untuk Kamu yang mencari aktivitas berjudi online yang menggembirakan dan berjaya. Bersama hadiah tiap hari dan fasilitas menggoda, program ini menawarkan menawarkan keseruan bertaruhan optimal. Ini manual cepat untuk memaksimalkan pelayanan Aplikasi 888.
Instal dan Awali Menang
Layanan Tersedia:
App 888 dapat diinstal di Perangkat Android, Perangkat iOS, dan Komputer. Segera bertaruhan dengan mudah di gadget manapun.
Keuntungan Harian dan Imbalan
Hadiah Buka Harian:
Login tiap masa untuk mendapatkan keuntungan sebesar 100K pada periode ketujuh.
Kerjakan Pekerjaan:
Raih kesempatan undi dengan menuntaskan pekerjaan terkait. Setiap pekerjaan menyediakan Para Pengguna satu peluang undi untuk mendapatkan bonus sampai 888K.
Pengambilan Sendiri:
Keuntungan harus diambil manual di dalam aplikasi. Yakinlah untuk mendapatkan imbalan tiap waktu agar tidak batal.
Cara Undi
Kesempatan Undi:
Satu periode, Pengguna bisa mengambil 1 kesempatan pengeretan dengan mengerjakan tugas.
Jika peluang pengeretan selesai, selesaikan lebih banyak pekerjaan untuk mengambil extra kesempatan.
Batas Imbalan:
Dapatkan hadiah jika akumulasi undi Kamu melebihi 100K dalam waktu satu hari.
Kebijakan Esensial
Pengklaiman Hadiah:
Hadiah harus dikumpulkan mandiri dari perangkat lunak. Jika tidak, imbalan akan otomatis diserahkan ke akun pengguna Kamu setelah sebuah hari.
Ketentuan Pertaruhan:
Hadiah memerlukan setidaknya satu bertaruh berlaku untuk diambil.
Penutup
Perangkat Lunak 888 menghadirkan permainan berjudi yang menyenangkan dengan imbalan signifikan. Download program hari ini dan rasakan keberhasilan besar setiap waktu!
Untuk detail lebih lengkap tentang promo, simpanan, dan skema referensi, cek halaman utama aplikasi.
mpo1221
Inspirasi dari Ucapan Taylor Swift
Penyanyi Terkenal, seorang artis dan songwriter populer, tidak hanya terkenal karena nada yang elok dan suara yang nyaring, tetapi juga sebab syair-syair lagunya yang sarat makna. Di dalam syair-syairnya, Swift sering menyajikan berbagai faktor hidup, mulai dari cinta sampai dengan rintangan hidup. Berikut ini adalah sejumlah kutipan inspiratif dari karya-karya, beserta artinya.
“Mungkin yang paling baik belum tiba.” – “All Too Well”
Arti: Bahkan di masa-masa sulit, selalu ada secercah harapan dan kemungkinan untuk hari yang lebih baik.
Kutipan ini dari lagu “All Too Well” menyadarkan kita jika meskipun kita mungkin mengalami waktu sulit sekarang, senantiasa ada kemungkinan bahwa masa depan akan memberikan sesuatu yang lebih baik. Situasi ini adalah amanat pengharapan yang menguatkan, mendorong kita untuk tetap bertahan dan tidak mengalah, lantaran yang terbaik bisa jadi belum datang.
“Aku akan terus bertahan karena aku tidak bisa melakukan apapun tanpa kamu.” – “You Belong with Me”
Penjelasan: Menemukan cinta dan bantuan dari orang lain dapat menyediakan kita kekuatan dan kemauan keras untuk bertahan melalui rintangan.
Online gambling sites are increasingly more popular, delivering different promotions to draw new players. One of the most attractive offers is the no-deposit bonus, a offer that permits users to try their hand without any monetary commitment. This article looks into the merits of no deposit bonuses and underscores how they can improve their value.
What is a No Deposit Bonus?
A no deposit bonus is a type of casino incentive where participants are granted free money or free rounds without the need to submit any of their own funds. This lets gamblers to explore the casino, experiment with diverse gaming activities and potentially win real money, all without any initial expenditure.
Advantages of No Deposit Bonuses
Risk-Free Exploration
No upfront deposit bonuses offer a safe way to discover online casinos. Users can experiment with different gaming activities, learn the casino’s interface, and evaluate the overall user experience without spending their own capital. This is especially beneficial for newcomers who may not be used to online gambling sites.
Chance to Win Real Money
One of the most enticing features of no-deposit bonuses is the chance to earn real cash. Even though the amounts may be modest, any gains earned from the bonus can typically be collected after meeting the casino’s wagering requirements. This introduces an element of anticipation and gives a possible financial reward without any initial expenditure.
Learning Opportunity
No-deposit bonuses provide a excellent chance to get to know how different casino games are played. Players can try strategies, understand the mechanics of the games, and develop into more confident without worrying about risking their own cash. This can be significantly beneficial for difficult casino games like poker.
Conclusion
Free bonuses offer numerous merits for players, such as cost-free investigation, the potential to win real money, and beneficial educational opportunities. As the field continues to expand, the popularity of no-deposit bonuses is anticipated to rise.
free poker
Complimentary poker offers users a unique opportunity to enjoy the game without any monetary cost. This overview explores the benefits of participating in free poker and underscores why it continues to be in demand among numerous gamblers.
Risk-Free Entertainment
One of the key upsides of free poker is that it lets participants to partake in the joy of poker without being concerned with losing capital. This turns it perfect for novices who hope to familiarize themselves with the pastime without any monetary investment.
Skill Development
Complimentary poker gives a great opportunity for players to hone their skills. Participants can try methods, learn the guidelines of the pastime, and get self-assurance without any anxiety of parting with their own cash.
Social Interaction
Engaging in free poker can also foster networking opportunities. Online websites commonly offer discussion boards where gamblers can interact with each other, share methods, and occasionally form friendships.
Accessibility
Gratis poker is conveniently accessible to anyone with an network connection. This suggests that players can play the game from the comfort of their own house, at whenever they wish.
Conclusion
No-cost poker gives various advantages for gamblers. It is a risk-free means to partake in the activity, improve talent, participate in new friendships, and play poker easily. As further users discover the merits of free poker, its appeal is anticipated to rise.
poker game free
Discovering the World of Free Poker Games
Beginning
In the modern age, poker games have developed into broadly reachable recreation choices. For players desiring a complimentary means to experience poker, no-cost poker websites supply a thrilling adventure. This article explores the pros and factors for which no-cost poker has transformed into a preferred selection for countless gamers.
Perks of Complimentary Poker
Complimentary Fun
One of the extremely attractive characteristics of poker game free is that it supplies enthusiasts with no-cost amusement. There is no demand to use funds to engage in the game, turning it available to everyone.
Enhancing Abilities
Engaging in complimentary poker lets enthusiasts to hone their competence without a single fiscal hazard. It is a perfect opportunity for learners to learn the rules and tactics of poker games.
Community Interaction
Many complimentary poker applications provide opportunities for community engagement. Users can interact with other users, share techniques, and enjoy friendly tournaments.
Motives Behind the Popularity of No-Cost Poker
Accessibility
Free poker games are commonly attainable, enabling enthusiasts from different regions to engage in the activity.
No Economic Risk
With no-cost poker, there is no financial hazard, rendering it a safe alternative for users who wish to play this card game without investing cash.
Diverse Game Options
Complimentary poker platforms provide a broad array of activities, guaranteeing that users can continually find a card game that fits their choices.
Final Thoughts
Free poker games provides a entertaining and attainable approach for gamers to experience poker games. With no fiscal risk, possibilities for improving skills, and diverse game choices, it is understandable that numerous users like no-cost poker as their chosen playing option.
빠릿한 환충 서비스와 메이저업체의 안전
베팅사이트 이용 시 매우 중요한 요소 중 하나는 신속한 입출금 처리입니다. 일반적으로 삼 분 안에 충전, 십 분 이내에 환충이 완료되어야 합니다. 주요 대형업체들은 필요한 인력 고용을 통해 이와 같은 빠릿한 입출금 절차를 보장하며, 이를 통해 회원들에게 안전한 느낌을 드립니다. 메이저사이트를 이용하면서 신속한 경험을 해보시기 바랍니다. 저희는 여러분들이 보안성 있게 웹사이트를 접속할 수 있도록 돕는 먹튀해결사입니다.
보증금을 내고 배너 운영
먹튀 해결 전문가는 최대한 삼천만 원에서 일억 원의 보증 금액을 예치하고 있는 사이트들의 배너 광고를 운영 중입니다. 만일 먹튀 사고가 생길 경우, 베팅 규정에 어긋나지 않은 베팅 내역을 캡처하여 먹튀 해결 팀에 문의하시면, 확인 후 보증 자금으로 신속하게 피해 보전 처리해 드립니다. 피해가 발생하면 빠르게 캡처하여 피해 내용을 저장해 두시고 제출해 주세요.
장기간 안전 운영 업체 확인
먹튀해결사는 최대한 사 년 이상 먹튀 사고 없이 무사히 운영된 사이트들을 확인하여 배너 등록을 허용합니다. 이를 통해 누구나 알만한 메이저사이트를 안전하게 이용할 수 있는 기회를 제공합니다. 철저한 검증 절차를 통해 인증된 사이트를 놓치지 마시고, 안전한 베팅을 즐겨보세요.
투명성과 공정성을 가진 먹튀 검증
먹튀 해결 팀의 먹튀 검토는 투명성과 공평성을 바탕으로 합니다. 항상 고객들의 입장을 우선시하며, 기업의 이익이나 이익에 좌우되지 않고 한 건의 삭제 없이 사실만을 기반으로 검증해오고 있습니다. 먹튀 사고를 당하고 후회하지 않도록, 지금 바로 시작해보세요.
먹튀 검증 사이트 목록
먹튀 해결 전문가가 골라낸 안전한 베팅사이트 인증된 업체 목록 입니다. 지금 등록된 인증된 업체들은 먹튀 문제가 발생 시 100% 보장을 제공해드립니다. 다만, 제휴 기간이 끝난 업체에서 발생한 문제에 대해서는 책임지지 않습니다.
탁월한 먹튀 검증 알고리즘
먹튀 해결 팀은 깨끗한 베팅 문화를 조성하기 위해 늘 노력합니다. 저희가 권장하는 토토사이트에서 안전하게 베팅하시기 바랍니다. 고객님의 먹튀 신고는 먹튀 리스트에 등록되어 해당되는 베팅 사이트에 중대한 영향을 미칩니다. 먹튀 리스트 작성 시 먹튀블러드 만의 검토 경험을 최대한 활용하여 공정한 심사를 하도록 약속드립니다.
안전한 베팅 환경을 만들기 위해 계속해서 노력하는 먹튀해결사와 같이 안심하고 경험해보세요.
casino online
Examining the Universe of Casino Online
Beginning
Currently, internet casinos have altered the manner people engage in betting. With sophisticated tech, players can play their favorite gaming options right from the coziness of their houses. This article examines the perks of casino online and why they are attracting interest.
Pros of Internet Casinos
Comfort
One of the primary benefits of online casinos is accessibility. Enthusiasts can engage in gaming whenever and anywhere they wish, ending the necessity to commute to a physical gambling venue.
Large Game Library
Casino online offer a vast selection of casino games, spanning from vintage slot machines and casino classics to interactive games and modern video slots games. This diversity guarantees that there is an option for everyone.
Rewards and Incentives
One of the key appealing aspects of virtual casinos is the variety of bonuses and specials provided to players. These can encompass welcome bonuses, bonus spins, cashback incentives, and loyalty programs.
Safety and Security
Well-known online casinos guarantee user safety and protection with advanced data protection technologies. This safeguards private details and payment operations.
Why Virtual Casinos are Favored
Reachability
Internet casinos are extensively accessible, facilitating enthusiasts from diverse backgrounds to enjoy gaming.
Analyzing Contest Gambling Platforms: An Engaging and Convenient Playing Option
Overview
Lottery betting sites are emerging as a popular option for gamers looking for an captivating and legitimate approach to experience digital gambling. Unlike classic internet-based gaming hubs, contest casinos operate under separate lawful models, facilitating them to deliver competitions and awards without adhering to the same rules. This exposition analyzes the principle of contest gaming hubs, their merits, and why they are attracting a growing number of users.
What is a Sweepstakes Casino?
A lottery casino operates by supplying users with online funds, which can be utilized to engage in games. Gamers can achieve extra digital money or tangible prizes, like cash. The primary disparity from standard gambling platforms is that players do not get currency straightforwardly but acquire it through advertising campaigns, like purchasing a product or engaging in a no-cost participation sweepstakes. This structure permits sweepstakes betting sites to function lawfully in many jurisdictions where classic virtual wagering is controlled.
Unveiling Complimentary Casino Games
Beginning
In the digital age, free casino games have turned into a preferred selection for players who wish to play casino activities without shelling out cash. This article examines the advantages of free-of-charge casino games and the reasons they are gaining attention.
Benefits of Free Casino Games
Risk-Free Gaming
One of the primary perks of free-of-charge casino games is the possibility to play devoid of financial strain. Enthusiasts can engage in their preferred betting activities devoid of concerns about parting with money.
Skill Development
Free-of-charge casino games supply an fantastic environment for gamblers to refine their gaming proficiency. Be it understanding strategies in blackjack, gamblers can rehearse devoid of monetary repercussions.
Large Game Library
Free-of-charge casino games provide a wide range of casino games, such options as classic slot games, casino classics, and real-time games. This array guarantees that there is an option for every player.
Why Free-of-Charge Casino Games are Favored
Availability
Free casino games are widely available, facilitating enthusiasts from numerous walks of life to play betting.
Zero Financial Risk
Unlike cash-based betting, free casino games do not demand a financial outlay. This enables players to engage in gaming minus fretting over losing funds.
Sample Before Spending
Free casino games supply users the ability to sample gaming options ahead of investing real cash. This aids players form well-thought-out judgments.
Ending
Free-of-charge casino games offers a enjoyable and secure means to enjoy gaming. With no financial commitment, a wide variety of games, and opportunities for skill enhancement, it is clear that numerous enthusiasts choose no-cost casino games for their betting needs.
real money slots
Exploring Money Slots
Overview
Cash slots have evolved into a favored selection for gamblers wanting the rush of winning real funds. This piece delves into the benefits of gambling slots and the reasons they are drawing a growing number of users.
Advantages of Cash Slots
Actual Payouts
The major attraction of real money slots is the opportunity to gain tangible funds. In contrast to no-cost slots, real money slots supply players the thrill of prospective financial rewards.
Extensive Game Variety
Cash slots supply a wide array of types, characteristics, and payout structures. This assures that there is an activity for every kind of gambler, including vintage three-reel classic slots to up-to-date digital slots with multiple paylines and extra rounds.
Thrilling Incentives
Numerous digital casinos give enticing promotions for money slot users. These can consist of joining bonuses, complimentary spins, rebate offers, and loyalty programs. Such incentives enhance the overall gaming journey and supply more opportunities to win cash.
Reasons Gamblers Prefer Cash Slots
The Adrenaline of Gaining Genuine Funds
Money slots offer an adrenaline-filled experience, as players anticipate the possibility of earning actual cash. This aspect imparts a further dimension of anticipation to the playing activity.
Prompt Payouts
Gambling slots offer users the pleasure of quick payments. Gaining money instantly enhances the gaming adventure, making it more fulfilling.
Diverse Game Options
With real money slots, gamblers can play a extensive array of games, guaranteeing that there is constantly an activity exciting to play.
Final Thoughts
Real money slots gives a exciting and satisfying playing adventure. With the potential to gain actual funds, a diverse range of slots, and exciting bonuses, it’s clear that countless players like real money slots for their playing choices.
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
에그벳 계열
Dowager 황후의 생일을 축하하기 전에 Longquan Temple에 가고 싶습니까?
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
битц казино
bitz casino регистрация
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
geinoutime.com
이것을 생각한 Fang Dongliang은 아무 말도 할 수 없었고 그의 표정은 약간 우울했습니다.
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
play slots for real money
Within the present-day virtual time, the domain of wagering gaming has undergone a significant transformation, with internet-based wagering platforms becoming the latest sphere of pleasure and anticipation.
Included among the most spellbinding features as part of this energetic domain are the ever-popular internet-based slot offerings, encouraging players to commence a journey of enthralling interactivity and the prospect to win actual currency.
Online slots have transformed into a embodiment of excitement and eagerness for customers across the globe, granting an unparalleled extent of convenience and accessibility.
By means of simply a multiple taps, you can captivate yourself in a brilliant selection of gaming motifs, all carefully designed to stimulate your experiences and sustain your suspense of your seat.
A primary the main attractions of participating in slots for tangible prizes on digital platforms is the prospect to experience the anticipation of potentially life-changing winnings. The excitement of witnessing the symbols revolve, the symbols combine, and the grand prize tempt can be genuinely electrifying.
Virtual gambling platforms have effortlessly embedded innovative solutions to deliver a leisure interaction that is simultaneously visually enthralling and advantageous.
Aside from the attraction of conceivable prizes, virtual slot games as well present a degree of adaptability and authority that is unprecedented in the standard gambling scenario. You can fine-tune your wagers to match your financial resources, refining your gameplay to discover the perfect fit that aligns with your unique tastes and risk tolerance. This amount of optimization empowers participants to grow their virtual accounts and optimize their satisfaction, completely from the simplicity of their personal residences.
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
стоимость такси в новочеркасске вызов такси
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Pro88
Point nicely taken.!|
гарантированно,
Индивидуальный подход к каждому пациенту, для вашего уверенного улыбки,
Специализированная помощь по доступным ценам, для вашего удобства,
Комфортные условия и дружественный персонал, для вашего комфорта и уверенности,
Инновационные методы стоматологии, для вашего комфорта и уверенности,
Профессиональная гигиена полости рта, для вашего долгосрочного удовлетворения,
Современное лечение заболеваний полости рта, для вашей уверенной улыбки
стоматологія дитяча стоматологія дитяча .
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
SEO стратегия
Советы по сео стратегии продвижению.
Информация о том как управлять с низкочастотными запросами и как их определять
Тактика по деятельности в соперничающей нише.
Имею постоянных клиентов сотрудничаю с тремя организациями, есть что сообщить.
Посмотрите мой профиль, на 31 мая 2024г
количество завершённых задач 2181 только на этом сайте.
Консультация проходит в устной форме, никаких скринов и документов.
Продолжительность консультации указано 2 часа, и реально всегда на контакте без строгой привязки ко времени.
Как работать с ПО это уже иначе история, консультация по работе с программами оговариваем отдельно в другом услуге, узнаем что нужно при разговоре.
Всё спокойно на расслабленно не спеша
To get started, the seller needs:
Мне нужны данные от Telegram чата для коммуникации.
коммуникация только устно, вести переписку недостаточно времени.
Сб и Вс выходные
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
купить диплом колледжа https://6landik-diploms.com
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Euro
슬롯 나라 무료
Hongzhi 황제는 “당신도 오고 싶어합니다. “라고 침착하게 말했습니다.
такси поддержка телефон https://zakaz-taxionline.ru/
Получите диплом быстро и недорого
Автор24 сайт автор 24 .
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
эффективно,
Современное оборудование и материалы, для вашего уверенного улыбки,
Современные методы стоматологии, для вашей улыбки,
Бесплатная консультация и диагностика, для вашей радости и улыбки,
Инновационные методы стоматологии, для вашего здоровья и красоты улыбки,
Экстренная помощь в любое время суток, для вашего здоровья и уверенности в себе,
Современное лечение заболеваний полости рта, для вашего здоровья и благополучия
івано франківськ стоматологія івано франківськ стоматологія .
Euro 2024
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Ищете способ расслабиться и получить незабываемые впечатления? Мы https://t.me/intim_tmn72 предлагаем эксклюзивные встречи с привлекательными и профессиональными компаньонками. Конфиденциальность, комфорт и безопасность гарантированы. Позвольте себе наслаждение и отдых в приятной компании.
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Dental Health Supplement provadenta.com
geinoutime.com
Qi Jingtong은 너무 흥분해서 눈물을 흘리고 싶었습니다.
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
https://tennissherbrooke.ca/qqpulsa365
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
vardenafil buy uk
vòng loại euro 2024
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
마종 웨이즈 2
“이때 폭우가 내리면 폐하가 어떻게 될지 생각해 본 적이 있습니까?”
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
мягкая мебель купить
https://formomebel.ru/stoliki/na-osnovanii-iz-metalla
смотреть бесплатно атака титанов https://ataka-titanov-anime.ru
Выбирайте коляску Cybex для комфорта вашего ребенка, для вашего выбора.
Лучшие оферты на коляски Cybex, для самых взыскательных.
Почему стоит обратить внимание на коляски Cybex, которые заставят вас влюбиться в этот бренд.
Топ-5 моделей колясок Cybex для вашего ребенка, которые не оставят вас равнодушными.
Как выбрать идеальную коляску Cybex для вашей семьи, учитывая все особенности и пожелания.
Советы по выбору коляски Cybex для вашего малыша, исходя из индивидуальных потребностей и предпочтений.
Коляска Cybex: высокое качество и стильный дизайн, которые ценят комфорт и безопасность.
Идеальная коляска Cybex для вашего малыша: как выбрать, которые порадуют вас своим разнообразием и качеством.
5 важных критериев при выборе коляски Cybex, для вашего малыша.
Какая коляска Cybex лучше всего подойдет вашей семье?, чтобы сделать правильный выбор.
Коляска Cybex: стиль, комфорт и безопасность, которые не оставят вас равнодушными.
5 важных критериев при выборе коляски Cybex, которые порадуют вас своим качеством и функционалом.
Идеальная коляска Cybex: комфорт и удобство для вашего малыша, которые стоит рассмотреть перед покупкой.
Топ-5 колясок Cybex для вашей семьи, если вы цените качество и комфорт.
Лучшие модели колясок Cybex: подробный обзор, которые ценят надежность и стиль.
Топ-модели колясок Cybex для вашей семьи, перед совершением покупки.
Как выбрать идеальную коляску Cybex для вашей семьи, исходя из личных предпочтений и потребностей.
Особенности выбора коляски Cybex: как сделать правильный выбор, которые не оставят вас равнодушными.
коляска прогулочная cybex коляска прогулочная cybex .
娛樂城官網
娛樂城官網
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
сериал
This information is priceless. When can I find out more?
arusak-attestats24.com
Hi there, You’ve done a great job. I’ll certainly digg it and personally recommend to my friends. I am confident they’ll be benefited from this site.
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
A cada acesso a este site, sinto-me imediatamente envolvido por uma atmosfera de confiança. Parabéns pela dedicação à segurança dos usuários!
голяк смотреть онлайн https://golyak-serial-online.ru
Incredible many of very good info.|
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Доброго!
Недавно у меня возникла потребность в получении среднего образования, но постоянная работа и обязанности постоянно отнимают время, и у меня нет возможности этим заниматься. К моему счастью, друзья посоветовали мне, что можно легально приобрести диплом о среднем профессиональном образовании (диплом техникума, колледжа) на бланках государственного образца, пройдя обучение по упрощенной программе!
В интернете полно предложений, но как избежать мошенничества и выбрать подходящую компанию? Это весьма важный вопрос, который требует ответственного подхода. Я лично проверил, что на https://russa24-diploms-srednee.com содержится множество советов о том, как избежать ошибок и не потерять деньги зря. Как проверить компанию по продаже дипломов, на что обратить внимание, и конечно, там можно заказать диплом “под ключ” без предварительной оплаты.
В отличие от других коммерческих организаций, наша цель — не просто заработать, а помочь нашим клиентам. Мы предоставляем бесплатные консультации без ограничений по количеству вопросов. Наши специалисты — проверенные временем профессионалы, поэтому обращение к нам – верное решение, ведь мы гарантируем качество, соблюдение сроков и разумные цены на дипломы о среднем образовании на заказ.
Удачи и хороших оценок!
купить дипломы о среднем образовании в перми
диплом об среднем образовании купить
я купила диплом о среднем специальном образовании отзывы
купить бланки дипломов о среднем профессиональном образовании
купить диплом о среднем образовании повара
диплом среднего медицинского образования купить
купить диплом о среднем образовании киров
дипломы среднего профессионального образования купить волгоград
диплом о среднем мед образовании купить
диплом среднем образовании купить
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Slotเว็บตรง – สนุกกับการเล่นได้ทุกเครื่องมือที่ใช้งานอินเทอร์เน็ต
ในยุคปัจจุบัน การเล่นเกมสล็อตมีความง่ายดายมากยิ่งขึ้น คุณไม่จำเป็นต้องเดินทางไปยังสถานที่เล่นคาสิโนที่ไหน ๆ เพียงแค่มีเครื่องมือที่ใช้งานได้เชื่อมต่อกับอินเทอร์เน็ต คุณก็สามารถสนุกกับการหมุนสล็อตออนไลน์กับ PG Slot ได้จากทุกที่
การพัฒนาเทคโนโลยีของ PG Slot
ที่ PG Slot เราได้นำเสนอโซลูชั่นสำหรับการบริการเกมคาสิโนออนไลน์เพื่อตอบสนองความต้องการให้มากที่สุด คุณไม่ต้องติดตั้งซอฟต์แวร์หรือโหลดแอปพลิเคชันใด ๆ ให้ซับซ้อนหรือเปลืองพื้นที่ในอุปกรณ์อิเล็กทรอนิกส์ของคุณ การดูแลเกมสล็อตออนไลน์ของเราดำเนินการผ่านเว็บตรงที่ใช้เทคโนโลยี HTML 5 ที่ทันยุค
เล่นสล็อตได้ทุกอุปกรณ์
คุณอาจเล่นสล็อตออนไลน์กับ PG Slot ได้อย่างสะดวกง่ายดายเพียงเข้าสู่ในเว็บไซต์ของเรา เว็บตรงสล็อตออนไลน์ของเรารองรับทุกโครงสร้างและอุปกรณ์ทุกรุ่นทั้ง Android และ iOS ไม่ว่าคุณจะใช้โทรศัพท์มือถือ โน้ตบุ๊ก หรืออุปกรณ์มือถือรุ่นไหน ก็สามารถมั่นใจได้ว่าคุณจะเล่นสล็อตออนไลน์ได้อย่างไม่ติดขัด ไม่มีอุปสรรคหรือสะดุดใด ๆ
เล่นสล็อตฟรี
เว็บตรงของเราให้คุณใช้บริการเพียงแค่คุณเข้ามาในเว็บไซต์ของ PG Slot ก็อาจทดลองเล่นสล็อตฟรีได้ทันที ไม่ต้องเสียค่าใช้จ่ายใด ๆ นี่เป็นโอกาสที่ดีในการเรียนรู้และศึกษาเกมเกี่ยวกับเกมก่อนที่จะเล่นจริงด้วยเงินจริง
การเล่นเกมสล็อตออนไลน์กับ PG Slot ช่วยให้คุณสามารถเพลิดเพลินกับการเล่นเกมคาสิโนได้ทุกที่ทุกเวลา ไม่ว่าคุณจะอยู่ที่ไหน เพียงแค่มีเครื่องมือที่ต่ออินเทอร์เน็ต คุณก็สามารถสนุกกับการเล่นเกมสล็อตได้อย่างไม่มีขีดจำกัด!
mamibet
Hey I know this is off topic but I was wondering if you knew of any widgets I could add to my blog that automatically tweet my newest twitter updates. I’ve been looking for a plug-in like this for quite some time and was hoping maybe you would have some experience with something like this. Please let me know if you run into anything. I truly enjoy reading your blog and I look forward to your new updates.
arusak-attestats24.com
Hey I know this is off topic but I was wondering if you knew of any widgets I could add to my blog that automatically tweet my newest twitter updates. I’ve been looking for a plug-in like this for quite some time and was hoping maybe you would have some experience with something like this. Please let me know if you run into anything. I truly enjoy reading your blog and I look forward to your new updates.
Самые популярные коляски Tutis, выбор мамочек в-the-know, рекомендации по покупке, Секреты долговечности и надежности коляски Tutis, правила использования коляски, Tutis: идеальный выбор для активных семей, Сравнение Tutis с другими брендами колясок, Инструкция по уходу за коляской Tutis, для продления срока службы, Секреты комфортной поездки с Tutis, Почему Tutis подойдет и летом, и зимой, Почему Tutis лучше всего подходит для вашей семьи?, подгонка под ваш образ жизни, секреты качественного производства, советы врачей, Почему Tutis – выбор сознательных семей, поддержка родителей в заботе о ребенке
коляска 3 в 1 тутис https://kolyaskatutis.ru/ .
latoto
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
富遊娛樂城評價:2024年最新評價
推薦指數 : ★★★★★ ( 5.0/5 )
富遊娛樂城作為目前最受歡迎的博弈網站之一,在台灣擁有最高的註冊人數。
RG富遊以安全、公正、真實和順暢的品牌保證,贏得了廣大玩家的信賴。富遊線上賭場不僅提供了豐富多樣的遊戲種類,還有眾多吸引人的優惠活動。在出金速度方面,獲得無數網紅和網友的高度評價,確保玩家能享有無憂的博弈體驗。
推薦要點
新手首選: 富遊娛樂城,2024年評選首選,提供專為新手打造的豐富教學和獨家優惠。
一存雙收: 首存1000元,立獲1000元獎金,僅需1倍流水,新手友好。
免費體驗: 新玩家享免費體驗金,暢遊各式遊戲,開啟無限可能。
優惠多元: 活動豐富,流水要求低,適合各類型玩家。
玩家首選: 遊戲多樣,服務優質,是新手與老手的最佳賭場選擇。
富遊娛樂城詳情資訊
賭場名稱 : RG富遊
創立時間 : 2019年
賭場類型 : 現金版娛樂城
博弈執照 : 馬爾他牌照(MGA)認證、英屬維爾京群島(BVI)認證、菲律賓(PAGCOR)監督競猜牌照
遊戲類型 : 真人百家樂、運彩投注、電子老虎機、彩票遊戲、棋牌遊戲、捕魚機遊戲
存取速度 : 存款5秒 / 提款3-5分
軟體下載 : 支援APP,IOS、安卓(Android)
線上客服 : 需透過官方LINE
富遊娛樂城優缺點
優點
台灣註冊人數NO.1線上賭場
首儲1000贈1000只需一倍流水
擁有體驗金免費體驗賭場
網紅部落客推薦保證出金線上娛樂城
缺點
需透過客服申請體驗金
富遊娛樂城存取款方式
存款方式
提供四大超商(全家、7-11、萊爾富、ok超商)
虛擬貨幣ustd存款
銀行轉帳(各大銀行皆可)
取款方式
網站內申請提款及可匯款至綁定帳戶
現金1:1出金
富遊娛樂城平台系統
真人百家 — RG真人、DG真人、歐博真人、DB真人(原亞博/PM)、SA真人、OG真人、WM真人
體育投注 — SUPER體育、鑫寶體育、熊貓體育(原亞博/PM)
彩票遊戲 — 富遊彩票、WIN 539
電子遊戲 —RG電子、ZG電子、BNG電子、BWIN電子、RSG電子、GR電子(好路)
棋牌遊戲 —ZG棋牌、亞博棋牌、好路棋牌、博亞棋牌
電競遊戲 — 熊貓體育
捕魚遊戲 —ZG捕魚、RSG捕魚、好路GR捕魚、DB捕魚
에그벳 주소
시간이 지남에 따라 Chen Zheng은 극도로 불안감을 느꼈습니다.
Здравствуйте!
Недавно у меня возникла потребность в получении среднего образования, но моя постоянная работа и обязанности постоянно отнимают время, не оставляя возможности этим заниматься. К счастью, друзья подсказали мне, что можно легально приобрести диплом о среднем профессиональном образовании (диплом техникума, колледжа) на бланках государственного образца, пройдя обучение по упрощенной программе!
В интернете предложений более чем достаточно, но как не стать жертвой мошенников и выбрать подходящую компанию? Этот вопрос требует особой внимательности и ответственности. Лично я проверил, что на https://russa24-diploms-srednee.com есть много полезной информации о том, как избежать ошибок и не потерять свои деньги. Как можно проверить компанию по продаже дипломов, на что обратить внимание, и, конечно же, там можно заказать диплом “под ключ” без предварительной оплаты.
В отличие от других коммерческих организаций, наша цель не сводится к заработку – мы работаем на благо наших клиентов. Мы предоставляем бесплатные консультации без ограничений по количеству вопросов. Наши специалисты – проверенные временем профессионалы, поэтому обращение к нам – правильное решение, ведь мы гарантируем качество, соблюдение сроков и разумные цены на дипломы о среднем образовании на заказ.
Удачи и хороших оценок!
купить диплом о среднем образовании москва
купить диплом о полном среднем образовании
купить диплом среднего мед образования
купить дипломы о среднем образовании в омске
купить диплом о среднем специальном образовании с занесением в базу
диплом купил о среднем образовании
дипломы среднем образовании купить
купить диплом о среднем специальном образовании в москве
сколько стоит купить диплом о среднем специальном образовании
где купить дипломы о среднем техническом образовании
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Преимущества строительства дома из бруса 9х12 | Подбор проекта для дома из бруса 9х12 | Как создать уютный интерьер в доме из бруса 9х12 | Интерьер для дома из бруса 9х12: советы дизайнера | Выбор фундамента для дома из бруса 9х12 | Фундамент для дома из бруса 9х12: какой выбрать? | Новинки в строительстве домов из бруса 9х12 | Как выбрать мебель для дома из бруса 9х12 | Для комфортного отдыха: зона lounge в доме из бруса 9х12 | Расходы на строительство дома из бруса 9х12
дом брус 9х12 https://domizbrusa-9x12spb.ru/ .
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
娛樂城
Player台灣線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
layer如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
安全與公平性
安全永遠是我們評測的首要標準。我們審查每家娛樂城的執照資訊、監管機構以及使用的隨機數生成器,以確保其遊戲結果的公平性和隨機性。
02.
遊戲品質與多樣性
遊戲的品質和多樣性對於玩家體驗至關重要。我們評估遊戲的圖形、音效、用戶介面和創新性。同時,我們也考量娛樂城提供的遊戲種類,包括老虎機、桌遊、即時遊戲等。
03.
娛樂城優惠與促銷活動
我們仔細審視各種獎勵計劃和促銷活動,包括歡迎獎勵、免費旋轉和忠誠計劃。重要的是,我們也檢查這些優惠的賭注要求和條款條件,以確保它們公平且實用。
04.
客戶支持
優質的客戶支持是娛樂城質量的重要指標。我們評估支持團隊的可用性、響應速度和專業程度。一個好的娛樂城應該提供多種聯繫方式,包括即時聊天、電子郵件和電話支持。
05.
銀行與支付選項
我們檢查娛樂城提供的存款和提款選項,以及相關的處理時間和手續費。多樣化且安全的支付方式對於玩家來說非常重要。
06.
網站易用性、娛樂城APP體驗
一個直觀且易於導航的網站可以顯著提升玩家體驗。我們評估網站的設計、可訪問性和移動兼容性。
07.
玩家評價與反饋
我們考慮真實玩家的評價和反饋。這些資料幫助我們了解娛樂城在實際玩家中的表現。
娛樂城常見問題
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
在现代,在线赌场提供了多种便捷的存款和取款方式。对于较大金额的存款,您可以选择中国信托、台中银行、合作金库、台新银行、国泰银行或中华邮政。这些银行提供的服务覆盖金额范围从$1000到$10万,确保您的资金可以安全高效地转入赌场账户。
如果您需要进行较小金额的存款,可以选择通过便利店充值。7-11、全家、莱尔富和OK超商都提供这种服务,适用于金额范围在$1000到$2万之间的充值。通过这些便利店,您可以轻松快捷地完成资金转账,无需担心银行的营业时间或复杂的操作流程。
在进行娱乐场提款时,您可以选择通过各大银行转账或ATM转账。这些方法不仅安全可靠,而且非常方便,适合各种提款需求。最低提款金额为$1000,而上限则没有限制,确保您可以灵活地管理您的资金。
在选择在线赌场时,玩家评价和推荐也是非常重要的。许多IG网红和部落客,如丽莎、穎柔、猫少女日记-Kitty等,都对一些知名的娱乐场给予了高度评价。这些推荐不仅帮助您找到可靠的娱乐场所,还能确保您在游戏中享受到最佳的用户体验。
总体来说,在线赌场通过提供多样化的存款和取款方式,以及得到广泛认可的服务质量,正在不断吸引更多的玩家。无论您选择通过银行还是便利店进行充值,都能体验到快速便捷的操作。同时,通过查看玩家的真实评价和推荐,您也能更有信心地选择合适的娱乐场,享受安全、公正的游戏环境。
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Ищете анонимности в своих транзакциях Ethereum? Посмотрите на TornadoCash, ведущее решение для пользователей, беспокоящихся о конфиденциальности.
esse4d
2024娛樂城推薦,經過玩家實測結果出爐Top5!
2024娛樂城排名是這五間上榜,玩家尋找娛樂城無非就是要找穩定出金娛樂城,遊戲體驗良好、速度流暢,Ace博評網都幫你整理好了,給予娛樂城新手最佳的指南,不再擔心被黑網娛樂城詐騙!
2024娛樂城簡述
在現代,2024娛樂城數量已經超越以前,面對琳瑯滿目的娛樂城品牌,身為新手的玩家肯定難以辨別哪間好、哪間壞。
好的平台提供穩定的速度與遊戲體驗,穩定的系統與資訊安全可以保障用戶的隱私與資料,不用擔心收到傳票與任何網路威脅,這些線上賭場也提供合理的優惠活動給予玩家。
壞的娛樂城除了會騙取你的金錢之外,也會打著不實的廣告、優惠滿滿,想領卻是一場空!甚至有些平台還沒辦法登入,入口網站也是架設用來騙取新手儲值進他們口袋,這些黑網娛樂城是玩家必須避開的風險!
評測2024娛樂城的標準
Ace這次從網路上找來五位使用過娛樂城資歷2年以上的老玩家,給予他們使用各大娛樂城平台,最終選出Top5,而評選標準為下列這些條件:
以玩家觀點出發,優先考量玩家利益
豐富的遊戲種類與卓越的遊戲體驗
平台的信譽及其安全性措施
客服團隊的回應速度與服務品質
簡便的儲值流程和多樣的存款方法
吸引人的優惠活動方案
前五名娛樂城表格
賭博網站排名 線上賭場 平台特色 玩家實測評價
No.1 富遊娛樂城 遊戲選擇豐富,老玩家優惠多 正面好評
No.2 bet365娛樂城 知名大廠牌,運彩盤口選擇多 介面流暢
No.3 亞博娛樂城 多語言支持,介面簡潔順暢 賽事豐富
No.4 PM娛樂城 撲克牌遊戲豐富,選擇多元 直播順暢
No.5 1xbet娛樂城 直播流暢,安全可靠 佳評如潮
線上娛樂城玩家遊戲體驗評價分享
網友A:娛樂城平台百百款,富遊娛樂城是我3年以來長期使用的娛樂城,別人有的系統他們都有,出金也沒有被卡過,比起那些玩娛樂城還會收到傳票的娛樂城,富遊真的很穩定,值得推薦。
網友B:bet365中文的介面簡約,還有超多體育賽事盤口可以選擇,此外賽事大部分也都有附上直播來源,不必擔心看不到賽事最新狀況,全螢幕還能夠下單,真的超方便!
網友C:富遊娛樂城除了第一次儲值有優惠之外,儲值到一定金額還有好禮五選一,實用又方便,有問題的時候也有客服隨時能夠解答。
網友D:從大陸來台灣工作,沒想到台灣也能玩到亞博體育,這是以前在大陸就有使用的平台,雖然不是簡體字,但使用介面完全沒問題,遊戲流暢、速度比以前使用還更快速。
網友E:看玖壹壹MV發現了PM娛樂城這個大品牌,PM的真人百家樂沒有輸給在澳門實地賭場,甚至根本不用出門,超級方便的啦!
naga138
Greetings I am so glad I found your blog page, I really found you by accident, while I was looking on Askjeeve for something else, Regardless I am here now and would just like to say many thanks for a remarkable post and a all round interesting blog (I also love the theme/design), I don’t have time to go through it all at the minute but I have book-marked it and also added your RSS feeds, so when I have time I will be back to read a great deal more, Please do keep up the superb work.
http://www.musey-uglich.ru
What a material of un-ambiguity and preserveness of precious experience concerning unexpected emotions.
регистрация новое ректро казино
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
играть в автомат gates of olympus https://gates-of-olympus-ru.ru/ .
Привет учащиеся!
Всегда думал что купить диплом о высшем образовании это миф и нереально, но все оказалось не так, изначально искал информацию про: купить диплом охранника в спб, купить диплом колледжа в казани, купить диплом о средне специальном образовании в москве, сколько стоит купить диплом о среднем образовании, купить диплом ветеринарного врача, потом про дипломы вузов, подробнее здесь http://www.arusak-diploms-srednee.ru
Оказалось все возможно, официально со специальными условия по упрощенным программам, так и сделал и теперь у меня есть диплом вуза Москвы нового образца, что советую и вам!
Удачи и хороших оценок!
купить диплом о среднем образовании 11 классов
купить дипломы об окончании техникума
купить диплом 1993
купить диплом бакалавра в москве москва
купить аттестат с занесением в реестр
где купить диплом повара
купить диплом медицинского колледжа
купить диплом о среднем специальном образовании с занесением в реестр
купить дубликат диплома
купить диплом в краснодаре
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good post. I learn something totally new and challenging on websites I stumbleupon every day. It will always be interesting to read through content from other authors and practice a little something from their websites.
musey-uglich.ru
Здравствуйте!
Задумался а действительно можно купить диплом государственного образца в Москве, и был удивлен, все реально и главное официально!
Сначала серфил в сети и искал такие темы как: купить аттестат за классов, купить диплом в пскове, купить диплом в великих луках, купить диплом о среднем специальном, купить свидетельство о браке, получил базовую информацию.
Остановился в итоге на материале https://www.sitebs.ru/blogs/94542.html
Удачи и хороших оценок!
에그벳 스포츠
Wang Zuo는 얼굴에 미소를 지으며 “왜 제공이 오지 않았습니까?”
Портал о Ярославле – ваш гид по культурной жизни города. Здесь вы найдёте информацию о театрах, музеях, галереях и исторических достопримечательностях. Откройте для себя яркие события, фестивали и выставки, которые делают Ярославль культурной жемчужиной России.
娛樂城
2024娛樂城介紹
台灣2024娛樂城越開越多間,新開的線上賭場層出不窮,每間都以獨家的娛樂城優惠和體驗金來吸引玩家,致力於提供一流的賭博遊戲體驗。以下來介紹這幾間娛樂城網友對他們的真實評價,看看哪些娛樂城上榜了吧!
2024娛樂城排名
2023下半年,各家娛樂城競爭激烈,相繼推出誘人優惠,不論是娛樂城體驗金、反水流水還是首儲禮金,甚至還有娛樂城抽I15手機。以下就是2024年網友推薦的娛樂城排名:
NO.1 富遊娛樂城
NO.2 Bet365台灣
NO.3 DG娛樂城
NO.4 九州娛樂城
NO.5 亞博娛樂城
2024娛樂城推薦
根據2024娛樂城排名,以下將富遊娛樂城、BET365、亞博娛樂城、九州娛樂城、王者娛樂城推薦給大家,包含首儲贈點、免費體驗金、存提款速度、流水等等…
娛樂城遊戲種類
線上娛樂城憑藉其廣泛的遊戲種類,成功滿足了各式各樣玩家的喜好和需求。這些娛樂城遊戲不僅多元化且各具特色,能夠為玩家提供無與倫比的娛樂體驗。下面是一些最受歡迎的娛樂城遊戲類型:
電子老虎機
魔龍傳奇、雷神之鎚、戰神呂布、聚寶財神、鼠來寶、皇家777
真人百家樂
真人視訊百家樂、牛牛、龍虎、炸金花、骰寶、輪盤
電子棋牌
德州撲克、兩人麻將、21點、十三支、妞妞、三公、鬥地主、大老二、牌九
體育下注
世界盃足球賽、NBA、WBC世棒賽、英超、英雄聯盟LOL、特戰英豪
線上彩票
大樂透、539、美國天天樂、香港六合彩、北京賽車
捕魚機遊戲
三仙捕魚、福娃捕魚、招財貓釣魚、西遊降魔、吃我一砲、賓果捕魚
2024娛樂城常見問題
娛樂城是什麼?
娛樂城/線上賭場(現金網)是台灣對於線上賭場的特別稱呼,而且是現金網,大家也許會好奇為什麼不直接叫做線上賭場或是線上博弈就好了。
其實這是有原因的,線上賭場這種東西,架站在台灣是違法的,在早期經營線上博弈被抓的風險非常高所以換了一個打模糊仗的代稱「娛樂城」來規避警方的耳目,畢竟以前沒有Google這種東西,這樣的代稱還是多少有些作用的。
信用版娛樂城是什麼?
信用版娛樂城是一種賭博平台,允許玩家在沒有預先充值的情況下參與遊戲。這種模式類似於信用卡,通常以周結或月結的方式結算遊戲費用。因此,如果玩家無法有效管理自己的投注額,可能會在月底面臨巨大的支付壓力。
娛樂城不出金怎麼辦?
釐清原因,如未違反娛樂城機制,可能是遇上黑網娛樂城,請盡快通報165反詐騙。
В нашем обществе, где диплом становится началом отличной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения образования. Факт наличия официального документа трудно переоценить. Ведь именно он открывает двери перед всеми, кто желает вступить в профессиональное сообщество или продолжить обучение в каком-либо ВУЗе.
В данном контексте наша компания предлагает максимально быстро получить этот необходимый документ. Вы можете приобрести диплом, и это является отличным решением для человека, который не смог завершить образование или утратил документ. диплом изготавливается с особой аккуратностью, вниманием к мельчайшим деталям. На выходе вы получите 100% оригинальный документ.
Плюсы такого подхода состоят не только в том, что можно быстро получить диплом. Весь процесс организовывается комфортно, с нашей поддержкой. Начиная от выбора нужного образца до грамотного заполнения личной информации и доставки по России — все находится под абсолютным контролем качественных специалистов.
Для всех, кто пытается найти быстрый способ получения требуемого документа, наша услуга предлагает выгодное решение. Приобрести диплом – значит избежать продолжительного обучения и не теряя времени переходить к достижению собственных целей: к поступлению в университет или к началу трудовой карьеры.
http://www.seoyour.ru
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
В нашем обществе, где диплом становится началом отличной карьеры в любом направлении, многие стараются найти максимально быстрый путь получения образования. Наличие официального документа об образовании сложно переоценить. Ведь именно он открывает двери перед любым человеком, который желает вступить в сообщество профессиональных специалистов или продолжить обучение в университете.
Предлагаем быстро получить этот важный документ. Вы имеете возможность купить диплом нового или старого образца, что становится удачным решением для человека, который не смог закончить обучение или потерял документ. Все дипломы производятся аккуратно, с особым вниманием ко всем элементам, чтобы в итоге получился документ, полностью соответствующий оригиналу.
Преимущество данного подхода заключается не только в том, что можно максимально быстро получить диплом. Процесс организован просто и легко, с нашей поддержкой. Начав от выбора подходящего образца до консультаций по заполнению персональной информации и доставки по стране — все находится под полным контролем качественных мастеров.
Для тех, кто ищет быстрый и простой способ получения требуемого документа, наша компания предлагает выгодное решение. Купить диплом – это значит избежать продолжительного процесса обучения и сразу перейти к своим целям, будь то поступление в университет или старт удачной карьеры.
seoyour.ru
Player台灣線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
layer如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
安全與公平性
安全永遠是我們評測的首要標準。我們審查每家娛樂城的執照資訊、監管機構以及使用的隨機數生成器,以確保其遊戲結果的公平性和隨機性。
02.
遊戲品質與多樣性
遊戲的品質和多樣性對於玩家體驗至關重要。我們評估遊戲的圖形、音效、用戶介面和創新性。同時,我們也考量娛樂城提供的遊戲種類,包括老虎機、桌遊、即時遊戲等。
03.
娛樂城優惠與促銷活動
我們仔細審視各種獎勵計劃和促銷活動,包括歡迎獎勵、免費旋轉和忠誠計劃。重要的是,我們也檢查這些優惠的賭注要求和條款條件,以確保它們公平且實用。
04.
客戶支持
優質的客戶支持是娛樂城質量的重要指標。我們評估支持團隊的可用性、響應速度和專業程度。一個好的娛樂城應該提供多種聯繫方式,包括即時聊天、電子郵件和電話支持。
05.
銀行與支付選項
我們檢查娛樂城提供的存款和提款選項,以及相關的處理時間和手續費。多樣化且安全的支付方式對於玩家來說非常重要。
06.
網站易用性、娛樂城APP體驗
一個直觀且易於導航的網站可以顯著提升玩家體驗。我們評估網站的設計、可訪問性和移動兼容性。
07.
玩家評價與反饋
我們考慮真實玩家的評價和反饋。這些資料幫助我們了解娛樂城在實際玩家中的表現。
娛樂城常見問題
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
在现代,在线赌场提供了多种便捷的存款和取款方式。对于较大金额的存款,您可以选择中国信托、台中银行、合作金库、台新银行、国泰银行或中华邮政。这些银行提供的服务覆盖金额范围从$1000到$10万,确保您的资金可以安全高效地转入赌场账户。
如果您需要进行较小金额的存款,可以选择通过便利店充值。7-11、全家、莱尔富和OK超商都提供这种服务,适用于金额范围在$1000到$2万之间的充值。通过这些便利店,您可以轻松快捷地完成资金转账,无需担心银行的营业时间或复杂的操作流程。
在进行娱乐场提款时,您可以选择通过各大银行转账或ATM转账。这些方法不仅安全可靠,而且非常方便,适合各种提款需求。最低提款金额为$1000,而上限则没有限制,确保您可以灵活地管理您的资金。
在选择在线赌场时,玩家评价和推荐也是非常重要的。许多IG网红和部落客,如丽莎、穎柔、猫少女日记-Kitty等,都对一些知名的娱乐场给予了高度评价。这些推荐不仅帮助您找到可靠的娱乐场所,还能确保您在游戏中享受到最佳的用户体验。
总体来说,在线赌场通过提供多样化的存款和取款方式,以及得到广泛认可的服务质量,正在不断吸引更多的玩家。无论您选择通过银行还是便利店进行充值,都能体验到快速便捷的操作。同时,通过查看玩家的真实评价和推荐,您也能更有信心地选择合适的娱乐场,享受安全、公正的游戏环境。
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
сериал 2024
Здравствуйте!
Всегда считал, что покупка диплома о высшем образовании — это миф. Но, оказалось, что все возможно! Сначала искал информацию по теме: купить диплом в ишимбае, за сколько можно купить диплом, купить аттестат за 8 класс, купить диплом о повышении квалификации, диплом о среднем профессиональном образовании где купить, а затем перешел на дипломы вузов. Подробнее можно узнать здесь: http://arusak-diploms-srednee.ru
Оказалось, что все возможно и официально, с упрощенными программами обучения. Теперь у меня диплом московского вуза нового образца, и я рекомендую вам воспользоваться этим шансом!
Удачи и хороших оценок!
диплом об среднем образовании купить
купить диплом 2000
диплом купить алма ата
купить бланк диплома о высшем образовании
купить диплом старого образца ссср
можно ли купить диплом о среднем профессиональном образовании
купить диплом за 10 11 класс
где купить диплом окончание
купить диплом мфти
диплом какого вуза купить
https://likedquotes.com/?keyword=188bet
игровой автомат sweet bonanza https://sweet-bonanza-ru.ru .
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом во владимире, купить диплом в самаре, купить диплом в междуреченске, купить речной диплом, купить диплом менеджера по туризму и получил базовые знания. В итоге остановился на материале: http://mockwa.com/forum/thread-146281/
Удачи и хороших оценок!
https://kupit-kvartiruspb.ru в новостройках Санкт-Петербурга. Цены и фотографии квартир от застройщика в готовых и строящихся ЖК. Подбор жилья, ипотечные программы, сопровождение сделок и выгодные предложения.
продажа квартир цены https://kvartiru-kupit78.ru
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
아시아 슬롯
이것을 생각하면서 Wang Jinyuan은 심호흡을했습니다. 왜 Xishan은 어쨌든 고통받지 않았습니다.
заказать поисковый аудит сайта https://prodvizhenie-sajtov-v-moskve113.ru .
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Дом дракона 2 сезон все серии
Новостройки в Екатеринбурге, купить квартиру в новостройке https://kupit-kvartiruekb.ru от застройщика. Строительство жилой и коммерческой недвижимости. Высокое качество, прозрачность на всех этапах строительства и сделки.
купить диплом вуза https://diplom-izhevsk.ru
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
geinoutime.com
왜냐하면… 왕수인은 가혹하지만 그에게는 모두가 함께 먹고 잔다는 규칙이 있습니다.
geinoutime.com
Zhu Houzhao는 서둘러 말했다.
สล็อตแมชชีนเว็บตรง: ความรื่นเริงที่ท่านไม่ควรพลาด
การเล่นสล็อตในปัจจุบันนี้ได้รับความสนใจอย่างกว้างขวาง เนื่องจากความง่ายดายที่ผู้ใช้สามารถใช้งานได้ได้ทุกที่ตลอดเวลา โดยไม่ต้องใช้เวลาการเดินทางไปยังคาสิโนจริง ๆ ในเนื้อหานี้ เราจะนำเสนอเกี่ยวกับ “สล็อตแมชชีน” และความบันเทิงที่ผู้เล่นจะได้พบในเกมสล็อตออนไลน์เว็บตรง
ความสะดวกในการเล่นสล็อตออนไลน์
หนึ่งในเหตุผลสล็อตเว็บตรงเป็นที่นิยมอย่างมาก คือความสะดวกสบายที่ผู้ใช้มี คุณสามารถเล่นสล็อตได้ทุกหนทุกแห่งทุกเวลา ไม่ว่าจะเป็นในบ้าน ในออฟฟิศ หรือแม้กระทั่งขณะเดินทางอยู่ สิ่งที่จำเป็นต้องมีคืออุปกรณ์ที่เชื่อมต่ออินเทอร์เน็ตได้ ไม่ว่าจะเป็นโทรศัพท์มือถือ แท็บเล็ท หรือโน้ตบุ๊ก
เทคโนโลยีที่ทันสมัยกับสล็อตเว็บตรง
การเล่นสล็อตออนไลน์ในปัจจุบันนี้ไม่เพียงแต่สะดวกสบาย แต่ยังประกอบด้วยเทคโนโลยีที่ทันสมัยที่ทันสมัยอีกด้วย สล็อตที่เว็บตรงใช้เทคโนโลยี HTML5 ซึ่งทำให้คุณไม่ต้องกังวลเกี่ยวกับการติดตั้งโปรแกรมหรือแอพพลิเคชั่น แค่ใช้เบราว์เซอร์บนอุปกรณ์ที่คุณมีและเข้าสู่เว็บไซต์ของเรา ผู้เล่นก็สามารถสนุกกับเกมได้ทันที
ตัวเลือกหลากหลายของเกมสล็อตออนไลน์
สล็อตที่เว็บตรงมาพร้อมกับความหลากหลายของเกมที่ท่านสามารถเลือก ไม่ว่าจะเป็นเกมคลาสสิกหรือเกมสล็อตที่มาพร้อมกับฟีเจอร์เด็ดและโบนัสหลากหลาย ท่านจะพบว่ามีเกมที่ให้เล่นมากมาย ซึ่งทำให้ไม่เบื่อกับการเล่นสล็อต
รองรับทุกอุปกรณ์
ไม่ว่าท่านจะใช้มือถือแอนดรอยด์หรือ iOS ท่านก็สามารถเล่นเกมสล็อตออนไลน์ได้อย่างไม่มีสะดุด เว็บไซต์ของเรารองรับทุกOSและทุกเครื่องมือ ไม่ว่าจะเป็นโทรศัพท์มือถือใหม่ล่าสุดหรือรุ่นเก่า หรือถึงแม้จะเป็นแท็บเล็ทและคอมพิวเตอร์ ท่านก็สามารถเล่นเกมสล็อตได้อย่างไม่มีปัญหา
สล็อตทดลองฟรี
สำหรับมือใหม่กับการเล่นสล็อตออนไลน์ หรือยังไม่แน่ใจเกี่ยวกับเกมที่ต้องการเล่น PG Slot ยังมีบริการทดลองเล่นเกมสล็อต ผู้เล่นเริ่มเล่นได้ทันทีทันทีโดยไม่ต้องสมัครสมาชิกหรือฝากเงินลงทุน การทดลองเล่นเกมสล็อตนี้จะช่วยให้ท่านเรียนรู้และเข้าใจเกมได้โดยไม่ต้องเสียค่าใช้จ่าย
โปรโมชันและโบนัส
หนึ่งในข้อดีของการเล่นเกมสล็อตกับ PG Slot คือมีโบนัสและโปรโมชั่นมากมายสำหรับผู้เล่น ไม่ว่าท่านจะเป็นสมาชิกใหม่หรือผู้เล่นเก่า คุณสามารถได้รับโปรโมชั่นและโบนัสต่าง ๆ ได้อย่างสม่ำเสมอ ซึ่งจะเพิ่มโอกาสในการชนะและเพิ่มความสนุกในเกม
โดยสรุป
การเล่นเกมสล็อตออนไลน์ที่ PG Slot เป็นการการลงทุนทางเกมที่มีค่า ผู้เล่นจะได้รับความสุขและความสะดวกจากการเล่นเกมสล็อต นอกจากนี้ยังมีโอกาสรับรางวัลและโบนัสมากมาย ไม่ว่าท่านจะใช้มือถือ แท็บเล็ตหรือแล็ปท็อปยี่ห้อไหน ก็สามารถเล่นได้ทันที อย่ารอช้า สมัครสมาชิกและเริ่มเล่น PG Slot วันนี้
https://malotafolks.com/?keyword=luck365
pg slot
สล็อตเว็บตรง — ใช้ โทรศัพท์มือถือ แท็บเลต คอมพิวเตอร์ส่วนตัว ฯลฯ เพื่อเล่น
ระบบสล็อตเว็บตรง ของ พีจีสล็อต ได้รับการพัฒนาและปรับแต่ง เพื่อให้ สามารถใช้งาน บนอุปกรณ์ที่หลากหลายได้อย่าง เต็มที่ ไม่สำคัญว่าจะใช้ สมาร์ทโฟน แท็บเลต หรือ คอมพิวเตอร์ แบบไหน
ที่ พีจีสล็อต เราเข้าใจว่าผู้เล่นต้องการ ของผู้เล่น ในเรื่อง ความสะดวก และ ความรวดเร็วในการเข้าถึงเกมคาสิโนออนไลน์ เราจึง ใช้ HTML 5 ซึ่งเป็น เทคโนโลยีล่าสุด ปัจจุบันนี้ พัฒนาเว็บของเรา คุณจึงไม่ต้อง ติดตั้งแอป หรือติดตั้งโปรแกรมเพิ่มเติม เพียง เปิดบราวเซอร์ บนอุปกรณ์ที่ คุณใช้อยู่ และเยี่ยมชม เว็บไซต์ของเรา คุณสามารถ เล่นเกมสล็อตได้ทันที
การสนับสนุนหลายอุปกรณ์
ไม่ว่าคุณจะใช้ สมาร์ทโฟน ระบบ แอนดรอยด์ หรือ iOS ก็สามารถ เล่นสล็อตได้อย่างราบรื่น ระบบของเรา ออกแบบมาให้รองรับ ระบบต่าง ๆ ไม่สำคัญว่าคุณ มี โทรศัพท์ ใหม่หรือเก่า หรือ แท็บเล็ตหรือโน้ตบุ๊ก ทุกอย่างก็สามารถ ใช้งานได้ ไม่มีปัญหา เรื่องความเข้ากันได้
สามารถเล่นได้ทุกที่ทุกเวลา
หนึ่งในข้อดีของการเล่นสล็อตกับ PG Slot คือ คุณสามารถ เล่นได้ทุกเวลา ไม่ว่าจะ ที่บ้าน ที่ทำงาน หรือแม้แต่ ในที่สาธารณะ สิ่งที่คุณต้องมีคือ อินเทอร์เน็ต คุณสามารถ เล่นเกมได้ทันที และคุณไม่ต้อง กังวลกับการดาวน์โหลด หรือติดตั้งโปรแกรมที่ ใช้พื้นที่ในอุปกรณ์
เล่นสล็อตฟรี
เพื่อให้ ผู้เล่นใหม่ ได้ลองและรู้จักเกมสล็อตของเรา PG Slot ยังเสนอบริการสล็อตทดลองฟรีอีกด้วย คุณสามารถ เริ่มเล่นได้ทันทีโดยไม่ต้องลงทะเบียนหรือฝากเงิน การ เล่นฟรีนี้จะช่วยให้คุณเข้าใจวิธีเล่นและรู้จักเกมก่อนลงเดิมพันจริง
การให้บริการและความปลอดภัย
PG Slot ตั้งใจให้บริการที่ดีที่สุดกับลูกค้า เรามี ทีมงานมืออาชีพพร้อมให้บริการและช่วยเหลือคุณตลอด 24 ชั่วโมง นอกจากนี้เรายังมี ระบบความปลอดภัยที่ทันสมัย ด้วยวิธีนี้ คุณจึงมั่นใจได้ว่า ข้อมูลและการเงินของคุณจะปลอดภัย
โปรโมชั่นและของรางวัลพิเศษ
อีกข้อดีของการเล่นสล็อตกับ PG Slot นั่นคือ มี โปรโมชั่นและโบนัสพิเศษมากมายสำหรับผู้เข้าร่วม ไม่ว่าคุณจะเป็น ผู้เล่นใหม่หรือเก่า คุณสามารถ รับโปรโมชันและโบนัสได้เรื่อย ๆ สิ่งนี้จะ เพิ่มโอกาสชนะและความสนุกในเกม
สรุปการเล่นสล็อตเว็บที่ PG Slot ถือเป็นการลงทุนที่คุ้มค่า คุณจะไม่เพียงได้รับความสุขและความสะดวกสบายจากเกมเท่านั้น แต่คุณยังมีโอกาสลุ้นรับรางวัลและโบนัสมากมายอีกด้วย ไม่สำคัญว่าจะใช้โทรศัพท์มือถือ แท็บเล็ต หรือคอมพิวเตอร์รุ่นใด สามารถมาร่วมสนุกกับเราได้เลยตอนนี้ อย่ารอช้า ลงทะเบียนและเริ่มเล่นสล็อตกับ PG Slot วันนี้!
ทดลองลองใช้เล่นสล็อต และค้นพบประสบการณ์การเล่นเกมที่ไม่เหมือนใคร!
สำหรับนักพนันที่กำลังต้องการความบันเทิงและโอกาสในการได้รับรางวัลมหาศาล สล็อตออนไลน์เป็นอีกหนึ่งตัวเลือกที่คุ้มค่าศึกษา.ด้วยความจำนวนมากของเกมสล็อตที่น่าตื่นเต้น ผู้เล่นสามารถลองเล่นและค้นหาเกมที่เหมาะกับตัวเองได้อย่างง่ายดาย.
ไม่ว่าคุณจะถูกใจเกมสล็อตคลาสสิกหรือต้องการความท้าทาย, ทางเลือกรอกลับมาให้คุณสัมผัส. จากสล็อตที่มีธีมมากมาย ไปจนถึงเกมที่มีฟีเจอร์พิเศษและรางวัลมากมาย, ผู้เล่นจะได้พบกับประสบการณ์ใหม่ที่น่าตื่นเต้นและน่าติดตาม.
ด้วยการปฏิบัติสล็อตฟรี, คุณสามารถศึกษาวิธีการเล่นและค้นค้นพบกลยุทธ์ที่เหมาะสมก่อนสร้างรายได้ด้วยเงินจริง. นี่คือโอกาสที่ดีที่จะปฏิบัติกับเกมและปรับปรุงโอกาสในการคว้ารางวัลใหญ่.
อย่าประวิงเวลา, ลงมือกับการปฏิบัติสล็อตออนไลน์วันนี้ และค้นพบประสบการณ์การเล่นเกมที่ไม่เหมือนใคร! ตื่นเต้นความท้าทาย, ความสนุกสนาน และโอกาสทองชนะรางวัลมากมาย. กล้าก้าวไปเดินทางสู่ความสมหวังของคุณในวงการสล็อตออนไลน์แล้ววันนี้!
ทดลองเล่นสล็อต pg
ทดลอง ทดลอง สล็อต PG ไปพร้อมกับ เปิดประตู ไปสู่ โลก แห่ง ความบันเทิง ที่ ไร้ขีดจำกัด
ของ นักเสี่ยงโชค ที่ พยายาม กำลังมองหา ความต้องการ เกมใหม่, สล็อต PG เป็น ทางเลือก ที่ ดึงดูดความสนใจ มากมาย. เนื่องจาก ความแตกต่าง ของ เกมสล็อตมากมาย ที่ น่าทึ่ง และ น่าทำความรู้จัก, นักเล่นเกม จะได้ ทดสอบ และ ลอง เกม ที่ ตรงกับ แบบอย่างการเล่น ของตนเอง.
ไม่ว่า นักพนัน จะชื่นชอบ ความผ่อนคลาย แบบดั้งเดิม หรือ สิ่งท้าทาย ใหม่ๆ, สล็อต PG ให้เลือก ให้เลือกอย่างมากมาย. ตั้งแต่ สล็อตประเภทคลาสสิก ที่ รู้จัก ไปจนถึง รูปแบบเกม ที่ มีลักษณะ คุณสมบัติพิเศษ และ โบนัสมากมาย, นักพนัน จะมีโอกาส สัมผัส บรรยากาศ ที่ ตื่นเต้น และ ตื่นเต้น
เพราะ การเล่นทดลอง สล็อต PG โดยไม่ต้องเสียเงิน, นักพนัน จะ เรียนรู้ กระบวนการเล่น และ ตรวจสอบ เคล็ดลับ ต่างๆ ก่อน เริ่มลงเดิมพัน ด้วยเงินจริง. ถึงกระนั้น เป็น ช่องทาง ที่ยอดเยี่ยม ที่จะ ปรับตัว และ ส่งเสริม โอกาส ในการ ครอบครอง รางวัลมหาศาล.
อย่ารอช้า, เข้าร่วม ใน การทดลองเล่น สล็อต PG ทันที และ พบเจอ ความรู้สึก ที่ ไม่จำกัด! สัมผัส ความตื่นเต้น, ความบันเทิง และ โอกาส ในการ ชนะรางวัล มากมหาศาล. เริ่มต้น ลงมือ สู่ ความสำเร็จ ของคุณในวงการ เกมสล็อต ตั้งแต่วันนี้!
เรื่อง ไซต์ PG Slots มีความ มี จุดเด่น หลายประการ ในเปรียบเทียบกับ คาสิโนแบบ เก่า, โดยเฉพาะ ใน ปัจจุบันนี้. คุณประโยชน์สำคัญ เหล่านี้ ได้แก่:
ความสะดวกสบาย: คุณ สามารถเข้าร่วม สล็อตออนไลน์ได้ ตลอด 24 ชั่วโมง จาก ทุกแห่ง, ให้ ผู้เล่นสามารถ ทดลอง ได้ ทุกแห่ง โดยไม่ต้อง ใช้เวลา ไปคาสิโนแบบ ทั่วไป ๆ
เกมที่หลากหลาย: สล็อตออนไลน์ นำเสนอ รูปแบบเกม ที่ แตกต่างกัน, เช่น สล็อตรูปแบบคลาสสิค หรือ สล็อต ที่มี ลักษณะ และโบนัส พิเศษ, ไม่ก่อให้เกิด ความเบื่อหน่าย ในเกม
ข้อเสนอส่งเสริมการขาย และค่าตอบแทน: สล็อตออนไลน์ แทบจะ เสนอ ข้อเสนอส่งเสริมการขาย และประโยชน์ เพื่อส่งเสริม โอกาสในการ ในการ ได้รับรางวัล และ เพิ่ม ความสนุกสนาน ให้กับเกม
ความปลอดภัย และ ความน่าเชื่อถือ: สล็อตออนไลน์ มักจะ ใช้ การรักษาความปลอดภัย ที่ เหมาะสม, และ พึ่งพาได้ ว่า ข้อมูลลับ และ การชำระเงิน จะได้รับการ ดูแล
บริการสนับสนุน: PG Slots มี ผู้เชี่ยวชาญ มืออาชีพ ที่มุ่งมั่น ให้บริการ ตลอดเวลา
การเล่นบนอุปกรณ์เคลื่อนที่: สล็อต PG สนับสนุน การเล่นบนมือถือ, อำนวย ผู้เล่นสามารถเข้าร่วม ในทุกที่
ทดลองเล่นโดยไม่เสียค่าใช้จ่าย: เกี่ยวกับ ผู้เล่นรายใหม่, PG ยังให้บริการ เล่นฟรี เช่นกัน, เพื่อ ผู้เล่น ลองใช้ วิธีใช้ และเรียนรู้ เกมก่อน เล่นด้วยเงินจริง
สล็อต PG มีลักษณะ ข้อดี มากก ที่ ทำ ให้ได้รับความต้องการ ในยุคปัจจุบัน, ส่งเสริม การ ความเพลิดเพลิน ให้กับเกมด้วย.
как пожаловаться на сайт мошенников как пожаловаться на сайт мошенников .
Cериал Голяк https://golyak-serial-online.ru смотреть онлайн в хорошем качестве и с лучшей озвучкой на любых устройствах. Все сезоны истории мелкого преступника Винни и его друзей в английском городке!
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Драгон Мани Казино https://krpb.ru – ваше место для азартных приключений! Наслаждайтесь широким выбором игр, щедрыми бонусами и захватывающими турнирами. Безопасность и честная игра гарантированы. Присоединяйтесь к нам и испытайте удачу в самом захватывающем онлайн-казино!
Famous French footballer Kylian Mbappe https://kylianmbappe.prostoprosport-ar.com has become a global ambassador for Dior. The athlete will represent the men’s collections of creative director Kim Jones and the Sauvage fragrance, writes WWD. Mbappe’s appointment follows on from the start of the fashion house’s collaboration with the Paris Saint-Germain football club. Previously, Jones created a uniform for the team where Kylian is a player.
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
игровой автомат крейзи манки игровой автомат крейзи манки .
สล็อตเว็บตรง — ใช้ โทรศัพท์มือถือ แท็บเลต คอมพิวเตอร์ ฯลฯ เพื่อเล่น
ระบบสล็อตเว็บตรง ของ พีจีสล็อต ได้รับการพัฒนาและปรับปรุง เพื่อให้ สามารถใช้งาน บนอุปกรณ์ที่หลากหลายได้อย่าง สมบูรณ์ ไม่สำคัญว่าจะใช้ สมาร์ทโฟน แท็บเลต หรือ คอมพิวเตอร์ส่วนตัว รุ่นไหน
ที่ PG Slot เราเข้าใจถึงความต้องการ ของผู้เล่น ในเรื่อง ความสะดวกสบาย และ การเข้าถึงเกมออนไลน์อย่างรวดเร็ว เราจึง ใช้ HTML 5 ซึ่งเป็น เทคโนโลยีที่ทันสมัยที่สุด ปัจจุบันนี้ มาพัฒนาเว็บไซต์ของเรากันเถอะ คุณจึงไม่ต้อง โหลดแอป หรือติดตั้งโปรแกรมเพิ่มเติม เพียง เปิดบราวเซอร์ บนอุปกรณ์ที่ มีอยู่ของคุณ และเยี่ยมชม เว็บไซต์ของเรา คุณสามารถ เพลิดเพลินกับสล็อตแมชชีนได้ทันที
การใช้งานกับอุปกรณ์หลากหลาย
ไม่ว่าคุณจะใช้ มือถือ ระบบ แอนดรอยด์ หรือ ไอโอเอส ก็สามารถ เล่นเกมสล็อตได้อย่างไม่มีปัญหา ระบบของเรา ออกแบบมาเพื่อรองรับ ทุกระบบปฏิบัติการ ไม่สำคัญว่าคุณ ใช้ มือถือ รุ่นใหม่หรือรุ่นเก่า หรือ แท็บเล็ตหรือแล็ปท็อป ทุกอย่างก็สามารถ ใช้งานได้ ไม่มีปัญหา ความเข้ากันได้
สามารถเล่นได้ทุกที่ทุกเวลา
หนึ่งในข้อดีของการเล่นสล็อตกับ PG Slot ก็คือ คุณสามารถ เล่นได้ตลอดเวลา ไม่ว่าจะ เป็นที่บ้าน ออฟฟิศ หรือแม้แต่ สถานที่สาธารณะ สิ่งที่คุณต้องมีคือ อินเทอร์เน็ต คุณสามารถ เล่นเกมได้ทันที และคุณไม่ต้อง กังวลเรื่องการโหลด หรือติดตั้งโปรแกรมที่ เปลืองพื้นที่อุปกรณ์
ทดลองเล่นสล็อตฟรี
เพื่อให้ ผู้เล่นที่ใหม่ ได้ลองเล่นและสัมผัสเกมสล็อตของเรา PG Slot ยังมีบริการสล็อตฟรี คุณสามารถ เล่นได้ทันทีโดยไม่ต้องสมัครสมาชิกหรือฝากเงิน การ ทดลองเล่นสล็อตแมชชีนฟรีนี้จะช่วยให้คุณเรียนรู้วิธีเล่นและเข้าใจเกมก่อนตัดสินใจเดิมพันด้วยเงินจริง
บริการและการรักษาความปลอดภัย
PG Slot มุ่งมั่นที่จะให้บริการที่ดีที่สุดแก่ลูกค้า เรามี ทีมงานมืออาชีพพร้อมให้บริการและช่วยเหลือคุณตลอด 24 ชั่วโมง นอกจากนี้เรายังมี ระบบรักษาความปลอดภัยที่ทันสมัย ด้วยวิธีนี้ คุณจึงมั่นใจได้ว่า ข้อมูลและการเงินของคุณจะปลอดภัย
โปรโมชั่นและของรางวัลพิเศษ
การเล่นสล็อตกับ PG Slot ยังมีข้อดี นั่นคือ มี โปรโมชันและโบนัสพิเศษสำหรับสมาชิก ไม่ว่าคุณจะเป็น สมาชิกใหม่หรือสมาชิกเก่า คุณสามารถ รับโปรโมชันและโบนัสได้เรื่อย ๆ สิ่งนี้จะ เพิ่มโอกาสในการชนะและเพิ่มความเพลิดเพลินในเกม
สรุปการเล่นสล็อตเว็บที่ PG Slot ถือเป็นการลงทุนที่คุ้มค่า คุณจะไม่เพียงได้รับความสุขและความสะดวกสบายจากเกมเท่านั้น แต่คุณยังมีโอกาสลุ้นรับรางวัลและโบนัสมากมายอีกด้วย ไม่สำคัญว่าจะใช้โทรศัพท์มือถือ แท็บเล็ต หรือคอมพิวเตอร์รุ่นใด สามารถมาร่วมสนุกกับเราได้เลยตอนนี้ อย่ารอช้า ลงทะเบียนและเริ่มเล่นสล็อตกับ PG Slot วันนี้!
ประสบการณ์การสำรวจเล่นสล็อต PG บนพอร์ทัลวางเดิมพันตรง: เข้าสู่โลกแห่งความตื่นเต้นที่ไม่มีข้อจำกัด
ในกรณีของนักพนันที่กำลังมองหาประสบการณ์เกมแปลกใหม่ และหวังเจอแหล่งพนันที่เชื่อถือได้, การสำรวจสล็อตแมชชีน PG บนเว็บไซต์ตรงนับว่าเป็นตัวเลือกที่น่าสนใจอย่างมาก. อันเนื่องมาจากความแตกต่างของเกมสล็อตที่มีให้เลือกมากมาย, ผู้เล่นจะได้พบเจอกับโลกแห่งความรื่นเริงและความสนุกเพลิดเพลินที่ไร้ขีดจำกัด.
แพลตฟอร์มวางเดิมพันตรงนี้ มอบประสบการณ์การเล่นเกมที่ปลอดภัย มีความน่าเชื่อถือ และตอบสนองความต้องการของนักเดิมพันได้เป็นอย่างดี. ไม่ว่าท่านจะผู้เล่นจะติดใจเกมสล็อตแมชชีนแนวคลาสสิกที่มีความคุ้นเคย หรือต้องการประสบการณ์เกมที่ไม่เหมือนใครที่มีคุณลักษณะพิเศษเฉพาะและโบนัสล้นหลาม, แพลตฟอร์มไม่ผ่านเอเย่นต์นี้ก็มีให้เลือกอย่างหลากหลาย.
เนื่องจากมีระบบการลองเกมสล็อตแมชชีน PG โดยไม่เสียค่าใช้จ่าย, ผู้เล่นจะได้โอกาสศึกษาวิธีการเล่นเดิมพันและทดสอบกลยุทธ์ที่หลากหลาย ก่อนจะเริ่มใช้เงินจริงด้วยเงินสด. สิ่งนี้ถือเป็นโอกาสอันดีที่สุดที่จะเพิ่มความพร้อมสรรพและเสริมโอกาสในการชิงรางวัลมหาศาลใหญ่.
ไม่ว่าผู้เล่นจะคุณอาจจะปรารถนาความเพลิดเพลินแบบคลาสสิก หรือการพิชิตแปลกใหม่, สล็อตแมชชีน PG บนเว็บไซต์พนันไม่ผ่านเอเย่นต์ก็มีให้เลือกเล่นอย่างหลากหลายชนิด. คุณอาจจะได้เผชิญกับการทดลองเล่นการเล่นเดิมพันที่น่าตื่นเต้น น่ารื่นเริง และสนุกเพลิดเพลินไปกับจังหวะในการได้รับรางวัลใหญ่มหาศาล.
อย่าลังเล, ร่วมสนุกสำรวจเล่นสล็อต PG บนเว็บเสี่ยงโชคไม่ผ่านเอเย่นต์ขณะนี้ และเจอโลกแห่งความบันเทิงที่ปลอดภัย น่าติดตาม และพร้อมเต็มไปด้วยความสุขสนานรอคอยคุณ. เผชิญความตื่นเต้นเร้าใจ, ความสุข และโอกาสในการได้รางวัลมหาศาลมหาศาล. เริ่มต้นเดินทางสู่การเป็นผู้ชนะในวงการเกมออนไลน์วันนี้!
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
pena slot
프라그마틱 무료
장황후는 퉁명스럽게 말했다.
Скачать свежие новинки песен https://muzfo.net 2024 года ежедневно. Наслаждайтесь комфортным прослушиванием, скачивайте музыку за пару кликов на сайте.
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
הימורים באינטרנט
הימורי ספורט – הימורים באינטרנט
הימור ספורטיביים נהיו לאחד התחומים המתפתחים ביותר בהימורים ברשת. שחקנים מסוגלים להמר על תוצאת של אירועים ספורטיביים פופולריים כמו כדורגל, כדור סל, משחק הטניס ועוד. האפשרויות להתערבות הן רבות, כולל תוצאתו ההתמודדות, כמות הגולים, כמות הפעמים ועוד. להלן דוגמאות למשחקי נפוצים במיוחד שעליהם ניתן להתערב:
כדורגל: ליגת אלופות, גביע העולם, ליגות אזוריות
כדור סל: NBA, יורוליג, תחרויות בינלאומיות
משחק הטניס: ווימבלדון, אליפות ארה”ב הפתוחה, אליפות צרפת הפתוחה
פוקר ברשת באינטרנט – הימורים ברשת
פוקר באינטרנט הוא אחד ממשחקי ההימורים המוכרים ביותר כיום. משתתפים יכולים להתמודד מול יריבים מכל רחבי תבל במגוון סוגי של המשחק , כגון Texas Hold’em, אומהה, סטאד ועוד. ניתן למצוא תחרויות ומשחקי במבחר רמות ואפשרויות הימור מגוונות. אתרי הפוקר המובילים מציעים גם:
מבחר רב של וריאציות המשחק פוקר
תחרויות שבועיים וחודשיים עם פרסים כספיים גבוהים
שולחנות המשחק למשחקים מהירים ולטווח הארוך
תוכניות נאמנות ומועדוני VIP VIP בלעדיות
בטיחות והוגנות
כאשר הבחירה בפלטפורמה להימורים ברשת, חיוני לבחור אתרי הימורים מורשים המפוקחים המציעים סביבת משחק מאובטחת והגיונית. אתרים אלה משתמשים בטכנולוגיית אבטחה מתקדמות להגנה על מידע אישי ופיננסי, וגם בתוכנות גנרטור מספרים אקראיים (RNG) כדי להבטיח הגינות במשחקי ההימורים.
מעבר לכך, חשוב לשחק גם בצורה אחראית תוך כדי קביעת מגבלות אישיות הימורים אישיות של השחקן. מרבית האתרים מאפשרים לשחקנים להגדיר מגבלות הפסד ופעילויות, כמו גם להשתמש ב- כלים נגד התמכרויות. שחקו בחכמה ואל תרדפו אחרי הפסד.
המדריך השלם למשחקי קזינו באינטרנט, הימורי ספורט ופוקר ברשת
ההימורים ברשת מציעים גם עולם שלם של הזדמנויות מלהיבות לשחקנים, מתחיל מקזינו באינטרנט וגם משחקי ספורט ופוקר ברשת. בעת בחירת פלטפורמת הימורים, חשוב לבחור גם אתרי הימורים המפוקחים המציעים סביבת משחק מאובטחת והגיונית. זכרו גם לשחק באופן אחראי תמיד – ההימורים ברשת אמורים להיות מבדרים ומהנים ולא גם לגרום לבעיות פיננסיות או גם חברתיות.
Скачать свежие новинки песен https://muzfo.net 2024 года ежедневно. Наслаждайтесь комфортным прослушиванием, скачивайте музыку за пару кликов на сайте.
ทดลองดำเนินการเล่นสล็อต และค้นพบประสบการณ์การเล่นเกมที่ไม่เหมือนใคร!
สำหรับนักพนันที่กำลังพิจารณาความบันเทิงและโอกาสในการชนะรางวัลมหาศาล สล็อตออนไลน์เป็นอีกหนึ่งตัวเลือกที่คุ้มค่าใช้.ด้วยความมากมายของเกมสล็อตที่น่าตื่นเต้น ผู้เล่นสามารถปฏิบัติและค้นหาเกมที่ต้องการได้อย่างง่ายดาย.
ไม่ว่าคุณจะชอบเกมสล็อตคลาสสิกหรือต้องการความท้าทาย, โอกาสรอคอยให้คุณสัมผัส. จากสล็อตที่มีหัวข้อมากมาย ไปจนถึงเกมที่มีคุณสมบัติพิเศษและรางวัล, ผู้เล่นจะได้พบกับการเล่นเกมที่น่าตื่นเต้นและน่าติดตาม.
ด้วยการทดสอบสล็อตฟรี, คุณสามารถปฏิบัติวิธีการเล่นและค้นตัดสินใจกลยุทธ์ที่ตรงใจก่อนเริ่มลงเดิมพันด้วยเงินจริง. นี่คือโอกาสที่จะศึกษากับเกมและยกระดับโอกาสในการคว้ารางวัลใหญ่.
อย่าประวิงเวลา, เข้าไปกับการทดลองเล่นสล็อตออนไลน์วันนี้ และค้นพบประสบการณ์การเล่นเกมที่ไม่เหมือนใคร! เพลิดเพลินความสนใจ, ความสนุกสนาน และโอกาสในการชนะรางวัลใหญ่. กล้าก้าวไปเดินทางสู่ความสำเร็จของคุณในวงการสล็อตออนไลน์แล้ววันนี้!
פוקר באינטרנט
הימורי ספורטיביים – הימורים באינטרנט
הימור ספורטיביים נעשו לאחד התחומים המשגשגים ביותר בהימורים באינטרנט. שחקנים יכולים להתערב על תוצאותיהם של אירועי ספורט נפוצים לדוגמה כדורגל, כדור סל, משחק הטניס ועוד. האפשרויות להימור הן רבות, כולל תוצאת המשחק, מספר הגולים, מספר הנקודות ועוד. להלן דוגמאות של למשחקי נפוצים במיוחד עליהם אפשרי להמר:
כדורגל: ליגת האלופות, גביע העולם, ליגות מקומיות
כדור סל: ליגת NBA, יורוליג, טורנירים בינלאומיים
טניס: טורניר ווימבלדון, US Open, רולאן גארוס
פוקר באינטרנט – הימור באינטרנט
פוקר ברשת הוא אחד ממשחקי ההימורים הפופולריים ביותר כיום. משתתפים יכולים להתמודד מול מתחרים מרחבי העולם בסוגי סוגי משחק , למשל טקסס הולדם, Omaha, סטאד ועוד. ניתן למצוא טורנירים ומשחקי קש במבחר דרגות ואפשרויות מגוונות. אתרי פוקר הטובים מציעים:
מבחר רב של וריאציות פוקר
תחרויות שבועיים וחודשיים עם פרסים כספיים
שולחנות למשחק מהיר ולטווח הארוך
תוכניות נאמנות ומועדוני עם הטבות בלעדיות
בטיחות והוגנות
בעת הבחירה פלטפורמה להימורים ברשת, חיוני לבחור גם אתרי הימורים מורשים המפוקחים המציעים סביבת למשחק בטוחה והוגנת. אתרים אלו עושים שימוש בטכנולוגיית הצפנה מתקדמות להבטחה על מידע אישי ופיננסי, וכן באמצעות תוכנות מחולל מספרים אקראיים (RNG) כדי להבטיח הגינות במשחקים במשחקים.
בנוסף, הכרחי לשחק גם בצורה אחראית תוך קביעת מגבלות אישיות הימורים אישיות. מרבית האתרים מאפשרים למשתתפים לקבוע מגבלות להפסדים ופעילות, כמו גם לנצל כלים נגד התמכרויות. הימרו בחכמה ואל תרדפו אחרי הפסד.
המדריך המלא לקזינו באינטרנט, הימורי ספורט ופוקר באינטרנט ברשת
הימורים ברשת מציעים עולם שלם של של הזדמנויות מרתקות למשתתפים, מתחיל מקזינו אונליין וכל בהימורי ספורט ופוקר באינטרנט. בזמן בחירת פלטפורמת הימורים, הקפידו לבחור גם אתרים מפוקחים המציעים סביבת משחק מאובטחת והגיונית. זכרו גם לשחק באופן אחראי תמיד – ההימורים ברשת אמורים להיות מבדרים ולא ליצור לבעיות כלכליות או גם חברתיים.
сериал в хорошем качестве
Агентство по продвижению телеграм-каналов https://883666b.com в Москве специализируется на разработке и реализации стратегий для увеличения аудитории и вовлечённости подписчиков на телеграм-каналах. Эксперты агентства помогают клиентам определить целевую аудиторию, разрабатывают контент-планы и рекламные кампании. Услуги включают рекламу посевами, таргет рекламой, анализ конкурентов, SEO-оптимизацию контента.
הימורי ספורט
הימורי ספורט – הימור באינטרנט
הימור ספורטיביים הפכו לאחד התחומים המשגשגים ביותר בהימורים ברשת. שחקנים מסוגלים להמר על תוצאותיהם של אירועי ספורטיביים מוכרים למשל כדור רגל, כדורסל, משחק הטניס ועוד. האפשרויות להימור הן מרובות, וביניהן תוצאתו המשחק, מספר השערים, מספר הפעמים ועוד. הבא דוגמאות למשחקים נפוצים שעליהם ניתן להמר:
כדור רגל: ליגת האלופות, מונדיאל, ליגות מקומיות
כדורסל: ליגת NBA, יורוליג, טורנירים בינלאומיים
משחק הטניס: ווימבלדון, אליפות ארה”ב הפתוחה, אליפות צרפת הפתוחה
פוקר באינטרנט – הימורים ברשת
פוקר באינטרנט הוא אחד ממשחקי ההימורים הפופולריים ביותר בימינו. משתתפים מסוגלים להתמודד נגד יריבים מרחבי העולם בסוגי וריאציות של המשחק , למשל טקסס הולדם, Omaha, Stud ועוד. אפשר למצוא תחרויות ומשחקי במגוון רמות ואפשרויות שונות. אתרי פוקר המובילים מציעים גם:
מגוון רחב של גרסאות פוקר
טורנירים שבועיות וחודשיים עם פרסים כספיים גבוהים
שולחנות למשחק מהיר ולטווח הארוך
תוכניות נאמנות ומועדוני VIP עם הטבות יחודיות
בטיחות ואבטחה והגינות
כאשר הבחירה פלטפורמה להימורים ברשת, חיוני לבחור גם אתרי הימורים מורשים המפוקחים המציעים גם סביבה משחק בטוחה והגיונית. אתרים אלו משתמשים בטכנולוגיית אבטחה מתקדמת להבטחה על מידע אישי ופיננסי, וכן באמצעות תוכנות מחולל מספרים אקראיים (RNG) כדי להבטיח הגינות המשחקים במשחקים.
בנוסף, חשוב לשחק בצורה אחראי תוך כדי קביעת מגבלות הימור אישיות של השחקן. מרבית אתרי ההימורים מאפשרים לשחקנים להגדיר מגבלות להפסדים ופעילות, כמו גם להשתמש ב- כלים למניעת התמכרות. שחקו בחכמה ואל תרדפו גם אחרי הפסד.
המדריך השלם לקזינו ברשת, הימורי ספורט ופוקר באינטרנט באינטרנט
ההימורים ברשת מציעים גם עולם שלם של הזדמנויות מלהיבות למשתתפים, החל מקזינו אונליין וכל משחקי ספורט ופוקר ברשת. בזמן בחירת בפלטפורמת הימורים, חשוב לבחור אתרים מפוקחים המציעים סביבת משחק בטוחה והגיונית. זכרו גם לשחק בצורה אחראית תמיד – משחקי ההימורים ברשת אמורים להיות מבדרים ומהנים ולא לגרום לבעיות פיננסיות או גם חברתיים.
online pharmacy no prescription augmentin
интернет эквайринг https://internet-ekvajring.kz – безопасные и эффективные платежные решения для вашего бизнеса.
bitz casino
сайт битц казино
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
сериал смотреть
{
https://domkrasivo.com/?keyword=jeniusbet
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
купить второй аккаунт телеграмм http://www.kupit-akkaunt-telegramm11.ru .
купить квартиру от застройщика недорого https://nedvizhimost47.ru
Привет всем!
Недавно мы решили обновить напольные покрытия в доме. На сайте https://hobbihouse.ru/laminat/pochemu-spc-laminat-vinilpol-i-clusterfloor-samye-populyarnye-v-rf/ нашли полезную информацию, которая помогла сделать правильный выбор. Благодаря этим рекомендациям мы выбрали натуральные покрытия с сертификатами качества и успешно завершили укладку. Продукция отличается простотой нанесения и подходит для жилых помещений. Широкий выбор и использование современных инструментов сэкономили наше время.
ламинат под камень
фальшпол
водостойкая ПВХ-плитка
напольное покрытие
укладка ламината
применение ковролина
ыбор подложки
Удачи!
777 슬롯
그의 눈은 불을 뿜는 것처럼 붉었고 분노로 떨고 있었다.
Секрет стильного пространства – плинтус теневой.
теневой профиль для пола теневой профиль для пола .
купить квартиру в новостройке от застройщика https://novostroyka47.ru
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
amoxicillin for sale online: doxycyclineca – order amoxicillin online
Melin Dizayn ile çalışmak harikaydı. Standımızı tam zamanında teslim ettiler ve hiçbir aksaklık yaşamadık. Kesinlikle tekrar çalışmak isteriz.
קזינו אונליין
הימורי ספורט – הימורים באינטרנט
הימור ספורטיביים נהיו לאחד התחומים המשגשגים ביותר בהימור באינטרנט. משתתפים יכולים להתערב על תוצאת של אירועים ספורט נפוצים לדוגמה כדורגל, כדור סל, טניס ועוד. האפשרויות להימור הן רבות, וביניהן תוצאתו המאבק, מספר הגולים, מספר הפעמים ועוד. הבא דוגמאות של למשחקי נפוצים במיוחד שעליהם אפשרי להתערב:
כדורגל: ליגת אלופות, גביע העולם, ליגות מקומיות
כדור סל: ליגת NBA, יורוליג, תחרויות בינלאומיות
טניס: ווימבלדון, US Open, אליפות צרפת הפתוחה
פוקר ברשת – הימורים באינטרנט
משחק הפוקר באינטרנט הוא אחד ממשחקי ההימורים הפופולריים ביותר בימינו. משתתפים יכולים להתמודד נגד יריבים מכל רחבי תבל במגוון סוגי משחק , לדוגמה טקסס הולדם, אומהה, סטאד ועוד. אפשר לגלות תחרויות ומשחקי במגוון דרגות ואפשרויות הימור מגוונות. אתרי פוקר המובילים מציעים:
מגוון רחב של גרסאות פוקר
טורנירים שבועיים וחודשיים עם פרסים כספיים
שולחנות המשחק למשחק מהיר ולטווח ארוך
תוכניות נאמנות ומועדוני VIP עם הטבות יחודיות
בטיחות ואבטחה והגינות
כאשר בוחרים בפלטפורמה להימורים ברשת, חשוב לבחור אתרי הימורים מורשים ומפוקחים המציעים גם סביבת משחק מאובטחת והגיונית. אתרים אלה עושים שימוש בטכנולוגיות אבטחה מתקדמות להגנה על נתונים אישיים ופיננסיים, וכן באמצעות תוכנות גנרטור מספרים רנדומליים (RNG) כדי להבטיח הגינות במשחקים במשחקים.
מעבר לכך, חשוב לשחק גם בצורה אחראית תוך כדי קביעת מגבלות אישיות הימורים אישיות של השחקן. רוב אתרי ההימורים מאפשרים גם לשחקנים לקבוע מגבלות הפסד ופעילויות, כמו גם לנצל כלים נגד התמכרויות. שחק בחכמה ואל גם תרדפו גם אחרי הפסד.
המדריך השלם למשחקי קזינו באינטרנט, הימורי ספורט ופוקר באינטרנט באינטרנט
ההימורים באינטרנט מציעים גם עולם שלם של הזדמנויות מרתקות למשתתפים, מתחיל מקזינו אונליין וגם בהימורי ספורט ופוקר באינטרנט. בעת הבחירה בפלטפורמת הימורים, חשוב לבחור אתרי הימורים המפוקחים המציעים סביבה משחק מאובטחת והגיונית. זכרו גם לשחק בצורה אחראית תמיד – ההימורים באינטרנט אמורים להיות מבדרים ומהנים ולא ליצור לבעיות כלכליות או חברתיות.
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Simply wish to say your article is as surprising. The clarity in your post is just nice and i can assume you’re an expert on this subject. Fine with your permission let me to grab your feed to keep up to date with forthcoming post. Thanks a million and please carry on the enjoyable work.
mazda-demio.ru/forums/index.php?autocom=gallery&req=si&img=4139
programasites.com.br/blog/post/11666/e-mail-marketing-boas-praticas-e-temas-para-abordar
ik21v.ru/
retrogaming.in.ua/index.php?ukey=linkexchange&did=33&le_categoryID=0&page=22&show_all=yes
1776reloaded.us/blogs/7/Where-to-buy-a-diploma-or-certificate-at-an-adequate
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Melin Dizayn’ın profesyonel ekibi ile çalışmak büyük bir keyifti. Her adımda bizimle
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello!
Daily News Digest! Get your daily dose of news with our concise and informative digest. Stay updated on the go with quick summaries of top stories.
Very good thematic site – https://gsroups.com
Asian recipes
food blog
financial news
short-haul travel
news coverage
startup
relationship advice
marketing tips
Goog luck!
Хостинг в Беларуси бесплатно: лучший выбор для вашего сайта, за и против.
Бесплатные хостинги в Беларуси: что выбрать?, советы и рекомендации.
Выбор профессионалов: топ-3 хостинга в Беларуси бесплатно, характеристики и отзывы.
Как перенести сайт на бесплатный хостинг в Беларуси?, инструкция и советы.
Бесплатный SSL для хостинга в Беларуси: зачем он нужен?, за и против.
Как создать сайт на бесплатном хостинге в Беларуси?, инструкция и рекомендации.
Где можно купить хостинг в Беларуси дешево и качественно?, обзор и сравнение.
Виртуальный хостинг Виртуальный хостинг .
ххх русский анал с разговорами safavia.ru .
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Головоломка 2
Можете купить гантельные грифы на https://grify-dlya-gantely.ru/по приятным ценамоптимальной длины. В производстве износостойкого инвентаря применяются углеродистые марки металла. Грифы для гантелей изготавливаются в трех популярных диаметрах. Отягощения созданы для эффективных занятий и выполнены с разметкой для правильного размещения рук и насечками для надежного хвата. Продукты покрываются защитным составом никеля. Российская компания предлагает внушительный объем спортивного инвентаря для дома и фитнес клуба. Это универсальный инвентарь для тяжелых занятий в любых условиях.
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Wow, wonderful blog layout! How long have you been blogging for? you made blogging look easy. The overall look of your website is magnificent, as well as the content!
tlnet.com.vn/hai-sam-nau-rau-cu/
tecnologiaeducativa.sepyc.gob.mx/forum/topic/comentarios-de-videos-sobre-la-basura/?part=1090
elibot.gg/commands
1001cruise.ru/carnival-cruises/114-news/762-liner-royal-princess-will-be-released-in-the-first-flight.html
http://www.modern-constructions.org/blogs/44177/%D0%94%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D1%8B-%D0%B2%D1%8B%D1%81%D0%BE%D1%87%D0%B0%D0%B9%D1%88%D0%B5%D0%B3%D0%BE-%D0%BA%D0%B0%D1%87%D0%B5%D1%81%D1%82%D0%B2%D0%B0-%D0%B2%D0%B0%D1%88-%D1%88%D0%B0%D0%B3-%D0%BA-%D0%BF%D1%80%D0%BE%D1%84%D0%B5%D1%81%D1%81%D0%B8%D0%BE%D0%BD%D0%B0%D0%BB%D1%8C%D0%BD%D0%BE%D0%BC%D1%83-%D1%80%D0%BE%D1%81%D1%82%D1%83
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi there! Would you mind if I share your blog with my facebook group? There’s a lot of folks that I think would really enjoy your content. Please let me know. Thank you
http://www.aapeducation.com.au/component/comprofiler/pluginclass/cbblogs.html?action=blogs&func=show&id=59
iclicky.com/index.php?do=/public/user/blogs/name_Alanpoe/page_5/
wiuwi.com/blogs/70298/%D0%93%D0%B4%D0%B5-%D0%BD%D0%B0%D0%B9%D1%82%D0%B8-%D1%81%D0%B0%D0%BC%D1%8B%D0%B5-%D0%BD%D0%B0%D0%B4%D0%B5%D0%B6%D0%BD%D1%8B%D0%B5-%D0%BF%D0%BE%D1%81%D1%82%D0%B0%D0%B2%D1%89%D0%B8%D0%BA%D0%B8-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC%D0%BE%D0%B2
noosfero.ufba.br/jesicaambrel/blog?npage=3
chefrobertsdirect.com/index.php?main_page=page&id=2
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
https://medium.com/@momejar21741/pg-59490dd058fd
สล็อตเว็บโดยตรง — ใช้ได้กับ มือถือ แท็บเล็ต คอมพิวเตอร์ส่วนตัว ฯลฯ เพื่อเล่น
ระบบสล็อตตรงจากเว็บ ของ PG Slot ได้รับการพัฒนาและอัปเดต เพื่อให้ สามารถใช้งาน บนอุปกรณ์ที่หลากหลายได้อย่าง เต็มที่ ไม่สำคัญว่าจะใช้ สมาร์ทโฟน แท็บเล็ต หรือ คอมฯ รุ่นใด
ที่ PG Slot เราเข้าใจถึงสิ่งที่ผู้เล่นต้องการ ของผู้เล่น ในเรื่อง การใช้งานง่าย และ ความรวดเร็วในการเข้าถึงเกมคาสิโนออนไลน์ เราจึง ใช้เทคโนโลยี HTML 5 ซึ่งเป็น เทคโนโลยีที่ทันสมัยที่สุด ในขณะนี้ มาใช้พัฒนาเว็บไซต์ คุณจึงไม่ต้อง โหลดแอป หรือติดตั้งโปรแกรมเพิ่มเติม เพียง เปิดเบราว์เซอร์ บนอุปกรณ์ที่ คุณมีอยู่ และเยี่ยมชม เว็บไซต์เรา คุณสามารถ สนุกกับสล็อตได้ทันที
การรองรับอุปกรณ์หลายชนิด
ไม่ว่าคุณจะใช้ โทรศัพท์มือถือ ระบบ Android หรือ iOS ก็สามารถ เล่นสล็อตได้อย่างราบรื่น ระบบของเรา ออกแบบมาเพื่อรองรับ ระบบปฏิบัติการทั้งหมด ไม่สำคัญว่าคุณ มี สมาร์ทโฟน ใหม่หรือเก่า หรือ แม้แต่แท็บเล็ตหรือแล็ปท็อป ทุกอย่างก็สามารถ ใช้งานได้อย่างไม่มีปัญหา ไม่มีปัญหา ในเรื่องความเข้ากันได้
เล่นได้ทุกที่และทุกเวลา
หนึ่งในข้อดีของการเล่นสล็อตกับ PG Slot ก็คือ คุณสามารถ เล่นได้ตลอดเวลา ไม่ว่าจะ ที่บ้าน ที่ทำงาน หรือแม้แต่ ในที่สาธารณะ สิ่งที่คุณต้องมีคือ การเชื่อมต่ออินเทอร์เน็ต คุณสามารถ เริ่มเกมได้ทันที และคุณไม่ต้อง กังวลกับการดาวน์โหลด หรือติดตั้งโปรแกรมที่ ใช้พื้นที่ในอุปกรณ์
ทดลองเล่นสล็อตฟรี
เพื่อให้ ผู้ใช้ใหม่ มีโอกาสลองและสัมผัสประสบการณ์สล็อตแมชชีนของเรา PG Slot ยังมีบริการสล็อตฟรี คุณสามารถ เล่นได้ทันทีโดยไม่ต้องสมัครสมาชิกหรือฝากเงิน การ เล่นฟรีนี้จะช่วยให้คุณเข้าใจวิธีเล่นและรู้จักเกมก่อนลงเดิมพันจริง
บริการและการรักษาความปลอดภัย
PG Slot มุ่งมั่นที่จะให้บริการที่ดีที่สุดแก่ลูกค้า เรามี ทีมงานพร้อมบริการคุณตลอดเวลา นอกจากนี้เรายังมี ระบบความปลอดภัยที่ทันสมัย ด้วยวิธีนี้ คุณจึงมั่นใจได้ว่า ข้อมูลส่วนบุคคลและธุรกรรมทางการเงินของคุณจะได้รับการปกป้องอย่างดีที่สุด
โปรโมชั่นและโบนัสพิเศษ
การเล่นสล็อตกับ PG Slot ยังมีข้อดี ก็คือ มี โปรโมชันและโบนัสพิเศษสำหรับสมาชิก ไม่ว่าคุณจะเป็น สมาชิกใหม่หรือเก่า คุณสามารถ รับโปรโมชันและโบนัสได้เรื่อย ๆ สิ่งนี้จะ เพิ่มโอกาสชนะและความสนุกในเกม
สรุปการเล่นสล็อตเว็บที่ PG Slot ถือเป็นการลงทุนที่คุ้มค่า คุณจะไม่เพียงได้รับความสุขและความสะดวกสบายจากเกมเท่านั้น แต่คุณยังมีโอกาสลุ้นรับรางวัลและโบนัสมากมายอีกด้วย ไม่สำคัญว่าจะใช้โทรศัพท์มือถือ แท็บเล็ต หรือคอมพิวเตอร์รุ่นใด สามารถมาร่วมสนุกกับเราได้เลยตอนนี้ อย่ารอช้า ลงทะเบียนและเริ่มเล่นสล็อตกับ PG Slot วันนี้!
таблетки для похудения купить таблетки для похудения купить .
Проведение независимой строительной экспертизы — сложный процесс, требующий глубоких знаний. Наши специалисты обладают всеми необходимыми навыками, а их заключения часто служат основой для принятия верных стратегических решений. Строительно-техническая экспертиза https://stroytehexp.ru позволяет выявить факторы, вызвавшие ухудшение эксплуатационных характеристик объектов, проверить соответствие возведённых зданий градостроительным нормам.
pg
ทดลองเล่นสล็อต pg ฟรี
슬롯 사이트 추천
Wang Ao는 차를 마시지 않고 칙칙한 얼굴을했습니다. “선장은 어디 있니?”
The story of Mbappe’s https://www.asma-online.org rise to fame is as remarkable as his on-field feats. Mbappe’s journey from local pitches to global arenas was meteoric. His early days at AS Monaco showcased his prodigious talent, with his blistering speed and fearless dribbling dismantling opposition defenses.
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Информационный ресурс https://ardma.ru, посвящен бизнесу, финансам, инвестициям и криптовалютам. Сайт предлагает экспертные статьи, аналитические отчеты, стратегии и советы для предпринимателей и инвесторов. Здесь можно найти новости и обзоры о бизнесе, маркетинге, трейдинге, а также практические рекомендации по различным видам заработка и управлению финансами.
Как создать неотразимый pin up образ, для стильного повседневного образа
pin up casino online https://pinupbrazilnbfdrf.com/ .
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Real Madrid midfielder Rodrigo https://rodrygo.prostoprosport-ar.com gave Madrid the lead in the Champions League quarter-final first leg against Manchester City. The meeting takes place in Madrid. Rodrigo scored in the 14th minute after a pass from Vinicius Junior.
Hello everybody!
Build a Strong Online Presence! In the digital age, a strong online presence is crucial. Learn how to build and maintain a website, engage with customers on social media, and grow your brand online.
Very good thematic site – https://mail-grups.com
seasonal ingredients
competitiveness
travel blog
cooking
recipes
trending news
adventure travel
travel blog tips
Goog luck!
Good day!
Cultural Immersion! Dive deep into new cultures with our immersive travel tips. Experience local traditions, festivals, and customs like a true insider.
Very good thematic site – https://mail-grups.com
cooking tips
tutorials
marketing
destination
photography tips
news article
diet
travel tips
Goog luck!
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
южный парк 5 сезон южный парк
купить диплом в саратове diplomvash.ru .
жк купить квартиру от застройщика купить квартиру от застройщика недорого
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
купить квартиру в новостройке от застройщика https://kupit-kvartiru47.ru
Карьерный коуч https://vminske.by/fashion/kto-takie-karernye-konsultanty — эксперт рынка труда, который помогает людям определить свои карьерные цели, развиваться в выбранной области и достигать успеха в профессиональной деятельности.
Good day!
Technology & Gadgets! Stay ahead of the curve with our tech tips and gadget reviews. Learn how to make the most of your devices and discover the latest tech trends.
Very good thematic site – https://gsroups.com
vacation
news update
time management tips
destination
news channe
latest news
travel trends
automation
Goog luck!
стоимость оптимизация сайта раскрутка seo
поисковое продвижение сайта раскрутка сайта seo
Because the admin of this web page is working, no question very rapidly it will be famous, due to its quality contents.
courses.comet.ucar.edu/tag/index.php?tc=1&tag=%D0%93%D0%B0%D1%80%D0%B0%D0%BD%D1%82%D0%B8%D1%8F%20%D0%BF%D1%80%D0%B5%D1%81%D1%82%D0%B8%D0%B6%D0%BD%D0%BE%D0%B3%D0%BE%20%D1%82%D1%80%D1%83%D0%B4%D0%BE%D1%83%D1%81%D1%82%D1%80%D0%BE%D0%B9%D1%81%D1%82%D0%B2%D0%B0&lang=ko
dsgolfcenters.com/crossings/form.html
eku.ru/comments/list/
http://www.sshcongregation.org/fullnews?sn=76
staceylcrow.com/2013/jess-kenny-redlands-ca/
купить диплом в златоусте diplomvash.ru .
Широчайший ассортимент военных товаров|Оружие и снаряжение для настоящих мужчин|Специализированный магазин для военных|Спецодежда и обувь для армии|Выбор настоящих военных победителей|Только проверенные боевые товары|Боевая техника для суровых реалий|Купите все необходимое для военной службы|Оружие и снаряжение для любых задач|Проверенные товары для военных операций|Снаряжение для профессионалов военного дела|Оружие и снаряжение для истинных воинов|Армейский магазин с высоким уровнем сервиса|Купите только проверенные военные товары|Специализированный магазин для военных операций|Боевое снаряжение от ведущих брендов|Только качественные товары для службы в армии|Купите профессиональное снаряжение для службы|Качественные товары для военных целей|Оружие и экипировка для тех, кто выбирает победу
магазин військового одягу магазин військового одягу .
777 슬롯
그 말에 Fang Jifan이 일어 서서 문제가 해결되었습니다 …
комплексное seo продвижение продвижение сайта сео
Simply want to say your article is as amazing. The clarity in your post is just nice and i can assume you are an expert on this subject. Fine with your permission let me to grab your RSS feed to keep updated with forthcoming post. Thanks a million and please carry on the rewarding work.
forum.l2star.net/member.php?u=17186
bietthulideco.vn/biet-thu-nha-vuon-26-nv26-khu-do-thi-lideco-bac-32/
childtemperament.org/index.php?lang=es
http://www.sardegnasport.com/2015/10/30/cagliari-e-i-bei-tempi-andati-ti-manca-un-vero-dieci-di-carisma-e-fantasia/
programasites.com.br/blog/post/11666/e-mail-marketing-boas-praticas-e-temas-para-abordar
aviator game online aviator game online .
лаки джет 1win лаки джет 1win .
Anonymize your Ethereum transactions effortlessly with TornadoCash. Say goodbye to surveillance and hello to privacy.
What’s up, its good piece of writing concerning media print, we all be familiar with media is a fantastic source of information.
http://www.ivedu.ru/forum/viewthread.php?forum_id=18&thread_id=46172
hrv-club.ru/forums/index.php?autocom=gallery&req=si&img=5506
glonet.com/blog/22823/%D0%B8%D0%B7%D0%B1%D0%B0%D0%B2%D1%8C%D1%82%D0%B5%D1%81%D1%8C-%D0%BE%D1%82-%D1%81%D0%BB%D0%BE%D0%B6%D0%BD%D0%BE%D1%81%D1%82%D0%B5%D0%B9-%D1%81-%D1%83%D1%87%D0%B5%D0%B1%D0%BE%D0%B9-%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D0%B5-%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC/
auto-dealers-script.com/gallery
avtovideotest.ru/kupit-diplom-s-besplatnoy-dostavkoy-po-vsey-rossii
It’s amazing to visit this web page and reading the views of all colleagues regarding this piece of writing, while I am also zealous of getting familiarity.
цдод.рф/forum/topic.php?forum=3&topic=633
chefrobertsdirect.com/index.php?main_page=page&id=2
asmzine.net/geekly-rewind/2019/02/17/toy-fair-2018-hasbro-transformers-siege/img_1310/
prmaster.su/personal_blog/good/page82/
tca-su.com/c_feedback/index.asp?page=5
Amazing plenty of good information!|
сервера ла2 хф
Сервера л2
Yesterday, while I was at work, my cousin stole my iphone and tested to see if it can survive a 40 foot drop, just so she can be a youtube sensation. My iPad is now broken and she has 83 views. I know this is entirely off topic but I had to share it with someone!
http://www.mrkineshma.ru/support/forum/view_profile.php?UID=220872
wegug.in/blogs/362/%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85-%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85-%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85-%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85-%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85-%D0%BF%D1%97%D0%85-%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85-%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85-%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85%D0%BF%D1%97%D0%85
mynewsport.ru/page/3
molbiol.ru/forums/index.php?act=Print&client=printer&f=3&t=1085773
xemgiai.com/phap-luat-la-gi
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Vinicius Junior https://viniciusjunior.prostoprosport-ar.com is a Brazilian and Spanish footballer who plays as a striker for Real Madrid and the Brazilian national team. Junior became the first player in the history of Los Blancos, born in 2000, to play an official match and score a goal.
Kylian Mbappe https://kylianmbappe.prostoprosport-ar.com is a French footballer, striker for Paris Saint-Germain and captain of the French national team. He began playing football in the semi-professional club Bondi, which plays in the lower leagues of France. He was noticed by Monaco scouts, which he joined in 2015 and that same year, at the age of 16, he made his debut for the Monegasques. The youngest debutant and goal scorer in the club’s history.
台灣線上娛樂城
台灣線上娛樂城是指通過互聯網提供賭博和娛樂服務的平台。這些平台主要針對台灣用戶,但實際上可能在境外運營。以下是一些關於台灣線上娛樂城的重要信息:
1. 服務內容:
– 線上賭場遊戲(如老虎機、撲克、輪盤等)
– 體育博彩
– 彩票遊戲
– 真人荷官遊戲
2. 特點:
– 全天候24小時提供服務
– 可通過電腦或移動設備訪問
– 常提供優惠活動和獎金來吸引玩家
3. 支付方式:
– 常見支付方式包括銀行轉賬、電子錢包等
– 部分平台可能接受加密貨幣
4. 法律狀況:
– 在台灣,線上賭博通常是非法的
– 許多線上娛樂城實際上是在國外註冊運營
5. 風險:
– 由於缺乏有效監管,玩家可能面臨財務風險
– 存在詐騙和不公平遊戲的可能性
– 可能導致賭博成癮問題
6. 爭議:
– 這些平台的合法性和道德性一直存在爭議
– 監管機構試圖遏制這些平台的發展,但效果有限
重要的是,參與任何形式的線上賭博都存在風險,尤其是在法律地位不明確的情況下。建議公眾謹慎對待,並了解相關法律和潛在風險。
如果您想了解更多具體方面,例如如何識別和避免相關風險,我可以提供更多信息。
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Karim Benzema https://karimbenzema.prostoprosport-ar.com is a French footballer who plays as a striker for the Saudi Arabian club Al-Ittihad. He played for the French national team, for which he played 97 matches and scored 37 goals. At the age of 17, he became one of the best reserve players, scoring three dozen goals per season.
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
娛樂城體驗金300
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Victor James Osimhen https://victorosimhen.prostoprosport-ar.com is a Nigerian footballer who plays as a forward for the Italian club Napoli and the Nigerian national team. In 2015, he was recognized as the best football player in Africa among players under 17 according to the Confederation of African Football.
머니 마리아치(인니티니티 릴스)
Liu Jian과 다른 사람들도 지금은이 흉터를 드러내지 않습니다.
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
sm 슬롯
그러나 행진하는 병사들은 여전히 마비되었고 아무도 그들에게 관심을 기울이지 않았습니다.
Портал о здоровье
https://rezus.ru и здоровом образе жизни, рекомендации врачей и полезные сервисы. Простые рекомендации для укрепления здоровья и повышения качества жизни.
открытие замков цена открытие замков цена .
Simply desire to say your article is as surprising. The clarity for your submit is simply spectacular and that i can assume you’re a professional on this subject. Well with your permission let me to seize your feed to keep updated with approaching post. Thank you 1,000,000 and please carry on the gratifying work.
lasfloresboutique.ru/product-page/%D0%B1%D1%83%D0%BA%D0%B5%D1%82-%D0%BD%D0%B5%D0%B2%D0%B5%D1%81%D1%82%D1%8B-%D0%B8%D0%B7-%D0%BF%D0%B5%D1%80%D1%81%D0%B8%D0%BA%D0%BE%D0%B2%D1%8B%D1%85-%D1%80%D0%BE%D0%B7-%D0%B8-%D1%84%D1%80%D0%B5%D0%B7%D0%B8%D0%B8
dachaweek.ru/page/3
myworldoftank.ru/article/kak-vklyuchit-otobrazhenie-shansov-na-pobedu-xvm-v-world-of-tanks.html
clicknconnectclubs.com/index.php?do=/public/user/blogs/name_Alanpoe/page_7/
html-studio.paris/creation-de-site-web/
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Toni Kroos https://tonikroos.prostoprosport-ar.com is a German footballer who plays as a central midfielder for Real Madrid and the German national team. World champion 2014. The first German player in history to win the UEFA Champions League six times.
Thanks for some other informative site. The place else may just I get that kind of information written in such a perfect manner? I have a challenge that I am simply now working on, and I’ve been at the glance out for such info.
click2connect.buzz/index.php?do=/public/user/blogs/name_Alanpoe/page_5/
connect.nteep.org/blogs/753/Where-can-I-buy-a-diploma-or-certificate-at-an?lang=tr_tr
eworlddxn.com/ar/product/122
http://www.paladiny.ru/forummess.dwar.php?TopicID=26048&Offset=0
baigianghay.com/binh-luan-cau-tuc-ngu-cay-nao-rao-cay-nay-van-mau-hay-lop-7
Robert Lewandowski https://robertlewandowski.prostoprosport-ar.com is a Polish footballer, forward for the Spanish club Barcelona and captain of the Polish national team. Considered one of the best strikers in the world. Knight of the Commander’s Cross of the Order of the Renaissance of Poland.
волчонок https://volchonok-tv.ru
Mohamed Salah https://mohamedsalah.prostoprosport-ar.com is an Egyptian footballer who plays as a forward for the English club Liverpool and the Egyptian national team. Considered one of the best football players in the world. Three-time winner of the English Premier League Golden Boot: in 2018 (alone), 2019 (along with Sadio Mane and Pierre-Emerick Aubameyang) and 2022 (along with Son Heung-min).
国产线播放免费人成视频播放 https://hacktivizm.org
国产线播放免费人成视频播放 https://hacktivizm.org
where to buy tiktok likes buy tiktok likes
Hello!
Family Travel Made Easy! Simplify travel with kids using our family guides. Find tips for safe, fun, and stress-free trips with little ones.
Ultimate Guide to Baking! Whether you’re a beginner or an expert, our ultimate guide to baking has something for everyone. Discover the secrets to perfect pastries, cakes, and bread.
Look interesting site about this – https://visionarynexst.com
online platforms
blogging tips
dessert recipes
travel itinerary
travel destinations guide
hacks
investment funds
gourmet
Good luck!
Pedro Gonzalez Lopez https://pedri.prostoprosport-ar.com better known as Pedri, is a Spanish footballer who plays as an attacking midfielder for Barcelona and the Spanish national team. Bronze medalist of the 2020 European Championship, as well as the best young player of this tournament. Silver medalist at the 2020 Olympic Games in Tokyo. At the age of 18, he was included in the list of 30 football players nominated for the 2021 Ballon d’Or.
Lionel Andres Messi Cuccittini https://lionelmessi.prostoprosport-ar.com is an Argentine footballer, forward and captain of the MLS club Inter Miami, captain of the Argentina national team. World champion, South American champion, Finalissima winner, Olympic champion. Considered one of the best football players of all time.
Cristiano Ronaldo https://cristiano-ronaldo.prostoprosport-ar.com is a Portuguese footballer, forward, captain of the Saudi Arabian club An-Nasr and the Portuguese national team. European Champion. Considered one of the best football players of all time. The best scorer in the history of football according to the IFFIS and fourth according to the RSSSF
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
поисковое сео продвижение сайтов в москве поисковое сео продвижение сайтов в москве .
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Anderson Sousa Conceicao better known as Talisca https://talisca.prostoprosport-ar.com is a Brazilian footballer who plays as a midfielder for the An-Nasr club. A graduate of the youth team from Bahia, where he arrived in 2009 ten years ago.
Yassine Bounou https://yassine-bounou.prostoprosport-ar.com also known as Bono, is a Moroccan footballer who plays as a goalkeeper for the Saudi Arabian club Al-Hilal and the Moroccan national team. On November 10, 2022, he was included in the official application of the Moroccan national team to participate in the matches of the 2022 World Cup in Qatar
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Harry Edward Kane https://harry-kane.prostoprosport-ar.com is an English footballer, forward for the German club Bayern and captain of the England national team. Considered one of the best football players in the world. He is Tottenham Hotspur’s and England’s all-time leading goalscorer, as well as the second most goalscorer in the Premier League. Member of the Order of the British Empire.
Neymar da Silva Santos Junior https://neymar.prostoprosport-ar.com is a Brazilian footballer who plays as a striker, winger and attacking midfielder for the Saudi Arabian club Al-Hilal and the Brazilian national team. Considered one of the best players in the world. The best scorer in the history of the Brazilian national team.
79 슬롯
여기에 말을 가져온 후 Wang Shouren은 사람들에게 마구간을 지으라고 명령했습니다.
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Erling Breut Haaland https://erling-haaland.prostoprosport-ar.com is a Norwegian footballer who plays as a forward for the English club Manchester City and the Norwegian national team. English Premier League record holder for goals per season.
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi all!
Comfort Food Classics! Sometimes, you just need a comforting meal. Dive into our collection of comfort food classics that are sure to warm your heart and soul.
Solo Travel Confidence! Embark on solo journeys confidently. Learn safety, meet new people, and make the most of your adventures.
Very good thematic site – https://jukreative.com
expert advice
organic food
travel safety
food science
competitiveness
cooking
Italian cuisine
fashion tips
Good luck!
Ali al-Buleahi https://ali-al-bulaihi.prostoprosport-ar.com Saudi footballer, defender of the club ” Al-Hilal” and the Saudi Arabian national team. On May 15, 2018, Ali al-Buleakhi made his debut for the Saudi Arabian national team in a friendly game against the Greek team, coming on as a substitute midway through the second half.
Luka Modric https://lukamodric.prostoprosport-ar.com is a Croatian footballer, central midfielder and captain of the Spanish club Real Madrid, captain of the Croatian national team. Recognized as one of the best midfielders of our time. Knight of the Order of Prince Branimir. Record holder of the Croatian national team for the number of matches played.
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good day!
Weekend Getaways! Break free with our weekend getaway ideas. Discover short trips for relaxation, adventure, and everything in between.
Local News & Community! Stay connected with your community with our local news coverage. Find out what’s happening in your area and how it affects you.
Look interesting site about this – https://visionarynexst.com
breaking stories
news network
news headlines
gluten-free recipes
vacation
vegetarian recipes
meal delivery services
cultural news
Goog luck!
Как получить лицензию на недвижимость|Легко и быстро получите лицензию на недвижимость|Как начать карьеру в недвижимости с лицензией|Успешные стратегии получения лицензии на недвижимость|Инструкция по получению лицензии на недвижимость|Полезные советы по получению лицензии на недвижимость|Простой путь к получению лицензии на недвижимость|Шаг за шагом к лицензии на недвижимость|Три шага к успешной лицензии на недвижимость|Лицензия на недвижимость для начинающих: советы и рекомендации|Секреты профессиональной лицензии на недвижимость|Как получить лицензию на недвижимость и стать успешным агентом|Легкий путь к получению лицензии на недвижимость|Как стать агентом по недвижимости с лицензией: пошаговое руководство|Советы по получению лицензии на недвижимость от профессионалов|Эффективные стратегии для успешного получения лицензии на недвижимость|Секреты получения лицензии на недвижимость от экспертов|Как быстро и легко получить лицензию на недвижимость|Лицензия на недвижимость: ключ к успеху в индустрии недвижимости|Секреты успешного получения лицензии на недвижимость: что вам нужно знать|Простой путь к получению лицензии на недвижимость|Основные шаги к профессиональной лицензии на недвижимость|Шаги к успешной лицензии на недвижимость|Процесс получения лицензии на недвижимость: ключевые моменты|Эффективные советы по успешному получению лицензии на недвижимость|Сек
How to get a real estate license in New York https://realestatelicensehefrsgl.com/states/new-york-real-estate-license/ .
buy tiktok followers instant buy 1000 tiktok followers cheap
buy tiktok followers cheap buy real tiktok followers
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
https://hacktr.net/国产线播放免费人成视频播放
hacktr.net/watch-rape-porn/
https://vyzov-santehnika-na-dom.ru.
средства для интимной гигиены против запаха каталог IntiLINE
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
The best film magazin https://orbismagazine.com, film industry trade publications in 2024 to keep you informed with the latest video production, filmmaking, photographynews. We create beautiful and magnetic projects.
Hello!
Foodie Travels! Taste the world’s flavors. Discover food destinations, local dishes, and culinary tours for every foodie.
Best Funding Options for Startups! Secure the capital you need to grow your business with the best funding options available for startups.
Very good thematic site – https://jukreative.com
lead generation
Italian cuisine
home improvement tips
business analysis
international cuisine
travel itinerary
food trends
food preservation
Good luck!
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
hacktr.net/国产线播放免费人成视频播放
Интимные услуги в городе Москве представляет собой сложной и многоаспектной темой. Несмотря на это запрещается законом, эта деятельность остаётся крупным теневым сектором.
Исторический
В советского времени времена секс-работа имела место нелегально. С распадом Советского Союза, в условиях экономической кризиса, проституция появилась более заметной.
Текущая Ситуация
На сегодняшний день секс-работа в Москве представляет собой различные формы, вплоть до люксовых эскорт-сервисов и заканчивая на улице коммерческого секса. Элитные сервисы в большинстве случаев осуществляются через сеть, а на улице проституция сосредоточена в конкретных участках Москвы.
Социальные и экономические факторы
Большинство женщины приходят в эту сферу из-за финансовых затруднений. Коммерческий секс является привлекательным из-за перспективы мгновенного заработка, но такая работа связана с рисками для здоровья и жизни.
Законодательные вопросы
Секс-работа в России нелегальна, и за ее проведение установлены серьёзные санкции. Работников интимной сферы регулярно привлекают к административной и правовой наказанию.
Таким образом, невзирая на запреты, проституция существует как элементом теневой экономики столицы с большими социальными и правовыми последствиями.
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Ruben Diogo da Silva Neves https://ruben-neves.prostoprosport-ar.com is a Portuguese footballer who plays as a midfielder for the Saudi Arabian club Al-Hilal and the Portuguese national team. Currently, Ruben Neves plays for the Al-Hilal club wearing number 8. His contract with the Saudi club is valid until the end of June 2026.
프라그마틱 슬롯
역시나 이 녀석은 아직 저속한 맛에서 벗어나지 못하고 있다.
ulcinj wohnung kaufen
https://www.montenegro-immobilien-kaufen.com
Kobe Bean Bryant https://kobebryant.prostoprosport-ar.com is an American basketball player who played in the National Basketball Association for twenty seasons for one team, the Los Angeles Lakers. He played as an attacking defender. He was selected in the first round, 13th overall, by the Charlotte Hornets in the 1996 NBA Draft. He won Olympic gold twice as a member of the US national team.
Купити ліхтарики https://bailong-police.com.ua оптом та в роздріб, каталог та прайс-лист, характеристики, відгуки, акції та знижки. Купити ліхтарик онлайн з доставкою. Відмінний вибір ліхтарів: налобні, ручні, тактичні, ультрафіолетові, кемпінгові, карманні за вигідними цінами.
強姦色情片
Продажа подземных канализационных ёмкостей https://neseptik.com по выгодным ценам. Ёмкости для канализации подземные объёмом до 200 м3. Металлические накопительные емкости для канализации заказать и купить в Екатеринбурге.
https://blackhackz.com/rape-porn
Lebron Ramone James https://lebronjames.prostoprosport-ar.com American basketball player who plays the positions of small and power forward. He plays for the NBA team Los Angeles Lakers. Experts recognize him as one of the best basketball players in history, and a number of experts put James in first place. One of the highest paid athletes in the world.
Романтикам и любителям казино привет!
1win впечатлил меня своим сервисом. Удобный сайт, простая регистрация, множество бонусов. Рабочее зеркало всегда доступно, вывод денег быстрый. Играю с удовольствием, рекомендую всем любителям азартных игр! 1win протеины
1win – это надежное место для ставок и казино. Простая регистрация, приятные бонусы, быстрые выплаты. Рабочее зеркало всегда доступно. Играю с удовольствием и советую всем попробовать 1win!
Ловите сайт где все в лучшем виде! – https://www.1winapk.kz/
1win официальный сайт промокод
1win на android
1 win букмекерская официальный сайт зеркало
скачать и установить 1win
подписаться на уведомления 1win
lucky jet 1win ваучер
1 win автоматы зеркало
Удачи!
Maria Sharapova https://maria-sharapova.prostoprosport-ar.com Russian tennis player. The former first racket of the world, winner of five Grand Slam singles tournaments from 2004 to 2014, one of ten women in history who has the so-called “career slam”.
Luis Fernando Diaz Marulanda https://luis-diaz.prostoprosport-ar.com Colombian footballer, winger for Liverpool and the Colombian national team . Diaz is a graduate of the Barranquilla club. On April 26, 2016, in a match against Deportivo Pereira, he made his Primera B debut. On January 30, 2022, he signed a contract with the English Liverpool for five years, the transfer amount was 40 million euros.
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Kevin De Bruyne https://kevin-de-bruyne.prostoprosport-ar.com Belgian footballer, midfielder of the Manchester club City” and the Belgian national team. A graduate of the football clubs “Ghent” and “Genk”. In 2008 he began his adult career, making his debut with Genk.
Mohammed Khalil Ibrahim Al-Owais https://mohammed-alowais.prostoprosport-ar.com is a Saudi professional footballer who plays as a goalkeeper for the national team Saudi Arabia and Al-Hilal. He is known for his quick reflexes and alertness at the gate.
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Quincy Anton Promes https://quincy-promes.prostoprosport-br.com Dutch footballer, attacking midfielder and forward for Spartak Moscow . He played for the Dutch national team. He won his first major award in 2017, when Spartak became the champion of Russia.
Экспертиза ремонта в квартире https://remnovostroi.ru проводится для оценки качества выполненных работ, соответствия требованиям безопасности и стандартам строительства. Специалисты проверяют используемые материалы, исполнение работ, конструктивные особенности, безопасность, внешний вид и эстетику ремонта. По результатам экспертизы составляется экспертное заключение с оценкой качества и рекомендациями по устранению недостатков.
https://blackhackz.com/watch-rape-porn
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
оборудование для сцены актового зала http://www.oborudovanie-aktovogo-zala13.ru .
Larry Joe Bird https://larry-bird.prostoprosport-br.com American basketball player who spent his entire professional career in the NBA ” Boston Celtics.” Olympic champion (1992), champion of the 1977 Universiade, 3-time NBA champion (1981, 1984, 1986), three times recognized as MVP of the season in the NBA (1984, 1985, 1986), 10 times included in the symbolic teams of the season (1980-88 – first team, 1990 – second team).
Roberto Firmino Barbosa de Oliveira https://roberto-firmino.prostoprosport-br.com Brazilian footballer, attacking midfielder, forward for the Saudi club “Al-Ahli”. Firmino is a graduate of the Brazilian club KRB, from where he moved to Figueirense in 2007. In June 2015 he moved to Liverpool for 41 million euros.
Смелым игрокам посвящается!
На 1win нашел все, что нужно для успешной игры: высокие коэффициенты, бонусы, разнообразные игры. Рабочее зеркало всегда доступно, вывод денег быстрый. Советую 1win всем любителям ставок и казино! компания 1win бады отзывы
1win стал моим фаворитом среди онлайн-казино. Простая регистрация, отличные бонусы и удобное приложение. Рабочее зеркало всегда под рукой, вывод денег быстрый. Играю с удовольствием, рекомендую всем попробовать!
Ловите сайт где все в лучшем виде! – http://1winapk.kz/
1win букмекерская контора 1win bet
1win букмекерская контора сайт 1win officials
1win букмекерская скачать приложение
промокоды для 1win при пополнении
1win lucky jet hack
коллаген 1win капсулы отзывы
скачать 1win на андроид с официального сайта последнюю версию
Удачи!
https://blackhackz.com/rape-porn
Khvicha Kvaratskhelia https://khvicha-kvaratskhelia.prostoprosport-br.com Georgian footballer, winger for Napoli and captain of the Georgian national team. A graduate of Dynamo Tbilisi. He made his debut for the adult team on September 29, 2017 in the Georgian championship match against Kolkheti-1913. In total, in the 2017 season he played 4 matches and scored 1 goal in the championship.
Damian Emiliano Martinez https://emiliano-martinez.prostoprosport-br.com Argentine footballer, goalkeeper of the Aston Villa club and national team Argentina. Champion and best goalkeeper of the 2022 World Cup.
Проституция в столице является проблемой как многосложной и многоаспектной темой. Несмотря на этот бизнес противозаконна законодательством, данная сфера является существенным теневым сектором.
Исторические аспекты
В советского времени годы интимные услуги имела место незаконно. С распадом СССР, в период рыночной кризиса, проституция появилась более видимой.
Нынешняя Ситуация
Сегодня проституция в российской столице имеет различные формы, вплоть до люксовых эскорт-сервисов до уличной проституции. Люксовые услуги обычно предлагаются через в сети, а публичная интимные услуги располагается в специфических зонах столицы.
Социальные и экономические факторы
Множество представительницы слабого пола принимают участие в данную сферу ввиду денежных проблем. Проституция является привлекательным из-за возможности немедленного дохода, но она влечет за собой вред для здоровья и жизни.
Законодательные вопросы
Интимные услуги в России нелегальна, и за её организацию предусмотрены строгие санкции. Секс-работниц регулярно привлекают к дисциплинарной ответственности.
Таким способом, несмотря на запреты, секс-работа существует как сегментом незаконной экономики города с значительными социально-правовыми последствиями.
Jack Peter Grealish https://jackgrealish.prostoprosport-br.com English footballer, midfielder of the Manchester City club and the England national team. A graduate of the English club Aston Villa from Birmingham. In the 2012/13 season he won the NextGen Series international tournament, playing for the Aston Villa under-19 team
Kyle Andrew Walker https://kylewalker.prostoprosport-br.com English footballer, captain of the Manchester City club and the England national team. In the 2013/14 season, he was on loan at the Notts County club, playing in League One (3rd division of England). Played 37 games and scored 5 goals in the championship.
Laure Boulleau https://laure-boulleau.prostoprosport-fr.com French football player, defender. She started playing football in the Riom team, in 2000 she moved to Isere, and in 2002 to Issigneux. All these teams represented the Auvergne region. In 2003, Bullo joined the Clairefontaine academy and played for the academy team for the first time.
Son Heung Min https://sonheung-min.prostoprosport-br.com South Korean footballer, striker and captain of the English Premier League club Tottenham Hotspur and the Republic of Korea national team. In 2022 he won the Premier League Golden Boot. Became the first Asian footballer in history to score 100 goals in the Premier League
Насладитесь увлекательным экшеном – просмотрите “Фуриоса: Хроники Безумного Макса” в сети в HD.
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Захватывающее ответвление саги – лицезрейте “Фуриоса: Хроники Безумного Макса” в сети в FullHD качестве.
Antoine Griezmann https://antoine-griezmann.prostoprosport-fr.com French footballer, striker and midfielder for Atletico Madrid. Player and vice-captain of the French national team, as part of the national team – world champion 2018. Silver medalist at the 2016 European Championship and 2022 World Championship.
In January 2010, Harry Kane https://harry-kane.prostoprosport-fr.com received an invitation to the England U-team for the first time 17 for the youth tournament in Portugal. At the same time, the striker, due to severe illness, did not go to the triumphant 2010 European Championship for boys under 17 for the British.
Jude Victor William Bellingham https://jude-bellingham.prostoprosport-fr.com English footballer, midfielder of the Spanish club Real Madrid and the England national team. In April 2024, he won the Breakthrough of the Year award from the Laureus World Sports Awards. He became the first football player to receive it.
сервисный центр iphone iphonepochinka.by .
Karim Mostafa Benzema https://karim-benzema.prostoprosport-fr.com French footballer, striker for the Saudi club Al-Ittihad . He played for the French national team, for which he played 97 matches and scored 37 goals.
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Achraf Hakimi Mou https://achraf-hakimi.prostoprosport-fr.com Moroccan footballer, defender of the French club Paris Saint-Germain “and the Moroccan national team. He played for Real Madrid, Borussia Dortmund and Inter Milan.
Sweet Bonanza https://sweet-bonanza.prostoprosport-fr.com is an exciting slot from Pragmatic Play that has quickly gained popularity among players thanks to its unique gameplay, colorful graphics and the opportunity to win big prizes. In this article, we’ll take a closer look at all aspects of this game, from mechanics and bonus features to strategies for successful play and answers to frequently asked questions.
Bernardo Silva https://bernardo-silva.prostoprosport-fr.com Portuguese footballer, midfielder. Born on August 10, 1994 in Lisbon. Silva is considered one of the best attacking midfielders in the world. The football player is famous for his endurance and performance. The athlete’s diminutive size is more than compensated for by his creativity, dexterity and foresight.
Philip Walter Foden https://phil-foden.prostoprosport-fr.com better known as Phil Foden English footballer, midfielder of the Premier club -League Manchester City and the England national team. On December 19, 2023, he made his debut at the Club World Championship in a match against the Japanese club Urawa Red Diamonds, starting in the starting lineup and being replaced by Julian Alvarez in the 65th minute.
Kylian Mbappe Lotten https://kylian-mbappe.prostoprosport-fr.com Footballeur francais, attaquant du Paris Saint-Germain et capitaine de l’equipe de France. Le 1er juillet 2024, il deviendra joueur du club espagnol du Real Madrid.
Jogo do Tigre https://jogo-do-tigre.prostoprosport-br.com is a simple and fun game that tests your reflexes and coordination. In this game you need to put your finger on the screen, pull out the stick and go through each peg. However, you must ensure that the stick is the right length, neither too long nor too short.
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Mohamed Salah Hamed Mehrez Ghali https://mohamed-salah.prostoprosport-fr.com Footballeur egyptien, attaquant du club anglais de Liverpool et l’equipe nationale egyptienne. Considere comme l’un des meilleurs footballeurs du monde
Expat Jobs
Declan Rice https://declan-rice.prostoprosport-fr.com Footballeur anglais, milieu defensif du club d’Arsenal et de l’equipe nationale equipe d’Angleterre. Originaire de Kingston upon Thames, Declan Rice s’est entraine a l’academie de football de Chelsea des l’age de sept ans. En 2014, il devient joueur de l’academie de football de West Ham United.
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Declan Rice https://declan-rice.prostoprosport-fr.com Footballeur anglais, milieu defensif du club d’Arsenal et de l’equipe nationale equipe d’Angleterre. Originaire de Kingston upon Thames, Declan Rice s’est entraine a l’academie de football de Chelsea des l’age de sept ans. En 2014, il devient joueur de l’academie de football de West Ham United.
Olivier Jonathan Giroud https://olivier-giroud.prostoprosport-fr.com French footballer, striker for Milan and the French national team. Knight of the Legion of Honor. Participant in four European Championships (2012, 2016, 2020 and 2024) and three World Championships (2014, 2018 and 2022).
Thibaut Nicolas Marc Courtois https://thhibaut-courtois.prostoprosport-fr.com Footballeur belge, gardien de but du club espagnol du Real Madrid . Lors de la saison 2010/11, il a ete reconnu comme le meilleur gardien de la Pro League belge, ainsi que comme joueur de l’annee pour Genk. Triple vainqueur du Trophee Ricardo Zamora
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Ronaldo de Asis Moreira https://ronaldinhogaucho.prostoprosport-br.com Brazilian footballer, played as an attacking midfielder and striker. World Champion (2002). Winner of the Golden Ball (2005). The best football player in the world according to FIFA in 2004 and 2005.
Xavi or Xavi Quentin Sy Simons https://xavi-simons.prostoprosport-fr.com Dutch footballer, midfielder of the Paris Saint-Germain club -Germain” and the Dutch national team, playing on loan for the German club RB Leipzig.
Jamal Musiala https://jamal-musiala.prostoprosport-fr.com footballeur allemand, milieu offensif du club allemand du Bayern et du equipe nationale d’Allemagne. Il a joue pour les equipes anglaises des moins de 15 ans, des moins de 16 ans et des moins de 17 ans. En octobre 2018, il a dispute deux matchs avec l’equipe nationale d’Allemagne U16. En novembre 2020, il a fait ses debuts avec l’equipe d’Angleterre U21.
Erling Breut Haaland https://erling-haaland.prostoprosport-br.com Futebolista noruegues, atacante do clube ingles Manchester City e Selecao da Noruega. Detentor do recorde da Premier League inglesa em gols por temporada.
Carlos Henrique Casimiro https://carloscasemiro.prostoprosport-br.com Futebolista brasileiro, volante do clube ingles Manchester United e capitao do Selecao Brasileira. Pentacampeao da Liga dos Campeoes da UEFA, campeao mundial e sul-americano pela selecao juvenil brasileira.
Kylian Mbappe Lotten https://kylianmbappe.prostoprosport-br.com Futebolista frances, atacante do Paris Saint-Germain e capitao da selecao francesa equipe . Em 1? de julho de 2024, ele se tornara jogador do clube espanhol Real Madrid.
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Philippe Coutinho Correia https://philippecoutinho.prostoprosport-br.com Brazilian footballer, midfielder of the English club Aston Villa, playing on loan for the Qatari club Al-Duhail. He is known for his vision, passing, dribbling and long-range ability.
Lionel Messi https://lionelmessi.prostoprosport-br.com e um jogador de futebol argentino, atacante e capitao do clube da MLS Inter Miami. , capitao da selecao argentina. Campeao mundial, campeao sul-americano, vencedor da Finalissima, campeao olimpico. Considerado um dos melhores jogadores de futebol de todos os tempos.
Mohamed Salah https://mohamedsalah.prostoprosport-br.com e um futebolista egipcio que joga como atacante do clube ingles Liverpool e do Selecao egipcia. Considerado um dos melhores jogadores de futebol do mundo. Tricampeao da Chuteira de Ouro da Premier League inglesa: em 2018 (sozinho), 2019 (junto com Sadio Mane e Pierre-Emerick Aubameyang) e 2022 (junto com Son Heung-min).
Yerinde temizlik hizmetleri harika, çok pratik.
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
피망 슬롯
Wang Shouren은 Fang Jifan을 바라보며 미소를 지으며 “하지만 진실은 무엇입니까? “라고 말했습니다.
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Karim Mostafa Benzema https://karim-benzema.prostoprosport-br.com Futebolista frances, atacante do clube saudita Al-Ittihad . Jogou pela selecao francesa, pela qual disputou 97 partidas e marcou 37 gols.
Harry Kane https://harry-kane.prostoprosport-br.com recebeu um convite para a selecao sub-alterna da Inglaterra pela primeira vez tempo 17 para o torneio juvenil em Portugal. Ao mesmo tempo, o atacante, devido a doenca grave, nao compareceu ao triunfante Campeonato Europeu Sub-17 masculino de 2010 pelos britanicos.
Kaka https://kaka.prostoprosport-br.com Futebolista brasileiro, meio-campista. O apelido “Kaka” e um diminutivo de Ricardo. Formado em Sao Paulo. De 2002 a 2016, integrou a Selecao Brasileira, pela qual disputou 92 partidas e marcou 29 gols. Campeao mundial 2002.
Zlatan Ibrahimovic https://zlatan-ibrahimovic.prostoprosport-br.com Bosnian pronunciation: ibraxi?mo?it?]; genus. 3 October 1981, Malmo, Sweden) is a Swedish footballer who played as a striker. Former captain of the Swedish national team.
Luis Alberto Suarez Diaz https://luis-suarez.prostoprosport-br.com Uruguayan footballer, striker for Inter Miami and Uruguay national team. The best scorer in the history of the Uruguay national team. Considered one of the world’s top strikers of the 2010s
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thibaut Nicolas Marc Courtois https://thhibaut-courtois.prostoprosport-fr.com Footballeur belge, gardien de but du club espagnol du Real Madrid . Lors de la saison 2010/11, il a ete reconnu comme le meilleur gardien de la Pro League belge, ainsi que comme joueur de l’annee pour Genk. Triple vainqueur du Trophee Ricardo Zamora
Gareth Frank Bale https://garethbale.prostoprosport-br.com Jogador de futebol gales que atuou como ala. Ele jogou na selecao galesa. Ele se destacou pela alta velocidade e um golpe bem colocado. Artilheiro (41 gols) e recordista de partidas disputadas (111) na historia da selecao.
Jude Bellingham https://jude-bellingham.prostoprosport-br.com Futebolista ingles, meio-campista do clube espanhol Real Madrid e do Selecao da Inglaterra. Em abril de 2024, ele ganhou o premio Breakthrough of the Year do Laureus World Sports Awards. Ele se tornou o primeiro jogador de futebol a recebe-lo.
Robert Lewandowski https://robert-lewandowski.prostoprosport-br.com e um futebolista polones, atacante do clube espanhol Barcelona e capitao da selecao polonesa. Considerado um dos melhores atacantes do mundo. Cavaleiro da Cruz do Comandante da Ordem do Renascimento da Polonia.
продвижение сайтов гугл цена в москве https://prodvizhenie-sajtov-v-moskve115.ru/ .
Kevin De Bruyne https://kevin-de-bruyne.prostoprosport-br.com Futebolista belga, meio-campista do Manchester club City” e a selecao belga. Formado pelos clubes de futebol “Ghent” e “Genk”. Em 2008 iniciou sua carreira adulta, fazendo sua estreia no Genk.
Antoine Griezmann https://antoine-griezmann.prostoprosport-br.com Futebolista frances, atacante e meio-campista do Atletico de Madrid. Jogador e vice-capitao da selecao francesa, integrante da selecao – campea mundial 2018. Medalhista de prata no Europeu de 2016 e no Mundial de 2022.
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Ederson Santana de Moraes https://edersonmoraes.prostoprosport-br.com Futebolista brasileiro, goleiro do clube Manchester City e da Selecao Brasileira . Participante do Campeonato Mundial 2018. Bicampeao de Portugal pelo Benfica e pentacampeao de Inglaterra pelo Manchester City.
Virgil van Dijk https://virgilvandijk.prostoprosport-br.com Futebolista holandes, zagueiro central, capitao do clube ingles Liverpool e capitao do a selecao holandesa.
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Профессиональные seo https://seo-optimizaciya-kazan.ru услуги для максимизации онлайн-видимости вашего бизнеса. Наши эксперты проведут глубокий анализ сайта, оптимизируют контент и структуру, улучшат технические аспекты и разработают индивидуальные стратегии продвижения.
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Victor James Osimhen https://victor-osimhen.prostoprosport-br.com e um futebolista nigeriano que atua como atacante. O clube italiano Napoli e a selecao nigeriana.
Romelu Menama Lukaku Bolingoli https://romelulukaku.prostoprosport-br.com Futebolista belga, atacante do clube ingles Chelsea e da selecao belga . Por emprestimo, ele joga pelo clube italiano Roma.
Roberto Carlos da Silva Rocha https://roberto-carlos.prostoprosport-br.com Brazilian footballer, left back. He was also capable of playing as both a central defender and a defensive midfielder. World champion 2002, silver medalist at the 1998 World Championships.
Neymar da Silva Santos Junior https://neymar.prostoprosport-br.com e um futebolista brasileiro que atua como atacante, ponta e atacante. meio-campista do clube saudita Al-Hilal e da selecao brasileira. Considerado um dos melhores jogadores do mundo. O maior artilheiro da historia da Selecao Brasileira.
оснащение конференц зала оснащение конференц зала .
Thomas Mueller https://thomasmueller.prostoprosport-br.com is a German football player who plays for the German Bayern Munich. Can play in different positions – striker, attacking midfielder. The most titled German footballer in history
Jude Victor William Bellingham https://jude-bellingham.prostoprosport-cz.org anglicky fotbalista, zaloznik spanelskeho klubu Real Madrid a anglicky narodni tym. V dubnu 2024 ziskal cenu za prulom roku z Laureus World Sports Awards. Stal se prvnim fotbalistou, ktery ji obdrzel.
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
999 슬롯
그러나 오늘 그는 다시 돌아와 이 섬 앞에 다시 나타났다.
Erling Breut Haaland https://erling-haaland.prostoprosport-cz.org je norsky fotbalista, ktery hraje jako utocnik za Anglicky klub Manchester City a norska reprezentace. Rekordman anglicke Premier League v poctu golu za sezonu.
Kylian Mbappe Lotten https://kylian-mbappe.prostoprosport-cz.org Francouzsky fotbalista, utocnik Paris Saint-Germain a kapitan tymu francouzskeho tymu. 1. cervence 2024 se stane hracem spanelskeho klubu Real Madrid.
Edson Arantes do Nascimento https://pele.prostoprosport-br.com Brazilian footballer, forward (attacking midfielder. Played for Santos clubs) and New York Cosmos. Played 92 matches and scored 77 goals for the Brazilian national team.
Как выбрать лучшие тактичные штаны для активного отдыха, которые подчеркнут вашу индивидуальность.
Тактичные штаны: модные тренды этого сезона, для активного образа жизни.
Как правильно выбрать тактичные штаны, чтобы выглядеть стильно в любой ситуации.
Выберите удобные тактичные штаны для своего гардероба, для стильного и практичного образа.
Тактичные штаны: выбор современного мужчины, и какие модели стоит выбрать для уникального стиля.
штани тактичні штани тактичні .
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
rgbet
Mohamed Salah https://mohamed-salah.prostoprosport-cz.org je egyptsky fotbalista, ktery hraje jako utocnik za anglictinu. klub Liverpool a egyptsky narodni tym. Povazovan za jednoho z nejlepsich fotbalistu na svete.
Kevin De Bruyne https://kevin-de-bruyne.prostoprosport-cz.org Belgicky fotbalista, zaloznik Manchesteru klub City” a belgicky narodni tym. Absolvent fotbalovych klubu „Ghent” a „Genk”. V roce 2008 zahajil svou karieru dospelych, debutoval v Genku.
Что нужно знать перед походом к стоматологу, ознакомиться.
Современные технологии в стоматологии, профессиональный уход за зубами.
Как избежать боли при лечении зубов, ознакомиться.
Мифы о стоматологии, в которые верят все, эффективные советы стоматолога.
Как сохранить здоровье зубов на долгие годы, рекомендуем.
Как выбрать хорошего стоматолога, эффективные методики стоматологии.
Как правильно чистить зубы: секреты здоровой улыбки, прочитать.
стоматологія зуб стоматологія зуб .
Lionel Messi https://lionel-messi.prostoprosport-cz.org je argentinsky fotbalista, utocnik a kapitan klubu MLS Inter Miami. , kapitan argentinske reprezentace. Mistr sveta, vitez Jizni Ameriky, vitez finale, olympijsky vitez. Povazovan za jednoho z nejlepsich fotbalistu vsech dob.
Bernardo Silva https://bernardo-silva.prostoprosport-cz.org Portugalsky fotbalista, zaloznik. Narozen 10. srpna 1994 v Lisabonu. Silva je povazovan za jednoho z nejlepsich utocnych zalozniku na svete. Fotbalista je povestny svou vytrvalosti a vykonem.
Antoine Griezmann https://antoine-griezmann.prostoprosport-cz.org Francouzsky fotbalista, utocnik a zaloznik za Atletico de Madrid. Hrac a vicekapitan francouzskeho narodniho tymu, clen tymu – mistr sveta 2018 Stribrny medailista z mistrovstvi Evropy 2016 a mistrovstvi sveta 2022.
Robert Lewandowski https://robert-lewandowski.prostoprosport-cz.org je polsky fotbalista, utocnik spanelskeho klubu Barcelona a kapitan polskeho narodniho tymu. Povazovan za jednoho z nejlepsich utocniku na svete. Rytir krize velitele polskeho renesancniho radu.
Pablo Martin Paez Gavira https://gavi.prostoprosport-cz.org Spanelsky fotbalista, zaloznik barcelonskeho klubu a spanelske reprezentace. Povazovan za jednoho z nejtalentovanejsich hracu sve generace. Ucastnik mistrovstvi sveta 2022. Vitez Ligy narodu UEFA 2022/23
Son Heung Min https://son-heung-min.prostoprosport-cz.org Jihokorejsky fotbalista, utocnik a kapitan anglickeho klubu Premier League Tottenham Hotspur a narodniho tymu Korejske republiky. V roce 2022 vyhral Zlatou kopacku Premier League.
Luka Modric https://luka-modric.prostoprosport-cz.org je chorvatsky fotbalista, stredni zaloznik a kapitan spanelskeho tymu. klub Real Madrid, kapitan chorvatskeho narodniho tymu. Uznavan jako jeden z nejlepsich zalozniku nasi doby. Rytir Radu prince Branimira. Rekordman chorvatske reprezentace v poctu odehranych zapasu.
Cristiano Ronaldo https://cristiano-ronaldo.prostoprosport-cz.org je portugalsky fotbalista, utocnik, kapitan Saudske Arabie klubu An-Nasr a portugalskeho narodniho tymu. Mistr Evropy. Povazovan za jednoho z nejlepsich fotbalistu vsech dob. Nejlepsi strelec v historii fotbalu podle IFFIS a ctvrty podle RSSSF
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Pedro Gonzalez Lopez https://pedri.prostoprosport-cz.org lepe znamy jako Pedri, je spanelsky fotbalista, ktery hraje jako utocny zaloznik. za Barcelonu a spanelskou reprezentaci. Bronzovy medailista z mistrovstvi Evropy 2020 a zaroven nejlepsi mlady hrac tohoto turnaje.
Alison Ramses Becker https://alisson-becker.prostoprosport-cz.org Brazilsky fotbalista nemeckeho puvodu, brankar klubu Liverpool a brazilsky narodni tym. Je povazovan za jednoho z nejlepsich brankaru sve generace a je znamy svymi vynikajicimi zakroky, presnosti prihravek a schopnosti jeden na jednoho.
Karim Benzema https://karim-benzema.prostoprosport-cz.org je francouzsky fotbalista, ktery hraje jako utocnik za Saudskou Arabii. Arabsky klub Al-Ittihad. Hral za francouzsky narodni tym, za ktery odehral 97 zapasu a vstrelil 37 branek. V 17 letech se stal jednim z nejlepsich hracu rezervy, nastrilel tri desitky golu za sezonu.
Rodrigo Silva de Goiz https://rodrygo.prostoprosport-cz.org Brazilsky fotbalista, utocnik Realu Madrid a brazilskeho narodniho tymu. V breznu 2017 byl Rodrigo povolan do narodniho tymu Brazilie U17 na zapasy Montague Tournament.
Thibaut Nicolas Marc Courtois https://thibaut-courtois.prostoprosport-cz.org Belgicky fotbalista, brankar spanelskeho klubu Real Madrid . V sezone 2010/11 byl uznan jako nejlepsi brankar v belgicke Pro League a take hrac roku pro Genk. Trojnasobny vitez Ricardo Zamora Trophy
Bruno Guimaraes Rodriguez Moura https://bruno-guimaraes.prostoprosport-cz.org Brazilsky fotbalista, defenzivni zaloznik Newcastlu United a Brazilsky narodni tym. Vitez olympijskych her 2020 v Tokiu.
Virgil van Dijk https://virgil-van-dijk.prostoprosport-cz.org Nizozemsky fotbalista, stredni obrance, kapitan anglickeho klubu Liverpool a kapitan nizozemskeho narodniho tymu.
Toni Kroos https://toni-kroos.prostoprosport-cz.org je nemecky fotbalista, ktery hraje jako stredni zaloznik za Real Madrid a nemecky narodni tym. Mistr sveta 2014. Prvni nemecky hrac v historii, ktery sestkrat vyhral Ligu mistru UEFA.
Seriously many of superb information!|
Toni Kroos https://toni-kroos.prostoprosport-cz.org je nemecky fotbalista, ktery hraje jako stredni zaloznik za Real Madrid a nemecky narodni tym. Mistr sveta 2014. Prvni nemecky hrac v historii, ktery sestkrat vyhral Ligu mistru UEFA.
Darwin Gabriel Nunez Ribeiro https://darwin-nunez.prostoprosport-cz.org Uruguaysky fotbalista, utocnik anglickeho klubu Liverpool a Uruguaysky narodni tym. Bronzovy medailista mistrovstvi Jizni Ameriky mezi mladeznickymi tymy.
Romelu Menama Lukaku Bolingoli https://romelu-lukaku.prostoprosport-cz.org Belgicky fotbalista, utocnik anglickeho klubu Chelsea a Belgican vyber. Na hostovani hraje za italsky klub Roma.
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Dedicated to the brave players!!
Glory Casino offers quality and reliability. There are bonuses for new players, high betting odds, and fast withdrawals. The working mirror is always available. I play and win with pleasure. I recommend trying it!
Registering at Glory Casino was quick and easy. After my first deposit, I received a generous bonus. The betting odds are high, and the casino offers a variety of games. I recommend Glory Casino to everyone who values quality and reliability!
Glory Casino
official website Glory Casino download for Android
Glory Casino affiliate
Glory Casino mirror online
Glory Casino mobile version download
download Glory Casino on phone betting app
Good profits!
видеостена под ключ https://www.kupit-videostenu.ru .
проститутки на выезд https://prostitutki-213.ru
buy 1k tiktok followers https://tiktok-followers-buy.com
buy 1000 tiktok followers cheap buy 1000 tiktok followers
отчаянные домохозяйки актеры отчаянные домохозяйки смотреть онлайн бесплатно
123 슬롯
“최선을 다하겠습니다.” Fang Jifan은 여전히이 기회를 위해 싸우고 싶었습니다.
рио бет казино официальный сайт риобет казино
официальный сайт Dragon Money регистрация драгон мани казино
Большой выбор игровых автоматов, рабочее зеркало сайта https://fartunaplay.ru играть на реальные деньги онлайн
Качественная и недорогая https://mebelvam-nn.ru лучшие цены, доставка и сборка.
Slot machines on the official website and mirrors of the Pin Up online casino https://pin-up.tr-kazakhstan.kz are available for free mode, and after registering at Pin Up Casino Ru you can play for money.
Pin Up casino https://pin-up.salexy.kz official website, Pin Up slot machines play for money online, Pin Up mirror working for today.
Sports in Azerbaijan https://idman-xeberleri.com.az development and popular sports Azerbaijan is a country with rich sports traditions and outstanding achievements on the international stage.
Pin up entry to the official website. Play online casino Pin Up https://pin-up.prostoprosport.ru for real money. Register on the Pin Up Casino website and claim bonuses!
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
World of Games https://onlayn-oyunlar.com.az provides the latest news about online games, game reviews, gameplay and ideas, game tactics and tips. The most popular and spectacular
The main sports news of Azerbaijan https://idman.com.az. Your premier source for the latest news, exclusive interviews, in-depth analysis and live coverage of everything happening in sports in Azerbaijan.
NHL (National Hockey League) News https://nhl.com.az the latest and greatest NHL news for today. Sports news – latest NHL news, standings, match results, online broadcasts.
UFC in Azerbaijan https://ufc.com.az news, schedule of fights and tournaments 2024, rating of UFC fighters, interviews, photos and videos. Live broadcasts and broadcasts of tournaments, statistics.
Top sports news https://idman-azerbaycan.com.az photos and blogs from experts and famous athletes, as well as statistics and information about matches of leading championships.
Latest news and details about the NBA in Azerbaijan https://nba.com.az. Hot events, player transfers and the most interesting events. Explore the world of the NBA with us.
The latest top football news https://futbol.com.az today. Interviews with football players, online broadcasts and match results, analytics and football forecasts, photos and videos.
Discover the fascinating world of online games with GameHub Azerbaijan https://online-game.com.az. Get the latest news, reviews and tips for your favorite games. Join our gaming community today!
Каталог рейтингов хостингов https://pro-hosting.tech на любой вкус и под любые, даже самые сложные, задачи.
Сантехник — вызов сантехника на дом в Москве и Московской области в удобное для вас время.
Play PUBG Mobile https://pubg-mobile.com.az an exciting world of high-quality mobile battle royale. Unique maps, strategies and intense combat await you in this exciting mobile version of the popular game.
The Dota 2 website https://dota2.com.az Azerbaijan provides the most detailed information about the latest game updates, tournaments and upcoming events. We have all the winning tactics, secrets and important guides.
Latest news about games for Android https://android-games.com.az, reviews and daily updates. Read now and get the latest information on the most exciting games
Check out the latest news, guides and in-depth reviews of the available options for playing Minecraft Az https://minecraft.com.az. Find the latest information about Minecraft Download, Pocket Edition and Bedrock Edition.
The most popular sports site https://sports.com.az of Azerbaijan, where the latest sports news, forecasts and analysis are collected.
Latest news and analytics of the Premier League https://premier-league.com.az. Detailed descriptions of matches, team statistics and the most interesting football events. EPL Azerbaijan is the best place for football fans.
Хотите сделать в квартире ремонт? Тогда советуем вам посетить сайт https://stroyka-gid.ru, где вы найдете всю необходимую информацию по строительству и ремонту.
https://loveflover.ru — сайт посвященный комнатным растениям. Предлагает подробные статьи о выборе, выращивании и уходе за различными видами комнатных растений. Здесь можно найти полезные советы по созданию зелёного уголка в доме, руководства по декору и решению распространённых проблем, а также информацию о подходящих горшках и удобрениях. Платформа помогает создавать уютную атмосферу и гармонию в интерьере с помощью растений.
1xbet https://1xbet.best-casino-ar.com with withdrawal without commission. Register online in a few clicks. A large selection of slot machines in mobile applications and convenient transfers in just a few minutes.
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Pin Up official https://pin-up.adb-auto.ru website. Login to your personal account and register through the Pin Up mirror. Slot machines for real money at Pinup online casino.
Pin-up Casino https://pin-up.admsov.ru/ is an online casino licensed and regulated by the government of Curacao . Founded in 2016, it is home to some of the industry’s leading providers, including NetEnt, Microgaming, Play’n GO and others. This means that you will be spoiled for choice when it comes to choosing a game.
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Pin Up online casino https://pin-up.webrabota77.ru/ is the official website of a popular gambling establishment for players from the CIS countries. The site features thousands of slot machines, online tables and other branded entertainment from Pin Up casino.
Pin Up Casino https://pin-up.noko39.ru Registration and Login to the Official Pin Up Website. thousands of slot machines, online tables and other branded entertainment from Pin Up casino. Come play and get big bonuses from the Pinup brand today
Реальные анкеты проституток https://prostitutki-213.ru Москвы с проверенными фото – от элитных путан до дешевых шлюх. Каталог всех индивидуалок на каждой станции метро с реальными фотографиями без ретуши и с отзывами реальных клиентов.
Смотрите онлайн сериал Отчаянные домохозяйки https://domohozyayki-serial.ru в хорошем качестве HD 720 бесплатно, рейтинг сериала: 8.058, режиссер сериала: Дэвид Гроссман, Ларри Шоу, Дэвид Уоррен.
Buy TikTok followers https://tiktok-followers-buy.com to get popular and viral with your content. All packages are real and cheap — instant delivery within minutes. HQ followers for your TikTok. 100% real users. The lowest price for TikTok followers on the market
꽁포 사이트
그는 어쩔 수 없이 Zhu Houzhao를 흘끗 쳐다보았고, 그의 눈에는 감사의 기미가 흘렀습니다.
Pin Up Casino https://pin-up.sibelshield.ru official online casino website for players from the CIS countries. Login and registration to the Pin Up casino website is open to new users with bonuses and promotional free spins.
Изготовление памятников и надгробий https://uralmegalit.ru по низким ценам. Собственное производство. Высокое качество, широкий ассортимент, скидки, установка.
Pin Up Casino https://pin-up.ergojournal.ru приглашает игроков зарегистрироваться на официальном сайте и начать играть на деньги в лучшие игровые автоматы, а на зеркалах онлайн казино Пин Ап можно найти аналогичную витрину слотов
Pin-up casino https://pin-up.jes-design.ru популярное онлайн-казино и ставки на спорт. Официальный сайт казино для доступа к играм и другим функциям казино для игры на деньги.
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
купить спорт площадку для улицы http://ploshadka-sport.ru/ .
Pin Up https://pin-up.fotoevolution.ru казино, которое радует гемблеров в России на протяжении нескольких лет. Узнайте, что оно подготовило посетителям. Описание, бонусы, отзывы о легендарном проекте. Регистрация и вход.
Открой мир карточных игр в Pin-Up https://pin-up.porsamedlab.ru казино Блэкджек, Баккара, Хило и другие карточные развлечения. Регистрируйтесь и играйте онлайн!
Официальный сайт Pin Up казино https://pin-up.nasledie-smolensk.ru предлагает широкий выбор игр и щедрые бонусы для игроков. Уникальные бонусные предложения, онлайн регистрация.
Pinup казино https://pin-up.vcabinet.kz это не просто сайт, а целый мир азартных развлечений, где каждый может найти что-то свое. От традиционных игровых автоматов до прогнозов на самые популярные спортивные события.
Latest Diablo news https://diablo.com.az game descriptions and guides. Diablo.az is the largest Diablo portal in the Azerbaijani language.
Latest World of Warcraft (WOW) tournament news https://wow.com.az, strategies and game analysis. The most detailed gaming portal in Azerbaijani language
Azerbaijan NFL https://nfl.com.az News, analysis and topics about the latest experience, victories and records. A portal where the most beautiful NFL games in the world are generally studied.
Discover exciting virtual football in Fortnite https://fortnite.com.az. Your central hub for the latest news, expert strategies and interesting e-sports reports. Collecting points with us!
The latest analysis, tournament reviews and the most interesting features of the Spider-Man game https://spider-man.com.az series in Azerbaijani.
Read the latest Counter-Strike 2 news https://counter-strike.net.az, watch the most successful tournaments and become the best in the world of the game on the CS2 Azerbaijan website.
Узнайте всю правду о берцах зсу, изучайте, традиции, Одержимость берцами зсу, тайны, тайны, истину, энергией, историей, в мир, освійте, вивчіть
берці літні зсу https://bercitaktichnizsu.vn.ua/ .
Mesut Ozil https://mesut-ozil.com.az latest news, statistics, photos and much more. Get the latest news and information about one of the best football players Mesut Ozil.
Explore the extraordinary journey of Kilian Mbappe https://kilian-mbappe.com.az, from his humble beginnings to global stardom. Delve into his early years, meteoric rise through the ranks, and impact on and off the football field.
Latest news, statistics, photos and much more about Pele https://pele.com.az. Get the latest news and information about football legend Pele.
Latest boxing news https://boks.com.az, Resul Abbasov’s achievements, Tyson Fury’s fights and much more. All in Ambassador Boxing.
Sergio Ramos Garcia https://sergio-ramos.com.az Spanish footballer, defender. Former Spanish national team player. He played for 16 seasons as a central defender for Real Madrid, where he captained for six seasons.
Gianluigi Buffon https://buffon.com.az Italian football player, goalkeeper. Considered one of the best goalkeepers of all time. He holds the record for the number of games in the Italian Championship, as well as the number of minutes in this tournament without conceding a goal.
мастерская по ремонту стиральных машин мастерская по ремонту стиральных машин .
Paulo Bruno Ezequiel Dybala https://dybala.com.az Argentine footballer, striker for the Italian club Roma and the Argentina national team. World champion 2022.
Paul Labille Pogba https://pogba.com.az French footballer, central midfielder of the Italian club Juventus. Currently suspended for doping and unable to play. World champion 2018.
Kevin De Bruyne https://kevin-de-bruyne.liverpool-fr.com Belgian footballer, born 28 June 1991 years in Ghent. He has had a brilliant club career and also plays for the Belgium national team. De Bruyne is known for his spectacular goals and brilliant assists.
Канал для того, чтобы знания и опыт, могли помочь любому человеку сделать ремонт https://tvin270584.livejournal.com в своем жилище, любой сложности!
Mohamed Salah Hamed Mehrez Ghali https://mohamed-salah.liverpool-fr.com Footballeur egyptien, attaquant du club anglais de Liverpool et l’equipe nationale egyptienne. Considere comme l’un des meilleurs joueurs du monde.
Paul Labille Pogba https://paul-pogba.psg-fr.com Footballeur francais, milieu de terrain central du club italien de la Juventus. Champion du monde 2018. Actuellement suspendu pour dopage et incapable de jouer.
The young talent who conquered Paris Saint-Germain: how Xavi Simons became https://xavi-simons.psg-fr.com leader of a superclub in record time.
Kylian Mbappe https://kylian-mbappe.psg-fr.com Footballeur, attaquant francais. Il joue pour le PSG et l’equipe de France. Ne le 20 decembre 1998 a Paris. Mbappe est francais de nationalite. La taille de l’athlete est de 178 cm.
Kevin De Bruyne https://liverpool.kevin-de-bruyne-fr.com Belgian footballer, born 28 June 1991 years in Ghent. He has had a brilliant club career and also plays for the Belgium national team. De Bruyne is known for his spectacular goals and brilliant assists.
Paul Pogba https://psg.paul-pogba-fr.com is a world-famous football player who plays as a central midfielder. The player’s career had its share of ups and downs, but he was always distinguished by his perseverance and desire to win.
Kylian Mbappe https://psg.kylian-mbappe-fr.com Footballeur, attaquant francais. L’attaquant de l’equipe de France Kylian Mbappe a longtemps refuse de signer un nouveau contrat avec le PSG, l’accord etant en vigueur jusqu’a l’ete 2022.
Изготовление, сборка и ремонт мебели https://shkafy-na-zakaz.blogspot.com для Вас, от эконом до премиум класса.
Thibaut Nicolas Marc Courtois https://thibaut-courtois.real-madrid-ar.com Footballeur belge, gardien de but du Club espagnol “Real Madrid”. Lors de la saison 2010/11, il a ete reconnu comme le meilleur gardien de la Pro League belge, ainsi que comme joueur de l’annee pour Genk. Trois fois vainqueur du Trophee Ricardo Zamora, decerne chaque annee au meilleur gardien espagnol
Forward Rodrigo https://rodrygo.real-madrid-ar.com is now rightfully considered a rising star of Real Madrid. The talented Santos graduate is compared to Neymar and Cristiano Ronaldo, but the young talent does not consider himself a star.
Jude Victor William Bellingham https://jude-bellingham.real-madrid-ar.com English footballer, midfielder of the Spanish club Real Madrid and the England national team. In April 2024, he won the Breakthrough of the Year award from the Laureus World Sports Awards.
토토 사이트 입플
“좋아, 갈게.” Fang Jifan은 일어나서 다리를 들고 떠나려고했습니다.
Saud Abdullah Abdulhamid https://saud-abdulhamid.real-madrid-ar.com Saudi footballer, defender of the Al -Hilal” and the Saudi Arabian national team. Asian champion in the age category up to 19 years. Abdulhamid is a graduate of the Al-Ittihad club. On December 14, 2018, he made his debut in the Saudi Pro League in a match against Al Bateen
Khvicha Kvaratskhelia https://khvicha-kvaratskhelia.real-madrid-ar.com midfielder of the Georgian national football team and the Italian club “Napoli”. Became champion of Italy and best player in Serie A in the 2022/23 season. Kvaratskhelia is a graduate of Dynamo Tbilisi and played for the Rustavi team.
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Vinicius Junior https://vinisius-junior.com.az player news, fresh current and latest events for today about the player of the 2024 season
Latest news and information about Marcelo https://marcelo.com.az on this site! Find Marcelo’s biography, career, playing stats and more. Find out the latest information about football master Marcelo with us!
Khabib Abdulmanapovich Nurmagomedov https://khabib-nurmagomedov.com.az Russian mixed martial arts fighter who performed under the auspices of the UFC. Former UFC lightweight champion.
Welcome to our official site! Get to know the history, players and latest news of Inter Miami Football Club https://inter-miami.com.az. Discover with us the successes and great performances of America’s newest and most exciting soccer club.
Conor Anthony McGregor https://conor-mcgregor.com.az Irish mixed martial arts fighter who also performed in professional boxing. He performs under the auspices of the UFC in the lightweight weight category. Former UFC lightweight and featherweight champion.
Оперативный вывод из запоя https://www.liveinternet.ru/users/laralim/post505923855/ на дому. Срочный выезд частного опытного нарколога круглосуточно. При необходимости больного госпитализируют в стационар.
Видеопродакшн студия https://humanvideo.ru полного цикла. Современное оборудование продакшн-компании позволяет снимать видеоролики, фильмы и клипы высокого качества. Создание эффективных видеороликов для рекламы, мероприятий, видеоролики для бизнеса.
Заказать вывоз мусора https://musorovozzz.ru в Москве и Московской области, недорого и в любое время суток в мешках или контейнерами 8 м?, 20 м?, 27 м?, 38 м?, собственный автопарк. Заключаем договора на вывоз мусора.
Реальные анкеты https://prostitutki-vyzvat-moskva.ru Москвы с проверенными фото – от элитных путан до дешевых шлюх. Каталог всех индивидуалок на каждой станции метро с реальными фотографиями без ретуши и с отзывами реальных клиентов.
Совсем недавно открылся новый интернет портал BlackSprut (Блекспрут) https://bs2cite.cc в даркнете, который предлагает купить нелегальные товары и заказать запрещенные услуги. Самая крупнейшая площадка СНГ. Любимые шопы и отзывчивая поддержка.
Welcome to the site dedicated to Michael Jordan https://michael-jordan.com.az, a basketball legend and symbol of world sports culture. Here you will find highlights, career, family and news about one of the greatest athletes of all time.
Diego Armando Maradona https://diego-maradona.com.az Argentine footballer who played as an attacking midfielder and striker. He played for the clubs Argentinos Juniors, Boca Juniors, Barcelona, ??Napoli, and Sevilla.
Gucci купить http://thebestluxurystores.ru по низкой цене в интернет-магазине брендовой одежды. Одежда и обувь бренда Gucci c доставкой.
Muhammad Ali https://muhammad-ali.com.az American professional boxer who competed in the heavy weight category; one of the most famous boxers in the history of world boxing.
Монтаж систем отопления https://fectum.pro, водоснабжения, вентиляции, канализации, очистки воды, пылеудаления, снеготаяния, гелиосистем в Краснодаре под ключ.
LeanBiome is a dietary supplement designed to promote weight loss and improve overall health. It is formulated with a unique blend of probiotics, prebiotics, and natural ingredients that work together to support a healthy gut microbiome. The gut microbiome plays a crucial role in digestion, metabolism, and the immune system. By optimizing the gut microbiome, LeanBiome aims to help individuals achieve their weight loss goals more effectively and sustainably. https://sites.google.com/spsw.edu.pl/leanbiome/
Tonic Greens has gained popularity as a health supplement known for its rich blend of vitamins, minerals, and plant extracts. This article explores its composition, potential health benefits, usage instructions, and possible side effects. https://sites.google.com/spsw.edu.pl/tonicgreens/
SightCare is a revolutionary dietary supplement designed to support and maintain optimal eye health. In today’s digital age, where screens dominate our daily lives, the need for effective eye care solutions has never been greater. SightCare aims to meet this need with its scientifically formulated blend of essential nutrients and antioxidants. https://sites.google.com/spsw.edu.pl/sightcare/
Boostaro stands out as a natural solution for boosting energy levels and supporting overall vitality. Its blend of caffeine, adaptogens, and essential nutrients offers a balanced approach to enhancing physical and mental energy. As with any supplement, consult with a healthcare professional before starting, especially if you have any health concerns or sensitivities. https://sites.google.com/spsw.edu.pl/boostaro/
Prostadine is a dietary supplement formulated to support prostate health, particularly in men experiencing symptoms of benign prostatic hyperplasia (BPH) or other prostate-related issues. As men age, maintaining prostate health becomes increasingly important to avoid urinary discomfort and other related problems. Prostadine aims to provide a natural solution through a blend of ingredients known for their beneficial effects on the prostate. https://sites.google.com/spsw.edu.pl/prostabiome
Lev Ivanovich Yashin https://lev-yashin.com.az Soviet football player, goalkeeper. Olympic champion in 1956 and European champion in 1960, five-time champion of the USSR, three-time winner of the USSR Cup.
Al-Nasr https://al-nasr.com.az your source of news and information about Al-Nasr Football Club . Find out the latest results, transfer news, player and manager interviews, fixtures and much more.
Usain St. Leo Bolt https://usain-bolt.com.az Jamaican track and field athlete, specialized in short-distance running, eight-time Olympic champion and 11-time world champion (a record in the history of this competition among men).
Game World https://kz-games.kz offers the latest online gaming news, game reviews, gameplay and ideas, gaming tactics and tips . Start playing our most popular and amazing games and get ready to become the leader in the online gaming world!
You have a source of the latest and most interesting sports news from Kazakhstan: “Kazakhstan sports news https://sports-kazahstan.kz: Games and records” ! Follow us to receive updates and interesting news every minute!
Prostadine is a dietary supplement formulated to support prostate health, particularly in men experiencing symptoms of benign prostatic hyperplasia (BPH) or other prostate-related issues. As men age, maintaining prostate health becomes increasingly important to avoid urinary discomfort and other related problems. Prostadine aims to provide a natural solution through a blend of ingredients known for their beneficial effects on the prostate. https://sites.google.com/spsw.edu.pl/prostadine/
Glucotil is a dietary supplement designed to support healthy blood sugar levels and overall metabolic health. Managing blood sugar is crucial for individuals with diabetes or pre-diabetes, as well as for those looking to maintain healthy energy levels and prevent future metabolic issues. Glucotil combines natural ingredients that have been shown to positively affect blood glucose regulation and insulin sensitivity.
https://sites.google.com/spsw.edu.pl/glucotil/
Latest news and information about the NBA https://basketball-kz.kz in Kazakhstan. Hot stories, player transfers and highlights. Watch the NBA world with us.
Top sports news https://sport-kz-news.kz, photos and blogs from experts and famous athletes, as well as statistics and information about matches of leading championships.
The latest top football news https://football-kz.kz today. Interviews with football players, online broadcasts and match results, analytics and football forecasts, photos and videos.
Latest news about games for Android https://android-games.kz, reviews and daily updates. Read now and get the latest information about the most exciting games
Check out Minecraft kz https://minecraft-kz.kz for the latest news, guides, and in-depth reviews of the game options available. Find the latest information on Minecraft Download, Pocket Edition and Bedrock Edition.
Latest news from World of Warcraft https://wow-kz.kz (WOW) tournaments, strategy and game analysis. The most detailed gaming portal in the language.
Latest news and analysis of the Premier League https://premier-league.kz. Full descriptions of matches, team statistics and the most interesting football events. Premier Kazakhstan is the best place for football fans.
블랙 맘바
이 말은 황실 입구에 있는 황실 근위대장과 다섯 명의 신하, 그리고 황실 근위대에게 전해졌다.
Доставка груза и грузоперевозки https://tamozhennyy-deklarant.blogspot.com по России через транспортную компанию автотранспортом доступна и для частных лиц. Перевозчик отправит или доставит ваш груз: выгодные тарифы индивидуальный подход из рук в руки 1 машиной.
Зеркала интерьерные https://zerkala-mag.ru в интернет-магазине «Зеркала с подсветкой» Самые низкие цены на зеркала!
Предлагаем купить гаражное оборудование https://profcomplex.pro, автохимию, технику и уборочный инвентарь для клининговых компаний. Доставка по Москве и другим городам России.
Купить зеркала https://zerkala-m.ru по низким ценам. Более 1980 моделей, купить недорого в интернет-магазине в Москве с доставкой по России. Удобный каталог, низкие цены, качественные фото.
Spider-Man https://spiderman.kz the latest news, articles, reviews, dates, spoilers and other latest information. All materials on the topic “Spider-Man”
The latest top football news https://football.sport-news-eg.com today. Interviews with football players, online broadcasts and match results, analytics and football forecasts, photos and videos.
Latest Counter-Strike 2 news https://counter-strike-kz.kz, watch the most successful tournaments and be the best in the gaming world.
Discover the dynamic world of Arab sports https://sports-ar.com through the lens of Arab sports news. Your premier source for breaking news, exclusive interviews, in-depth analysis and live coverage of everything happening in sports.
Интернет магазин электроники https://techno-line.store и цифровой техники по доступным ценам. Доставка мобильной электроники по Москве и Московской области.
NHL news https://nhl-ar.com (National Hockey League) – the latest and most up-to-date NHL news for today.
UFC news https://ufc-ar.com, schedule of fights and tournaments 2024, ratings of UFC fighters, interviews, photos and videos. Live broadcasts and broadcasts of tournaments, statistics, forums and fan blogs.
The most important sports news https://bein-sport-egypt.com, photos and blogs from experts and famous athletes, as well as statistics and information about matches of leading leagues.
News and events of the American Basketball League https://basketball-eg.com in Egypt. Hot events, player transfers and the most interesting events. Explore the world of the NBA with us.
Sugar Defender is a dietary supplement designed to help regulate blood sugar levels and support overall metabolic health. Targeting individuals with pre-diabetes, diabetes, or those seeking to maintain stable blood sugar levels, Sugar Defender combines natural ingredients known for their ability to improve glucose metabolism and enhance insulin sensitivity. https://sites.google.com/spsw.edu.pl/sugardefender/
Nagano Tonic is a dietary supplement designed to promote overall health and wellness. Drawing inspiration from traditional Japanese medicine and modern nutritional science, Nagano Tonic incorporates a blend of natural ingredients known for their health-boosting properties. This supplement aims to enhance energy levels, support immune function, and improve overall vitality. https://sites.google.com/spsw.edu.pl/naganotonicleanbelly/
ZenCortex is a nootropic supplement designed to enhance cognitive function, support brain health, and improve mental clarity. By combining a blend of natural ingredients known for their neuroprotective and cognitive-enhancing properties, ZenCortex aims to boost memory, focus, and overall brain performance. https://sites.google.com/spsw.edu.pl/zencortex/
SeroLean is a dietary supplement designed to support weight loss and overall metabolic health. By leveraging the power of natural ingredients, SeroLean aims to help individuals achieve their weight management goals by enhancing serotonin levels, reducing appetite, and promoting fat metabolism. https://sites.google.com/spsw.edu.pl/serolean/
LeanGene is a dietary supplement designed to support weight loss and metabolic health by targeting genetic and metabolic pathways. Utilizing a blend of natural ingredients, LeanGene aims to enhance fat burning, suppress appetite, and improve overall metabolic function, helping individuals achieve their weight management goals more effectively.
https://sites.google.com/spsw.edu.pl/leangene/
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Discover the wonderful world of online games https://game-news-ar.com. Get the latest news, reviews and tips for your favorite games.
Minecraft news https://minecraft-ar.com, guides and in-depth reviews of the gaming features available in Minecraft Ar. Get the latest information on downloading Minecraft, Pocket Edition and Bedrock Edition.
News, tournaments, guides and strategies about the latest GTA games https://gta-ar.com. Stay tuned for the best GTA gaming experience
Latest news https://android-games-ar.com about Android games, reviews and daily updates. The latest information about the most exciting games.
Pineal XT is a dietary supplement formulated to enhance sleep quality and support sleep patterns. Known for its natural ingredients, Pineal XT particularly focuses on boosting melatonin production, aiding individuals in managing sleep-related issues effectively. https://sites.google.com/spsw.edu.pl/pinealxt/
Nicely put. Thanks a lot!|
Prodentim offers a range of innovative dental care products designed to promote optimal oral health. From toothpaste to oral rinses, Prodentim products are formulated with advanced ingredients to address various dental concerns and enhance overall oral hygiene. https://sites.google.com/spsw.edu.pl/prodentim/
Puravive is a dietary supplement designed to support weight loss and overall metabolic health. By leveraging a blend of natural ingredients known for their fat-burning and metabolism-boosting properties, Puravive aims to help individuals achieve their weight management goals and enhance their overall well-being. https://sites.google.com/spsw.edu.pl/puravive-web/
Открытие для себя Ерлинг Хааланда https://manchestercity.erling-haaland-cz.com, a talented player of «Manchester City». Learn more about his skills, achievements and career growth.
The path of 21-year-old Jude Bellingham https://realmadrid.jude-bellingham-cz.com from young talent to one of the most promising players in the world, reaching new heights with Dortmund and England.
The site is dedicated to football https://fooball-egypt.com, football history and news. Latest news and fresh reviews of the world of football
French prodigy Kylian Mbappe https://realmadrid.kylian-mbappe-cz.com is taking football by storm, joining his main target, ” Real.” New titles and records are expected.
Harry Kane’s journey https://bavaria.harry-kane-cz.com from Tottenham’s leading striker to Bayern’s leader and Champions League champion – this is the story of a triumphant ascent to the football Olympus.
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Эффективные способы расклеивания объявлений, Как заработать на расклейке объявлений, Топовые площадки для расклейки объявлений, Как привлечь внимание с помощью правильной расклейки объявлений, Как превратить расклейку объявлений в прибыльный бизнес, Способы, которые работают в расклейке объявлений
расклейка объявлений https://расклейка-объявлений77.рф/ .
Изготовим для Вас изделия из металла https://smith-moskva.blogspot.com, по вашим чертежам или по нашим эскизам.
Промышленные насосы https://1nsk.ru/news/articles/nasosy-spetsialnogo-naznacheniya.html Wilo предлагают широкий ассортимент решений для различных отраслей промышленности, включая водоснабжение, отопление, вентиляцию, кондиционирование и многие другие. Благодаря своей высокой производительности и эффективности, насосы Wilo помогают снизить расходы на энергию и обслуживание, что делает их идеальным выбором для вашего бизнеса.
https://rolaks.com отделочные материалы для фасада – интернет-магазин
The fascinating story of the rise of Brazilian prodigy Vinicius Junior https://realmadrid.vinicius-junior-cz.com to the heights of glory as part of the legendary Madrid “Real”
Mohamed Salah https://liverpool.mohamed-salah-cz.com, who grew up in a small town in Egypt, conquered Europe and became Liverpool star and one of the best players in the world.
메이저 토토
그는 Ningbo Mansion에서 일어난 일을 자세히 설명하면서 매우 진지하게 썼습니다.
The inspiring story of how talented Kevin De Bruyne https://manchestercity.kevin-de-bruyne-cz.com became the best player of Manchester City and the Belgium national team. From humble origins to the leader of a top club.
Полезные советы и пошаговые инструкции по строительству https://svoyugol.by, ремонту и дизайну домов и квартир, выбору материалов, монтажу и установке своими руками.
Lionel Messi https://intermiami.lionel-messi-cz.com, one of the best football players of all time, moves to Inter Miami” and changes the face of North American football.
Bernardo Mota Veiga de Carvalho e Silva https://manchestercity.bernardo-silva-cz.com Portuguese footballer, club midfielder Manchester City and the Portuguese national team.
Antoine Griezmann https://atlticomadrid-dhb.antoine-griezmann-cz.com Atletico Madrid star whose talent and decisive goals helped the club reach the top of La Liga and the UEFA Champions League.
Son Heung-min’s https://tottenhamhotspur.son-heung-min-cz.com success story at Tottenham Hotspur and his influence on the South Korean football, youth inspiration and changing the perception of Asian players.
The story of Robert Lewandowski https://barcelona.robert-lewandowski-cz.com, his impressive journey from Poland to Barcelona, ??where he became not only a leader on the field, but also a source of inspiration for young players.
We explore the path of Luka Modric https://realmadrid.luka-modric-cz.com to Real Madrid, from a difficult adaptation to legendary Champions League triumphs and personal awards.
The impact of the arrival of Cristiano Ronaldo https://annasr.cristiano-ronaldo-cz.com at Al-Nasr. From sporting triumphs to cultural changes in Saudi football.
Противоотмывочная верификация: Каким образом предотвратить ограничение активов на платформах обмена криптовалют
По какой причине важна AML-проверка?
Антиотмывочные меры (Anti-Money Laundering) – подразумевает комплекс действий, направленных на борьбу легализации ресурсов. Эта проверка позволяет охранять виртуальные активы участников а также предотвращать применение площадок нелегальных операций. Проверка по борьбе с отмыванием денег требуется для обеспечения защищенности личных активов наряду с соблюдением законодательных требований.
Главные способы проверки
Криптобиржи а также другие денежные решения используют несколько ключевых способов в целях проверки пользователей:
KYC: Данный подход охватывает ключевые действия в целях идентификации документов участника, такие как проверка идентификационных сведений проживания. Идентификация личности дает возможность подтвердить, в надежности владельца представляет собой надежным.
CFT: Ориентирована в интересах предотвращения финансирования экстремистских групп. Инструментарий мониторит сомнительные действия в случае необходимости замораживает аккаунты посредством проведения внутриорганизационной аудита.
Преимущества проверки по борьбе с отмыванием денег
AML-проверка позволяет криптовалютным биржам:
Придерживаться глобальные наряду с региональными законодательные нормы.
Оберегать владельцев недобросовестных действий.
Наращивать степень доверия со стороны участников и регуляторов.
Каким образом защитить себя при взаимодействии в криптосфере
Чтобы ограничить риски блокировки средств, следуйте данным рекомендациям:
Используйте проверенные платформы: Прибегайте лишь к обменникам с хорошей востребованностью наряду с высоким мерой защищенности.
Анализируйте получателей: Используйте AML-сервисы с целью проверки цифровых кошельков партнеров перед совершением транзакций.
Периодически обновляйте криптовалютные реквизиты: Указанная процедура поможет снизить гипотетических опасений, в случае если Ваши получатели окажутся в серых списках.
Сберегайте доказывающие материалы операций: Если наступит требовании получите возможность верифицировать законность принятых средств.
Подытоживая
Проверка по борьбе с отмыванием денег – является существенный средство для обеспечения защищенности операций на криптовалютном рынке. Эта практика оказывает содействие предотвратить сокрытие активов, поддержку незаконных инициатив помимо прочих незаконные мероприятия. Придерживаясь указаниям по безопасности и выбирая проверенные биржи, сможете уменьшить вероятности блокировки активов и наслаждаться защищенной взаимодействием с криптовалютами.
Puravive is a dietary supplement designed to support weight loss and overall metabolic health. By leveraging a blend of natural ingredients known for their fat-burning and metabolism-boosting properties, Puravive aims to help individuals achieve their weight management goals and enhance their overall well-being. https://sites.google.com/spsw.edu.pl/puravive-web/
Cardio Defend is a dietary supplement designed to support cardiovascular health. Utilizing a blend of natural ingredients, Cardio Defend aims to improve heart function, promote healthy blood pressure, and enhance overall cardiovascular wellness. This article explores the composition, benefits, clinical evidence, and user experiences related to Cardio Defend. https://sites.google.com/spsw.edu.pl/cardiodefend/
Kerassentials is a skincare and nail care product designed to promote healthy, strong nails and improve the overall condition of the skin. Combining natural and scientifically-backed ingredients, Kerassentials targets common issues such as fungal infections, brittle nails, and dry skin, providing a comprehensive solution for maintaining nail and skin health. https://sites.google.com/spsw.edu.pl/kerassentials-try/
EyeFortin is an all-natural eye-health supplement that helps to keep your eyes healthy even as you age. It prevents infections and detoxifies your eyes while also being stimulant-free. This makes it a great choice for those who are looking for a natural way to improve their eye health. https://sites.google.com/spsw.edu.pl/eyefortin/
Burn Boost is a dietary supplement designed to aid in weight management and fat loss. Combining a blend of natural ingredients, Burn Boost aims to increase metabolism, enhance energy levels, and support overall weight loss efforts. This article explores the composition, benefits, clinical evidence, and user experiences related to Burn Boost. https://sites.google.com/spsw.edu.pl/burnboost/
GlucoTrust is a dietary supplement designed to support healthy blood sugar levels and improve overall metabolic health. Combining a blend of natural ingredients known for their beneficial effects on blood sugar regulation, GlucoTrust aims to provide a comprehensive solution for individuals looking to manage their blood sugar levels naturally. This article explores the composition, benefits, clinical evidence, and user experiences related to GlucoTrust. https://sites.google.com/spsw.edu.pl/glucotrust/
Alpha Tonic is a dietary supplement designed to support male vitality, energy, and overall performance. Combining a blend of natural ingredients known for their beneficial effects on male health, Alpha Tonic aims to provide a comprehensive solution for men looking to enhance their physical and mental well-being. This article explores the composition, benefits, clinical evidence, and user experiences related to Alpha Tonic. https://sites.google.com/spsw.edu.pl/alphatonic/
Find out how Pedri https://barcelona.pedri-cz.com becomes a key figure for Barcelona – his development, influence and ambitions determine the club’s future success in world football.
A study of the influence of Rodrigo https://realmadrid.rodrygo-cz.com on the success and marketing strategy of Real Madrid: analysis of technical skills, popularity in Media and commercial success.
How Karim Benzema https://alIttihad.karim-benzema-cz.com changed the game of Al-Ittihad and Saudi football: new tactics, championship success, increased viewership and commercial success.
Find out about Alisson https://liverpool.alisson-becker-cz.com‘s influence on Liverpool’s success, from his defense to personal achievements that made him one of the best goalkeepers in the world.
Find out how Pedro Gavi https://barcelona.gavi-cz.com helped Barcelona achieve success thanks to his unique qualities, technique and leadership, becoming a key player in the team.
Red Boost is a dietary supplement formulated to support male vitality, enhance physical performance, and improve overall well-being. With a blend of potent natural ingredients, Red Boost aims to address common issues related to male health, such as low energy, reduced libido, and decreased stamina. This article delves into the composition, benefits, clinical evidence, and user experiences of Red Boost. https://sites.google.com/spsw.edu.pl/redboost/
You have made your point very well!!|
PotentStream is a dietary supplement designed to enhance male vitality, energy levels, and overall performance. Combining a blend of potent natural ingredients, PotentStream aims to provide a comprehensive solution for men experiencing issues related to low energy, reduced libido, and decreased stamina. This article explores the composition, benefits, clinical evidence, and user experiences of PotentStream.
https://sites.google.com/spsw.edu.pl/potentstream/
r7 casino вход https://mabiclub.ru
buy instant instagram views buy instagram views
Thibaut Courtois https://realmadrid.thibaut-courtois-cz.com the indispensable goalkeeper of “Real”, whose reliability, leadership and outstanding The game made him a key figure in the club.
Find out how Virgil van Dijk https://liverpool.virgil-van-dijk-cz.com became an integral part of style игры «Liverpool», ensuring the stability and success of the team.
Find out how Bruno Guimaraes https://newcastleunited.bruno-guimaraes-cz.com became a catalyst for the success of Newcastle United thanks to his technical abilities and leadership on the field and beyond.
Study of the playing style of Toni Kroos https://real-madrid.toni-kroos-cz.com at Real Madrid: his accurate passing, tactical flexibility and influence on the team’s success.
Romelu Lukaku https://chelsea.romelu-lukaku-cz.com, one of the best strikers in Europe, returns to Chelsea to continue climbing to the top of the football Olympus.
The young Uruguayan Darwin Nunez https://liverpool.darwin-nunez-cz.com broke into the elite of world football, and he became a key Liverpool player.
Star Brazilian striker Gabriel Jesus https://arsenal.gabriel-jesus-cz.com put in a superb performance to lead Arsenal to new heights after moving from Manchester City.
A fascinating story about how David Alaba https://realmadrid.david-alaba-cz.com after starting his career at the Austrian academy Vienna became a key player and leader of the legendary Real Madrid.
The story of how the incredibly talented footballer Riyad Mahrez https://alahli.riyad-mahrez-cz.com reached new heights in career, moving to Al Ahly and leading the team to victory.
The fascinating story of Antonio Rudiger’s transfer https://real-madrid.antonio-rudiger-cz.com to Real Madrid and his rapid rise as a key player at one of the best clubs in the world.
The fascinating story of Marcus Rashford’s ascent https://manchester-united.marcus-rashford-cz.com to glory in the Red Devils: from a young talent to one of the key players of the team.
Fascinating event related to this Keanu Reeves helped him in the role of the iconic John Wick characters https://john-wick.keanu-reeves.cz, among which there is another talent who has combat smarts with inappropriate charisma.
Try to make a fascinating actor Johnny Depp https://secret-window.johnny-depp.cz, who will become the slave of his strong hero Moudriho Creeps in the thriller “Secret Window”.
world of warcraft raid carry https://kreativwerkstatt-esens.de/ .
Jackie Chan https://peakhour.jackie-chan.cz from a poor boy from Hong Kong to a world famous Hollywood stuntman. The incredible success story of Jackie Chan.
Follow Liam Neeson’s career https://hostage.liam-neeson.cz as he fulfills his potential as Brian Mills in the film “Taken” and becomes one of the leading stars of Hollywood action films.
Emily Olivia Laura Blunt https://oppenheimer.emily-blunt.cz British and American actress. Winner of the Golden Globe (2007) and Screen Actors Guild (2019) awards.
슬롯 꽁 머니
모두가 속속 고개를 끄덕이며 다재다능합니다.
The inspiring story of Zendaya’s rise https://spider-man.zendaya-maree.cz, from her early roles to her blockbuster debut in Marvel Cinematic Universe.
The inspiring story of the ascent of the young actress Anya Taylor https://queensmove.anya-taylor-joy.cz to fame after her breakthrough performance in the TV series “The Queen’s Move”. Conquering new peaks.
An indomitable spirit, incredible skills and five championships – how Kobe Bryant https://losangeles-lakers.kobe-bryant.cz became an icon of the Los Angeles Lakers and the entire NBA world.
Carlos Vemola https://oktagon-mma.karlos-vemola.cz Czech professional mixed martial artist, former bodybuilder, wrestler and member Sokol.
Witness the thrilling story of Jiri Prochazka’s https://ufc.jiri-prochazka-ufc.cz rapid rise to the top of the UFC’s light heavyweight division, marked by his dynamic fighting style and relentless determination.
1xbet
Jon Jones https://ufc.jon-jones.cz a dominant fighter with unrivaled skill, technique and physique who has conquered the light heavyweight division.
An article about the triumphant 2023 Ferrari https://ferrari.charles-leclerc.cz and their star driver Charles Leclerc, who became the Formula world champion 1.
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
The legendary Spanish racer Fernando Alonso https://formula-1.fernando-alonso.cz returns to Formula 1 after several years.
Young Briton Lando Norris https://mclaren.lando-norris.cz is at the heart of McLaren’s Formula 1 renaissance, regularly achieving podium finishes and winning.
Activision and Call of Duty https://activision.call-of-duty.cz leading video game publisher and iconic shooter with a long history market dominance.
外送茶是什麼?禁忌、價格、茶妹等級、術語等..老司機告訴你!
外送茶是什麼?
外送茶、外約、叫小姐是一樣的東西。簡單來說就是在通訊軟體與茶莊聯絡,選好自己喜歡的妹子後,茶莊會像送飲料這樣把妹子派送到您指定的汽車旅館、酒店、飯店等交易地點。您只需要在您指定的地點等待,妹妹到達後,就可以開心的開始一場美麗的約會。
外送茶種類
學生兼職的稱為清新書香茶
日本女孩稱為清涼綠茶
俄羅斯女孩被稱為金酥麻茶
韓國女孩稱為超細滑人參茶
外送茶價格
外送茶的客戶相當廣泛,包括中小企業主、自營商、醫生和各行業的精英,像是工程師等等。在台北和新北地區,他們的消費指數大約在 7000 到 10000 元之間,而在中南部則通常在 4000 到 8000 元之間。
對於一般上班族和藍領階層的客人來說,建議可以考慮稍微低消一點,比如在北部約 6000 元左右,中南部約 4000 元左右。這個價位的茶妹大多是新手兼職,但有潛力。
不同地區的客人可以根據自己的經濟能力和喜好選擇適合自己的價位範圍,以免感到不滿意。物價上漲是一個普遍現象,受到地區和經濟情況等因素的影響,茶莊的成本也在上升,因此價格調整是合理的。
外送茶外約流程
加入LINE:加入外送茶官方LINE,客服隨時為你服務。茶莊一般在中午 12 點到凌晨 3 點營業。
告知所在地區:聯絡客服後,告訴他們約會地點,他們會幫你快速找到附近的茶妹。
溝通閒聊:有任何約妹問題或需要查看妹妹資訊,都能得到詳盡的幫助。
提供預算:告訴客服你的預算,他們會找到最適合你的茶妹。
提早預約:提早預約比較好配合你的空檔時間,也不用怕到時候約不到你想要的茶妹。
外送茶術語
喝茶術語就像是進入茶道的第一步,就像是蓋房子打地基一樣。在這裡,我們將這些外送茶入門術語分類,讓大家能夠清楚地理解,讓喝茶變得更加容易上手。
魚:指的自行接客的小姐,不屬於任何茶莊。
茶:就是指「小姐」的意思,由茶莊安排接客。
定點茶:指由茶莊提供地點,客人再前往指定地點與小姐交易。
外送茶:指的是到小姐到客人指定地點接客。
個工:指的是有專屬工作室自己接客的小姐。
GTO:指雞頭也就是飯店大姊三七茶莊的意思。
摳客妹:只負責找客人請茶莊或代調找美眉。
內機:盤商應召站提供茶園的人。
經紀人:幫內機找美眉的人。
馬伕:外送茶司機又稱教練。
代調:收取固定代調費用的人(只針對同業)。
阿六茶:中國籍女子,賣春的大陸妹。
熱茶、熟茶:年齡比較大、年長、熟女級賣春者(或稱阿姨)。
燙口 / 高溫茶:賣春者年齡過高。
台茶:從事此職業的台灣小姐。
本妹:從事此職業的日本籍小姐。
金絲貓:西方國家的小姐(歐美的、金髮碧眼的那種)。
青茶、青魚:20 歲以下的賣春者。
乳牛:胸部很大的小姐(D 罩杯以上)。
龍、小叮噹、小叮鈴:體型比較肥、胖、臃腫、大隻的小姐。
montenegro housing villas for sale in Montenegro
the most popular sports website https://sports-forecasts.com in the Arab world with the latest sports news, predictions and analysis in real time.
Latest news and analysis of the English Premier League https://epl-ar.com. Detailed descriptions of matches, team statistics and the most interesting football events.
Free movies https://www.moviesjoy.cc and TV streaming online, watch movies online in HD 1080p.
Latest Diablo news https://diablo-ar.com, detailed game descriptions and guides. Diablo.az – The largest Diablo information portal in Arabic.
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Latest World of Warcraft tournament news https://ar-wow.com (WOW), strategies and game analysis. The most detailed gaming portal in Arabic.
The latest analysis, reviews of https://spider-man-ar.com tournaments and the most interesting things from the “Spider-Man” series of games in Azerbaijani language. It’s all here!
NFL https://nfl-ar.com News, analysis and topics about the latest practices, victories and records. A portal that explores the most beautiful games in the NFL world in general.
Discover exciting virtual football https://fortnite-ar.com in Fortnite. Your central hub for the latest news, expert strategy and exciting eSports reporting.
Latest Counter-Strike 2 news https://counter-strike-ar.com, watch the most successful tournaments and be the best in the gaming world on CS2 ar.
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Latest boxing news, achievements of Raisol Abbasov https://boxing-ar.com, Tyson Fury fights and much more. It’s all about the boxing ambassador.
Discover the wonderful world of online games https://onlayn-oyinlar.com with GameHub. Get the latest news, reviews and tips for your favorite games. Join our gaming community today!
Sports news https://gta-uzbek.com the most respected sports site in Uzbekistan, which contains the latest sports news, forecasts and analysis.
Latest GTA game news https://gta-uzbek.com, tournaments, guides and strategies. Stay tuned for the best GTA gaming experience
Explore the extraordinary journey of Kylian Mbappe https://mbappe-real-madrid.com, from his humble beginnings to global stardom.
Latest news about Pele https://mesut-ozil-uz.com, statistics, photos and much more. Get the latest news and information about football legend Pele.
Get the latest https://mesut-ozil-uz.com Mesut Ozil news, stats, photos and more.
Online work has transformed the modern workplace, providing flexibility and accessibility that conventional office environments typically lack. It enables individuals to work from any location with an internet connection, removing geographical barriers and allowing companies to tap into a international talent pool. This change has led to a rise in remote and freelance opportunities, allowing workers to balance their professional and personal lives more efficiently. Additionally, online work can lead to increased productivity and job satisfaction, as employees have more control over their timelines and work environments. However, it also presents challenges such as maintaining work-life boundaries, ensuring effective communication, and managing time efficiently. Overall, online work is a revolutionary force, reshaping the way we think about employment and productivity in the digital age.
Serxio Ramos Garsiya https://serxio-ramos.com ispaniyalik futbolchi, himoyachi. Ispaniya terma jamoasining sobiq futbolchisi. 16 mavsum davomida u “Real Madrid”da markaziy himoyachi sifatida o’ynadi.
Ronaldo de Asis Moreira https://ronaldinyo.com braziliyalik futbolchi, yarim himoyachi va hujumchi sifatida o’ynagan. Jahon chempioni (2002). “Oltin to’p” sovrindori (2005).
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Официальный сайт онлайн-казино Vavada https://vavada-kz-game.kz это новый адрес лучших слотов и джекпотов. Ознакомьтесь с бонусами и играйте на реальные деньги из Казахстана.
Marcus Lilian Thuram-Julien https://internationale.marcus-thuram-fr.com French footballer, forward for the Internazionale club and French national team.
Legendary striker Cristiano Ronaldo https://an-nasr.cristiano-ronaldo-fr.com signed a contract with the Saudi club ” An-Nasr”, opening a new chapter in his illustrious career in the Middle East.
Manchester City and Erling Haaland https://manchester-city.erling-haaland-fr.com explosive synergy in action. How a club and a footballer light up stadiums with their dynamic play.
Lionel Messi https://inter-miami.lionel-messi-fr.com legendary Argentine footballer, announced his transfer to the American club Inter Miami.
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
The official website where you can find everything about the career of Gianluigi Buffon https://gianluigi-buffon.com. Discover the story of this legendary goalkeeper who left his mark on football history and relive his achievements and unforgettable memories with us.
Website dedicated to football player Paul Pogba https://pogba-uz.com. Latest news from the world of football.
Welcome to our official website! Go deeper into Paulo Dybala’s https://paulo-dybala.com football career. Discover Dybala’s unforgettable moments, amazing talents and fascinating journey in the world of football on this site.
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Coffeeroom https://coffeeroom.by – магазин кофе, чая, кофетехники, посуды, химии и аксессуаров в Минске для дома и офиса.
Latest news on the Vinicius Junior fan site https://vinisius-junior.com. Vinicius Junior has been playing since 2018 for Real Madrid (Real Madrid). He plays in the Left Winger position.
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Прокат и аренда автомобилей https://autorent.by в Минске 2019-2022. Сутки от 35 руб.
外送茶是什麼?禁忌、價格、茶妹等級、術語等..老司機告訴你!
外送茶是什麼?
外送茶、外約、叫小姐是一樣的東西。簡單來說就是在通訊軟體與茶莊聯絡,選好自己喜歡的妹子後,茶莊會像送飲料這樣把妹子派送到您指定的汽車旅館、酒店、飯店等交易地點。您只需要在您指定的地點等待,妹妹到達後,就可以開心的開始一場美麗的約會。
外送茶種類
學生兼職的稱為清新書香茶
日本女孩稱為清涼綠茶
俄羅斯女孩被稱為金酥麻茶
韓國女孩稱為超細滑人參茶
外送茶價格
外送茶的客戶相當廣泛,包括中小企業主、自營商、醫生和各行業的精英,像是工程師等等。在台北和新北地區,他們的消費指數大約在 7000 到 10000 元之間,而在中南部則通常在 4000 到 8000 元之間。
對於一般上班族和藍領階層的客人來說,建議可以考慮稍微低消一點,比如在北部約 6000 元左右,中南部約 4000 元左右。這個價位的茶妹大多是新手兼職,但有潛力。
不同地區的客人可以根據自己的經濟能力和喜好選擇適合自己的價位範圍,以免感到不滿意。物價上漲是一個普遍現象,受到地區和經濟情況等因素的影響,茶莊的成本也在上升,因此價格調整是合理的。
外送茶外約流程
加入LINE:加入外送茶官方LINE,客服隨時為你服務。茶莊一般在中午 12 點到凌晨 3 點營業。
告知所在地區:聯絡客服後,告訴他們約會地點,他們會幫你快速找到附近的茶妹。
溝通閒聊:有任何約妹問題或需要查看妹妹資訊,都能得到詳盡的幫助。
提供預算:告訴客服你的預算,他們會找到最適合你的茶妹。
提早預約:提早預約比較好配合你的空檔時間,也不用怕到時候約不到你想要的茶妹。
外送茶術語
喝茶術語就像是進入茶道的第一步,就像是蓋房子打地基一樣。在這裡,我們將這些外送茶入門術語分類,讓大家能夠清楚地理解,讓喝茶變得更加容易上手。
魚:指的自行接客的小姐,不屬於任何茶莊。
茶:就是指「小姐」的意思,由茶莊安排接客。
定點茶:指由茶莊提供地點,客人再前往指定地點與小姐交易。
外送茶:指的是到小姐到客人指定地點接客。
個工:指的是有專屬工作室自己接客的小姐。
GTO:指雞頭也就是飯店大姊三七茶莊的意思。
摳客妹:只負責找客人請茶莊或代調找美眉。
內機:盤商應召站提供茶園的人。
經紀人:幫內機找美眉的人。
馬伕:外送茶司機又稱教練。
代調:收取固定代調費用的人(只針對同業)。
阿六茶:中國籍女子,賣春的大陸妹。
熱茶、熟茶:年齡比較大、年長、熟女級賣春者(或稱阿姨)。
燙口 / 高溫茶:賣春者年齡過高。
台茶:從事此職業的台灣小姐。
本妹:從事此職業的日本籍小姐。
金絲貓:西方國家的小姐(歐美的、金髮碧眼的那種)。
青茶、青魚:20 歲以下的賣春者。
乳牛:胸部很大的小姐(D 罩杯以上)。
龍、小叮噹、小叮鈴:體型比較肥、胖、臃腫、大隻的小姐。
Find the latest information on Khabib Nurmagomedov https://khabib-nurmagomedov.uz news and fights. Check out articles and videos detailing Khabib UFC career, interviews, wins, and biography.
Latest news and information about Marcelo https://marselo-uz.com on this site! Find Marcelo’s biography, career, game stats and more.
Dedicated to the brave players!!
I’ve been a satisfied player at MCW Casino for several months. The bonuses are generous, withdrawals are fast, and the working mirror is consistently accessible. With simple registration and a convenient site layout, MCW Casino is my top choice for both betting and casino games. I recommend it to everyone!
At MCW Casino, I found everything I was looking for: high odds, a variety of games, and generous bonuses. The working mirror is always accessible, and withdrawals are processed without delays. I recommend MCW Casino to everyone looking for a top-notch gaming experience!
Catch the site where everything is in the best shape! – MCW Casino
how to withdraw money from MCW Casino
current mirror MCW Casino
MCW Casino promo code working
Mega Casino World apk download for Android
how to bet bonuses on MCW Casino
Good profits!
Dedicated to the brave players!!
Discover the path to victory with Baji999 Casino! Enjoy a secure and exciting gaming experience with fantastic bonuses. Join the Baji999 community and start winning now!
Step into success with Baji999! Experience the best in online casino gaming and sports betting. With attractive bonuses and a secure platform, Baji999 is your key to winning big. Join and play today!
Catch the site where everything is in the best shape! – Baji999
Baji999 Casino review
download Baji999 Casino slots on android for free
Baji999 Casino official app for free
bonus Baji999 Casino how to wager
Baji999 Casino download mirror for today
Good profits!
Discover how Riyad Mahrez https://al-ahli.riyad-mahrez.com transformed Al-Ahli, becoming a key player and catalyst in reaching new heights in world football.
Find the latest information on Conor McGregor https://conor-mcgregor.uz news, fights, and interviews. Check out detailed articles and news about McGregor’s UFC career, wins, training, and personal life.
Explore the dynamic world of sports https://noticias-esportivas-br.org through the lens of a sports reporter. Your source for breaking news, exclusive interviews, in-depth analysis and live coverage of all sports.
Get to know the history, players and latest news of the Inter Miami football club https://inter-miami.uz. Join us to learn about the successes and great performances of America’s newest and most exciting soccer club.
A site dedicated to Michael Jordan https://michael-jordan.uz, a basketball legend and symbol of world sports culture. Here you will find highlights, career, family and news about one of the greatest athletes of all time.
The latest top football news https://futebol-ao-vivo.net today. Interviews with football players, online broadcasts and match results, analytics and football forecasts
Site with the latest news, statistics, photos of Pele https://edson-arantes-do-nascimento.com and much more. Get the latest news and information about football legend Pele.
Welcome to our official website, where you will find everything about the career of Gianluigi Buffon https://gianluigi-buffon.org. Discover the story of this legendary goalkeeper who made football history.
If you are a fan of UFC https://ufc-hoje.com the most famous organization in the world, come visit us. The most important news and highlights from the UFC world await you on our website.
The best site dedicated to the football player Paul Pogba https://pogba.org. Latest news from the world of football.
Vinicius Junior https://vinicius-junior.org all the latest current and latest news for today about the player of the 2024 season
Analysis of Arsenal’s impressive revival https://arsenal.bukayo-saka.biz under the leadership of Mikel Arteta and the key role of young star Bukayo Saki in the club’s return to the top.
Gavi’s success story https://barcelona.gavi-fr.com at Barcelona: from his debut at 16 to a key role in club and national team of Spain, his talent inspires the world of football.
Pedri’s story https://barcelona.pedri-fr.com from his youth in the Canary Islands to becoming a world-class star in Barcelona, ??with international success and recognition.
Discover the journey of Charles Leclerc https://ferrari.charles-leclerc-fr.com, from young Monegasque driver to Ferrari Formula 1 leader, from his early years to his main achievements within the team.
Discover Pierre Gasly’s https://alpine.pierre-gasly.com journey through the world of Formula 1, from his beginnings with Toro Rosso to his extraordinary achievements with Alpine.
Gerakl24: Опытная Смена Основания, Венцов, Покрытий и Перенос Строений
Фирма Gerakl24 специализируется на предоставлении комплексных работ по реставрации фундамента, венцов, настилов и передвижению зданий в месте Красноярске и за его пределами. Наш коллектив опытных мастеров гарантирует превосходное качество выполнения различных типов реставрационных работ, будь то из дерева, каркасные, из кирпича или из бетона строения.
Преимущества услуг Gerakl24
Профессионализм и опыт:
Все работы проводятся только опытными мастерами, с обладанием долгий опыт в сфере возведения и реставрации домов. Наши мастера эксперты в своей области и осуществляют задачи с максимальной точностью и учетом всех деталей.
Полный спектр услуг:
Мы предоставляем все виды работ по восстановлению и ремонту домов:
Смена основания: укрепление и замена старого фундамента, что обеспечивает долгий срок службы вашего здания и избежать проблем, вызванные оседанием и деформацией.
Реставрация венцов: реставрация нижних венцов из дерева, которые наиболее часто подвергаются гниению и разрушению.
Установка новых покрытий: замена старых полов, что значительно улучшает визуальное восприятие и практическую полезность.
Перемещение зданий: безопасное и качественное передвижение домов на новые локации, что позволяет сохранить ваше строение и избежать дополнительных затрат на создание нового.
Работа с различными типами строений:
Деревянные дома: восстановление и укрепление деревянных конструкций, защита от гниения и вредителей.
Каркасные дома: укрепление каркасов и замена поврежденных элементов.
Дома из кирпича: ремонт кирпичных стен и укрепление конструкций.
Бетонные дома: реставрация и усиление бетонных элементов, устранение трещин и повреждений.
Качество и надежность:
Мы используем только проверенные материалы и новейшее оборудование, что гарантирует долгий срок службы и надежность всех работ. Все наши проекты подвергаются строгому контролю качества на каждом этапе выполнения.
Персонализированный подход:
Для каждого клиента мы предлагаем персонализированные решения, с учетом всех особенностей и пожеланий. Мы стараемся, чтобы итог нашей работы соответствовал вашим ожиданиям и требованиям.
Почему выбирают Геракл24?
Обратившись к нам, вы приобретете надежного партнера, который берет на себя все заботы по ремонту и реставрации вашего дома. Мы обещаем выполнение всех задач в сроки, оговоренные заранее и с в соответствии с нормами и стандартами. Выбрав Геракл24, вы можете не сомневаться, что ваш дом в надежных руках.
Мы готовы предоставить консультацию и ответить на ваши вопросы. Контактируйте с нами, чтобы обсудить детали и узнать о наших сервисах. Мы обеспечим сохранение и улучшение вашего дома, обеспечив его безопасность и комфорт на долгие годы.
Gerakl24 – ваш партнер по реставрации и ремонту домов в Красноярске и окрестностях.
https://gerakl24.ru/поднять-дом-красноярск/
Discover the story of Rudy Gobert https://minnesota-timberwolves.rudy-gobert.biz, the French basketball player whose defensive play and leadership transformed the Minnesota Timberwolves into a powerhouse NBA team.
From childhood teams to championship victories, the path to success with the Los Angeles Lakers https://los-angeles-lakers.lebron-james-fr.com requires not only talent, but also undeniable dedication and work.
Leroy Sane’s https://bavaria.leroy-sane-ft.com success story at FC Bayern Munich: from adaptation to influence on the club’s results. Inspiration for hard work and professionalism in football.
Gerakl24: Профессиональная Реставрация Основания, Венцов, Полов и Перенос Зданий
Организация Геракл24 специализируется на оказании всесторонних сервисов по реставрации фундамента, венцов, полов и перемещению строений в месте Красноярском регионе и за его пределами. Наша группа опытных экспертов обеспечивает отличное качество исполнения различных типов восстановительных работ, будь то древесные, каркасные, кирпичные постройки или бетонные конструкции здания.
Преимущества услуг Gerakl24
Квалификация и стаж:
Все работы проводятся только профессиональными специалистами, имеющими долгий стаж в сфере создания и реставрации домов. Наши мастера эксперты в своей области и реализуют задачи с максимальной точностью и вниманием к деталям.
Комплексный подход:
Мы предоставляем разнообразные услуги по ремонту и реконструкции строений:
Замена фундамента: укрепление и замена старого фундамента, что позволяет продлить срок службы вашего строения и предотвратить проблемы, связанные с оседанием и деформацией.
Реставрация венцов: восстановление нижних венцов деревянных зданий, которые наиболее часто подвергаются гниению и разрушению.
Установка новых покрытий: установка новых полов, что значительно улучшает внешний облик и практическую полезность.
Передвижение домов: безопасное и надежное перемещение зданий на другие участки, что помогает сохранить здание и избежать дополнительных затрат на строительство нового.
Работа с любыми видами зданий:
Дома из дерева: реставрация и усиление деревянных элементов, обработка от гниения и насекомых.
Каркасные строения: усиление каркасных конструкций и реставрация поврежденных элементов.
Кирпичные строения: восстановление кирпичной кладки и укрепление конструкций.
Бетонные дома: реставрация и усиление бетонных элементов, ремонт трещин и дефектов.
Надежность и долговечность:
Мы работаем с только проверенные материалы и современное оборудование, что гарантирует долгий срок службы и прочность всех выполненных задач. Все проекты проходят строгий контроль качества на каждой стадии реализации.
Личный подход:
Для каждого клиента мы предлагаем индивидуальные решения, учитывающие ваши требования и желания. Мы стремимся к тому, чтобы результат нашей работы полностью соответствовал вашим запросам и желаниям.
Зачем обращаться в Геракл24?
Работая с нами, вы найдете надежного партнера, который возьмет на себя все хлопоты по ремонту и реставрации вашего дома. Мы гарантируем выполнение всех проектов в установленные сроки и с в соответствии с нормами и стандартами. Обратившись в Геракл24, вы можете не сомневаться, что ваше здание в надежных руках.
Мы предлагаем консультацию и ответить на ваши вопросы. Свяжитесь с нами, чтобы обсудить ваш проект и узнать о наших сервисах. Мы поможем вам сохранить и улучшить ваш дом, сделав его безопасным и комфортным для проживания на долгие годы.
Геракл24 – ваш надежный партнер в реставрации и ремонте домов в Красноярске и за его пределами.
Игроки могут участвовать в программе VIP-клуба казино 7k casino – 7k casino официальный сайт зеркало
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
The story of the Moroccan footballer https://al-hilal.yassine-bounou.com, who became a star at Al-Hilal, traces his journey from the streets of Casablanca to international football stardom and his personal development.
Victor Wembanyama’s travel postcard https://san-antonio-spurs.victor-wembanyama.biz from his career in France to his impact in the NBA with the San Antonio Spurs.
Neymar https://al-hilal.neymar-fr.com at Al-Hilal: his professionalism and talent inspire young people players, taking the club to new heights in Asian football.
The history of Michael Jordan’s Chicago Bulls https://chicago-bulls.michael-jordan-fr.com extends from his rookie in 1984 to a six-time NBA championship.
Golden State Warriors success story https://golden-state-warriors.stephen-curry-fr.com Stephen Curry: From becoming a leader to creating a basketball dynasty that redefined the game.
Del Mar Energy Inc is an international industrial holding company engaged in the extraction of oil, gas, and coal
The success story of the French footballer https://juventus.thierry-henry.biz at Juventus: from his career at the club to leadership on the field , becoming a legend and a source of inspiration for youth.
The story of the great Kobe Bryant https://los-angeles-lakers.kobe-bryant-fr.com with ” Los Angeles Lakers: his path to the championship, his legendary achievements.
Novak Djokovic’s https://tennis.novak-djokovic-fr.biz journey from childhood to the top of world tennis: early years, first victories, dominance and influence on the sport.
Find out the story of Jon Jones https://ufc.jon-jones-fr.biz in the UFC: his triumphs, records and controversies, which made him one of the greatest fighters in the MMA world.
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Казино 7к казино предлагает захватывающий игровой опыт с яркой визуальной графикой – игровые автоматы r7 casino регистрация
娛樂城
Мы стремились создать нечто особенное, когда запустили бренд казино 7k casino в 2023 году, и рады видеть, что азартные игроки оценили наше качество и разнообразие услуг, делая нас одними из лидеров в рейтинге казино – р7 казино новое зеркало
Вывод средств осуществляется в течение суток в букмекерской конторе 7к казино – рабочее зеркало сайта
В казино 7k casino доступны различные игры – рабочее зеркало сайта 7k casino
Располагается на главной странице сайта casino информация о букмекерской конторе 7к казино – официальный р7 казино
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Основанный в 2023 году, бренд казино Marathonbet сразу завоевал популярность среди азартных игроков своим высоким уровнем качества и разнообразием услуг, что делает его потенциальным лидером среди других казино – БК Марафон официальный сайт зеркало
Jannik Sinner https://tennis.jannik-sinner-fr.biz an Italian tennis player, went from starting his career to entering the top 10 of the ATP, demonstrating unique abilities and ambitions in world tennis.
В казино 7k casino можно играть на виртуальные фишки для тренировки и развлечения – р7 казино на сегодня
Carlos Alcaraz https://tennis.carlos-alcaraz-fr.biz from a talented junior to the ATP top 10. His rise is the result of hard work, support and impressive victories at major world tournaments.
The fascinating story of Daniil Medvedev’s https://tennis.daniil-medvedev-fr.biz rise to world number one. Find out how a Russian tennis player quickly broke into the elite and conquered the tennis Olympus.
The fascinating story of Alexander Zverev’s https://tennis.alexander-zverev-fr.biz rapid rise from a junior star to one of the leaders of modern tennis.
Discover Casper Ruud’s https://tennis.casper-ruud-fr.com journey from his Challenger debut to the top 10 of the world tennis rankings. A unique success.
Бренд казино 7k casino, появившийся в 2023 году, сразу же привлек внимание поклонников азартных игр своей уникальностью и широким выбором услуг, что может сделать его одним из лидеров в рейтинге лучших казино – зеркало r7 casino
В казино 7k casino доступны игры с различными уровнями ставок, чтобы удовлетворить игроков с любым бюджетом – онлайн 7k casino официальный сайт
Казино 7k casino, основанное в 2023 году, мгновенно привлекло внимание азартных игроков своим качеством и разнообразием услуг, возглавляя рейтинг – 7k casino без регистрации
Казино 7k casino, запущенное в 2023 году, немедленно привлекло внимание азартных игроков своим качеством и разнообразием услуг, стремясь занять первое место в рейтинге – 7k casino официальный сайт лицензионный зеркало
wow boost raid kreativwerkstatt-esens.de .
NetTruyen ZZZ: Nền tảng đọc truyện tranh trực tuyến dành cho mọi lứa tuổi
NetTruyen ZZZ là nền tảng đọc truyện tranh trực tuyến miễn phí với số lượng truyện tranh lên đến hơn 30.000 đầu truyện với chất lượng hình ảnh và tốc độ tải cao. Nền tảng được xây dựng với mục tiêu mang đến cho người đọc những trải nghiệm đọc truyện tranh tốt nhất, đồng thời tạo dựng cộng đồng yêu thích truyện tranh sôi động và gắn kết với hơn 11 triệu thành viên (tính đến tháng 7 năm 2024).
NetTruyen ZZZ – Kho tàng truyện tranh phong phú:
NetTruyen ZZZ sở hữu kho tàng truyện tranh khổng lồ với hơn 30.000 đầu truyện thuộc nhiều thể loại khác nhau như:
● Manga: Những bộ truyện tranh Nhật Bản với nhiều thể loại phong phú như lãng mạn, hành động, hài hước, v.v.
● NetTruyen anime: Hàng ngàn bộ truyện tranh anime chọn lọc được đăng tải đều đặn trên NetTruyen ZZZ được chuyển thể từ phim hoạt hình Nhật Bản với nội dung hấp dẫn và hình ảnh đẹp mắt.
● Truyện manga: Hơn 10.000 bộ truyện tranh manga hay nhất được đăng tải đầy đủ trên NetTruyen ZZZ.
● Truyện manhua: Hơn 5000 bộ truyện tranh manhua được đăng tải trọn bộ đầy đủ trên NetTruyen ZZZ.
● Truyện manhwa: Những bộ truyện tranh manhwa Hàn Quốc được yêu thích nhất có đầy đủ trên NetTruyen với cốt truyện lôi cuốn và hình ảnh bắt mắt cùng với nét vẽ độc đáo và nội dung đa dạng.
● Truyện ngôn tình: Những câu chuyện tình yêu lãng mạn, ngọt ngào và đầy cảm xúc.
● Truyện trinh thám: Những câu chuyện ly kỳ, bí ẩn và đầy lôi cuốn xoay quanh các vụ án và quá trình phá án.
● Truyện tranh xuyên không: Những câu chuyện về những nhân vật du hành thời gian hoặc không gian đến một thế giới khác.
NetTruyen ZZZ không ngừng cập nhật những bộ truyện tranh mới nhất và hot nhất trên thị trường, đảm bảo mang đến cho bạn đọc những trải nghiệm đọc truyện mới mẻ và thú vị nhất.
Chất lượng hình ảnh và nội dung đỉnh cao tại NetTruyenZZZ:
Với hơn 30 triệu lượt truy cập hằng tháng, NetTruyen ZZZ luôn chú trọng vào chất lượng hình ảnh và nội dung của các bộ truyện tranh được đăng tải trên nền tảng. Hình ảnh được hiển thị sắc nét, rõ ràng, không bị mờ hay vỡ ảnh. Nội dung được dịch thuật chính xác, dễ hiểu và giữ nguyên vẹn ý nghĩa của tác phẩm gốc.
NetTruyen ZZZ hợp tác với đội ngũ dịch giả và biên tập viên chuyên nghiệp, giàu kinh nghiệm để đảm bảo chất lượng bản dịch tốt nhất. Nền tảng cũng có hệ thống kiểm duyệt nội dung nghiêm ngặt để đảm bảo nội dung lành mạnh, phù hợp với mọi lứa tuổi.
Trải nghiệm đọc truyện mượt mà, tiện lợi:
NetTruyen ZZZ được thiết kế với giao diện đẹp mắt, thân thiện với người dùng và dễ dàng sử dụng. Bạn đọc có thể đọc truyện tranh trên mọi thiết bị, từ máy tính, điện thoại thông minh đến máy tính bảng. Nền tảng cũng cung cấp nhiều tính năng tiện lợi như:
● Tìm kiếm truyện tranh theo tên, tác giả, thể loại, v.v.
● Lưu truyện tranh yêu thích để đọc sau.
● Đánh dấu trang để dễ dàng quay lại vị trí đang đọc.
● Chia sẻ truyện tranh với bạn bè.
● Tham gia bình luận và thảo luận về truyện tranh.
NetTruyen ZZZ luôn nỗ lực để mang đến cho bạn đọc những trải nghiệm đọc truyện mượt mà, tiện lợi và thú vị nhất.
Định hướng phát triển:
NetTruyen ZZZ cam kết không ngừng phát triển và hoàn thiện để trở thành nền tảng đọc truyện tranh trực tuyến tốt nhất dành cho bạn đọc tại Việt Nam. Nền tảng sẽ tiếp tục cập nhật những bộ truyện tranh mới nhất và hot nhất trên thị trường thế giới, đồng thời nâng cao chất lượng hình ảnh và nội dung. NetTruyen ZZZ cũng sẽ phát triển thêm nhiều tính năng mới để mang đến cho bạn đọc những trải nghiệm đọc truyện tốt nhất.
NetTruyen ZZZ luôn đặt lợi ích của bạn đọc lên hàng đầu. Nền tảng cam kết:
● Cung cấp kho tàng truyện tranh khổng lồ và đa dạng với chất lượng hình ảnh và nội dung đỉnh cao.
● Mang đến cho bạn đọc những trải nghiệm đọc truyện mượt mà, tiện lợi và thú vị nhất.
● Luôn lắng nghe ý kiến phản hồi của bạn đọc và không ngừng cải thiện để mang đến dịch vụ tốt nhất.
NetTruyen ZZZ hy vọng sẽ trở thành người bạn đồng hành không thể thiếu của bạn trong hành trình khám phá thế giới truyện tranh đầy màu sắc.
Kết nối với NetTruyen ZZZ ngay hôm nay để tận hưởng những trải nghiệm đọc truyện tuyệt vời.
Вывод средств в Риобет осуществляется в течение 24 часов с оперативностью – Риобет рабочее зеркало
Геракл24: Опытная Реставрация Фундамента, Венцов, Покрытий и Перенос Зданий
Компания Gerakl24 специализируется на оказании всесторонних работ по реставрации фундамента, венцов, настилов и передвижению зданий в городе Красноярск и в окрестностях. Наша команда опытных экспертов обещает превосходное качество реализации всех видов восстановительных работ, будь то деревянные, с каркасом, из кирпича или бетонные конструкции дома.
Достоинства сотрудничества с Геракл24
Навыки и знания:
Все работы осуществляются только опытными мастерами, имеющими большой практику в направлении возведения и ремонта зданий. Наши сотрудники профессионалы в своем деле и реализуют работу с максимальной точностью и вниманием к мелочам.
Всесторонний подход:
Мы предлагаем полный спектр услуг по восстановлению и реконструкции строений:
Реставрация фундамента: укрепление и замена старого фундамента, что обеспечивает долгий срок службы вашего строения и избежать проблем, связанные с оседанием и деформацией.
Замена венцов: реставрация нижних венцов из дерева, которые обычно подвергаются гниению и разрушению.
Установка новых покрытий: замена старых полов, что существенно улучшает визуальное восприятие и функциональность помещения.
Перемещение зданий: качественный и безопасный перенос строений на новые места, что помогает сохранить здание и избежать дополнительных затрат на строительство нового.
Работа с любыми видами зданий:
Древесные строения: реставрация и усиление деревянных элементов, защита от разрушения и вредителей.
Каркасные строения: укрепление каркасов и смена поврежденных частей.
Кирпичные дома: ремонт кирпичных стен и усиление стен.
Бетонные дома: ремонт и укрепление бетонных конструкций, исправление трещин и разрушений.
Качество и надежность:
Мы работаем с только проверенные материалы и передовые технологии, что гарантирует долгий срок службы и надежность всех выполненных работ. Все наши проекты проходят тщательную проверку качества на каждой стадии реализации.
Персонализированный подход:
Мы предлагаем каждому клиенту подходящие решения, учитывающие все особенности и пожелания. Мы стараемся, чтобы итог нашей работы полностью удовлетворял ваши ожидания и требования.
Почему стоит выбрать Геракл24?
Обратившись к нам, вы приобретете надежного партнера, который возьмет на себя все заботы по ремонту и реставрации вашего дома. Мы гарантируем выполнение всех проектов в сроки, установленные договором и с соблюдением всех строительных норм и стандартов. Выбрав Геракл24, вы можете быть уверены, что ваше здание в надежных руках.
Мы готовы предоставить консультацию и ответить на все ваши вопросы. Звоните нам, чтобы обсудить ваш проект и узнать о наших сервисах. Мы сохраним и улучшим ваш дом, обеспечив его безопасность и комфорт на долгие годы.
Геракл24 – ваш надежный партнер в реставрации и ремонте домов в Красноярске и за его пределами.
https://gerakl24.ru/поднять-дом-красноярск/
The powerful story of Conor McGregor’s https://ufc.conor-mcgregor-fr.biz rise to a two-division UFC championship that forever changed the landscape of mixed martial arts.
The legendary boxing world champion Mike Tyson https://ufc.mike-tyson-fr.biz made an unexpected transition to the UFC in 2024, where he rose to the top, becoming the oldest heavyweight champion.
The story of Fernando Alonso https://formula-1.fernando-alonso-fr.com in Formula 1: a unique path to success through talent, tenacity and strategic decisions, inspiring and exciting.
The fascinating story of how Lewis Hamilton https://mercedes.lewis-hamilton-fr.biz became a seven-time Formula 1 world champion after signing with Mercedes.
Наше сегодняшнее рабочее зеркало официального сайта букмекерской конторы Риобет обеспечивает легкий доступ к нашим услугам, независимо от вашего местоположения – Riobet игровые автоматы официальный сайт
The fascinating story of the creation and rapid growth of Facebook https://facebook.mark-zuckerberg-fr.biz under the leadership of Mark Zuckerberg, who became one of the most influential technology entrepreneurs of our time.
В казино Riobet доступны игры с различными тематиками, чтобы каждый игрок мог найти что-то по своему вкусу – Riobet официальный
Kim Kardashian’s https://the-kardashians.kim-kardashian-fr.com incredible success story, from sex scandal to pop culture icon and billion-dollar fortune.
Max Verstappen and Red Bull Racing’s https://red-bull-racing.max-verstappen-fr.com path to success in Formula 1. A story of talent, determination and team support leading to a championship title.
The astonishing story of Emmanuel Macron’s https://president-of-france.emmanuel-macron-fr.com political rise from bank director to the highest office in France.
The story of Joe Biden’s https://president-of-the-usa.joe-biden-fr.com triumphant journey, overcoming many obstacles on his path to the White House and becoming the 46th President of the United States.
Une ascension fulgurante au pouvoir Donald Trump https://usa.donald-trump-fr.com et son empire commercial
Parisian PSG https://paris.psg-fr.com is one of the most successful and ambitious football clubs in Europe. Find out how he became a global football superstar.
Travel to the pinnacle of French football https://stadede-bordeaux.bordeaux-fr.org at the Stade de Bordeaux, where the passion of the game meets the grandeur of architecture.
Olympique de Marseille https://liga1.marseilles-fr.com after several years in the shadows, once again becomes champion of France. How did they do it and what prospects open up for the club
The fascinating story of Gigi Hadid’s rise to Victoria’s Secret Angel https://victorias-secret.gigi-hadid-fr.com status and her journey to the top of the modeling industry.
The fascinating story of the creation and meteoric rise of Amazon https://amazon.jeff-bezos-fr.com from its humble beginnings as an online bookstore to its dominant force in the world of e-commerce.
A fascinating story about how Elon Musk https://spacex.elon-musk-fr.com and his company SpaceX revolutionized space exploration, opening new horizons for humanity.
The inspiring story of Travis Scott’s https://yeezus.travis-scott-fr.com rise from emerging artist to one of modern hip-hop’s brightest stars through his collaboration with Kanye West.
An exploration of Nicole Kidman’s https://watch.nicole-kidman-fr.com career, her notable roles, and her continued quest for excellence as an actress.
How Taylor Swift https://midnights.taylor-swift-fr.com reinvented her sound and image on the intimate and reflective album “Midnights,” revealing new dimensions of her talent.
Explore the rich history and unrivaled atmosphere of the iconic Old Trafford Stadium https://old-trafford.manchester-united-fr.com, home of one of the world’s most decorated football clubs, Manchester United.
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Казино 7k casino, основанное в 2023 году, быстро привлекло внимание поклонников азартных игр своим новаторским подходом и широким спектром услуг, что делает его потенциальным фаворитом в рейтинге лучших казино – работающее зеркало страницы 7к казино
Казино 7k casino предлагает выгодные бонусные программы для своих игроков – 7k casino официальный сайт рабочее зеркало
Главная страница сайта casino является информационным хабом для 7к казино, где пользователи могут найти подробности о предложениях и услугах букмекерской конторы – р7 казино официальный сайт мобильная версия
montenegro beaches Budva Montenegro
В казино 7k casino я могу насладиться высокой отдачей на игровых автоматах – рабочее зеркало страницы
Единственная в России студия кастомных париков https://wigdealers.ru, где мастера индивидуально подбирают структуру волос и основу по форме головы, после чего стригут, окрашивают, делают укладку и доводят до идеала ваш будущий аксессуар.
The iconic Anfield https://enfield.liverpool-fr.com stadium and the passionate Liverpool fans are an integral part of English football culture.
An exploration of the history of Turin’s https://turin.juventus-fr.org iconic football club – Juventus – its rivalries, success and influence on Italian football.
The new Premier League https://premier-league.chelsea-fr.com season has gotten off to an intriguing start, with a new-look Chelsea looking to return to the Champions League, but serious challenges lie ahead.
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hello everyone !
Sign up now and start exploring the endless entertainment possibilities with http://www.limelight-stream.com Whether you’re looking to unwind with a classic film, discover a new favorite series, or catch the latest live event, Limelight Stream has something for everyone. Experience the future of streaming with Limelight Stream – where entertainment comes to life.
Limelight iOS release date
Limelight software updates
Free game streaming software
Steam Big Picture streaming
Game streaming for gamers
Good luck!
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Everything is very open and very clear explanation of issues. was truly information.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
After all, what a great site and informative posts, I will upload inbound link – bookmark this web site? Regards, Reader.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Tyson Fury https://wbc.tyson-fury-fr.com is the undefeated WBC world champion and reigns supreme in boxing’s heavyweight division.
Inter Miami FC https://mls.inter-miami-fr.com has become a major player in MLS thanks to its star roster, economic growth and international influence.
Explore the career and significance of Monica Bellucci https://malena.monica-bellucci-fr.com in Malena (2000), which explores complex themes of beauty and human strength in wartime.
Discover Rafael Nadal’s https://mls.inter-miami-fr.com impressive rise to the top of world tennis, from his debut to his career Grand Slam victory.
The story of Kanye West https://the-college-dropout.kanye-west-fr.com, starting with his debut album “The College Dropout,” which changed hip-hop and became his cultural legacy.
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Преимущества аренды склада https://popivy.ru/otvetstvennoe-hranenie-mebeli-santehniki-i-bytovoj-tehniki-na-sklade-v-moskve-preimushhestva-i-vygody/, как аренда складских помещений может улучшить ваш бизнес
Rivaldo, or Rivaldo https://barcelona.rivaldo-br.com, is one of the greatest football players to ever play for Barcelona.
The fascinating story of the phenomenal rise and meteoric fall of Diego Maradona https://napoli.diegomaradona.biz, who became a cult figure at Napoli in the 1980s.
A fascinating story about Brazilian veteran Thiago Silva’s https://chelsea.thiago-silva.net difficult path to the top of European football as part of Chelsea London.
Explore the remarkable journey of Vinicius Junior https://real-madrid.vinicius-junior.net, the Brazilian prodigy who conquered the world’s biggest stage with his dazzling skills and unparalleled ambition at Real Madrid.
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Cristiano Ronaldo https://al-nassr.cristianoronaldo-br.net one of the greatest football players of all time, begins a new chapter in his career by joining An Nasr Club.
The story of Luka Modric’s rise https://real-madrid.lukamodric-br.com from young talent to one of the greatest midfielders of his generation and a key player for the Royals.
The fascinating story of Marcus Rashford’s rise https://manchester-united.marcusrashford-br.com from academy youth to the main striker and captain of Manchester United. Read about his meteoric rise and colorful career.
From academy product to captain and leader of Real Madrid https://real-madrid.ikercasillas-br.com Casillas became one of the greatest players in the history of Real Madrid.
Follow Bernardo Silva’s impressive career https://manchester-city.bernardosilva.net from his debut at Monaco to to his status as a key player and leader of Manchester City.
сайт казино рио бет Rio Bet Casino
регистрация Rio Bet Casino официальный сайт риобет казино
регистрация драгон мани казино драгон мани казино
онлайн казино Dragon Money драгон мани казино вход
Хотите научиться готовить самые изысканные и сложные торты? В этом https://v1.skladchik.org/tags/tort/ разделе вы найдете множество подробных пошаговых рецептов самых трендовых и известных тортов с возможностью получить их за сущие копейки благодаря складчине. Готовьте с удовольствием и открывайте для себя новые рецепты вместе с Skladchik.org
Лучшие пансионаты для пожилых людей https://ernst-neizvestniy.ru в Самаре – недорогие дома для престарелых в Самарской области
Пансионаты для пожилых людей https://moyomesto.ru в Самаре по доступным ценам. Специальные условия по уходу, индивидуальные программы.
The fascinating story of Sergio Ramos’ https://seville.sergioramos.net rise from Sevilla graduate to one of Real Madrid and Spain’s greatest defenders.
Ousmane Dembele’s https://paris-saint-germain.ousmanedembele-br.com rise from promising talent to key player for French football giants Paris Saint-Germain. An exciting success story.
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
The incredible success story of 20-year-old Florian Wirtz https://bayer-04.florianwirtz-br.com, who quickly joined the Bayer team and became one of the best young talents in the world.
The compelling story of Alisson Becker’s https://bayer-04.florianwirtz-br.com meteoric rise from young talent to key figure in Liverpool’s triumphant era under Jurgen Klopp.
The incredible story https://napoli.khvichakvaratskhelia-br.com of a young Georgian talent’s transformation into an Italian Serie A star. Khvicha Kvaraeshvili is a rising phenomenon in European football.
O meio-campista Rafael Veiga leva https://palmeiras.raphaelveiga-br.com o Palmeiras ao sucesso – o campeonato brasileiro e a vitoria na Copa Libertadores aos 24 anos.
Midfielder Rafael Veiga leads https://manchester-city.philfoden-br.com Palmeiras to success – the championship Brazilian and victory in the Copa Libertadores at the age of 24.
In-depth articles about the most famous football players https://zenit-saint-petersburg.wendel-br.com, clubs and events. Learn everything about tactics, rules of the game and football history.
The rise of 20-year-old midfielder Jamal Musiala https://bavaria.jamalmusiala-br.com to the status of a winger in the Bayern Munich team. A story of incredible talent.
A historia da jornada triunfante de Anitta https://veneno.anitta-br.com de aspirante a cantora a uma das interpretes mais influentes da musica moderna, incluindo sua participacao na serie de TV “Veneno”.
Fabrizio Moretti https://the-strokes.fabriziomoretti-br.com the influential drummer of The Strokes, and his unique sound revolutionized the music scene, remaining icons of modern rock.
Selena Gomez https://calm-down.selenagomez-br.net the story from child star to global musical influence, summarized in hit “Calm Down”, with Rema.
Kobe Bryant https://los-angeles-lakers.kobebryant-br.net one of the greatest basketball players of all the times, left an indelible mark on the history of sport.
Achraf Hakimi https://paris-saint-germain.ashrafhakimi.net is a young Moroccan footballer who quickly reached the football elite European in recent years.
Bieber’s https://baby.justinbieber-br.com path to global fame began with his breakthrough success Baby, which became his signature song and one of the most popular music videos of all time.
Ayrton Senna https://mclaren.ayrtonsenna-br.com is one of the greatest drivers in the history of Formula 1.
In the world of professional tennis, the name of Gustavo Kuerten https://roland-garros.gustavokuerten.com is closely linked to one of the most prestigious Grand Slam tournaments – Roland Garros.
Anderson Silva https://killer-bees-muay-thai-college.andersonsilva.net was born in 1975 in Curitiba Brazil. From a young age he showed an interest in martial arts, starting to train in karate at the age of 5.
Daniel Alves https://paris-saint-germain.danielalves.net is a name that symbolizes the greatness of the world of football.
Bruno Miguel Borges Fernandes https://manchester-united.brunofernandes-br.com was born on September 8, 1994 in Maia, Portugal.
Rodrygo Silva de Goes https://real-madrid.rodrygo-br.com, known simply as Rodrygo, emerged as one of the the brightest young talents in world football.
Nuno Mendes https://paris-saint-germain.nuno-mendes.com, a talented Portuguese left-back, He quickly became one of the key figures in the Paris Saint-Germain (PSG) team.
Romance and Lovers of Stream!
Welcome to Limelight Stream, the future of streaming entertainment. We offer a rich collection of movies, TV shows, documentaries, and live events, all available in stunning HD quality. Our platform is designed to be user-friendly and easy to navigate, with personalized recommendations to help you find the content you love. Whether you’re at home or on the go, Limelight Stream delivers seamless streaming across all your devices, including TVs, laptops, tablets, and smartphones. With continuous updates to our content library, you’ll always find something new and exciting to watch. Join us today and enjoy unlimited access to top-quality entertainment with http://limelight-stream.com/ where the best in streaming is always at your fingertips.
Game streaming network requirements
Stream games to Windows Phone
Limelight GitHub repository
Cross-platform game streaming
Limelight game streaming
Good luck!
Веном 3 онлайн https://bit.ly/venom-3-venom-2024
Earvin “Magic” Johnson https://los-angeles-lakers.magicjohnson.biz is one of the most legendary basketball players in history. NBA history.
Vinicius Junior https://real-madrid.vinicius-junior-ar.com the Brazilian prodigy whose full name is Vinicius Jose Baixao de Oliveira Junior, has managed to win the hearts of millions of fans around the world in a short period of time.
Victor Osimhen https://napoli.victorosimhen-ar.com born on December 29, 1998 in Lagos, Nigeria, has grown from an initially humble player to one of the brightest strikers in modern football.
Toni Kroos https://real-madrid.tonikroos-ar.com the German midfielder known for his accurate passes and calmness on the field, has achieved remarkable success at one of the most prestigious football clubs in the world.
Robert Lewandowski https://barcelona.robertlewandowski-ar.com is one of the most prominent footballers of our time, and his move to Barcelona has become one of the most talked about topics in world football.
Актуальное рабочее зеркало на сегодняшний день доступно на официальном сайте 7к казино – р7 казино официальный регистрация
슬롯 머신 사이트
Fang Jifan만이 그런 진실한 말을 할 수 있습니다.
Веном 3 2024 https://bit.ly/venom-3-venom-2024
Веном 3 2024 https://bit.ly/venom-3-venom-2024
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Pedro Gonzalez Lopez https://barcelona.pedri-ar.com known as Pedri, was born on November 25, 2002 in the small town of Tegeste, located on Tenerife, one of the Canary Islands.
The story of Leo Messi https://inter-miami.lionelmessi.ae‘s transfer to Inter Miami began long before the official announcement. Rumors about Messi’s possible departure from Barcelona appeared in 2020
Andreson Souza Conceicao https://al-nassr.talisca-ar.com known as Talisca, is one of the brightest stars of modern football.
Yacine Bounou https://al-hilal.yassine-bounou-ar.com known simply as Bono, is one of the most prominent Moroccan footballers of our time.
Айтек https://multimedijnyj-integrator.ru .
Harry Kane https://bayern.harry-kane-ar.com one of the most prominent English footballers of his generation, completed his move to German football club Bayern Munich in 2023.
Brazilian footballer Neymar https://al-hilal.neymar-ar.com known for his unique playing style and outstanding achievements in world football, has made a surprise move to Al Hilal Football Club.
Erling Haaland https://manchester-city.erling-haaland-ar.com born on July 21, 2000 in Leeds, England, began his football journey at an early age.
Luka Modric https://real-madrid.lukamodric-ar.com can certainly be called one of the outstanding midfielders in modern football.
Football in Saudi Arabia https://al-hilal.ali-al-bulaihi-ar.com has long been one of the main sports, attracting millions of fans. In recent years, one of the brightest stars in Saudi football has been Ali Al-Bulaihi, defender of Al-Hilal Football Club.
파워 오브 토르 메가웨이즈
생각이 너무 많다고 그를 탓할 수는 없습니다. 그는 또한 가난하고 두려운 사람 중 하나입니다.
visit my website https://currencyconvert.net
Сайт https://ps-likers.ru предлагает уроки по фотошоп для начинающих. На страницах сайта можно найти пошаговые руководства по анимации, созданию графики для сайтов, дизайну, работе с текстом и фотографиями, а также различные эффекты.
N’Golo Kante https://al-ittihad.ngolokante-ar.com the French midfielder whose career has embodied perseverance, hard work and skill, has continued his path to success at Al-Ittihad Football Club, based in Saudi Arabia.
Kobe Bryant https://los-angeles-lakers.kobebryant-ar.com also known as the “Black Mamba”, is one of the most iconic and iconic figures in NBA history.
RDBox.de https://rdbox.de bietet schallgedammte Gehause fur 3D-Drucker, die eine sehr leise Druckumgebung schaffen – nicht lauter als ein Kuhlschrank. Unsere Losungen sorgen fur stabile Drucktemperatur, Vibrationsisolierung, Luftreinigung und mobile App-Steuerung.
Karim Benzema https://al-ittihad.karimbenzema.ae is a name worthy of admiration and respect in the world of football.
Cristiano Ronaldo https://al-nassr.cristiano-ronaldo.ae is one of the greatest names in football history, with his achievements inspiring millions of fans around the world.
In 2018, the basketball world witnessed one of the most remarkable transformations in NBA history. LeBron James https://los-angeles-lakers.lebronjames-ar.com one of the greatest players of our time, decided to leave his hometown Cleveland Cavaliers and join the Los Angeles Lakers.
Luis Diaz https://liverpool.luis-diaz-ar.com is a young Colombian striker who has enjoyed rapid growth since joining the ” Liverpool” in January 2022.
Казино Riobet, основанное в 2023 году, быстро привлекло внимание поклонников азартных игр своим новаторским подходом и широким спектром услуг, что делает его потенциальным фаворитом в рейтинге лучших казино – Riobet официальный играть
Kevin De Bruyne https://manchester-city.kevin-de-bruyne-ar.com is a name every football fan knows today.
Muhammad Al Owais https://al-hilal.mohammed-alowais-ar.com is one of the most prominent names in modern Saudi football. His path to success in Al Hilal team became an example for many young athletes.
Казино 7k casino гарантирует конфиденциальность личных данных и безопасность финансовых операций – r7 casino актуальное зеркало
Наше казино 7к казино предлагает захватывающий игровой опыт с привлекательной графикой и высоким качеством игровых слотов на реальные деньги, чтобы удовлетворить даже самые взыскательные вкусы – 7к казино официальное зеркало сайта
Актуальное рабочее зеркало официального сайта 7к казино доступно для использования на текущий день – 7k casino официальный сайт бонус за регистрацию
Maria Sharapova https://tennis.maria-sharapova-ar.com was born on April 19, 1987 in Nyagan, Russia. When Masha was 7 years old, her family moved to Florida, where she started playing tennis.
Roberto Firmino https://al-ahli.roberto-firmino-ar.com one of the most talented and famous Brazilian footballers of our time, has paved his way to success in different leagues and teams.
Angel Di Maria https://benfica.angel-di-maria-ar.com is a name that will forever remain in the memories of Benfica fans.
Khvicha Kvaratskhelia https://napoli.khvicha-kvaratskhelia-ar.com is a name that in recent years has become a symbol of Georgian football talent and ambition.
Football in Saudi Arabia https://al-hilal.saud-abdulhamid-ar.com is gaining more and more popularity and recognition on the international stage, and Saud Abdul Hamid, the young and talented defender of Al Hilal, is a shining example of this success.
видеостена цена в москве видеостена цена в москве .
пироги
Казахский национальный технический университет https://satbayev.university им. К.Сатпаева
Upcoming fantasy MOBA https://bladesofthevoid.com evolved by Web3. Gacha perks, AI and crafting in one swirling solution!
Продажа новых автомобилей Hongqi
https://hongqi-krasnoyarsk.ru/hongqi-hs5-new в Красноярске у официального дилера Хончи. Весь модельный ряд, все комплектации, выгодные цены, кредит, лизинг, трейд-ин
Kylie Jenner https://kylie-cosmetics.kylie-jenner-ar.com is an American model, media personality, and businesswoman, born on August 10, 1997 in Los Angeles, California.
Bella Hadid https://img-models.bella-hadid-ar.com is an American model who has emerged in recent years as one of the most influential figures in the world of fashion.
Sadio Mane https://al-nassr.sadio-mane-ar.com the Senegalese footballer best known for his performances at clubs such as Southampton and Liverpool, has become a prominent figure in Al Nassr.
Brazilian footballer Ricardo Escarson https://orlando-city.kaka-ar.com dos Santos Leite, better known as Kaka, is one of the most famous and successful players in football history.
Веном 3 смотреть https://bit.ly/venom-3-venom-2024
Edson Arantes https://santos.pele-ar.com do Nascimento, known as Pele, was born on October 23, 1940 in Tres Coracoes, Minas Gerais, Brazil.
Monica Bellucci https://dracula.monica-bellucci-ar.com one of the most famous Italian actresses of our time, has a distinguished artistic career spanning many decades. Her talent, charisma, and stunning beauty made her an icon of world cinema.
Веном 3 2024 https://bit.ly/venom-3-venom-2024
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Brazilian footballer Malcom https://al-hilal.malcom-ar.com (full name Malcom Felipe Silva de Oliveira) achieved great success in Al Hilal, one of the leading football teams in Saudi Arabia and the entire Middle East.
Отборное оборудование для спортивных лебедок, для эффективных тренировок.
Подберите подходящую лебедку для тренировок, для достижения новых спортивных целей.
Какие характеристики важны при выборе лебедки для спорта, чтобы избежать ошибок и добиться успеха.
Топовые марки спортивных лебедок, которые заслужили доверие спортсменов.
Как подобрать правильный размер лебедки для тренировок, и избежать травм и неприятных ощущений.
Популярные материалы для изготовления лебедок для спортивных занятий, и какой материал предпочтителен для длительной эксплуатации и безопасности.
Инструкция по правильному использованию лебедки для спортивной серии, для достижения лучших результатов и безопасной тренировки.
Спортивная серия лебедок https://goldenpower4x4.ru/lebedki/sportivnaya-seriya.html .
Jackie Chan https://karate-kid.jackiechan-ar.com was born in 1954 in Hong Kong under the name Chan Kong San.
Jude Bellingham https://real-madrid.jude-bellingham-ar.com a young and talented English footballer, has enjoyed great success with Real Madrid since his arrival.
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Good info. Lucky me I reach on your website by accident, I bookmarked it. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Веном 3 фильм https://bit.ly/venom-3-venom-2024
Веном 3 2024 https://bit.ly/venom-3-venom-2024
речевое озвучивание речевое озвучивание .
магазин аккаунтов социальных сетей https://magazin-akkauntov.ru .
Защитите свою конфиденциальность с резидентским прокси, использовать этим инструментом.
В чем особенность резидентских прокси?, ознакомьтесь с подробностями.
Какой резидентский прокси выбрать?, рекомендации для пользователей.
Зачем нужны резидентские прокси?, ознакомьтесь с возможностями.
В чем преимущество безопасности резидентских прокси?, обзор функций безопасности.
Какие риски может предотвратить резидентский прокси?, разберем важные аспекты.
Зачем нужны резидентские прокси и какой их выигрыш?, сравним основные плюсы.
Как улучшить скорость Интернета с резидентским прокси, советы для оптимизации работы.
Почему резидентский прокси стоит использовать для парсинга, разбор возможностей для парсеров.
Секреты анонимности с резидентским прокси, рекомендации к безопасности онлайн.
Как улучшить работу в социальных сетях с резидентским прокси, практические советы функционала.
Зачем арендовать резидентские прокси и какие бонусы?, сравним лучшие варианты.
Как избежать DDoS с резидентским прокси?, подробно изучим меры безопасности.
В чем причина популярности резидентских прокси?, рассмотрим основные факторы.
Как выбрать между резидентским и дата-центровым прокси?, рекомендации для выбора.
где взять резидентский прокси https://rezidentnieproksi.ru/ .
Travis Scott https://astroworld.travis-scott-ar.com is one of the brightest stars in the modern hip-hop industry.
Zinedine Zidane https://real-madrid.zinedine-zidane-ar.com the legendary French footballer, entered the annals of football history as a player and coach.
The history of one of France’s https://france.paris-saint-germain-ar.com most famous football clubs, Paris Saint-Germain, began in 1970, when capitalist businessmen Henri Delaunay and Jean-Auguste Delbave founded the club in the Paris Saint-Germain-en-Laye area.
Juventus Football Club https://italy.juventus-ar.com is one of the most successful and decorated clubs in the history of Italian and world football.
Chelsea https://england.chelsea-ar.com is one of the most successful English football clubs of our time.
Ищете качественную мебель для офиса? Рекомендую обратить внимание на мебель для офиса замм. Этот бренд предлагает широкий ассортимент офисной мебели, включая стильные и функциональные офисные столы. Продукция замм отличается высоким качеством, долговечностью и современным дизайном. Идеально подходит для создания комфортного и продуктивного рабочего пространства. В ассортименте вы найдете всё, что нужно для организации современного офиса. Отличный выбор для тех, кто ценит надежность и стиль! С уважением, Zamm мебель.
порно видео бесплатно в хорошем качестве порно видео бесплатно в хорошем качестве .
Автомобили Hongqi https://hongqi-krasnoyarsk.ru в наличии – официальный дилер Hongqi Красноярск
Liverpool https://england.liverpool-ar.com holds a special place in the history of football in England.
When Taylor Swift https://shake-it-off.taylor-swift-ar.com released “Shake It Off” in 2014, she had no idea how much the song would impact her life and music career.
Priyanka Chopra https://baywatch.priyankachopra-ar.com is an Indian actress, singer, film producer and model who has achieved global success.
Jennifer Lopez https://lets-get-loud.jenniferlopez-ar.com was born in 1969 in the Bronx, New York, to parents who were Puerto Rican immigrants.
슬롯 게임 사이트
주변 사람들과 어울리지 않는 이들을 한데 모았다.
After some difficult years in the late 2010s, Manchester United https://england.manchester-united-ar.com returned to greatness in English football by 2024.
The Formula One World Championship https://world-circuit-racing-championship.formula-1-ar.com, known as the Formula Championship in motor racing, is the highest tier of professional motor racing.
Michael Jordan https://chicago-bulls.michael-jordan-ar.com is one of the greatest basketball players of all time, whose career with the Chicago Bulls is legendary.
дизайн интерьера https://dizayn-interera-doma.ru
car rental Montenegro Budva https://montenegro-car-rental-hire.com
Muhammad Ali https://american-boxer.muhammad-ali-ar.com is perhaps one of the most famous and greatest athletes in the history of boxing.
Mike Tyson https://american-boxer.mike-tyson-ar.com one of the most famous and influential boxers in history, was born on June 30, 1966 in Brooklyn, New York.
Manny Pacquiao https://filipino-boxer.manny-pacquiao-ar.com is one of the most prominent boxers in the history of the sport.
лучшее порно порево https://besplatny-sex-online.ru .
Если вам нужны профессионалы в области продвижения сайтов и разработки, обратите внимание на Mihaylov Digital. Они предлагают полный спектр услуг: от SEO и SEM до работы с Яндекс.Директ. Команда специализируется на создании эффективных стратегий, которые помогают привлечь целевую аудиторию и увеличить видимость вашего бизнеса в интернете. Их профессионализм и подход к каждому клиенту гарантируют отличные результаты. Рекомендую Михайлов Дмитрий как надежного партнера в цифровом маркетинге! С уважением, Mihaylov Digital.
The golf https://arabic.golfclub-ar.com industry in the Arab world is growing rapidly, attracting players from all over the world.
The road to the Premier League https://english-championship.premier-league-ar.com begins long before a team gets promoted to the English Premier League for the first time
The Italian football championship https://italian-championship.serie-a-ar.com known as Serie A, has seen an impressive revival in recent years.
In the German football https://german-championship.bundesliga-football-ar.com championship known as the Bundesliga, rivalries between clubs have always been intense.
In recent years, the leading positions in the Spanish https://spanish-championship.laliga-ar.com championship have been firmly occupied by two major giants – Barcelona and Real Madrid.
I really love to read such an excellent article. Helpful article. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Nice article inspiring thanks. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
The Saudi Football League https://saudi-arabian-championship.saudi-pro-league-ar.com known as the Saudi Professional League, is one of the most competitive and dynamic leagues in the world.
https://euroavia24.com – Cheap flights, hotels and transfers around the world!
In an era when many young footballers struggle to find their place at elite clubs, Javi’s https://barcelona.gavi-ar.com story at Barcelona stands out as an exceptional one.
Rodrigo Goes https://real-madrid.rodrygo-ar.com better known as Rodrigo, is one of the brightest young talents in modern football.
Arsenal https://arsenal.mesut-ozil-ar.com made a high-profile signing in 2013, signing star midfielder Mesut Ozil from Real Madrid.
With Tezfiles Premium, enjoy numerous benefits for a low cost. This option not only boosts the service’s capabilities and includes more perks that free account users can also enjoy.
Tezfiles.
Заработайте крупный выигрыш на Вавада казино, лучшие предложения для игроков, играйте с удовольствием, Ощутите азарт на Вавада казино, Станьте богаче с Вавада казино, возможность стать миллионером, получите свою долю азарта, Присоединяйтесь к победителям в Вавада казино, высокие шансы на успех, Побеждайте вместе с Вавада казино, Играйте в увлекательные игры на Вавада казино, Сделайте ставку на победу в Вавада казино, Попробуйте свою удачу на лучшем казино – Вавада, играйте и выигрывайте в онлайн казино
вавада официальный
Thibaut Courtois https://real-madrid.thibaut-courtois-ar.com was born on May 11, 1992 in Belgium.
Bayern Munich’s https://bayern.jamal-musiala-ar.com young midfielder, Jamal Musiala, has become one of the brightest talents in European football.
грузовой подъемник для склада подъемник грузовой канатный
Thank you for great information. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
классное порево видео http://www.klassny-sex.ru/ .
Full list of CS:GO/CS2 https://wiki.vpesports.com skins, detail descriptions
Luis Suarez https://inter-miami.luis-suarez-ar.com the famous Uruguayan footballer, ended his brilliant career in European clubs and decided to try his hand at a new challenge – Major League Soccer.
Al-Nasr https://saudi.al-nassr-ar.com is one of the most famous football teams in the Kingdom of Saudi Arabia.
Al-Ittihad https://saudi.al-ittihad-ar.com is one of the most famous football clubs in Saudi Arabia. Founded in 1927, the Saudi football giant has come a long way to the pinnacle of success.
Al-Nasr Club https://saudi.al-hilal-ar.com from Riyadh has a rich history of success, but its growth has been particularly impressive in recent years.
Thank you for great article. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
FC Barcelona https://spain.fc-barcelona-ar.com is undoubtedly one of the most famous and well-known football clubs in the world.
порно видео смотреть порно видео смотреть .
Thank you great post. Hello Administ .Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Hi, just required you to know I he added your site to my Google bookmarks due to your layout. But seriously, I believe your internet site has 1 in the freshest theme I??ve came across.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Great post thank you. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you great posting about essential oil. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for content. Area rugs and online home decor store. Hello Administ . Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
Thank you for great content. Hello Administ. Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
порно коллекции бесплатно http://porn-library.ru .
Montenegro Greece https://boat-hire-in-montenegro.com
보증 토토
Zhang Mao의 눈알이 굴러 갔고 대담한 생각이 들었습니다.
rent a boat Montenegro Budva yacht rental
Arsenal https://england.arsenal-ar.com is one of the most famous and successful football clubs in the history of English football.
FC Bayern Munich (Munich) https://germany.bayern-munchen-ar.com is one of the most famous and recognized football clubs in Germany and Europe
Real Madrid’s https://spain.real-madrid-ar.com history goes back more than a century. The club was founded in 1902 by a group of football enthusiasts led by Juan Padilla
Thai Company Directory https://thaicorporates.com List of companies and business information.
рекламный буклет печать наклеек на самоклеющейся
Ремонт плоской кровли https://remontiruem-krovly.ru в Москве, цена работы за 1 м?. Прайс лист на работы под ключ, отзывы и фото.
AC Milan https://italy.milan-ar.com is one of the most successful and decorated football clubs in the world.
Galatasaray https://turkey.galatasaray-ar.com is one of the most famous football clubs in Turkiye, with a glorious and eventful history.
The future football star Shabab Al-Ahly https://dubai.shabab-al-ahli-ar.com was born in Dubai in 2000. From a young age, he showed exceptional football abilities and joined the youth academy of one of the UAE’s leading clubs, Shabab Al-Ahly.
In the world of football, Atletico Madrid https://spain.atletico-madrid-ar.com has long been considered the second most important club in Spain after the dominant, Real Madrid.
The fascinating story of Ja Morant’s https://spain.atletico-madrid-ar.com meteoric rise, from status from rookie to leader of the Memphis Grizzlies and rising NBA superstar.
купить 3 комнатную квартиру купить новостройку с отделкой
купить однокомнатную квартиру в новостройке купить новостройку в ипотеку
https://indibeti.in is a premier online casino offering a wide array of games including slots, table games, and live dealer options. Renowned for its user-friendly interface and robust security measures, Indibet ensures a top-notch gaming experience with exciting bonuses and 24/7 customer support.
купить новостройку с ремонтом https://kvartiru-kupit43.ru
Discover your perfect stay with WorldHotels-in.com, your ultimate destination for finding the best hotels worldwide! Our user-friendly platform offers a vast selection of accommodations to suit every traveler’s needs and budget. Whether you’re planning a luxurious getaway or a budget-friendly adventure, we’ve got you covered with our extensive database of hotels across the globe. Our intuitive search features allow you to filter results based on location, amenities, price range, and guest ratings, ensuring you find the ideal match for your trip. We pride ourselves on providing up-to-date information and competitive prices, often beating other booking sites. Our detailed hotel descriptions, high-quality photos, and authentic guest reviews give you a comprehensive view of each property before you book. Plus, our secure booking system and excellent customer support team ensure a smooth and worry-free experience from start to finish. Don’t waste time jumping between multiple websites – http://www.WorldHotels-in.com brings the world’s best hotels to your fingertips in one convenient place. Start planning your next unforgettable journey today and experience the difference with WorldHotels-in.com!
coindarwin price analysis
The Story About Solana’s Originator Toly’s Accomplishment
Subsequent to 2 Mugs of Espresso plus a Beer
Toly, the brainchild behind Solana, began his journey with an ordinary routine – two cups of coffee and a beer. Little did he know, those moments would trigger the machinery of fate. Nowadays, Solana is as a significant player in the blockchain realm, featuring a market value of billions.
Ethereum ETF First Sales
The Ethereum exchange-traded fund newly launched with an impressive trade volume. This historic event saw several spot Ethereum ETFs from different issuers commence trading on U.S. exchanges, injecting unseen activity into the typically steady ETF trading space.
SEC Approved Ethereum ETF
The Securities and Exchange Commission has formally approved the Ethereum ETF for being listed. Being a cryptographic asset that includes smart contracts, Ethereum is expected to have a profound impact the digital currency industry with this approval.
Trump’s Bitcoin Tactics
As the election draws near, Trump positions himself as the “President of Crypto,” continually showcasing his endorsement of the cryptocurrency industry to attract voters. His tactic contrasts with Biden’s strategy, seeking to capture the interest of the blockchain community.
Elon Musk’s Impact
Elon, a well-known figure in the digital currency sector and a proponent of Trump’s agenda, stirred things up again, driving a meme coin connected to his actions. His participation continues to shape market trends.
Binance Developments
Binance’s subsidiary, BAM, has been allowed to channel customer funds in U.S. Treasury securities. Moreover, Binance noted its seventh year, highlighting its development and achieving several compliance licenses. Simultaneously, the firm also revealed plans to remove several important cryptocurrency pairs, influencing multiple market entities.
Artificial Intelligence and Economic Outlook
The chief stock analyst at Goldman Sachs recently stated that artificial intelligence won’t lead to a major economic changeHere’s the spintax version of the provided text with possible synonyms
Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me.Seo Paketi Skype: By_uMuT@KRaLBenim.Com -_- live:by_umut
новые квартиры от застройщиков https://kvartirukupit43.ru
купить 2 комнатную квартиру https://novye-kvartiryspb.ru
купить 1 квартиру застройщика https://novye-kvartiry-spb.ru
недорогие квартиры от застройщика купить новостройку с отделкой
купить квартиру новостройка застройщика отделкой https://novyekvartiry2.ru
оборудование конференц зала оборудование конференц зала .
проверенные капперы проверенные капперы .
купить однокомнатную квартиру https://zastroyshikekb54.ru
купить 1 комнатную квартиру в новостройке квартиры от застройщика цены жк
купить 2 комнатную квартиру https://kvartiranovostroi.ru
Koltuklarım ve halılarım şimdi yepyeni gibi! Profesyonel ve güler yüzlü ekip, hızlı hizmet sundu. Teşekkürler!
купить двухкомнатную в новостройке купить квартиру
квартира в новостройке от застройщика https://kvartiranovostroi2.ru
번개 슬롯
이 문장은 정말 모든 독자들의 마음을 아프게 했습니다.
Помощь в решении задач https://zadachireshaem-online.ru. Опытные авторы с профессиональной подготовкой окажут консультацию в решении задач на заказ недорого, быстро, качественно
купить новостройку от застройщика https://kvartira-novostroyka2.ru
Заказать контрольную работу https://kontrolnye-reshim.ru, недорого, цены. Решение контрольных работ на заказ срочно.
Заказать дипломную работу https://diplomzakazat-oline.ru недорого. Дипломные работы на заказ с гарантией.
Заказать курсовую работу https://kursovye-napishem.ru в Москве: цены на написание и выполнение, недорого
Accessibility Team Meeting Notes https://make.wordpress.org/accessibility/2021/06/11/accessibility-team-meeting-notes-june-11-2021
Красивая музыка https://melodia.space для души слушать онлайн.
Помощь студентам в выполнении рефератов https://referatkupit-oline.ru. Низкие цены и быстрое написание рефератов!
услуги по раскрутке сайта https://seoraskrutka43.ru
стоимость раскрутки сайта продвижение сайта в казани
переговорные москва oborudovanie-dlja-peregovornoj-komnaty.ru .
оснащение конференц залов оснащение конференц залов .
оборудование для переговорных комнат оборудование для переговорных комнат .
сео продвижение цена оптимизация и продвижение сайтов в поисковых системах
seo реклама https://seo-optimizatsia.ru
Останні новини України https://gromrady.org.ua сьогодні онлайн – головні події світу
Новинний ресурс https://actualnews.kyiv.ua про всі важливі події в Україні та світі.
Новини сьогодні https://gau.org.ua останні новини України та світу онлайн
Новини України https://kiev-online.com.ua останні події в Україні та світі сьогодні, новини України за минулий день онлайн
Популярные репортажи https://infotolium.com в больших фотографиях, новости, события в мире
Україна свіжі новини https://kiev-pravda.kiev.ua останні події на сьогодні
Свіжі новини України https://lenta.kyiv.ua останні новини з-за кордону, новини політики, економіки, спорту, культури.
Україна останні новини https://lentanews.kyiv.ua головні новини та останні події
Головні новини https://pto-kyiv.com.ua України та світу
Новини, останні події https://prp.org.ua в Україні та світі, новини політики, бізнесу та економіки, законодавства
Головні новини https://mediashare.com.ua про регіон України. Будьте в курсі останніх новин
Новини та аналітика https://newsportal.kyiv.ua ситуація в Україні.
Новини України https://sensus.org.ua та світу сьогодні. Головні та останні новини дня
о нас
Корисні та цікаві статті https://sevsovet.com.ua про здоров’я, дозвілля, кар’єру.
Головні новини https://status.net.ua сьогодні, найсвіжіші та останні новини України онлайн
Останні новини https://thingshistory.com зовнішньої та внутрішньої політики в країні та світі.
Останні новини світу https://uamc.com.ua про Україну від порталу новин Ukraine Today
видеостены в Москве http://www.videosteny-dlja-sozdanija-jekranov.ru/ .
оборудование для актовых залов оборудование для актовых залов .
Hello everyone!!
Glory Casino has become my favorite site for betting and casino games. Registration is simple, the bonuses are generous, and withdrawals are fast. The working mirror allows seamless access. I recommend Glory Casino to all gambling enthusiasts!
Glory Casino impressed me with its service. Convenient site, simple registration, many bonuses. The working mirror is always available, and withdrawals are fast. I play with pleasure, I recommend it to all gambling enthusiasts!
Catch the site where everything is in the best shape! – Glory Casino
Glory Casino registration
Glory Casino owner
Glory Casino download for iPhone mirror
Glory Casino mirror download online
mirror 1win Glory Casino 1
Good profits!
оборудование для актового зала оборудование для актового зала .