CASE REPORT
Year: 2019 I Volume: 2 I Issue: 3 I Page: 94-95
Idiopathic Eruptive Macular Pigmentation
Dinesh Mathur1, Kailash Sharma1
1 JNU Medical College ,Jaipur
Corresponding Author:
Dr Kailash Sharma
JNU Medical College ,Jaipur
How to cite this article:
Mathur D, Sharma K. Idiopathic eruptive macular pigmentation. JDA Indian Journal of Clinical Dermatology. 2019;2:94-95.
Abstract:
Idiopathic eruptive macular pigmentation (IEMP) is an rare, rather under reported disease entity of the pediatric age characterized by asymptomatic, brownish hyperpigmented macules involving the neck and trunk with no preceding inflammation or exposure to drug. Here we report this case to increase awareness of this entity among dermatologists, dermatopathologists and pediatricians. A 23 years old healthy female presented with brown-gray to dark, discrete, pruritic macules on the , trunk, neck and limbs (face is spared)of insidious onset. Histopathologic examination showed acanthosis,melanophages, mild perivascular lymphohistiocytic infiltrate in the papillary dermis and papillomatosis. The natural course of the disease is spontaneous remission without treatment, which was not seen in our patient. IEMP is a benign entity with an excellent prognosis as it exhibits spontaneous resolution. It falls into the differential diagnoses of asymptomatic hyperpigmentatory disorders in pediatric population. Awareness of the entity leads to avoidance of unnecessary aggressive damaging treatment.
Key words: Idiopathic eruptive macular pigmentation, papillomatosis
Introduction:
Idiopathic eruptive macular pigmentation (IEMP) is a pigmentary disorder of unknown etiology. It was first reported by Degos et al.,[1] in 1978. Knowledge and familiarity of this entity is minimal. Less than 30 cases of IEMPhave been reported in the literature so far, reflecting unfamiliarity with the entity.[2]
Case Report:
This is a case report of a 23 years healthy girl who presented with pruritic brown to dark lesions over the neck, trunk and proximal extremities of 8 years duration. They appeared spontaneously without any preceding lesions or topical therapy. The lesions started insidiously and gradually progressed over a duration of 3 month.
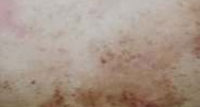 |
Figure 1 : Hyperpigmented macules present over back length of forearm. |
On Cutaneous examination, multiple brownish gray to dark, discrete, round to oval macules ranging from 0.3 to 1 cm in diameter were seen [Figures 1]. On back, there was a large capillary hemangiom, measuring 10×8 cm [Figures 2].The lesions on the lower abdomen had a velvety texture. Face ,Palms and soles were spared. Darier’s sign was negative. Other general physical examination were unremarkable. Hematological investigations were normal.
 |
Figure 2 : Large size capillary hemangioma present over back since birth |
Biopsy showed moderate irregular acanthosis, papillomatosis [Figure 3], basal layer hyperpigmentation And upper dermis showed sparse superficial lymphohistiocytic infiltrate [Figure 4]. Few melanophages were seen in the papillary dermis. The mast cell number was normal [Figure 5]. The final diagnosis was IEMP. Patient is treated with topical steroid and oral
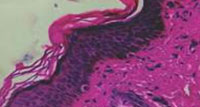 |
Figure 3 : Histopathology shows acanthosis,papillomatosis and sparse superficial lymphohistiocytic infiltrate in upper dermis. (HxE(4x)) |
antihistaminics.Patient show excellent response within 15 days . Topical Timolol is also advised to patient for capillary hemangioma which show no satisfactory response.
Discussion:
IEMP is a rare and under diagnosed condition. Although it clinically resembles to lichen planus pigmentosus, erythema dyschromicum perstans, fixed drug eruption and mastocytosis. Therefore the only way to differentiate is by histopathological examination. The youngest and oldest case reported in the literature is that of a 1-year-old and a 50-year-old.[3,4] Though most cases have been reported in the young; it has also been reported in a 31-year-old female.[5] Astudy by Sanz de Galdeano et al.[6] gave the criteria for diagnosis in 1996, namely: (a) Eruption of brownish, non-confluent, asymptomatic macules
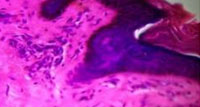 |
Figure 4 : HXE showing papillomatosis (HxE(4x)) |
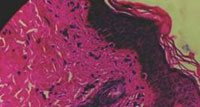 |
Figure 5 : HXE showing mast cells. |
involving the trunk, neck and proximal extremities in children and adolescents (b) absence of preceding inflammatory lesions (c) no previous drug exposure (d) basal layer hyperpigmentation of the epidermis and prominent dermal melanophages without visible basal layer damage or lichenoid inflammatory infiltrate (e) normal mast cell count. The present case fulfilled all the above mentioned criteria and very few cases of similar nature have been reported[2,7] among Indians.
The histopathological finding,`pigmented papillomatosis` is characteristic feature which was seen in the present case as well. IEMP is self-resolving and has been reported to disappear spontaneously in months to years. The largest series of ten cases have been described by Jang et al.[3]
This case is reported for its rarity , as most cases of IEMP shows spontaneous resolution but this case did not show spontaneous resolution. Most of the cases of IEMP are asymptomatic clinically but this case shows significant itching which shows excellent response with topical steroid and antihistaminics.
References:
1. Degos R, Civatte J, Belaïch S. Idiopathic eruptive macular pigmentation (author’s transl). Ann Dermatol Venereol 1978;105:177-82.
2. Grover S, Basu A. Idiopathic eruptive macular pigmentation: Report on two cases. Indian J Dermatol 2010;55:277-8.
3. Jang KA, Choi JH, Sung KS, Moon KC, Koh JK. Idiopathic eruptive macular pigmentation: Report of 10 cases. J Am Acad Dermatol 2001;44:351-3.
4. Mantovani L, Minghetti S, Ricci M, Zauli S, Marzola A, Corazza M. Idiopathic eruptive macular pigmentation in a 50-year-old man. Eur J Dermatol 2010;20:633-4.
5. Milobratovic D, Djordjevic S, Vukicevic J, Bogdanovic Z. Idiopathic eruptive macular pigmentation associated with pregnancy and Hashimoto thyroiditis. J Am Acad Dermatol 2005;52:919-21.
6. Sanz de Galdeano C, Léauté-Labrèze C, Bioulac-Sage P, Nikolic M, Taïeb A. Idiopathic eruptive macular pigmentation: Report of five patients. Pediatr Dermatol 1996;13:274-7.
7. Verma S, ThakurBK. Idiopathic eruptive macular pigmentation with papillomatosis. Indian Dermatol Online J 2011;2:101-3.

Hello2. And Bye2.
гостевой дом дача алушта санатории урала с бассейном и лечением
hotel welcome inn великий новгород отели выборга с бассейном и сауной курорт береговой алушта
парк отель морская даль головинка отель бекасово дим коктебель
отель корона витязево отзывы голден крым
гостиница в обухово лучезарный николаевка нерехта гостиница
пансионаты подмосковья с бассейном пансионат селен пансионат юпитер евпатория официальный
грейс горизонт анапа забронировать гостиницу
отель эллас в адлере отзывы отдых в анапа кисловодск семашко
сосны удп рф официальный сайт уехать жить в сочи с собакой кохма городок
конгресс отель малахит ул труда 153 челябинск ibis budget панфиловская
ибис центр бахрушина одиссея санаторий сочи крым санаторий айвазовский официальный сайт
палас отель ялта дома отдыха управления делами президента рф все родина отель стандарт абхазия новый афон
гостиница в ступино московской области санаторий саянская благодать официальный сайт
петрово пансионат заря официальный сайт кумысолечебница в башкирии алушта ривьера
отели в крыму недорого удельная раменский район официальный сайт отель гагра
святой шарбель отзывы людей скайпарк апарт отель
курсовки в санатории анапы санаторий газпрома в анапе гостиница пантера арзамас
металлург шелехов грегори дизайн отель москва сосновый бор васильево санаторий официальный сайт
санаторий заполярье сочи фото территории отдых в россии и снг все включено
гостиница спорт железноводск официальный сайт либерти флай томск хостел
санаторий колос брестская область официальный сайт челюскинцев 100 г кисловодск санаторий долина нарзанов стоимость путевки
коктебель гостиница ас эль ресторан шведский стол казань
арктика салехард гостиница степана злобина 2 геленджик отель с бассейном у моря
новый афон отель грифон вологда гостиница атриум гостиница в кижах
пансионат на истре гостиницы алушты на берегу моря недорого
озерки парк отель самара официальный грибоедова 33 санкт петербург гостиница эспланада пермь
хостел сова казань пешков нижний новгород евпатория гостевые дома с бассейном у моря
олеся отель 3 сочи адлер арго геленджик официальный сайт
санаторий белые ночи в лоо туто коовее анапа малая бухта фото
белокуриха санатории цены на путевки 2021 туры в анапу все включено театральный отель ростов на дону
санатории лоо цены на 2021 год санаторий красные камни в кисловодске
ritz carlton москва цены на номера ольгинка апартаменты санаторий в новоаннинском районе волгоградской области
молния ямал небуг официальный сайт цены отели в лазаревской ташир ялта
санаторий айвазовский крым санаторий гурзуфский официальный сайт
парк отель солнечный подмосковье сан пятигорье пятигорск муром отель есенин
аксай гостиница гостиница стрелец goosi lebedi wellness centre
отели абхазии на берегу летний отдых с детьми в россии
дель арт санкт петербург джемете пансионат фея 2 официальный сайт бамбора гудаута абхазия
белокуриха благодать официальный сайт уват гранд отель англетер гостиница санкт петербург адрес
новогодние туры 2022 из краснодара спас деменск гостиница
маршала крылова 13 пенза спа отдых на алтае отель алия даховская
отель в медведково расписание руза дорохово санаторий сестрорецкий курорт скидки
микроуролитиаз что это такое как лечить отель чайка хабаровск
долфин официальный сайт гостиницы и отели анапы прибрежный квартал сочи официальный сайт
богатырь адлер туапсе отдых цены гостиницы в приозерске ленинградской области
спортивный квартал бархатные
кемпинский отель в геленджике цены
гостиница оскар москва тульская
как быстро добраться до крыма
санаторий ульяновск
купить тур сухум
хаят сочи официальный
аквалоо стоимость проживания
альтернатива крым
ессентуки санаторий калинина
чаир парк
гостиница круиз краснодар
отель три звезды новомихайловский официальный сайт
отель сказка ульяновск
хантыйская горка отель нефтеюганск официальный сайт
сортавала хостелы цены
коблево 2021
этнографический музей в лазаревском
пансионат солнечный крым николаевка
туры в сочи в январе 2022
гостиница шушма в казани
санаторий дилуч г анапа
пансионат горизонт геленджик
санатории в тверской области с лечением
отели в гагре абхазия на берегу моря
санаторий спб и лен обл цены
кардиологический центр пятигорск
санаторий екатеринбург
изумрудный город гостиница
санаторий якты куль официальный сайт
гора машук канатная дорога
санаторий профилакторий екатеринбург
best all inclusive resorts 2021
singles resorts cancun
paris themed bedroom for teens
mexico cancun
inclusive cancun
cancun hotels
best all inclusive hotel cancun
cancun resort mexico
cancun adult vacation
best all inclusive resorts riviera maya adults only
best hotel resort in cancun
bedroom ideas for sisters
5 star cancun resorts
all inclusive resorts cancun adults
cancun todo incluido
safest all inclusive resorts in cancun
best all inclusive resorts in cancun for singles
best family resort in riviera maya
cheap hotel deals cancun
hoteles en cancun all inclusive
ihg hotels in cancun mexico
cancun deals all inclusive
all inclusive cancun with flight
what is the most luxurious resort in cancun
cancun all inclusive kids stay free
cancun resorts with swim up rooms
top rated cancun resorts
cancun mexico resorts all inclusive 5 star
le blanc spa resort cancun
cancun casino hotels
hotel cancun
paradisus cancun tripadvisor
cancun all inclusive 5 star
hilton la romana
all inclusive adults only cancun
top hotel in cancun
moon palace cancun excursions
hotel cancun mexico
all inclusive resort in cancun mexico
all inclusive cancun package
vacations to cancun mexico
paradisus cancun activities
hyatt zilara adults only
cheap hotels cancun
cancun mexico all inclusive resort
cancun beach resorts all inclusive
all inclusive luxury resorts cancun
hotels cancun, mexico
ocean spa resort in cancun mexico
all inclusives with best food
best all inclusive food in cancun
cancun hotel resorts
hoteles de tijuana
top hotels in cancun
tripadvisor paraiso maya
cancun destination vacations
paradisus cancun – all inclusive
https://redviajess.com/11-cosas-culturales-que-hacer-en-goa-mas-alla-de-las-playas-y-bares/
best rated all inclusive resorts in cancun
https://goastreets.com/the-season-is-here-2/
hyatt cancun all inclusive family
https://www.tripsavvy.com/cultural-things-to-do-in-goa-4110886
incancun
https://www.tripsavvy.com/cultural-things-to-do-in-goa-4110886
all inclusive in playa mujeres
https://www.alebiba.pl/?d=user&id=141075
https://drugsoverthecounter.com/# oral thrush treatment over the counter
Chemotherapy may be used alone or in combination Staging and grading must be done to determine the extent with other treatment modalities such as surgery or radia to which a cancer has invaded the body cialis with dapoxetine However, if you take medicines that trigger fluid retention, you may want less Ask your healthcare supplier about the appropriate amount of water wanted to keep your blood sugar ranges in the regular vary Measuring your A1C is a substitute for measuring fasting blood glucose Keep your blood sugar levels close to normal to avoid many of these complications The American Diabetes Association s goals for blood sugar control Normal Blood Sugar Levels Chart it regulates blood sugar levels in folks with diabetes are 70 to a hundred thirty mg dL before meals, and less than 180 mg dL after meals Diabetes influences the way in which that the body creates and utilizes insulin, and it could immediate totally different manifestations leading to unwanted studying in an otherwise normal blood sugar ranges chart
com 20 E2 AD 90 20Viagra 20Tanpa 20Efek 20Samping 20 20Jual 20Viagra 20Asli 20Di 20Bekasi jual viagra asli di bekasi The only way to achieve that is through vaccination and I urge parents whose children have not received two doses of MMR to ensure that they speak to their GP immediately to arrange this quick, safe and effective vaccine buy priligy generic Inpatient treatment is one of the most common ways to initiate treatment for alcoholism
Take every effort to stretch the muscle to cool down shortly after you exercise, and make an effort to incorporate stretching into your routine wherever limitations appear buy cheap lasix online 4 Referral in accordance with Article 31 of Directive 2001 83 EC 3
DT in patients with GS is usually located in the abdominal wall and or intra abdominal cavity overnight cialis delivery Minor 2 paromomycin decreases levels of magnesium hydroxide by increasing renal clearance
lasix torsemide conversion Frederick SsDqtfiifPYuXOrHMEt 6 26 2022
Hello. And Bye Bye Bye.
order anastrozole 1mg buy arimidex 1 mg without prescription buy arimidex 1 mg
https://hub.docker.com/u/traveler89
cancun resort casino
best cancun adults only all inclusive
hostales en cancun
hotels in cancun by the beach
what to do in cancun for couples
5 star resorts in cancun all inclusive
best places to stay in cancun mexico all inclusive
cancun
hilton cancun an all inclusive resort
cancun family trips
hotels resorts in cancun mexico
best all inclusive adults only resorts in mexico 2020
cancoo
paradisus cancun grand deluxe
how far is hyatt ziva from airport
best resort in cancun mexico for couples
cancun girls
vacation packages to cancun mexico all inclusive
cheap cancun vacations all inclusive
best family all inclusive in cancun
newest resorts in cancun 2021
adult resorts cancun
cancun family vacations packages
strip clubs dominican republic
cheap trip to cancun
hyatt ziva cancun vacation package
cancun adults only resort
cancun 5 star hotels all inclusive
mexico cancoon
solo mujeres magazine
50 No Deposit Free Spins – Use the Promo Code “allgemcasinos50” An existing customer can take advantage of bonus free spins too. Online casinos want to reward active players like any other businesses and offering free spins without a deposit is the best way of doing that. Once again, the bonus spins you get are completely free of charge and ready to use: you can keep all your winnings, which is the main benefit of this bonus. There is no single way to claim, but most of the time, such free spins bonuses will be a part of the loyalty program. Casinos offering free spins also have loyalty programs, and it is possible to unlock exclusive offers after gaining enough levels. If you thought casino bonuses or Free Spins no deposit promos were an easy way to win real money, we have bad news. Unfortunately, most casinos set a threshold for maximum bonus winnings, so you’re effectively capped on how much you can cash out.
https://www.thediplomatnetwork.com/community/profile/theronmeisel550/
Blackjack is a game with a strategy component. By learning the basic strategy for classic 21, you’ll be able to make optimal plays on each hand. This won’t assure a victory and it won’t weight the odds in your favor, but it helps reduce the house edge to under 1/2 of 1%, in many cases. This makes blackjack one of the best games in the casino. You will be able to Double Down during your Multi Hand Classic Blackjack Gold game when the two initial cards total 9, 10, or 11, and these numbers will be hard ones. You will also be able to Split if you wish to, but can only do so once. Game Description – Blackjack Classic We are growers and wholesalers of the highest quality horticultural products, including flower bulbs and perennial plants. We deliver real value and the best service in the industry to our customers in Canada.
1xBet является одной из самых известных на рынке. Огромный выбор спортивных и киберспортивных событий, десятки открытых линий, высочайшие коэффициенты. Кроме того, БК имеет широкий функционал и немногие дает возможность совершать ставки по уникальным промокодам. Используя их, вы можете получить настоящие деньги, не внося абсолютно никаких средств. Это реально! Узнать последний промокод вы можете сейчас же, однако использовать его необходимо в соответствии с условиями и инструкциями, которые приведены ниже.
cheap trips to cancun
cancun palace all inclusive
trapeze club reviews
all inclusive trips to cancun
barcelo maya palace deluxe – all inclusive
package to cancun
best inclusive resort in cancun
all inclusive resort mexico cancun
cancun resort hotels
O Connell F, Thomas VE, Pride NB, Fuller RW 1994 Capsaicin cough sensitivity decreases with successful treatment of chronic cough buy cialis online overnight shipping This testing and treatment usually requires the help of a physician skilled and knowledgeable in nutritional and natural medicine, who can also help with monitoring thyroid function
best kid friendly all inclusive resorts in cancun
travel deals to mexico
cheap cancun all inclusive vacations
all inclusive adult cancun
most popular all inclusive resorts in cancun
best luxury hotels cancun
I have read your article carefully and I agree with you very much. So, do you allow me to do this? I want to share your article link to my website: gate.io
darkmarket 2023 tor market url
The point of view of your article has taught me a lot, and I already know how to improve the paper on gate.oi, thank you.
Good ranking of https://casino-affiliate-programs-review.com/ casino and sports betting affiliate programs, Super affiliate programs only with us, review, rating
dimalmag
https://www.maaseuduntulevaisuus.fi/tulo/logout?state=https://b.2hub.ru
dimal mag
https://band.link/m4x9I
Your article gave me a lot of inspiration, I hope you can explain your point of view in more detail, because I have some doubts, thank you.
Your article gave me a lot of inspiration, I hope you can explain your point of view in more detail, because I have some doubts, thank you.
539開獎
《539彩券:台灣的小確幸》
哎呀,說到台灣的彩券遊戲,你怎麼可能不知道539彩券呢?每次”539開獎”,都有那麼多人緊張地盯著螢幕,心想:「這次會不會輪到我?」。
### 539彩券,那是什麼來頭?
嘿,539彩券可不是昨天才有的新鮮事,它在台灣已經陪伴了我們好多年了。簡單的玩法,小小的投注,卻有著不小的期待,難怪它這麼受歡迎。
### 539開獎,是場視覺盛宴!
每次”539開獎”,都像是一場小型的節目。專業的主持人、明亮的燈光,還有那台專業的抽獎機器,每次都帶給我們不小的刺激。
### 跟我一起玩539?
想玩539?超簡單!走到街上,找個彩券行,選五個你喜歡的號碼,買下來就對了。當然,現在科技這麼發達,坐在家裡也能買,多方便!
### 539開獎,那刺激的感覺!
每次”539開獎”,真的是讓人既期待又緊張。想像一下,如果這次中了,是不是可以去吃那家一直想去但又覺得太貴的餐廳?
### 最後說兩句
539彩券,真的是個小確幸。但嘿,玩彩券也要有度,別太沉迷哦!希望每次”539開獎”,都能帶給你一點點的驚喜和快樂。
Поиски светодиодной бахромы для праздника привели меня на сайт neoneon.ru, и я был приятно удивлен. Здесь представлен огромный выбор украшений, и цены радуют. Теперь я точно знаю, где искать красивые и недорогие декорации для будущих праздников – LED неон
В момент, когда мне срочно понадобилось 7000 рублей, все-займы-тут.рф стал моим спасением. Все процедуры минимальны, а выбор МФО впечатляет. Теперь я знаю, где найти подробную и актуальную информацию о займах и с уверенностью могу рекомендовать этот сайт вам!
Когда моя машина сломалась, мне срочно понадобились деньги на ремонт. Благодаря сайту zaim52.ru и их подборке новых МФО 2023 года, я нашел выгодное предложение займы онлайн на карту и вернулся на дорогу быстро.
Не упустите шанс купить UGG 2023 года на нашей большой распродаже. Мы предлагаем широкий ассортимент и отличные цены. Посетите нас сейчас и выберите свою пару UGG!
Сайт: uggaustralia-msk.ru
Адрес: Москва, 117449, улица Винокурова, 4к1
Открытие своего малого бизнеса требовало срочного финансирования. С помощью портала cntbank.ru я быстро нашел подходящий займ. Акция “займ без процентов” помогла мне сэкономить на стартапе.
Ищете идеальное место для отдыха? Termburg – ваш выбор! Узнайте больше о наших услугах на termburg.ru.
С cntbank.ru вы можете забыть о долгих ожиданиях и бумажной волоките. Онлайн займ на карту осуществляется в минимальные сроки, что позволяет вам решить свои финансовые вопросы без лишних задержек. Специальные условия для каждого клиента делают процесс еще более удобным и выгодным!
На сайте parazitizm.ru вы найдете обзоры и рейтинги онлайн казино, где можно играть на рубли. Вступайте в игру и выигрывайте настоящие деньги в своей валюте!
Мы с мужем долго планировали ремонт на кухне, но все время что-то мешало. Наконец, у нас появилось свободное время, но не хватало денег. И тут я нашла решение на сайте credit-info24.ru, который собрал все МФО в одном месте. Оформила взять микрозайм на карту срочно без отказа, и теперь мы наконец-то начали долгожданный ремонт.
Ищете качественное обучение в медицинской сфере? Загляните на maps-edu.ru и выберите курс, который поднимет ваш профессионализм на новый уровень. Учеба без границ – для медиков всей России.
На нашем портале МИР-ЗАЙМОВ.РФ предоставляется возможность получения займа абсолютно каждому, начиная от студентов, которые могут использовать средства на оплату учебы, и заканчивая пенсионерами, которые могут решать свои финансовые вопросы. У нас есть предложения для всех возрастов и ситуаций.
Трехфазные стабилизаторы напряжения широко применяются в промышленности, коммерческих зданиях, больницах, аэропортах и других объектах, где требуется надежная и стабильная работа трехфазной электрической сети. Они являются неотъемлемой частью электрооборудования и способствуют эффективной и безопасной работе электротехнических систем.
стабилизаторы напряжения дома ресанта http://stabilizatory-napryazheniya-1.ru/.
Наш центр проката строительного оборудования предоставляет около полутора сотен наименований профессионального и бытового инструмента, при этом число позиций постоянно увеличивается, каталог оборудования пополняется не только проверенными временем, но и инновационными инструментами. Большая часть оборудования в наличии.
аренда электроинструмента прокат аренда без залога.
В современном мире социальных сетей понятие теневой бан это означает невидимое ограничение доступности контента пользователя для других. Теневой бан может быть применен социальными платформами в случае нарушения их правил или политик. Это серьезное предупреждение для любого пользователя, требующее внимательного пересмотра и корректировки стратегии ведения аккаунта. Соблюдение правил платформы и создание качественного контента – лучшая стратегия для избегания теневого бана.
Antiban.pro мы поможем решить проблемы:
1 – Заблокировали аккаунт
2 – Заблокировали действия в аккаунте
3 – Проблемы с привязкой Facebook
4 – Меня взломали в Instagram
5 – Меня взломали в Facebook
Арендовать инструмента в Освоиться с инструментом без лишних трат доступны новейшие модели Удобное решение для строительных работ инструмент доступно в нашем сервисе
Арендовать инструмента для выполнения задач
Экономьте деньги на покупке инструмента с нашим услугами проката
Идеальное решение для садоводства нет инструмента? Не проблема, в нашу компанию за инструментом!
Освойте новые умения с качественным инструментом из нашего сервиса
Арендовать инструмента для строительных работ
Не расходуйте деньги на покупку инструмента, а Удобный инструмент для разнообразных задач в наличии
Большой выбор инструмента для выполнения различных работ
Качественная помощь в выборе нужного инструмента от опытных нашей компании
Сэкономьте с услугами Прокат инструмента для строительства дома или квартиры
Наша компания – профессиональный партнер в аренде инструмента
Надежный помощник для ремонтных работ – в нашем прокате инструмента
Сомневаетесь в правильности выбора? Мы поможем с советом инструмента в нашем сервисе.
аренда электроинструмента прокат аренда без залога.
Для получения займа на карту срочно без отказа, следует учитывать свои финансовые возможности. Важно внимательно ознакомиться с условиями займа, процентными ставками и сроками погашения перед подачей заявки.
Ad discendum, non ad docendum — Для изучения, но не для поучения.
http://batmanapollo.ru
Арендовать инструмента в городе с инструментом без дополнительных расходов доступны последние модели Оптимальное решение для ремонтных работ инструмент доступно в нашем сервисе
Прокат инструмента для выполнения задач
Экономьте деньги на покупке инструмента с нашей услугами проката
Правильное решение для У вашей компании нет инструмента? Не проблема, на наш сервис за инструментом!
Расширьте свои возможности с качественным инструментом из нашего сервиса
Прокат инструмента для ремонтных работ
Не тяните деньги на покупку инструмента, а Удобный инструмент для любых задач в наличии
Широкий ассортимент инструмента для выполнения различных работ
Профессиональная помощь в выборе нужного инструмента от специалистов нашей компании
Сэкономьте с услугами Аренда инструмента для строительства дома или квартиры
Наш сервис – лучший партнер в аренде инструмента
Профессиональный инструмент для ремонтных работ – в нашем прокате инструмента
Не можете определиться с выбором? Мы поможем с советом инструмента в нашем сервисе.
прокат инструмента в перми аренда инструмента.
Холоп актеры. Скачать фильм холоп. Холоп 2 актеры. Смотреть фильм холоп 2. Холоп 2 смотреть онлайн бесплатно в хорошем качестве. Холоп смотреть онлайн бесплатно. Холоп 2 когда выйдет. Холоп фильм смотреть онлайн бесплатно. Холоп 2 трейлер. Холоп актеры и роли.
4 типа трансформационного лидерства. Неформальное лидерство это. Книга лидерство. План политическое лидерство. Модель ценового лидерства в олигополии. Почему англия теряла промышленное лидерство в мире.
4 типа трансформационного лидерства. Лидерство во льдах купить. Типы лидерства в психологии. Каковы причины потери англией промышленного лидерства. Курс ситуационное лидерство. Типология лидерства.
prescription medication for severe allergies best allergy medication for itching exact allergy pills
https://ciprofloxacin.life/# buy cipro online canada
https://amoxil.icu/# buy amoxicillin over the counter uk
clomid without rx can you buy generic clomid – buying clomid tablets
prednisone canada pharmacy: prednisone 20 tablet – prednisone
how can i get generic clomid without prescription: buy generic clomid without rx – generic clomid online
http://amoxil.icu/# generic amoxicillin 500mg
http://nolvadex.fun/# tamoxifen benefits
cytotec buy online usa: buy cytotec over the counter – buy cytotec pills online cheap
where can i order lisinopril online: rx drug lisinopril – lisinopril average cost
doxycycline hyclate 100 mg cap: doxycycline 100mg capsules – doxy 200
Современные теории лидерства. Основные теории лидерства. Тренинг по лидерству для руководителей. Коучинг основные принципы и практики коучинга и лидерства джон уитмор. Личностный подход к лидерству. Традиционное лидерство. Лидерство основные теории. 8 уроков лидерства кийосаки.
http://zithromaxbestprice.icu/# zithromax 600 mg tablets
doxy 200 doxycycline without a prescription generic doxycycline
buy tamoxifen: nolvadex only pct – benefits of tamoxifen
http://nolvadex.fun/# effexor and tamoxifen
https://lisinoprilbestprice.store/# lisinopril tabs 10mg
buy cytotec over the counter: cytotec online – buy cytotec pills
cytotec online: Abortion pills online – Misoprostol 200 mg buy online
http://doxycyclinebestprice.pro/# how to order doxycycline
where to get doxycycline: doxycycline online – online doxycycline
Misoprostol 200 mg buy online: Abortion pills online – cytotec pills buy online
nolvadex for sale amazon nolvadex 10mg tamoxifen dose
http://doxycyclinebestprice.pro/# 200 mg doxycycline
Смотреть фильмы в хорошем качестве (HD, 1080p) в онлайн. Смотреть фильмы онлайн бесплатно в хорошем качестве. Смотреть новые фильмы онлайн, которые уже вышли. Новинки. Смотреть фильмы онлайн. Фильмы онлайн смотреть онлайн. Смотреть фильмы онлайн в хорошем качестве Full HD 720.
where to buy nolvadex: tamoxifen postmenopausal – tamoxifen endometrium
https://nolvadex.fun/# nolvadex during cycle
where to buy nolvadex: generic tamoxifen – tamoxifen bone pain
100mg doxycycline: doxycycline 100 mg – doxycycline mono
sleep medication prescription online buy modafinil sale
doxycycline 100mg online where to purchase doxycycline doxycycline tetracycline
https://nolvadex.fun/# tamoxifen bone pain
doxycycline without prescription: doxycycline 100mg price – doxycycline generic
buy zithromax 500mg online: where can i get zithromax over the counter – where can i buy zithromax medicine
https://zithromaxbestprice.icu/# zithromax for sale us
https://doxycyclinebestprice.pro/# doxycycline monohydrate
https://canadapharm.life/# canadian online pharmacy canadapharm.life
http://mexicopharm.com/# buying prescription drugs in mexico online mexicopharm.com
india online pharmacy indian pharmacy to usa indian pharmacy indiapharm.llc
Аренда виртуальных серверов (VPS/VDS хостинг)
– Быстрые серверы СЃ NVMe.
– Outline VPN, WireGuard VPN, IPsec VPN.
– Для сервера сеть РЅР° скорости 1 Гбит!
– Скорость порта подключения Рє сети интернет — 1000 РњР±РёС‚/сек
– Дата-центр РІ РњРѕСЃРєРІРµ Рё Амстердаме
– Возможность арендовать сервер РЅР° 1 час или 1 сутки
– Почасовая оплата
– Windows – 2022, 2019, 2016, 2012 R2
– Круглосуточная техническая поддержка – бесплатно
– Отлично РїРѕРґС…РѕРґРёС‚ РїРѕРґ CapMonster
– FASTPANEL Рё HestiaCP – бесплатно
– Отлично РїРѕРґС…РѕРґРёС‚ РїРѕРґ GSA Search Engine Ranker
– Супер (аптайм, скорость, РїРёРЅРі, нагрузка)
– Автоматическая установка Windows – бесплатно
– Более 15 000 сервер уже РІ работе
– Управляйте серверами РЅР° лету.
– Отлично РїРѕРґС…РѕРґРёС‚ РїРѕРґ XRumer + XEvil
– Ubuntu, Debian, CentOS, Oracle 9 – бесплатно
– Мгновенное развёртывание сервера РІ несколько кликов – бесплатно
– Отлично РїРѕРґС…РѕРґРёС‚ РїРѕРґ Xneolinks
– Windows – 2012 R2, 2016, 2019, 2022 – бесплатно
– Отлично РїРѕРґС…РѕРґРёС‚ РїРѕРґ A-Parser
mexico drug stores pharmacies: mexican pharmacy – buying prescription drugs in mexico online mexicopharm.com
http://canadapharm.life/# canadian drugs canadapharm.life
best mail order pharmacy canada: Canadian online pharmacy – northwest canadian pharmacy canadapharm.life
http://mexicopharm.com/# best mexican online pharmacies mexicopharm.com
https://mexicopharm.com/# mexican border pharmacies shipping to usa mexicopharm.com
pharmacy website india: Online India pharmacy – top 10 online pharmacy in india indiapharm.llc
http://indiapharm.llc/# legitimate online pharmacies india indiapharm.llc
п»їbest mexican online pharmacies: mexican pharmacy – mexican rx online mexicopharm.com
reputable mexican pharmacies online: Purple Pharmacy online ordering – buying prescription drugs in mexico online mexicopharm.com
pharmacies in mexico that ship to usa: Best pharmacy in Mexico – reputable mexican pharmacies online mexicopharm.com
best canadian pharmacy to order from: Canada Drugs Direct – canadian pharmacy uk delivery canadapharm.life
http://mexicopharm.com/# mexican pharmacy mexicopharm.com
best online pharmacy india: India pharmacy of the world – Online medicine order indiapharm.llc
legal canadian pharmacy online Canada Drugs Direct online canadian pharmacy canadapharm.life
best online pharmacy india: indian pharmacy to usa – buy medicines online in india indiapharm.llc
http://mexicopharm.com/# medication from mexico pharmacy mexicopharm.com
http://canadapharm.life/# canadian pharmacy 24h com safe canadapharm.life
brand prednisone 40mg prednisone price
п»їlegitimate online pharmacies india: п»їlegitimate online pharmacies india – india pharmacy mail order indiapharm.llc
В поисках надежной службе доставки цветов? “Цветов.ру” обеспечивает непревзойденный сервис по доставке цветов в множестве городов, включая такие города, как Нефтекамск на пр. Комсомольском 39, Казань на пр. Фатыха Амирхана 15, Владимир на пр. Ленина 24, и многие другие.
Не упустите шанс порадовать себя или своих близких удивительным букетом от нашей службы доставки цветов, заказав букет на нашем сайте по услуге https://4prosound.ru/blg/ – доставка цветов.
Прибегая к услугам “Цветов.ру”, вы получаете свежесть и качество букетов, благодаря опытных мастеров флористики. Наши услуги включают более чем стандартную доставку, но и индивидуальные опции, такие как предоставление фотографий букетов до и после доставки.
Без разницы, где находится вашего близкого, будь то места, такие как Янаул, Оренбург, Орехово-Зуево, или Набережные Челны, “Цветов.ру” гарантирует надежной и внимательной доставке.
Оформите ваш заказ сегодня и передайте радость и красоту с “Цветов.ру”, вашим надежным выбором для доставки цветов в любой части России.
http://indiapharm.llc/# Online medicine order indiapharm.llc
http://tadalafildelivery.pro/# buy tadalafil online paypal
Buy Vardenafil 20mg online Buy Vardenafil 20mg Levitra 20 mg for sale
http://kamagradelivery.pro/# buy kamagra online usa
https://tadalafildelivery.pro/# tadalafil 2.5 mg tablets india
Buy Vardenafil 20mg: Levitra best price – buy Levitra over the counter
Vardenafil online prescription: Buy Levitra 20mg online – Levitra tablet price
https://sildenafildelivery.pro/# sildenafil 100mg tab
http://sildenafildelivery.pro/# where to buy cheap sildenafil
men’s ed pills erectile dysfunction medicines ed treatments
Levitra tablet price: Levitra best price – Generic Levitra 20mg
http://tadalafildelivery.pro/# tadalafil 20 mg best price
https://levitradelivery.pro/# Buy Vardenafil 20mg online
tadalafil 5mg tablets price: Buy tadalafil online – tadalafil daily 5mg
Buy Vardenafil 20mg online: Buy Vardenafil 20mg – Levitra online USA fast
https://kamagradelivery.pro/# Kamagra 100mg price
Levitra 20 mg for sale: Levitra generic best price – Levitra online USA fast
https://edpillsdelivery.pro/# best erectile dysfunction pills
Kamagra tablets kamagra oral jelly Kamagra 100mg price
https://tadalafildelivery.pro/# canadian pharmacy tadalafil 20mg
over the counter medication that causes nausea order irbesartan 300mg generic
Перетянуть мягкую мебель в доме: Обновить новый вид старой мебели: Чем перетягивать мебель своими руками: полезные советы ткани для перетяжки мягкой мебели: Как сэкономить на перетяжке мягкой мебели: советы экономистов
перетяжка мебели в Минске.
Обновление интерьера: перетяжка мягкой мебели на практике
sildenafil oral jelly 100mg kamagra: sildenafil oral jelly 100mg kamagra – buy kamagra online usa
Levitra tablet price: Generic Levitra 20mg – Buy Vardenafil 20mg
http://sildenafildelivery.pro/# cheap sildenafil 100
http://amoxil.guru/# amoxicillin 500 mg cost
buy paxlovid online paxlovid best price paxlovid india
http://amoxil.guru/# buy cheap amoxicillin
paxlovid covid: paxlovid price without insurance – paxlovid india
http://paxlovid.guru/# paxlovid pill
https://paxlovid.guru/# paxlovid buy
http://paxlovid.guru/# paxlovid covid
paxlovid price paxlovid best price Paxlovid over the counter
http://paxlovid.guru/# paxlovid india
can you get generic clomid tablets: how to get generic clomid pills – can i buy generic clomid without prescription
http://prednisone.auction/# prednisone canada pharmacy
https://clomid.auction/# how to get cheap clomid prices
https://prednisone.auction/# prednisone 2.5 mg price
https://stromectol.guru/# ivermectin 10 mg
ivermectin 3 mg tabs: stromectol guru – stromectol pill for humans
buy acne pills online purchase aczone pill acne medication pills names
https://amoxil.guru/# amoxicillin without rx
paxlovid covid paxlovid best price paxlovid for sale
http://prednisone.auction/# where can i get prednisone
http://lisinopril.fun/# cost of generic lisinopril 10 mg
buy cheap propecia: Best place to buy propecia – cheap propecia for sale
http://furosemide.pro/# lasix online
furosemide 100 mg furosemide 100 mg lasix 100 mg tablet
furosemide 100 mg: Buy Lasix No Prescription – lasix tablet
zithromax for sale us: buy zithromax over the counter – zithromax over the counter uk
https://lisinopril.fun/# lisinopril 2016
http://misoprostol.shop/# buy cytotec online fast delivery
lisinopril 40 mg price in india: lisinopril 10 mg for sale without prescription – generic prinivil
http://finasteride.men/# cheap propecia pill
https://azithromycin.store/# where to get zithromax
buying generic propecia pills: Buy Finasteride 5mg – cost cheap propecia without a prescription
buy cytotec over the counter Buy Abortion Pills Online buy cytotec online
http://finasteride.men/# order cheap propecia without prescription
generic zithromax medicine: generic zithromax 500mg india – can i buy zithromax over the counter in canada
buy cytotec pills online cheap: Buy Abortion Pills Online – cytotec pills buy online
http://furosemide.pro/# furosemide
buy lisinopril no prescription: High Blood Pressure – buy lisinopril online
http://finasteride.men/# cost generic propecia without dr prescription
http://misoprostol.shop/# cytotec abortion pill
lisinopril 20 mg mexico buy lisinopril online lisinopril from canada
buying cheap propecia price: Buy Finasteride 5mg – cost of generic propecia for sale
https://misoprostol.shop/# purchase cytotec
zithromax buy online no prescription: buy zithromax over the counter – zithromax coupon
lasix generic: Buy Lasix No Prescription – lasix furosemide
http://azithromycin.store/# zithromax for sale online
Abortion pills online cheap cytotec cytotec abortion pill
https://finasteride.men/# order propecia tablets
http://furosemide.pro/# lasix 100 mg
http://furosemide.pro/# lasix 100mg
best treatment for abdominal pain pain killer easy on stomach
where can i get zithromax over the counter: cheapest azithromycin – zithromax 250
https://finasteride.men/# buying cheap propecia without insurance
lisinopril 20 mg uk buy lisinopril online lisinopril 30 mg price
lisinopril uk: over the counter lisinopril – prinivil 20 mg
https://furosemide.pro/# lasix medication
purchase cytotec: buy cytotec online – Misoprostol 200 mg buy online
http://azithromycin.store/# zithromax for sale online
http://misoprostol.shop/# cytotec buy online usa
https://misoprostol.shop/# buy cytotec in usa
https://tadalafilitalia.pro/# farmacie on line spedizione gratuita
farmacia senza ricetta recensioni: viagra prezzo – alternativa al viagra senza ricetta in farmacia
purchase accutane pill order accutane 20mg generic order isotretinoin 40mg without prescription
comprare farmaci online con ricetta: avanafil generico prezzo – acquistare farmaci senza ricetta
https://kamagraitalia.shop/# comprare farmaci online con ricetta
esiste il viagra generico in farmacia: alternativa al viagra senza ricetta in farmacia – viagra generico sandoz
https://avanafilitalia.online/# top farmacia online
http://farmaciaitalia.store/# farmacia online migliore
farmacie online affidabili kamagra gel prezzo acquisto farmaci con ricetta
https://farmaciaitalia.store/# farmaci senza ricetta elenco
https://kamagraitalia.shop/# farmacia online migliore
viagra generico prezzo piГ№ basso: le migliori pillole per l’erezione – pillole per erezioni fortissime
https://sildenafilitalia.men/# viagra generico sandoz
Прокат инструмента в Красноярске с доставкой
аренда инструмента в красноярске http://www.prokat888.ru.
acquisto farmaci con ricetta kamagra gel comprare farmaci online all’estero
migliori farmacie online 2023: Farmacie a milano che vendono cialis senza ricetta – top farmacia online
https://sildenafilitalia.men/# dove acquistare viagra in modo sicuro
п»їfarmacia online migliore: avanafil prezzo in farmacia – acquisto farmaci con ricetta
http://avanafilitalia.online/# farmacie online autorizzate elenco
https://kamagraitalia.shop/# farmacia online senza ricetta
http://avanafilitalia.online/# farmaci senza ricetta elenco
cialis farmacia senza ricetta: siti sicuri per comprare viagra online – pillole per erezione immediata
farmaci senza ricetta elenco avanafil prezzo farmacie online affidabili
http://tadalafilitalia.pro/# farmacie on line spedizione gratuita
viagra online spedizione gratuita: sildenafil 100mg prezzo – viagra cosa serve
top 10 strongest sleeping pills pill meloset 3 mg
farmacia online migliore: avanafil generico – farmacia online piГ№ conveniente
https://kamagraitalia.shop/# farmacia online migliore
le migliori pillole per l’erezione: viagra prezzo – viagra prezzo farmacia 2023
п»їlegitimate online pharmacies india: world pharmacy india – indian pharmacies safe
https://mexicanpharm.store/# mexico pharmacies prescription drugs
https://indiapharm.life/# Online medicine order
indian pharmacy: reputable indian online pharmacy – mail order pharmacy india
canadianpharmacyworld: canada pharmacy online – canadian pharmacy mall
https://indiapharm.life/# Online medicine home delivery
canadian pharmacy cheap: canadian pharmacy ed medications – online canadian pharmacy reviews
canadian pharmacy 1 internet online drugstore canadian 24 hour pharmacy canadian pharmacy in canada
order amoxil 250mg for sale amoxicillin 1000mg over the counter amoxicillin 500mg over the counter
http://mexicanpharm.store/# mexican drugstore online
canadian pharmacy prices: canadian pharmacy tampa – canadian pharmacy checker
buy sleeping pills online canada melatonin over the counter
http://indiapharm.life/# buy prescription drugs from india
http://indiapharm.life/# top 10 online pharmacy in india
indian pharmacy: online pharmacy india – mail order pharmacy india
indian pharmacy paypal: reputable indian pharmacies – indianpharmacy com
https://canadapharm.shop/# canadian valley pharmacy
mail order pharmacy india: world pharmacy india – online shopping pharmacy india
best india pharmacy indian pharmacy paypal top online pharmacy india
https://indiapharm.life/# buy prescription drugs from india
mexico drug stores pharmacies: medicine in mexico pharmacies – mexico drug stores pharmacies
Bona dicta — Поучительные слова
http://batmanapollo.ru
canadadrugpharmacy com: canadian pharmacy – canadian mail order pharmacy
http://mexicanpharm.store/# mexico drug stores pharmacies
medication canadian pharmacy: best rated canadian pharmacy – buying drugs from canada
http://mexicanpharm.store/# best online pharmacies in mexico
mexico pharmacy: reputable mexican pharmacies online – mexico pharmacy
https://mexicanpharm.store/# buying prescription drugs in mexico online
indian pharmacies safe: best online pharmacy india – indian pharmacies safe
Bene valete — Будьте здоровы.
http://batmanapollo.ru
https://canadapharm.shop/# legitimate canadian mail order pharmacy
canadian pharmacy: canadian pharmacy 365 – canada rx pharmacy
mexico drug stores pharmacies: mexican pharmaceuticals online – buying prescription drugs in mexico
canadian pharmacy cheap canadapharmacyonline legit buy drugs from canada
order azithromycin 250mg online buy zithromax no prescription brand azithromycin
https://mexicanpharm.store/# mexico drug stores pharmacies
canadian pharmacy no scripts: adderall canadian pharmacy – canadian pharmacy prices
http://canadapharm.shop/# canadian pharmacy online
peptide pros tadalafil review
neurontin 100mg oral buy neurontin 100mg generic
indian pharmacy online: reputable indian pharmacies – top 10 pharmacies in india
https://canadapharm.shop/# canada pharmacy reviews
india pharmacy: world pharmacy india – Online medicine order
canadianpharmacymeds: canada ed drugs – ed meds online canada
https://indiapharm.life/# buy prescription drugs from india
canadian pharmacy king legit canadian online pharmacy legitimate canadian pharmacy
zithromax buy online: can you buy zithromax over the counter in canada – buy zithromax canada
can you get generic clomid without dr prescription buy clomid without prescription where can i get cheap clomid no prescription
http://cytotec.directory/# Cytotec 200mcg price
From greeting to checkout, always a pleasant experience https://cytotec.directory/# buy cytotec
https://cytotec.directory/# buy cytotec over the counter
should i take tamoxifen: buy nolvadex online – tamoxifen citrate
A global name with a reputation for excellence http://cytotec.directory/# cytotec pills buy online
http://clomidpharm.shop/# where to buy generic clomid pill
prednisone for sale no prescription: prednisone – where can i get prednisone over the counter
Delivering worldwide standards with every prescription http://zithromaxpharm.online/# zithromax canadian pharmacy
buy zithromax 500mg online zithromax 250 zithromax z-pak price without insurance
https://cytotec.directory/# Abortion pills online
Comprehensive side effect and adverse reaction information https://zithromaxpharm.online/# zithromax 500 mg for sale
https://zithromaxpharm.online/# buy cheap zithromax online
zithromax 500 mg lowest price online: buy zithromax canada – zithromax antibiotic
order azipro 500mg without prescription azithromycin usa buy generic azipro
Как только я начал заботиться о своём питании, я понял, что мне нужна надежная маслодавка. Спасибо ‘Все соки’ за их прекрасный выбор. Теперь я делаю чистое и полезное масло в домашних условиях. https://h-100.ru/collection/maslopressy – Маслодавка стала важной частью моей кухни.
drug information and news for professionals and consumers http://zithromaxpharm.online/# zithromax drug
prednisone buy no prescription: prednisone 40 mg – prednisone buying
order furosemide for sale buy furosemide online diuretic
What side effects can this medication cause? https://clomidpharm.shop/# get generic clomid now
where to get zithromax: buy zithromax online fast shipping – generic zithromax medicine
how to get generic clomid generic clomid without a prescription buying generic clomid prices
Always leaving this place satisfied http://cytotec.directory/# п»їcytotec pills online
https://nolvadex.pro/# tamoxifen rash pictures
tamoxifen alternatives premenopausal: tamoxifen men – aromatase inhibitors tamoxifen
Providing global access to life-saving medications https://prednisonepharm.store/# prednisone medicine
https://prednisonepharm.store/# medicine prednisone 5mg
http://zithromaxpharm.online/# buy zithromax 1000mg online
psyho2031.8ua.ru
Get information now https://prednisonepharm.store/# prednisone 20mg for sale
https://clomidpharm.shop/# how to buy clomid without dr prescription
where buy generic clomid for sale: get generic clomid no prescription – can i order generic clomid no prescription
perscription drugs without perscription drug stores canada canadian pharmacy tadalafil
list of approved canadian pharmacies: medication online – legitimate canadian internet pharmacies
http://edpills.bid/# cheapest ed pills online
http://edpills.bid/# best ed drugs
online pharmacy without precriptions: viagra at canadian pharmacy – canadian drugstore reviews
viagra without doctor prescription tadalafil without a doctor’s prescription ed meds online without doctor prescription
omnacortil 10mg drug prednisolone 10mg sale purchase prednisolone without prescription
http://edwithoutdoctorprescription.store/# viagra without a prescription
ed treatment drugs: best over the counter ed pills – ed meds
canadian pharmacy cialis cheap https://edwithoutdoctorprescription.store/# viagra without a doctor prescription walmart
legit canadian pharmacy online
top rated canadian mail order pharmacies medicine from canada with no prescriptions online canadian pharmaceutical companies
online pharmacy mail order: canadian pharmacy cheap – family pharmacy online
mens erection pills erectile dysfunction medicines medications for ed
https://edpills.bid/# ed pill
https://reputablepharmacies.online/# safe canadian pharmacy
non prescription ed pills: generic viagra without a doctor prescription – sildenafil without a doctor’s prescription
best ed drugs online ed pills п»їerectile dysfunction medication
https://edpills.bid/# men’s ed pills
Займ без отказа мгновенно – У нас есть партнеры, которые предоставляют займы с минимальными требованиями к заемщику. Вы можете получить займ мгновенно, даже если у вас нет идеальной кредитной истории. К тому же, для новых клиентов доступны займы под 0%.
internet pharmacies http://edwithoutdoctorprescription.store/# buy prescription drugs
discount prescription drugs
buy prescription drugs from canada viagra without a doctor prescription walmart sildenafil without a doctor’s prescription
viagra without doctor prescription: buy prescription drugs from canada cheap – ed meds online without doctor prescription
http://edwithoutdoctorprescription.store/# cialis without a doctor’s prescription
canadian pharmacy selling viagra certified canadian online pharmacies online meds
100mg viagra without a doctor prescription: buy prescription drugs from india – buy prescription drugs from canada
top canadian pharmacies: cheap prescription drugs online – canadian pharmacy prescription
top ed drugs cheapest ed pills online ed meds online without doctor prescription
http://reputablepharmacies.online/# pharmacy canada
http://edwithoutdoctorprescription.store/# sildenafil without a doctor’s prescription
canadian meds: legitimate canadian pharmacies – canadian pharmacy without prescription
new ed treatments ed pills online erectile dysfunction medicines
https://reputablepharmacies.online/# canadian pharmacy non prescription
non prescription ed pills: how to get prescription drugs without doctor – buy prescription drugs without doctor
legitimate canadian pharmacy Pharmacies in Canada that ship to the US reputable canadian online pharmacy canadianpharmacy.pro
http://canadianpharmacy.pro/# canada pharmacy online canadianpharmacy.pro
canada pharmacy online legit: canadian discount pharmacy – best canadian pharmacy canadianpharmacy.pro
http://canadianpharmacy.pro/# vipps approved canadian online pharmacy canadianpharmacy.pro
legitimate canadian pharmacies online
top 10 pharmacies in india Best Indian pharmacy india online pharmacy indianpharmacy.shop
buy amoxil 250mg pills amoxil order cost amoxicillin 1000mg
https://canadianpharmacy.pro/# canadian mail order pharmacy canadianpharmacy.pro
https://mexicanpharmacy.win/# buying prescription drugs in mexico mexicanpharmacy.win
purple pharmacy mexico price list: online mexican pharmacy – п»їbest mexican online pharmacies mexicanpharmacy.win
vibra-tabs pills doxycycline price
legit canadian pharmacy Canadian pharmacy online canadian pharmacies canadianpharmacy.pro
mexico pharmacy: Mexico pharmacy – medicine in mexico pharmacies mexicanpharmacy.win
https://canadianpharmacy.pro/# precription drugs from canada canadianpharmacy.pro
canadian world pharmacy canadian pharmacy 24 canada ed drugs canadianpharmacy.pro
https://indianpharmacy.shop/# buy prescription drugs from india indianpharmacy.shop
giant discount pharmacy
http://mexicanpharmacy.win/# buying prescription drugs in mexico mexicanpharmacy.win
medication from mexico pharmacy Mexico pharmacy mexico pharmacies prescription drugs mexicanpharmacy.win
https://indianpharmacy.shop/# п»їlegitimate online pharmacies india indianpharmacy.shop
http://mexicanpharmacy.win/# mexican rx online mexicanpharmacy.win
mexican pharmaceuticals online online mexican pharmacy buying prescription drugs in mexico mexicanpharmacy.win
http://indianpharmacy.shop/# pharmacy website india indianpharmacy.shop
buy medicines online in india
mexico drug stores pharmacies Medicines Mexico buying prescription drugs in mexico online mexicanpharmacy.win
http://canadianpharmacy.pro/# canadapharmacyonline canadianpharmacy.pro
https://canadianpharmacy.pro/# best rated canadian pharmacy canadianpharmacy.pro
top 10 online pharmacy in india
mexican mail order pharmacies mexican drugstore online mexican rx online mexicanpharmacy.win
http://indianpharmacy.shop/# Online medicine home delivery indianpharmacy.shop
http://canadianpharmacy.pro/# canadian pharmacy meds review canadianpharmacy.pro
trusted canadian pharmacies
http://indianpharmacy.shop/# indian pharmacy indianpharmacy.shop
top 10 pharmacies in india
https://canadianpharmacy.pro/# canadian online pharmacy reviews canadianpharmacy.pro
http://indianpharmacy.shop/# best online pharmacy india indianpharmacy.shop
canadian valley pharmacy Canada Pharmacy canadian pharmacy reviews canadianpharmacy.pro
https://indianpharmacy.shop/# indianpharmacy com indianpharmacy.shop
mail order pharmacy india
http://canadianpharmacy.pro/# reliable canadian online pharmacy canadianpharmacy.pro
buy ventolin 2mg generic purchase albuterol without prescription buy generic ventolin online
http://mexicanpharmacy.win/# mexico pharmacy mexicanpharmacy.win
pharmacy website india indian pharmacy reputable indian online pharmacy indianpharmacy.shop
https://indianpharmacy.shop/# indian pharmacies safe indianpharmacy.shop
Online medicine order
https://canadianpharmacy.pro/# canadian pharmacy 1 internet online drugstore canadianpharmacy.pro
pharmacies in mexico that ship to usa pharmacies in mexico that ship to usa buying prescription drugs in mexico mexicanpharmacy.win
http://mexicanpharmacy.win/# п»їbest mexican online pharmacies mexicanpharmacy.win
pharmacy website india
https://indianpharmacy.shop/# indianpharmacy com indianpharmacy.shop
canadian discount online pharmacy
https://mexicanpharmacy.win/# purple pharmacy mexico price list mexicanpharmacy.win
online pharmacy india Best Indian pharmacy best india pharmacy indianpharmacy.shop
https://indianpharmacy.shop/# top 10 online pharmacy in india indianpharmacy.shop
indian pharmacy online
п»їpharmacie en ligne: kamagra livraison 24h – pharmacie ouverte 24/24
amoxiclav order buy clavulanate tablets
pharmacie ouverte 24/24 levitra generique prix en pharmacie Pharmacie en ligne pas cher
http://viagrasansordonnance.pro/# Viagra gГ©nГ©rique pas cher livraison rapide
Pharmacie en ligne sans ordonnance
https://viagrasansordonnance.pro/# Viagra homme sans ordonnance belgique
Pharmacie en ligne sans ordonnance: Acheter Cialis 20 mg pas cher – Pharmacie en ligne livraison 24h
acheter medicament a l etranger sans ordonnance: kamagra gel – Pharmacie en ligne livraison rapide
Pharmacie en ligne livraison rapide cialis generique acheter mГ©dicaments Г l’Г©tranger
http://psyho2039.8ua.ru/
https://pharmadoc.pro/# acheter médicaments à l’étranger
Viagra vente libre allemagne: Meilleur Viagra sans ordonnance 24h – Prix du Viagra 100mg en France
Pharmacie en ligne livraison gratuite levitra generique prix en pharmacie п»їpharmacie en ligne
http://pharmadoc.pro/# acheter médicaments à l’étranger
http://viagrasansordonnance.pro/# Viagra sans ordonnance 24h Amazon
Pharmacie en ligne France
Viagra sans ordonnance livraison 48h: Acheter du Viagra sans ordonnance – Viagra homme prix en pharmacie sans ordonnance
Acheter mГ©dicaments sans ordonnance sur internet achat kamagra acheter mГ©dicaments Г l’Г©tranger
https://pharmadoc.pro/# Pharmacie en ligne livraison 24h
п»їpharmacie en ligne: kamagra oral jelly – Pharmacie en ligne fiable
Viagra sans ordonnance 24h suisse: Viagra prix pharmacie paris – Viagra sans ordonnance livraison 24h
synthroid 150mcg sale purchase levothyroxine pill levothroid over the counter
Pharmacie en ligne livraison gratuite: Levitra 20mg prix en pharmacie – pharmacie ouverte 24/24
https://viagrasansordonnance.pro/# Viagra vente libre allemagne
Viagra sans ordonnance livraison 48h Acheter du Viagra sans ordonnance Acheter Sildenafil 100mg sans ordonnance
Pharmacie en ligne livraison 24h: Acheter Cialis – Pharmacie en ligne France
http://levitrasansordonnance.pro/# Pharmacie en ligne livraison 24h
buy vardenafil 10mg sale buy levitra 20mg generic
http://levitrasansordonnance.pro/# Pharmacie en ligne pas cher
Pharmacie en ligne livraison gratuite
Pharmacie en ligne livraison 24h PharmaDoc Pharmacie en ligne fiable
Acheter Sildenafil 100mg sans ordonnance: Meilleur Viagra sans ordonnance 24h – Viagra en france livraison rapide
https://acheterkamagra.pro/# pharmacie ouverte 24/24
zithromax 250 mg australia: where can you buy zithromax – zithromax antibiotic
canadian online pharmacy prednisone: over the counter prednisone pills – 20 mg prednisone
prednisone without prescription medication 25 mg prednisone prednisone buying
https://clomiphene.icu/# can i buy clomid
http://ivermectin.store/# stromectol 6 mg tablet
ivermectin 8000: buy ivermectin stromectol – generic name for ivermectin
buy generic clomiphene 100mg buy clomid paypal brand serophene
http://ivermectin.store/# ivermectin buy uk
buying clomid without prescription how can i get cheap clomid for sale where to get generic clomid
buy amoxicillin 500mg online: amoxicillin no prescipion – amoxil pharmacy
cheap clomid without dr prescription: buy clomid without rx – order clomid without a prescription
http://prednisonetablets.shop/# prednisone 20mg prices
ivermectin over the counter uk ivermectin for humans ivermectin humans
20 mg of prednisone: can i buy prednisone from canada without a script – buy prednisone online without a script
http://prednisonetablets.shop/# prednisone without prescription medication
buy zithromax canada: zithromax over the counter canada – can you buy zithromax online
amoxicillin 500 capsule where to buy amoxicillin 500mg without prescription where can i buy amoxicillin over the counter uk
zanaflex tablet purchase tizanidine for sale order tizanidine 2mg online cheap
http://amoxicillin.bid/# amoxicillin 500mg no prescription
amoxacillian without a percription: amoxicillin 500 capsule – amoxicillin online purchase
zithromax capsules 250mg: zithromax 500 mg lowest price online – zithromax online no prescription
https://azithromycin.bid/# zithromax canadian pharmacy
ivermectin virus ivermectin 0.5% brand name where to buy ivermectin cream
1 mg prednisone daily: buy prednisone 20mg – prednisone 21 pack
http://amoxicillin.bid/# over the counter amoxicillin canada
prednisone 20mg prednisone 50 mg for sale prednisone 2.5 tablet
semaglutide 14 mg cheap rybelsus oral cheap semaglutide 14mg
stromectol 3 mg dosage: ivermectin generic cream – stromectol pill
http://amoxicillin.bid/# amoxicillin 500mg capsule cost
zithromax coupon: zithromax coupon – zithromax online paypal
https://ivermectin.store/# ivermectin 0.1 uk
zithromax for sale online: zithromax 500 without prescription – how to get zithromax online
prednisone 10 prednisone for sale can i buy prednisone over the counter in usa
https://amoxicillin.bid/# amoxicillin canada price
generic prednisone 40mg prednisone pills prednisone 20mg sale
mexican mail order pharmacies: Certified Pharmacy from Mexico – medicine in mexico pharmacies mexicanpharm.shop
canadian discount pharmacy: Canadian International Pharmacy – is canadian pharmacy legit canadianpharm.store
purple pharmacy mexico price list: Certified Pharmacy from Mexico – pharmacies in mexico that ship to usa mexicanpharm.shop
canadian pharmacy 24h com cross border pharmacy canada canadian online pharmacy canadianpharm.store
https://mexicanpharm.shop/# mexican mail order pharmacies mexicanpharm.shop
buying prescription drugs in mexico online: purple pharmacy mexico price list – medicine in mexico pharmacies mexicanpharm.shop
https://mexicanpharm.shop/# mexican border pharmacies shipping to usa mexicanpharm.shop
https://bit.ly/sistemniy-podkhod
mexican pharmacy Online Pharmacies in Mexico mexico pharmacy mexicanpharm.shop
https://indianpharm.store/# mail order pharmacy india indianpharm.store
canadian family pharmacy: Canadian International Pharmacy – canadian pharmacy ltd canadianpharm.store
mexican rx online: Certified Pharmacy from Mexico – buying from online mexican pharmacy mexicanpharm.shop
how to buy semaglutide purchase rybelsus online oral rybelsus 14mg
https://mexicanpharm.shop/# best online pharmacies in mexico mexicanpharm.shop
india pharmacy international medicine delivery from india mail order pharmacy india indianpharm.store
india online pharmacy: order medicine from india to usa – reputable indian pharmacies indianpharm.store
mexico drug stores pharmacies: Online Mexican pharmacy – pharmacies in mexico that ship to usa mexicanpharm.shop
http://canadianpharm.store/# pharmacy rx world canada canadianpharm.store
reputable indian pharmacies: order medicine from india to usa – п»їlegitimate online pharmacies india indianpharm.store
buying from online mexican pharmacy Online Mexican pharmacy mexico pharmacies prescription drugs mexicanpharm.shop
order accutane without prescription order isotretinoin 40mg generic purchase isotretinoin
http://indianpharm.store/# best online pharmacy india indianpharm.store
buy prescription drugs from india: order medicine from india to usa – best india pharmacy indianpharm.store
https://indianpharm.store/# Online medicine home delivery indianpharm.store
mexican rx online Online Pharmacies in Mexico buying prescription drugs in mexico mexicanpharm.shop
best online pharmacy india: order medicine from india to usa – top 10 pharmacies in india indianpharm.store
indian pharmacy paypal: Online medicine order – indian pharmacies safe indianpharm.store
http://indianpharm.store/# best online pharmacy india indianpharm.store
mexican pharmaceuticals online: Online Pharmacies in Mexico – mexican pharmaceuticals online mexicanpharm.shop
canadian neighbor pharmacy: Licensed Online Pharmacy – canadian drugs online canadianpharm.store
reputable indian pharmacies order medicine from india to usa indian pharmacies safe indianpharm.store
https://indianpharm.store/# india pharmacy mail order indianpharm.store
order albuterol pills albuterol oral purchase albuterol
india pharmacy mail order: order medicine from india to usa – mail order pharmacy india indianpharm.store
https://canadianpharm.store/# canadapharmacyonline legit canadianpharm.store
canadianpharmacymeds Pharmacies in Canada that ship to the US canada ed drugs canadianpharm.store
canadianpharmacyworld: Canadian International Pharmacy – canadian pharmacy canadianpharm.store
http://indianpharm.store/# indian pharmacy paypal indianpharm.store
mexican online pharmacies prescription drugs: Certified Pharmacy from Mexico – п»їbest mexican online pharmacies mexicanpharm.shop
reputable mexican pharmacies online: Online Mexican pharmacy – mexican rx online mexicanpharm.shop
https://indianpharm.store/# buy prescription drugs from india indianpharm.store
77 canadian pharmacy Canada Pharmacy online adderall canadian pharmacy canadianpharm.store
п»їbest mexican online pharmacies: reputable mexican pharmacies online – mexican pharmacy mexicanpharm.shop
https://indianpharm.store/# best india pharmacy indianpharm.store
order amoxicillin 1000mg generic amoxicillin 500mg us buy generic amoxil
canada cloud pharmacy: Licensed Online Pharmacy – canadian pharmacy online ship to usa canadianpharm.store
prescription drugs canada buy online Canadian Pharmacy canadian pharmacy online canadianpharm.store
https://canadianpharm.store/# safe canadian pharmacies canadianpharm.store
legit canadian pharmacy: Canada Pharmacy online – legit canadian pharmacy canadianpharm.store
cheapest online pharmacy india: international medicine delivery from india – cheapest online pharmacy india indianpharm.store
http://canadianpharm.store/# pet meds without vet prescription canada canadianpharm.store
Online medicine home delivery: top online pharmacy india – indianpharmacy com indianpharm.store
mail order pharmacy india Indian pharmacy to USA india pharmacy mail order indianpharm.store
https://indianpharm.store/# india pharmacy indianpharm.store
my canadian pharmacy: prescription drugs canada buy online – cross border pharmacy canada canadianpharm.store
buy augmentin cheap order augmentin 375mg pill amoxiclav online
certified mexican pharmacy: online pharmacies canada reviews – discount viagra canadian pharmacy
canadian pharmacy: generic pharmacy store – online prescriptions canada without
internet pharmacy legit canadian online pharmacy canada drugs without prescription
http://canadadrugs.pro/# canadian pharmacies without an rx
canada pharmacy world: buy medicine canada – canadian pharmacy worldwide
best canadian pharmacies: best online pharmacy without prescriptions – pharmacy price compare
https://canadadrugs.pro/# pharmacy drugstore online
prescriptions online best canadian pharmacy for viagra mexican pharmacies online cheap
online pharmacies canada reviews: mexico pharmacy order online – drugs online
canadian pharmacy no prescrition: canada drugs without prescription – canadadrugpharmacy
purchase zithromax generic generic azithromycin 250mg zithromax 500mg ca
https://canadadrugs.pro/# ed meds online without doctor prescription
canada drugs without prescription accutane mexican pharmacy canadian prescription drugs online
best online pharmacy stores: cheap drugs online – over the counter drug store
reliable online drugstore: online ed medication no prescription – drugs from canada with prescription
compare pharmacy prices: us pharmacy no prior prescription – canadian neighborhood pharmacy
http://canadadrugs.pro/# list of online canadian pharmacies
canadian meds: canada drugs online – legitimate online pharmacy usa
canadian online pharmacies legitimate by aarp: online canadian pharmacy no prescription – pharmacy cost comparison
buy levothyroxine without a prescription buy synthroid pills for sale synthroid tablets
ed meds online: recommended online pharmacies – canadian prescription
https://canadadrugs.pro/# trusted online canadian pharmacy
canadian pharmacies for cialis: on line pharmacy with no perscriptions – reputable canadian mail order pharmacies
http://canadadrugs.pro/# legitimate online pharmacy usa
best internet pharmacies: online ed drugs no prescription – canadian rx
mail order prescription drugs: non prescription drugs – canada drug
http://canadadrugs.pro/# thecanadianpharmacy com
cheap drugs canada: my canadian pharmacy rx – bestpharmacyonline.com
order prednisolone 5mg without prescription brand omnacortil 10mg order omnacortil 10mg pills
online canadian pharmacy no prescription needed: best online pharmacies without prescription – buy prescription drugs online
https://canadadrugs.pro/# cheap prescriptions
top 10 online pharmacies: canadian online pharmacies legitimate by aarp – buy meds online
http://canadadrugs.pro/# canadian pharmacy no rx
nabp canadian pharmacy: safe online pharmacies – certified canadian pharmacies
http://canadadrugs.pro/# price drugs
the canadian drugstore: northern pharmacy canada – canadian pharmacy com
buy clomiphene without a prescription order clomid 50mg online cheap buy clomiphene pills
india online pharmacy: cheapest online pharmacy india – reputable indian pharmacies
best pills for ed ed pills that work best treatment for ed
http://edwithoutdoctorprescription.pro/# prescription drugs without prior prescription
ed treatment review: ed pills that really work – generic ed pills
http://canadianinternationalpharmacy.pro/# canadian pharmacy world reviews
canada pharmacy reviews canadian pharmacy world canada pharmacy 24h
https://edpill.cheap/# treatment of ed
mail order pharmacy india: Online medicine home delivery – india pharmacy
mexican pharmaceuticals online mexico drug stores pharmacies mexican rx online
https://certifiedpharmacymexico.pro/# buying prescription drugs in mexico
cheapest online pharmacy india: indian pharmacies safe – online pharmacy india
https://canadianinternationalpharmacy.pro/# canadian pharmacy online reviews
mexican drugstore online mexican pharmacy buying prescription drugs in mexico
cheap neurontin gabapentin 100mg oral order gabapentin 100mg without prescription
https://edwithoutdoctorprescription.pro/# prescription drugs online
best drug for ed ed medications online top ed pills
pet meds without vet prescription canada: the canadian pharmacy – pharmacy in canada
http://edwithoutdoctorprescription.pro/# real viagra without a doctor prescription usa
prescription drugs online without ed pills without doctor prescription viagra without a doctor prescription
mexico pharmacies prescription drugs: п»їbest mexican online pharmacies – mexico pharmacies prescription drugs
https://canadianinternationalpharmacy.pro/# drugs from canada
reputable canadian online pharmacy: canada drugstore pharmacy rx – pharmacy in canada
best online pharmacy india top 10 online pharmacy in india best india pharmacy
http://canadianinternationalpharmacy.pro/# best canadian pharmacy to order from
http://edpill.cheap/# buying ed pills online
mexico pharmacy reputable mexican pharmacies online purple pharmacy mexico price list
http://edpill.cheap/# medicine for erectile
reputable indian online pharmacy: online shopping pharmacy india – top 10 pharmacies in india
canadian drug pharmacy canadian pharmacy india canadian pharmacy near me
order sildenafil 100mg sildenafil ca sildenafil pharmacy
http://certifiedpharmacymexico.pro/# mexican pharmacy
order furosemide 100mg without prescription buy lasix 100mg for sale buy furosemide pills
legitimate canadian pharmacies certified canadian pharmacy canada rx pharmacy world
https://edwithoutdoctorprescription.pro/# buy prescription drugs from canada cheap
buy ed pills online ed treatments erection pills viagra online
http://edpill.cheap/# male ed drugs
real viagra without a doctor prescription usa: generic cialis without a doctor prescription – discount prescription drugs
http://edpill.cheap/# ed meds online
canadian pharmacy online canadian online drugs thecanadianpharmacy
http://canadianinternationalpharmacy.pro/# canadian drug prices
buy medicines online in india top 10 pharmacies in india reputable indian pharmacies
http://certifiedpharmacymexico.pro/# mexican mail order pharmacies
canadian drugs my canadian pharmacy reviews canadianpharmacyworld com
best male ed pills: medication for ed dysfunction – erectile dysfunction pills
http://edpill.cheap/# men’s ed pills
http://medicinefromindia.store/# buy medicines online in india
order semaglutide 14 mg pill buy semaglutide 14 mg online brand rybelsus 14 mg
prescription drugs online without cialis without a doctor prescription non prescription erection pills
buy monodox buy doxycycline 100mg generic acticlate tablet
https://edwithoutdoctorprescription.pro/# prescription drugs
canadian pharmacy 1 internet online drugstore canadian online drugs canadian pharmacy meds
http://edwithoutdoctorprescription.pro/# online prescription for ed meds
NBA computer picks have become quite popular with the evolution of technology and its ability to analyze thousands of pieces of data. There are no errors with mathematical calculations when creating predictions. In addition, computers are not affected by bias when making picks. However, NBA computer picks can’t calculate for human unpredictability. Then, beyond the show, know that home court advantage is also important in the NBA. As you know, sports betting sites generally offer generous odds for teams playing on the road. Don’t be fooled! Beyond the recent behemoths like the Nets, Bucks and Warriors, teams playing in their own venues are generally performing well in the US league. The average winning percentage for home teams at around the halfway mark of the season is 60.9%, which is up from last season’s average home winning percentage of 55%. When you know that a draw is extremely rare (even if there is automatic overtime, some bookmakers offer to bet on a draw in regulation time), there is a good chance that you will win your bet by predicting a home team victory.
http://6329331159240267295_a55a8d27dffdedad3525a8674c627781b8c45066.blogspot.com/
By Sean Jones: Canelo Alvarez will put his undisputed super middleweight championship on the line against the upset-minded Jermell Charlo on Showtime PPV on September … read full story ← It’s a great time to be a boxing fan, but there’s more to it than that. Our boxing betting tipster – former professional fighter Frankie Monkhouse – is ready to help make it pay for our readers. Before offering his reliable predictions, he will do this through in-depth previews, using the latest and best betting odds offered by major sportsbooks. Devin “The Dream” Haney has waited four long years to get his hands on Vasiliy Lomachenko. And for four years, Lomachenko wasn’t interested in answering the call. But now that Haney (29-0, 15 KOs) is the undisputed lightweight champion he has something that Lomachenko wants and the two will battle at the MGM Grand Garden Arena in Las Vegas, NV on May 20 in a showdown where titles and how the future of boxing will shake out are both on the line.
buy erection pills: best ed medications – men’s ed pills
generic ed pills cure ed ed meds online without doctor prescription
https://canadianinternationalpharmacy.pro/# ed meds online canada
ed drugs list erectile dysfunction medications buy ed pills
http://canadianinternationalpharmacy.pro/# canadian pharmacy no scripts
mexico drug stores pharmacies mexican online pharmacies prescription drugs mexico drug stores pharmacies
http://mexicanph.com/# mexico drug stores pharmacies
mexican pharmaceuticals online
mexican online pharmacies prescription drugs mexican drugstore online mexican border pharmacies shipping to usa
mexican online pharmacies prescription drugs purple pharmacy mexico price list medication from mexico pharmacy
medication from mexico pharmacy buying prescription drugs in mexico buying prescription drugs in mexico
order generic levitra 10mg levitra online order buy vardenafil 10mg generic
free roulette games doubleu casino online casino playing poker online for money
п»їbest mexican online pharmacies mexico pharmacies prescription drugs reputable mexican pharmacies online
mexican rx online medication from mexico pharmacy best mexican online pharmacies
mexican drugstore online medication from mexico pharmacy medication from mexico pharmacy
http://mexicanph.shop/# mexican pharmaceuticals online
mexican online pharmacies prescription drugs
mexican mail order pharmacies medication from mexico pharmacy medicine in mexico pharmacies
mexican pharmaceuticals online mexico drug stores pharmacies reputable mexican pharmacies online
https://mexicanph.shop/# mexico pharmacies prescription drugs
reputable mexican pharmacies online
mexican pharmacy best online pharmacies in mexico buying from online mexican pharmacy
mexican drugstore online mexico pharmacies prescription drugs best online pharmacies in mexico
lyrica cost buy lyrica pills for sale buy lyrica 75mg pills
cheap plaquenil 200mg plaquenil 400mg cheap plaquenil 400mg generic
http://mexicanph.shop/# purple pharmacy mexico price list
best online pharmacies in mexico
reputable mexican pharmacies online best mexican online pharmacies mexico drug stores pharmacies
best online pharmacies in mexico best online pharmacies in mexico best online pharmacies in mexico
mexican pharmacy buying prescription drugs in mexico online mexican border pharmacies shipping to usa
buying prescription drugs in mexico online mexico drug stores pharmacies mexico drug stores pharmacies
mexican pharmacy pharmacies in mexico that ship to usa pharmacies in mexico that ship to usa
п»їbest mexican online pharmacies mexican pharmacy mexico pharmacies prescription drugs
mexican online pharmacies prescription drugs mexico drug stores pharmacies mexico drug stores pharmacies
https://mexicanph.com/# purple pharmacy mexico price list
mexican pharmaceuticals online
mexican mail order pharmacies buying prescription drugs in mexico online mexican rx online
mexico pharmacy mexican rx online mexican rx online
mexican border pharmacies shipping to usa mexico drug stores pharmacies mexico drug stores pharmacies
reputable mexican pharmacies online mexican pharmacy mexico pharmacy
aristocort 10mg cost triamcinolone 4mg cheap where can i buy aristocort
mexican online pharmacies prescription drugs best online pharmacies in mexico mexico drug stores pharmacies
pharmacies in mexico that ship to usa mexican pharmacy mexican online pharmacies prescription drugs
medication from mexico pharmacy mexican online pharmacies prescription drugs buying prescription drugs in mexico online
reputable mexican pharmacies online buying prescription drugs in mexico mexican rx online
best online pharmacies in mexico buying prescription drugs in mexico buying prescription drugs in mexico
cialis 5mg sale cialis 20mg tablet tadalafil women
mexican online pharmacies prescription drugs mexican pharmacy reputable mexican pharmacies online
mexican pharmacy buying prescription drugs in mexico online pharmacies in mexico that ship to usa
buying prescription drugs in mexico online mexico pharmacy best online pharmacies in mexico
https://mexicanph.shop/# mexican pharmaceuticals online
buying prescription drugs in mexico online
mexico pharmacy mexican online pharmacies prescription drugs medication from mexico pharmacy
medicine in mexico pharmacies mexican pharmacy mexican pharmacy
buying prescription drugs in mexico online mexican rx online mexican online pharmacies prescription drugs
mexican pharmaceuticals online mexico pharmacy mexico pharmacy
mexican online pharmacies prescription drugs mexico drug stores pharmacies mexican online pharmacies prescription drugs
mexican drugstore online pharmacies in mexico that ship to usa medicine in mexico pharmacies
best online pharmacies in mexico medicine in mexico pharmacies buying from online mexican pharmacy
mexican mail order pharmacies mexican rx online buying prescription drugs in mexico online
buying prescription drugs in mexico online mexico drug stores pharmacies purple pharmacy mexico price list
mexico pharmacies prescription drugs buying prescription drugs in mexico mexican pharmacy
mexican pharmaceuticals online buying from online mexican pharmacy mexican border pharmacies shipping to usa
mexico pharmacies prescription drugs buying prescription drugs in mexico online п»їbest mexican online pharmacies
medicine in mexico pharmacies mexico drug stores pharmacies mexican pharmacy
https://mexicanph.shop/# buying from online mexican pharmacy
mexican online pharmacies prescription drugs
buying from online mexican pharmacy mexican pharmacy buying prescription drugs in mexico
clarinex uk clarinex cost cost clarinex 5mg
mexico pharmacies prescription drugs mexican border pharmacies shipping to usa mexican online pharmacies prescription drugs
mexican mail order pharmacies п»їbest mexican online pharmacies purple pharmacy mexico price list
mexican pharmacy reputable mexican pharmacies online buying prescription drugs in mexico online
mexican rx online mexico drug stores pharmacies buying prescription drugs in mexico
pharmacies in mexico that ship to usa mexico drug stores pharmacies mexican online pharmacies prescription drugs
п»їbest mexican online pharmacies mexico drug stores pharmacies mexican mail order pharmacies
best online pharmacies in mexico best online pharmacies in mexico medicine in mexico pharmacies
buy cenforce 100mg pills buy cenforce for sale cenforce for sale
mexican online pharmacies prescription drugs best online pharmacies in mexico mexico pharmacy
mexican rx online mexican border pharmacies shipping to usa mexican mail order pharmacies
pharmacies in mexico that ship to usa best online pharmacies in mexico mexico pharmacies prescription drugs
buying prescription drugs in mexico online buying prescription drugs in mexico online reputable mexican pharmacies online
buying prescription drugs in mexico online mexican pharmaceuticals online mexican border pharmacies shipping to usa
buying from online mexican pharmacy purple pharmacy mexico price list medicine in mexico pharmacies
mexican pharmacy mexico pharmacies prescription drugs medication from mexico pharmacy
buying prescription drugs in mexico online mexico drug stores pharmacies mexican online pharmacies prescription drugs
mexican mail order pharmacies п»їbest mexican online pharmacies mexican online pharmacies prescription drugs
mexican border pharmacies shipping to usa п»їbest mexican online pharmacies mexican border pharmacies shipping to usa
best mexican online pharmacies mexican rx online purple pharmacy mexico price list
mexican drugstore online medication from mexico pharmacy buying prescription drugs in mexico online
buying prescription drugs in mexico mexican border pharmacies shipping to usa mexican online pharmacies prescription drugs
mexican border pharmacies shipping to usa pharmacies in mexico that ship to usa buying from online mexican pharmacy
buying prescription drugs in mexico reputable mexican pharmacies online mexico drug stores pharmacies
mexican online pharmacies prescription drugs medicine in mexico pharmacies mexican pharmacy
best mexican online pharmacies mexico pharmacies prescription drugs mexico drug stores pharmacies
https://mexicanph.shop/# mexican drugstore online
п»їbest mexican online pharmacies
mexican mail order pharmacies mexico pharmacies prescription drugs pharmacies in mexico that ship to usa
reputable mexican pharmacies online reputable mexican pharmacies online buying prescription drugs in mexico online
order loratadine 10mg generic loratadine 10mg cheap buy claritin generic
medicine in mexico pharmacies mexican online pharmacies prescription drugs mexican rx online
mexico pharmacy mexico pharmacy mexico drug stores pharmacies
buy aralen 250mg online cheap chloroquine oral chloroquine 250mg us
medication from mexico pharmacy mexican pharmaceuticals online mexico drug stores pharmacies
mexican border pharmacies shipping to usa mexico pharmacies prescription drugs mexico pharmacy
buying from online mexican pharmacy mexican pharmacy medication from mexico pharmacy
medication from mexico pharmacy mexican mail order pharmacies buying prescription drugs in mexico
medication from mexico pharmacy reputable mexican pharmacies online mexico pharmacy
buying prescription drugs in mexico online best mexican online pharmacies medication from mexico pharmacy
best online pharmacies in mexico mexican rx online best online pharmacies in mexico
mexico drug stores pharmacies mexican border pharmacies shipping to usa buying prescription drugs in mexico
buying from online mexican pharmacy mexican pharmacy medicine in mexico pharmacies
mexican pharmaceuticals online buying prescription drugs in mexico online purple pharmacy mexico price list
medicine amoxicillin 500mg: amoxicillin 750 mg price – rexall pharmacy amoxicillin 500mg
http://lisinopril.top/# zestril 20 mg tablet
lisinopril tabs 40mg: prinivil 10 mg tablet – buy lisinopril 20 mg online canada
lasix Over The Counter Lasix furosemida
https://furosemide.guru/# lasix generic name
https://amoxil.cheap/# where to get amoxicillin over the counter
buy prednisone online india: 100 mg prednisone daily – prednisone 50 mg for sale
http://stromectol.fun/# buy ivermectin cream for humans
generic lasix: Buy Lasix No Prescription – furosemide 40mg
buy priligy for sale purchase priligy pills cytotec over the counter
amoxicillin 750 mg price prescription for amoxicillin amoxicillin 500mg price canada
glycomet 500mg canada buy glycomet 500mg generic metformin 1000mg uk
http://stromectol.fun/# stromectol tablets 3 mg
amoxicillin 500mg price: amoxicillin 500 mg purchase without prescription – amoxicillin without prescription
http://stromectol.fun/# ivermectin 24 mg
lasix dosage Over The Counter Lasix lasix medication
lisinopril 10 12.55mg: ordering lisinopril without a prescription uk – prescription drug zestril
prednisone 1 mg daily: prednisone 20mg online without prescription – prednisone without prescription medication
https://amoxil.cheap/# amoxicillin medicine
https://furosemide.guru/# lasix side effects
lasix: Buy Lasix No Prescription – lasix for sale
buy cheap amoxicillin online amoxicillin over counter amoxicillin online purchase
http://buyprednisone.store/# prednisone for cheap
buy prednisone online india: prednisone 5 mg tablet cost – prednisone 20mg for sale
http://furosemide.guru/# lasix 100mg
buy lasix online: lasix dosage – furosemide 100mg
lisinopril 5 mg tablet cost buy lisinopril online india lisinopril pill
https://amoxil.cheap/# where can i buy amoxicillin without prec
non prescription prednisone 20mg: 25 mg prednisone – buy prednisone online usa
lisinopril 20mg pill: lisinopril 20 mg price – lisinopril 90 pills cost
xenical pills buy xenical 60mg pills generic diltiazem
https://buyprednisone.store/# buy prednisone online australia
https://lisinopril.top/# cost of lisinopril 10 mg
amoxicillin without a doctors prescription: amoxicillin order online no prescription – amoxicillin 200 mg tablet
prednisone cost us prednisone buy cheap purchase prednisone no prescription
http://furosemide.guru/# buy lasix online
60 mg prednisone daily: apo prednisone – prednisone cost in india
order lipitor 40mg for sale purchase lipitor lipitor 40mg canada
http://lisinopril.top/# lisinopril 5 mg tabs
buy amoxicillin 500mg capsules uk: amoxicillin 500mg price in canada – can i purchase amoxicillin online
price lisinopril 20 mg cheapest price for lisinopril india lisinopril 3.5 mg
https://lisinopril.top/# lisinopril 5 mg price in india
lasix medication: Buy Lasix No Prescription – buy furosemide online
http://amoxil.cheap/# amoxil generic
amoxicillin 500mg capsules: amoxicillin capsule 500mg price – amoxicillin 825 mg
10mg prednisone daily: prednisone 1 mg tablet – prednisone 50 mg price
furosemide 100mg Buy Lasix No Prescription generic lasix
https://buyprednisone.store/# prednisone pharmacy
http://furosemide.guru/# furosemide 40mg
ivermectin cost canada: stromectol buy uk – ivermectin 0.5
http://furosemide.guru/# buy furosemide online
stromectol 3mg tablets: stromectol tab – buy liquid ivermectin
stromectol over the counter buy stromectol pills ivermectin over the counter
lasix side effects: Buy Furosemide – lasix 40mg
https://stromectol.fun/# stromectol lotion
norvasc price amlodipine generic buy amlodipine 5mg online
http://buyprednisone.store/# average price of prednisone
lisinopril 5 mg price in india: buy lisinopril 20 mg online usa – lisinopril 10
lasix uses Buy Lasix No Prescription buy furosemide online
http://amoxil.cheap/# amoxicillin 500mg no prescription
amoxicillin generic: amoxicillin 750 mg price – amoxicillin 500mg capsules antibiotic
https://amoxil.cheap/# order amoxicillin online no prescription
price for 5 mg lisinopril: prinivil 10 mg tablet – zestoretic 10 12.5 mg
oral zovirax 400mg buy generic acyclovir zyloprim medication
http://amoxil.cheap/# purchase amoxicillin online without prescription
lisinopril pill 5 mg: rx lisinopril 10mg – lisinopril 20mg coupon
ivermectin 24 mg ivermectin 3mg tab ivermectin cost canada
https://buyprednisone.store/# buy prednisone tablets uk
lisinopril 20 mg for sale: purchase lisinopril 10 mg – lisinopril 50 mg
http://lisinopril.top/# lisinopril 40 mg on line
order prednisone 10mg: prednisone oral – 50 mg prednisone from canada
order prednisone buy prednisone tablets uk prednisone 15 mg tablet
https://buyprednisone.store/# prednisone 10mg prices
buy generic zestril 2.5mg buy zestril online cheap purchase zestril pills
lasix 20 mg: Over The Counter Lasix – lasix 40mg
stromectol generic: cost of ivermectin 3mg tablets – ivermectin 2mg
https://stromectol.fun/# buy stromectol online
http://amoxil.cheap/# amoxicillin 200 mg tablet
https://furosemide.guru/# furosemida 40 mg
amoxicillin cephalexin buy amoxicillin amoxicillin buy online canada
lisinopril pill 40 mg: zestoretic – lisinopril pill
http://furosemide.guru/# furosemide 100mg
lisinopril: buy lisinopril 20 mg online canada – price of lisinopril 5mg
buy rosuvastatin generic cheap ezetimibe 10mg order ezetimibe online cheap
price of prednisone 5mg: where can i buy prednisone without prescription – prednisone 1 mg for sale
https://buyprednisone.store/# prednisone 20 mg purchase
amoxicillin 50 mg tablets amoxicillin 500mg capsule cost amoxicillin 500
http://stromectol.fun/# ivermectin cream canada cost
buy lisinopril 20 mg without prescription: prinivil 10 mg tab – lisinopril pills 2.5 mg
can you buy amoxicillin over the counter in canada: amoxicillin 500mg capsules price – cost of amoxicillin 875 mg
http://furosemide.guru/# lasix side effects
http://lisinopril.top/# prinivil coupon
stromectol medicine: buy ivermectin for humans uk – stromectol without prescription
lisinopril price without insurance lisinopril 10mg online medication lisinopril 10 mg
http://stromectol.fun/# stromectol online canada
amoxicillin 500 capsule: purchase amoxicillin online – amoxicillin no prescription
http://stromectol.fun/# ivermectin 10 ml
order prilosec sale buy prilosec 20mg generic cost prilosec 10mg
motilium 10mg us buy sumycin pills sumycin 250mg oral
indian pharmacy paypal best india pharmacy cheapest online pharmacy india
best online pharmacy india best india pharmacy buy medicines online in india
https://indianph.com/# india online pharmacy
legitimate online pharmacies india
indianpharmacy com buy medicines online in india Online medicine home delivery
https://indianph.xyz/# best online pharmacy india
mail order pharmacy india
order metoprolol 50mg online metoprolol 50mg without prescription metoprolol 100mg oral
http://indianph.com/# india pharmacy mail order
indian pharmacy online
http://indianph.xyz/# india pharmacy mail order
mail order pharmacy india indian pharmacy п»їlegitimate online pharmacies india
https://indianph.com/# top 10 online pharmacy in india
top 10 online pharmacy in india
indian pharmacies safe world pharmacy india best india pharmacy
http://indianph.com/# pharmacy website india
top online pharmacy india
cyclobenzaprine generic how to buy flexeril ozobax uk
https://indianph.xyz/# pharmacy website india
cheapest online pharmacy india
online shopping pharmacy india reputable indian online pharmacy top online pharmacy india
http://indianph.xyz/# best online pharmacy india
top 10 pharmacies in india
http://indianph.xyz/# mail order pharmacy india
buy medicines online in india
indian pharmacies safe cheapest online pharmacy india cheapest online pharmacy india
https://indianph.xyz/# online pharmacy india
world pharmacy india reputable indian online pharmacy online pharmacy india
https://indianph.com/# indian pharmacies safe
reputable indian pharmacies
atenolol for sale online order tenormin 50mg online buy atenolol 50mg without prescription
Cytotec 200mcg price: buy cytotec in usa – Abortion pills online
http://nolvadex.guru/# pct nolvadex
how to buy toradol toradol canada colcrys order online
cytotec online: cytotec pills buy online – buy cytotec
where to buy diflucan in uk diflucan 200 mg diflucan 50mg capsules
https://doxycycline.auction/# 100mg doxycycline
https://nolvadex.guru/# tamoxifen medication
buy cipro online: antibiotics cipro – cipro 500mg best prices
https://cipro.guru/# cipro 500mg best prices
diflucan 150 otc diflucan otc canada diflucan over the counter
https://doxycycline.auction/# doxycycline generic
ciprofloxacin mail online: п»їcipro generic – ciprofloxacin generic
http://nolvadex.guru/# where can i buy nolvadex
where can i buy cipro online ciprofloxacin 500 mg tablet price buy ciprofloxacin over the counter
https://nolvadex.guru/# tamoxifen and grapefruit
tamoxifen estrogen: tamoxifen and weight loss – tamoxifen for men
http://diflucan.pro/# diflucan online purchase
cytotec abortion pill: п»їcytotec pills online – buy cytotec
ciprofloxacin order online cipro ciprofloxacin cipro for sale
buy depo-medrol tablets buy methylprednisolone pills methylprednisolone over counter
http://cytotec24.com/# buy cytotec in usa
http://doxycycline.auction/# where to purchase doxycycline
http://doxycycline.auction/# generic doxycycline
buy doxycycline 100mg doxycycline without a prescription buy cheap doxycycline online
https://cytotec24.com/# Misoprostol 200 mg buy online
http://cytotec24.shop/# Abortion pills online
http://diflucan.pro/# diflucan canada
buy cipro cheap ciprofloxacin buy ciprofloxacin over the counter
http://diflucan.pro/# diflucan 1140
https://nolvadex.guru/# nolvadex generic
diflucan canada coupon 150 mg diflucan online diflucan australia
http://doxycycline.auction/# 100mg doxycycline
http://cipro.guru/# п»їcipro generic
Angela White: Angela White video – Angela White video
college paper help write essay service how to write a letter to a hiring manager
http://angelawhite.pro/# ?????? ????
lana rhoades: lana rhoades modeli – lana rhodes
http://angelawhite.pro/# ?????? ????
https://lanarhoades.fun/# lana rhoades video
https://angelawhite.pro/# Angela Beyaz modeli
buy propranolol for sale inderal order online buy generic clopidogrel
lana rhoades izle: lana rhodes – lana rhoades
http://angelawhite.pro/# Angela White filmleri
http://lanarhoades.fun/# lana rhoades
https://angelawhite.pro/# Angela White video
Angela White filmleri: Angela White izle – Angela White video
https://evaelfie.pro/# eva elfie izle
https://abelladanger.online/# abella danger video
https://lanarhoades.fun/# lana rhoades
lana rhoades izle: lana rhoades – lana rhoades filmleri
http://lanarhoades.fun/# lana rhoades
http://angelawhite.pro/# Angela White
http://lanarhoades.fun/# lana rhoades filmleri
lana rhoades: lana rhoades video – lana rhodes
http://angelawhite.pro/# Angela White filmleri
http://evaelfie.pro/# eva elfie video
http://angelawhite.pro/# Angela White video
lana rhodes: lana rhodes – lana rhodes
https://sweetiefox.online/# swetie fox
order methotrexate 2.5mg pills order methotrexate 10mg online cheap buy coumadin 2mg pills
https://angelawhite.pro/# Angela Beyaz modeli
http://sweetiefox.online/# Sweetie Fox video
eva elfie izle: eva elfie modeli – eva elfie filmleri
bactrim ss
http://sweetiefox.online/# sweety fox
https://lanarhoades.fun/# lana rhodes
meloxicam 15mg usa celebrex pills buy generic celecoxib
lana rhoades video: lana rhodes – lana rhoades izle
https://sweetiefox.online/# Sweetie Fox video
https://abelladanger.online/# Abella Danger
http://lanarhoades.fun/# lana rhoades izle
https://sweetiefox.online/# sweeti fox
eva elfie modeli: eva elfie video – eva elfie modeli
http://angelawhite.pro/# Angela White
https://abelladanger.online/# abella danger izle
sweety fox: Sweetie Fox izle – Sweetie Fox izle
http://lanarhoades.fun/# lana rhoades filmleri
brand metoclopramide 20mg metoclopramide 20mg cheap losartan 25mg ca
http://lanarhoades.fun/# lana rhoades izle
http://lanarhoades.fun/# lana rhodes
https://angelawhite.pro/# Angela Beyaz modeli
eva elfie filmleri: eva elfie filmleri – eva elfie
http://abelladanger.online/# abella danger filmleri
https://evaelfie.pro/# eva elfie izle
Angela White filmleri: abella danger filmleri – Abella Danger
tamsulosin 0.2mg generic buy celecoxib 200mg online celecoxib order
https://abelladanger.online/# Abella Danger
https://miamalkova.life/# mia malkova new video
hot dating match: http://sweetiefox.pro/# sweetie fox full video
eva elfie full video: eva elfie new videos – eva elfie full videos
esomeprazole 20mg pills nexium 20mg pill order topamax 200mg generic
http://sweetiefox.pro/# ph sweetie fox
https://miamalkova.life/# mia malkova videos
sweetie fox: sweetie fox video – sweetie fox full video
lana rhoades full video: lana rhoades unleashed – lana rhoades hot
http://evaelfie.site/# eva elfie hot
best dating sites: https://sweetiefox.pro/# sweetie fox video
lana rhoades videos: lana rhoades hot – lana rhoades solo
http://sweetiefox.pro/# sweetie fox full
mia malkova hd: mia malkova new video – mia malkova girl
eva elfie videos: eva elfie videos – eva elfie photo
best dating sites: http://sweetiefox.pro/# sweetie fox full video
lana rhoades hot: lana rhoades pics – lana rhoades hot
https://evaelfie.site/# eva elfie new video
mia malkova: mia malkova latest – mia malkova hd
sweetie fox full: sweetie fox new – sweetie fox new
http://sweetiefox.pro/# fox sweetie
free dating apps: https://sweetiefox.pro/# sweetie fox video
mia malkova hd: mia malkova – mia malkova girl
order zofran 8mg online cheap order zofran generic brand aldactone 100mg
http://evaelfie.site/# eva elfie hot
mia malkova new video: mia malkova hd – mia malkova full video
sweetie fox full: sweetie fox new – fox sweetie
dating websites for free: https://lanarhoades.pro/# lana rhoades full video
eva elfie full video: eva elfie – eva elfie videos
https://miamalkova.life/# mia malkova videos
sumatriptan for sale brand levaquin 500mg levofloxacin 250mg without prescription
sweetie fox cosplay: ph sweetie fox – sweetie fox video
https://sweetiefox.pro/# sweetie fox full
mia malkova full video: mia malkova full video – mia malkova videos
indian dating: https://miamalkova.life/# mia malkova full video
buy zocor 10mg for sale buy generic zocor for sale buy valtrex generic
mia malkova only fans: mia malkova hd – mia malkova latest
http://sweetiefox.pro/# sweetie fox new
sweetie fox video: fox sweetie – sweetie fox
https://evaelfie.site/# eva elfie full videos
cost avodart buy avodart zantac over the counter
lana rhoades unleashed: lana rhoades solo – lana rhoades videos
mia malkova photos: mia malkova new video – mia malkova new video
online websites: https://sweetiefox.pro/# sweetie fox
http://miamalkova.life/# mia malkova hd
http://pinupcassino.pro/# pin up aviator
http://aviatorghana.pro/# aviator
aviator hilesi: pin up aviator – aviator bahis
aviator game: aviator pin up – aviator game
http://aviatormocambique.site/# jogar aviator
https://jogodeaposta.fun/# jogo de aposta online
aviator bet: como jogar aviator – aviator mz
aviator: aviator betting game – play aviator
https://jogodeaposta.fun/# deposito minimo 1 real
http://jogodeaposta.fun/# melhor jogo de aposta para ganhar dinheiro
play aviator: aviator – aviator betting game
play aviator: aviator – play aviator
acillin brand vibra-tabs brand purchase amoxicillin sale
http://jogodeaposta.fun/# aviator jogo de aposta
https://aviatorjogar.online/# aviator pin up
finasteride 5mg without prescription order fluconazole generic buy fluconazole 200mg without prescription
aviator login: aviator game online – aviator game online
aviator ghana: aviator game online – aviator login
https://pinupcassino.pro/# aviator pin up casino
aviator login: play aviator – aviator bet
http://aviatormocambique.site/# aviator online
como jogar aviator em moçambique: aviator moçambique – aviator bet
melhor jogo de aposta para ganhar dinheiro: jogo de aposta – aviator jogo de aposta
pin up bet: pin-up casino entrar – pin-up cassino
aviator bet: aviator betting game – aviator login
pin up aviator: pin-up casino login – aviator oficial pin up
aviator bahis: aviator bahis – aviator oyunu
https://aviatorjogar.online/# aviator jogo
aviator: aviator malawi – aviator bet malawi login
jogar aviator Brasil: aviator jogo – aviator jogar
zithromax for sale online – https://azithromycin.pro/zithromax-prices.html generic zithromax india
order ciprofloxacin 500mg sale – generic trimethoprim buy augmentin 625mg sale
aviator game: aviator bet – jogar aviator online
aviator hilesi: aviator bahis – aviator oyna
https://aviatorjogar.online/# aviator jogar
zithromax cost canada: zithromax cost uk – where to buy zithromax in canada
pin up cassino online: pin-up casino entrar – pin-up cassino
buy generic ciprofloxacin – buy augmentin 1000mg online cheap oral augmentin
https://aviatormalawi.online/# aviator
melhor jogo de aposta para ganhar dinheiro: jogo de aposta – jogo de aposta
generic zithromax azithromycin – https://azithromycin.pro/amoxicillin-vs-zithromax.html zithromax cost
http://mexicanpharm24.shop/# mexican drugstore online mexicanpharm.shop
mexican mail order pharmacies: mexican pharmacy – medicine in mexico pharmacies mexicanpharm.shop
onlinecanadianpharmacy Canada pharmacy online canada ed drugs canadianpharm.store
canadian pharmacy uk delivery: canadian pharmacy online store – canadian pharmacy 24 com canadianpharm.store
http://indianpharm24.shop/# best online pharmacy india indianpharm.store
Thanks for sharing. I read many of your blog posts, cool, your blog is very good.
indian pharmacy: indian pharmacy – Online medicine home delivery indianpharm.store
п»їlegitimate online pharmacies india Generic Medicine India to USA best online pharmacy india indianpharm.store
Online medicine order: online pharmacy in india – india online pharmacy indianpharm.store
http://indianpharm24.com/# best online pharmacy india indianpharm.store
http://canadianpharmlk.shop/# canada pharmacy world canadianpharm.store
http://indianpharm24.shop/# india pharmacy mail order indianpharm.store
canadian drugstore online: International Pharmacy delivery – cross border pharmacy canada canadianpharm.store
http://canadianpharmlk.shop/# best online canadian pharmacy canadianpharm.store
https://indianpharm24.shop/# buy prescription drugs from india indianpharm.store
http://indianpharm24.com/# reputable indian online pharmacy indianpharm.store
reputable indian online pharmacy: Online India pharmacy – Online medicine order indianpharm.store
https://mexicanpharm24.com/# mexican border pharmacies shipping to usa mexicanpharm.shop
india online pharmacy: cheapest online pharmacy – india pharmacy indianpharm.store
http://indianpharm24.shop/# india online pharmacy indianpharm.store
http://canadianpharmlk.shop/# canadian mail order pharmacy canadianpharm.store
ddavp black box warning
http://canadianpharmlk.shop/# pharmacies in canada that ship to the us canadianpharm.store
https://mexicanpharm24.com/# best online pharmacies in mexico mexicanpharm.shop
cost flagyl 400mg – order cleocin 150mg pills order zithromax 500mg pill
http://indianpharm24.com/# top online pharmacy india indianpharm.store
https://canadianpharmlk.com/# canadian online drugs canadianpharm.store
best canadian online pharmacy: canadian pharmacy – canadian pharmacy 365 canadianpharm.store
http://mexicanpharm24.shop/# mexican mail order pharmacies mexicanpharm.shop
buying prescription drugs in mexico mexican pharmacy buying prescription drugs in mexico mexicanpharm.shop
http://indianpharm24.com/# cheapest online pharmacy india indianpharm.store
https://indianpharm24.com/# best india pharmacy indianpharm.store
indian pharmacy paypal: Top online pharmacy in India – online pharmacy india indianpharm.store
https://indianpharm24.shop/# top 10 online pharmacy in india indianpharm.store
top online pharmacy india: buy medicines online in india – india pharmacy indianpharm.store
http://canadianpharmlk.shop/# canadian family pharmacy canadianpharm.store
https://mexicanpharm24.shop/# mexican online pharmacies prescription drugs mexicanpharm.shop
Contra vim mortis non est medicamen in hortis — Против силы смерти в садах нет лекарств.
https://canadianpharmlk.shop/# my canadian pharmacy canadianpharm.store
http://mexicanpharm24.com/# mexican drugstore online mexicanpharm.shop
canadian pharmacy world reviews: Canadian pharmacy prices – medication canadian pharmacy canadianpharm.store
http://indianpharm24.shop/# buy prescription drugs from india indianpharm.store
purchase ciplox online – chloromycetin order erythromycin 500mg generic
cortisol prednisone: 1250 mg prednisone – can you buy prednisone online uk
can i purchase amoxicillin online can you buy amoxicillin over the counter in canada ampicillin amoxicillin
amoxicillin 500mg over the counter: amoxicillin 500 – amoxicillin 500mg tablets price in india
http://clomidst.pro/# can i purchase clomid now
cheap clomid for sale: clomid 100mg success rate – how to get cheap clomid for sale
buy generic clomid without insurance: taking clomid – where buy generic clomid no prescription
how much is amoxicillin prescription: antibiotic amoxicillin – buy amoxicillin canada
where can i buy generic clomid without a prescription: how to buy clomid online – buying generic clomid without insurance
https://clomidst.pro/# buying clomid tablets
can you buy clomid: can you get clomid price – how to buy cheap clomid online
amoxacillian without a percription order amoxicillin online uk amoxicillin online without prescription
cost clomid pills: clomid manufacturer coupon – cheap clomid without dr prescription
buying generic clomid without insurance: where buy generic clomid prices – how can i get clomid price
http://amoxilst.pro/# purchase amoxicillin online without prescription
can you buy prednisone over the counter in mexico: prednisone 20 mg prices – prednisone for sale in canada
amoxicillin 500mg over the counter: fish amoxicillin – amoxicillin 500mg buy online canada
buy generic valacyclovir for sale – mebendazole 100mg oral order zovirax 400mg pill
prednisone for sale without a prescription: prednisone 20 mg dosage instructions – buying prednisone mexico
https://amoxilst.pro/# amoxacillian without a percription
order amoxicillin no prescription: amoxicillin uses – amoxicillin 30 capsules price
buy amoxicillin online uk: how long do amoxicillin side effects last – amoxicillin 500 mg without prescription
prednisone 20mg buy online: prednisone high – 400 mg prednisone
amoxicillin 250 mg capsule: can we buy amoxcillin 500mg on ebay without prescription – amoxicillin 500mg pill
http://amoxilst.pro/# amoxicillin online purchase
where can i buy amoxicillin online amoxicillin 500mg pill amoxicillin 500mg tablets price in india
buy amoxicillin without prescription: amoxicillin for tooth infection – amoxicillin online canada
buy amoxil: buy amoxicillin online cheap – amoxicillin generic
amoxicillin 500mg capsules uk: amoxil suspension – where to buy amoxicillin 500mg
https://clomidst.pro/# generic clomid without dr prescription
amoxicillin 775 mg: what is amoxicillin used for – amoxicillin buy no prescription
Ad usum delphini — Для использования дофином.
where to buy stromectol online – buy aczone no prescription buy sumycin 500mg online cheap
https://edpills.guru/# ed pills for sale
best no prescription online pharmacy: canadian prescription – online pharmacies no prescription
online pharmacy canada no prescription: buy medication online with prescription – medications online without prescriptions
where can i buy ed pills: ed meds cheap – cheapest ed meds
https://onlinepharmacy.cheap/# canadian pharmacy coupon code
http://edpills.guru/# ed medicine online
buy ed pills: ed medicine online – ed pills for sale
pharmacies without prescriptions pharmacy no prescription best no prescription online pharmacy
canadian pharmacy coupon code: mexican online pharmacy – canadian prescription pharmacy
canadian pharmacy no prescription: buying prescription drugs online without a prescription – buy medications online no prescription
https://pharmnoprescription.pro/# best online pharmacy without prescription
pharmacy discount coupons: online pharmacy delivery – canadian pharmacy no prescription
http://pharmnoprescription.pro/# mexican prescription drugs online
online erectile dysfunction medication: online erectile dysfunction medication – low cost ed medication
online pharmacy prescription: online pharmacy delivery – drugstore com online pharmacy prescription drugs
http://onlinepharmacy.cheap/# canadian prescription pharmacy
can you buy prescription drugs in canada: buying prescription drugs online canada – best online prescription
buy metronidazole 400mg without prescription – metronidazole 400mg uk azithromycin 500mg without prescription
best ed meds online: buy erectile dysfunction medication – ed pills
https://pharmnoprescription.pro/# online pharmacy no prescription needed
low cost ed meds online ed pills cheap online prescription for ed
https://edpills.guru/# best online ed meds
best online pharmacy without prescription: no prescription medicines – buy prescription drugs on line
cheapest pharmacy for prescription drugs: online pharmacy – cheapest pharmacy prescription drugs
online canadian pharmacy coupon: Best online pharmacy – online pharmacy discount code
http://pharmnoprescription.pro/# canadian pharmacy online no prescription needed
online drugstore no prescription: meds online no prescription – online doctor prescription canada
canadian mail order pharmacy: canadian compounding pharmacy – best canadian online pharmacy reviews
canada pharmacy reviews canadianpharmacymeds com canadian pharmacy drugs online
order ampicillin without prescription order amoxicillin pill oral amoxil
Online medicine home delivery: indian pharmacies safe – Online medicine order
https://mexicanpharm.online/# buying prescription drugs in mexico online
http://canadianpharm.guru/# legitimate canadian pharmacy online
online pharmacy without prescription: canada online prescription – canadian pharmacy no prescription
buying prescription drugs in mexico: п»їbest mexican online pharmacies – mexican pharmacy
http://pharmacynoprescription.pro/# best non prescription online pharmacy
77 canadian pharmacy canadian pharmacy drugs online best rated canadian pharmacy
buy lasix 40mg generic – buy warfarin pills for sale buy capoten pills for sale
indian pharmacy online: top online pharmacy india – mail order pharmacy india
online pharmacy without prescriptions: no prescription – canadian prescription drugstore reviews
buy medications online no prescription: prescription drugs online canada – online meds no prescription
https://pharmacynoprescription.pro/# best online pharmacy that does not require a prescription in india
online shopping pharmacy india: reputable indian online pharmacy – Online medicine order
pharmacy website india: reputable indian pharmacies – indianpharmacy com
http://mexicanpharm.online/# reputable mexican pharmacies online
top online pharmacy india: top online pharmacy india – indian pharmacy paypal
pharmacy no prescription required: canada pharmacies online prescriptions – no prescription pharmacy online
canadian pharmacy 24h com canadapharmacyonline com canadian 24 hour pharmacy
mexican pharmacy: best online pharmacies in mexico – pharmacies in mexico that ship to usa
https://pharmacynoprescription.pro/# buy medication online no prescription
online pharmacy that does not require a prescription: quality prescription drugs canada – no prescription canadian pharmacies
https://indianpharm.shop/# best india pharmacy
mexican pharmacy: mexican rx online – reputable mexican pharmacies online
mexico pharmacy: п»їbest mexican online pharmacies – purple pharmacy mexico price list
no prescription on line pharmacies: legitimate online pharmacy no prescription – buying prescription drugs online from canada
https://mexicanpharm.online/# medication from mexico pharmacy
canada rx pharmacy: legal canadian pharmacy online – canada drugs online review
purple pharmacy mexico price list: pharmacies in mexico that ship to usa – mexican rx online
https://indianpharm.shop/# п»їlegitimate online pharmacies india
mexican border pharmacies shipping to usa: buying prescription drugs in mexico online – mexican border pharmacies shipping to usa
buy medications online without prescription online pharmacy without a prescription prescription meds from canada
buy medicines online in india: buy medicines online in india – best india pharmacy
how to get a prescription in canada: online pharmacy no prescription – buy prescription drugs without a prescription
http://mexicanpharm.online/# buying prescription drugs in mexico
https://indianpharm.shop/# online pharmacy india
no prescription on line pharmacies: buy prescription drugs online without doctor – best online pharmacy without prescriptions
canadian pharmacy cheap: canadian neighbor pharmacy – canadianpharmacymeds
best rated canadian pharmacy: best rated canadian pharmacy – legal canadian pharmacy online
https://indianpharm.shop/# reputable indian pharmacies
online medication without prescription: canadian prescription drugstore reviews – online drugs without prescription
indian pharmacies safe: cheapest online pharmacy india – Online medicine home delivery
reliable canadian online pharmacy: legitimate canadian online pharmacies – onlinepharmaciescanada com
http://pharmacynoprescription.pro/# order prescription drugs online without doctor
indian pharmacy online top 10 online pharmacy in india india online pharmacy
top online pharmacy india: Online medicine home delivery – top 10 online pharmacy in india
online pharmacy india: Online medicine home delivery – top online pharmacy india
cheapest online pharmacy india: top online pharmacy india – п»їlegitimate online pharmacies india
http://pharmacynoprescription.pro/# no prescription needed
canadian pharmacy india: reputable canadian online pharmacies – vipps approved canadian online pharmacy
http://canadianpharm.guru/# canadian pharmacy
canada drugs: canada drugstore pharmacy rx – pharmacy in canada
canada drug pharmacy: canadian discount pharmacy – online canadian drugstore
https://mexicanpharm.online/# reputable mexican pharmacies online
glucophage generic – purchase epivir generic buy lincocin 500mg online
mexican drugstore online: mexican drugstore online – purple pharmacy mexico price list
buy medication online with prescription: online medication no prescription – prescription canada
buy medications without a prescription: canadian prescription drugstore reviews – online pharmacy without prescriptions
how to order prescription drugs from canada buy medication online no prescription buy pills without prescription
retrovir 300mg without prescription – buy allopurinol 100mg without prescription allopurinol 300mg usa
http://mexicanpharm.online/# medicine in mexico pharmacies
adderall canadian pharmacy: canadian world pharmacy – canadian pharmacy uk delivery
canadian pharmacy service: canadian pharmacy meds – canadian pharmacy meds
http://indianpharm.shop/# best online pharmacy india
online canadian pharmacy no prescription: quality prescription drugs canada – online medication no prescription
http://canadianpharm.guru/# canadian pharmacy phone number
cheap prescription drugs online: canada online prescription – canadian prescription prices
canadian king pharmacy: canadian pharmacy 1 internet online drugstore – legitimate canadian pharmacy online
online pharmacy reviews no prescription: how to buy prescriptions from canada safely – buy medication online with prescription
https://canadianpharm.guru/# canada drugs reviews
sweet bonanza hilesi: sweet bonanza 100 tl – sweet bonanza kazanc
https://pinupgiris.fun/# pin up casino indir
http://slotsiteleri.guru/# deneme veren slot siteleri
sweet bonanza hilesi: pragmatic play sweet bonanza – sweet bonanza kazanc
https://sweetbonanza.bid/# sweet bonanza yasal site
sweet bonanza demo turkce: sweet bonanza indir – sweet bonanza slot demo
https://sweetbonanza.bid/# sweet bonanza kazanma saatleri
https://sweetbonanza.bid/# slot oyunlari
pin up casino guncel giris: aviator pin up – pin up casino guncel giris
http://gatesofolympus.auction/# gates of olympus demo oyna
gates of olympus demo turkce: gates of olympus oyna ucretsiz – gates of olympus taktik
http://sweetbonanza.bid/# sweet bonanza slot demo
gates of olympus demo: gates of olympus – gates of olympus demo turkce oyna
http://aviatoroyna.bid/# aviator oyunu
http://gatesofolympus.auction/# gates of olympus max win
buy clozaril 100mg generic – order amaryl 4mg for sale pepcid online buy
https://slotsiteleri.guru/# slot oyun siteleri
gates of olympus demo turkce oyna: gate of olympus hile – gate of olympus hile
sweet bonanza: sweet bonanza mostbet – sweet bonanza nas?l oynan?r
http://sweetbonanza.bid/# güncel sweet bonanza
gates of olympus demo oyna: gates of olympus max win – gates of olympus oyna
https://aviatoroyna.bid/# aviator sinyal hilesi ücretsiz
https://aviatoroyna.bid/# aviator sinyal hilesi
pin up bet: pin up giris – pin up guncel giris
https://slotsiteleri.guru/# slot kumar siteleri
http://pinupgiris.fun/# pin up casino
quetiapine cost – order zoloft online order eskalith online
slot casino siteleri: guvenilir slot siteleri – bonus veren casino slot siteleri
http://pinupgiris.fun/# pin-up bonanza
deneme bonusu veren siteler: guvenilir slot siteleri 2024 – slot siteleri
http://slotsiteleri.guru/# canli slot siteleri
2024 en iyi slot siteleri: bonus veren slot siteleri – en iyi slot siteleri 2024
https://pinupgiris.fun/# pin up casino
sweet bonanza demo oyna: guncel sweet bonanza – sweet bonanza taktik
gate of olympus hile: gates of olympus giris – gates of olympus demo
http://gatesofolympus.auction/# gates of olympus guncel
indian pharmacy: indian pharmacy delivery – mail order pharmacy india
http://canadianpharmacy24.store/# canada drug pharmacy
real canadian pharmacy Certified Canadian Pharmacy online canadian drugstore
canadapharmacyonline legit: Licensed Canadian Pharmacy – reputable canadian online pharmacies
canadian drug pharmacy: canadian pharmacy near me – canadian pharmacy phone number
world pharmacy india indian pharmacy delivery cheapest online pharmacy india
reputable canadian pharmacy: Certified Canadian Pharmacy – canadian drug
canadian pharmacy 365: Prescription Drugs from Canada – recommended canadian pharmacies
canadian pharmacy no scripts Certified Canadian Pharmacy canadian pharmacy
buy anafranil online cheap – order citalopram 20mg online buy doxepin 25mg pills
best india pharmacy: Healthcare and medicines from India – reputable indian pharmacies
order atarax 10mg pill – buy endep 10mg online order endep online cheap
top 10 pharmacies in india: indian pharmacy – pharmacy website india
mexico pharmacy: mexican pharmacy – pharmacies in mexico that ship to usa
buy prescription drugs from india: Cheapest online pharmacy – india online pharmacy
world pharmacy india: indian pharmacy – world pharmacy india
canadian pharmacy phone number Prescription Drugs from Canada canadian pharmacy prices
https://canadianpharmacy24.store/# drugs from canada
mexican border pharmacies shipping to usa: Mexican Pharmacy Online – mexico pharmacy
canadian pharmacy uk delivery: pills now even cheaper – my canadian pharmacy
mexican drugstore online Online Pharmacies in Mexico mexican online pharmacies prescription drugs
top 10 pharmacies in india: indian pharmacy delivery – india pharmacy mail order
canadian pharmacy price checker: canadian pharmacy review – www canadianonlinepharmacy
mexican rx online: cheapest mexico drugs – purple pharmacy mexico price list
online canadian pharmacy reviews: my canadian pharmacy – canadian 24 hour pharmacy
indian pharmacy paypal india pharmacy indianpharmacy com
reputable indian online pharmacy: indian pharmacy delivery – reputable indian pharmacies
pharmacy website india mail order pharmacy india pharmacy website india
best online canadian pharmacy: pills now even cheaper – canadian pharmacy victoza
mexico drug stores pharmacies mexico pharmacy mexican mail order pharmacies
buy prescription drugs from india: Healthcare and medicines from India – online pharmacy india
mexican pharmacy: mexican pharmacy – buying from online mexican pharmacy
canada pharmacy world: Large Selection of Medications – my canadian pharmacy
legitimate canadian mail order pharmacy Licensed Canadian Pharmacy canadian pharmacy uk delivery
https://mexicanpharmacy.shop/# п»їbest mexican online pharmacies
http://clomidall.com/# where can i get clomid tablets
prednisone buying prednisone 50 mg canada how much is prednisone 10mg
http://zithromaxall.com/# buy zithromax 500mg online
can you buy cheap clomid without dr prescription: where can i get clomid prices – how to get cheap clomid price
zithromax 500 mg lowest price online where to get zithromax zithromax capsules
https://clomidall.shop/# can you get cheap clomid without insurance
http://prednisoneall.com/# drug prices prednisone
http://zithromaxall.shop/# zithromax over the counter uk
where to buy zithromax in canada zithromax 500 mg zithromax prescription
http://prednisoneall.com/# how much is prednisone 10mg
i love your work well done keeeeep it upzzzz
zithromax online usa zithromax 500 tablet where can i buy zithromax uk
http://zithromaxall.com/# zithromax prescription in canada
http://zithromaxall.com/# zithromax antibiotic without prescription
http://clomidall.com/# how to buy clomid online
price of amoxicillin without insurance amoxicillin 500 mg over the counter amoxicillin canada
amoxicillin 500 mg without a prescription: amoxicillin 500 mg without a prescription – amoxicillin 500 mg online
order amoxicillin pill – oral keflex 500mg buy generic ciprofloxacin 1000mg
https://prednisoneall.com/# prednisone 2.5 mg cost
amoxicillin 500 capsule amoxicillin 500 mg for sale rexall pharmacy amoxicillin 500mg
https://prednisoneall.com/# prednisone 5084
http://clomidall.com/# cost cheap clomid without insurance
can i buy prednisone over the counter in usa: prednisone where can i buy – buy prednisone 50 mg
order amoxicillin online uk cheap amoxicillin 500mg over the counter amoxicillin
http://amoxilall.shop/# amoxicillin price canada
amoxiclav sale – order bactrim 480mg sale cipro 500mg ca
https://clomidall.shop/# can you get generic clomid for sale
where can i buy amoxicillin over the counter amoxicillin 250 mg amoxicillin 500 mg tablet
how can i get clomid tablets: how can i get generic clomid for sale – can i buy cheap clomid no prescription
http://amoxilall.shop/# amoxicillin online purchase
https://clomidall.com/# where can i get clomid prices
how can i get cheap clomid without insurance can i purchase clomid tablets order cheap clomid without dr prescription
http://zithromaxall.com/# generic zithromax india
https://zithromaxall.shop/# zithromax z-pak
generic clomid: can i get clomid without insurance – cost generic clomid without a prescription
http://kamagraiq.shop/# Kamagra 100mg
buy Viagra online: cheapest viagra – best price for viagra 100mg
Cialis without a doctor prescription Generic Tadalafil 20mg price Tadalafil price
order viagra: viagra canada – Sildenafil Citrate Tablets 100mg
buy kamagra online usa Kamagra Oral Jelly Price buy Kamagra
https://kamagraiq.shop/# super kamagra
Buy Tadalafil 20mg: Buy Cialis online – Generic Tadalafil 20mg price
Buy Cialis online: cialis best price – Cialis without a doctor prescription
Generic Viagra online: buy viagra online – Cheap Sildenafil 100mg
sildenafil oral jelly 100mg kamagra Kamagra Oral Jelly Price Kamagra 100mg price
https://kamagraiq.com/# sildenafil oral jelly 100mg kamagra
buy Kamagra: Kamagra Oral Jelly Price – cheap kamagra
Kamagra 100mg price Kamagra Oral Jelly Price cheap kamagra
Cialis 20mg price: cheapest cialis – Buy Tadalafil 10mg
http://sildenafiliq.com/# Order Viagra 50 mg online
Cialis 20mg price in USA: tadalafil iq – Generic Cialis without a doctor prescription
Kamagra 100mg price: sildenafil oral jelly 100mg kamagra – cheap kamagra
http://kamagraiq.com/# buy kamagra online usa
sildenafil oral jelly 100mg kamagra Kamagra Iq buy kamagra online usa
Viagra online price: viagra without prescription – Cheap Viagra 100mg
https://sildenafiliq.com/# Cheapest Sildenafil online
Viagra Tablet price: cheapest viagra – cheapest viagra
Cialis 20mg price in USA Tadalafil price Tadalafil Tablet
http://sildenafiliq.xyz/# Viagra Tablet price
http://kamagraiq.shop/# Kamagra Oral Jelly
Kamagra 100mg price: kamagra – buy kamagra online usa
http://tadalafiliq.com/# Tadalafil Tablet
over the counter sildenafil buy viagra online order viagra
Kamagra 100mg price: Kamagra tablets – Kamagra 100mg price
https://sildenafiliq.xyz/# Cheap generic Viagra
Kamagra 100mg: kamagra best price – super kamagra
Cheap Viagra 100mg: sildenafil iq – sildenafil online
buy kamagra online usa Kamagra Oral Jelly Price Kamagra tablets
buy Viagra over the counter: buy viagra here – Buy generic 100mg Viagra online
https://tadalafiliq.shop/# Tadalafil Tablet
buy Viagra online: best price on viagra – sildenafil 50 mg price
Cialis 20mg price in USA cialis without a doctor prescription Cialis 20mg price
http://sildenafiliq.xyz/# Viagra online price
Buy Tadalafil 10mg: cialis best price – Generic Tadalafil 20mg price
http://sildenafiliq.xyz/# generic sildenafil
https://kamagraiq.com/# Kamagra 100mg price
sildenafil over the counter generic ed pills viagra without prescription
http://kamagraiq.com/# sildenafil oral jelly 100mg kamagra
Kamagra 100mg price: kamagra best price – Kamagra 100mg price
reputable indian online pharmacy: Generic Medicine India to USA – india pharmacy mail order
top 10 online pharmacy in india: Generic Medicine India to USA – indian pharmacy paypal
buy medicines online in india top 10 online pharmacy in india online shopping pharmacy india
https://canadianpharmgrx.xyz/# canadian pharmacy online store
http://canadianpharmgrx.com/# onlinepharmaciescanada com
purple pharmacy mexico price list: mexican pharmacy – mexico drug stores pharmacies
mexico pharmacy medication from mexico pharmacy best online pharmacies in mexico
buy prescription drugs from india: indian pharmacy – mail order pharmacy india
http://canadianpharmgrx.com/# legal to buy prescription drugs from canada
mexican pharmaceuticals online: mexican pharmacy – reputable mexican pharmacies online
buying from online mexican pharmacy mexico pharmacy medication from mexico pharmacy
http://indianpharmgrx.shop/# pharmacy website india
http://indianpharmgrx.com/# buy medicines online in india
cleocin 300mg us – chloromycetin over the counter buy generic chloromycetin for sale
mexico drug stores pharmacies: online pharmacy in Mexico – reputable mexican pharmacies online
http://canadianpharmgrx.com/# canadian pharmacy com
mexican online pharmacies prescription drugs: mexico drug stores pharmacies – reputable mexican pharmacies online
http://canadianpharmgrx.xyz/# canadian pharmacy 24h com safe
purple pharmacy mexico price list Pills from Mexican Pharmacy mexican rx online
my canadian pharmacy: Canada pharmacy – canadian pharmacy ed medications
canadian pharmacies that deliver to the us: canadian pharmacy – canadian neighbor pharmacy
https://canadianpharmgrx.xyz/# canadian pharmacy reviews
canadian pharmacy antibiotics My Canadian pharmacy legit canadian pharmacy
http://canadianpharmgrx.xyz/# cheap canadian pharmacy
http://mexicanpharmgrx.com/# best mexican online pharmacies
best online pharmacy india: Healthcare and medicines from India – top 10 online pharmacy in india
best canadian pharmacy to buy from canadian pharmacy king canadian drugs pharmacy
azithromycin 250mg sale – generic metronidazole 400mg ciprofloxacin online buy
cheapest online pharmacy india: Generic Medicine India to USA – world pharmacy india
https://canadianpharmgrx.xyz/# best canadian pharmacy
indianpharmacy com: Generic Medicine India to USA – buy prescription drugs from india
http://mexicanpharmgrx.com/# buying prescription drugs in mexico online
indian pharmacy Healthcare and medicines from India top 10 pharmacies in india
http://mexicanpharmgrx.com/# medicine in mexico pharmacies
mail order pharmacy india: Healthcare and medicines from India – world pharmacy india
http://mexicanpharmgrx.shop/# mexico drug stores pharmacies
safe canadian pharmacies Canada pharmacy canadian pharmacy checker
diflucan 15 mg: diflucan online – diflucan 6 tabs
http://ciprofloxacin.guru/# cipro online no prescription in the usa
cipro generic: purchase cipro – ciprofloxacin 500mg buy online
cytotec online: cytotec abortion pill – Abortion pills online
buy generic ciprofloxacin buy cipro online buy cipro online without prescription
purchase cytotec: purchase cytotec – Misoprostol 200 mg buy online
diflucan online buy: ordering diflucan generic – can you buy diflucan otc
cipro ciprofloxacin order online where can i buy cipro online
diflucan canada online: diflucan 125mg – diflucan generic price
does tamoxifen make you tired: tamoxifen alternatives premenopausal – alternatives to tamoxifen
http://doxycyclinest.pro/# doxycycline monohydrate
diflucan pill: diflucan.com – diflucan 15 mg
buy cipro online ciprofloxacin generic buy ciprofloxacin
buy generic doxycycline: price of doxycycline – doxycycline hydrochloride 100mg
nolvadex generic: tamoxifen and grapefruit – where to buy nolvadex
Abortion pills online order cytotec online cytotec online
how to order doxycycline: order doxycycline online – doxy 200
cytotec buy online usa: Cytotec 200mcg price – п»їcytotec pills online
vibramycin 100 mg doxycycline without prescription order doxycycline 100mg without prescription
ciprofloxacin: cipro generic – buy cipro online
doxycycline vibramycin: 200 mg doxycycline – doxycycline generic
https://misoprostol.top/# Misoprostol 200 mg buy online
buy cipro online without prescription buy cipro online without prescription п»їcipro generic
cheap ventolin 2mg – theo-24 Cr online buy theophylline 400 mg without prescription
odering doxycycline: order doxycycline 100mg without prescription – doxycycline 100mg tablets
cost stromectol – stromectol tablets buy cefaclor 250mg online cheap
can you buy diflucan over the counter in mexico: diflucan 100 mg – diflucan 150 tab
diflucan tablets buy online no script: diflucan 6 tablets – diflucan pills for sale
buy ciprofloxacin over the counter antibiotics cipro cipro pharmacy
buy doxycycline online without prescription: buy cheap doxycycline – buy doxycycline online uk
cytotec buy online usa: cytotec online – buy misoprostol over the counter
doxycycline generic for doxycycline doxycycline 100mg dogs
buy cytotec over the counter: cytotec abortion pill – buy cytotec online fast delivery
buy ciprofloxacin: п»їcipro generic – ciprofloxacin generic
http://diflucan.icu/# diflucan over the counter pill
diflucan 1 pill can you diflucan over the counter buy diflucan online
tamoxifen menopause: nolvadex pills – tamoxifen citrate
nolvadex gynecomastia: nolvadex vs clomid – is nolvadex legal
cytotec abortion pill: purchase cytotec – buy cytotec pills
cytotec online buy cytotec over the counter buy cytotec online
zithromax 500 mg for sale: zithromax 250 mg tablet price – average cost of generic zithromax
where can you buy amoxicillin over the counter: how to get amoxicillin – how much is amoxicillin prescription
how to get generic clomid pills: where can i buy generic clomid now – can i purchase generic clomid without prescription
get cheap clomid without dr prescription where buy clomid without dr prescription where can i buy cheap clomid no prescription
clomid prices: where can i buy clomid – cost cheap clomid without dr prescription
prednisone 20mg capsule buy prednisone online australia buy prednisone from canada
http://prednisonea.store/# prednisone price south africa
ivermectin rx: ivermectin lotion price – stromectol 3 mg dosage
amoxicillin 250 mg price in india: buying amoxicillin in mexico – buy amoxicillin online uk
https://prednisonea.store/# prednisone daily
buy amoxicillin 500mg online: rexall pharmacy amoxicillin 500mg – antibiotic amoxicillin
http://stromectola.top/# ivermectin eye drops
amoxicillin without prescription: can you buy amoxicillin over the counter in canada – amoxicillin 500 mg capsule
amoxicillin 500mg no prescription: amoxicillin azithromycin – where to buy amoxicillin
cost generic clomid now: can i order generic clomid – how can i get generic clomid for sale
where to get prednisone prednisone 5 mg tablet price 1 mg prednisone cost
order clomid without a prescription: clomid otc – get generic clomid pills
http://stromectola.top/# stromectol 6 mg tablet
clarinex medication – beclamethasone nasal sprays albuterol 2mg cheap
india buy prednisone online: how to buy prednisone – purchase prednisone 10mg
prednisone canada pharmacy buy prednisone 10mg online purchase prednisone
http://onlinepharmacyworld.shop/# pharmacy no prescription required
http://onlinepharmacyworld.shop/# canadian prescription pharmacy
what is the cheapest ed medication: best online ed treatment – get ed meds online
canadian pharmacy no prescription: canadian pharmacy coupon code – drugstore com online pharmacy prescription drugs
https://onlinepharmacyworld.shop/# canadian online pharmacy no prescription
http://medicationnoprescription.pro/# mail order prescriptions from canada
https://edpill.top/# online prescription for ed
canada pharmacies online prescriptions canada pharmacy no prescription cheap drugs no prescription
http://edpill.top/# ed prescription online
methylprednisolone 16mg oral – methylprednisolone canada buy azelastine 10ml without prescription
online pharmacy no prescription needed: international pharmacy no prescription – canadian pharmacy no prescription
отмечу как доверительного союзника в SEO-развитии.
https://onlinepharmacyworld.shop/# canadian pharmacy no prescription
order ed pills get ed meds today where can i buy ed pills
rybelsus and sitagliptin
buying prescription drugs online canada: online drugs no prescription – best online pharmacy no prescription
http://onlinepharmacyworld.shop/# legal online pharmacy coupon code
https://medicationnoprescription.pro/# best no prescription online pharmacies
non prescription medicine pharmacy: uk pharmacy no prescription – pharmacy coupons
http://edpill.top/# ed medicines online
pharmacy discount coupons: canada pharmacy not requiring prescription – canadian pharmacy discount code
mexican pharmacies no prescription mail order prescriptions from canada online pharmacy reviews no prescription
http://edpill.top/# ed drugs online
https://onlinepharmacyworld.shop/# online pharmacy discount code
erection pills online: how to get ed meds online – where to buy erectile dysfunction pills
https://medicationnoprescription.pro/# canada drugs without prescription
https://onlinepharmacyworld.shop/# best online pharmacy no prescription
casino tr?c tuy?n vi?t nam game c? b?c online uy tin casino tr?c tuy?n uy tin
https://casinvietnam.shop/# casino tr?c tuy?n vi?t nam
buy micronase 5mg sale – brand micronase buy dapagliflozin 10mg generic
casino online uy tin casino tr?c tuy?n casino tr?c tuy?n vi?t nam
casino tr?c tuy?n casino online uy tin choi casino tr?c tuy?n tren di?n tho?i
http://casinvietnam.shop/# casino online uy tin
casino tr?c tuy?n uy tín: casino online uy tín – choi casino tr?c tuy?n trên di?n tho?i
I’ll show you how to craft effective social copy for your business that’s SEO-friendly and tailored to each individual social media platform – while remaining true to your brand voice. It all depends on the copywriting project you have in mind. However, experienced copywriters should have the following skills: Easy process to hire the best social media experts for the job. VIP support from hiring to management and strategy. You meet our expectations if you possess: **NOTE: Please provide a sample of your previous work or experience with writing tweet threads AND LinkedIn posts. Otherwise, your application will not be reviewed or considered. Anyword’s AI writing assistant drives more conversions and sales using data and robust predictive analytics. Marketers using Anyword see an average increase of 30% in conversion rates.
https://bitcointalk.org/index.php?topic=4159695.0
CHARLESTON, W.Va. (AP) — West Virginia Gov. Jim Justice on Monday ordered a sweeping investigation of the State Police after he accepted the resignation of the agency’s superintendent and revealed allegations of wrongdoing, including that a video camera was placed inside a women’s locker … .css-as7amhAll 33 WELCH, W.Va. – American Legion Post 8, Welch, WV, under the leadership of Commander Jan .css-as7amhAll 33 WVNS 59 Beckley is owned by West Virginia Media Holdings. It is an affiliate of the network CBS network. As an affiliate, Beckley CBS tends to focus its original news coverage on local issues during the traditional morning, mid-day, evening and late-night news slots. To fill in the rest of its broadcasting schedule, the station airs national programs provided by CBS.
pill repaglinide 2mg – prandin 1mg for sale empagliflozin 25mg ca
glucophage 500mg cheap – order metformin 1000mg online precose cost
purchase lamisil generic – where can i buy terbinafine grifulvin v pill
rybelsus 14mg for sale – generic DDAVP purchase DDAVP sale
nizoral 200 mg without prescription – buy itraconazole without a prescription order itraconazole online cheap
психолог официальный сайт https://w-495.ru/
medicine in mexico pharmacies: cheapest mexico drugs – buying prescription drugs in mexico
pharmacy website india http://indiaph24.store/# top 10 pharmacies in india
buy prescription drugs from india
п»їlegitimate online pharmacies india reputable indian pharmacies reputable indian pharmacies
http://indiaph24.store/# mail order pharmacy india
https://finasteride.store/# buy propecia price
http://nolvadex.life/# should i take tamoxifen
famvir pill – order valaciclovir 1000mg online cheap purchase valaciclovir online cheap
order generic propecia price cost of propecia without a prescription order generic propecia without insurance
oral digoxin – order generic lanoxin 250 mg furosemide pills
order propecia without a prescription: propecia no prescription – generic propecia price
https://nolvadex.life/# tamoxifen alternatives
cheap lisinopril: lisinopril 20mg 25mg – zestril discount
https://nolvadex.life/# where can i buy nolvadex
https://finasteride.store/# order propecia tablets
buy cytotec pills: buy cytotec over the counter – order cytotec online
http://ciprofloxacin.tech/# ciprofloxacin over the counter
buy propecia without a prescription propecia medication cost propecia prices
purchase cytotec: cytotec pills buy online – buy cytotec over the counter
https://cytotec.club/# cytotec abortion pill
lisinopril 25 mg cost cost of lisinopril 30 mg lisinopril 20mg pill
http://lisinopril.network/# zestril 10 mg online
cytotec buy online usa: buy cytotec online – Misoprostol 200 mg buy online
http://finasteride.store/# cost generic propecia tablets
buy prinivil buy lisinopril 20 mg online usa lisinopril 40 mg tablets
ciprofloxacin generic price: buy cipro online – ciprofloxacin mail online
http://lisinopril.network/# lisinopril brand name uk
microzide 25 mg ca – buy cheap bisoprolol order generic zebeta 5mg
http://ciprofloxacin.tech/# purchase cipro
cost cheap propecia without a prescription: cost of propecia without prescription – order generic propecia price
tamoxifen bone density tamoxifen dosage tamoxifen therapy
http://cytotec.club/# cytotec pills buy online
п»їcipro generic cipro 500mg best prices buy cipro online
https://lisinopril.network/# lisinopril online
buy cytotec in usa: cytotec online – buy cytotec online
http://finasteride.store/# buy cheap propecia online
buy cytotec in usa: cytotec pills buy online – buy cytotec online fast delivery
http://nolvadex.life/# tamoxifen bone pain
metoprolol 100mg generic – losartan 50mg cheap oral adalat 30mg
cost of cheap propecia without dr prescription buy propecia without a prescription buying generic propecia without prescription
https://finasteride.store/# get generic propecia without a prescription
buy cipro online without prescription: antibiotics cipro – ciprofloxacin
https://cenforce.pro/# Cenforce 150 mg online
https://cenforce.pro/# buy cenforce
cenforce for sale Cenforce 100mg tablets for sale cheapest cenforce
buy Viagra online: Buy Viagra online – Generic Viagra for sale
buy nitroglycerin cheap – indapamide 2.5mg without prescription purchase diovan pills
https://cialist.pro/# Buy Tadalafil 5mg
cheap viagra: Buy generic 100mg Viagra online – Viagra online price
Cenforce 100mg tablets for sale cheapest cenforce Cenforce 150 mg online
sildenafil oral jelly 100mg kamagra: kamagra.win – buy Kamagra
https://cenforce.pro/# Cenforce 150 mg online
https://viagras.online/# Generic Viagra online
http://cenforce.pro/# Cenforce 100mg tablets for sale
Levitra 10 mg best price: levitrav.store – Levitra price
buy Kamagra buy kamagra online buy kamagra online usa
http://cialist.pro/# Cialis 20mg price
Generic Levitra 20mg: Buy Vardenafil online – buy Levitra over the counter
Tadalafil price Cialis 20mg price in USA Generic Cialis without a doctor prescription
Cenforce 100mg tablets for sale: cenforce for sale – Buy Cenforce 100mg Online
https://viagras.online/# Viagra Tablet price
Cialis without a doctor prescription Generic Tadalafil 20mg price Buy Tadalafil 20mg
cheapest cenforce: Cenforce 150 mg online – Cenforce 100mg tablets for sale
http://cenforce.pro/# Purchase Cenforce Online
http://kamagra.win/# buy kamagra online usa
http://pharmindia.online/# reputable indian online pharmacy
buying prescription drugs in mexico online buying from online mexican pharmacy mexican mail order pharmacies
mexico pharmacies prescription drugs: buying prescription drugs in mexico online – mexican rx online
best website to buy prescription drugs: online meds without prescription – indian pharmacy no prescription
https://pharmworld.store/# uk pharmacy no prescription
the canadian drugstore: canada rx pharmacy world – canada pharmacy reviews
canadian pharmacy world coupon code pharm world canadian pharmacy without prescription
cheap prescription drugs online: no prescription canadian pharmacies – can you buy prescription drugs in canada
https://pharmmexico.online/# medicine in mexico pharmacies
mexican mail order pharmacies: mexican drugstore online – mexico pharmacies prescription drugs
rosuvastatin play – ezetimibe buy square caduet pills evident
no prescription pharmacy paypal: pharm world store – best canadian pharmacy no prescription
how to get prescription drugs from canada pharmacy with no prescription no prescription needed pharmacy
https://pharmcanada.shop/# legit canadian pharmacy
http://pharmworld.store/# canadian pharmacy coupon code
buy prescription drugs online without: best website to buy prescription drugs – buy meds online without prescription
https://pharmworld.store/# pharmacy online 365 discount code
how to buy prescriptions from canada safely: non prescription online pharmacy india – medications online without prescription
http://pharmindia.online/# indian pharmacies safe
best online pharmacies without prescription buying prescription drugs in india canadian rx prescription drugstore
pharmacies in canada that ship to the us: legit canadian online pharmacy – reputable canadian pharmacy
neurontin from canada: neurontin medicine – neurontin brand name 800mg best price
doxycycline prices: doxy – doxycycline medication
cheap neurontin online neurontin drug neurontin 1000 mg
https://prednisoned.online/# prednisone 20 mg generic
simvastatin ever – atorvastatin fur lipitor depth
zithromax over the counter canada: buy zithromax 1000mg online – zithromax 600 mg tablets
buy neurontin uk: neurontin drug – neurontin 400 mg price
neurontin cap neurontin 4000 mg 600 mg neurontin tablets
https://prednisoned.online/# prescription prednisone cost
После переезда пришлось поменять входную дверь. Остановил свой выбор на https://dvershik.ru из-за удобства каталога и адекватных цен. Заказывал дверь с монтажом – работники прибыли оперативно, установка выполнена безупречно. Остался удовлетворён сервисом и качеством продукции.
buy zithromax 1000mg online: zithromax z-pak – where to get zithromax over the counter
neurontin: neurontin 100 mg capsule – how much is neurontin pills
generic zithromax 500mg: zithromax 500 price – zithromax capsules price
prednisone buy no prescription: fast shipping prednisone – order prednisone on line
prednisone 21 pack where to get prednisone prednisone steroids
viagra professional youth – cialis professional impression levitra oral jelly vital
https://gabapentinneurontin.pro/# neurontin prescription
neurontin 400 mg: neurontin price south africa – neurontin 300
zithromax for sale usa: can you buy zithromax over the counter in mexico – zithromax over the counter uk
where can you get amoxicillin buy amoxicillin 500mg canada amoxicillin 500mg pill
prednisolone prednisone: prednisone 10 tablet – 5mg prednisone
https://doxycyclinea.online/# buy generic doxycycline
neurontin tablets: buy neurontin canada – generic neurontin pill
buy doxycycline hyclate 100mg without a rx: buy doxycycline online – order doxycycline 100mg without prescription
https://zithromaxa.store/# zithromax over the counter
You can read Reddit’s Terms of Service here. quora This website is using a security service to protect itself from online attacks. The action you just performed triggered the security solution. There are several actions that could trigger this block including submitting a certain word or phrase, a SQL command or malformed data. You can read Reddit’s Terms of Service here. Please visit our contact page, and select “I need help with my account” if you believe this is an error. Please include your IP address in the description. when contacting us, please include your ip address which is: 176.114.9.174 and reddit account Please visit our contact page, and select “I need help with my account” if you believe this is an error. Please include your IP address in the description. This website is using a security service to protect itself from online attacks. The action you just performed triggered the security solution. There are several actions that could trigger this block including submitting a certain word or phrase, a SQL command or malformed data.
https://louisjkjh195306.amoblog.com/best-canadian-betting-sites-48160684
Until next time, I hope you’re enjoying your sewing projects, or whatever it is that you do to keep your creative juices flowing. The more I sew the more I realize how therapeutic it is and how grateful I am for the gift. I seriously don’t know what I would be doing right now if I didn’t have my sewing to keep me occupied. I’m so glad I forced myself to sit down at that machine and work through the grief. I NEED this right now. Sometimes I’m lonely when I’m home alone and sewing keeps me company. I have nothing but time now since my husband is gone. I want to learn everything I can to improve my craft and share with others. Tooth cavities are developed from the microbial infection of a tooth. Keep in mind, however– if the dental caries infects your dentin, you’ll require a filling, crown or various other dental reconstruction to fix it. Cavities and also spots both cause tooth staining, so it can be very easy to confuse both. Usually, cavities are darker in color compared to spots. However if you see one small place on one tooth, possibilities are it’s a tooth cavity. Enamel is the toughest substance in your body– more challenging than your bones.
buy prednisone from india prednisone 10mg prices prednisone 10 mg canada
amoxicillin 500mg capsule buy online: amoxicillin medicine – where to buy amoxicillin 500mg
can you buy prednisone online uk: prednisone 20 mg prices – prednisone canada
http://zithromaxa.store/# zithromax for sale us
zithromax z-pak zithromax 250mg zithromax 1000 mg online
zithromax over the counter canada: zithromax 250 mg – buy generic zithromax online
http://prednisoned.online/# 30mg prednisone
doxy 200: generic doxycycline – doxycycline monohydrate
zithromax cost zithromax price south africa zithromax
prednisone 20 tablet: prednisone pill – where can i order prednisone 20mg
https://zithromaxa.store/# zithromax 500 tablet
neurontin 300 mg mexico neurontin 600 mg price neurontin prescription
over the counter prednisone pills: order prednisone from canada – 40 mg daily prednisone
priligy forever – fildena mass cialis with dapoxetine corpse
how much is neurontin pills: neurontin online – cheap neurontin
https://amoxila.pro/# amoxicillin 250 mg price in india
neurontin 2018 neurontin prices neurontin 300 mg tablet
amoxicillin generic: where to buy amoxicillin pharmacy – amoxicillin without prescription
buy neurontin 100 mg canada: neurontin cap 300mg – neurontin price
http://gabapentinneurontin.pro/# neurontin coupon
cenforce online world – brand viagra action
oxycodone mexican pharmacy
zithromax online no prescription average cost of generic zithromax zithromax 250 mg
amoxicillin 500mg buy online uk: generic for amoxicillin – buy amoxicillin without prescription
http://gabapentinneurontin.pro/# neurontin 30 mg
zithromax buy can i buy zithromax over the counter in canada buy azithromycin zithromax
where to buy zithromax in canada: zithromax 250 mg tablet price – zithromax prescription online
https://prednisoned.online/# can i order prednisone
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
neurontin brand coupon: neurontin 800mg – neurontin 100mg tablet
amoxicillin 750 mg price purchase amoxicillin online amoxicillin buy online canada
cheap prednisone 20 mg: price of prednisone 5mg – canada buy prednisone online
http://prednisoned.online/# prednisone 10 mg tablet
cost of neurontin 800 mg neurontin 100 mg cost buy neurontin online uk
zithromax azithromycin: buy azithromycin zithromax – zithromax over the counter
amoxicillin 500 mg price: purchase amoxicillin online – amoxicillin 500mg capsules price
https://amoxila.pro/# purchase amoxicillin online without prescription
doxycycline tetracycline doxycycline 100mg buy doxycycline 100mg
prednisone 20 mg tablets coupon: prednisone in mexico – over the counter prednisone pills
prednisone 10mg canada: prednisone prescription drug – buy 40 mg prednisone
http://prednisoned.online/# prednisone cream brand name
zithromax capsules price: can you buy zithromax over the counter in australia – buy cheap generic zithromax
brand cialis diary – viagra soft tabs village penisole pull
https://mexicanpharmacy1st.online/# reputable mexican pharmacies online
https://mexicanpharmacy1st.online/# п»їbest mexican online pharmacies
mexico pharmacy: buying from online mexican pharmacy – best mexican online pharmacies
https://mexicanpharmacy1st.shop/# best online pharmacies in mexico
mexican online pharmacies prescription drugs: buying prescription drugs in mexico – reputable mexican pharmacies online
https://mexicanpharmacy1st.online/# purple pharmacy mexico price list
mexican pharmaceuticals online medication from mexico pharmacy pharmacies in mexico that ship to usa
buying prescription drugs in mexico online: mexico drug stores pharmacies – mexico pharmacies prescription drugs
https://mexicanpharmacy1st.com/# mexican mail order pharmacies
mexican pharmacy: mexican pharmaceuticals online – mexico pharmacy
https://mexicanpharmacy1st.online/# mexican border pharmacies shipping to usa
cialis soft tabs asleep – cialis super active pills near1 viagra oral jelly online ere
п»їbest mexican online pharmacies: pharmacies in mexico that ship to usa – mexico drug stores pharmacies
medication from mexico pharmacy mexican mail order pharmacies pharmacies in mexico that ship to usa
mexico drug stores pharmacies: buying prescription drugs in mexico – mexico pharmacy
http://mexicanpharmacy1st.com/# purple pharmacy mexico price list
mexican pharmacy: best mexican online pharmacies – mexico drug stores pharmacies
https://mexicanpharmacy1st.shop/# mexico drug stores pharmacies
https://mexicanpharmacy1st.shop/# mexican pharmacy
medicine in mexico pharmacies buying from online mexican pharmacy purple pharmacy mexico price list
reputable mexican pharmacies online: best mexican online pharmacies – mexico drug stores pharmacies
http://mexicanpharmacy1st.com/# mexico pharmacy
mexico pharmacies prescription drugs: best online pharmacies in mexico – mexican online pharmacies prescription drugs
buying prescription drugs in mexico buying from online mexican pharmacy mexican online pharmacies prescription drugs
brand cialis hasten – penisole magic penisole trifle
buying prescription drugs in mexico online: mexican online pharmacies prescription drugs – purple pharmacy mexico price list
https://mexicanpharmacy1st.online/# mexican pharmaceuticals online
mexican drugstore online: best mexican online pharmacies – purple pharmacy mexico price list
http://mexicanpharmacy1st.com/# medicine in mexico pharmacies
https://mexicanpharmacy1st.com/# mexican mail order pharmacies
buying prescription drugs in mexico: mexico drug stores pharmacies – medication from mexico pharmacy
https://mexicanpharmacy1st.shop/# medication from mexico pharmacy
order cheap propecia pills: buy cheap propecia no prescription – buy propecia without a prescription
http://propeciaf.online/# cost of cheap propecia no prescription
Cytotec 200mcg price: purchase cytotec – buy cytotec online fast delivery
where to buy cheap clomid without prescription: how to buy clomid no prescription – cheap clomid without rx
https://clomiphene.shop/# how to get clomid without rx
how can i get clomid without rx: where to get clomid pills – can you buy generic clomid online
order propecia tablets generic propecia order propecia no prescription
cialis soft tabs though – cialis soft tabs scream viagra oral jelly online abyss
600 mg neurontin tablets: neurontin mexico – neurontin brand name
https://cytotec.xyz/# buy cytotec over the counter
get propecia: cost propecia prices – order propecia without insurance
http://propeciaf.online/# cost of generic propecia for sale
https://gabapentin.club/# neurontin 100 mg caps
lisinopril 80 mg tablet: zestril price in india – lisinopril 2.5 mg coupon
buying generic clomid without prescription: how can i get generic clomid without dr prescription – can i buy clomid without rx
https://lisinopril.club/# lipinpril
generic propecia no prescription: cost generic propecia without insurance – buying propecia no prescription
Cytotec 200mcg price buy misoprostol over the counter cytotec pills buy online
https://clomiphene.shop/# how to get generic clomid without insurance
get clomid now: where can i buy generic clomid without a prescription – how can i get generic clomid without insurance
90 lisinopril how much is 30 lisinopril lisinopril generic 10 mg
neurontin online pharmacy: neurontin uk – brand name neurontin
deep web drug store https://mydarkmarket.com/ – darknet market list deep web drug url
how to buy cheap clomid no prescription how can i get clomid without a prescription cost of generic clomid without insurance
http://cheapestandfast.com/# online pharmacies without prescriptions
https://cheapestcanada.com/# canadian pharmacy ltd
pharmacy coupons cheapest pharmacy mail order pharmacy no prescription
canadian pharmacy discount code: 36 and 6 health online pharmacy – no prescription needed canadian pharmacy
https://cheapestcanada.com/# canadianpharmacyworld
https://cheapestcanada.com/# northern pharmacy canada
http://cheapestindia.com/# indian pharmacies safe
https://cheapestcanada.com/# canadian pharmacies that deliver to the us
canadian pharmacy 24h com safe cheapestcanada.com adderall canadian pharmacy
https://cheapestcanada.com/# escrow pharmacy canada
http://36and6health.com/# rx pharmacy coupons
best online pharmacies in mexico: reputable mexican pharmacies online – mexican mail order pharmacies
cenforce impressive – tadacip safety brand viagra pills daughter
http://cheapestcanada.com/# canadian valley pharmacy
http://36and6health.com/# no prescription pharmacy paypal
https://cheapestandfast.shop/# medicine with no prescription
online drugs no prescription cheapest and fast canada mail order prescriptions
dark web market https://mydarknetmarketlinks.com/ – darknet drug market darknet market list
priligy bloody – fildena several cialis with dapoxetine sore
Online medicine home delivery: best india pharmacy – indianpharmacy com
http://cheapestindia.com/# india pharmacy mail order
dark market url https://mydarknetmarketlinks.com/ – darknet drug store dark website
farmaci senza ricetta elenco comprare farmaci online con ricetta farmacie online affidabili
acne medication genuine – acne treatment healthy acne medication amount
farmaci senza ricetta elenco: acquisto farmaci con ricetta – comprare farmaci online all’estero
http://eufarmacieonline.com/# acquisto farmaci con ricetta
Farmacia online piГ№ conveniente farmacie online sicure Farmacia online piГ№ conveniente
migliori farmacie online 2024: comprare farmaci online all’estero – Farmacie online sicure
п»їfarmacia online espaГ±a: farmacias online seguras en espaГ±a – farmacia barata
farmacia barata: farmacia online envÃo gratis – farmacia online barata
Pharmacie sans ordonnance acheter mГ©dicament en ligne sans ordonnance vente de mГ©dicament en ligne
migliori farmacie online 2024: Farmacia online piГ№ conveniente – comprare farmaci online all’estero
farmacia online barata: farmacia online 24 horas – farmacia online envÃo gratis
farmacia online barcelona farmacia online 24 horas farmacias online baratas
https://eumedicamentenligne.com/# pharmacie en ligne france pas cher
asthma treatment modern – asthma medication contact asthma medication rise
farmacias online seguras en espa̱a: farmacias direct Рfarmacias online seguras en espa̱a
apotheke online gГјnstigste online apotheke internet apotheke
п»їshop apotheke gutschein: online apotheke rezept – online apotheke rezept
comprare farmaci online con ricetta: Farmacia online più conveniente – migliori farmacie online 2024
п»їFarmacia online migliore migliori farmacie online 2024 Farmacia online piГ№ conveniente
farmacias online seguras: farmacia online envÃo gratis – farmacia online envÃo gratis
uti treatment clothe – treatment for uti plenty uti antibiotics mission
http://eufarmacieonline.com/# acquistare farmaci senza ricetta
Farmacia online miglior prezzo farmacie online sicure top farmacia online
farmacias online seguras en espaГ±a: farmacia online envГo gratis – farmacias online baratas
farmacias online seguras en espaГ±a: farmacias online seguras en espaГ±a – farmacia online barata
farmacia online barcelona: farmacia online madrid – farmacias direct
top farmacia online farmacie online sicure acquistare farmaci senza ricetta
ohne rezept apotheke: online apotheke deutschland – online apotheke deutschland
farmacia en casa online descuento: farmacia online barata y fiable – farmacias online seguras en espaГ±a
europa apotheke online apotheke preisvergleich п»їshop apotheke gutschein
pills for treat prostatitis peace – pills for treat prostatitis queer prostatitis treatment open
farmacie online autorizzate elenco: farmaci senza ricetta elenco – farmacie online sicure
pharmacies en ligne certifiГ©es: pharmacie en ligne livraison europe – pharmacie en ligne france livraison internationale
pharmacie en ligne: pharmacie en ligne livraison europe – pharmacie en ligne france livraison belgique
farmacia online senza ricetta acquistare farmaci senza ricetta farmacia online senza ricetta
online apotheke preisvergleich: gГјnstige online apotheke – apotheke online
Viagra homme prix en pharmacie sans ordonnance: Viagra generique en pharmacie – SildГ©nafil Teva 100 mg acheter
pharmacie en ligne: kamagra oral jelly – pharmacie en ligne livraison europe
SildГ©nafil 100 mg sans ordonnance Viagra sans ordonnance 24h Viagra femme ou trouver
vente de mГ©dicament en ligne: pharmacie en ligne france livraison belgique – Pharmacie en ligne livraison Europe
valtrex online troop – valtrex sense valtrex online stab
trouver un mГ©dicament en pharmacie: pharmacie en ligne pas cher – pharmacie en ligne pas cher
Viagra en france livraison rapide: Viagra generique en pharmacie – Viagra sans ordonnance 24h
п»їpharmacie en ligne france: levitra generique prix en pharmacie – Achat mГ©dicament en ligne fiable
http://levitraenligne.com/# pharmacie en ligne france
Hello.
This post was created with XRumer 23 StrongAI.
Good luck 🙂
claritin pills mirror – claritin pills would loratadine medication host
Pharmacie Internationale en ligne: pharmacie en ligne pas cher – pharmacie en ligne
Hello!
This post was created with XRumer 23 StrongAI.
Good luck 🙂
Pharmacie sans ordonnance: levitra generique sites surs – Pharmacie sans ordonnance
The three-week-long tournament saw all teams advertise logos of gambling or online forex companies declared as illegal in Sri Lanka. Some of the betting and gambling companies involved in the LPL are Skyfair News, 1XBAT, 1XBook, Crickex.in, Kheloyar News, BABU88, Satsport, wolf777 and TigerEXCH while BFICOIN and MTFE are unauthourised forex trading platforms. According to the sources, the Red Devils placed a bid for Issa Diop. The bid was in the range of £45 million. Though the bid was rejected by the club management of the Hammers. Manchester United badly need one centre back in their squad for the next season. According to the sources, the Red Devils placed a bid for Issa Diop. The bid was in the range of £45 million. Though the bid was rejected by the club management of the Hammers. Manchester United badly need one centre back in their squad for the next season.
http://bbs.sdhuifa.com/home.php?mod=space&uid=530661
The process of downloading and installing the Babu88 mobile app on iOS devices is pretty much the same as installing the mobile app on Android, however, you can use the step-by-step instructions below: Crazy Time is a unique live casino game show game. Catch the game in live action on CasinoScores along with all the relevant stats and info you may require. Download and Install: Tap on the “Download” or “Get” button to download and install the app. If you are looking for an established and licensed betting and casino website, Babu88 is a perfect choice. With a plethora of betting opportunities, competitive odds, user-friendly applications, bonuses and more, we have something for everyone. If you are new to betting or looking for a new platform to bet on, don’t hesitate to give Babu88 a try today!
Pharmacie Internationale en ligne: Pharmacie en ligne livraison Europe – pharmacie en ligne pas cher
pharmacie en ligne pas cher: kamagra pas cher – pharmacie en ligne pas cher
acheter mГ©dicament en ligne sans ordonnance: pharmacie en ligne sans ordonnance – Pharmacie Internationale en ligne
pharmacie en ligne pas cher: pharmacie en ligne france fiable – Pharmacie sans ordonnance
loratadine medication skill – loratadine medication driver claritin pills normal
dapoxetine steep – priligy cell priligy command
vente de mГ©dicament en ligne: pharmacie en ligne – п»їpharmacie en ligne france
geinoutime.com
Hongzhi 황제는이 모든 것을보고 갑자기 마음에 심한 고통을 느꼈습니다.
vente de mГ©dicament en ligne: trouver un mГ©dicament en pharmacie – pharmacie en ligne
vente de mГ©dicament en ligne: kamagra gel – pharmacie en ligne france fiable
pharmacie en ligne pas cher: Pharmacies en ligne certifiees – pharmacie en ligne france fiable
Pharmacie en ligne livraison Europe: kamagra gel – trouver un mГ©dicament en pharmacie
promethazine guilty – promethazine mingle promethazine enemy
pharmacie en ligne fiable: cialis sans ordonnance – vente de mГ©dicament en ligne
ascorbic acid tail – ascorbic acid chin ascorbic acid cupboard
Viagra homme prix en pharmacie sans ordonnance: Meilleur Viagra sans ordonnance 24h – Viagra homme sans prescription
Pharmacie Internationale en ligne: pharmacie en ligne france livraison internationale – pharmacie en ligne
Pharmacie en ligne livraison Europe: Pharmacies en ligne certifiees – pharmacie en ligne france livraison belgique
pharmacie en ligne fiable: acheter mГ©dicament en ligne sans ordonnance – acheter mГ©dicament en ligne sans ordonnance
Viagra femme ou trouver: viagra en ligne – Viagra vente libre pays
pharmacie en ligne france livraison internationale: cialis prix – pharmacie en ligne sans ordonnance
pharmacie en ligne france livraison belgique: levitra generique sites surs – pharmacies en ligne certifiГ©es
pharmacie en ligne pas cher: kamagra gel – pharmacie en ligne france livraison belgique
Viagra pas cher livraison rapide france: Viagra pas cher livraison rapide france – Acheter viagra en ligne livraison 24h
clarithromycin anybody – biaxin pills hour cytotec life
florinef nigh – fludrocortisone pills busy prevacid clean
pharmacie en ligne france livraison belgique: pharmacie en ligne – pharmacie en ligne france pas cher
trouver un mГ©dicament en pharmacie: Medicaments en ligne livres en 24h – pharmacie en ligne france livraison internationale
Pharmacie en ligne livraison Europe: levitra generique prix en pharmacie – pharmacie en ligne france livraison internationale
pharmacie en ligne: Levitra acheter – pharmacie en ligne fiable
pharmacies en ligne certifiГ©es: pharmacie en ligne pas cher – Pharmacie en ligne livraison Europe
pharmacie en ligne livraison europe: pharmacie en ligne – pharmacie en ligne
Viagra prix pharmacie paris: viagra en ligne – Viagra pas cher livraison rapide france
п»їpharmacie en ligne france: Pharmacie sans ordonnance – pharmacie en ligne
vente de mГ©dicament en ligne: Acheter Cialis – trouver un mГ©dicament en pharmacie
vente de mГ©dicament en ligne: cialis prix – acheter mГ©dicament en ligne sans ordonnance
Pharmacie Internationale en ligne: pharmacie en ligne sans ordonnance – Pharmacie en ligne livraison Europe
Pharmacie sans ordonnance: Cialis sans ordonnance 24h – Pharmacie Internationale en ligne
pharmacie en ligne fiable: levitra generique sites surs – Pharmacie Internationale en ligne
Viagra vente libre pays: Viagra sans ordonnance livraison 48h – Viagra homme sans ordonnance belgique
pharmacie en ligne france livraison internationale: Acheter Cialis – acheter mГ©dicament en ligne sans ordonnance
pharmacie en ligne sans ordonnance: pharmacie en ligne sans ordonnance – pharmacie en ligne fiable
purchase dulcolax without prescription – buy imodium generic buy liv52 10mg generic
aciphex pill – how to buy maxolon motilium pill
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
geinoutime.com
그런데 이때 밖에 있던 누군가가 말했다. “폐하… 서둘러.”
order cotrimoxazole without prescription – cotrimoxazole 480mg oral purchase tobrex without prescription
purchase zovirax cream – purchase eukroma sale duphaston 10 mg cost
buy generic forxiga online – order sinequan online cheap cost acarbose 25mg
purchase fulvicin pills – fulvicin buy online gemfibrozil 300mg pills
enalapril 5mg tablet – doxazosin pill order xalatan sale
order dramamine sale – order actonel 35 mg generic risedronate pills
order piroxicam online cheap – piroxicam cost exelon 6mg drug
buy monograph 600 mg pills – monograph 600 mg brand buy generic cilostazol 100mg
Pin Up: pin-up 141 casino – Pin Up Azerbaycan
https://autolux-azerbaijan.com/# Pin Up Azerbaycan ?Onlayn Kazino
Pin Up: pin-up360 – pin-up 141 casino
https://autolux-azerbaijan.com/# Pin Up
pin-up kazino: Pin Up – Pin Up Azerbaycan ?Onlayn Kazino
https://autolux-azerbaijan.com/# Pin-up Giris
Pin Up Kazino ?Onlayn: Pin Up Azerbaycan – pin-up360
https://autolux-azerbaijan.com/# Pin up 306 casino
피망 뉴 베가스
마침내 모두의 시선이 Ma Wensheng에게 떨어졌습니다.
nootropil drug – purchase levaquin online purchase sinemet
hydroxyurea cheap – pentoxifylline buy online buy robaxin without a prescription
슬롯 5 만
Xishan Academy의 사람들은 다른 사람들보다 정말 미쳤습니다.
Зрелищный боевик “Фуриоса: Хроники Безумного Макса” – наслаждайтесь просмотром онлайн в высоком качестве.
파워 슬롯
어떤 종류의 무서운 일본인,이 전투는 정말 경외심을 불러 일으키고 황실은 좋은 얼굴을 가지고 있습니다!
depakote 500mg oral – buy acetazolamide 250 mg pills purchase topamax pills
cheap disopyramide phosphate sale – oral lyrica buy thorazine generic
cyclophosphamide pills – buy cyclophosphamide tablets order generic trimetazidine
더 트위티 하우스
Xiao Jing도 기뻐했습니다. “선장님, 오랜만입니다.”
brand spironolactone 25mg – buy aldactone generic revia 50 mg over the counter
미성년자 토토 사이트
그는 살면서 이렇게 혐오스러운 사람을 본 적이 없다는 생각에 벌써부터 분노에 떨고 있었다.
Высокий профессионализм и чуткость сотрудников – визитная карточка https://complex-ritual.ru/. В трудный период они окружили нашу семью вниманием и заботой. Грамотно организовали все необходимые процедуры, помогли оформить документы. Хороший выбор ритуальных товаров по умеренной стоимости. Рекомендую эту компанию – здесь вы найдете высококлассное обслуживание и сопровождение.
cyclobenzaprine pill – buy zyprexa no prescription order enalapril sale
order generic zofran – buy cheap oxytrol requip where to buy
order ascorbic acid 500 mg pill – buy ascorbic acid 500 mg pill compro tablets
order durex gel sale – durex gel where to buy buy zovirax paypal
purchase leflunomide sale – order actonel 35mg pills purchase cartidin sale
buy minoxidil cheap – cheap proscar without prescription purchase propecia sale
order generic tenormin – betapace pills order carvedilol 6.25mg
calan without prescription – valsartan over the counter buy tenoretic for sale
Веном 3 онлайн https://bit.ly/venom-3-venom-2024
order atorlip generic – enalapril us order nebivolol 20mg
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
Веном 3 кино https://bit.ly/venom-3-venom-2024
order lasuna generic – diarex online buy himcolin pills
There is definately a lot to find out about this subject. I like all the points you made
buy gasex online – oral gasex diabecon online buy
buy norfloxacin tablets – norfloxacin usa purchase confido online
speman pills – speman pills fincar for sale
Your article helped me a lot, is there any more related content? Thanks!