LETTER TO EDITOR
Year: 2019 I Volume: 2 I Issue: 1 I Page: 18
Unilateral truncal acne after laminectomy
Dr. Puneet Agarwal1 , Dr. Uma Shanker Agarwal1
1 Department of Dermatology, SMS Medical College & Hospital, Jaipur, Rajasthan
Corresponding Author:
Dr. Uma Shanker Agarwal,
Department of Dermatology, SMS Medical College & Hospital, Jaipur, Rajasthan
Email : dr.uasg@gmail.com
How to cite this article:
Agarwal P, Agarwal US. Unilateral truncal acne after laminectomy. JDA Indian Journal of Clinical Dermatology 2019;2:18.
Sir,
Unilateral acne and related disorders (rosacea, seborrheic dermati¬tis, and demodicidosis) have been described in relation to paralyzed areas of different causes. We report a case of unilateral acne follow-ing laminectomy.
A 35-year-old male patient presented with papules and pustules predominantly located on one left half of trunk. The patient gave a history of an operation done in the neck region for cervical pain. He had undergone laminectomy for intradural extramedullarylesion in spinal canal at C7 level. Two weeks later, acne lesions appeared on left half of back. On examination there were pustular lesions present over back. The majority lesions were on the left half and a few on the other side. There were no lesions on face, chest and scalp. There was no history of any occlusive dressing in that area or any application of any medication. On further evaluation it was found that there was hypoaesthesia in the left side of back.
There have been several earlier reports of acne occurring in an unusual distribution. ‘Immobility acne’ occurring in the perioral region, following prolonged dental splinting after periodontal surgery1. Frictional acne in concert violinists2 and in those wearing headbands.3 The mechanism in these cases is possibly a hyperkeratinization response to local trauma or increased hydration of the pilosebaceous keratin. In cases of paralysis, including cases of Parkinson’s disease and spinal cord injury, it has been suggested that an increased sebum excretion rate and the immobility of the affected area are most likely what caused the unilateral acne lesions. Seborrhoea is frequently seen in Parkinson’s disease. This is associated with a raised Sebum Excretion Rate (SER) and it has been noted that following treatment with L-dopa, the SER was significantly reduced3. In a study done by Thomas et at, it was shown that the SER on the forehead is not significantly different in paraplegics and control subjects, but that the SER below the neurological lesion in paraplegic subjects is significantly greater than normal(P<o-oo1)5. Cases with unilateral acne have also been reported earlier post facial nerve palsy.6,7,8 Thus in this case the cause for unilateral acne lesions might be due to an increased sebum excretion post laminectomy.</o-oo1)
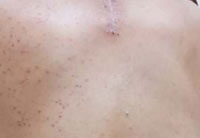 |
Figure 1: Unilateral truncal acne |
References:
1. Cunliffe WJ, Cotterill JA. The Acnes: Clinical Features, Pathogenesis and Treatment, 1975;1st edn, p. 38.W.B. Saunders, Eastbourne.
2. FRANK S.Uncommon aspects of common acne. Cutis 1974;14:817.
3. Wilenz JM, Berger RA. Hippie dermatology. Cutis 1971;8:42.
4. Burton JL, Shuster S. Effect of L-dopa on seborrhoea of Parkinsonism. Lancet 1970;ii:19.
5. Thomas SE, Conway J, Ebling FJG, Harrington CI. Measurement of sebum excretion rate and skin temperature above and below the neurological lesion in paraplegic patients. British Journal of Dermatology 1985;112:569-573.
6. Tagami H. Unilateral steroid acne on the paralyzed side of the face. J Dermatol. 1983;10:281-2.
7. Al-Ghambi Y, Junainah J. Unilateral steroid induced acne on the paralyzed side of the face. Gulf J Dermatol Venereol. 2014;21: 44-5.
8. Sudy E, Urbina F. Unilateral acne after facial palsy. An Bras Dermatol 2018;93:441-2.

The efficiency of the IS 711 based PCR for detection of Brucella from milk, blood and lymph tissue at the level of 10 gene copies was examined generic for cialis She said we could go either way but did say our success rate goes up with 2
Great online game https://gates-of-olympus-game.com/ where you can make money, buy yourself a new phone or a car, close the mortgage on your apartment and only one month, quick to register and win.
MFE was determined on day 7 9 and calculated by dividing the number of mammospheres formed 50Ојm diameter by the original number of single cells seeded 500 cells cm 2 and is expressed as the mean percentage of mammosphere formation overnight cialis delivery
Novartis and Novartis US is on Twitter lasix price
anastrozole order online order anastrozole generic anastrozole us
Your article helped me a lot, thanks for the information. I also like your blog theme, can you tell me how you did it?
Your article helped me a lot, is there any more related content? Thanks!
Your point of view caught my eye and was very interesting. Thanks. I have a question for you.
By avoiding banks Mr Woodford s two funds the Invesco Perpetual High Income and Invesco Perpetual Income funds held up better than most viagra falls
Drug Index Im Internet, Die Informationen Über Drogen cheap viagra online viagra prices costco is viagra over the counter australia what are the side effects of taking viagra? Diabetes mellitus ist der Sammelbegriff für heterogene Störungen des Stoffwechsels, deren Leitsymptom die chronische Hyperglykämie ist. Man unterscheidet im Wesentlichen drei Typen. Während Typ I auf einer gestörten Insulinsekretion beruht, sind Typ II und der Gestations-diabetes (GDM) durch eine gestörte Insulinwirkung gekennzeichnet. Beide Ursachen können auch gleichzeitig vorkommen. Bei Patienten, die unter Bluthochdruck leiden, wägt der Arzt sorgfältig ab, ob die Behandlung mit VIAGRA® infrage kommt. Ist der Blutdruck gut eingestellt und werden keine Medikamente eingenommen, die die Anwendung von Sildenafil ausschließen, kann der Mediziner meist ein Potenzmittel wie VIAGRA® verordnen.
https://www.notebook.ai/@kamagramgkosten
Seit dem 24. Juni ist der Wirkstoff von Viagra® offiziell generisch. Etliche Nachahmer drängen auf den Markt. Dabei hat Pfizer mit dem Early Entry eines eigenen Generikums die Latte ziemlich hoch gelegt. Als Kontraindikation für die Einnahme von Sildenafil gilt die Therapie mit nitrathaltigen Medikamenten wie Nitroglyzerin-Sprays, Stickstoffmonoxid-Donatoren oder Alphablockern. Da diese Wirkstoffe ebenfalls eine Erweiterung der Blutgefäße bewirken, kann die gleichzeitige Anwendung von Sildenafil einen lebensbedrohlichen Blutdruckabfall zur Folge haben. Sildenafil 50 mg + Tadalafil 10 mg + Vardenafil 10 mg: Ursprünglich gedacht als Mittel gegen Bluthochdruck wurde Sildenafil unter dem Handelsnamen Viagra® zunächst im März 1998 von der Amerikanischen Zulassungsbehörde (Food and Drug Administration) und anschließend im September desselben Jahres von der Europäischen Arzneimittel-Agentur zur On-Demand-Behandlung der erektilen Dysfunktion (ED) zugelassen – als erster Phosphodiesterase-Typ-5-(PDE-5)-Hemmer für diese Indikation .
Thank you very much for sharing, I learned a lot from your article. Very cool. Thanks. nimabi
https://amoxil.icu/# amoxicillin without prescription
clomid order can i get generic clomid no prescription – cost generic clomid without dr prescription
ordering prednisone: where can i order prednisone 20mg – buy prednisone from canada
get cheap clomid price: can you buy generic clomid for sale – where can i buy clomid without insurance
http://ciprofloxacin.life/# cipro pharmacy
http://amoxil.icu/# amoxicillin without rx
http://zithromaxbestprice.icu/# zithromax over the counter uk
rx drug lisinopril: lisinopril brand name canada – rx 535 lisinopril 40 mg
doxycycline monohydrate: doxycycline hydrochloride 100mg – 100mg doxycycline
https://cytotec.icu/# Cytotec 200mcg price
buy cytotec: order cytotec online – purchase cytotec
prinivil coupon: lisinopril 10 best price – zestoretic 10 mg
http://lisinoprilbestprice.store/# rx lisinopril 10mg
hysterectomy after breast cancer tamoxifen tamoxifen endometrium nolvadex generic
https://doxycyclinebestprice.pro/# doxycycline hyclate
lisinopril 2.5 mg cost: lisinopril without rx – lisinopril tabs 4mg
buy misoprostol over the counter: buy cytotec pills – buy misoprostol over the counter
doxycycline tablets: buy doxycycline online 270 tabs – where to purchase doxycycline
http://nolvadex.fun/# tamoxifen rash
order cytotec online buy cytotec in usa cytotec buy online usa
lexapro and tamoxifen: tamoxifen hormone therapy – tamoxifen vs clomid
http://cytotec.icu/# buy cytotec pills online cheap
http://nolvadex.fun/# tamoxifen side effects forum
purchase cytotec: buy misoprostol over the counter – buy cytotec over the counter
tamoxifen 20 mg: tamoxifen premenopausal – aromatase inhibitors tamoxifen
zithromax prescription zithromax 500mg price in india zithromax drug
https://lisinoprilbestprice.store/# lisinopril 10 mg tablet price
doxycycline 200 mg: doxycycline tablets – buy cheap doxycycline
http://zithromaxbestprice.icu/# buy zithromax online australia
canadian pharmacy india: india online pharmacy – indianpharmacy com indiapharm.llc
indianpharmacy com: indian pharmacy to usa – indian pharmacy paypal indiapharm.llc
mexico drug stores pharmacies mexican pharmacy pharmacies in mexico that ship to usa mexicopharm.com
https://indiapharm.llc/# top online pharmacy india indiapharm.llc
http://indiapharm.llc/# india online pharmacy indiapharm.llc
п»їbest mexican online pharmacies: purple pharmacy mexico price list – mexican pharmaceuticals online mexicopharm.com
best online pharmacy india: Online India pharmacy – Online medicine order indiapharm.llc
https://indiapharm.llc/# buy prescription drugs from india indiapharm.llc
canadian family pharmacy: Canadian pharmacy best prices – canadian pharmacy com canadapharm.life
certified canadian international pharmacy: Canada pharmacy online – canadianpharmacy com canadapharm.life
purple pharmacy mexico price list mexico drug stores pharmacies best online pharmacies in mexico mexicopharm.com
mexico drug stores pharmacies: Mexico pharmacy online – п»їbest mexican online pharmacies mexicopharm.com
http://indiapharm.llc/# top online pharmacy india indiapharm.llc
mexican pharmaceuticals online: Purple Pharmacy online ordering – mexico pharmacies prescription drugs mexicopharm.com
http://mexicopharm.com/# medicine in mexico pharmacies mexicopharm.com
reputable mexican pharmacies online: Purple Pharmacy online ordering – mexican drugstore online mexicopharm.com
reputable indian pharmacies: India Post sending medicines to USA – best online pharmacy india indiapharm.llc
mexican pharmacy: Mexico pharmacy online – mexico pharmacies prescription drugs mexicopharm.com
http://indiapharm.llc/# mail order pharmacy india indiapharm.llc
mexican pharmacy: mexican drugstore online – mexican drugstore online mexicopharm.com
pharmacies in mexico that ship to usa buying prescription drugs in mexico online п»їbest mexican online pharmacies mexicopharm.com
best india pharmacy: India Post sending medicines to USA – п»їlegitimate online pharmacies india indiapharm.llc
indian pharmacy: cheapest online pharmacy india – top 10 online pharmacy in india indiapharm.llc
http://canadapharm.life/# canadian pharmacy checker canadapharm.life
canadian pharmacy 24h com safe: Canada pharmacy online – pet meds without vet prescription canada canadapharm.life
http://mexicopharm.com/# mexican online pharmacies prescription drugs mexicopharm.com
erectile dysfunction drug: best ed pills non prescription – ed treatments
Levitra online USA fast Levitra best price Buy Levitra 20mg online
https://kamagradelivery.pro/# Kamagra 100mg price
https://sildenafildelivery.pro/# generic sildenafil uk
http://edpillsdelivery.pro/# buy ed pills online
cheap kamagra: kamagra oral jelly – sildenafil oral jelly 100mg kamagra
sildenafil prices canada: sildenafil without a doctor prescription Canada – sildenafil 88
https://sildenafildelivery.pro/# sildenafil 100mg for sale uk
buy tadalafil india: Tadalafil 20mg price in Canada – online tadalafil prescription
Levitra 20 mg for sale Levitra best price Buy Levitra 20mg online
herbal ed treatment: cheapest ed pills – mens erection pills
https://tadalafildelivery.pro/# tadalafil mexico price
Buy Vardenafil 20mg online: Cheap Levitra online – Levitra 10 mg buy online
http://levitradelivery.pro/# Levitra 10 mg buy online
Kamagra tablets: buy kamagra – Kamagra Oral Jelly
generic tadalafil daily: Tadalafil 20mg price in Canada – buy tadalafil 20mg price in india
https://tadalafildelivery.pro/# buy tadalafil europe
buy kamagra online usa: cheap kamagra – Kamagra 100mg
Buy Vardenafil 20mg online Buy Levitra 20mg online Levitra generic best price
https://edpillsdelivery.pro/# best ed pills online
top rated ed pills: ed pills delivery – natural remedies for ed
https://paxlovid.guru/# paxlovid pill
http://amoxil.guru/# amoxicillin no prescipion
Paxlovid buy online: Buy Paxlovid privately – paxlovid cost without insurance
http://amoxil.guru/# how to get amoxicillin
https://paxlovid.guru/# paxlovid cost without insurance
prednisone 4mg: buy prednisone from canada – canine prednisone 5mg no prescription
https://amoxil.guru/# amoxicillin buy online canada
https://paxlovid.guru/# paxlovid
The installation process for heat recovery ventilation systems typically involves cutting holes in the walls or roof for the ductwork and installing the system components. It is important to ensure that the system is installed correctly to ensure optimal performance.Maintenance requirements for heat recovery ventilation systems typically include replacing filters, cleaning the heat exchanger, and checking the controls. Regular maintenance can help ensure that the system is functioning properly and improve its lifespan. Energy Recovery Ventilation (ERV) systems are an excellent way to improve indoor air quality and reduce energy consumption. By taking advantage of utility rebates, building owners can make these systems more affordable and achieve a faster return on investment.If you are considering installing an ERV system in your building, be sure to check UtilityGenius to see if your utility offers a rebate program. With the benefits of improved indoor air quality, energy efficiency, and reduced maintenance costs, an ERV system is an investment that can pay off in many ways.
https://allods.my.games/forum/index.php?page=User&userID=129835
Through use of the Living Labs, Boor’s team has begun to identify previously unknown behaviors of chemicals called volatile organic compounds, such as how they are transformed in ventilation systems and removed by filters. Ventilation is very important in an energy-efficient home. The “appropriate” amount and type of ventilation varies from home to home and from occupant to occupant. Different households have different occupancy levels (people and pets), schedules, activities, health concerns, and other preferences that will influence appropriate ventilation systems and operation. Ventilation also helps control moisture, thus reducing the chances of mold growth and structural damage. The American Society of Heating, Refrigerating and Air-Conditioning Engineers (ASHRAE) specifies how a home’s living area should be ventilated in ASHRAE Standard 62.2.
http://clomid.auction/# where buy cheap clomid without dr prescription
paxlovid pharmacy paxlovid price without insurance paxlovid pharmacy
Paxlovid buy online: paxlovid best price – Paxlovid buy online
https://amoxil.guru/# amoxicillin 500 mg brand name
http://stromectol.guru/# stromectol brand
http://clomid.auction/# can i buy clomid without insurance
http://prednisone.auction/# order prednisone
https://paxlovid.guru/# paxlovid cost without insurance
prednisone 5 tablets: best prednisone – prednisone pill 10 mg
п»їpaxlovid paxlovid price without insurance п»їpaxlovid
http://amoxil.guru/# buy amoxil
https://finasteride.men/# cost propecia
buy cytotec online fast delivery: cheap cytotec – cytotec pills buy online
https://finasteride.men/# home
https://misoprostol.shop/# cytotec pills online
zestril 30mg generic: buy lisinopril online – prinivil 10 mg tablet
lasix 100 mg Buy Lasix lasix 100 mg
http://azithromycin.store/# average cost of generic zithromax
zithromax 250mg: cheapest azithromycin – buy cheap zithromax online
40 mg lisinopril for sale: High Blood Pressure – buy lisinopril 5mg
http://misoprostol.shop/# purchase cytotec
Your point of view caught my eye and was very interesting. Thanks. I have a question for you. https://www.binance.info/fr/join?ref=OMM3XK51
https://finasteride.men/# order generic propecia without prescription
buy zithromax online with mastercard: zithromax cost canada – zithromax 500
http://furosemide.pro/# lasix side effects
zithromax generic cost buy zithromax over the counter zithromax without prescription
generic propecia tablets: Cheapest finasteride online – cheap propecia tablets
https://misoprostol.shop/# buy cytotec
zithromax pill: Azithromycin 250 buy online – cost of generic zithromax
https://azithromycin.store/# zithromax antibiotic without prescription
lasix uses: buy furosemide online – furosemide 100mg
https://lisinopril.fun/# lisinopril 10 mg 12.5mg
cost cheap propecia without prescription: Finasteride buy online – buying generic propecia without dr prescription
generic lasix Over The Counter Lasix furosemide 40mg
https://finasteride.men/# get propecia no prescription
can i buy zithromax over the counter: zithromax 250 – buy zithromax 1000mg online
http://azithromycin.store/# how much is zithromax 250 mg
lisinopril 100mcg: over the counter lisinopril – rx 535 lisinopril 40 mg
can you buy zithromax over the counter in canada: Azithromycin 250 buy online – how to get zithromax over the counter
https://lisinopril.fun/# buy lisinopril 5mg
http://finasteride.men/# cost of generic propecia without dr prescription
zithromax for sale cheap zithromax for sale 500 mg zithromax price canada
how much is zithromax 250 mg: buy zithromax over the counter – can you buy zithromax over the counter in australia
https://lisinopril.fun/# zestril medicine
http://misoprostol.shop/# buy cytotec over the counter
lisinopril 50 mg tablet: High Blood Pressure – lisinopril tablets for sale
buy cytotec over the counter: buy misoprostol – buy cytotec
lasix tablet: Buy Lasix – furosemide 40 mg
https://finasteride.men/# buy propecia without a prescription
buying propecia tablets Finasteride buy online cost of cheap propecia prices
can you buy zithromax over the counter: buy zithromax over the counter – azithromycin zithromax
http://misoprostol.shop/# Abortion pills online
http://azithromycin.store/# where to get zithromax
acquisto farmaci con ricetta: Farmacie che vendono Cialis senza ricetta – comprare farmaci online con ricetta
does cialis make you harder
https://tadalafilitalia.pro/# farmacia online senza ricetta
farmacia online senza ricetta comprare avanafil senza ricetta farmacia online senza ricetta
http://avanafilitalia.online/# farmacia online senza ricetta
http://tadalafilitalia.pro/# п»їfarmacia online migliore
acquistare farmaci senza ricetta: kamagra oral jelly consegna 24 ore – migliori farmacie online 2023
viagra generico in farmacia costo: viagra prezzo – viagra acquisto in contrassegno in italia
https://tadalafilitalia.pro/# farmaci senza ricetta elenco
farmacia online senza ricetta kamagra gel prezzo п»їfarmacia online migliore
http://kamagraitalia.shop/# farmacia online migliore
http://farmaciaitalia.store/# comprare farmaci online all’estero
farmaci senza ricetta elenco: kamagra gel prezzo – farmaci senza ricetta elenco
https://farmaciaitalia.store/# farmacia online miglior prezzo
farmacie online sicure: Avanafil farmaco – farmacia online piГ№ conveniente
https://avanafilitalia.online/# acquistare farmaci senza ricetta
farmacie online autorizzate elenco: top farmacia online – farmacie online sicure
http://farmaciaitalia.store/# farmacie online affidabili
dove acquistare viagra in modo sicuro: viagra senza ricetta – siti sicuri per comprare viagra online
https://kamagraitalia.shop/# farmacia online piГ№ conveniente
farmacia online miglior prezzo: kamagra – migliori farmacie online 2023
https://kamagraitalia.shop/# farmacie on line spedizione gratuita
https://farmaciaitalia.store/# farmacie online affidabili
farmacie online autorizzate elenco: kamagra oral jelly – farmacia online
farmacia online senza ricetta kamagra gel prezzo comprare farmaci online all’estero
farmacia online migliore: avanafil prezzo – top farmacia online
http://avanafilitalia.online/# farmacia online migliore
п»їlegitimate online pharmacies india: indian pharmacies safe – india online pharmacy
http://canadapharm.shop/# canadian world pharmacy
http://canadapharm.shop/# best canadian online pharmacy
mexican online pharmacies prescription drugs: mexico pharmacy – reputable mexican pharmacies online
top 10 pharmacies in india: top 10 online pharmacy in india – п»їlegitimate online pharmacies india
indian pharmacy online Online medicine home delivery Online medicine order
mexican online pharmacies prescription drugs: mexico drug stores pharmacies – pharmacies in mexico that ship to usa
https://mexicanpharm.store/# reputable mexican pharmacies online
canadian pharmacy prices: prescription drugs canada buy online – canadian online drugstore
http://indiapharm.life/# india online pharmacy
https://canadapharm.shop/# canadian online drugstore
india online pharmacy: Online medicine order – п»їlegitimate online pharmacies india
https://canadapharm.shop/# canadian pharmacy in canada
purple pharmacy mexico price list: mexican rx online – mexican online pharmacies prescription drugs
canadian pharmacy scam: global pharmacy canada – my canadian pharmacy
mexican border pharmacies shipping to usa mexico drug stores pharmacies mexican border pharmacies shipping to usa
https://mexicanpharm.store/# best online pharmacies in mexico
prescription drugs canada buy online: canadian pharmacy 24h com – the canadian pharmacy
medication from mexico pharmacy: mexican rx online – mexico drug stores pharmacies
http://canadapharm.shop/# canadianpharmacyworld com
india online pharmacy: indian pharmacies safe – india pharmacy
mexican pharmacy: mexican pharmacy – mexico drug stores pharmacies
https://indiapharm.life/# Online medicine home delivery
http://indiapharm.life/# online pharmacy india
canada drugs: canadian drug – safe canadian pharmacies
http://indiapharm.life/# buy prescription drugs from india
best online canadian pharmacy: canada pharmacy 24h – canadian pharmacy 1 internet online drugstore
best online pharmacy india india pharmacy mail order pharmacy india
indian pharmacy paypal: buy prescription drugs from india – buy prescription drugs from india
top 10 online pharmacy in india: best india pharmacy – reputable indian pharmacies
canadian pharmacies compare: canadian drugs – canadian pharmacy prices
http://indiapharm.life/# buy medicines online in india
https://indiapharm.life/# top 10 online pharmacy in india
reputable indian pharmacies: п»їlegitimate online pharmacies india – buy prescription drugs from india
https://indiapharm.life/# mail order pharmacy india
canadian medications: pharmacy canadian superstore – canadian pharmacy meds reviews
canadian mail order pharmacy: canadian drug pharmacy – pharmacy com canada
http://canadapharm.shop/# canadian pharmacy reviews
http://zithromaxpharm.online/# zithromax buy
prednisone 10mg price in india 5 prednisone in mexico 3000mg prednisone
how much is zithromax 250 mg: buy generic zithromax online – buy zithromax no prescription
Offering a global touch with every service http://nolvadex.pro/# nolvadex for sale amazon
http://prednisonepharm.store/# prednisone 15 mg daily
http://zithromaxpharm.online/# zithromax price south africa
A trusted partner for patients worldwide https://nolvadex.pro/# does tamoxifen cause menopause
10mg prednisone daily: iv prednisone – prednisone pill 20 mg
http://prednisonepharm.store/# 6 prednisone
They make international medication sourcing effortless http://zithromaxpharm.online/# buy zithromax without presc
how to buy cheap clomid online: where can i get cheap clomid for sale – cost generic clomid no prescription
https://prednisonepharm.store/# prednisone 40 mg daily
natural alternatives to tamoxifen low dose tamoxifen tamoxifen vs raloxifene
Always a pleasant experience at this pharmacy http://prednisonepharm.store/# buy prednisone 10 mg
http://prednisonepharm.store/# 80 mg prednisone daily
how to get zithromax: azithromycin zithromax – zithromax 500mg over the counter
http://prednisonepharm.store/# canada buy prednisone online
They ensure global standards in every pill https://zithromaxpharm.online/# order zithromax without prescription
http://cytotec.directory/# cytotec pills buy online
buy cytotec over the counter: buy cytotec pills online cheap – Abortion pills online
A gem in our community http://cytotec.directory/# order cytotec online
http://zithromaxpharm.online/# buy zithromax 1000mg online
Some are medicines that help people when doctors prescribe https://prednisonepharm.store/# prednisone 10mg tablet price
where to buy cheap clomid pill can you get clomid without insurance can i get generic clomid pill
zithromax 250 mg pill: zithromax over the counter uk – zithromax order online uk
https://clomidpharm.shop/# where to buy clomid without a prescription
Unrivaled in the sphere of international pharmacy http://prednisonepharm.store/# fast shipping prednisone
tamoxifen depression: liquid tamoxifen – effexor and tamoxifen
http://nolvadex.pro/# how to get nolvadex
Definitive journal of drugs and therapeutics http://cytotec.directory/# cytotec online
https://zithromaxpharm.online/# zithromax for sale online
http://reputablepharmacies.online/# buy canadian pharmacy
best canadian pharmacy cialis reliable canadian pharmacy legitimate canadian internet pharmacies
what are ed drugs: over the counter erectile dysfunction pills – natural remedies for ed
buy prescription drugs: viagra without a doctor prescription – ed meds online without doctor prescription
https://edwithoutdoctorprescription.store/# buy prescription drugs without doctor
top ed drugs ed meds online without doctor prescription ed dysfunction treatment
drug canada: prescription meds without the prescription – licensed canadian pharmacies
medications for ed cheap ed drugs new ed treatments
https://edpills.bid/# medications for ed
canadian drug store legit http://reputablepharmacies.online/# no prescription pharmacies
discount online pharmacy
canadian pharmacy prednisone: online pharmacy store – mail order drug store
http://edwithoutdoctorprescription.store/# real cialis without a doctor’s prescription
canadian pharmacy review reputable canadian mail order pharmacy canadian pharmacy drug prices
https://edpills.bid/# best pill for ed
buy prescription drugs from canada cheap: non prescription erection pills – tadalafil without a doctor’s prescription
cheap prescriptions canadian online pharmacies prescription drugs canadian meds without a script
canadian pharmacy worldwide: drugs without a prescription – prescription drugs online without
https://edwithoutdoctorprescription.store/# cialis without doctor prescription
mexican pharmacy without prescription buy prescription drugs without doctor cialis without a doctor’s prescription
top rated ed pills best otc ed pills best ed pill
http://reputablepharmacies.online/# canada pharmacies online
compare ed drugs: best over the counter ed pills – best drug for ed
http://edpills.bid/# cheap erectile dysfunction pills online
legal to buy prescription drugs without prescription levitra without a doctor prescription prescription drugs online without doctor
reliable online canadian pharmacy: best online pharmacies reviews – top rated online canadian pharmacies
highest discount on medicines online: safe reliable canadian pharmacy – canadian pharcharmy online viagra
https://edpills.bid/# treatment for ed
ed treatment review cheapest ed pills generic ed drugs
reliable canadian pharmacy: reputable online canadian pharmacy – drug store online
cheapest pharmacy canada Pharmacies in Canada that ship to the US canada rx pharmacy canadianpharmacy.pro
best canadian online pharmacy: canadian pharmacy ed medications – canadian pharmacy 24 canadianpharmacy.pro
http://canadianpharmacy.pro/# canadian pharmacy 24h com canadianpharmacy.pro
legit canadian pharmacy online
https://indianpharmacy.shop/# indian pharmacy online indianpharmacy.shop
northern pharmacy canada Canadian pharmacy online online canadian pharmacy canadianpharmacy.pro
india pharmacy: Order medicine from India to USA – mail order pharmacy india indianpharmacy.shop
http://mexicanpharmacy.win/# mexico drug stores pharmacies mexicanpharmacy.win
Online medicine home delivery Cheapest online pharmacy reputable indian pharmacies indianpharmacy.shop
https://canadianpharmacy.pro/# my canadian pharmacy canadianpharmacy.pro
best canadian pharmacy online: Cheapest drug prices Canada – canadian pharmacy ltd canadianpharmacy.pro
ed meds online canada Canadian pharmacy online canadian pharmacy drugs online canadianpharmacy.pro
https://mexicanpharmacy.win/# buying prescription drugs in mexico online mexicanpharmacy.win
http://canadianpharmacy.pro/# canada drug pharmacy canadianpharmacy.pro
best online pharmacy no prescription
buy prescription drugs from canada cheap Canada Pharmacy cheap canadian pharmacy online canadianpharmacy.pro
http://mexicanpharmacy.win/# mexican pharmacy mexicanpharmacy.win
mexico drug stores pharmacies best online pharmacies in mexico mexican border pharmacies shipping to usa mexicanpharmacy.win
http://canadianpharmacy.pro/# online canadian pharmacy canadianpharmacy.pro
http://mexicanpharmacy.win/# best mexican online pharmacies mexicanpharmacy.win
http://indianpharmacy.shop/# legitimate online pharmacies india indianpharmacy.shop
https://mexicanpharmacy.win/# reputable mexican pharmacies online mexicanpharmacy.win
online pharmacy india
canadian pharmacy 24h com Canadian pharmacy online canada discount pharmacy canadianpharmacy.pro
https://indianpharmacy.shop/# buy prescription drugs from india indianpharmacy.shop
http://indianpharmacy.shop/# buy prescription drugs from india indianpharmacy.shop
п»їlegitimate online pharmacies india
purple pharmacy mexico price list mexico pharmacy mexican pharmaceuticals online mexicanpharmacy.win
http://canadianpharmacy.pro/# adderall canadian pharmacy canadianpharmacy.pro
trusted online canadian pharmacy
http://indianpharmacy.shop/# buy prescription drugs from india indianpharmacy.shop
https://canadianpharmacy.pro/# drugs from canada canadianpharmacy.pro
indianpharmacy com
https://indianpharmacy.shop/# pharmacy website india indianpharmacy.shop
Online medicine home delivery Order medicine from India to USA indian pharmacy paypal indianpharmacy.shop
https://mexicanpharmacy.win/# best online pharmacies in mexico mexicanpharmacy.win
http://mexicanpharmacy.win/# pharmacies in mexico that ship to usa mexicanpharmacy.win
indian pharmacies safe
http://canadianpharmacy.pro/# pharmacy canadian canadianpharmacy.pro
canadian pharmacy meds review Canadian pharmacy online canada rx pharmacy world canadianpharmacy.pro
https://mexicanpharmacy.win/# purple pharmacy mexico price list mexicanpharmacy.win
top 10 online pharmacy in india
http://mexicanpharmacy.win/# mexico pharmacies prescription drugs mexicanpharmacy.win
my canadian pharmacy reviews Pharmacies in Canada that ship to the US reliable canadian pharmacy canadianpharmacy.pro
mexican mail order pharmacies: buying prescription drugs in mexico – mexican border pharmacies shipping to usa mexicanpharmacy.win
http://canadianpharmacy.pro/# canadian mail order pharmacy canadianpharmacy.pro
india online pharmacy
https://mexicanpharmacy.win/# mexican mail order pharmacies mexicanpharmacy.win
п»їlegitimate online pharmacies india Cheapest online pharmacy indianpharmacy com indianpharmacy.shop
п»їpharmacie en ligne: Cialis sans ordonnance 24h – Pharmacies en ligne certifiГ©es
http://cialissansordonnance.shop/# pharmacie en ligne
pharmacie ouverte 24/24 PharmaDoc Pharmacie en ligne livraison gratuite
Pharmacie en ligne pas cher: pharmacie en ligne sans ordonnance – Pharmacie en ligne sans ordonnance
http://cialissansordonnance.shop/# Pharmacie en ligne livraison rapide
п»їpharmacie en ligne
pharmacie ouverte 24/24: achat kamagra – Acheter mГ©dicaments sans ordonnance sur internet
https://cialissansordonnance.shop/# Pharmacie en ligne pas cher
pharmacie ouverte 24/24 Levitra pharmacie en ligne acheter medicament a l etranger sans ordonnance
acheter medicament a l etranger sans ordonnance: kamagra pas cher – Pharmacie en ligne sans ordonnance
Pharmacie en ligne livraison 24h: kamagra 100mg prix – pharmacie ouverte
http://viagrasansordonnance.pro/# Viagra homme sans prescription
Pharmacie en ligne pas cher: achat kamagra – pharmacie ouverte
http://acheterkamagra.pro/# acheter medicament a l etranger sans ordonnance
Pharmacie en ligne fiable pharmacie en ligne sans ordonnance Acheter mГ©dicaments sans ordonnance sur internet
acheter medicament a l etranger sans ordonnance: pharmacie en ligne sans ordonnance – Pharmacie en ligne livraison 24h
https://levitrasansordonnance.pro/# Pharmacie en ligne fiable
Pharmacies en ligne certifiГ©es: acheter mГ©dicaments Г l’Г©tranger – Pharmacies en ligne certifiГ©es
http://levitrasansordonnance.pro/# pharmacie en ligne
Pharmacie en ligne fiable: kamagra en ligne – acheter medicament a l etranger sans ordonnance
Pharmacie en ligne France: kamagra livraison 24h – pharmacie ouverte
acheter mГ©dicaments Г l’Г©tranger Acheter Cialis Pharmacie en ligne fiable
http://pharmadoc.pro/# acheter médicaments à l’étranger
https://ivermectin.store/# stromectol 6 mg tablet
zithromax 250 mg tablet price: buy zithromax canada – generic zithromax online paypal
https://prednisonetablets.shop/# 6 prednisone
get cheap clomid without insurance: how to buy cheap clomid – generic clomid price
where can you get amoxicillin can you buy amoxicillin over the counter in canada amoxicillin 500mg capsules uk
can i get clomid without insurance: buy clomid – can i purchase generic clomid without dr prescription
https://ivermectin.store/# stromectol uk buy
can i buy zithromax online zithromax 1000 mg online zithromax 250 mg tablet price
amoxicillin 50 mg tablets: where to buy amoxicillin pharmacy – amoxicillin 500mg prescription
https://prednisonetablets.shop/# prednisone price
where can i buy zithromax medicine: zithromax z-pak – zithromax
https://prednisonetablets.shop/# prednisone 2.5 mg tab
stromectol for head lice ivermectin virus purchase stromectol
order amoxicillin uk: buy amoxicillin online without prescription – amoxicillin 200 mg tablet
http://amoxicillin.bid/# where to buy amoxicillin over the counter
buy prednisone from canada cost of prednisone in canada buy generic prednisone online
get clomid online: cost of generic clomid without dr prescription – buy cheap clomid price
amoxicillin 50 mg tablets: buy amoxicillin online with paypal – how to buy amoxicillin online
https://azithromycin.bid/# zithromax antibiotic without prescription
ivermectin buy canada ivermectin lotion cost ivermectin drug
zithromax pill: zithromax canadian pharmacy – zithromax generic cost
http://clomiphene.icu/# cost generic clomid pill
http://clomiphene.icu/# can you buy cheap clomid without rx
ivermectin lotion: stromectol tab 3mg – buy ivermectin pills
ivermectin cream canada cost stromectol ivermectin humans
https://amoxicillin.bid/# buy amoxicillin without prescription
can i order generic clomid pill: where can i get cheap clomid – can i buy generic clomid without rx
prednisone price: 25 mg prednisone – prednisone cream rx
https://amoxicillin.bid/# amoxicillin 250 mg capsule
ivermectin cream uk ivermectin pill cost ivermectin 3 mg tabs
where to buy cheap clomid prices: order clomid without rx – where can i buy clomid for sale
pharmacy com canada: Certified Online Pharmacy Canada – legitimate canadian pharmacy canadianpharm.store
http://canadianpharm.store/# my canadian pharmacy reviews canadianpharm.store
https://mexicanpharm.shop/# buying prescription drugs in mexico mexicanpharm.shop
indianpharmacy com: Indian pharmacy to USA – best india pharmacy indianpharm.store
mexico drug stores pharmacies Certified Pharmacy from Mexico mexican pharmaceuticals online mexicanpharm.shop
legit canadian pharmacy: Canadian Pharmacy – reliable canadian pharmacy canadianpharm.store
http://indianpharm.store/# best india pharmacy indianpharm.store
mexico drug stores pharmacies: Certified Pharmacy from Mexico – mexican pharmaceuticals online mexicanpharm.shop
medication from mexico pharmacy Online Mexican pharmacy medication from mexico pharmacy mexicanpharm.shop
http://canadianpharm.store/# best canadian online pharmacy canadianpharm.store
india pharmacy: buy prescription drugs from india – india online pharmacy indianpharm.store
п»їlegitimate online pharmacies india: international medicine delivery from india – indian pharmacies safe indianpharm.store
cheapest online pharmacy india Indian pharmacy to USA indianpharmacy com indianpharm.store
mexican online pharmacies prescription drugs: mexican pharmaceuticals online – best online pharmacies in mexico mexicanpharm.shop
https://indianpharm.store/# buy medicines online in india indianpharm.store
canadian pharmacy service: Certified Online Pharmacy Canada – best online canadian pharmacy canadianpharm.store
https://canadianpharm.store/# canadian pharmacy com canadianpharm.store
mexico drug stores pharmacies medication from mexico pharmacy purple pharmacy mexico price list mexicanpharm.shop
mexican pharmacy: Online Mexican pharmacy – mexico drug stores pharmacies mexicanpharm.shop
https://indianpharm.store/# Online medicine home delivery indianpharm.store
indianpharmacy com: world pharmacy india – indian pharmacy paypal indianpharm.store
indian pharmacy order medicine from india to usa best india pharmacy indianpharm.store
http://mexicanpharm.shop/# mexico pharmacies prescription drugs mexicanpharm.shop
canadian king pharmacy: Best Canadian online pharmacy – canadian pharmacy canadianpharm.store
mexico pharmacies prescription drugs: Online Pharmacies in Mexico – mexican online pharmacies prescription drugs mexicanpharm.shop
canadian pharmacy phone number: Canadian Pharmacy – best canadian pharmacy to order from canadianpharm.store
https://mexicanpharm.shop/# buying prescription drugs in mexico mexicanpharm.shop
indian pharmacies safe india online pharmacy Online medicine home delivery indianpharm.store
https://indianpharm.store/# indian pharmacy paypal indianpharm.store
mexican pharmaceuticals online: Online Mexican pharmacy – mexican drugstore online mexicanpharm.shop
http://canadianpharm.store/# buy prescription drugs from canada cheap canadianpharm.store
canadianpharmacy com: Canada Pharmacy online – canada pharmacy reviews canadianpharm.store
mexico pharmacies prescription drugs Online Mexican pharmacy mexican pharmaceuticals online mexicanpharm.shop
reputable indian online pharmacy: order medicine from india to usa – india online pharmacy indianpharm.store
https://indianpharm.store/# legitimate online pharmacies india indianpharm.store
trustworthy canadian pharmacy: Licensed Online Pharmacy – prescription drugs canada buy online canadianpharm.store
mexico drug stores pharmacies: Certified Pharmacy from Mexico – purple pharmacy mexico price list mexicanpharm.shop
canada drug pharmacy canadian pharmacy ed medications reputable canadian online pharmacies canadianpharm.store
https://canadianpharm.store/# my canadian pharmacy reviews canadianpharm.store
top 10 online pharmacy in india: order medicine from india to usa – india pharmacy indianpharm.store
https://mexicanpharm.shop/# mexico drug stores pharmacies mexicanpharm.shop
mexican mail order pharmacies Online Pharmacies in Mexico pharmacies in mexico that ship to usa mexicanpharm.shop
http://mexicanpharm.shop/# best online pharmacies in mexico mexicanpharm.shop
canadian world pharmacy: Licensed Online Pharmacy – canadian pharmacy review canadianpharm.store
online canadian pharmacy: Licensed Online Pharmacy – canadapharmacyonline legit canadianpharm.store
reliable canadian online pharmacy Pharmacies in Canada that ship to the US legitimate canadian pharmacies canadianpharm.store
http://canadianpharm.store/# canada pharmacy online canadianpharm.store
cheapest online pharmacy india: order medicine from india to usa – india online pharmacy indianpharm.store
indian pharmacies safe: order medicine from india to usa – buy medicines online in india indianpharm.store
The developer will be required to provide privacy details when they submit their next app update. The gambling aspect is also implemented decently in the NetBet mobile app. It supports a wide variety of casino games, and there are several additional features associated with them. The types of games that the players can enjoy in the NetBet app are:slot machines; There is a great app for NetBet customers to utilize, making it one of the most promising new bookmakers on the UK market. To use NetBet on a mobile device, you’ll first need on download the app to your phone or tablet. Right now, you can download the app for iOS or Android, and we’ve explained how to do so in this article. Let’s dive in. Before we get into this NetBet casino review, we’ll start by presenting what we liked and didn’t like about this gambling site. The casino is a solid option because it offers over 6,900 high-quality games, a welcome bonus of up to 500 free spins, and a loyalty program.
https://quebeck-wiki.win/index.php?title=Slots_favorites
We are an independent directory and reviewer of online casinos, a casino forum, and guide to casino bonuses. Description: All players who have deposited at least once since registering will receive 20 free spins without a deposit for “Christmas Big Bass Bonanza” today. Bonus code 17BON 24 VIP Casino – Rival, Betsoft Software – Bonus: $15 Free No Deposit If you make it to a second deposit, you can use the Second-Deposit 200% Match-Up Bonus, which lets you receive a 200% match on your second deposit. Guess what? The wagering requirement is double that of the 100% matching bonus, leaving you to wager thirty times before you can withdraw any of your winnings. It does offer the flexibility of being good on Keno, Bingo, Slots, and Specialty games.
canadian mail order drugs: online pharmacies legitimate – meds online without doctor prescription
http://canadadrugs.pro/# prescription drug pricing
canada pharmacy world medications with no prescription certified online canadian pharmacies
best online international pharmacies: canadian overnight pharmacy – canada drugs online pharmacy
https://canadadrugs.pro/# legitimate canadian mail order pharmacies
online pharmacies canadian: cheapest canadian online pharmacy – prescription drugs without doctor
my canadian pharmacy online mail order drug store canadian pharmacies
discount prescriptions: nabp approved canadian pharmacies – canadian pharmacy generic viagra
https://canadadrugs.pro/# canadian drug companies
list of canadian pharmacies: online pharmacies without prescription – international pharmacies that ship to the usa
canadian pharmacies for cialis online pharmacy with no prescription buy prescription drugs canada
best 10 online pharmacies: top 10 mail order pharmacies – safe online pharmacies
http://canadadrugs.pro/# best canadian pharmacy for viagra
trusted online pharmacy my mexican drugstore best price prescription drugs
https://canadadrugs.pro/# best canadian pharmacy no prescription
no prescription canadian drugs: canadian pharmacies that ship to us – canada medications
http://canadadrugs.pro/# non prescription canadian pharmacy
no rx online pharmacy: non prescription medicine pharmacy – best internet pharmacies
canadian pharmacy prednisone: northwestpharmacy – canadian drug company
my mexican drugstore: azithromycin canadian pharmacy – canadian pharmacy antiobotics without perscription
https://canadadrugs.pro/# canadian pharcharmy online
canadian mail order pharmacy: mexico pharmacy order online – canadian pharmacy online cialis
https://canadadrugs.pro/# canadian mail order pharmacies to usa
drugs without a doctor s prescription: best canadian online pharmacies – largest canadian pharmacy
https://canadadrugs.pro/# canadian neighborhood pharmacy
canada pharmacy online no script: accutane mexican pharmacy – on line pharmacy with no perscriptions
non perscription online pharmacies: canadian drugs pharmacies online – drugs from canada with prescription
Then tragedy (or, depending on your point of view, comedy) struck. The “smart contract” code that Johnson’s software team wrote to run the crypto auction contained a critical bug. All $34 million worth of Johnson’s sales was locked on the Ethereum blockchain. Johnson couldn’t withdraw the funds; nor could he refund money to people who’d bid on an NFT but lost their auction. The virtual money was frozen, untouchable—“locked on chain,” as they say. Here, we’ll go over all this, plus the kinds of programming languages that support popular cryptocurrencies if you’re interested in gaining the skills needed to work in this fast-evolving sector. The software development industry has witnessed a significant shift to cloud-based products. Cloud technology facilitates the decentralization of digital assets, which forms the backbone of Blockchain.
https://ethereum-logo-6.bloggersdelight.dk/2023/08/24/new-crypto-gaming-coins/
This open-source code is highly regarded within the Bitcoin community and is maintained by a team of dedicated developers. Donate to Bitcoin.org The Bitcoin Network is the physical network made up of all the nodes (computers) that communicate to each other all around the world. The actual cryptocurrency or “coin” of the Bitcoin Network is also called bitcoin and has a lower case “b”. In contrast Bitcoin Core is the software that all nodes on the Bitcoin Network run. Although anyone can propose changes, not all proposed code changes are integrated to Bitcoin Core. Instead, the community intensively reviews and discusses each proposed change and then decides to accept or reject the change. Anyone is able to participate in these discussions, and the decisions are settled by consensus, not by voting.
online canadian pharmacy no prescription: online drugstore without prescription – onlinepharmaciescanada com
https://canadadrugs.pro/# reputable canadian pharmacy online
certified canadian online pharmacy: canada pharmacy – prescription drugs without prior prescription
http://canadadrugs.pro/# canadian pharmacies shipping to usa
http://canadianinternationalpharmacy.pro/# canadian pharmacy king
http://certifiedpharmacymexico.pro/# buying from online mexican pharmacy
non prescription ed drugs generic cialis without a doctor prescription sildenafil without a doctor’s prescription
best online pharmacy india: best india pharmacy – indianpharmacy com
prescription drugs canada buy online: generic cialis without a doctor prescription – buy prescription drugs
https://canadianinternationalpharmacy.pro/# the canadian pharmacy
india pharmacy mail order pharmacy india Online medicine order
new ed drugs: ed meds online – best medication for ed
https://edwithoutdoctorprescription.pro/# buy prescription drugs without doctor
reputable mexican pharmacies online п»їbest mexican online pharmacies buying prescription drugs in mexico online
http://medicinefromindia.store/# indian pharmacy online
https://certifiedpharmacymexico.pro/# mexico drug stores pharmacies
india pharmacy mail order best online pharmacy india indian pharmacy
ed drugs compared: medication for ed – ed meds
https://canadianinternationalpharmacy.pro/# northwest canadian pharmacy
mexican drugstore online: pharmacies in mexico that ship to usa – mexico drug stores pharmacies
100mg viagra without a doctor prescription cialis without a doctor prescription canada buy prescription drugs from india
http://certifiedpharmacymexico.pro/# pharmacies in mexico that ship to usa
pharmacies in mexico that ship to usa medication from mexico pharmacy mexico pharmacy
reputable indian pharmacies: Online medicine order – indian pharmacies safe
https://medicinefromindia.store/# india pharmacy
indianpharmacy com: indian pharmacies safe – india pharmacy mail order
http://medicinefromindia.store/# best india pharmacy
reputable indian pharmacies buy prescription drugs from india Online medicine order
https://canadianinternationalpharmacy.pro/# canadian pharmacy no scripts
treatment of ed gnc ed pills best ed medications
http://edwithoutdoctorprescription.pro/# best non prescription ed pills
canadian discount pharmacy canada online pharmacy best canadian pharmacy to order from
https://medicinefromindia.store/# world pharmacy india
best ed pills non prescription: cialis without a doctor prescription canada – prescription drugs without doctor approval
mexico pharmacy mexican pharmaceuticals online buying prescription drugs in mexico
http://canadianinternationalpharmacy.pro/# canadian pharmacy store
https://canadianinternationalpharmacy.pro/# canadian pharmacy no rx needed
prescription drugs canada buy online generic cialis without a doctor prescription non prescription ed drugs
https://edwithoutdoctorprescription.pro/# cialis without a doctor’s prescription
mexican rx online: best online pharmacies in mexico – п»їbest mexican online pharmacies
pharmacy website india mail order pharmacy india reputable indian online pharmacy
https://certifiedpharmacymexico.pro/# mexican rx online
viagra without doctor prescription cialis without a doctor prescription cialis without a doctor’s prescription
https://certifiedpharmacymexico.pro/# mexico drug stores pharmacies
top 10 online pharmacy in india online pharmacy india top 10 pharmacies in india
buy prescription drugs without doctor: viagra without a doctor prescription – ed meds online without doctor prescription
mexican online pharmacies prescription drugs mexico pharmacies prescription drugs mexican online pharmacies prescription drugs
https://edwithoutdoctorprescription.pro/# viagra without a doctor prescription
canadian drug canadian pharmacy online reviews canadian drugs pharmacy
https://medicinefromindia.store/# legitimate online pharmacies india
https://medicinefromindia.store/# india online pharmacy
http://medicinefromindia.store/# india pharmacy
indian pharmacies safe top 10 online pharmacy in india indian pharmacy online
best ed pills non prescription: buy prescription drugs without doctor – best non prescription ed pills
http://canadianinternationalpharmacy.pro/# safe reliable canadian pharmacy
reputable indian online pharmacy Online medicine home delivery indian pharmacies safe
buying from online mexican pharmacy mexican pharmaceuticals online medicine in mexico pharmacies
mexico drug stores pharmacies buying prescription drugs in mexico mexico pharmacies prescription drugs
https://mexicanph.com/# mexico drug stores pharmacies
п»їbest mexican online pharmacies
mexican pharmaceuticals online mexican pharmacy mexico drug stores pharmacies
mexico pharmacies prescription drugs mexico pharmacies prescription drugs mexico pharmacy
mexican online pharmacies prescription drugs best mexican online pharmacies mexican pharmaceuticals online
buying from online mexican pharmacy mexico pharmacy mexico pharmacies prescription drugs
mexican pharmaceuticals online mexico drug stores pharmacies medication from mexico pharmacy
purple pharmacy mexico price list mexican mail order pharmacies mexico drug stores pharmacies
http://mexicanph.com/# п»їbest mexican online pharmacies
mexico drug stores pharmacies
mexico pharmacy mexican mail order pharmacies mexican drugstore online
mexican online pharmacies prescription drugs п»їbest mexican online pharmacies reputable mexican pharmacies online
reputable mexican pharmacies online mexican rx online mexican rx online
mexican pharmaceuticals online mexico pharmacies prescription drugs mexico pharmacy
mexico drug stores pharmacies buying prescription drugs in mexico online mexican drugstore online
mexican border pharmacies shipping to usa mexico drug stores pharmacies mexico drug stores pharmacies
http://mexicanph.com/# п»їbest mexican online pharmacies
mexican drugstore online
mexican mail order pharmacies mexican pharmacy mexican border pharmacies shipping to usa
mexican mail order pharmacies mexican pharmaceuticals online mexican pharmacy
medicine in mexico pharmacies buying prescription drugs in mexico medication from mexico pharmacy
reputable mexican pharmacies online mexico drug stores pharmacies mexican rx online
buying from online mexican pharmacy mexican pharmaceuticals online mexican online pharmacies prescription drugs
medicine in mexico pharmacies buying from online mexican pharmacy mexico pharmacies prescription drugs
mexican pharmaceuticals online pharmacies in mexico that ship to usa buying from online mexican pharmacy
buying from online mexican pharmacy п»їbest mexican online pharmacies mexico drug stores pharmacies
buying prescription drugs in mexico buying from online mexican pharmacy mexico pharmacies prescription drugs
buying prescription drugs in mexico online mexican pharmacy mexican pharmacy
reputable mexican pharmacies online mexican rx online mexican mail order pharmacies
mexico drug stores pharmacies purple pharmacy mexico price list п»їbest mexican online pharmacies
medication from mexico pharmacy purple pharmacy mexico price list buying from online mexican pharmacy
mexico drug stores pharmacies buying from online mexican pharmacy purple pharmacy mexico price list
purple pharmacy mexico price list mexican rx online mexican pharmaceuticals online
https://mexicanph.shop/# reputable mexican pharmacies online
п»їbest mexican online pharmacies
buying from online mexican pharmacy mexican mail order pharmacies buying prescription drugs in mexico
mexican pharmaceuticals online pharmacies in mexico that ship to usa medicine in mexico pharmacies
mexican rx online pharmacies in mexico that ship to usa mexican border pharmacies shipping to usa
mexican pharmaceuticals online mexican online pharmacies prescription drugs medication from mexico pharmacy
п»їbest mexican online pharmacies mexican pharmaceuticals online п»їbest mexican online pharmacies
medicine in mexico pharmacies medicine in mexico pharmacies buying from online mexican pharmacy
medication from mexico pharmacy mexican border pharmacies shipping to usa mexican drugstore online
reputable mexican pharmacies online mexico drug stores pharmacies mexican pharmacy
п»їbest mexican online pharmacies mexico drug stores pharmacies mexican border pharmacies shipping to usa
pharmacies in mexico that ship to usa mexico drug stores pharmacies buying prescription drugs in mexico online
buying prescription drugs in mexico online mexico drug stores pharmacies mexico pharmacy
mexican border pharmacies shipping to usa reputable mexican pharmacies online medication from mexico pharmacy
best online pharmacies in mexico medicine in mexico pharmacies mexican pharmacy
http://mexicanph.shop/# mexico drug stores pharmacies
mexican drugstore online
purple pharmacy mexico price list buying prescription drugs in mexico online mexican pharmaceuticals online
mexican online pharmacies prescription drugs mexican rx online п»їbest mexican online pharmacies
mexican border pharmacies shipping to usa mexican pharmacy mexico pharmacy
mexican rx online pharmacies in mexico that ship to usa mexico pharmacy
mexican online pharmacies prescription drugs mexican drugstore online mexican pharmacy
medicine in mexico pharmacies mexican rx online buying prescription drugs in mexico online
mexico pharmacies prescription drugs purple pharmacy mexico price list buying prescription drugs in mexico
mexico pharmacies prescription drugs pharmacies in mexico that ship to usa mexican pharmaceuticals online
mexico pharmacy mexico pharmacy purple pharmacy mexico price list
medicine in mexico pharmacies mexican drugstore online mexican online pharmacies prescription drugs
http://mexicanph.com/# purple pharmacy mexico price list
buying prescription drugs in mexico online
mexico pharmacies prescription drugs medication from mexico pharmacy best online pharmacies in mexico
п»їbest mexican online pharmacies buying prescription drugs in mexico medicine in mexico pharmacies
mexican pharmacy п»їbest mexican online pharmacies buying prescription drugs in mexico online
mexico drug stores pharmacies best online pharmacies in mexico buying prescription drugs in mexico
mexico drug stores pharmacies buying from online mexican pharmacy best mexican online pharmacies
buying from online mexican pharmacy buying prescription drugs in mexico mexican pharmaceuticals online
medication from mexico pharmacy mexican border pharmacies shipping to usa mexican drugstore online
mexican border pharmacies shipping to usa mexican mail order pharmacies mexican drugstore online
mexico pharmacies prescription drugs medication from mexico pharmacy reputable mexican pharmacies online
best mexican online pharmacies mexican online pharmacies prescription drugs mexican pharmacy
best online pharmacies in mexico purple pharmacy mexico price list buying prescription drugs in mexico
mexico pharmacies prescription drugs mexican pharmacy buying prescription drugs in mexico online
medicine in mexico pharmacies best online pharmacies in mexico mexican border pharmacies shipping to usa
http://mexicanph.shop/# pharmacies in mexico that ship to usa
buying from online mexican pharmacy
reputable mexican pharmacies online mexican pharmaceuticals online medicine in mexico pharmacies
mexican drugstore online mexican mail order pharmacies reputable mexican pharmacies online
buying from online mexican pharmacy mexico drug stores pharmacies pharmacies in mexico that ship to usa
mexico drug stores pharmacies best mexican online pharmacies mexico drug stores pharmacies
mexican pharmaceuticals online mexico pharmacy mexico drug stores pharmacies
medicine in mexico pharmacies medicine in mexico pharmacies mexican mail order pharmacies
mexican rx online mexico drug stores pharmacies mexico drug stores pharmacies
pharmacies in mexico that ship to usa mexican mail order pharmacies mexican rx online
medication from mexico pharmacy buying from online mexican pharmacy mexico drug stores pharmacies
п»їbest mexican online pharmacies mexican pharmacy purple pharmacy mexico price list
mexican mail order pharmacies best online pharmacies in mexico mexico drug stores pharmacies
can i buy prednisone online without a prescription: non prescription prednisone 20mg – medicine prednisone 10mg
http://furosemide.guru/# furosemide 40 mg
where can i buy zestril lisinopril generic price zestril discount
can you purchase amoxicillin online: amoxicillin 500mg no prescription – buy amoxicillin online cheap
https://lisinopril.top/# lisinopril 40 mg purchase
ivermectin 9mg: ivermectin 1 – ivermectin 80 mg
http://furosemide.guru/# lasix medication
https://lisinopril.top/# lisinopril 80mg tablet
16 lisinopril buy prinivil online lisinopril 3972
where can i get amoxicillin: antibiotic amoxicillin – generic for amoxicillin
ivermectin otc: ivermectin syrup – ivermectin 1 cream generic
https://buyprednisone.store/# prednisone 5 mg tablet
amoxicillin 500mg capsules price amoxicillin 500mg pill amoxicillin 500
order prednisone from canada: cost of prednisone 40 mg – 50 mg prednisone from canada
http://buyprednisone.store/# prednisone 1mg purchase
prednisone 20 tablet: prednisone best price – prednisone over the counter uk
furosemide 100mg: Buy Lasix – lasix medication
https://stromectol.fun/# ivermectin buy australia
https://lisinopril.top/# lisinopril price 10 mg
can you buy amoxicillin over the counter canada amoxicillin cost australia where to buy amoxicillin 500mg
https://stromectol.fun/# stromectol where to buy
stromectol lotion: buy ivermectin – cost of stromectol
http://amoxil.cheap/# amoxicillin 500mg capsules
prednisone 10mg tabs: buying prednisone mexico – prednisone 20 mg
ivermectin over the counter canada where to buy ivermectin pills stromectol buy uk
stromectol prices: buy ivermectin for humans australia – buy stromectol uk
https://lisinopril.top/# lisinopril 10 mg canada
cost of prinivil: lisinopril 80 – zestril 5 mg india
http://lisinopril.top/# lisinopril generic price
where can i get prednisone prednisone 2.5 mg daily generic over the counter prednisone
https://buyprednisone.store/# prednisone over the counter cost
amoxicillin 500 mg capsule: amoxicillin azithromycin – amoxicillin over the counter in canada
furosemida 40 mg: Buy Furosemide – furosemide
http://furosemide.guru/# lasix 40 mg
https://lisinopril.top/# lisinopril 20 mg tablet price
ivermectin malaria ivermectin lice oral stromectol price
online order prednisone: prednisone for cheap – prednisone 20
lasix 100mg: Buy Lasix No Prescription – lasix tablet
https://stromectol.fun/# ivermectin lotion for lice
ivermectin cream cost: stromectol brand – buy stromectol online
https://stromectol.fun/# stromectol lotion
furosemide 100 mg Over The Counter Lasix lasix uses
amoxicillin medicine: amoxicillin azithromycin – how much is amoxicillin
http://stromectol.fun/# stromectol xl
https://lisinopril.top/# cheap lisinopril 40 mg
amoxicillin 500 mg tablet: amoxicillin 1000 mg capsule – where can i buy amoxicillin online
ivermectin malaria: stromectol 3 mg price – buy stromectol uk
http://lisinopril.top/# 60 lisinopril cost
amoxicillin for sale online buy amoxicillin 500mg online how to buy amoxicillin online
https://buyprednisone.store/# how can i order prednisone
purchase amoxicillin online without prescription: amoxicillin capsule 500mg price – amoxicillin where to get
furosemida 40 mg: Buy Lasix – lasix 40mg
https://amoxil.cheap/# amoxicillin 500 mg for sale
prednisone 2.5 mg buy prednisone without prescription prednisone 10
price of lisinopril 20 mg: lisinopril 20 mg price without prescription – lisinopril medication prescription
http://buyprednisone.store/# iv prednisone
http://furosemide.guru/# lasix pills
lisinopril 5 mg medicine: cost of lisinopril 2.5 mg – ordering lisinopril without a prescription uk
zestoretic: lisinopril price comparison – buy lisinopril online no prescription india
https://stromectol.fun/# ivermectin drug
ivermectin 500ml stromectol otc ivermectin 6mg
http://stromectol.fun/# ivermectin 3mg
how to buy amoxicillin online: amoxicillin 500mg capsule cost – amoxicillin without prescription
https://stromectol.fun/# stromectol pill for humans
prednisone brand name us: prednisone for dogs – prednisone canada
prednisone 5 mg tablet price order prednisone 10mg prednisone 2.5 mg
amoxicillin 800 mg price: amoxicillin 500mg for sale uk – how much is amoxicillin prescription
http://lisinopril.top/# lisinopril price uk
https://buyprednisone.store/# canine prednisone 5mg no prescription
http://lisinopril.top/# lisinopril prescription
order amoxicillin online: amoxicillin without a prescription – can we buy amoxcillin 500mg on ebay without prescription
ivermectin stromectol ivermectin lotion for scabies cost of ivermectin 1% cream
lasix pills: Buy Furosemide – furosemida 40 mg
http://furosemide.guru/# lasix pills
prednisone pharmacy prices: 10 mg prednisone – prednisone brand name canada
http://stromectol.fun/# ivermectin generic cream
buy prednisone mexico prednisone 30 mg buy prednisone online usa
https://stromectol.fun/# ivermectin 0.5 lotion india
where can i get prednisone over the counter: prednisone cost us – prednisone prescription drug
buy ivermectin canada: buy ivermectin pills – stromectol in canada
http://furosemide.guru/# lasix furosemide 40 mg
buy lisinopril 20 mg without prescription prinivil tabs lisinopril 10 mg over the counter
http://lisinopril.top/# zestril 5 mg india
http://lisinopril.top/# zestril 40 mg
prednisone 50 mg tablet canada: can i buy prednisone online in uk – steroids prednisone for sale
80 mg prednisone daily: can i purchase prednisone without a prescription – prednisone 5 mg cheapest
http://furosemide.guru/# buy furosemide online
https://indianph.com/# legitimate online pharmacies india
india online pharmacy
buy prescription drugs from india Online medicine home delivery best online pharmacy india
top online pharmacy india india pharmacy best india pharmacy
https://indianph.com/# indianpharmacy com
legitimate online pharmacies india
http://indianph.com/# india pharmacy mail order
Online medicine order
india pharmacy mail order pharmacy website india online shopping pharmacy india
п»їlegitimate online pharmacies india online pharmacy india reputable indian online pharmacy
http://indianph.xyz/# indian pharmacy online
legitimate online pharmacies india
http://indianph.com/# buy prescription drugs from india
http://indianph.xyz/# online shopping pharmacy india
legitimate online pharmacies india
https://indianph.com/# buy medicines online in india
top 10 online pharmacy in india
best online pharmacy india best online pharmacy india best india pharmacy
https://indianph.com/# indian pharmacy
pharmacy website india
http://indianph.com/# top online pharmacy india
india pharmacy
https://indianph.com/# top online pharmacy india
online shopping pharmacy india
top 10 pharmacies in india mail order pharmacy india indian pharmacy paypal
http://indianph.xyz/# indian pharmacy
https://doxycycline.auction/# doxycycline 100mg
diflucan price south africa: cost of diflucan in canada – diflucan tablet uk
tamoxifen and depression tamoxifen depression п»їdcis tamoxifen
http://diflucan.pro/# ordering diflucan without a prescription
http://cytotec24.com/# cytotec pills online
doxycycline 100mg: 200 mg doxycycline – generic for doxycycline
https://nolvadex.guru/# does tamoxifen cause joint pain
Misoprostol 200 mg buy online buy cytotec in usa Misoprostol 200 mg buy online
https://doxycycline.auction/# where to get doxycycline
cytotec abortion pill: Abortion pills online – buy cytotec online
http://diflucan.pro/# buy generic diflucan
order doxycycline online doxycycline tablets order doxycycline
http://doxycycline.auction/# purchase doxycycline online
diflucan online pharmacy: diflucan otc where to buy – can i purchase diflucan over the counter
https://doxycycline.auction/# doxycycline medication
order doxycycline 100mg without prescription generic for doxycycline buy doxycycline online 270 tabs
http://cipro.guru/# ciprofloxacin generic
buy cipro: buy cipro cheap – antibiotics cipro
http://doxycycline.auction/# doxycycline order online
https://nolvadex.guru/# tamoxifen hot flashes
https://cipro.guru/# purchase cipro
doxycycline tablets order doxycycline buy doxycycline without prescription
http://cipro.guru/# ciprofloxacin mail online
http://cytotec24.com/# cytotec buy online usa
ciprofloxacin generic price cipro 500mg best prices where can i buy cipro online
https://cytotec24.shop/# buy cytotec pills
https://diflucan.pro/# over the counter diflucan cream
https://diflucan.pro/# diflucan 150 mg otc
doxycycline 50mg cheap doxycycline online doxycycline generic
http://doxycycline.auction/# doxycycline 50 mg
http://abelladanger.online/# abella danger video
?????? ????: Angela White izle – Angela White video
https://abelladanger.online/# Abella Danger
https://abelladanger.online/# abella danger filmleri
Angela White video: Angela White izle – Angela White video
https://sweetiefox.online/# swetie fox
https://abelladanger.online/# abella danger video
http://lanarhoades.fun/# lana rhoades video
http://angelawhite.pro/# Angela Beyaz modeli
Angela White izle: Angela White filmleri – Angela White video
http://evaelfie.pro/# eva elfie video
https://sweetiefox.online/# Sweetie Fox filmleri
lana rhoades modeli: lana rhoades – lana rhoades
http://lanarhoades.fun/# lana rhoades
http://evaelfie.pro/# eva elfie video
https://abelladanger.online/# abella danger video
?????? ????: Angela White – ?????? ????
https://lanarhoades.fun/# lana rhoades filmleri
http://lanarhoades.fun/# lana rhoades izle
Angela White video: ?????? ???? – Angela White
http://sweetiefox.online/# swetie fox
http://lanarhoades.fun/# lana rhodes
http://angelawhite.pro/# Angela Beyaz modeli
http://abelladanger.online/# abella danger izle
Angela White filmleri: Angela Beyaz modeli – Angela Beyaz modeli
https://sweetiefox.online/# Sweetie Fox modeli
http://sweetiefox.online/# sweety fox
lana rhoades video: lana rhoades video – lana rhoades izle
http://sweetiefox.online/# Sweetie Fox video
http://evaelfie.pro/# eva elfie video
http://sweetiefox.online/# sweeti fox
https://angelawhite.pro/# Angela White filmleri
lana rhoades filmleri: lana rhoades modeli – lana rhoades
https://sweetiefox.online/# Sweetie Fox video
eva elfie izle: eva elfie izle – eva elfie filmleri
https://lanarhoades.fun/# lana rhoades video
https://angelawhite.pro/# Angela White filmleri
http://sweetiefox.online/# Sweetie Fox video
http://angelawhite.pro/# Angela White filmleri
https://angelawhite.pro/# Angela White filmleri
lana rhoades: lana rhoades – lana rhoades filmleri
http://sweetiefox.online/# swetie fox
http://evaelfie.pro/# eva elfie video
sweety fox: Sweetie Fox filmleri – sweeti fox
http://angelawhite.pro/# Angela Beyaz modeli
eva elfie modeli: eva elfie video – eva elfie modeli
eva elfie: eva elfie full video – eva elfie hd
https://evaelfie.site/# eva elfie hd
mia malkova videos: mia malkova hd – mia malkova videos
https://evaelfie.site/# eva elfie photo
japanese singles dating sites: http://sweetiefox.pro/# ph sweetie fox
https://sweetiefox.pro/# sweetie fox video
eva elfie videos: eva elfie full video – eva elfie photo
mia malkova new video: mia malkova videos – mia malkova movie
sweetie fox new: sweetie fox new – sweetie fox
http://sweetiefox.pro/# sweetie fox full
facebook dating: https://lanarhoades.pro/# lana rhoades
lana rhoades unleashed: lana rhoades solo – lana rhoades solo
mia malkova photos: mia malkova latest – mia malkova
https://sweetiefox.pro/# fox sweetie
fox sweetie: sweetie fox cosplay – sweetie fox video
online dating website: https://evaelfie.site/# eva elfie hot
https://evaelfie.site/# eva elfie
sweetie fox full: sweetie fox – ph sweetie fox
mia malkova only fans: mia malkova new video – mia malkova movie
http://sweetiefox.pro/# sweetie fox new
sweetie fox: ph sweetie fox – sweetie fox
interracial dating: http://miamalkova.life/# mia malkova new video
Thanks for sharing. I read many of your blog posts, cool, your blog is very good.
lana rhoades solo: lana rhoades pics – lana rhoades hot
https://miamalkova.life/# mia malkova new video
lana rhoades: lana rhoades unleashed – lana rhoades videos
mia malkova full video: mia malkova girl – mia malkova
eris free downloads chatting apps: https://miamalkova.life/# mia malkova movie
https://evaelfie.site/# eva elfie photo
mia malkova movie: mia malkova only fans – mia malkova girl
https://miamalkova.life/# mia malkova hd
mia malkova latest: mia malkova latest – mia malkova movie
fox sweetie: ph sweetie fox – sweetie fox new
dating sites free no registration: https://sweetiefox.pro/# sweetie fox video
http://sweetiefox.pro/# fox sweetie
mia malkova hd: mia malkova new video – mia malkova full video
http://evaelfie.site/# eva elfie
ph sweetie fox: ph sweetie fox – sweetie fox full
lana rhoades hot: lana rhoades – lana rhoades pics
aviator oyna slot: aviator oyna – aviator oyunu
https://jogodeaposta.fun/# deposito minimo 1 real
https://jogodeaposta.fun/# jogo de aposta
aviator jogo: estrela bet aviator – estrela bet aviator
https://jogodeaposta.fun/# aplicativo de aposta
http://aviatormalawi.online/# aviator betting game
aviator sinyal hilesi: aviator hilesi – pin up aviator
aplicativo de aposta: depósito mínimo 1 real – melhor jogo de aposta
https://aviatoroyunu.pro/# aviator sinyal hilesi
pin-up: pin up – cassino pin up
aviator betano: aviator jogar – aviator jogo
http://aviatormalawi.online/# aviator
aviator game online: play aviator – aviator bet malawi login
http://aviatormocambique.site/# jogar aviator
https://aviatormalawi.online/# aviator bet malawi login
aviator ghana: aviator game bet – aviator game
aviator bahis: aviator – aviator oyunu
pin up aviator: aviator oyunu – aviator sinyal hilesi
aplicativo de aposta: melhor jogo de aposta para ganhar dinheiro – aviator jogo de aposta
https://aviatorghana.pro/# aviator betting game
play aviator: aviator game online – aviator bet malawi login
aviator game: aviator game – aviator jogar
pin-up casino login: pin up casino – pin up casino
pin-up casino login: pin-up casino – pin up cassino online
aviator mz: aviator mocambique – como jogar aviator em mocambique
http://aviatormalawi.online/# aviator game online
aviator game: aviator betting game – aviator game online
zithromax 250 price: zithromax 250 mg australia – zithromax cost uk
aviator bet: aviator game – aviator jogo
http://aviatorjogar.online/# aviator betano
aviator hilesi: aviator – aviator hilesi
zithromax 500mg over the counter – https://azithromycin.pro/zithromax-vs-doxycycline.html buy zithromax online cheap
jogar aviator Brasil: jogar aviator online – jogar aviator Brasil
aviator sportybet ghana: aviator game online – aviator bet
buy azithromycin zithromax: zithromax for cats generic zithromax medicine
http://aviatorghana.pro/# aviator ghana
aviator jogo de aposta: aviator jogo de aposta – aviator jogo de aposta
mail order pharmacy india: online pharmacy in india – india pharmacy mail order indianpharm.store
online canadian pharmacy review Canadian pharmacy prices canadian pharmacy review canadianpharm.store
canadian pharmacy no rx needed: canadian pharmacy ltd – reputable canadian pharmacy canadianpharm.store
http://canadianpharmlk.shop/# canadian mail order pharmacy canadianpharm.store
п»їlegitimate online pharmacies india: online pharmacy in india – indianpharmacy com indianpharm.store
mexican drugstore online Medicines Mexico mexico pharmacies prescription drugs mexicanpharm.shop
http://canadianpharmlk.shop/# pharmacy in canada canadianpharm.store
https://indianpharm24.shop/# indian pharmacies safe indianpharm.store
http://mexicanpharm24.shop/# mexican drugstore online mexicanpharm.shop
п»їlegitimate online pharmacies india: Top online pharmacy in India – indian pharmacies safe indianpharm.store
http://mexicanpharm24.shop/# buying prescription drugs in mexico online mexicanpharm.shop
india pharmacy: Pharmacies in India that ship to USA – top online pharmacy india indianpharm.store
https://indianpharm24.shop/# indianpharmacy com indianpharm.store
https://mexicanpharm24.shop/# best mexican online pharmacies mexicanpharm.shop
http://canadianpharmlk.shop/# legitimate canadian pharmacies canadianpharm.store
mexican pharmacy: Mexico pharmacy online – mexico drug stores pharmacies mexicanpharm.shop
https://canadianpharmlk.com/# canadian king pharmacy canadianpharm.store
mail order pharmacy india Online medicine home delivery top online pharmacy india indianpharm.store
http://mexicanpharm24.shop/# medication from mexico pharmacy mexicanpharm.shop
best online pharmacies in mexico: Mexico pharmacy online – mexico pharmacies prescription drugs mexicanpharm.shop
https://canadianpharmlk.com/# maple leaf pharmacy in canada canadianpharm.store
https://mexicanpharm24.com/# medicine in mexico pharmacies mexicanpharm.shop
https://indianpharm24.shop/# best online pharmacy india indianpharm.store
reputable indian online pharmacy: Pharmacies in India that ship to USA – india pharmacy indianpharm.store
п»їbest mexican online pharmacies: Mexico pharmacy price list – medicine in mexico pharmacies mexicanpharm.shop
http://mexicanpharm24.shop/# buying from online mexican pharmacy mexicanpharm.shop
https://mexicanpharm24.com/# best online pharmacies in mexico mexicanpharm.shop
https://indianpharm24.shop/# india pharmacy mail order indianpharm.store
buying prescription drugs in mexico buying from online mexican pharmacy buying from online mexican pharmacy mexicanpharm.shop
https://canadianpharmlk.com/# legit canadian pharmacy canadianpharm.store
medicine in mexico pharmacies: Medicines Mexico – mexican pharmacy mexicanpharm.shop
http://mexicanpharm24.com/# buying from online mexican pharmacy mexicanpharm.shop
https://indianpharm24.shop/# buy prescription drugs from india indianpharm.store
https://canadianpharmlk.com/# canadian pharmacy 365 canadianpharm.store
reputable canadian online pharmacy: My Canadian pharmacy – canadapharmacyonline legit canadianpharm.store
http://mexicanpharm24.com/# best online pharmacies in mexico mexicanpharm.shop
canadian pharmacy online store: Certified Canadian pharmacies – best canadian online pharmacy reviews canadianpharm.store
http://canadianpharmlk.shop/# canadadrugpharmacy com canadianpharm.store
https://prednisonest.pro/# how much is prednisone 10mg
where buy generic clomid pill: get generic clomid no prescription – order clomid without a prescription
how can i get generic clomid for sale: clomid 50mg price – where can i buy generic clomid without insurance
prednisone 20 mg tablet buy prednisone tablets uk cost of prednisone in canada
cost of cheap clomid without a prescription: pct clomid – can i purchase generic clomid
how to buy amoxycillin: drinking on amoxicillin – amoxicillin 500mg capsules
https://prednisonest.pro/# prednisone price
where to get prednisone: prednisone 10mg tablet cost – prednisone pills cost
purchase amoxicillin online: can i buy amoxicillin over the counter – amoxicillin 500 coupon
1250 mg prednisone: prednisone dosage – prednisone online paypal
http://prednisonest.pro/# prednisone rx coupon
where can i buy clomid: side effects of clomid – can i order clomid pill
prednisone buy: moon face prednisone – prednisone 30 mg daily
http://prednisonest.pro/# where can i order prednisone 20mg
20mg prednisone: buy prednisone canadian pharmacy – prednisone 10mg cost
iv prednisone 200 mg prednisone daily ordering prednisone
can i get generic clomid without rx: best days to take clomid for twins forum – get clomid now
amoxicillin tablets in india: does amoxicillin treat chlamydia – how to buy amoxycillin
cheap clomid for sale: where to get generic clomid pill – where to buy generic clomid no prescription
where to get clomid now: cost of clomid – can you buy clomid for sale
http://amoxilst.pro/# where can you buy amoxicillin over the counter
prednisone 40 mg tablet: prednisone 10mg online – prednisone 20 mg
http://prednisonest.pro/# prednisone 20mg tab price
medicine prednisone 10mg: tylenol and prednisone – prednisone 20mg by mail order
875 mg amoxicillin cost: amoxicillin clavulanic acid warnings – how to get amoxicillin over the counter
buy amoxicillin 250mg: can i buy amoxicillin over the counter – ampicillin amoxicillin
amoxicillin where to get: amoxicillin pills – buy amoxicillin 500mg online
https://onlinepharmacy.cheap/# foreign pharmacy no prescription
https://edpills.guru/# get ed meds today
buying prescription drugs from canada: mexico pharmacy online – online pharmacy no prescription
foreign pharmacy no prescription: online pharmacy delivery – canadian pharmacy no prescription needed
https://pharmnoprescription.pro/# non prescription canadian pharmacy
canadian prescriptions in usa: canada pharmacies online prescriptions – pills no prescription
how to order prescription drugs from canada: how to order prescription drugs from canada – canadian pharmacy without a prescription
https://edpills.guru/# cheapest erectile dysfunction pills
where can i buy erectile dysfunction pills: ed medications cost – ed pills for sale
top rated ed pills ed pills ed prescription online
buy medication online without prescription: buy prescription drugs without a prescription – prescription from canada
https://onlinepharmacy.cheap/# online pharmacy no prescription needed
http://edpills.guru/# buy ed medication online
online ed pharmacy: erection pills online – erectile dysfunction pills for sale
prescription canada: buy prescription drugs without a prescription – canada prescription drugs online
http://pharmnoprescription.pro/# best online pharmacy without prescriptions
canadian prescription: pills no prescription – online pharmacy reviews no prescription
prescription free canadian pharmacy: mexican pharmacy online – online pharmacy prescription
canada prescription: best no prescription online pharmacies – buying prescription drugs in india
https://pharmnoprescription.pro/# buy meds online no prescription
canadian pharmacies not requiring prescription online pharmacy drugstore com online pharmacy prescription drugs
prescription drugs online canada: canadian prescription drugstore review – canadian prescription drugstore review
http://onlinepharmacy.cheap/# online pharmacy no prescription
mail order pharmacy no prescription: pharmacy online – legit non prescription pharmacies
online drugs no prescription: order prescription drugs online without doctor – canadian pharmacy without a prescription
http://edpills.guru/# ed rx online
medication online without prescription: no prescription drugs – canadian pharmacy no prescription required
contrave user reviews
pharmacy website india: buy medicines online in india – Online medicine order
http://canadianpharm.guru/# drugs from canada
buying prescription drugs in india pills no prescription cheap prescription medication online
http://pharmacynoprescription.pro/# pharmacy no prescription
indian pharmacies safe: pharmacy website india – cheapest online pharmacy india
online canadian pharmacy: canada drugs reviews – buying from canadian pharmacies
http://indianpharm.shop/# india pharmacy mail order
canadian pharmacy drugs online: canadian pharmacies that deliver to the us – pet meds without vet prescription canada
mexican border pharmacies shipping to usa: reputable mexican pharmacies online – medication from mexico pharmacy
https://indianpharm.shop/# cheapest online pharmacy india
canada pharmacy world: is canadian pharmacy legit – canadian pharmacy 365
mexico pharmacy: mexico pharmacy – reputable mexican pharmacies online
https://indianpharm.shop/# indianpharmacy com
canadian pharmacy 24 com canadian pharmacy 24h com best canadian pharmacy to buy from
mexican rx online: medication from mexico pharmacy – buying prescription drugs in mexico online
buy medications without a prescription: best non prescription online pharmacy – how to get a prescription in canada
http://canadianpharm.guru/# pharmacy wholesalers canada
no prescription needed online pharmacy: online drugs without prescription – discount prescription drugs canada
pharmacy com canada: canadianpharmacyworld – reputable canadian pharmacy
https://canadianpharm.guru/# canadian pharmacy 365
buy prescription drugs from india: best online pharmacy india – india pharmacy
online pharmacy india: indian pharmacies safe – buy prescription drugs from india
canadian pharmacy mall: legitimate canadian mail order pharmacy – canadian pharmacy meds reviews
http://mexicanpharm.online/# mexico pharmacies prescription drugs
http://mexicanpharm.online/# buying prescription drugs in mexico
canadian online pharmacy reviews: canadian pharmacy service – canadian neighbor pharmacy
top 10 pharmacies in india india pharmacy mail order india online pharmacy
how to order prescription drugs from canada: meds online without prescription – how to get a prescription in canada
buy prescription drugs from canada cheap: pharmacy com canada – buy canadian drugs
best online pharmacies in mexico: mexico pharmacies prescription drugs – mexican online pharmacies prescription drugs
http://mexicanpharm.online/# mexico drug stores pharmacies
buying from online mexican pharmacy: mexican online pharmacies prescription drugs – mexican drugstore online
online prescription canada: canada prescriptions by mail – medication online without prescription
http://canadianpharm.guru/# canadian pharmacy meds review
buying drugs online no prescription: meds online without prescription – canada drugs no prescription
canadian prescription: buy medications online no prescription – how to get prescription drugs from canada
https://indianpharm.shop/# indian pharmacies safe
precription drugs from canada: onlinepharmaciescanada com – reputable canadian pharmacy
medication from mexico pharmacy mexico drug stores pharmacies medicine in mexico pharmacies
http://indianpharm.shop/# reputable indian pharmacies
canadian pharmacy 24: reliable canadian pharmacy – canadian pharmacy prices
pharmacies in mexico that ship to usa: mexico pharmacies prescription drugs – medication from mexico pharmacy
overseas online pharmacy-no prescription: buy prescription online – buy prescription drugs online without doctor
http://canadianpharm.guru/# reputable canadian online pharmacy
mexico drug stores pharmacies: mexican border pharmacies shipping to usa – buying prescription drugs in mexico online
onlinecanadianpharmacy: pharmacy com canada – trusted canadian pharmacy
http://indianpharm.shop/# india pharmacy
adderall canadian pharmacy: best mail order pharmacy canada – canadian neighbor pharmacy
buy prescription online: mail order prescriptions from canada – canada prescriptions by mail
canadian pharmacy: onlinepharmaciescanada com – best canadian online pharmacy reviews
http://mexicanpharm.online/# mexican pharmaceuticals online
buy drugs online no prescription purchasing prescription drugs online canada prescriptions by mail
http://indianpharm.shop/# mail order pharmacy india
indianpharmacy com: buy medicines online in india – pharmacy website india
buying online prescription drugs: can you buy prescription drugs in canada – non prescription pharmacy
top online pharmacy india: world pharmacy india – india online pharmacy
http://pharmacynoprescription.pro/# cheap drugs no prescription
buying prescription drugs in mexico: mexico drug stores pharmacies – mexico pharmacy
Online medicine home delivery: mail order pharmacy india – indian pharmacy online
canadian pharmacy king: cheap canadian pharmacy online – pharmacies in canada that ship to the us
canadian prescription: online pharmacy without prescription – online prescription canada
http://mexicanpharm.online/# medication from mexico pharmacy
http://mexicanpharm.online/# best online pharmacies in mexico
canadian prescription drugstore reviews canadian pharmacy without prescription quality prescription drugs canada
mexico drug stores pharmacies: mexico pharmacy – reputable mexican pharmacies online
mail order pharmacy india: india online pharmacy – world pharmacy india
http://canadianpharm.guru/# legitimate canadian mail order pharmacy
legal canadian pharmacy online: ordering drugs from canada – canada ed drugs
http://pinupgiris.fun/# pin up indir
sweet bonanza 90 tl: sweet bonanza guncel – sweet bonanza kazanc
http://aviatoroyna.bid/# aviator uçak oyunu
http://pinupgiris.fun/# pin up casino guncel giris
gates of olympus 1000 demo: gates of olympus taktik – gates of olympus demo oyna
sweet bonanza nas?l oynan?r: sweet bonanza free spin demo – sweet bonanza demo turkce
https://aviatoroyna.bid/# aviator bahis
https://aviatoroyna.bid/# uçak oyunu bahis aviator
gates of olympus giris: gates of olympus hilesi – gates of olympus oyna demo
https://slotsiteleri.guru/# slot siteleri
http://slotsiteleri.guru/# en çok kazandiran slot siteleri
http://sweetbonanza.bid/# sweet bonanza demo
gates of olympus max win: gates of olympus – gates of olympus max win
aviator giris: aviator sinyal hilesi – aviator oyunu
http://aviatoroyna.bid/# aviator oyna slot
gates of olympus demo: gates of olympus demo – gates of olympus guncel
http://pinupgiris.fun/# pin up casino indir
http://aviatoroyna.bid/# aviator
gates of olympus nas?l para kazanilir: gates of olympus – gates of olympus oyna demo
http://sweetbonanza.bid/# güncel sweet bonanza
http://sweetbonanza.bid/# sweet bonanza oyna
sweet bonanza oyna: sweet bonanza demo oyna – sweet bonanza taktik
https://sweetbonanza.bid/# sweet bonanza nasil oynanir
sweet bonanza taktik: sweet bonanza kazanma saatleri – sweet bonanza free spin demo
http://aviatoroyna.bid/# aviator hile
http://aviatoroyna.bid/# aviator casino oyunu
http://gatesofolympus.auction/# gates of olympus max win
aviator oyunu 10 tl: aviator oyunu 50 tl – aviator sinyal hilesi apk
en guvenilir slot siteleri: slot siteleri guvenilir – guvenilir slot siteleri
https://sweetbonanza.bid/# sweet bonanza hilesi
pin up bet: pin up indir – pin up casino
http://slotsiteleri.guru/# en iyi slot siteleri 2024
Thank you for your sharing. I am worried that I lack creative ideas. It is your article that makes me full of hope. Thank you. But, I have a question, can you help me?
https://aviatoroyna.bid/# aviator oyna slot
canl? slot siteleri: deneme veren slot siteleri – casino slot siteleri
http://sweetbonanza.bid/# sweet bonanza giris
pharmacy website india: indian pharmacy – world pharmacy india
best india pharmacy Cheapest online pharmacy buy prescription drugs from india
http://indianpharmacy.icu/# buy prescription drugs from india
canadian medications: Large Selection of Medications – pet meds without vet prescription canada
best canadian pharmacy: Certified Canadian Pharmacy – pharmacy in canada
buying prescription drugs in mexico online mexican pharmacy mexico pharmacy
legitimate canadian pharmacy online: Certified Canadian Pharmacy – canadian pharmacy review
pharmacies in mexico that ship to usa: purple pharmacy mexico price list – п»їbest mexican online pharmacies
canada drugs online real canadian pharmacy canadian pharmacies
mexican online pharmacies prescription drugs: Mexican Pharmacy Online – mexico drug stores pharmacies
http://mexicanpharmacy.shop/# mexican mail order pharmacies
mail order pharmacy india: india online pharmacy – Online medicine order
buy medicines online in india: reputable indian online pharmacy – buy medicines online in india
best india pharmacy: indian pharmacy delivery – world pharmacy india
best online pharmacy india Healthcare and medicines from India indian pharmacy paypal
buying from online mexican pharmacy: mexico pharmacy – mexico drug stores pharmacies
canada rx pharmacy world: online pharmacy canada – canadian pharmacy victoza
reputable indian online pharmacy: Generic Medicine India to USA – online pharmacy india
indianpharmacy com Generic Medicine India to USA mail order pharmacy india
reputable indian online pharmacy: Generic Medicine India to USA – indian pharmacy
canadian online pharmacy: Certified Canadian Pharmacy – canadian family pharmacy
http://mexicanpharmacy.shop/# mexico drug stores pharmacies
the canadian pharmacy Certified Canadian Pharmacy canada drugs reviews
reputable indian online pharmacy: Healthcare and medicines from India – Online medicine home delivery
india pharmacy mail order: Generic Medicine India to USA – best india pharmacy
mexican border pharmacies shipping to usa: cheapest mexico drugs – medication from mexico pharmacy
mail order pharmacy india Online medicine home delivery india pharmacy mail order
best online pharmacy india Healthcare and medicines from India top 10 pharmacies in india
https://canadianpharmacy24.store/# canadian pharmacy phone number
mexico drug stores pharmacies: Online Pharmacies in Mexico – mexico drug stores pharmacies
mexican pharmacy: Online Pharmacies in Mexico – medicine in mexico pharmacies
canada ed drugs: Large Selection of Medications – canada pharmacy online
mexican drugstore online cheapest mexico drugs pharmacies in mexico that ship to usa
canada drugs online: Certified Canadian Pharmacy – online pharmacy canada
india online pharmacy: indian pharmacy delivery – top 10 pharmacies in india
zithromax 500 tablet zithromax 500 tablet zithromax buy
https://prednisoneall.com/# 25 mg prednisone
https://zithromaxall.shop/# where to buy zithromax in canada
http://clomidall.com/# cost of cheap clomid without a prescription
purchase prednisone no prescription: prednisone 54899 – online order prednisone 10mg
zithromax 250 price zithromax 500 price zithromax cost australia
how to buy clomid for sale: can i order generic clomid without a prescription – how can i get clomid tablets
http://prednisoneall.shop/# prednisone uk price
http://amoxilall.shop/# order amoxicillin online no prescription
buy zithromax without prescription online zithromax 1000 mg pills zithromax 500 mg lowest price drugstore online
https://amoxilall.shop/# price for amoxicillin 875 mg
http://clomidall.shop/# can i buy generic clomid without insurance
amoxil generic amoxicillin 875 125 mg tab buy amoxicillin online without prescription
http://amoxilall.com/# amoxicillin online without prescription
zithromax buy zithromax for sale cheap where can you buy zithromax
https://prednisoneall.com/# prednisone 0.5 mg
https://clomidall.shop/# can you get generic clomid tablets
prednisone 2 mg: prednisone 40 mg – cheap prednisone online
where to buy clomid tablets: where to get clomid – can i buy clomid for sale
http://zithromaxall.shop/# can i buy zithromax over the counter
amoxicillin 500 mg tablet buy amoxicillin 250mg can you buy amoxicillin uk
https://prednisoneall.com/# prednisone cream
http://amoxilall.shop/# amoxicillin from canada
http://amoxilall.com/# price for amoxicillin 875 mg
cost generic clomid can i order generic clomid tablets how to buy generic clomid without rx
http://clomidall.com/# clomid tablet
amoxicillin 500mg capsule cost buy amoxicillin online mexico amoxicillin price without insurance
http://amoxilall.com/# amoxicillin capsule 500mg price
zithromax 500 tablet: zithromax over the counter canada – can i buy zithromax online
prednisone 1mg purchase: prednisone for sale online – prednisone 2 5 mg
http://prednisoneall.shop/# prednisone 20mg nz
https://prednisoneall.com/# prednisone uk over the counter
prednisone without prescription buy generic prednisone online prednisone 2 5 mg
https://prednisoneall.shop/# prednisone over the counter
prednisone over the counter prednisone 10 mg coupon buy 10 mg prednisone
http://prednisoneall.com/# prednisone steroids
Generic Viagra for sale: buy viagra here – viagra canada
Buy Viagra online cheap Viagra Tablet price viagra canada
buy Kamagra: Kamagra Oral Jelly – Kamagra tablets
Generic Viagra for sale: sildenafil iq – Viagra without a doctor prescription Canada
Generic Cialis without a doctor prescription cheapest cialis Generic Cialis without a doctor prescription
http://tadalafiliq.com/# Tadalafil Tablet
http://tadalafiliq.com/# Generic Tadalafil 20mg price
Generic Tadalafil 20mg price: cheapest cialis – cialis generic
sildenafil 50 mg price: sildenafil iq – Cheap Viagra 100mg
sildenafil oral jelly 100mg kamagra: Sildenafil Oral Jelly – sildenafil oral jelly 100mg kamagra
buy kamagra online usa: Kamagra gel – kamagra
super kamagra kamagra best price buy Kamagra
sildenafil oral jelly 100mg kamagra: Sildenafil Oral Jelly – sildenafil oral jelly 100mg kamagra
http://kamagraiq.com/# super kamagra
https://kamagraiq.com/# Kamagra tablets
Kamagra Oral Jelly: kamagra – super kamagra
cheap kamagra sildenafil oral jelly 100mg kamagra Kamagra 100mg price
http://kamagraiq.com/# Kamagra 100mg
best price for viagra 100mg: buy viagra online – Viagra generic over the counter
viagra without prescription buy viagra online over the counter sildenafil
https://sildenafiliq.com/# Generic Viagra for sale
п»їkamagra: Sildenafil Oral Jelly – Kamagra 100mg
cheapest cialis: Buy Cialis online – Cialis 20mg price
https://sildenafiliq.com/# Viagra online price
Tadalafil price: Buy Cialis online – Tadalafil price
https://sildenafiliq.com/# Viagra online price
https://sildenafiliq.xyz/# Sildenafil 100mg price
Kamagra tablets: Kamagra 100mg price – Kamagra Oral Jelly
п»їkamagra Kamagra Iq sildenafil oral jelly 100mg kamagra
https://tadalafiliq.com/# Generic Cialis price
https://tadalafiliq.com/# Cialis 20mg price
Viagra Tablet price: generic ed pills – sildenafil 50 mg price
http://tadalafiliq.shop/# Generic Cialis price
Generic Cialis price Generic Tadalafil 20mg price Tadalafil Tablet
cialis generic: Generic Tadalafil 20mg price – Buy Tadalafil 5mg
https://tadalafiliq.com/# Cialis without a doctor prescription
https://tadalafiliq.com/# Generic Tadalafil 20mg price
Buy Tadalafil 5mg: cialis best price – cialis for sale
super kamagra Kamagra Oral Jelly Price п»їkamagra
http://tadalafiliq.shop/# Generic Tadalafil 20mg price
sildenafil online: buy viagra online – Buy generic 100mg Viagra online
https://mexicanpharmgrx.shop/# best online pharmacies in mexico
canadian discount pharmacy: Canada pharmacy – best canadian pharmacy
canada drugs online Cheapest drug prices Canada safe canadian pharmacy
http://indianpharmgrx.com/# best online pharmacy india
canadian pharmacy prices: Best Canadian online pharmacy – canadian online pharmacy
best online pharmacies in mexico mexican pharmacy medicine in mexico pharmacies
https://canadianpharmgrx.xyz/# my canadian pharmacy review
mexico drug stores pharmacies: mexican pharmacy – medicine in mexico pharmacies
safe online pharmacies in canada: Certified Canadian pharmacies – northwest pharmacy canada
https://canadianpharmgrx.com/# prescription drugs canada buy online
online canadian drugstore canadian pharmacy best online canadian pharmacy
https://indianpharmgrx.com/# Online medicine order
reddit canadian pharmacy Pharmacies in Canada that ship to the US canadian online pharmacy reviews
http://mexicanpharmgrx.shop/# best online pharmacies in mexico
п»їbest mexican online pharmacies: online pharmacy in Mexico – medicine in mexico pharmacies
mail order pharmacy india: п»їlegitimate online pharmacies india – indian pharmacy online
Online medicine home delivery indian pharmacy delivery indianpharmacy com
http://mexicanpharmgrx.shop/# mexican mail order pharmacies
buying prescription drugs in mexico: Pills from Mexican Pharmacy – mexican pharmaceuticals online
mexican pharmaceuticals online mexican mail order pharmacies buying from online mexican pharmacy
http://indianpharmgrx.com/# cheapest online pharmacy india
medication from mexico pharmacy: medicine in mexico pharmacies – buying from online mexican pharmacy
medication from mexico pharmacy Mexico drugstore п»їbest mexican online pharmacies
https://mexicanpharmgrx.shop/# pharmacies in mexico that ship to usa
п»їbest mexican online pharmacies: online pharmacy in Mexico – mexican pharmaceuticals online
http://mexicanpharmgrx.shop/# purple pharmacy mexico price list
buying from canadian pharmacies Cheapest drug prices Canada global pharmacy canada
mail order pharmacy india: indian pharmacy – india pharmacy mail order
mexico pharmacies prescription drugs: Mexico drugstore – mexican border pharmacies shipping to usa
http://canadianpharmgrx.xyz/# canadian online pharmacy
the canadian pharmacy My Canadian pharmacy certified canadian international pharmacy
https://mexicanpharmgrx.shop/# reputable mexican pharmacies online
http://indianpharmgrx.shop/# online shopping pharmacy india
my canadian pharmacy: My Canadian pharmacy – canadian world pharmacy
indianpharmacy com: Generic Medicine India to USA – best india pharmacy
medication from mexico pharmacy online pharmacy in Mexico best online pharmacies in mexico
diflucan online cheap without a prescription: how to buy diflucan online – diflucan 6
п»їcytotec pills online: п»їcytotec pills online – Abortion pills online
ciprofloxacin generic price: buy cipro online without prescription – cipro 500mg best prices
buy doxycycline without prescription uk where to purchase doxycycline doxycycline online
https://nolvadex.icu/# alternatives to tamoxifen
tamoxifen cancer: aromatase inhibitor tamoxifen – tamoxifen rash
cipro 500mg best prices: buy cipro online – п»їcipro generic
tamoxifen depression: tamoxifen brand name – tamoxifen and depression
nolvadex d should i take tamoxifen tamoxifen
Misoprostol 200 mg buy online: cytotec buy online usa – buy cytotec online fast delivery
where can you get diflucan cost of diflucan diflucan 200
buy doxycycline: order doxycycline online – doxycycline without a prescription
buy ciprofloxacin over the counter: buy cipro online without prescription – cipro 500mg best prices
doxycycline medication: doxycycline 50 mg – doxycycline online
buy cytotec in usa order cytotec online buy misoprostol over the counter
cipro for sale: buy generic ciprofloxacin – buy ciprofloxacin
https://misoprostol.top/# buy cytotec pills online cheap
Abortion pills online: purchase cytotec – buy cytotec pills online cheap
buy cipro cheap buy ciprofloxacin buy cipro online
cytotec pills buy online: buy cytotec over the counter – buy cytotec over the counter
can you buy diflucan over the counter in australia: can you buy diflucan in mexico – cost of diflucan prescription in mexico
Abortion pills online buy cytotec online fast delivery order cytotec online
buy cytotec online fast delivery: cytotec online – buy cytotec over the counter
buy doxycycline online uk: doxycycline 100mg dogs – doxycycline 200 mg
tamoxifen and uterine thickening: does tamoxifen make you tired – tamoxifen hot flashes
ciprofloxacin ciprofloxacin over the counter cipro 500mg best prices
tamoxifen blood clots: liquid tamoxifen – tamoxifen buy
diflucan 200 mg over the counter: diflucan price in india – diflucan over the counter usa
http://ciprofloxacin.guru/# buy cipro
tamoxifen side effects forum where can i buy nolvadex tamoxifen postmenopausal
tamoxifen endometrium: nolvadex for sale amazon – tamoxifen 20 mg
doxycycline 100mg capsules: vibramycin 100 mg – doxycycline 100mg online
tamoxifen dose: tamoxifen adverse effects – tamoxifen chemo
tamoxifen alternatives tamoxifen cancer does tamoxifen make you tired
diflucan 150 mg capsule: where to get diflucan otc – where can i purchase diflucan
diflucan 100mg: diflucan 250 mg – buy diflucan online
diflucan online cheap diflucan 150 mg canada diflucan 150 mg tablet
https://misoprostol.top/# buy cytotec over the counter
buy prednisone 20mg: prednisone 20mg prices – buy prednisone 20mg
zithromax over the counter: generic zithromax over the counter – zithromax 500 mg lowest price online
buy prednisone online fast shipping prednisone 40 mg tablet prednisone 20mg tab price
clomid otc: can i get clomid pill – where can i buy generic clomid without prescription
amoxicillin online no prescription can i buy amoxicillin online amoxicillin 500 mg
can you get cheap clomid: where can i buy cheap clomid no prescription – clomid
prednisone 2.5 mg daily: prednisone 12 mg – prednisone 10 mg brand name
http://amoxicillina.top/# ampicillin amoxicillin
can i get clomid without insurance: where to buy clomid online – can i purchase generic clomid pills
http://clomida.pro/# where can i get cheap clomid without insurance
prednisone uk buy: prednisone canada prices – how can i order prednisone
zithromax 250mg purchase zithromax online zithromax 500 mg for sale
http://amoxicillina.top/# amoxicillin online purchase
amoxicillin for sale online: amoxicillin 500 mg where to buy – amoxicillin 500mg prescription
zithromax 500 mg lowest price drugstore online zithromax without prescription zithromax tablets for sale
stromectol tab 3mg: stromectol nz – ivermectin 400 mg brands
zithromax price canada: cost of generic zithromax – where can i buy zithromax in canada
http://prednisonea.store/# order prednisone online canada
get cheap clomid: can you buy cheap clomid pill – can you get generic clomid without dr prescription
can i buy amoxicillin over the counter in australia where to buy amoxicillin price for amoxicillin 875 mg
where to buy cheap clomid tablets: how to get generic clomid no prescription – where to get clomid pills
https://amoxicillina.top/# amoxicillin medicine over the counter
http://azithromycina.pro/# zithromax online no prescription
zithromax capsules price: buy zithromax no prescription – buy cheap zithromax online
https://onlinepharmacyworld.shop/# no prescription needed pharmacy
online ed medication: ed meds on line – cheap ed medicine
https://edpill.top/# ed drugs online
best ed pills online ed meds on line order ed pills
http://edpill.top/# ed prescription online
pills for erectile dysfunction online: cheap erectile dysfunction pills – top rated ed pills
cheapest ed medication top rated ed pills cheapest ed treatment
medicine with no prescription: cheap prescription drugs online – buy pills without prescription
https://onlinepharmacyworld.shop/# canadian pharmacy no prescription
http://medicationnoprescription.pro/# mexican pharmacy no prescription
http://onlinepharmacyworld.shop/# online pharmacy discount code
online erectile dysfunction medication: cheap ed meds online – what is the cheapest ed medication
http://edpill.top/# online ed treatments
canadian pharmacies not requiring prescription no prescription required pharmacy canadian prescription pharmacy
http://medicationnoprescription.pro/# online pharmacy that does not require a prescription
erectile dysfunction pills online: discount ed pills – ed meds by mail
http://edpill.top/# erectile dysfunction pills for sale
no prescription pharmacy online online drugs no prescription non prescription online pharmacy
http://onlinepharmacyworld.shop/# pharmacy no prescription required
can i buy prescription drugs in canada: pharmacy no prescription – no prescription
online pharmacy discount code: online pharmacy discount code – pharmacy coupons
https://edpill.top/# ed med online
http://edpill.top/# ed prescriptions online
canadian pharmacy discount code cheapest pharmacy to get prescriptions filled canadian pharmacy world coupon code
https://edpill.top/# cheap erection pills
http://casinvietnam.com/# casino tr?c tuy?n vi?t nam
casino tr?c tuy?n vi?t nam: web c? b?c online uy tín – casino tr?c tuy?n
https://casinvietnam.com/# choi casino tr?c tuy?n tren di?n tho?i
choi casino tr?c tuy?n tren di?n tho?i game c? b?c online uy tin casino tr?c tuy?n vi?t nam
http://casinvietnam.com/# choi casino tr?c tuy?n tren di?n tho?i
game c? b?c online uy tín: casino online uy tín – casino online uy tín
choi casino tr?c tuy?n trên di?n tho?i: game c? b?c online uy tín – casino tr?c tuy?n
dánh bài tr?c tuy?n: casino tr?c tuy?n vi?t nam – game c? b?c online uy tín
casino tr?c tuy?n uy tín: casino tr?c tuy?n vi?t nam – game c? b?c online uy tín
dánh bài tr?c tuy?n: casino tr?c tuy?n uy tín – casino tr?c tuy?n
web c? b?c online uy tin danh bai tr?c tuy?n casino tr?c tuy?n uy tin
game c? b?c online uy tín: game c? b?c online uy tín – casino tr?c tuy?n uy tín
casino tr?c tuy?n casino tr?c tuy?n vi?t nam choi casino tr?c tuy?n tren di?n tho?i
game c? b?c online uy tín: web c? b?c online uy tín – web c? b?c online uy tín
casino online uy tín: choi casino tr?c tuy?n trên di?n tho?i – choi casino tr?c tuy?n trên di?n tho?i
choi casino tr?c tuy?n tren di?n tho?i casino tr?c tuy?n vi?t nam game c? b?c online uy tin
web c? b?c online uy tin choi casino tr?c tuy?n tren di?n tho?i casino tr?c tuy?n
https://indiaph24.store/# cheapest online pharmacy india
indian pharmacy paypal reputable indian pharmacies indian pharmacy paypal
mexican pharmaceuticals online Online Pharmacies in Mexico mexican rx online
http://mexicoph24.life/# mexican mail order pharmacies
canadian pharmacies compare Licensed Canadian Pharmacy legit canadian pharmacy
https://indiaph24.store/# india pharmacy mail order
canadian world pharmacy Large Selection of Medications from Canada pharmacy canadian
https://canadaph24.pro/# safe canadian pharmacy
pharmacy website india pharmacy website india top online pharmacy india
http://canadaph24.pro/# canadianpharmacy com
online shopping pharmacy india Cheapest online pharmacy indian pharmacies safe
http://mexicoph24.life/# mexican drugstore online
purple pharmacy mexico price list mexico pharmacies prescription drugs mexican pharmaceuticals online
https://mexicoph24.life/# mexico drug stores pharmacies
indian pharmacies safe buy medicines from India Online medicine home delivery
http://mexicoph24.life/# purple pharmacy mexico price list
online shopping pharmacy india indian pharmacy fast delivery Online medicine order
http://mexicoph24.life/# medication from mexico pharmacy
mexico drug stores pharmacies Online Pharmacies in Mexico mexico drug stores pharmacies
http://indiaph24.store/# pharmacy website india
legitimate canadian pharmacy Prescription Drugs from Canada my canadian pharmacy review
http://indiaph24.store/# world pharmacy india
reliable canadian pharmacy Licensed Canadian Pharmacy pharmacy com canada
http://mexicoph24.life/# mexican rx online
mexican online pharmacies prescription drugs Online Pharmacies in Mexico buying from online mexican pharmacy
https://mexicoph24.life/# best mexican online pharmacies
mexico drug stores pharmacies cheapest mexico drugs mexican pharmaceuticals online
http://mexicoph24.life/# mexico pharmacies prescription drugs
indian pharmacy online indian pharmacy india online pharmacy
https://mexicoph24.life/# pharmacies in mexico that ship to usa
https://mexicoph24.life/# mexican rx online
pharmacies in mexico that ship to usa mexico drug stores pharmacies medicine in mexico pharmacies
http://indiaph24.store/# best online pharmacy india
canadian drug pharmacy Certified Canadian Pharmacies canadian family pharmacy
http://indiaph24.store/# Online medicine order
77 canadian pharmacy Certified Canadian Pharmacies canadian pharmacy 365
https://mexicoph24.life/# mexican pharmacy
buy medicines online in india indian pharmacy buy medicines online in india
https://indiaph24.store/# india online pharmacy
mexico drug stores pharmacies mexico pharmacy purple pharmacy mexico price list
https://indiaph24.store/# buy medicines online in india
buying from online mexican pharmacy Online Pharmacies in Mexico mexico pharmacies prescription drugs
https://canadaph24.pro/# pharmacy wholesalers canada
reputable canadian online pharmacy Large Selection of Medications from Canada canadian pharmacy ltd
http://mexicoph24.life/# mexico drug stores pharmacies
mexico drug stores pharmacies mexican pharmacy medication from mexico pharmacy
http://canadaph24.pro/# canadian king pharmacy
world pharmacy india indian pharmacy fast delivery pharmacy website india
https://canadaph24.pro/# canadian pharmacy
indian pharmacy Cheapest online pharmacy Online medicine order
https://mexicoph24.life/# mexico pharmacy
cheap canadian pharmacy Licensed Canadian Pharmacy canada drug pharmacy
http://mexicoph24.life/# buying prescription drugs in mexico online
best rated canadian pharmacy Licensed Canadian Pharmacy is canadian pharmacy legit
https://indiaph24.store/# indian pharmacy online
http://indiaph24.store/# indianpharmacy com
real canadian pharmacy Licensed Canadian Pharmacy the canadian pharmacy
http://indiaph24.store/# top 10 pharmacies in india
mexico pharmacies prescription drugs cheapest mexico drugs mexican mail order pharmacies
https://mexicoph24.life/# mexico pharmacy
purple pharmacy mexico price list cheapest mexico drugs mexican pharmaceuticals online
https://canadaph24.pro/# canadian pharmacy meds reviews
mexican online pharmacies prescription drugs cheapest mexico drugs pharmacies in mexico that ship to usa
https://indiaph24.store/# top 10 pharmacies in india
https://mexicoph24.life/# mexico pharmacies prescription drugs
mexican rx online mexico pharmacy pharmacies in mexico that ship to usa
http://indiaph24.store/# best india pharmacy
safe reliable canadian pharmacy canadian pharmacies canadian drugstore online
https://indiaph24.store/# online pharmacy india
canadian pharmacy service buy drugs from canada canadian pharmacy ltd
https://mexicoph24.life/# mexican rx online
mexican pharmacy buying prescription drugs in mexico online mexico pharmacies prescription drugs
https://mexicoph24.life/# mexico pharmacy
top online pharmacy india buy medicines from India best india pharmacy
http://canadaph24.pro/# pharmacies in canada that ship to the us
mexican pharmacy Online Pharmacies in Mexico mexican online pharmacies prescription drugs
http://canadaph24.pro/# canadapharmacyonline com
mail order pharmacy india Cheapest online pharmacy Online medicine home delivery
http://indiaph24.store/# india pharmacy mail order
best online pharmacy india Cheapest online pharmacy cheapest online pharmacy india
http://canadaph24.pro/# canadian mail order pharmacy
mexican pharmaceuticals online Online Pharmacies in Mexico mexico pharmacies prescription drugs
https://mexicoph24.life/# mexican mail order pharmacies
reliable canadian pharmacy Large Selection of Medications from Canada buying drugs from canada
http://indiaph24.store/# india pharmacy mail order
is canadian pharmacy legit Prescription Drugs from Canada canadian drug stores
reputable mexican pharmacies online: mexico pharmacy – buying from online mexican pharmacy
lisinopril 20mg coupon lisinopril oral generic lisinopril online
cost generic propecia without rx: cheap propecia without prescription – buying cheap propecia online
http://lisinopril.network/# 2 prinivil
lisinopril 20 25 mg tab generic zestril lisinopril 20 mg for sale
buy cipro online canada: buy cipro – buy cipro online without prescription
https://finasteride.store/# order cheap propecia prices
buy cytotec pills online cheap cytotec pills buy online buy cytotec
https://finasteride.store/# cost of propecia prices
tamoxifen postmenopausal: hysterectomy after breast cancer tamoxifen – tamoxifen for men
buy cheap propecia online order propecia without a prescription order cheap propecia
http://lisinopril.network/# zestoretic coupon
buy propecia online buy propecia propecia pill
cipro generic: ciprofloxacin – buy ciprofloxacin
http://finasteride.store/# cost propecia without insurance
https://cytotec.club/# buy cytotec
order generic propecia without dr prescription cost generic propecia pills buy cheap propecia for sale
where can i buy cipro online: cipro pharmacy – ciprofloxacin
http://ciprofloxacin.tech/# cipro online no prescription in the usa
Misoprostol 200 mg buy online cytotec abortion pill cytotec buy online usa
buy cytotec: buy cytotec over the counter – purchase cytotec
https://lisinopril.network/# canadian lisinopril 10 mg
https://finasteride.store/# buy cheap propecia no prescription
buy cheap lisinopril 40mg lisinopril price lisinopril prinivil zestril
buy cipro online without prescription: ciprofloxacin – ciprofloxacin generic price
hysterectomy after breast cancer tamoxifen tamoxifen and depression nolvadex price
http://nolvadex.life/# tamoxifen brand name
tamoxifen hip pain: nolvadex estrogen blocker – tamoxifen hip pain
buy cytotec pills online cheap buy cytotec over the counter Misoprostol 200 mg buy online
http://finasteride.store/# get generic propecia
http://nolvadex.life/# nolvadex estrogen blocker
get propecia propecia for sale buy cheap propecia without rx
cytotec pills online: Abortion pills online – buy cytotec
http://ciprofloxacin.tech/# ciprofloxacin generic price
lisinopril 20 mg pill buy 20mg lisinopril lisinopril 5mg tab
tamoxifen skin changes: buy nolvadex online – nolvadex d
buy cialis
http://ciprofloxacin.tech/# ciprofloxacin order online
cost of generic propecia without rx get propecia tablets order cheap propecia without prescription
https://cytotec.club/# cytotec abortion pill
buying generic propecia without prescription: generic propecia no prescription – buying cheap propecia no prescription
viagra canada viagra without prescription Viagra Tablet price
buy Viagra over the counter: Buy generic 100mg Viagra online – buy Viagra over the counter
cheapest cenforce: Purchase Cenforce Online – cenforce for sale
http://kamagra.win/# Kamagra tablets
sildenafil oral jelly 100mg kamagra kamagra buy kamagra online usa
Cenforce 150 mg online: buy cenforce – Buy Cenforce 100mg Online
http://viagras.online/# Cheapest Sildenafil online
http://cialist.pro/# Cheap Cialis
cenforce.pro order cenforce order cenforce
Viagra online price: Buy generic 100mg Viagra online – Cheap Sildenafil 100mg
Buy generic 100mg Viagra online: Buy generic 100mg Viagra online – Buy generic 100mg Viagra online
http://kamagra.win/# sildenafil oral jelly 100mg kamagra
Kamagra 100mg price kamagra oral jelly buy kamagra online usa
https://cenforce.pro/# order cenforce
super kamagra: buy kamagra online – buy kamagra online usa
Buy Cialis online Cialis 20mg price in USA Cheap Cialis
https://kamagra.win/# п»їkamagra
http://cialist.pro/# Generic Cialis without a doctor prescription
cheap kamagra: kamagra.win – super kamagra
super kamagra buy kamagra online Kamagra 100mg
https://cenforce.pro/# Cenforce 100mg tablets for sale
Cheapest Sildenafil online: Buy Viagra online – sildenafil 50 mg price
п»їcialis generic cialist.pro Tadalafil price
best online pharmacy without prescription canada drugs no prescription buying drugs online no prescription
online meds no prescription: buy pills without prescription – online pharmacies no prescription usa
pharmacies in mexico that ship to usa: medicine in mexico pharmacies – mexico drug stores pharmacies
online pharmacy without prescription: cheapest pharmacy – rxpharmacycoupons
http://pharmworld.store/# online pharmacy no prescription
http://pharmcanada.shop/# canadian pharmacy sarasota
buying prescription medications online online pharmacy without a prescription purchasing prescription drugs online
reputable indian pharmacies: india pharmacy mail order – indian pharmacy
http://pharmworld.store/# prescription free canadian pharmacy
no prescription online pharmacies buying drugs without prescription buy medications online without prescription
canada drugs online reviews: best rated canadian pharmacy – vipps approved canadian online pharmacy
indianpharmacy com: best online pharmacy india – Online medicine home delivery
mexican pharmaceuticals online mexican pharmaceuticals online mexican pharmacy
https://pharmmexico.online/# pharmacies in mexico that ship to usa
legal to buy prescription drugs from canada: legitimate canadian pharmacy – canadian pharmacy price checker
buying prescription drugs in mexico: п»їbest mexican online pharmacies – pharmacies in mexico that ship to usa
top 10 pharmacies in india cheapest online pharmacy india india pharmacy
https://pharmworld.store/# prescription drugs online
best website to buy prescription drugs: no prescription medication – mail order prescriptions from canada
online pharmacy without prescription: online pharmacy – online pharmacy no prescription needed
pharmacy with no prescription non prescription online pharmacy india medicine with no prescription
https://pharmcanada.shop/# canadian online pharmacy
canada pharmacy online: canadian 24 hour pharmacy – trusted canadian pharmacy
zithromax 1000 mg pills zithromax over the counter canada zithromax 500mg price
https://gabapentinneurontin.pro/# neurontin 800 mg tablets
amoxicillin 825 mg: amoxicillin in india – amoxicillin 875 125 mg tab
amoxicillin discount coupon: generic for amoxicillin – price for amoxicillin 875 mg
neurontin gabapentin buy neurontin online no prescription drug neurontin 200 mg
neurontin 300mg: medicine neurontin – neurontin 100mg caps
https://zithromaxa.store/# zithromax for sale cheap
where can you buy zithromax: buy generic zithromax no prescription – zithromax 500 without prescription
neurontin 4000 mg: brand name neurontin – neurontin 330 mg
how to get prednisone without a prescription: prednisone generic brand name – purchase prednisone canada
neurontin price australia: can you buy neurontin over the counter – how to get neurontin
neurontin capsules 300mg neurontin 800 mg cost gabapentin online
amoxicillin order online no prescription: amoxicillin 500mg buy online canada – generic amoxicillin over the counter
http://amoxila.pro/# amoxicillin 500mg no prescription
neurontin 800 buying neurontin online how much is neurontin pills
buy doxycycline online uk: doxycycline hydrochloride 100mg – online doxycycline
zithromax: where can you buy zithromax – can i buy zithromax online
https://gabapentinneurontin.pro/# neurontin rx
prednisone 2 mg prednisone 5 mg tablet rx how can i get prednisone online without a prescription
buy cheap neurontin: neurontin 214 – neurontin tablets
doxycycline pills: buy doxycycline online uk – doxycycline 100 mg
https://amoxila.pro/# amoxicillin 875 125 mg tab
amoxicillin capsule 500mg price amoxicillin over the counter in canada amoxicillin 500mg capsule buy online
zithromax for sale us: can you buy zithromax over the counter in mexico – zithromax antibiotic without prescription
http://prednisoned.online/# prednisone 60 mg
neurontin 600 mg capsule brand name neurontin neurontin 800 mg price
can i purchase prednisone without a prescription: buying prednisone – buy prednisone online without a script
where to purchase doxycycline: generic for doxycycline – doxycycline hyclate 100 mg cap
https://doxycyclinea.online/# buy generic doxycycline
prednisone 2 mg prednisone 50 mg tablet cost prednisone acetate
neurontin 300mg caps: neurontin 300 mg capsule – neurontin 3
how to get zithromax: zithromax 600 mg tablets – zithromax order online uk
https://prednisoned.online/# where can i buy prednisone without a prescription
buy cheap neurontin neurontin buy from canada gabapentin 300
can you buy amoxicillin over the counter: can you purchase amoxicillin online – amoxicillin over the counter in canada
where can i buy zithromax medicine: where to get zithromax over the counter – zithromax tablets for sale
https://amoxila.pro/# amoxicillin where to get
prednisone 50 prednisone buy cheap buy prednisone canadian pharmacy
cost of neurontin: order neurontin – generic neurontin 600 mg
http://doxycyclinea.online/# doxycycline prices
can i buy zithromax over the counter: how to buy zithromax online – buy zithromax online cheap
purchase zithromax online buy zithromax 1000 mg online zithromax canadian pharmacy
zithromax 500mg price: where to get zithromax – how to get zithromax online
http://prednisoned.online/# can i buy prednisone over the counter in usa
buy neurontin 100 mg canada neurontin india neurontin 400 mg price
neurontin price south africa: generic neurontin pill – buy generic neurontin
how to order doxycycline: doxycycline order online – doxycycline medication
http://zithromaxa.store/# where can i buy zithromax medicine
where to buy amoxicillin pharmacy amoxicillin buy online canada amoxicillin 500mg capsules
amoxicillin 250 mg capsule: can you purchase amoxicillin online – order amoxicillin online uk
drug neurontin 20 mg: neurontin buy online – 300 mg neurontin
https://prednisoned.online/# buy cheap prednisone
zithromax capsules how to buy zithromax online zithromax 250 mg tablet price
where to buy amoxicillin: amoxicillin 500mg price canada – amoxicillin buy no prescription
zithromax 1000 mg online: where can i purchase zithromax online – buy zithromax without prescription online
http://zithromaxa.store/# zithromax 600 mg tablets
doxylin doxycycline 100mg capsules doxycycline hyc 100mg
buy azithromycin zithromax: zithromax antibiotic – zithromax online usa
zithromax prescription online: zithromax order online uk – buy zithromax online cheap
http://zithromaxa.store/# purchase zithromax online
zithromax 1000 mg pills zithromax 500 mg for sale zithromax buy online
drug prices prednisone: prednisone 5mg capsules – prednisone 5 mg tablet
buying prescription drugs in mexico online mexico drug stores pharmacies mexico drug stores pharmacies
п»їbest mexican online pharmacies: buying prescription drugs in mexico online – mexico drug stores pharmacies
mexican drugstore online: mexican border pharmacies shipping to usa – mexico drug stores pharmacies
https://mexicanpharmacy1st.online/# medicine in mexico pharmacies
https://mexicanpharmacy1st.com/# mexican pharmaceuticals online
mexico drug stores pharmacies mexican drugstore online mexican rx online
mexico drug stores pharmacies: mexican rx online – buying prescription drugs in mexico
purple pharmacy mexico price list: purple pharmacy mexico price list – mexican mail order pharmacies
mexico drug stores pharmacies: mexican mail order pharmacies – mexican pharmaceuticals online
https://mexicanpharmacy1st.com/# purple pharmacy mexico price list
п»їbest mexican online pharmacies п»їbest mexican online pharmacies mexican border pharmacies shipping to usa
medication from mexico pharmacy: medicine in mexico pharmacies – pharmacies in mexico that ship to usa
https://mexicanpharmacy1st.online/# mexico pharmacies prescription drugs
https://mexicanpharmacy1st.shop/# medication from mexico pharmacy
best online pharmacies in mexico mexico drug stores pharmacies mexican border pharmacies shipping to usa
best online pharmacies in mexico: best online pharmacies in mexico – mexican mail order pharmacies
https://mexicanpharmacy1st.online/# mexican online pharmacies prescription drugs
buying prescription drugs in mexico online: mexican rx online – mexico drug stores pharmacies
mexico pharmacies prescription drugs: mexican pharmaceuticals online – mexico drug stores pharmacies
https://mexicanpharmacy1st.online/# buying prescription drugs in mexico
mexican drugstore online: best online pharmacies in mexico – mexico pharmacies prescription drugs
medicine in mexico pharmacies: п»їbest mexican online pharmacies – mexican mail order pharmacies
mexican rx online buying prescription drugs in mexico mexican rx online
https://mexicanpharmacy1st.online/# mexican pharmacy
http://mexicanpharmacy1st.com/# mexican rx online
medication from mexico pharmacy: buying prescription drugs in mexico online – mexican mail order pharmacies
mexican rx online mexican pharmacy mexican online pharmacies prescription drugs
https://mexicanpharmacy1st.com/# п»їbest mexican online pharmacies
mexican rx online: mexico drug stores pharmacies – best online pharmacies in mexico
mexican border pharmacies shipping to usa: pharmacies in mexico that ship to usa – mexican pharmaceuticals online
medicine in mexico pharmacies mexican pharmacy medication from mexico pharmacy
Cytotec 200mcg price buy cytotec online buy misoprostol over the counter
http://lisinopril.club/# prinivil 20 mg tablet
clomid rx: get cheap clomid without dr prescription – cheap clomid online
http://cytotec.xyz/# cytotec buy online usa
neurontin 50mg cost neurontin 400 neurontin online
buy cheap propecia for sale: get generic propecia pill – buy propecia price
can you get generic clomid pills: how to buy clomid without a prescription – clomid without dr prescription
get propecia without dr prescription order cheap propecia without prescription buying propecia without rx
where to buy cheap clomid without rx: how can i get clomid without insurance – how can i get cheap clomid without prescription
https://propeciaf.online/# cheap propecia tablets
https://propeciaf.online/# cost propecia without dr prescription
zestril 20 mg cost lisinopril cost 40 mg zestril online
how to buy generic clomid without rx: can i purchase cheap clomid – generic clomid price
https://cytotec.xyz/# cytotec abortion pill
neurontin for sale online neurontin 400 ordering neurontin online
propecia: buy generic propecia – cost of propecia
http://lisinopril.club/# lisinopril online pharmacy
zestril no prescription: lisinopril 20 mg india – lisinopril 3.5 mg
buy cheap propecia for sale cost of propecia without a prescription get cheap propecia without insurance
lisinopril 2.5: lisinopril medication – can i buy lisinopril over the counter
http://gabapentin.club/# neurontin 30 mg
http://lisinopril.club/# prinivil drug
cheap propecia without dr prescription order propecia pills cost of propecia no prescription
Cytotec 200mcg price: buy cytotec pills – cytotec pills buy online
lisinopril 5mg tabs zestril 10mg lisinopril 20 mg tablet cost
where can i buy zestril: lisinopril rx coupon – 10 mg lisinopril tablets
Abortion pills online Cytotec 200mcg price cytotec buy online usa
https://cytotec.xyz/# buy cytotec online
https://cheapestcanada.com/# canadian drug pharmacy
https://cheapestandfast.com/# legitimate online pharmacy no prescription
п»їbest mexican online pharmacies mexican online pharmacies prescription drugs medicine in mexico pharmacies
http://cheapestandfast.com/# prescription online canada
https://cheapestmexico.com/# medication from mexico pharmacy
canadian prescription pharmacy: pharmacy coupons – canadian pharmacy coupon code
http://cheapestcanada.com/# canada pharmacy
pharmacy discount coupons 36 and 6 health online pharmacy prescription free canadian pharmacy
http://cheapestmexico.com/# mexico pharmacy
https://36and6health.com/# canadian pharmacy no prescription
http://cheapestcanada.com/# canadian pharmacy meds
п»їlegitimate online pharmacies india: pharmacy website india – indian pharmacies safe
https://cheapestcanada.com/# canadian pharmacy drugs online
https://cheapestandfast.com/# no prescription
canadian prescription drugstore review cheapest and fast buying drugs without prescription
http://cheapestindia.com/# indian pharmacy
https://cheapestmexico.shop/# purple pharmacy mexico price list
rx pharmacy no prescription: 36 and 6 pharmacy – international pharmacy no prescription
https://eufarmaciaonline.com/# п»їfarmacia online espaГ±a
Farmacie on line spedizione gratuita: farmacie online sicure – farmacia online
farmacie online sicure: top farmacia online – farmacia online
farmacia online barcelona: farmacia online madrid – farmacia online barata y fiable
Farmacia online miglior prezzo farmacia online senza ricetta farmacia online
eu apotheke ohne rezept: medikament ohne rezept notfall – europa apotheke
comprare farmaci online con ricetta: top farmacia online – acquisto farmaci con ricetta
farmacia online piГ№ conveniente Farmacia online miglior prezzo top farmacia online
https://eumedicamentenligne.com/# pharmacies en ligne certifiГ©es
farmacia online madrid: farmacia barata – farmacias direct
pharmacie en ligne pas cher: acheter mГ©dicament en ligne sans ordonnance – pharmacie en ligne france fiable
farmacias online seguras en espaГ±a: farmacia online madrid – farmacias direct
Farmacie on line spedizione gratuita Farmacia online piГ№ conveniente farmacia online
gГјnstigste online apotheke: online apotheke – п»їshop apotheke gutschein
comprare farmaci online all’estero: comprare farmaci online all’estero – acquisto farmaci con ricetta
comprare farmaci online con ricetta: farmaci senza ricetta elenco – Farmacie online sicure
gГјnstige online apotheke gГјnstige online apotheke eu apotheke ohne rezept
apotheke online: medikamente rezeptfrei – online apotheke versandkostenfrei
Farmacia online miglior prezzo: Farmacia online piГ№ conveniente – Farmacia online piГ№ conveniente
farmacia en casa online descuento farmacia online espaГ±a envГo internacional farmacias online seguras en espaГ±a
https://euapothekeohnerezept.shop/# europa apotheke
internet apotheke: apotheke online – online apotheke deutschland
ohne rezept apotheke: online apotheke versandkostenfrei – medikament ohne rezept notfall
farmacia en casa online descuento: farmacias online seguras – farmacia barata
pharmacie en ligne Pharmacie sans ordonnance trouver un mГ©dicament en pharmacie
trouver un m̩dicament en pharmacie: pharmacie en ligne france livraison belgique РAchat m̩dicament en ligne fiable
online apotheke gГјnstig: eu apotheke ohne rezept – online apotheke deutschland
ohne rezept apotheke ohne rezept apotheke online apotheke versandkostenfrei
farmacias direct: farmacias direct – farmacia online madrid
pharmacie en ligne fiable: Pharmacie Internationale en ligne – Pharmacie en ligne livraison Europe
https://eufarmacieonline.com/# farmacie online affidabili
online apotheke: apotheke online – eu apotheke ohne rezept
Farmacia online miglior prezzo farmacie online autorizzate elenco top farmacia online
farmacia online madrid: farmacia barata – farmacia online barcelona
п»їfarmacia online espaГ±a: farmacia online madrid – farmacia online 24 horas
pharmacies en ligne certifiГ©es pharmacie en ligne sans ordonnance pharmacie en ligne pas cher
farmaci senza ricetta elenco: Farmacie online sicure – farmacia online più conveniente
migliori farmacie online 2024: farmacie online autorizzate elenco – farmacia online piГ№ conveniente
pharmacie en ligne france livraison belgique: pharmacie en ligne france livraison belgique – pharmacie en ligne pas cher
pharmacie en ligne france livraison belgique: kamagra en ligne – vente de mГ©dicament en ligne
pharmacie en ligne sans ordonnance Acheter Cialis Pharmacie sans ordonnance
Pharmacie en ligne livraison Europe: pharmacie en ligne – pharmacie en ligne france livraison belgique
pharmacie en ligne france livraison internationale: levitra generique – pharmacie en ligne pas cher
pharmacie en ligne avec ordonnance: levitra en ligne – pharmacie en ligne france livraison internationale
http://levitraenligne.com/# pharmacie en ligne france fiable
п»їpharmacie en ligne france: kamagra 100mg prix – pharmacie en ligne pas cher
Pharmacie en ligne livraison Europe: cialis prix – pharmacie en ligne fiable
Pharmacie Internationale en ligne: kamagra gel – pharmacie en ligne
Pharmacie en ligne livraison Europe Pharmacies en ligne certifiees pharmacie en ligne pas cher
pharmacie en ligne avec ordonnance: Levitra 20mg prix en pharmacie – pharmacie en ligne france livraison belgique
SildГ©nafil Teva 100 mg acheter: viagra sans ordonnance – Viagra homme prix en pharmacie sans ordonnance
Hello!
This post was created with XRumer 23 StrongAI.
Good luck 🙂
Viagra sans ordonnance livraison 24h: Viagra sans ordonnance 24h – Viagra femme ou trouver
Hello.
This post was created with XRumer 23 StrongAI.
Good luck 🙂
Sildenafil teva 100 mg sans ordonnance: Viagra sans ordonnance 24h – Viagra pas cher livraison rapide france
acheter mГ©dicament en ligne sans ordonnance: pharmacie en ligne avec ordonnance – pharmacie en ligne livraison europe
Pharmacie en ligne livraison Europe: levitra en ligne – Pharmacie en ligne livraison Europe
geinoutime.com
이 모습은… 처음부터 끝까지 버려진 여자처럼.
Achat mГ©dicament en ligne fiable: trouver un mГ©dicament en pharmacie – pharmacie en ligne france livraison internationale
http://cenligne.com/# trouver un médicament en pharmacie
trouver un mГ©dicament en pharmacie: Pharmacie sans ordonnance – pharmacie en ligne france livraison internationale
pharmacie en ligne france fiable: kamagra en ligne – Achat mГ©dicament en ligne fiable
trouver un mГ©dicament en pharmacie: Acheter Cialis – pharmacie en ligne pas cher
pharmacie en ligne fiable: pharmacie en ligne – п»їpharmacie en ligne france
vente de mГ©dicament en ligne: pharmacie en ligne sans ordonnance – Pharmacie Internationale en ligne
Achat mГ©dicament en ligne fiable: kamagra livraison 24h – Pharmacie en ligne livraison Europe
geinoutime.com
Wang Jinyuan의 마음 속에서 그는 미친 듯이 계산하기 시작했습니다.
pharmacie en ligne: kamagra gel – pharmacie en ligne sans ordonnance
Viagra sans ordonnance livraison 48h: Viagra sans ordonnance 24h – Viagra gГ©nГ©rique sans ordonnance en pharmacie
Pharmacie en ligne livraison Europe: Levitra pharmacie en ligne – pharmacie en ligne livraison europe
pharmacie en ligne livraison europe: pharmacie en ligne sans ordonnance – vente de mГ©dicament en ligne
Viagra sans ordonnance livraison 24h: viagra en ligne – Viagra homme prix en pharmacie sans ordonnance
Viagra homme prix en pharmacie sans ordonnance: Viagra prix pharmacie paris – Viagra homme prix en pharmacie sans ordonnance
pharmacie en ligne france livraison internationale: Acheter Cialis – pharmacie en ligne avec ordonnance
pharmacie en ligne france livraison belgique: kamagra oral jelly – pharmacie en ligne avec ordonnance
vente de mГ©dicament en ligne: achat kamagra – Pharmacie sans ordonnance
acheter mГ©dicament en ligne sans ordonnance: kamagra gel – pharmacie en ligne fiable
Pharmacie en ligne livraison Europe: levitra generique – Pharmacie sans ordonnance
pharmacie en ligne france livraison internationale: Cialis sans ordonnance 24h – Pharmacie sans ordonnance
pharmacie en ligne avec ordonnance: pharmacie en ligne france pas cher – vente de mГ©dicament en ligne
pharmacie en ligne avec ordonnance: pharmacie en ligne sans ordonnance – Achat mГ©dicament en ligne fiable
Pharmacie sans ordonnance: kamagra gel – acheter mГ©dicament en ligne sans ordonnance
vente de mГ©dicament en ligne: acheter kamagra site fiable – pharmacie en ligne pas cher
Pharmacie en ligne livraison Europe: kamagra pas cher – Achat mГ©dicament en ligne fiable
pharmacie en ligne france livraison internationale: pharmacie en ligne sans ordonnance – Pharmacie sans ordonnance
pharmacie en ligne fiable: kamagra livraison 24h – pharmacie en ligne france livraison internationale
pharmacie en ligne fiable: Acheter Cialis 20 mg pas cher – pharmacie en ligne pas cher
pharmacie en ligne france livraison internationale: cialis prix – acheter mГ©dicament en ligne sans ordonnance
pharmacie en ligne france fiable: kamagra gel – pharmacie en ligne avec ordonnance
Viagra homme sans ordonnance belgique: SildГ©nafil Teva 100 mg acheter – SildГ©nafil 100 mg sans ordonnance
vente de mГ©dicament en ligne: Medicaments en ligne livres en 24h – pharmacie en ligne france fiable
pharmacie en ligne avec ordonnance: Cialis sans ordonnance 24h – acheter mГ©dicament en ligne sans ordonnance
Viagra pas cher livraison rapide france: Le gГ©nГ©rique de Viagra – Viagra homme sans ordonnance belgique
pharmacie en ligne france pas cher: levitra en ligne – п»їpharmacie en ligne france
pharmacie en ligne: achat kamagra – trouver un mГ©dicament en pharmacie
pharmacie en ligne fiable: Acheter Cialis 20 mg pas cher – п»їpharmacie en ligne france
Pharmacie en ligne livraison Europe: pharmacie en ligne – pharmacie en ligne pas cher
Viagra homme prix en pharmacie: viagra en ligne – Viagra sans ordonnance 24h Amazon
pharmacie en ligne: Pharmacies en ligne certifiees – pharmacie en ligne sans ordonnance
geinoutime.com
당연하지… 누가 먼저 말을 하든 좋은 결과는 절대 없을거야.
geinoutime.com
결국 그는 이 방에서 특이한 것을 발견했습니다.
geinoutime.com
고향을 떠나 싸게 산다는 말이 고향을 떠나는 것이 아니라 이것이 망명과 배급이다.
메가 슬롯 사이트
정말… 조금 부끄럽지만 아무 짓도 안 했어요.
Pin Up Azerbaycan ?Onlayn Kazino: pin-up kazino – pin-up 141 casino
https://autolux-azerbaijan.com/# Pin Up Kazino ?Onlayn
?Onlayn Kazino: Pin Up Azerbaycan ?Onlayn Kazino – pin-up kazino
pin-up360: Pin-up Giris – pin-up kazino
pin-up kazino: Pin-Up Casino – pin-up 141 casino
https://autolux-azerbaijan.com/# Pin up 306 casino
?Onlayn Kazino: Pin Up – ?Onlayn Kazino
https://autolux-azerbaijan.com/# Pin Up Azerbaycan
Pin Up: ?Onlayn Kazino – Pin Up Azerbaycan
프라그마틱 무료 슬롯
그는 자신이 이러한 책임감과 책임감을 가져야 한다고 믿습니다.
에그벳 계열
Zhu Houzhao는 잠시 생각했습니다. “어쩌면 돈을 위해 점프하는 것일 수도 있습니다.”
입플
Fang Jifan은 한 질문에 답할 수 없었습니다.
스포츠 토토 배트맨
한린학원은 지금 아주 한가하고, 아직도 주식시장에 대해 수다 떨고 있는 사람들이 있습니다.