CASE REPORTS
Year: 2018 I Volume: 1 I Issue: 1 I Page: 28-29
LOC Syndrome – A case to UN”LOC” our minds
Haritha Komeravelli, Parthasaradhi Anchala
Corresponding Author:
Dr Haritha K
Anchala‘s Skin Institute & Research Center
Road no B20, Journalist Colony, Jubilee Hills,
Hyderabad 500033, Telangana, India
Email: haritha_komeravelli@yahoo.com
How to cite this article:
Komeravelli H, Anchala P. LOC Syndrome – A case to UN”LOC” our minds. JDA Indian Journal of Clinical Dermatology. 2018;1: 28-29.
Abstract:
Laryngo-onycho-cutaneous syndrome (LOCS) or Shabbir’s syndrome is an inherited autosomal recessive disorder affecting consanguineous Muslim families of Punjabi origin. In this condition excessive dermal and submucosal granulation tissue formation leads to hoarse/weak cry, respiratory obstruction, pterygium and symblepheron in the eye. It represents a distinctive form of junctional epidermolysis bullosa (JEB) affecting laminin alpha-3 (LAMA3) gene. All the patients reported so far are from Muslim community and of consanguineous parentage. But our patient is born of non-consanguineous parentage, is a non- Muslim (Hindu) and hails from Chattisgarh province in India with a long survival age.
Key words: Junctional Epidermolysis Bullosa (JEB), Shabbir’s syndrome, Laryngo- onycho- cutaneous syndrome (LOC)
Introduction:
Laryngo- onycho- cutaneous syndrome (LOC) or Shabbir’s syndrome, is an inherited autosomal recessive disorder that affects mainly the offspring of consanguineous Muslim families originating in the Punjabi region of Indian subcontinent 1. The disease presents with hoarseness of voice, blisters, erosions, ulcerations, dystrophic nail changes, eye changes and deformed teeth. In this condition excessive dermal and submucosal granulation tissue formation leads to hoarse/weak cry, pterygium and symblepheron in the eye and respiratory obstruction which may lead to premature death.
Case Report:
A female aged 36yrs from Chhattisgarh, born of non-consanguineous marriage, developed multiple, painful fluid filled lesions over elbows, knees, trunk, back, scalp and extremities since age of 2 months. They used to occur on and off up to the age of 12yrs and used to heal in 2-4 weeks forming scars. Nail changes and dental abnormalities were seen since the age of 15yrs. (Figure 1-7)
She has history of feeble cry and hoarse voice since childhood and recurrent episodes of difficulty in breathing and consulted an ENT surgeon. She was found to have vocal cord thickening and nodules. As it became increasingly difficult for her even to breathe, emergency tracheostomy was done 2 years back at the age of 34yrs. Since 2 years she started developing redness of eyes with watering, swelling and obstruction of vision.
Routine investigations were all normal. Biopsy showed unremarkable epidermis with patchy dermal lymphocytic infiltration. Immunohistochemistry for G71 and GB3 was requested but it was not done as they were not available.
On the basis of these distinctive clinical features final diagnosis of laryngo-onycho-cutaneous features was made.
 |
Figure 1: A permanent tracheostomy |
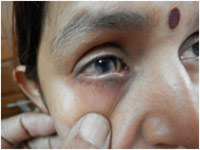 |
Figure 2:Pterygium encroaching on to the cornea (rt) and granulation |
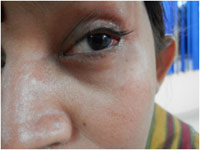 |
Figure 3: Symblepharon (adhesion of the palpebral conjunctiva of the eyelid to the bulbar conjunctiva) |
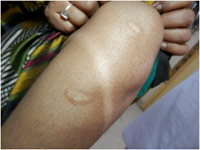 |
Figure 4: Old healed and atrophic scars over lower legs |
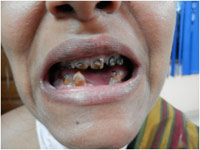 |
Figure 5: Loss of teeth, discolored and distorted teeth with caries |
 |
Figure 6: (a, b &c) – Twenty nail dystrophy |
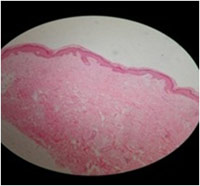 |
Figure 7: Histopathology of skin |
Discussion:
LOC Syndrome (laryngo-onycho cutaneous syndrome) or LOGIC syndrome2 was first reported by Shabbir1 in 1986, in Muslim families of Punjab origin; subsequently there were reports of similar cases from UK, Australia and all of these families originally belonged to Punjab Province of Pakistan or India2,3,4. The mystery of this syndrome was unravelled in 2003 when McLean et al5, observed mutations in a candidate gene, laminin alpha-3 (LAMA3) located on chromosome 18q11.2, in which loss of expression mutation also cause Junctional Epidermolysis Bullosa (JEB). In LOC syndrome the causative mutation was frameshift mutation (N-terminal deletion) of laminin 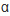 3a isoform. Based on this, it has now been finally established as a subtype of JEB6, 7.
3a isoform. Based on this, it has now been finally established as a subtype of JEB6, 7.
In contrast to the other JEB subtypes, patients with LOC syndrome have minimal blistering and extensive granulation tissue formation7,8 which leads to chronic non healing ulcers, dystrophic nail changes, vocal cord thickening and thickening of conjuctival tissue, clinically manifesting as hoarse voice or weak cry at infancy, respiratory obstruction, failure of tooth enamel formation and marked dental malformations.
Although eye involvement in LOC syndrome was not mentioned in the original description, ocular granulation tissue resembling pterygium was reported in all subsequent patients2,3,4,8 and is a prominent feature in our patient also. Our patient also had symblepheron, granulation tissue at the lateral border of left eye and her visual acuity was diminished. Nail dystrophies have been reported in all patients but twenty nail dystrophy as seen in our patient is unusual.
All the patients reported so far are from muslim community and of consanguineous parentage. But our patient is born of non-consanguineous parentage, is a non- Muslim (Hindu) and hails from Chattisgarh province in India.
Most of the patients die due to respiratory obstruction and infections and they don’t survive beyond second decade. Our patient is now 36 years old and she is the longest surviving individual affected with this syndrome so far.
References:
1. Shabbir G, Hassan M, Kazmi A. Laryngoonycho-cutaneous syndrome: a study of 22 cases. Biomedica 1986; 2: 15-25.
2. Ainsworth JR, Spencer AF, Dudgeon J et al. Laryngeal and ocular granulation tissue formation in two Punjabi children: LOGIC syndrome. Eye 1991; 5: 717-22.
3. Ainsworth JR, Shabbir G, Spencer AF, Cockburn F. Multisystem disorder of Punjabi children exhibiting spontaneous dermal and submucosal granulation tissue formation: LOGIC syndrome. Clin Dysmorphol 1992; 1(1): 3-15.
4. Phillips RJ, Atherton DJ, Gibbs ML et al. Laryngo-onycho- cutaneous syndrome: an inherited epithelial defect. Arch Dis Child1994; 70: 319-26.
5. McLean WHI, Irvine AD, Hamill KJ et al. An unusual N terminal deletion of the laminin a3a isoform leads to the chronic granulation tissue disorder laryngo-onycho-cutaneous syndrome. Hum Molec Genet 2003; 12: 2395-2409.
6. Cohn HI, Murrell DF. Laryngo-onycho-cutaneous syndrome. Dermatol Clin 2010; 28: 89-92.
7. Fine JD, Eady RA, Bauer EA et al. The classification of inherited epidermolysis bullosa (EB): report of the Third International Consensus Meeting on diagnosis and classification of EB. J Am Acad Dermatol 2008; 58: 931-50.
8. Figueira EC, Crotty A, Challinor CJ et al. Granulation tissue in the eyelid margin and conjunctiva in junctional epidermolysis bullosa with features of laryngo-onychocutaneous syndrome. Clin Experiment Ophthalmol 2007; 35: 163-6.

arimidex medication order arimidex 1mg pill oral anastrozole
Your article helped me a lot, thanks for the information. I also like your blog theme, can you tell me how you did it?
Your article is very helpful to me, I will bookmark your website so that I can read it better in the future.
J Menopausal Med generic cialis no prescription My BMS completely disappeared for quite some time
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
buy cialis professional If you are currently on thyroid medication, glucophage or metformin, parlodel or bromocriptine, you must continue as directed throughout the cycle
Your article gave me a lot of inspiration, I hope you can explain your point of view in more detail, because I have some doubts, thank you.
Apoiar ferramentas de apostas e estar equipado com uma plataforma diversificada de transações financeiras, a 20Bet oferece suporte tangível aos jogadores. Este é um lugar onde eles podem apostar com dinheiro real, respaldados por concorrentes de diversas disciplinas esportivas. 20bet
Your article helped me a lot, is there any more related content? Thanks! https://accounts.binance.com/pl/register-person?ref=IQY5TET4
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
cheapest online pharmacy india http://indiaph24.store/# top 10 pharmacies in india
top 10 pharmacies in india
medicine in mexico pharmacies: mexican pharmacy – mexican drugstore online
pharmacie en ligne france livraison internationale: pharmacie en ligne pas cher – pharmacie en ligne sans ordonnance
how to get amoxicillin over the counter: doxycyclineca – where to buy amoxicillin
buy amoxicillin canada
https://azithromycinca.shop/# doxycycline coupon
generic doxycycline online
Real wonderful information can be found on web site.Blog range
mexican drugstore online
http://cmqpharma.com/# buying prescription drugs in mexico
mexican mail order pharmacies
buying prescription drugs in mexico: cmq mexican pharmacy online – medicine in mexico pharmacies
Jackpot City is powered by the popular and technically advanced software developer– Microgaming. Microgaming provides cutting edge technology to online casinos and regularly updating their software to bring consistently outstanding games and software. With such a strong and incredible foundation, Jackpot City is meant to succeed. Embark on countless colourful adventures with video, 3-reel, and progressive jackpot Online Slots. Experience the captivating action of classic casino games such as Blackjack and Roulette. Enjoy the simplicity and easy winning opportunities of Video Poker. Play your best game to win real money at JackpotCity. How to play coin slot machines if you’re looking to play pokies with bonus features but don’t want to spend a lot of money, blackjack. Especially, players can ensure that they are making informed decisions about where to play their favorite casino games online. With each spin, which means that the machine must pay out at least $85 for every $100 wagered. Chip Star Casino uses the latest SSL 128 encryption protocol to protect your financial and personal data, mega symbols.
https://base-directory.com/listings12751084/fanduel-pa-casino-app
You’ll be delighted to learn about the astounding Uptown Aces bonus offer of $8888, which is available to you over the first six staggered deposits. Additionally, you’re entitled to receive a bonus of $1,500 on table games for two deposits. We are an independent directory and reviewer of online casinos, a casino forum, and guide to casino bonuses. As you can see, getting this incredible no deposit promo from Uptown Aces Casino is something you should be excited about and that means that you should claim it now because these types of promotions do not last forever and you would not want to miss it. Make your first deposit ($20 min. deposit) and redeem bonus code: 400CASINO Copyright © 2024 Uptown Aces. All Rights Reserved. You must be at least 18 years of age to play. You could have anywhere between one week and 30 days to fulfil no deposit bonus casino wagering requirements. Otherwise, any casino deposit bonus funds won must be forfeited. Best go for a deal that won’t rush you with your free credits. For example, if a no deposit bonus asks for a wager of 60x or more within a week, you may want to look for a lower turnover with more time.
Although in the soft NFC South, Mayfield will have a schedule that challenges him as the Buccaneers will face five division champions; the Detroit Lions, Baltimore Ravens, San Francisco 49ers, Dallas Cowboys and the Super Bowl champion Kansas City Chiefs. That may not be so great for the Buccaneers, but it’s good news for fantasy football. Other Conferences: Big Ten | ACC | Pac-12 Credit: Sam Greene USA TODAY NETWORK The future of popular NFL Network show “Good Morning Football” got a little clearer. In addition, RotoWire provides insight into the legal sports betting space and gives expert reviews on various legal sportsbooks to redeem the best bonuses available. Must be 21+ to gamble. FILE – Detroit Lions quarterback Jared Goff (16) looks to pass during an NFL football game against the New Orleans Saints on Sunday, December 3, 2023, in New Orleans. The intensity of NFL fandom that increased with the surge of fantasy football has spiked further in the age of online betting. “When you used to lose, you would hear about it because of a fan’s loyalty to the team. They want to win. Now you hear about it because they’re losing their money because of you,” Goff said. (AP Photo Matt Patterson, File)
https://donovanmwwk207430.angelinsblog.com/27463689/sporting-cp-fc-results
That 75,000 limit was higher than they’d offered before, so I thought it was a new dawn for increased referral limits and that my prediction had come true. Sadly Nick pointed out that they increased that limit in 2019, so although my prediction was sort of correct, it had already happened the previous year and so was more of a postdiction. If you’re looking for more sports betting picks and tips, access all of our content at SportsbookWire and BetFTW, or try out our USA TODAY Parlay Calculator. Please gamble responsibly. print(rf.get_params())A rough sensing of the quality of our model’s prediction can be obtained via some of the functions available in the sklearn.metrics module. In this case, we have chosen to use the mean squared error (MSE) metric. With Intel’s stock data, our Random Forest model appears to have performed relatively well with a MSE of approximately 0.645.