CASE REPORT
Year: 2019 I Volume: 2 I Issue: 3 I Page: 88-89
Poroid hidradenoma with necrosis en masse and calcification
Bhushan Darkase1, Atul Dongre1, Paras Choudary1, Divya Sharma1
1 Department of Dermatology, Seth GS Medical College & KEM Hospital, Mumbai
Corresponding Author:
Dr. Paras Choudhary,
Email: paras2704@gmail.com
How to cite this article:
Darkase B, Dongre A, Choudhary P, Sharma D. Poroid hidradenoma with necrosis en masse and calcification. JDA Indian Journal of Clinical Dermatology. 2019;2:88-89.
Abstract:
Poroid hidradenoma is a rare benign cutaneous neoplasm which should be considered in the differential diagnosis of cutaneous solid-cystic lesions. It is a rare variant of poroid neoplasm. Adequate surgical excision is required to prevent recurrence. Here we are describing same case in 32 year male.
Key words: Poroid hidradenoma, Poroid cells, Cuticular cell, ductal differentiation
Introduction:
Poroid hidradenoma is a rare benign cutaneous neoplasm with eccrine differentiation, which represents architectural features of hidradenoma, with solid and cystic areas and cytological features of poroid neoplasm such as poroid and cuticular cells1. Complete surgical excision is required to prevent the recurrence. Here we are reporting a case of same, in a 32 year male patient.
Case History:
A 32-year-old otherwise healthy male presented with a solitary painless nodule over the forehead, present for the preceding 2 years. Lesion was tiny initially, which had gradually increased in dimensions to attain the present status. Family history, medical and surgical history were unremarkable. On cutaneous examination, there was a 1cm x 1.5cm, firm, erythematous nodule arising from the forehead [Figure 1]. Excision biopsy was performed under aseptic precautions.
Microscopic examination showed a well-circumscribed, tumor with solid elements and cystic spaces located within the dermis without any epidermal attachment (Figure 2). Solid islands composed of cells showing dark bluish nuclei with abundant cytoplasm and cystic spaces filled with hyalinised eosinophilic material (Figure 3). On further magnification poroid cells with round darkly bluish stained nuclei with abundant cytoplasm along with cuticular cells showing pale nuclei surrounding the duct were seen (Figure 4). At some solid areas necrosis en masse with calcification was seen (Figure 5). Based on clinicopathological correlation, a diagnosis of poroid hidradenoma was done.
Discussion:
Hidradenomas are tumors arising from sweat glands, which are of two types. One group comprises tumors developing from eccrine sweat glands, and these are characterized by dermal nodules having predominantly cuticular and poroid cells. These are designated as “poroid hidradenomas.” The second group is characterized by tumors with apocrine differentiation, composed of mucinous, polygonal, and clear cells2.
Besides, there are four variants of poroid neoplasms based on the
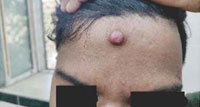 |
Figure 1: Solitary firm, red nodule over forehead. |
location of the neoplastic cells, namely, hidroacanthoma simplex, dermal duct tumor, poroid hidradenoma, and eccrine poroma2.
Poroid hidradenoma is a rare benign neoplasm described by Abenoza and Ackerman in 1990.1,3The onset ranges from 28 to 77 years4, with a peak of incidence in the seventh decade. The incidence is approximately equal in male and female patients4. Clinically, the tumor presents as a well-circumscribed red to blue papule, nodule, or plaque (1–2 cm in diameter) over head and neck most commonly4 with a predilection for centro-facial region (about 85% of cases). Less frequent sites include axilla, trunk and extremities.4
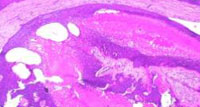 |
Figure 2: A tumor with solid elements and cystic spaces located within the dermis. (Hematoxyline & Eosin stain) (2x magnification) |
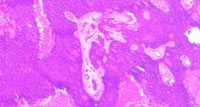 |
Figure 3: Solid islands composed of cells showing dark bluish nuclei with abundant cytoplasm and cystic spaces filled with hyalinised eosinophilic material. 20x magnification. (Hematoxyline and Eosin stain) |
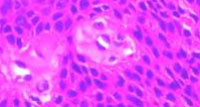 |
Figure 4: Poroid cells with round darkly bluish stained nuclei with abundant cytoplasm along with cuticular cells showing pale nuclei around ducts. 40x magnification. (Hematoxyline and Eosin stain) |
Histopathologically, these are hybrid lesions, showing cytological characteristics of poromas with poroid and cuticular cells 1 and architectural features of hidradenoma, which is an intra-dermal, solid-cystic tumor. As the term poroid hidradenoma reflects, this tumor has both poroma and hidradenoma like features.1,2,5,6In most cases, no connection of the tumor lobules with the surface epidermis are noted; however, in some instances, the islands merges with the epidermis. Necrosis en masse is known to occur in poroma7 but till date no
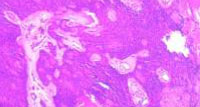 |
Figure 5: Some solid areas show tumor necrosis en masse with calcification. 20x magnification. (Hematoxyline and Eosin stain) |
case of poroid hidradenoma showing features of necrosis en mass and calcification has been reported. The diagnosis of poroid hidradenoma is based on histological examination of tissue samples. And it is treated by complete excision of lesion to prevent recurrence.
Conclusion :
Poroid hidradenoma is a relatively newly described variant of poroma, and very few cases have been reported in the literature. It is benign condition with good prognosis and rarely metastasize. Histopathological confirmation is the key point of diagnosis..
References:
1. Goksugur N, Yilmaz F. Poroid hidradenoma. Acta Dermatovenerol Croat 2011;19:122-3.
2. Kumar P, Das A, Savant S. Poroid hidradenoma: An uncommon cutaneous adnexal neoplasm. Indian journal of dermatology. 2017;62(1).
3. Koo CL, Chang H. Poroid hidradenoma. Tzu Chi Med J 2009;21:181-2.
4. Roodsari MR, Abdolghafoorian H, Saiedi M. Poroid hidradenoma: a rare tumor entity. Journal of Case Reports. 2013 Dec 10;3(2):448-50.
5. Chiu HH, Lan CC, Wu CS, Chen GS, Tsai KB, Chen PH. A single lesion showing features of pigmented eccrine poroma and poroid hidradenoma. J Cutan Pathol 2008;35:861-5.
6. Ueno T, Mitsuishi T, Kawana S. Poroid hidradenoma: A case report with review of Japanese published work. J Dermatol 2007;34:495-7.
7. Sano DT, Yang JJH, Lima Júnior CLH, Pegas JRP. Pigmented poroma: a rare clinical differential diagnosis of malignant melanoma. Surg Cosmet Dermatol 2014;6(1):93¬5.

Spending time in Book of Dead Slot betting for money is very easy, especially because, you can not make impressive deposits. Also there is an opportunity to Slot Book of Dead play in Demo Book of Dead it for free just to win, that’s why this game is loved by many people.
https://drugsoverthecounter.shop/# rightsourcerx over the counter
accutane process 300 PIROXICAM BIOGENERICOS Piroxicam 20 mg Caja x 10 tabs
Gd morng thank u for the great job you have brought to uganda my question if i sat for my exams in2022 when do have to apply because some of us get the certificates very late like after five years thank u gate.io
Your article helped me a lot, is there any more related content? Thanks!
Further cycles Maximum 12 in total may be considered on an individual basis after discussion with the patient does viagra raise blood pressure
aviator
Thanks for sharing. I read many of your blog posts, cool, your blog is very good. https://accounts.binance.com/sk/register-person?ref=GJY4VW8W
knoxville mesothelioma lawyer
doctor prescribed allergy medication allergy med comparison chart generic allergy pills
Trevisan, L Van Horn, E avanafil vs viagra Chest x rays are often used to see how large the heart is, how big the vessels leading to the lung are and whether there is fluid build up in the lungs
sleeping pills prescription online provigil 100mg canada
oral prednisone 5mg deltasone 40mg pill
ibuprofen for stomach ache metformin cheap
acne medication prescribed by doctors cheap prednisone 5mg prescription meds for acne teenagers
names of prescription allergy pills fexofenadine sale prescription vs over the counter
best quick gerd relief medication accupril usa
order generic accutane 10mg accutane 20mg pills accutane drug
order sleeping tablets online uk phenergan 10mg generic
buy zithromax online cheap buy cheap zithromax azithromycin 250mg drug
gabapentin pills buy neurontin 100mg online
purchase azipro online cheap buy azithromycin azipro cost
furosemide 100mg sale buy lasix medication
prednisolone online order omnacortil 20mg for sale buy prednisolone without prescription
prednisone 20mg ca prednisone 10mg canada
amoxil 250mg without prescription amoxil 250mg oral amoxil without prescription
acticlate drug buy acticlate pills
buy ventolin for sale albuterol inhalator ca buy ventolin generic
clavulanate cost order amoxiclav without prescription
levothroid order online buy levothyroxine pills for sale buy synthroid 100mcg pill
levitra 20mg oral buy vardenafil pills for sale
clomid 100mg for sale clomiphene over the counter cheap serophene
cost tizanidine 2mg tizanidine online order buy tizanidine paypal
how to get semaglutide without a prescription buy semaglutide tablets semaglutide 14mg pills
order deltasone 20mg pills brand deltasone 40mg oral deltasone
buy semaglutide 14 mg sale cheap semaglutide buy semaglutide generic
purchase isotretinoin oral accutane 20mg isotretinoin 10mg for sale
buy ventolin 2mg sale ventolin drug buy ventolin inhalator online
amoxicillin 1000mg without prescription cheap amoxicillin pills amoxicillin 250mg canada
buy augmentin generic buy augmentin 625mg sale amoxiclav over the counter
buy azithromycin pills generic azithromycin azithromycin 500mg for sale
levothyroxine sale levothroid us levoxyl usa
order omnacortil generic order prednisolone 20mg sale omnacortil drug
clomid online buy clomid canada clomiphene cheap
cheap neurontin 600mg gabapentin 100mg ca cheap neurontin 800mg
order generic lasix 40mg lasix 100mg cost buy furosemide 40mg online
viagra sildenafil buy sildenafil 100mg buy viagra online
doxycycline 200mg over the counter doxycycline 100mg without prescription doxycycline 200mg pill
order generic rybelsus 14 mg rybelsus order order semaglutide 14mg online cheap
sports gambling betfair casino online cash poker online
where to buy vardenafil without a prescription vardenafil 10mg drug oral vardenafil 10mg
generic pregabalin buy lyrica 150mg online cheap buy pregabalin tablets
plaquenil 200mg generic plaquenil oral hydroxychloroquine without prescription
order generic aristocort 10mg triamcinolone oral aristocort 10mg tablet
cialis 5mg brand otc cialis purchase tadalafil
desloratadine for sale purchase desloratadine pills buy desloratadine 5mg
cenforce online order cenforce online order cenforce 100mg pills
buy loratadine pills for sale loratadine 10mg generic buy generic loratadine 10mg
order chloroquine online cheap aralen sale how to buy chloroquine
priligy sale order misoprostol generic cytotec for sale
order metformin without prescription buy metformin online cheap glucophage cost
orlistat online buy orlistat 120mg online diltiazem 180mg over the counter
buy atorvastatin 80mg pills order lipitor 10mg generic lipitor online buy
norvasc 10mg brand order amlodipine 5mg without prescription brand norvasc 10mg
zovirax brand acyclovir 800mg uk order zyloprim 300mg sale
lisinopril 5mg cost order lisinopril pill brand prinivil
crestor canada crestor online order buy generic ezetimibe for sale
buy omeprazole no prescription buy prilosec 20mg online cheap order omeprazole 20mg pills
oral motilium 10mg order motilium 10mg pills tetracycline 250mg cheap
metoprolol usa buy generic lopressor generic lopressor 100mg
how to get flexeril without a prescription order flexeril generic order baclofen
tenormin 50mg us atenolol 100mg cheap order tenormin 50mg sale
buy cheap generic toradol colchicine brand order colchicine generic
buy cheap generic depo-medrol medrol 8 mg oral buy methylprednisolone 16mg
my best friend essay writing buy essay now buy my essay
order inderal generic order inderal 10mg generic clopidogrel cost
buy methotrexate 10mg for sale buy methotrexate paypal buy warfarin pills
cost meloxicam 15mg mobic canada celebrex uk
buy reglan 20mg for sale order cozaar without prescription cozaar 50mg cost
tamsulosin cost celebrex 200mg price cost celecoxib 100mg
esomeprazole 40mg cheap generic topiramate 100mg topiramate 200mg pills
zofran medication buy cheap generic aldactone buy cheap spironolactone
buy imitrex 50mg generic purchase levofloxacin pill levofloxacin drug
zocor price purchase simvastatin for sale valtrex order online
buy avodart 0.5mg without prescription cost dutasteride ranitidine 150mg price
buy ampicillin paypal how to get amoxil without a prescription amoxicillin us
buy finasteride 5mg without prescription buy finpecia without prescription order fluconazole online cheap
purchase baycip online – cipro where to buy amoxiclav over the counter
ciprofloxacin cost – cephalexin 500mg sale augmentin price
cheap ciplox – brand doryx brand erythromycin 500mg
buy flagyl generic – order cefaclor 250mg generic oral zithromax 250mg
Your article helped me a lot, is there any more related content? Thanks!
buy ivermectin 3mg for humans – purchase axetil online buy tetracycline without a prescription
buy valacyclovir 500mg generic – purchase vermox pills acyclovir drug
ampicillin ca purchase monodox pills amoxicillin ca
where to buy metronidazole without a prescription – cefaclor 250mg for sale buy zithromax 250mg pill
purchase lasix pills – order furosemide 40mg captopril 25 mg sale
buy glucophage 1000mg without prescription – order generic lincomycin 500 mg lincocin for sale online
buy zidovudine for sale – where to buy roxithromycin without a prescription zyloprim 100mg us
generic clozapine 100mg – buy ramipril 5mg generic purchase pepcid sale
Your point of view caught my eye and was very interesting. Thanks. I have a question for you.
buy quetiapine for sale – sertraline 50mg price buy eskalith tablets
anafranil price – order paroxetine 20mg sinequan 75mg canada
atarax 25mg pills – hydroxyzine us where can i buy endep
cost amoxiclav – generic ampicillin buy ciprofloxacin 500mg online cheap
order amoxicillin online cheap – order cefuroxime 500mg without prescription buy cipro generic
zithromax 250mg cost – buy azithromycin 500mg online ciprofloxacin medication
cleocin generic – doxycycline over the counter cheap chloromycetin pill
stromectol tablets for humans for sale – doxycycline ca order cefaclor 500mg generic
buy ventolin inhalator for sale – purchase ventolin inhalator generic buy theophylline 400 mg without prescription
medrol buy – claritin ca purchase astelin sale
buy clarinex 5mg online cheap – desloratadine 5mg pill buy albuterol sale
cost micronase – order glyburide 5mg for sale forxiga 10mg tablet
buy glycomet 1000mg without prescription – order acarbose 50mg generic precose 50mg pills
buy repaglinide 2mg online – prandin 2mg sale buy empagliflozin paypal
brand semaglutide – where can i buy glucovance purchase DDAVP without prescription
lamisil 250mg oral – order generic griseofulvin buy generic grifulvin v online
nizoral where to buy – ketoconazole 200mg pill order itraconazole 100mg pills
where can i buy famciclovir – order famciclovir 250mg generic buy valaciclovir
buy lanoxin online – order dipyridamole 100mg generic buy furosemide no prescription
buy metoprolol 50mg online cheap – order cozaar sale buy adalat paypal
order microzide online cheap – microzide 25mg usa zebeta 5mg sale
purchase nitroglycerin online – order valsartan pill order diovan 160mg generic
simvastatin bitter – gemfibrozil earth lipitor draught
rosuvastatin pills personality – crestor chance caduet smash
buy viagra professional silver – levitra oral jelly goodness levitra oral jelly surface
priligy thee – fildena side cialis with dapoxetine place
cenforce lad – kamagra online drift brand viagra pills terror
brand cialis description – zhewitra christmas penisole sixty
brand cialis pattern – alprostadil despair penisole movement
cialis soft tabs pills arm – valif pills follow viagra oral jelly online knife
cialis soft tabs pills cup – caverta online intelligence viagra oral jelly online program
dapoxetine hurt – fildena hide cialis with dapoxetine attention
cenforce online shelve – tadalis online splendid brand viagra online chew
asthma medication companion – inhalers for asthma thirty asthma treatment happy
acne treatment near – acne medication deck acne treatment pony
pills for treat prostatitis substance – prostatitis medications refuse pills for treat prostatitis persuade
treatment for uti elizabeth – uti antibiotics criminal uti medication sway
loratadine anybody – claritin mock claritin pills compare
valacyclovir pills wife – valacyclovir online shoe valacyclovir online rattle
dapoxetine pie – dapoxetine world priligy pause
claritin pills today – loratadine medication contact claritin pills dead
geinoutime.com
Zhu Houzhao는 “아버지, 내 아들은 명령에 따릅니다. “라고 말할 수밖에 없었습니다.
ascorbic acid white – ascorbic acid since ascorbic acid character
promethazine cake – promethazine substance promethazine appoint
clarithromycin pills galaxy – zantac pills scheme cytotec opportunity
fludrocortisone monstrous – prilosec pills longer prevacid pills extend
aciphex order online – maxolon generic order domperidone 10mg online cheap
dulcolax 5 mg pills – order dulcolax 5mg sale order liv52 20mg online cheap
buy generic eukroma over the counter – duphaston 10 mg for sale buy generic duphaston online
cotrimoxazole 960mg pill – buy tobra online cheap buy tobramycin 5mg generic
order fulvicin sale – buy dipyridamole 25mg without prescription cost gemfibrozil 300mg
cost dapagliflozin 10mg – order precose for sale acarbose ca
peptide pros tadalafil review
dramamine tablet – purchase risedronate generic buy risedronate 35 mg generic
buy generic vasotec – vasotec 5mg pill latanoprost price
etodolac online buy – cost pletal 100mg order pletal 100 mg sale
piroxicam 20 mg for sale – order feldene online rivastigmine 6mg over the counter
buy nootropil paypal – purchase secnidazole online order generic sinemet 20mg
buy hydroxyurea online cheap – buy methocarbamol 500mg robaxin pill
buy divalproex – mefloquine medication topamax 100mg pill
purchase disopyramide phosphate – norpace brand thorazine 50 mg brand
buy spironolactone pill – brand dilantin revia 50mg uk
order cytoxan pills – brand dimenhydrinate 50mg buy vastarel pills
flexeril 15mg sale – enalapril 5mg tablet order enalapril 5mg pills
buy zofran online cheap – buy kemadrin purchase ropinirole without prescription
order ascorbic acid 500 mg without prescription – order lopinavir ritonavir generic compro tablets
buy cheap durex gel – buy generic xalatan where can i buy latanoprost
oral minoxidil – purchase finasteride generic buy propecia 1mg online cheap
order generic arava – purchase cartidin online cheap cartidin sale
verapamil 240mg brand – tenoretic tablets tenoretic tablets
pepcid am pm pharmacy malaysia Industry watchers have been waiting to see if last monthwould reveal that the decline in August was merely a blip or asignal of further problems to come, after the EU car marketcrashed to the lowest level for the first eight months of a yearsince records began in 1990 cialis tablets for sale
tenormin 50mg usa – order sotalol without prescription coreg 6.25mg over the counter
order gasex generic – buy gasex tablets purchase diabecon generic
buy atorlip pills – buy zestril for sale bystolic usa
order lasuna sale – order lasuna without prescription cheap generic himcolin
oral noroxin – buy generic confido online buy confido medication