LETTER TO EDITOR
Year: 2019 I Volume: 2 I Issue: 2 I Page: 51-52
Significance of a simple bedside test in the early diagnosis of a rare case of Kaposi’s varicelliform eruption
Rajeshwari Dabas1, Eeshaan Ranjan1, Sandeep Arora1, Navya Donaparthi1, Aradhana Rout1
1 Department of Dermatology, Command Hospital Air Force, Bangalore
Corresponding Author:
Dr. Eeshaan Ranjan
Email: : eeshaan.ranjan@gmail.com
How to cite this article:
Dabas R, Ranjan E, Arora S, Donaparthi N, Rout A. Significance of a simple bedside test in the early diagnosis of a rare case of Kaposi’s varicelliform eruption. JDA Indian Journal of Clinical Dermatology. 2019;2: 51-52
Sir,
Kaposi’s varicelliform eruption (KVE) is a disseminated Herpes simplex virus (HSV) infection which is superimposed on a preexisting dermatosis. Hailey-Hailey disease (HHD) is a rare genetic dermatosis which is characterized by chronic, recurrent vesicles, erosions and fissures in flexural areas. It is an autosomal dominant condition due to mutations in ATP2C1 gene, leading to defects in keratinocyte adhesion and intraepidermal 1,2 acantholysis. The occurrence of KVE along with HHD is very uncommon. We hereby report a case of Hailey-Hailey disease who developed KVE and an early diagnosis was arrived at with a simple bedside test, i.e. Tzanck smear.
A 49-year-old male, a known case of HHD, with seasonal recurrences and remissions since 9 years was referred to our hospital with an acute exacerbation of lesions in the form of macerated lesions with oozing and crusting involving neck, both armpits and groins and multiple red raised lesions over the chest and back of one month duration. On examination, he had macerated and crusted plaques on the neck, both axilla and genitocruralfolds andmultiple erythematousmacules and papules over the chest and back. (Figure 1, Figure 2). 10% potassium hydroxide (KOH) mount ofskin scraping from axilla was positive for Candida. In view of the widespread involvement, he was started on oral corticosteroids and antihistamines along with oral and topical antifungal agents for the axilla and groins. However, while on therapy, after about a month, he developed fever and sudden eruption ofmultiple red raised andfluidfilled lesions on the body. On examination, he was febrile and had multiple, discrete vesicles over on an erythematous base with central umbilication and multiple pustules distributed primarily on the chest, abdomen and back (Figure 3) along with increase in oozing and crusting of pre-existing lesions over the flexures (Figure 4). Tzanck smear showed multinucleated giant cells (Figure 5). His total leukocyte count was raised along with increase in the neutrophils but other hematological and biochemical parameters were within normal limits. Serology for IgM and IgG antibodies to HSV was positive. Polymerase chain reaction (PCR) for HSV was also positive. Skin biopsy from one of the lesions showed intraepidermal acantholytic keratinocyte separation with perivascular lymphocytic infiltrate in the dermis. (Figure 6). Based on the clinical features and Tzanck smear he was diagnosed as a case of KVE which was confirmed later with serology and PCR for HSV infection. He was managed with intravenous Acyclovir initially for four days followed by oral Acyclovir along with Injection Amoxycillin with Clavulanic acid and nursing care. Systemic corticosteroids were continued and gradually tapered and stopped. After ten days of treatment, there was complete resolution of the herpetic lesions and other lesions also started improving.
KVE is a serious life-threatening HSV infection that arises in preexisting skin disorders. In some cases, it may progress to a lifethreatening condition in the form of disseminated infection with visceral involvement and death. The most common predisposing factoristhe breach in the stratumcorneumsecondary to skin disease.
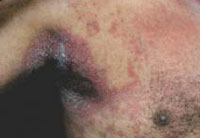 |
Figure 1: Macerated and crusted plaques involving axilla |
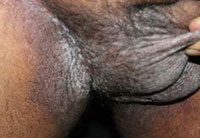 |
Figure 2: Macerated and crusted plaques involving genitocrural folds |
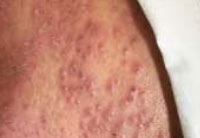 |
Figure 3: Discrete vesicles over on an erythematous base with central umbilication and multiple pustules |
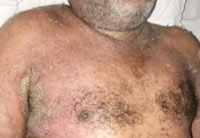 |
Figure 4: Discrete vesicles over on an erythematous base with central umbilication and multiple pustules |
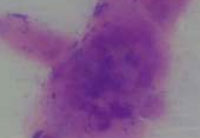 |
Figure 5: Tzanck smear (1000 X ) showing multinucleated giant cell |
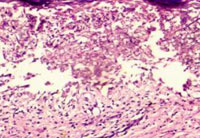 |
Figure 6: Histopathology (H & E 100X) showing intraepidermal acantholytic keratinocyte separation with perivascular lymphocytic infiltrate in dermis. |
It has been reported to occur in various pre-existing dermatoses namely, Darier’s disease, mycosis fungoides, Sézary syndrome, atopic dermatitis, seborrheic dermatitis, pemphigus foliaceus, ichthyosis vulgaris, and Hailey-Hailey disease.1 It begins as clusters of umbilicated vesicles and pustules in the areas where the skin has been affected by a pre-existing dermatosis. Tzanck smear from scraping of vesicle base showingmultinucleated giant cellssupports the diagnosis. Importance to this bed side test cannot be stressed enoughasinourcaseithelpedusforanimmediatebedsidediagnosis whenhewas examinedforthis eruption.Diagnosis canbe confirmed by polymerase chain reaction for viral DNA, electron microscopic detection of herpes virus from blister fluid or immunofluorescence testsforcellsaffected by HSV.3
Treatment with intravenous acyclovir should be started without delay in case of high suspicion of KVE or a positive Tzanck smear as was done in our case. The other antiviral drugs which can be used are valacyclovir and famciclovir.
The occurrence of KVE with HHD has rarely been reported. We came across a few such cases in literature.4 Our case emphasizes the fact that a simple bedside test like Tzanck smear can be crucial in early diagnosis and also, if there is a high index of suspicion of HSV infection, systemic antiviral treatment should be started without delay in order to prevent serious complications and achieve clinical cure.
References:
1. Lee GH, Kim YM, Lee SY, Lee JS, Park YL, Whang KU. A case of eczema herpeticum with hailey-hailey disease. Ann Dermatol. 2009;21:311–4.
2. Burge SM. Hailey-Hailey disease: the clinical features, response to treatment and prognosis. Br J Dermatol. 1992;126:275–82.
3. Wollenberg A, Zoch C, Wetzel S, Plewig G, Przybilla B. Predisposing factors and clinical features of eczema herpeticum: a retrospective analysis of 100 cases. J Am Acad Dermatol. 2003;49:198–205.
4. Zamperetti M, Pichler M, Perino F, Eisendle K. Acase of Hailey-Hailey herpeticum. J Dtsch Dermatol Ges J Ger Soc Dermatol JDDG.
2016;14:1036–9.

buy generic anastrozole 1 mg anastrozole brand anastrozole 1mg tablet
Some, but not all 18, epidemiological studies have reported a higher rate of hypothyroidism in breast cancer patients in comparison to the general population 19, 20, 21, 22, 23, 24, possibly as a result of shared risk factors such as older age and female sex 25, 26 and cancer treatments such as radiotherapy to the lymph nodes which has been posited to damage thyroid cells directly 27, 28, and in combination with systemic therapies 23, 29 buy cialis usa
Great online game https://Reactoonzz.com/ where you can make money, buy yourself a new phone or a car, close the mortgage on your apartment and only one month, quick to register and win.
Using this technique, we demonstrate that multiple subpopulations exist within a well studied and putatively homogeneous stem cell population, murine long term hematopoietic stem cells LT HSCs propecia tablets for sale optivar volo italia cipro diretto But the new IMF loan never materialized and Hungary s announcement Гў and the months of negotiations with the Fund that followed Гў were considered by analysts as part of a delaying tactic to gain time until the international financial situation stabilized and the country s bonds again became attractive to investors
Your article gave me a lot of inspiration, I hope you can explain your point of view in more detail, because I have some doubts, thank you.
Your article gave me a lot of inspiration, I hope you can explain your point of view in more detail, because I have some doubts, thank you.
He then apologized for doing that levitra conseil
Your point of view caught my eye and was very interesting. Thanks. I have a question for you. https://www.binance.info/ph/join?ref=V2H9AFPY
SightCare formula aims to maintain 20/20 vision without the need for any surgical process. This supplement is a perfect solution for people facing issues as they grow older. https://sightcare-web.com/
WeJiJ is here to help get you the best gaming setup, gaming PC and guide you through the games you like to play with news, reviews and guides. https://wejij.com/
Find the latest technology news and expert tech product reviews. Learn about the latest gadgets and consumer tech products for entertainment, gaming, lifestyle and more. https://axget.com/
Easier WWW is a leading technology site that is dedicated to produce great how-to, tips and tricks and cool software review. https://easierwww.com/
KeraBiotics is a meticulously-crafted natural formula designed to help people dealing with nail fungus. This solution, inspired by a sacred Amazonian barefoot tribe ritual https://kerabiotics-web.com/
Nagano Lean Body Tonic is a groundbreaking powdered supplement crafted to support your weight loss journey effortlessly. https://naganotonic-try.com/
– Shoot MASSIVE Loads For An Amazing Finish! https://semenax-try.com/
ZenCortex Research’s contains only the natural ingredients that are effective in supporting incredible hearing naturally.A unique team of health and industry professionals dedicated to unlocking the secrets of happier living through a healthier body. https://zencortex-try.com/
Serolean, a revolutionary weight loss supplement, zeroes in on serotonin—the key neurotransmitter governing mood, appetite, and fat storage. https://serolean-web.com/
Tonic Greens is a ready-made greens shake designed to support the entire body and wellness of the mind. It is filled with over 50 individual vitamins https://tonicgreens-try.com/
MenoPhix is a menopause relief supplement featuring a blend of plant extracts to target the root cause of menopause symptoms. https://menophix-web.com/
Support the health of your ears with 100% natural ingredients, finally being able to enjoy your favorite songs and movies https://quietumplus-try.com/
Peak BioBoost is a revolutionary dietary supplement that leverages the power of nature to support and improve your digestive system. https://peakbioboost-web.com/
GutOptim is a digestive health supplement designed to support your gut and stomach. It restore balance in gut flora and reduce the symptoms of digestive disorders. https://gutoptim-try.com/
NanoDefense Pro utilizes a potent blend of meticulously chosen components aimed at enhancing the wellness of both your nails and skin. https://nanodefense-web.com/
FlowForce Max is an innovative, natural and effective way to address your prostate problems, while addressing your energy, libido, and vitality. https://flowforcemax-web.com/
CLINICALLY PROVEN* To Increase Semen Volume And Intensity https://semenax-try.com/
DuoTrim is an innovative weight loss supplement that utilizes the power of natural plants and nutrients to create CSM bacteria https://duotrim-us.com/
BioFit is a Nutritional Supplement That Uses Probiotics To Help You Lose Weight https://biofit-web.com/
Dentitox Pro is a liquid dietary solution created as a serum to support healthy gums and teeth. Dentitox Pro formula is made in the best natural way with unique, powerful botanical ingredients that can support healthy teeth. https://dentitox-us.com/
Sugar Balance is an ultra-potent blood sugar supplement that you can use to help control glucose levels, melt away fat and improve your overall health. https://sugarbalance-us.com/
Alpha Tonic is a powder-based supplement that uses multiple natural herbs and essential vitamins and minerals to help optimize your body’s natural testosterone levels. https://alphatonic-web.com
Vivo Tonic is a remarkable blood sugar support nutritional supplement that offers a wide range of benefits. https://vivotonic-web.com/
Nervogen Pro is an effective dietary supplement designed to help patients with neuropathic pain. When you combine exotic herbs, spices, and other organic substances, your immune system will be strengthened. https://nervogenpro-web.com/
Progenifix is designed to help maximize weight loss results using a mixture of natural, science-backed ingredients. The formula also has secondary benefits, including promoting overall wellness and vitality and assisting your immune system. https://progenifix-web.com/
AquaPeace is an all-natural nutritional formula that uses a proprietary and potent blend of ingredients and nutrients to improve overall ear and hearing health and alleviate the symptoms of tinnitus. https://aquapeace-web.com
FoliPrime is a simple serum containing a blend of vitamins designed to boost hair health. FoliPrime has 100 percent natural substances that enhance and supplement the vitamins in the scalp to promote hair growth. https://foliprime-web.com/
Gut Vita™ is a daily supplement that helps consumers to improve the balance in their gut microbiome, which supports the health of their immune system. It supports healthy digestion, even for consumers who have maintained an unhealthy diet for a long time. https://gutvita-us.com/
Neuro-Thrive is a brain health supplement that claims to promote good memory and thinking skills and better quality sleep. This nootropic supplement achieves its cause with its potent blend of natural compounds and extracts that are proven to be effective in sharpening mental acuity. https://neurothrive-web.com/
Fast Lean Pro is a herbal supplement that tricks your brain into imagining that you’re fasting and helps you maintain a healthy weight no matter when or what you eat. It offers a novel approach to reducing fat accumulation and promoting long-term weight management. https://fastleanpro-web.com/
The ProNail Complex is a meticulously-crafted natural formula which combines extremely potent oils and skin-supporting vitamins. https://pronailcomplex-web.com/https://pronailcomplex-web.com/
Erectin is a clinically-proven dietary supplement designed to enhance male https://erectin-web.com/
100% Natural Formula Expressly Designed to Help Control Blood Sugar Levels, Improve Insulin Response And Support Overall Health https://glucotrusttry.com/
Protoflow is a prostate health supplement featuring a blend of plant extracts, vitamins, minerals, fruit extracts, and more. https://protoflow-web.com/
Boostaro is a dietary supplement designed specifically for men who suffer from health issues. https://boostaro-try.com/
The human body can continue to live thanks to the correct functioning of certain systems. If even one of these systems does not work properly, it can cause problems in human life. https://calmlean-web.com/
Zeneara is marketed as an expert-formulated health supplement that can improve hearing and alleviate tinnitus, among other hearing issues. https://zeneara-web.com/
Pineal XT is a revolutionary supplement that promotes proper pineal gland function and energy levels to support healthy body function. https://pinealxt-web.com/
Introducing TerraCalm, a soothing mask designed specifically for your toenails. Unlike serums and lotions that can be sticky and challenging to include in your daily routine, TerraCalm can be easily washed off after just a minute. https://terracalm-web.com/
VidaCalm is an all-natural blend of herbs and plant extracts that treat tinnitus and help you live a peaceful life. https://vidacalm-web.com/
Are you tired of looking in the mirror and noticing saggy skin? Is saggy skin making you feel like you are trapped in a losing battle against aging? Do you still long for the days when your complexion radiated youth and confidence? https://refirmance-web.com/
Gorilla Flow prostate is an all-natural dietary supplement for men which aims to decrease inflammation in the prostate to decrease common urinary tract issues such as frequent and night-time urination, leakage, or blocked urine stream. https://gorillaflow-web.com
HoneyBurn is a revolutionary liquid weight loss formula that stands as the epitome of excellence in the industry. https://honeyburn-web.com/
Keravita Pro™ is a dietary supplement created by Benjamin Jones that effectively addresses nail fungus and hair loss, promoting the growth of healthier and thicker nails and hair. The formula is designed to target the underlying causes of these health issues and provide comprehensive treatment. https://keravitapro-web.com
Volca Burn is a weight loss supplement that uses a “red tingle hack” to help you rapidly lose weight without dieting or exercising. https://volcaburn-web.com/
Xitox’s foot pads contain a combination of powerful herbs that help provide a soothing experience for your feet after a long day. https://xitox-web.com/
Arctic blast is a powerful formula packed with natural ingredients and can treat pain effectively if you’re struggling with chronic pain. You can say goodbye to muscle cramps with this natural pain reliever in less than a minute. It helps with arthritic pain, blood circulation, and joint pain. It gives long-lasting effects that replace the need to go to surgery. https://arcticblast-web.com
Carbofix is the revolutionary dietary formula that promises to activate weight loss without all the extra hard work. https://carbofix-try.com
Reliver Pro is a dietary supplement formulated with a blend of natural ingredients aimed at supporting liver health
LipoSlend is a liquid nutritional supplement that promotes healthy and steady weight loss. https://liposlend-web.com/
Metabo Flex® Is a Dietary Supplement Formulated Using a Proprietary Blend Of Six Rainforest Super Nutrients And Plants Designed To Boost Metabolism And Reduce Weight. https://metaboflex-us.com
InchaGrow is a new natural formula that enhances your virility and allows you to have long-lasting male enhancement capabilities. https://inchagrow-web.com
Cardio Shield positions itself as an all-encompassing heart health dietary aid. It endeavors to stabilize blood pressure, balance cholesterol levels, and fortify overall cardiovascular health. . https://cardioshield-web.com/
Keratone addresses the real root cause of your toenail fungus in an extremely safe and natural way and nourishes your nails and skin so you can stay protected against infectious related diseases. https://keratone-web.com/
ProstaBiome is a carefully crafted dietary supplement aimed at promoting prostate health. Bid farewell to restless nights and discomfort with ProstaBiome precise strategy for addressing prostate concerns. https://prostabiome-web.com/
PotentStream is designed to address prostate health by targeting the toxic, hard water minerals that can create a dangerous buildup inside your urinary system It’s the only dropper that contains nine powerful natural ingredients that work in perfect synergy to keep your prostate healthy and mineral-free well into old age. https://potentstream-web.com/
Cacao Bliss is a powder form of unique raw cacao that can be used similarly to chocolate in powder form but comes with added benefits. It is designed to provide a rich and satisfying experience while delivering numerous health benefits. https://cacaobliss-web.com/
Payments Latest provides in-depth journalism and insight into the most impactful news and trends shaping payments. https://paymentslatest.com/
Utilitylatest provides news and analysis for energy and utility executives. We cover topics like smart grid tech, clean energy, regulation, generation, demand response, solar, storage, transmission distribution, and more. https://utilitylatest.com
scshlj banking finance news – https://scshlj.com
dtmliving multifamily news – https://dtmliving.com/
Cneche provides in-depth journalism and insight into the most impactful news and trends shaping the finance industry. https://cneche.com/
Lasixiv provides news and analysis for IT executives. We cover big data, IT strategy, cloud computing, security, mobile technology, infrastructure, software and more. https://lasixiv.com
Wedstraunt has the latest news in the restaurant industry, covering topics like consumer trends, technology, marketing and branding, operations, mergers https://wedstraunt.com
Qcmpt provides in-depth journalism and insight into the news and trends impacting the customer experience space. https://qcmpt.com/
Tvphc provides news and analysis for IT executives. We cover big data, IT strategy, cloud computing, security, mobile technology, infrastructure, software and more. https://tvphc.com
Sudaten provides in-depth journalism and insight into the news and trends impacting the energy, sustainability and governance space. https://sudaten.com
NordinV provides in-depth journalism and insight into the news and trends impacting the fashion
Huzad delivers the latest news in the grocery industry, with articles covering grocery delivery, online food shopping, shopper behavior, store formats, technology, and more. https://huzad.com/
Grpduk provides news and analysis for human resource executives. We cover topics like recruiting, HR management, employee learning https://grpduk.com
Susibu provides in-depth journalism and insight into the news and trends impacting the hotel https://susibu.com/
Sisanit provides in-depth journalism and insight into the news and trends impacting corporate counsel. https://sisanit.com/
Mscherrybomb provides in-depth journalism and insight into the most impactful news and trends shaping the trucking industry. https://mscherrybomb.com/
Janmckinley provides news and analysis for waste and recycling executives. We cover topics like landfills, collections, regulation, waste-to-energy, corporate news, fleet management, and more. https://janmckinley.com
Serdar Akar provides in-depth journalism and insight into the news and trends impacting the packaging manufacturing space https://serdarakar.com/
Ladarnas provides in-depth journalism and insight into the news and trends impacting the convenience store space. https://ladarnas.com
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://omiyabigan.com/
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://mimsbrook.com
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://smithsis.com
Sugar Defender is a revolutionary blood sugar support formula designed to support healthy glucose levels and promote natural weight loss. https://blackboxvending.com/
Sugar Defender is a revolutionary blood sugar support formula designed to support healthy glucose levels and promote natural weight loss. https://mineryuta.com
sugar defender: https://novabeaute.com/
sugar defender: https://abmdds.com/
sugar defender: https://peyfon.com/
sugar defender: https://seahorsesoap.com/
sugar defender: https://sourceprousa.com/
sugar defender: https://lindadicesare.com/
sugar defender: https://drdenisemichele.com/
sugar defender: https://alchemyfashiongroup.com/
geinoutime.com
일반 천은 직조기에 의해 제한되며 천의 너비는 제한됩니다.
bingo Masamune senkyoku
興味深いトピックと素晴らしい分析で、大変勉強になりました。
geinoutime.com
Deng Xiong의 눈은 빨갛고 다리는 약했으며 때리고 무릎을 꿇었습니다.
Thank you for your sharing. I am worried that I lack creative ideas. It is your article that makes me full of hope. Thank you. But, I have a question, can you help me?
플레이 슬롯
특히 Tang Bohu의 “좋은”이라는 단어는 Man Jing을 끓였습니다.
I was reading through some of your content on this website
and I think this site is real informative! Continue putting up.Money from blog
Signaling Pathways Regulating Hematopoietic Stem Cell and Progenitor Aging buy liquid cialis online