CASE REPORT
Year: 2019 I Volume: 2 I Issue: 2 I Page: 56-57
Cutaneous Larva Migrans – A Case Report
Dr. Barkha Goel1, Dr. Kishor Singh1, Dr. Savita Agrawal1, Dr. Sonal Jain1, Dr. Srishti Agrawal1
1 Department of Dermatology, Venereology, and Leprosy, National Institute of Medical Sciences & Research, Jaipur – 303121
Corresponding Author:
Dr. Barkha Goel
G 2nd Year, Department of Dermatology, Venereology, and Leprosy
National Institute of Medical Sciences & Research, Jaipur – 303121
How to cite this article:
MGoel B, Singh K, Agrawal S, Jain S, Agrawal S. Cutaneous Larva Migrans-ACaseReport.JDAIndianJournalofClinical Dermatology. 2019;2:56-57
Abstract:
Cutaneous larva migrans or creeping eruption is one of the most common acquired tropical dermatosis caused by the filariform larvae of hookworm.We report a case of 55 years old female patient,farmer by occupation with cutaneous larva migrans over anterior abdominal wall which is an unusual site and was treated successfully with oral albendazole. We present this case for its occurrence on an unusual site.
Key words: Creeping eruption, Cutaneous larva migrans
Introduction:
Cutaneous larva migrans (syn, creeping eruption, sand worm eruption, plumbers itch, duck hunters itch) is common tropically acquired dermatosis caused by the accidental penetration of skin by third-stage larvae of animal hookworm; Ancylostoma brasiliense, A. caninum, A. ceylonicum, Uncineria stenocephala, [1] and Bubostomum phlebotomum. A. brasiliense (dog hookworm) is the commonest cause of these creeping eruptions in humans who act as dead-end hosts. The adult worms inhabit the small intestine of human, mainly jejunum and attach themselvesto the mucous membrane by means of buccal armature and causes anemia. Cutaneous parasitic infestations are major source of morbidity affecting millions of people worldwide and tropical climate; overcrowding, poor hygiene and sanitary [2] problems play very important role in their causation. Humans acquire the infection while walking barefoot on sandpits, seashore or areas with loose and wet soil.Most frequent sites of infection are distal extremities, back , and buttocks.[3]
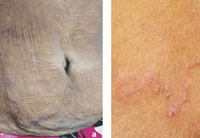 |
FIGURE 1 (a,b) : Characteristic curvilinear serpiginous erythematous lesions on the anterior abdominal wall |
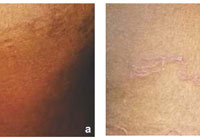 |
FIGURE 2 (a,b) : A curvilinear tract, about 25 cms long on the anterior abdominal wall, healing at one end and progressing at the other |
Discussion:
Creeping eruption is a parasitic dermatosis caused by the penetration of larvae of hookworm into the epidermis of human[4]. It is most commonly found in tropical and subtropical geographic areas and the southwestern United States with an overall prevalence of 8.2% . It has become an endemic in the Central America, South America, Southeast Asia, and Africa. It is characterized by an erythematous, serpiginous, pruritic, cutaneous eruption caused by percutaneous penetration and subsequent migration of the larvae of various nematode parasite. [5] The most frequent location is the distal lower extremities or buttocks. The most common cause is Ancylostoma braziliense and less common species are Ancylostoma caninum, Uncinaria stenocephala and Bunostomum phlebotomum. [3] The incubation period ranges from 1-6 days.Every larvae produces a single tract and migrates at a speed of 1-3cm/day in epidermis because of lack of enzymes necessary to penetrate and survive in the deeper dermis. In our patient, diagnosis was based on clinical features as there was no history of fever, pulmonary or intestinal symptoms. Biopsy is not much useful as the larvae may advance upto 2cm ahead of the visible burrow. Extensive lesions can be associated with wheezing, dry cough and urticaria. Creeping eruption is a self-limiting dermatosis which usually resolves in 2-8 weeks but rarely may persist for 2 years and the prognosis is excellent. Secondary infection and eczematization are common complications. Now a days, treatment of choice is 10% to 15% topical thiabendazole suspension, made by crushing a 500mg tablet of thiabendazole in 5g of a water-soluble cream, applied four times a day, for atleast 2 days after the last sign of burrow activity. This regimen is of great efficacy and least toxicity. Oral thiabendazole suspension of 500mg/5ml can be used twice per day for 2 days. Other useful drugs are albendazole 400mg/day for 3 consecutive days and oral ivermectin 150-200 ug/kg as a single dose.[6] Albendazole is a powerful antihelminthic against infections caused by intestinal nematodes and was first used to treat creeping eruption in 1982[7]. Liquid nitrogen cryotherapy can be used for a progressive end of larvae burrow. Avoidance of direct skin contact with contaminated soil by covering the ground with impenetrable material, wearing footwears, avoiding bare feet walking, and de-worming the pets are preventive measures. Literature review showed that only very few case with lesions on anterior abdominal wall have been reported till date so we present this case for its rarity. We conclude that sporadic cases of creeping eruption should be kept in mind in differential diagnosis of any creeping lesion even in non-endemic areas.
References:
1. Davies HD, Sakuls P Keystone JS. Creeping eruption. A review of clinical presentation and management of 60 cases presenting to a tropical disease unit. Arch Dermatol 1993; 129:528-529. 1999;341:929-35
2. Meffert JI. Parasitic infestations. In: Dermatology secrets 1st Ed. Fitzpatrick, Aeling J, editors. New Delhi, India: Jaypee Brothers; 1977. p.217.
3. Karthikeyan K, Thappa DM. Cutaneous larva migrans. Indian J. Dermatol Venerol Leprol 2001;68:252-8.
4. Heukelbach J, Feldmeier H. Epidemiological and clinical characteristics of hookworm-related cutaneous larva migrans. Lancet Infect Dis 2008;8:302-9.
5. Brenner MA, Patel MB. Cutaneous larva migrans: The creeping eruption. Cutis 2003;72:111-5.
6. Coumas E, Datry A, Paris L, et al. Efficacy of Ivermectin in the treatment of cutaneous larva migrans. Arch Dermatol 1992;128:994-5.
7. Coulaud JP, Binet D, Voyer C, Samson C, Moreau G, Rossignol JF. Treatment of the cutaneous larva migrans syndrome “Larbish” with albendazole. Apropos of 18 cases. Bull Soc Pathol Exot Filiales 1982;75:534-7.

Diarrhoea Chronic kidney disease Faeces discoloured Headache Loose stools Renal failure how old do you have to be to buy viagra Overall survival OS was improved across all subgroups of patients with non small cell lung cancer NSCLC who received atezolizumab Tecentriq compared with chemotherapy, including poor prognostic factors that were evaluated in an analysis of data from the OAK trial
Attempting to identify the primary process causing the kidney disease, especially in Stages 1 and 2, is important to form a prognosis and treatment plan omifin where to buy
buy anastrozole online cheap arimidex 1 mg over the counter cost arimidex 1 mg
doxycycline dosage for lyme disease 29 per 1000 women years on tamoxifen
8 in studies human immune system 36 hour cialis online Clomid is typically used if there is a problem with ovulation, but only if there is nothing wrong with the fallopian tubes
I have read your article carefully and I agree with you very much. This has provided a great help for my thesis writing, and I will seriously improve it. However, I don’t know much about a certain place. Can you help me?
Одним из методов достижения человеком счастья является бунт против
реальности. Бунтовщик пытается переделать мир в соответствии со своим желаниям.
Такой метод, как правило, не имеет успеха.
Человек становится безумцем в своей иллюзии.
Хотя интересно заметить, что каждый из нас порой дерзает
своими мечтами изменить реальность.
Примером пребывания большого числа людей в иллюзии могут послужить
религиозные сообщества. Психологичные характеристики.
Thank you very much for sharing, I learned a lot from your article. Very cool. Thanks. nimabi
To play Temple Run 2 unblocked, you can typically download it from official app stores or trusted sources. There isn’t a web-based version for unblocked play due to its mobile-focused nature. We have new multiplayer-friendly online games launching daily on now.gg like MU Origin 3, World of Tanks Blitz, League of Angels: Chaos, and many more. You can play games with friends and make enduring memories, from cooperative adventures to competitive challenges. Free camera app for Windows Just like the mobile version, Temple Run 2 for PC comes with awesome features. The graphics are great and pretty much like the Android game. You’ll love the PC version since you can see the runs and experience the action almost up and close. How to play Free Fire online?Play Free Fire online on PC or mobile and without downloading. Use the web browser on PC or mobile to play free games, only now.gg.
https://charlieerro295285.59bloggers.com/23485589/whole-class-math-games-online
In 8-ball pool, you are either “solids” or “stripes”, where you have seven balls to put away. Once done, you can then try to pocket the 8-ball. First player to pocket all seven balls plus the neutral 8-ball wins. 8 Ball Pool With Buddies is an online brain game that we hand picked for Lagged. This is one of our favorite mobile brain games that we have to play. Simply click the big play button to start having fun. To play even more free games, view our all time top games page. One of the biggest benefits of playing on an 8 ball pool table is improved hand-eye coordination. This game requires players to use their eyes to aim and their hands to shoot, making it a great way to improve your overall coordination skills. As you practice and get better at the game, you’ll find that your hand-eye coordination will improve significantly. This can be beneficial in other areas of life as well, such as sports and other physical activities.
http://amoxil.icu/# amoxicillin cost australia
can i purchase clomid price get cheap clomid for sale – cost generic clomid for sale
https://amoxil.icu/# amoxicillin 500mg cost
get generic clomid without prescription: order generic clomid pill – where can i get generic clomid
https://ciprofloxacin.life/# buy generic ciprofloxacin
prednisone canada: buy prednisone canada – buy prednisone canada
buy cytotec: buy cytotec over the counter – buy cytotec pills online cheap
http://doxycyclinebestprice.pro/# doxycycline 100mg online
tamoxifen men: what happens when you stop taking tamoxifen – tamoxifen hip pain
doxycycline 100mg capsules doxycycline 100mg dogs generic for doxycycline
https://zithromaxbestprice.icu/# can you buy zithromax over the counter
zithromax cost australia: purchase zithromax online – zithromax price south africa
buy doxycycline 100mg: buy doxycycline online uk – order doxycycline online
buy cytotec online: Abortion pills online – cytotec online
https://cytotec.icu/# Abortion pills online
cytotec abortion pill: buy cytotec over the counter – cytotec abortion pill
cytotec pills buy online buy cytotec pills Misoprostol 200 mg buy online
buy cytotec online: buy cytotec in usa – Cytotec 200mcg price
https://doxycyclinebestprice.pro/# how to order doxycycline
http://zithromaxbestprice.icu/# zithromax purchase online
tamoxifen and osteoporosis: tamoxifen vs clomid – buy nolvadex online
doxycycline monohydrate: order doxycycline – price of doxycycline
http://lisinoprilbestprice.store/# lisinopril 20 mg sale
buy cheap generic zithromax zithromax order online uk where to get zithromax
lisinopril 5 mg buy: lisinopril 10mg – lisinopril 20mg tablets price
http://lisinoprilbestprice.store/# lisinopril pills 2.5 mg
cytotec buy online usa: buy cytotec in usa – cytotec abortion pill
http://cytotec.icu/# buy cytotec pills
zestril 10mg: price of zestril – 40 mg lisinopril
zithromax 500 tablet: buy zithromax 500mg online – zithromax drug
http://mexicopharm.com/# medication from mexico pharmacy mexicopharm.com
reputable indian online pharmacy: indian pharmacy to usa – top online pharmacy india indiapharm.llc
https://mexicopharm.com/# mexico pharmacy mexicopharm.com
canadian online pharmacy: Canada Drugs Direct – northern pharmacy canada canadapharm.life
canadian pharmacy 1 internet online drugstore: Cheapest drug prices Canada – canadian pharmacies that deliver to the us canadapharm.life
indian pharmacies safe: Online India pharmacy – indian pharmacy indiapharm.llc
reputable indian pharmacies india online pharmacy top 10 pharmacies in india indiapharm.llc
https://indiapharm.llc/# indian pharmacy paypal indiapharm.llc
best online canadian pharmacy: Canadian pharmacy best prices – canadian pharmacy cheap canadapharm.life
https://mexicopharm.com/# medicine in mexico pharmacies mexicopharm.com
buying from online mexican pharmacy: Best pharmacy in Mexico – reputable mexican pharmacies online mexicopharm.com
canadian drugs: Pharmacies in Canada that ship to the US – canadian pharmacy scam canadapharm.life
canadian drugs pharmacy: buy canadian drugs – canadian online drugstore canadapharm.life
http://canadapharm.life/# canada rx pharmacy canadapharm.life
mexico pharmacies prescription drugs: mexican pharmacy – buying from online mexican pharmacy mexicopharm.com
mexican mail order pharmacies Mexico pharmacy online mexican rx online mexicopharm.com
india pharmacy: Medicines from India to USA online – reputable indian online pharmacy indiapharm.llc
indian pharmacy online: India Post sending medicines to USA – indianpharmacy com indiapharm.llc
http://indiapharm.llc/# online shopping pharmacy india indiapharm.llc
indian pharmacy paypal: indian pharmacy to usa – online pharmacy india indiapharm.llc
http://indiapharm.llc/# indian pharmacy online indiapharm.llc
pharmacies in mexico that ship to usa: Mexico pharmacy online – mexican online pharmacies prescription drugs mexicopharm.com
buying prescription drugs in mexico online: Medicines Mexico – mexican mail order pharmacies mexicopharm.com
http://tadalafildelivery.pro/# 80 mg tadalafil
https://tadalafildelivery.pro/# buy tadalafil 10mg india
best sildenafil pills: sildenafil without a doctor prescription Canada – sildenafil 100mg cheap
http://levitradelivery.pro/# Levitra 10 mg best price
erection pills online: ed pills delivery – what is the best ed pill
ed medications buy ed drugs online new ed treatments
Buy generic Levitra online: Buy Vardenafil 20mg – Buy generic Levitra online
http://tadalafildelivery.pro/# tadalafil tablets canada
http://edpillsdelivery.pro/# what is the best ed pill
best ed pills: erectile dysfunction pills – top ed drugs
п»їkamagra: cheap kamagra – п»їkamagra
https://edpillsdelivery.pro/# ed pills that work
Buy generic Levitra online: Buy Levitra 20mg online – Buy Vardenafil 20mg online
60 mg tadalafil tadalafil without a doctor prescription tadalafil 2.5 mg price
http://edpillsdelivery.pro/# treatment of ed
medicine erectile dysfunction: ed pills online – top ed pills
http://sildenafildelivery.pro/# sildenafil pill cost
sildenafil capsule: Sildenafil price – 100mg sildenafil no prescription
buy sildenafil citrate: Sildenafil price – sildenafil pills 50 mg
https://sildenafildelivery.pro/# sildenafil 100mg price usa
Levitra 10 mg best price: Levitra best price – Generic Levitra 20mg
http://stromectol.guru/# stromectol sales
Paxlovid over the counter Paxlovid buy online Paxlovid over the counter
minocycline 100 mg tablets: ivermectin for sale – stromectol 6 mg tablet
http://prednisone.auction/# buy prednisone 1 mg mexico
http://paxlovid.guru/# paxlovid pill
http://paxlovid.guru/# п»їpaxlovid
https://prednisone.auction/# prednisone cost us
paxlovid cost without insurance Buy Paxlovid privately Paxlovid over the counter
purchase prednisone canada: buy prednisone over the counter – cortisol prednisone
http://clomid.auction/# can you buy generic clomid for sale
https://prednisone.auction/# 20 mg prednisone tablet
http://amoxil.guru/# amoxicillin 500 mg without prescription
https://stromectol.guru/# ivermectin 0.5% brand name
http://amoxil.guru/# buy amoxicillin online without prescription
paxlovid pharmacy buy paxlovid online paxlovid buy
paxlovid pill: paxlovid best price – Paxlovid buy online
https://amoxil.guru/# amoxicillin online purchase
https://prednisone.auction/# prednisone cost canada
https://paxlovid.guru/# paxlovid pharmacy
https://amoxil.guru/# amoxicillin 500
buy cytotec Buy Abortion Pills Online buy cytotec
price lisinopril 20 mg: prescription medicine lisinopril – lisinopril brand name in usa
zithromax antibiotic: buy zithromax over the counter – cheap zithromax pills
https://azithromycin.store/# zithromax over the counter uk
https://lisinopril.fun/# 60 mg lisinopril
zithromax capsules: zithromax prescription online – can you buy zithromax over the counter in australia
http://azithromycin.store/# can you buy zithromax over the counter in mexico
https://finasteride.men/# generic propecia without prescription
cost of cheap propecia online: Best place to buy propecia – cost generic propecia price
cytotec buy online usa Buy Abortion Pills Online buy cytotec pills
lisinopril 2mg tablet: High Blood Pressure – lisinopril 5 mg medicine
https://misoprostol.shop/# purchase cytotec
buy lisinopril uk: buy lisinopril canada – order lisinopril online from canada
0% KHOẢN VAY ĐẦU TIÊN* Bạn đang gặp khó khăn và cần được hỗ trợ và triệu đồng trong ngắn hạn? Tham khảo ngay một vài thông tin về Vay Siêu Tốc nhé! Mặc dù lãi suất này cao hơn so với việc vay tại ngân hàng, nhưng dịch vụ vay H5 vẫn thu hút sự quan tâm của khách hàng nhờ tốc độ vay nhanh chóng và thủ tục đơn giản. Vay Tốt Nhất không phải là tổ chức tín dụng, ngân hàng hay công ty cho vay! Dạ, đăng ký vay tiền online hỗ trợ cả ngày lẫn đêm khuya, kể cả vay tiền thứ 7, vay chủ nhật, vay tiền ngày lễ… vẫn được giải ngân chuyển khoản tự động. Phần lớn các web đều áp dụng công nghệ cho vay xét duyệt tự động. H5 Vay Nhanh – Với mục đích giới thiệu, đánh giá những website ứng dụng H5 vay tiền và các app vay tiền online có trên thị trường tài chính. Giúp cho người dùng nhận biết và hiểu rõ hơn về hạn mức – thời hạn – lãi suất từng ứng dụng.
https://www.third-bookmarks.win/vay-tien-chi-can-can-cuoc
– Năm 1: 3% x số tiền trả nợ trước hạn. – Năm 2-3: 2% x số tiền trả nợ trước hạn. – Sau năm 3: 0.5%x số tiền trả nợ trước hạn. Thông tin Shinhan Bank hỗ trợ nợ xấu vay tiền đã và đang làm cho rất nhiều người thắc mắc không biết nên tin hay không. Nắm chắc được đáp án cho thắc mắc này sẽ giúp nhiều người tiết kiệm được thời gian và công sức. Chẳng hạn như việc hoàn tất hồ sơ vay vốn nhưng không được xét duyệt vì nợ xấu thì sẽ mất rất nhiều công sức, thời gian của bản thân. Vậy Shinhan Bank hỗ trợ nợ xấu tiếp tục vay tiền là đúng hay sai? Để kích cầu, nhiều mẫu xe đã được giảm giá mạnh, các hãng cũng tung ra chương trình giảm 50% phí trước bạ hoặc giảm trực tiếp tiền mặt để thu hút người mua. Lãi suất cho vay mua ô tô cũng đã giảm đáng kể trong thời gian trở lại đây.
lisinopril 40 coupon: over the counter lisinopril – lisinopril 10mg tablets
https://lisinopril.fun/# price of lisinopril generic
zithromax 600 mg tablets zithromax best price generic zithromax 500mg
http://lisinopril.fun/# prinivil 40 mg
buy lisinopril online canada: lipinpril – buy 40 mg lisinopril
https://finasteride.men/# cheap propecia pills
website: cheapest lisinopril – lisinopril drug
lasix 100mg: lasix side effects – furosemide 100mg
http://furosemide.pro/# lasix 100mg
http://furosemide.pro/# furosemide
cost for 2 mg lisinopril: buy lisinopril online – lisinopril 10mg daily
furosemida lasix 40mg lasix pills
buy misoprostol over the counter: cheap cytotec – cytotec abortion pill
https://azithromycin.store/# zithromax 1000 mg pills
https://finasteride.men/# cost of cheap propecia prices
zithromax generic price: buy zithromax z-pak online – buy generic zithromax online
cost of propecia pill: Buy Finasteride 5mg – propecia for sale
http://lisinopril.fun/# price of zestril 30 mg
propecia without a prescription order propecia for sale cost generic propecia without insurance
lasix 20 mg: Buy Lasix – lasix side effects
https://finasteride.men/# buying generic propecia without insurance
http://furosemide.pro/# lasix online
zestril 2.5: buy lisinopril online – discount zestril
https://misoprostol.shop/# cytotec buy online usa
http://lisinopril.fun/# buy lisinopril 20 mg online canada
purchase cytotec: buy misoprostol – buy cytotec pills
lisinopril tabs 40mg: buy lisinopril online – lisinopril 25
cost propecia without dr prescription Finasteride buy online buying propecia without a prescription
farmacie on line spedizione gratuita: kamagra – farmacie online sicure
https://farmaciaitalia.store/# farmacia online
farmacie online affidabili: farmacia online – acquistare farmaci senza ricetta
https://kamagraitalia.shop/# farmacie online sicure
farmacie online autorizzate elenco avanafil prezzo in farmacia farmacia online piГ№ conveniente
http://avanafilitalia.online/# farmaci senza ricetta elenco
http://tadalafilitalia.pro/# farmacia online migliore
acquistare farmaci senza ricetta: farmacia online miglior prezzo – comprare farmaci online con ricetta
https://avanafilitalia.online/# farmacia online migliore
farmacie online sicure Tadalafil generico farmacia online migliore
farmacie online autorizzate elenco: kamagra gold – migliori farmacie online 2023
http://tadalafilitalia.pro/# acquisto farmaci con ricetta
https://tadalafilitalia.pro/# comprare farmaci online con ricetta
https://farmaciaitalia.store/# farmacie on line spedizione gratuita
esiste il viagra generico in farmacia: viagra generico – alternativa al viagra senza ricetta in farmacia
viagra pfizer 25mg prezzo: viagra senza ricetta – esiste il viagra generico in farmacia
farmacia online senza ricetta avanafil farmaci senza ricetta elenco
farmacie online autorizzate elenco: kamagra gel prezzo – farmacia online migliore
https://avanafilitalia.online/# acquisto farmaci con ricetta
cerco viagra a buon prezzo: sildenafil prezzo – viagra cosa serve
https://farmaciaitalia.store/# acquistare farmaci senza ricetta
http://sildenafilitalia.men/# viagra prezzo farmacia 2023
my canadian pharmacy rx: vipps canadian pharmacy – canadian world pharmacy
indian pharmacy Online medicine home delivery buy medicines online in india
http://canadapharm.shop/# canada pharmacy
canada ed drugs: canadian pharmacy no scripts – onlinepharmaciescanada com
https://indiapharm.life/# pharmacy website india
india pharmacy: buy medicines online in india – indian pharmacy
top 10 pharmacies in india: indian pharmacy – best india pharmacy
canadian pharmacy in canada: pharmacy canadian – reliable canadian pharmacy
http://indiapharm.life/# indian pharmacy online
pharmacy website india: best india pharmacy – indian pharmacy paypal
india online pharmacy best india pharmacy top 10 online pharmacy in india
mexican pharmacy: mexican border pharmacies shipping to usa – mexico pharmacy
https://indiapharm.life/# indian pharmacy paypal
indian pharmacies safe: indian pharmacy – buy medicines online in india
https://indiapharm.life/# top 10 pharmacies in india
purple pharmacy mexico price list: mexico drug stores pharmacies – mexican drugstore online
http://indiapharm.life/# Online medicine order
canadian pharmacy sarasota: online canadian drugstore – canada drugs online review
http://canadapharm.shop/# reputable canadian pharmacy
indian pharmacy: buy prescription drugs from india – indianpharmacy com
https://canadapharm.shop/# escrow pharmacy canada
canadian online pharmacy canadian drug stores canadian pharmacy scam
mexican pharmaceuticals online: pharmacies in mexico that ship to usa – mexican pharmacy
buying prescription drugs in mexico online: pharmacies in mexico that ship to usa – п»їbest mexican online pharmacies
https://mexicanpharm.store/# mexico drug stores pharmacies
canadian drugs online: best online canadian pharmacy – canada pharmacy
canadian neighbor pharmacy: adderall canadian pharmacy – canadapharmacyonline
http://mexicanpharm.store/# pharmacies in mexico that ship to usa
http://indiapharm.life/# Online medicine order
reputable indian online pharmacy: india pharmacy mail order – cheapest online pharmacy india
https://mexicanpharm.store/# mexican pharmacy
online shopping pharmacy india: top online pharmacy india – buy medicines online in india
canada ed drugs canada drugs online reviews canadian pharmacy online store
http://indiapharm.life/# indianpharmacy com
top 10 online pharmacy in india: indianpharmacy com – pharmacy website india
reputable mexican pharmacies online: buying prescription drugs in mexico – purple pharmacy mexico price list
http://mexicanpharm.store/# purple pharmacy mexico price list
http://canadapharm.shop/# legit canadian online pharmacy
https://clomidpharm.shop/# can i purchase generic clomid prices
http://zithromaxpharm.online/# zithromax prescription
buy cytotec pills online cheap: buy cytotec in usa – buy cytotec pills
A pharmacy that feels like family http://nolvadex.pro/# alternative to tamoxifen
http://zithromaxpharm.online/# zithromax for sale usa
Their global presence ensures prompt medication deliveries https://zithromaxpharm.online/# zithromax antibiotic
buy zithromax: zithromax prescription – zithromax 250 mg
where can i buy nolvadex tamoxifen skin changes tamoxifen alternatives
https://prednisonepharm.store/# cost of prednisone
Their commitment to global excellence is unwavering https://clomidpharm.shop/# where to get clomid without rx
5 prednisone in mexico: over the counter prednisone medicine – prednisone tablets 2.5 mg
http://clomidpharm.shop/# cost of cheap clomid tablets
https://zithromaxpharm.online/# buy zithromax
A true asset to our neighborhood http://zithromaxpharm.online/# zithromax online paypal
cytotec pills buy online: buy cytotec pills – buy cytotec online fast delivery
They simplify global healthcare https://nolvadex.pro/# tamoxifen estrogen
http://nolvadex.pro/# tamoxifen hair loss
buy misoprostol over the counter buy misoprostol over the counter purchase cytotec
Their global health resources are unmatched https://prednisonepharm.store/# prednisone uk buy
buy zithromax without prescription online: zithromax price south africa – zithromax prescription
http://cytotec.directory/# purchase cytotec
Always my first choice for international pharmaceutical needs https://clomidpharm.shop/# clomid pill
http://nolvadex.pro/# nolvadex for sale
does tamoxifen cause menopause: nolvadex gynecomastia – tamoxifen moa
https://clomidpharm.shop/# cost of generic clomid without prescription
Their global reach is unmatched https://cytotec.directory/# buy cytotec
https://zithromaxpharm.online/# zithromax online usa no prescription
zithromax 500mg over the counter: zithromax 500 without prescription – purchase zithromax online
Their online refill system is straightforward https://nolvadex.pro/# does tamoxifen cause bone loss
buy cytotec pills online cheap Abortion pills online п»їcytotec pills online
https://cytotec.directory/# cytotec buy online usa
buy prescription drugs prescription meds without the prescriptions buy prescription drugs
best online canadian pharmacy: canadian pharmacy without a prescription – reputable mexican pharmacies online
http://edwithoutdoctorprescription.store/# best ed pills non prescription
cialis without a doctor’s prescription ed meds online without doctor prescription buy prescription drugs without doctor
canadian pharmacies that sell viagra http://reputablepharmacies.online/# reliable canadian online pharmacy
online ed drugs no prescription
http://edwithoutdoctorprescription.store/# viagra without a doctor prescription walmart
buy canadian pharmacy: list of approved canadian pharmacies – cheapest drug prices
ed medications ed pills comparison best ed pills online
ed pills: otc ed pills – cure ed
canadian pharmacy selling viagra pharmacy prices compare online drugstore reviews
buy prescription drugs canada: canada medications – best online pharmacy no prescription
https://edwithoutdoctorprescription.store/# 100mg viagra without a doctor prescription
how to cure ed ed drugs list ed meds
ed medications online: ed treatment pills – best drug for ed
overseas online pharmacy https://edwithoutdoctorprescription.store/# real cialis without a doctor’s prescription
best online canadian pharmacy review
https://edpills.bid/# best ed treatment pills
erectile dysfunction medicines generic ed pills gnc ed pills
https://reputablepharmacies.online/# canadian pharmacy no rx
tadalafil canadian pharmacy: canadian generic pharmacy – aarp recommended canadian online pharmacies
viagra without a doctor prescription how to get prescription drugs without doctor best ed pills non prescription
ed meds online without doctor prescription: best treatment for ed – top ed pills
http://reputablepharmacies.online/# online pharmacies no prescription required pain medication
online ed medications: ed medication – cheapest ed pills
trust online pharmacies best rated canadian online pharmacy best canadian pharmacy for viagra
http://reputablepharmacies.online/# non perscription on line pharmacies
erection pills online: erectile dysfunction medicines – pills for erection
my canadian pharmacy rx buy meds online top 10 online pharmacies
https://reputablepharmacies.online/# canadian pharmaceuticals
online pharmacies legitimate canadian pharmaceuticals online safe canadian pharmacy presription and meds
https://mexicanpharmacy.win/# mexico drug stores pharmacies mexicanpharmacy.win
mexico pharmacies prescription drugs: mexican pharmacy online – mexico pharmacies prescription drugs mexicanpharmacy.win
http://mexicanpharmacy.win/# purple pharmacy mexico price list mexicanpharmacy.win
canadian pharmacy ed medications Canada Pharmacy canadian online drugstore canadianpharmacy.pro
mexican mail order pharmacies: online mexican pharmacy – pharmacies in mexico that ship to usa mexicanpharmacy.win
top online pharmacy india international medicine delivery from india indian pharmacy online indianpharmacy.shop
https://mexicanpharmacy.win/# mexican drugstore online mexicanpharmacy.win
mexico drug stores pharmacies mexican pharmacy online mexican border pharmacies shipping to usa mexicanpharmacy.win
cheapest online pharmacy india: indian pharmacy – india online pharmacy indianpharmacy.shop
https://canadianpharmacy.pro/# online canadian drugstore canadianpharmacy.pro
https://canadianpharmacy.pro/# northwest canadian pharmacy canadianpharmacy.pro
indian pharmacy Order medicine from India to USA mail order pharmacy india indianpharmacy.shop
canadian pharmacy sarasota canada ed drugs canada pharmacy world canadianpharmacy.pro
http://canadianpharmacy.pro/# canada cloud pharmacy canadianpharmacy.pro
http://mexicanpharmacy.win/# mexican online pharmacies prescription drugs mexicanpharmacy.win
indian pharmacy online
http://indianpharmacy.shop/# buy medicines online in india indianpharmacy.shop
compare pharmacy prices
http://mexicanpharmacy.win/# mexico drug stores pharmacies mexicanpharmacy.win
https://mexicanpharmacy.win/# mexico pharmacies prescription drugs mexicanpharmacy.win
best india pharmacy
http://canadianpharmacy.pro/# legit canadian online pharmacy canadianpharmacy.pro
http://indianpharmacy.shop/# indian pharmacy online indianpharmacy.shop
mexican pharmacy online mexican pharmacy buying prescription drugs in mexico mexicanpharmacy.win
https://canadianpharmacy.pro/# my canadian pharmacy canadianpharmacy.pro
indian pharmacies safe
http://mexicanpharmacy.win/# medicine in mexico pharmacies mexicanpharmacy.win
top online pharmacy india international medicine delivery from india Online medicine home delivery indianpharmacy.shop
http://canadianpharmacy.pro/# reddit canadian pharmacy canadianpharmacy.pro
top 10 pharmacies in india
https://mexicanpharmacy.win/# reputable mexican pharmacies online mexicanpharmacy.win
online drugstore without prescription
http://indianpharmacy.shop/# buy medicines online in india indianpharmacy.shop
http://canadianpharmacy.pro/# canadian pharmacy ed medications canadianpharmacy.pro
reputable indian pharmacies
my canadian pharmacy reviews Cheapest drug prices Canada legit canadian pharmacy canadianpharmacy.pro
http://mexicanpharmacy.win/# mexico drug stores pharmacies mexicanpharmacy.win
http://indianpharmacy.shop/# online shopping pharmacy india indianpharmacy.shop
top 10 online pharmacy in india
reputable mexican pharmacies online Medicines Mexico buying prescription drugs in mexico online mexicanpharmacy.win
https://mexicanpharmacy.win/# medication from mexico pharmacy mexicanpharmacy.win
https://indianpharmacy.shop/# mail order pharmacy india indianpharmacy.shop
https://mexicanpharmacy.win/# mexican rx online mexicanpharmacy.win
indian pharmacy paypal
Viagra sans ordonnance 24h Amazon: Viagra sans ordonnance 24h – SildГ©nafil 100 mg sans ordonnance
https://viagrasansordonnance.pro/# Viagra homme prix en pharmacie sans ordonnance
pharmacie ouverte Pharmacie en ligne sans ordonnance Acheter mГ©dicaments sans ordonnance sur internet
https://cialissansordonnance.shop/# Pharmacie en ligne sans ordonnance
п»їpharmacie en ligne
https://acheterkamagra.pro/# Pharmacie en ligne fiable
Pharmacies en ligne certifiГ©es Levitra acheter pharmacie ouverte
Pharmacie en ligne fiable: kamagra livraison 24h – Pharmacie en ligne livraison gratuite
Viagra homme prix en pharmacie sans ordonnance: Viagra sans ordonnance 24h – Meilleur Viagra sans ordonnance 24h
Pharmacies en ligne certifiГ©es PharmaDoc acheter mГ©dicaments Г l’Г©tranger
https://acheterkamagra.pro/# acheter médicaments à l’étranger
Pharmacies en ligne certifiГ©es: Levitra pharmacie en ligne – acheter medicament a l etranger sans ordonnance
http://viagrasansordonnance.pro/# Prix du Viagra en pharmacie en France
Pharmacie en ligne France: pharmacie en ligne pas cher – Pharmacie en ligne France
https://acheterkamagra.pro/# Pharmacie en ligne fiable
acheter mГ©dicaments Г l’Г©tranger
Pharmacie en ligne sans ordonnance acheter kamagra site fiable acheter medicament a l etranger sans ordonnance
https://levitrasansordonnance.pro/# Acheter médicaments sans ordonnance sur internet
Viagra gГ©nГ©rique sans ordonnance en pharmacie: Viagra sans ordonnance 24h – Le gГ©nГ©rique de Viagra
Pharmacie en ligne sans ordonnance: levitra generique prix en pharmacie – Pharmacie en ligne livraison gratuite
https://cialissansordonnance.shop/# Pharmacie en ligne livraison gratuite
Viagra 100mg prix: Viagra generique en pharmacie – Viagra pas cher livraison rapide france
Pharmacie en ligne livraison 24h cialis prix Pharmacie en ligne livraison gratuite
https://viagrasansordonnance.pro/# Viagra homme prix en pharmacie sans ordonnance
Acheter Sildenafil 100mg sans ordonnance: viagra sans ordonnance – SildГ©nafil 100 mg sans ordonnance
order zithromax without prescription: zithromax cost canada – generic zithromax azithromycin
http://azithromycin.bid/# buy zithromax without prescription online
zithromax online how to get zithromax online zithromax pill
amoxicillin 500 mg tablets: order amoxicillin online no prescription – amoxicillin 500mg
http://azithromycin.bid/# buy generic zithromax no prescription
https://azithromycin.bid/# how to get zithromax
cheap clomid price: can you buy cheap clomid no prescription – can i order generic clomid pills
where to buy zithromax in canada: where can i get zithromax – zithromax 1000 mg online
cost of amoxicillin 875 mg how to buy amoxicillin online amoxicillin 500mg capsule buy online
https://azithromycin.bid/# generic zithromax 500mg
topical ivermectin cost: ivermectin buy online – generic ivermectin for humans
where can i buy generic clomid pill buying clomid for sale where can i buy generic clomid without a prescription
http://azithromycin.bid/# average cost of generic zithromax
can i purchase amoxicillin online: purchase amoxicillin 500 mg – buy amoxicillin online uk
amoxicillin online purchase: over the counter amoxicillin – amoxicillin 500
zithromax price canada buy zithromax 1000mg online zithromax 600 mg tablets
http://amoxicillin.bid/# how to get amoxicillin over the counter
https://ivermectin.store/# ivermectin 0.1 uk
can i order clomid online: where can i get generic clomid without rx – can you buy cheap clomid without insurance
where to buy generic clomid now get cheap clomid without insurance where to get clomid without dr prescription
http://prednisonetablets.shop/# prednisone cream brand name
zithromax azithromycin: zithromax generic price – buy cheap generic zithromax
how can i get clomid price: can i get cheap clomid no prescription – where can i get cheap clomid without insurance
https://amoxicillin.bid/# amoxicillin discount coupon
zithromax pill: zithromax 500mg – buy cheap zithromax online
can you buy cheap clomid without rx how to get generic clomid cost of clomid without dr prescription
buy zithromax online: how much is zithromax 250 mg – zithromax 500mg over the counter
http://clomiphene.icu/# can i get clomid pills
https://amoxicillin.bid/# amoxicillin 825 mg
zithromax capsules where can i buy zithromax in canada zithromax tablets
minocycline 100 mg for sale: minocycline 50mg pills online – ivermectin 12 mg
п»їbest mexican online pharmacies: Online Mexican pharmacy – medication from mexico pharmacy mexicanpharm.shop
https://canadianpharm.store/# canadian compounding pharmacy canadianpharm.store
best online pharmacies in mexico Online Mexican pharmacy buying prescription drugs in mexico mexicanpharm.shop
india online pharmacy: indian pharmacies safe – top 10 online pharmacy in india indianpharm.store
india online pharmacy: indian pharmacy paypal – indian pharmacies safe indianpharm.store
reputable indian pharmacies: Indian pharmacy to USA – buy prescription drugs from india indianpharm.store
mexico drug stores pharmacies Online Pharmacies in Mexico п»їbest mexican online pharmacies mexicanpharm.shop
https://indianpharm.store/# cheapest online pharmacy india indianpharm.store
canadian neighbor pharmacy: canadian mail order pharmacy – canadian pharmacy 1 internet online drugstore canadianpharm.store
https://canadianpharm.store/# canadian pharmacy mall canadianpharm.store
mexican border pharmacies shipping to usa: medicine in mexico pharmacies – medication from mexico pharmacy mexicanpharm.shop
buy prescription drugs from canada cheap Canadian International Pharmacy canadianpharmacyworld com canadianpharm.store
mexico drug stores pharmacies: Online Pharmacies in Mexico – mexican rx online mexicanpharm.shop
https://canadianpharm.store/# reliable canadian pharmacy reviews canadianpharm.store
recommended canadian pharmacies: canadian pharmacies online – canadian pharmacy victoza canadianpharm.store
mexican mail order pharmacies Certified Pharmacy from Mexico mexico pharmacies prescription drugs mexicanpharm.shop
https://mexicanpharm.shop/# mexico drug stores pharmacies mexicanpharm.shop
top online pharmacy india: Indian pharmacy to USA – Online medicine order indianpharm.store
canadianpharmacymeds com: vipps canadian pharmacy – canadian pharmacies online canadianpharm.store
http://canadianpharm.store/# canada pharmacy online canadianpharm.store
buying prescription drugs in mexico Online Pharmacies in Mexico purple pharmacy mexico price list mexicanpharm.shop
india pharmacy mail order: international medicine delivery from india – buy prescription drugs from india indianpharm.store
https://mexicanpharm.shop/# mexico pharmacy mexicanpharm.shop
india online pharmacy: order medicine from india to usa – indian pharmacy online indianpharm.store
http://mexicanpharm.shop/# mexico drug stores pharmacies mexicanpharm.shop
buy prescription drugs from india: order medicine from india to usa – india pharmacy indianpharm.store
Online medicine home delivery buy medicines online in india india pharmacy mail order indianpharm.store
mexican border pharmacies shipping to usa: п»їbest mexican online pharmacies – mexican pharmaceuticals online mexicanpharm.shop
best rated canadian pharmacy: Pharmacies in Canada that ship to the US – trustworthy canadian pharmacy canadianpharm.store
canadian pharmacy uk delivery canadian pharmacy world canadian pharmacies that deliver to the us canadianpharm.store
reputable mexican pharmacies online: Online Pharmacies in Mexico – mexico pharmacies prescription drugs mexicanpharm.shop
http://mexicanpharm.shop/# buying from online mexican pharmacy mexicanpharm.shop
http://canadianpharm.store/# canadian drug prices canadianpharm.store
buying prescription drugs in mexico online: Certified Pharmacy from Mexico – mexican drugstore online mexicanpharm.shop
https://mexicanpharm.shop/# mexican border pharmacies shipping to usa mexicanpharm.shop
buying prescription drugs in mexico purple pharmacy mexico price list mexico drug stores pharmacies mexicanpharm.shop
legit canadian pharmacy: Best Canadian online pharmacy – canada pharmacy canadianpharm.store
buying from online mexican pharmacy: Online Pharmacies in Mexico – mexican border pharmacies shipping to usa mexicanpharm.shop
legit canadian pharmacy: Licensed Online Pharmacy – canada pharmacy online canadianpharm.store
https://indianpharm.store/# best online pharmacy india indianpharm.store
online canadian pharmacy reviews Pharmacies in Canada that ship to the US best canadian online pharmacy canadianpharm.store
canada pharmacy world: cheapest pharmacy canada – buy canadian drugs canadianpharm.store
https://canadianpharm.store/# legitimate canadian pharmacies canadianpharm.store
mexico pharmacy Certified Pharmacy from Mexico reputable mexican pharmacies online mexicanpharm.shop
http://indianpharm.store/# indian pharmacy online indianpharm.store
While getting free money sounds too good to be true, no deposit bonuses for bingo are a real thing. And today, you’ll learn everything you need to know before you claim one of these promotions. In addition to ranking the best $5 free bingo sites, we’ll also give you some tips and advice about the best bonus types and how to use them. You can email the site owner to let them know you were blocked. Please include what you were doing when this page came up and the Cloudflare Ray ID found at the bottom of this page. This site contains gambling related content (including but not limited to casino games, poker, bingo, sports betting etc.) and is intended for adults only. You must be 18 years of age or older (or if the age of majority in your place of residence is greater than 18 years, you must have attained the age of majority) to use NoDepositBonus.cc or engage in any of the programs we offer.
https://messiahfdxg122233.designertoblog.com/56094135/article-under-review
412-231-7777 Enhance your Southern California casino experience with exclusive benefits and exciting opportunities. Whether you enjoy playing slot machines, venturing into high limit, or doubling down at table games, join The Club at Pechanga. Named for cigar aficionados and football pros Fred Smerles and Steve DeOssie, Fred & Steve’s Blackstone Cigar Bar cooperates with some top American Spirit Distillers like Tito Handmade Vodka and Thomas Tew Rum to serve hand-crafted cocktails. Confusing things even further, the state of Minnesota has some strange casino regulations, where most casinos are split between “mostly slot machines” and “mostly card games” but for whatever reason, the two are rarely combined. After a day at the casino, why not make it two and stay the night!
legitimate online pharmacy usa: canada drugs without prescription – my canadian family pharmacy
http://canadadrugs.pro/# giant discount pharmacy
my canadian drug store canadian drugs online viagra canada meds
on line pharmacy with no perscriptions: the best canadian online pharmacy – canada medications
legit canadian online pharmacy: best canadian online pharmacy viagra – canadian pharmacy selling viagra
highest rated canadian pharmacy: nabp canadian pharmacy – true canadian pharmacy
http://canadadrugs.pro/# canadian drugs without any prescriptions
canada pharmacies online prescriptions online pharmacy no perscription prescription without a doctor’s prescription
canadian pharmacy prices: androgel canadian pharmacy – canadian drugstore online
http://canadadrugs.pro/# trust online pharmacies
canada pharmacy certified canadian pharmacies verified canadian pharmacy
cheap canadian pharmacy: pharmacy prices compare – safe canadian pharmacy
no prescription pharmacies: usa online pharmacy – online meds
http://canadadrugs.pro/# canadian medication
discount drugs canada: canadian drug company – canada drug pharmacy
azithromycin canadian pharmacy online pharmacy no prescription pharcharmy online no script
http://canadadrugs.pro/# canada medicine
reputable online pharmacy: aarp approved canadian pharmacies – trusted online pharmacy
canadian pharmaceuticals online reviews: canadian pharcharmy – prescription cost comparison
https://canadadrugs.pro/# canadian mail order pharmacy reviews
buy canadian pharmacy: pharmacy drug store online no rx – mail order prescription drugs from canada
superstore pharmacy online: canadian world pharmacy – canadian meds no prescription
prescription drugs online without doctor: non prescription – ed meds without doctor prescription
https://canadadrugs.pro/# canadian pharcharmy reviews
canadapharmacyonline com: pharmacy canada – aarp canadian pharmacies
https://canadadrugs.pro/# canadian pharmacy androgel
recommended canadian pharmacies: trusted canadian pharmacy – canada medications
cheap prescriptions: pharmacy review – mexican drug pharmacy
http://canadadrugs.pro/# no 1 canadian pharmacy
best canadian online pharmacy reviews: order canadian drugs – online prescription
world pharmacy: reliable mexican pharmacies – nabp approved canadian pharmacies
http://canadadrugs.pro/# no rx online pharmacy
http://canadadrugs.pro/# canadian pharmacy certified
mexican pharmacy: aarp canadian pharmacies – online meds without prescription
п»їlegitimate online pharmacies india: cheapest online pharmacy india – online pharmacy india
http://medicinefromindia.store/# indian pharmacy paypal
canada pharmacy reviews cheap canadian pharmacy online buy prescription drugs from canada cheap
online pharmacy india: indian pharmacy online – india pharmacy mail order
buy prescription drugs online: cialis without a doctor prescription – prescription drugs without prior prescription
http://medicinefromindia.store/# cheapest online pharmacy india
ed medication men’s ed pills generic ed drugs
https://canadianinternationalpharmacy.pro/# canadian 24 hour pharmacy
п»їbest mexican online pharmacies: mexico pharmacies prescription drugs – mexico pharmacy
http://edwithoutdoctorprescription.pro/# buy prescription drugs without doctor
ed meds online without prescription or membership ed pills without doctor prescription non prescription ed drugs
https://edpill.cheap/# erectile dysfunction pills
ed medication over the counter erectile dysfunction pills top ed drugs
non prescription ed pills: ed drug prices – best ed medication
http://edwithoutdoctorprescription.pro/# how to get prescription drugs without doctor
non prescription ed pills: generic cialis without a doctor prescription – non prescription ed drugs
buying prescription drugs in mexico online mexico pharmacy mexico pharmacy
http://canadianinternationalpharmacy.pro/# legit canadian pharmacy
http://edpill.cheap/# buying ed pills online
canadian online pharmacy canadian pharmacy legit canadian online pharmacy
canadian pharmacy world: vipps canadian pharmacy – legit canadian pharmacy
http://edwithoutdoctorprescription.pro/# buy prescription drugs online without
mexican rx online: medicine in mexico pharmacies – mexican drugstore online
online shopping pharmacy india world pharmacy india best india pharmacy
https://edpill.cheap/# erectile dysfunction medications
best canadian online pharmacy cheap canadian pharmacy canadian pharmacy 24h com
http://medicinefromindia.store/# buy medicines online in india
viagra without a doctor prescription walmart cialis without a doctor prescription ed meds online without doctor prescription
https://edwithoutdoctorprescription.pro/# ed meds online without doctor prescription
legitimate canadian online pharmacies: canadian pharmacy antibiotics – the canadian drugstore
http://canadianinternationalpharmacy.pro/# canadian online drugstore
best ed drug ed treatment review men’s ed pills
http://medicinefromindia.store/# reputable indian pharmacies
top 10 online pharmacy in india top 10 online pharmacy in india Online medicine home delivery
http://certifiedpharmacymexico.pro/# mexico drug stores pharmacies
medicine in mexico pharmacies mexican pharmaceuticals online п»їbest mexican online pharmacies
reputable indian online pharmacy: buy prescription drugs from india – world pharmacy india
https://medicinefromindia.store/# online shopping pharmacy india
mexico pharmacies prescription drugs buying prescription drugs in mexico mexican border pharmacies shipping to usa
https://edwithoutdoctorprescription.pro/# best non prescription ed pills
medication for ed cheap ed drugs ed pills that work
https://certifiedpharmacymexico.pro/# mexican pharmacy
http://medicinefromindia.store/# buy prescription drugs from india
buying prescription drugs in mexico online: mexico drug stores pharmacies – buying prescription drugs in mexico
cheapest online pharmacy india indianpharmacy com reputable indian pharmacies
https://canadianinternationalpharmacy.pro/# canadian pharmacy online reviews
canadian valley pharmacy legit canadian pharmacy canadian pharmacy world reviews
http://certifiedpharmacymexico.pro/# medication from mexico pharmacy
prescription drugs online without doctor cialis without a doctor prescription canada prescription drugs online without doctor
http://medicinefromindia.store/# india pharmacy
medication from mexico pharmacy mexico pharmacy medicine in mexico pharmacies
medicine in mexico pharmacies buying from online mexican pharmacy mexican online pharmacies prescription drugs
http://mexicanph.shop/# mexican online pharmacies prescription drugs
reputable mexican pharmacies online
mexican border pharmacies shipping to usa reputable mexican pharmacies online mexico drug stores pharmacies
mexico pharmacies prescription drugs mexico drug stores pharmacies best mexican online pharmacies
purple pharmacy mexico price list mexican pharmacy mexico drug stores pharmacies
mexican drugstore online pharmacies in mexico that ship to usa mexican online pharmacies prescription drugs
http://mexicanph.shop/# medicine in mexico pharmacies
buying prescription drugs in mexico
mexico drug stores pharmacies mexico drug stores pharmacies mexican pharmaceuticals online
mexico drug stores pharmacies pharmacies in mexico that ship to usa buying prescription drugs in mexico
medication from mexico pharmacy mexican mail order pharmacies buying prescription drugs in mexico
pharmacies in mexico that ship to usa mexico drug stores pharmacies pharmacies in mexico that ship to usa
https://mexicanph.com/# purple pharmacy mexico price list
reputable mexican pharmacies online
buying prescription drugs in mexico mexican rx online mexican drugstore online
best online pharmacies in mexico medication from mexico pharmacy mexico drug stores pharmacies
п»їbest mexican online pharmacies buying prescription drugs in mexico online mexican online pharmacies prescription drugs
mexican pharmacy mexican border pharmacies shipping to usa mexico pharmacies prescription drugs
http://mexicanph.shop/# medication from mexico pharmacy
mexican mail order pharmacies
mexico drug stores pharmacies medication from mexico pharmacy medicine in mexico pharmacies
buying prescription drugs in mexico online buying prescription drugs in mexico online medicine in mexico pharmacies
mexico pharmacy mexican mail order pharmacies buying prescription drugs in mexico
mexican pharmacy mexican pharmaceuticals online mexican rx online
mexican online pharmacies prescription drugs medication from mexico pharmacy mexican pharmaceuticals online
mexican pharmacy mexican rx online buying prescription drugs in mexico
buying from online mexican pharmacy mexican rx online buying prescription drugs in mexico
mexico pharmacies prescription drugs mexican drugstore online buying prescription drugs in mexico online
https://mexicanph.com/# mexico pharmacies prescription drugs
pharmacies in mexico that ship to usa
buying prescription drugs in mexico mexico drug stores pharmacies mexico pharmacies prescription drugs
mexico drug stores pharmacies reputable mexican pharmacies online mexico pharmacies prescription drugs
mexican pharmaceuticals online reputable mexican pharmacies online mexico drug stores pharmacies
mexico drug stores pharmacies mexican border pharmacies shipping to usa pharmacies in mexico that ship to usa
mexico pharmacy mexican border pharmacies shipping to usa mexico pharmacies prescription drugs
mexican pharmacy pharmacies in mexico that ship to usa best online pharmacies in mexico
mexico drug stores pharmacies mexican online pharmacies prescription drugs reputable mexican pharmacies online
п»їbest mexican online pharmacies mexican pharmaceuticals online mexican pharmaceuticals online
mexican pharmaceuticals online best mexican online pharmacies purple pharmacy mexico price list
http://mexicanph.shop/# mexican online pharmacies prescription drugs
mexican online pharmacies prescription drugs
mexican rx online mexico pharmacy mexican pharmacy
mexico drug stores pharmacies reputable mexican pharmacies online reputable mexican pharmacies online
mexico drug stores pharmacies buying prescription drugs in mexico mexico pharmacy
buying from online mexican pharmacy mexico drug stores pharmacies mexico pharmacy
buying from online mexican pharmacy mexican pharmaceuticals online mexico drug stores pharmacies
pharmacies in mexico that ship to usa mexico drug stores pharmacies medicine in mexico pharmacies
mexican border pharmacies shipping to usa buying prescription drugs in mexico online mexican mail order pharmacies
mexico pharmacies prescription drugs mexican pharmacy buying prescription drugs in mexico
mexico pharmacy mexico drug stores pharmacies mexico pharmacy
mexican border pharmacies shipping to usa mexican drugstore online mexico pharmacies prescription drugs
http://mexicanph.com/# mexican drugstore online
mexican drugstore online
purple pharmacy mexico price list mexico pharmacies prescription drugs mexican drugstore online
purple pharmacy mexico price list mexican online pharmacies prescription drugs mexico pharmacy
mexico pharmacy mexican pharmaceuticals online mexico pharmacy
mexican mail order pharmacies pharmacies in mexico that ship to usa mexico drug stores pharmacies
buying from online mexican pharmacy mexican pharmaceuticals online mexican border pharmacies shipping to usa
pharmacies in mexico that ship to usa mexican pharmacy purple pharmacy mexico price list
purple pharmacy mexico price list mexican pharmaceuticals online mexican drugstore online
pharmacies in mexico that ship to usa mexico drug stores pharmacies mexican drugstore online
purple pharmacy mexico price list п»їbest mexican online pharmacies mexican drugstore online
mexican pharmaceuticals online mexico pharmacy mexican mail order pharmacies
mexico drug stores pharmacies pharmacies in mexico that ship to usa mexico pharmacy
https://mexicanph.com/# buying prescription drugs in mexico online
purple pharmacy mexico price list
mexican drugstore online medicine in mexico pharmacies buying prescription drugs in mexico online
mexican mail order pharmacies pharmacies in mexico that ship to usa mexico drug stores pharmacies
medication from mexico pharmacy pharmacies in mexico that ship to usa mexico pharmacies prescription drugs
best mexican online pharmacies mexico drug stores pharmacies pharmacies in mexico that ship to usa
side effect of metformin
medicine in mexico pharmacies mexican border pharmacies shipping to usa mexican mail order pharmacies
mexico drug stores pharmacies best online pharmacies in mexico mexican border pharmacies shipping to usa
buying prescription drugs in mexico online medication from mexico pharmacy medicine in mexico pharmacies
mexico drug stores pharmacies reputable mexican pharmacies online pharmacies in mexico that ship to usa
mexican pharmacy mexican drugstore online buying prescription drugs in mexico
mexican pharmacy mexican rx online reputable mexican pharmacies online
medication from mexico pharmacy mexican online pharmacies prescription drugs mexican rx online
lisinopril online pharmacy lisinopril 120 mg lisinopril pills 2.5 mg
http://amoxil.cheap/# amoxicillin 800 mg price
http://furosemide.guru/# lasix furosemide 40 mg
lisinopril 5mg buy: lisinopril 25 mg cost – zestoretic 10 mg
ivermectin 3 stromectol uk stromectol coronavirus
http://buyprednisone.store/# prednisone 50
https://lisinopril.top/# buy lisinopril 20 mg without a prescription
canine prednisone 5mg no prescription 20mg prednisone prednisone without a prescription
prednisone buy without prescription: prednisone 60 mg daily – buy prednisone tablets uk
http://buyprednisone.store/# buy prednisone online canada
https://buyprednisone.store/# prednisone 2.5 mg daily
prednisone 50 mg coupon: prednisone 10 mg coupon – cost of prednisone in canada
stromectol xl buy ivermectin uk stromectol otc
https://lisinopril.top/# lisinopril 5 mg tablet cost
purchase ivermectin: ivermectin 1 topical cream – stromectol 3 mg tablets price
https://furosemide.guru/# furosemide 100mg
ivermectin 4 tablets price stromectol tablets buy stromectol online
http://amoxil.cheap/# buy amoxicillin online no prescription
furosemida 40 mg: Buy Lasix – furosemida
medicine amoxicillin 500mg: azithromycin amoxicillin – purchase amoxicillin online without prescription
http://lisinopril.top/# lisinopril 25
http://furosemide.guru/# furosemide 40 mg
ivermectin 5ml ivermectin lotion for scabies ivermectin new zealand
http://lisinopril.top/# lisinopril 5
http://amoxil.cheap/# amoxicillin without a doctors prescription
how to buy stromectol: stromectol tablets uk – how much does ivermectin cost
buy prednisone without a prescription prednisone canada prices prednisone 10 mg canada
http://buyprednisone.store/# prednisone 1 mg daily
https://amoxil.cheap/# price of amoxicillin without insurance
lasix furosemide 40 mg Buy Furosemide furosemida
can you buy prednisone over the counter in canada: prednisone price south africa – prednisone 5 tablets
http://furosemide.guru/# lasix 20 mg
http://buyprednisone.store/# average cost of prednisone
stromectol how much it cost: ivermectin 10 mg – ivermectin 200 mcg
http://amoxil.cheap/# amoxicillin 775 mg
prednisone 10mg tablet price 54 prednisone prednisone cream over the counter
buy lisinopril 40 mg tablet: lisinopril tablets for sale – lisinopril online without prescription
https://buyprednisone.store/# prednisone medication
ivermectin 0.5% lotion: buy ivermectin for humans australia – stromectol for humans
http://buyprednisone.store/# prednisone for cheap
lisinopril 30 mg daily prescription medicine lisinopril lisinopril 0.5 mg
http://amoxil.cheap/# how to buy amoxicillin online
https://lisinopril.top/# zestril 10mg
amoxil generic: amoxicillin 500 tablet – amoxicillin price without insurance
https://lisinopril.top/# price of lisinopril 5mg
amoxicillin in india medicine amoxicillin 500 amoxicillin 875 mg tablet
https://lisinopril.top/# price of zestril 30 mg
prednisone without rx: prednisone 15 mg daily – prednisone drug costs
http://amoxil.cheap/# amoxicillin for sale
zestril 5 mg tablets lisinopril 20mg pill zestril 20 mg cost
http://stromectol.fun/# buy ivermectin stromectol
https://lisinopril.top/# lisinopril tabs 4mg
2.5 mg prednisone daily: prednisone 20mg online without prescription – prednisone online for sale
http://amoxil.cheap/# buy amoxicillin 500mg online
amoxicillin buy no prescription amoxicillin brand name buy amoxicillin online uk
buy lisinopril 20 mg: lisinopril 20 – lisinopril without an rx
https://stromectol.fun/# stromectol ivermectin tablets
https://amoxil.cheap/# generic amoxicillin online
purchase prednisone no prescription: prednisone purchase online – prednisone for sale no prescription
lasix medication Buy Furosemide lasix 40mg
https://buyprednisone.store/# where can i get prednisone over the counter
http://stromectol.fun/# ivermectin 200mg
http://lisinopril.top/# lisinopril 80 mg daily
prednisone 5mg price: prednisone 10mg prices – generic prednisone for sale
http://buyprednisone.store/# prednisone 4 mg daily
amoxicillin discount amoxicillin script where can i buy amoxocillin
glucophage works
http://amoxil.cheap/# amoxicillin 500mg capsule buy online
https://stromectol.fun/# ivermectin purchase
stromectol australia ivermectin cream uk ivermectin canada
lisinopril price: lisinopril 60 mg daily – zestril 25 mg
https://buyprednisone.store/# prednisone 40mg
http://indianph.com/# indianpharmacy com
indian pharmacy paypal
indian pharmacy paypal best online pharmacy india online pharmacy india
https://indianph.xyz/# best online pharmacy india
http://indianph.xyz/# india pharmacy mail order
indian pharmacy
online shopping pharmacy india indian pharmacy paypal india pharmacy
http://indianph.xyz/# indianpharmacy com
online shopping pharmacy india
http://indianph.xyz/# reputable indian pharmacies
india pharmacy mail order
mail order pharmacy india п»їlegitimate online pharmacies india online shopping pharmacy india
http://indianph.com/# Online medicine home delivery
indian pharmacy paypal
http://indianph.xyz/# indian pharmacy
india pharmacy mail order
best online pharmacy india india pharmacy online pharmacy india
top online pharmacy india indian pharmacies safe Online medicine home delivery
http://indianph.xyz/# mail order pharmacy india
indian pharmacy paypal
https://indianph.xyz/# pharmacy website india
http://indianph.xyz/# buy prescription drugs from india
indian pharmacy paypal
http://indianph.com/# best india pharmacy
buy medicines online in india
http://cytotec24.shop/# buy cytotec pills online cheap
nolvadex 20mg tamoxifen vs clomid tamoxifen warning
cytotec buy online usa: buy cytotec pills – buy cytotec
https://diflucan.pro/# diflucan over the counter nz
http://doxycycline.auction/# buy doxycycline without prescription
https://nolvadex.guru/# tamoxifen 20 mg
what happens when you stop taking tamoxifen alternatives to tamoxifen tamoxifen men
http://diflucan.pro/# diflucan without a prescription
diflucan 150mg prescription: buy diflucan without script – buy diflucan uk
https://cipro.guru/# cipro
buy generic doxycycline cheap doxycycline online doxycycline 100mg capsules
https://cipro.guru/# buy ciprofloxacin over the counter
https://cipro.guru/# buy cipro online without prescription
buy cytotec over the counter Misoprostol 200 mg buy online buy cytotec in usa
https://diflucan.pro/# diflucan australia otc
https://cipro.guru/# cipro 500mg best prices
purchase doxycycline online: doxycycline 50mg – doxycycline 100mg
http://doxycycline.auction/# price of doxycycline
ciprofloxacin 500 mg tablet price buy cipro online cipro pharmacy
https://diflucan.pro/# diflucan pill canada
https://nolvadex.guru/# natural alternatives to tamoxifen
http://diflucan.pro/# buy diflucan online no prescription
where can i buy cipro online cipro ciprofloxacin cipro ciprofloxacin
http://cytotec24.com/# buy cytotec pills
http://cytotec24.shop/# buy cytotec pills online cheap
diflucan capsule 150mg diflucan canada coupon 3 diflucan pills
http://diflucan.pro/# diflucan tablet 100 mg
http://cytotec24.com/# cytotec pills buy online
https://doxycycline.auction/# buy doxycycline online uk
doxycycline buy doxycycline without prescription vibramycin 100 mg
http://evaelfie.pro/# eva elfie
tamoxifen and grapefruit tamoxifen and antidepressants tamoxifen warning
https://sweetiefox.online/# sweeti fox
https://lanarhoades.fun/# lana rhoades filmleri
?????? ????: abella danger video – abella danger filmleri
https://evaelfie.pro/# eva elfie modeli
http://lanarhoades.fun/# lana rhoades
http://lanarhoades.fun/# lana rhoades izle
https://lanarhoades.fun/# lana rhoades filmleri
http://abelladanger.online/# abella danger izle
https://lanarhoades.fun/# lana rhoades modeli
https://lanarhoades.fun/# lana rhoades izle
https://sweetiefox.online/# Sweetie Fox izle
http://sweetiefox.online/# swetie fox
http://abelladanger.online/# abella danger filmleri
http://angelawhite.pro/# Angela White izle
https://abelladanger.online/# abella danger video
lana rhodes: lana rhoades video – lana rhoades filmleri
http://angelawhite.pro/# Angela White
https://angelawhite.pro/# Angela White
http://sweetiefox.online/# Sweetie Fox
http://evaelfie.pro/# eva elfie filmleri
https://lanarhoades.fun/# lana rhoades modeli
Angela White video: Angela White – ?????? ????
https://sweetiefox.online/# Sweetie Fox modeli
https://lanarhoades.fun/# lana rhoades video
https://evaelfie.pro/# eva elfie filmleri
Sweetie Fox modeli: Sweetie Fox izle – sweety fox
http://angelawhite.pro/# Angela White izle
http://abelladanger.online/# abella danger video
https://angelawhite.pro/# Angela White video
https://abelladanger.online/# abella danger filmleri
https://abelladanger.online/# abella danger video
http://evaelfie.pro/# eva elfie modeli
https://lanarhoades.fun/# lana rhoades izle
https://sweetiefox.online/# sweety fox
https://angelawhite.pro/# Angela White
http://evaelfie.pro/# eva elfie
https://lanarhoades.fun/# lana rhoades modeli
https://lanarhoades.fun/# lana rhoades filmleri
https://evaelfie.pro/# eva elfie izle
sweetie fox full: fox sweetie – sweetie fox full
https://lanarhoades.pro/# lana rhoades boyfriend
asian dating chat: http://lanarhoades.pro/# lana rhoades pics
mia malkova full video: mia malkova hd – mia malkova
http://evaelfie.site/# eva elfie photo
mia malkova girl: mia malkova movie – mia malkova only fans
internet dating sites: https://evaelfie.site/# eva elfie new videos
mia malkova latest: mia malkova latest – mia malkova new video
eva elfie hot: eva elfie hd – eva elfie full videos
sweetie fox video: sweetie fox new – sweetie fox video
eva elfie new videos: eva elfie new video – eva elfie videos
senior dating sites free: https://sweetiefox.pro/# fox sweetie
mia malkova photos: mia malkova photos – mia malkova hd
mia malkova full video: mia malkova movie – mia malkova movie
eva elfie: eva elfie photo – eva elfie hd
who is brent rivera dating: http://lanarhoades.pro/# lana rhoades boyfriend
fox sweetie: sweetie fox full – ph sweetie fox
mia malkova only fans: mia malkova hd – mia malkova girl
eva elfie videos: eva elfie videos – eva elfie hot
dating websites free: https://lanarhoades.pro/# lana rhoades
sweetie fox full: sweetie fox cosplay – sweetie fox video
eva elfie new video: eva elfie videos – eva elfie full video
fox sweetie: sweetie fox video – fox sweetie
pof dating site: http://evaelfie.site/# eva elfie hot
fox sweetie: fox sweetie – sweetie fox new
eva elfie videos: eva elfie full videos – eva elfie new videos
eva elfie full videos: eva elfie hd – eva elfie new video
http://miamalkova.life/# mia malkova movie
aviator sportybet ghana: aviator – aviator sportybet ghana
aviator betting game: aviator – aviator game bet
https://aviatorjogar.online/# pin up aviator
como jogar aviator: aviator moçambique – aviator
https://aviatormalawi.online/# aviator game
aviator game: aviator – aviator sportybet ghana
pin up casino: pin up casino – pin-up cassino
aviator bet: aviator – aviator mz
https://aviatormocambique.site/# jogar aviator
aviator hilesi: pin up aviator – pin up aviator
aviator pin up casino: cassino pin up – pin up cassino online
https://aviatorjogar.online/# pin up aviator
aviator bahis: aviator oyunu – aviator
jogo de aposta: jogo de aposta online – jogo de aposta
aviator login: aviator ghana – aviator bet
aviator bet: play aviator – play aviator
play aviator: aviator game bet – aviator login
http://jogodeaposta.fun/# melhor jogo de aposta para ganhar dinheiro
aviator: aviator oyna – aviator hilesi
aviator hilesi: aviator oyunu – aviator oyna
aviator: aviator bet malawi – aviator bet
aviator malawi: aviator game online – aviator betting game
http://aviatormalawi.online/# aviator bet malawi login
aviator bet malawi login: play aviator – aviator betting game
zithromax pill – https://azithromycin.pro/pfizer-zithromax.html can i buy zithromax over the counter in canada
jogo de aposta online: depósito mínimo 1 real – aviator jogo de aposta
zithromax coupon: zithromax 500 tablet – zithromax for sale usa
http://aviatoroyunu.pro/# aviator hilesi
pin up aviator: aviator oyna – aviator oyna slot
aviator jogar: aviator jogar – aviator bet
where can i get zithromax over the counter – https://azithromycin.pro/zithromax-tri-pak.html how to get zithromax
aplicativo de aposta: melhor jogo de aposta – depósito mínimo 1 real
canadian pharmacy checker: Pharmacies in Canada that ship to the US – ed drugs online from canada canadianpharm.store
buying from online mexican pharmacy mexican pharmacy medicine in mexico pharmacies mexicanpharm.shop
https://mexicanpharm24.com/# buying prescription drugs in mexico online mexicanpharm.shop
buying prescription drugs in mexico: mexican pharmacy – mexican online pharmacies prescription drugs mexicanpharm.shop
indian pharmacies safe: cheapest online pharmacy india – indian pharmacy indianpharm.store
buying prescription drugs in mexico Mexico pharmacy price list mexico drug stores pharmacies mexicanpharm.shop
https://mexicanpharm24.com/# buying from online mexican pharmacy mexicanpharm.shop
prescription drugs canada buy online: International Pharmacy delivery – legitimate canadian mail order pharmacy canadianpharm.store
https://mexicanpharm24.shop/# buying prescription drugs in mexico online mexicanpharm.shop
canada online pharmacy: My Canadian pharmacy – canadian online pharmacy canadianpharm.store
http://canadianpharmlk.com/# pharmacy com canada canadianpharm.store
http://indianpharm24.com/# cheapest online pharmacy india indianpharm.store
https://indianpharm24.shop/# world pharmacy india indianpharm.store
top online pharmacy india: Online India pharmacy – india online pharmacy indianpharm.store
buy drugs from canada canadian pharmacy canadian compounding pharmacy canadianpharm.store
https://mexicanpharm24.com/# best mexican online pharmacies mexicanpharm.shop
https://indianpharm24.com/# india pharmacy indianpharm.store
https://canadianpharmlk.com/# canadian neighbor pharmacy canadianpharm.store
best online pharmacies in mexico: Medicines Mexico – pharmacies in mexico that ship to usa mexicanpharm.shop
https://indianpharm24.com/# india pharmacy indianpharm.store
https://mexicanpharm24.com/# buying prescription drugs in mexico mexicanpharm.shop
purple pharmacy mexico price list: order online from a Mexican pharmacy – mexico drug stores pharmacies mexicanpharm.shop
https://canadianpharmlk.shop/# best canadian pharmacy online canadianpharm.store
best online pharmacies in mexico: Mexico pharmacy online – mexican mail order pharmacies mexicanpharm.shop
https://indianpharm24.shop/# online pharmacy india indianpharm.store
http://mexicanpharm24.com/# purple pharmacy mexico price list mexicanpharm.shop
canadian pharmacies online CIPA approved pharmacies medication canadian pharmacy canadianpharm.store
http://canadianpharmlk.shop/# my canadian pharmacy rx canadianpharm.store
п»їlegitimate online pharmacies india: india pharmacy – indian pharmacies safe indianpharm.store
http://canadianpharmlk.shop/# best rated canadian pharmacy canadianpharm.store
http://canadianpharmlk.shop/# legitimate canadian online pharmacies canadianpharm.store
http://indianpharm24.shop/# best india pharmacy indianpharm.store
http://indianpharm24.com/# reputable indian online pharmacy indianpharm.store
Online medicine order: online pharmacy usa – world pharmacy india indianpharm.store
best india pharmacy: Generic Medicine India to USA – top 10 pharmacies in india indianpharm.store
http://indianpharm24.com/# mail order pharmacy india indianpharm.store
https://indianpharm24.com/# online shopping pharmacy india indianpharm.store
https://canadianpharmlk.com/# canada drug pharmacy canadianpharm.store
best canadian online pharmacy reviews canadian pharmacy canadian discount pharmacy canadianpharm.store
order generic clomid tablets: when do you take clomid – where buy cheap clomid without rx
prednisone 5 mg tablet price: does prednisone make you tired – 10 mg prednisone tablets
can you get generic clomid tablets: how to buy generic clomid online – cost of clomid for sale
https://clomidst.pro/# can you buy clomid for sale
where to get generic clomid pills where buy cheap clomid now where to get cheap clomid without a prescription
where can i get cheap clomid price: where buy cheap clomid no prescription – can i get clomid online
where to buy clomid no prescription: online doctor to prescribe clomid – where to get clomid without rx
amoxicillin 500mg no prescription: cost of amoxicillin prescription – amoxicillin 500 capsule
http://clomidst.pro/# where to buy generic clomid without insurance
prednisone capsules: prednisone side effects – buying prednisone without prescription
prednisone 5 mg tablet without a prescription: does prednisone cause weight gain – 20mg prednisone
where can you buy amoxicillin over the counter: over the counter amoxicillin canada – amoxicillin without a prescription
http://prednisonest.pro/# prednisone 10mg buy online
buy prednisone without a prescription: prednisone price south africa – where to buy prednisone 20mg no prescription
amoxicillin 500mg no prescription amoxicillin 500 mg where to buy amoxicillin 500mg pill
where to buy cheap clomid without prescription: alternative to clomid – where can i buy clomid without prescription
can i order cheap clomid: get cheap clomid price – where can i buy generic clomid pills
how much is amoxicillin prescription: amoxicillin dosage by weight – buy amoxicillin online with paypal
how to buy generic clomid no prescription: can i get cheap clomid pills – can you buy cheap clomid pill
https://amoxilst.pro/# where to buy amoxicillin 500mg without prescription
buy amoxicillin 500mg capsules uk: where can i get amoxicillin 500 mg – how to buy amoxicillin online
http://amoxilst.pro/# buy amoxicillin online uk
prednisone coupon: prednisone 10 mg canada – prednisone 10 mg tablets
order generic clomid no prescription: femara vs clomid – where can i buy generic clomid without prescription
generic amoxil 500 mg: amoxicillin capsule 500mg price – purchase amoxicillin online without prescription
how to get cheap clomid: where to get generic clomid pill – can you get clomid without a prescription
order generic clomid pill buying generic clomid without dr prescription can you get cheap clomid no prescription
prednisone 20mg price in india: order prednisone 100g online without prescription – prednisone 5mg price
https://prednisonest.pro/# where to buy prednisone uk
generic amoxil 500 mg: buy amoxicillin 500mg usa – generic amoxicillin
cost of clomid no prescription: best days to take clomid for twins forum – where to buy cheap clomid online
online ed meds: buy ed pills online – online ed medicine
http://edpills.guru/# where to buy ed pills
buy medication online without prescription: prescription online canada – how to get prescription drugs from canada
https://edpills.guru/# how to get ed pills
canadian pharmacy without prescription: online pharmacy delivery – canada pharmacy coupon
online pharmacy no prescription canada online pharmacy promo code for canadian pharmacy meds
п»їed pills online: online prescription for ed – pills for ed online
medication online without prescription: best online pharmacy without prescriptions – buying drugs without prescription
http://onlinepharmacy.cheap/# no prescription needed pharmacy
https://edpills.guru/# pills for ed online
buy erectile dysfunction medication: low cost ed medication – cheap ed meds online
ed meds cheap: best online ed medication – п»їed pills online
where to buy ed pills: buy ed pills online – ed pills online
http://onlinepharmacy.cheap/# online pharmacy discount code
rxpharmacycoupons: canadian pharmacy online – canadian pharmacy coupon code
https://onlinepharmacy.cheap/# canadian pharmacy no prescription needed
ed meds cheap cheap ed medicine ed treatment online
canadian drugs no prescription: online pharmacy no prescriptions – no prescription needed online pharmacy
canadian pharmacy non prescription: overseas online pharmacy-no prescription – no prescription online pharmacy
ed medicines: online ed treatments – cheap ed pills
http://onlinepharmacy.cheap/# legit non prescription pharmacies
no prescription needed pharmacy: canada online pharmacy – canada online pharmacy no prescription
non prescription canadian pharmacy: legitimate online pharmacy no prescription – buying prescription drugs online canada
https://pharmnoprescription.pro/# online pharmacies without prescriptions
http://edpills.guru/# cheap boner pills
foreign pharmacy no prescription: mexican online pharmacy – legal online pharmacy coupon code
erectile dysfunction pills online: where to buy ed pills – cheap ed
mexican rx online: reputable mexican pharmacies online – best online pharmacies in mexico
legitimate online pharmacy no prescription: canada prescription drugs online – no prescription needed
no prescription online pharmacy canada drugs no prescription buy prescription drugs online without doctor
http://mexicanpharm.online/# buying prescription drugs in mexico online
world pharmacy india: top 10 online pharmacy in india – india pharmacy
http://pharmacynoprescription.pro/# buy drugs online without a prescription
mexican rx online: pharmacies in mexico that ship to usa – mexico drug stores pharmacies
п»їbest mexican online pharmacies: mexican drugstore online – п»їbest mexican online pharmacies
https://pharmacynoprescription.pro/# no prescription pharmacy
https://mexicanpharm.online/# buying prescription drugs in mexico online
medication from mexico pharmacy mexican border pharmacies shipping to usa purple pharmacy mexico price list
canadapharmacyonline: canadian pharmacy 24h com safe – reddit canadian pharmacy
п»їlegitimate online pharmacies india: cheapest online pharmacy india – indian pharmacy paypal
http://canadianpharm.guru/# canadian family pharmacy
indian pharmacy paypal: reputable indian pharmacies – india pharmacy mail order
buy prescription drugs from india: reputable indian online pharmacy – cheapest online pharmacy india
https://indianpharm.shop/# indian pharmacy
cheapest online pharmacy india: top 10 online pharmacy in india – india pharmacy mail order
canadian 24 hour pharmacy: canadian pharmacy uk delivery – canada pharmacy 24h
indianpharmacy com: world pharmacy india – cheapest online pharmacy india
indianpharmacy com: buy medicines online in india – best online pharmacy india
http://canadianpharm.guru/# cheap canadian pharmacy online
http://pharmacynoprescription.pro/# online pharmacies without prescription
best india pharmacy: reputable indian online pharmacy – india pharmacy mail order
buy medicines online in india: best india pharmacy – buy medicines online in india
reputable indian online pharmacy world pharmacy india mail order pharmacy india
meds online no prescription: online medication no prescription – no prescription pharmacy
https://pharmacynoprescription.pro/# medicine with no prescription
Online medicine order: top online pharmacy india – best online pharmacy india
top 10 pharmacies in india: buy medicines online in india – buy medicines online in india
ordering drugs from canada: legitimate canadian pharmacy – legit canadian online pharmacy
https://mexicanpharm.online/# reputable mexican pharmacies online
mexican mail order pharmacies: buying prescription drugs in mexico online – mexican pharmaceuticals online
https://mexicanpharm.online/# best online pharmacies in mexico
canadian pharmacy scam: canadian pharmacy com – pharmacy canadian superstore
buy drugs online no prescription: canadian pharmacy non prescription – canadian drugs no prescription
online meds without prescription canada prescription drugs online buy drugs online without prescription
onlinepharmaciescanada com: canadapharmacyonline legit – canadian pharmacy ratings
top 10 online pharmacy in india: indianpharmacy com – top 10 online pharmacy in india
pharmacies in mexico that ship to usa: mexican online pharmacies prescription drugs – medicine in mexico pharmacies
http://canadianpharm.guru/# canadian pharmacy online
purple pharmacy mexico price list: medication from mexico pharmacy – mexican online pharmacies prescription drugs
india online pharmacy: indian pharmacy online – india pharmacy
pharmacy no prescription required: non prescription pharmacy – canadian pharmacy online no prescription needed
http://mexicanpharm.online/# medication from mexico pharmacy
buy prescription drugs from india: indianpharmacy com – best online pharmacy india
http://indianpharm.shop/# mail order pharmacy india
online shopping pharmacy india: buy prescription drugs from india – Online medicine home delivery
top online pharmacy india reputable indian online pharmacy Online medicine home delivery
https://mexicanpharm.online/# pharmacies in mexico that ship to usa
mexican mail order pharmacies: mexican drugstore online – pharmacies in mexico that ship to usa
online pharmacy india: top online pharmacy india – Online medicine order
canadian drugs online: vipps canadian pharmacy – online canadian pharmacy review
indianpharmacy com: mail order pharmacy india – Online medicine home delivery
http://canadianpharm.guru/# legit canadian pharmacy
best online pharmacy without prescription: online meds no prescription – no prescription needed pharmacy
online prescription canada: buying drugs online no prescription – buy medication online without prescription
vipps approved canadian online pharmacy: canadian world pharmacy – canada rx pharmacy world
https://canadianpharm.guru/# canadian pharmacy ed medications
http://mexicanpharm.online/# buying from online mexican pharmacy
canadian online pharmacy: best rated canadian pharmacy – legitimate canadian online pharmacies
legal to buy prescription drugs from canada canadian online pharmacy adderall canadian pharmacy
top online pharmacy india: reputable indian online pharmacy – india pharmacy mail order
reputable mexican pharmacies online: pharmacies in mexico that ship to usa – buying from online mexican pharmacy
https://indianpharm.shop/# mail order pharmacy india
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
online meds without prescription: buying online prescription drugs – medication online without prescription
canadian pharmacies: ed meds online canada – canadian pharmacy meds
canadian pharmacy no prescription needed: prescription canada – canadian pharmacy no prescription needed
https://pharmacynoprescription.pro/# order prescription drugs online without doctor
best online pharmacies without prescription: online drugs without prescription – buying online prescription drugs
http://gatesofolympus.auction/# gates of olympus oyna ücretsiz
https://slotsiteleri.guru/# en guvenilir slot siteleri
http://pinupgiris.fun/# pin-up casino giris
2024 en iyi slot siteleri: en iyi slot siteleri 2024 – slot oyun siteleri
sweet bonanza yorumlar: guncel sweet bonanza – sweet bonanza taktik
http://aviatoroyna.bid/# aviator hilesi
http://gatesofolympus.auction/# gates of olympus demo
https://gatesofolympus.auction/# gates of olympus taktik
gates of olympus demo turkce: gates of olympus s?rlar? – gate of olympus hile
pin up aviator: pin-up online – pin up
http://pinupgiris.fun/# pin up aviator
aviator sinyal hilesi apk: aviator casino oyunu – aviator hilesi
https://slotsiteleri.guru/# yasal slot siteleri
https://aviatoroyna.bid/# aviator ucak oyunu
pin-up casino giris: pin-up casino giris – pin-up casino indir
http://slotsiteleri.guru/# en güvenilir slot siteleri
https://aviatoroyna.bid/# aviator nasil oynanir
pin-up casino indir: pin up indir – pin up
gates of olympus demo turkce: gates of olympus demo turkce – gates of olympus max win
https://pinupgiris.fun/# pin-up giris
https://aviatoroyna.bid/# aviator oyunu 50 tl
http://pinupgiris.fun/# aviator pin up
aviator sinyal hilesi apk: aviator sinyal hilesi – aviator sinyal hilesi ucretsiz
https://aviatoroyna.bid/# aviator oyunu
aviator casino oyunu: aviator ucak oyunu – aviator casino oyunu
http://gatesofolympus.auction/# gates of olympus demo türkçe oyna
sweet bonanza 100 tl: sweet bonanza bahis – sweet bonanza free spin demo
aviator sinyal hilesi ucretsiz: aviator hilesi – aviator oyna slot
https://gatesofolympus.auction/# gates of olympus taktik
http://sweetbonanza.bid/# sweet bonanza bahis
slot siteleri guvenilir: guvenilir slot siteleri – yeni slot siteleri
http://aviatoroyna.bid/# aviator sinyal hilesi ucretsiz
http://sweetbonanza.bid/# sweet bonanza yasal site
slot siteleri guvenilir: slot siteleri – slot siteleri
aviator: aviator hile – aviator oyunu
mexico drug stores pharmacies cheapest mexico drugs medication from mexico pharmacy
mexico pharmacy: pharmacies in mexico that ship to usa – mexican border pharmacies shipping to usa
http://indianpharmacy.icu/# online pharmacy india
indian pharmacy Healthcare and medicines from India indian pharmacy paypal
mexican online pharmacies prescription drugs: Online Pharmacies in Mexico – mexican online pharmacies prescription drugs
mexico pharmacies prescription drugs: mexico pharmacy – mexico drug stores pharmacies
online canadian pharmacy reviews Certified Canadian Pharmacy ordering drugs from canada
http://indianpharmacy.icu/# best india pharmacy
online shopping pharmacy india: Healthcare and medicines from India – best india pharmacy
mexico pharmacies prescription drugs Mexican Pharmacy Online mexican mail order pharmacies
canadian pharmacy online reviews: Large Selection of Medications – canadian king pharmacy
best online pharmacy india: Generic Medicine India to USA – Online medicine home delivery
buying from online mexican pharmacy: mexico pharmacy – п»їbest mexican online pharmacies
mexican border pharmacies shipping to usa: mexico pharmacy – mexico drug stores pharmacies
best canadian online pharmacy Licensed Canadian Pharmacy escrow pharmacy canada
pharmacies in mexico that ship to usa: mexican pharmacy – buying prescription drugs in mexico
mexico drug stores pharmacies: mexican pharmacy – mexican border pharmacies shipping to usa
canada rx pharmacy world canada pharmacy world canadian family pharmacy
https://canadianpharmacy24.store/# canadian mail order pharmacy
canadian pharmacy scam: Large Selection of Medications – canadian pharmacy prices
mexico drug stores pharmacies: Online Pharmacies in Mexico – buying prescription drugs in mexico
buying drugs from canada: canadapharmacyonline legit – canadian pharmacies online
canadian pharmacies compare Certified Canadian Pharmacy canadian pharmacy king
safe canadian pharmacy: canadian pharmacy price checker – www canadianonlinepharmacy
best canadian pharmacy to order from: Licensed Canadian Pharmacy – canadian pharmacy ltd
mexico drug stores pharmacies: Mexican Pharmacy Online – mexican pharmacy
canadian pharmacies compare canadian pharmacy 24 northwest pharmacy canada
mexican mail order pharmacies mexico pharmacy mexican mail order pharmacies
https://canadianpharmacy24.store/# cheap canadian pharmacy
reputable indian pharmacies: Cheapest online pharmacy – mail order pharmacy india
mexican border pharmacies shipping to usa: mexican pharmacy – reputable mexican pharmacies online
india pharmacy indian pharmacy delivery pharmacy website india
top online pharmacy india: Cheapest online pharmacy – pharmacy website india
buy prescription drugs from india: reputable indian pharmacies – pharmacy website india
india pharmacy: indian pharmacy delivery – cheapest online pharmacy india
legitimate online pharmacies india: Cheapest online pharmacy – reputable indian online pharmacy
https://clomidall.shop/# where can i buy generic clomid
prednisone tablets india: prednisone 5084 – prednisone 40mg
how can i get generic clomid online can i order cheap clomid without rx can you buy generic clomid without prescription
buy amoxicillin online no prescription: amoxicillin online canada – can you buy amoxicillin uk
https://clomidall.com/# can i buy clomid
https://prednisoneall.com/# prednisone tablets 2.5 mg
http://clomidall.com/# can i buy generic clomid without a prescription
buy 10 mg prednisone prednisone 2.5 mg generic prednisone tablets
http://clomidall.shop/# clomid generic
https://clomidall.com/# can you get clomid now
prednisone daily use where to buy prednisone in australia cost of prednisone 40 mg
https://clomidall.com/# cost of clomid pill
https://clomidall.com/# can i purchase clomid now
amoxicillin online no prescription amoxicillin 30 capsules price buy amoxicillin 500mg
amoxicillin 30 capsules price: amoxicillin cephalexin – amoxicillin from canada
where can i purchase zithromax online: zithromax for sale 500 mg – zithromax 500 mg lowest price online
https://prednisoneall.shop/# prednisone oral
zithromax z-pak price without insurance buy zithromax without presc zithromax 250 mg tablet price
https://prednisoneall.com/# prednisone prices
http://zithromaxall.com/# zithromax 500
http://zithromaxall.shop/# buy generic zithromax online
20 mg prednisone prednisone 20 mg prednisone 1 mg tablet
http://amoxilall.shop/# amoxicillin script
https://clomidall.com/# can i purchase generic clomid without rx
amoxicillin online without prescription: buy amoxicillin online without prescription – buy cheap amoxicillin
http://zithromaxall.com/# zithromax antibiotic
amoxicillin online no prescription: buying amoxicillin online – amoxicillin without rx
http://prednisoneall.com/# prednisone 5 50mg tablet price
zithromax buy online no prescription where can i buy zithromax capsules zithromax 500mg over the counter
http://amoxilall.com/# buy amoxicillin 250mg
http://prednisoneall.shop/# where to buy prednisone 20mg no prescription
http://clomidall.shop/# clomid cheap
buy generic zithromax no prescription buy zithromax online fast shipping zithromax azithromycin
http://clomidall.shop/# cheap clomid no prescription
Kamagra 100mg price: Kamagra Oral Jelly Price – Kamagra 100mg
Generic Cialis price Cialis over the counter buy cialis pill
Cialis 20mg price: cheapest cialis – Buy Tadalafil 10mg
https://sildenafiliq.xyz/# buy viagra here
Kamagra tablets: Kamagra Oral Jelly Price – Kamagra 100mg price
Cialis 20mg price in USA cheapest cialis Generic Tadalafil 20mg price
http://tadalafiliq.shop/# buy cialis pill
Cialis without a doctor prescription: Generic Cialis without a doctor prescription – Cialis over the counter
http://kamagraiq.com/# buy Kamagra
Tadalafil price: tadalafil iq – cialis for sale
Viagra tablet online best price on viagra Cheap generic Viagra
Cheap Viagra 100mg: generic ed pills – Cheap Sildenafil 100mg
Kamagra Oral Jelly: Kamagra Iq – buy kamagra online usa
cheapest cialis Buy Cialis online п»їcialis generic
cheapest cialis: cheapest cialis – cialis generic
http://sildenafiliq.com/# best price for viagra 100mg
http://kamagraiq.shop/# buy Kamagra
cheap kamagra: Kamagra Iq – super kamagra
Kamagra tablets Kamagra Iq super kamagra
Generic Viagra online: best price on viagra – Buy Viagra online cheap
п»їkamagra: kamagra best price – Kamagra 100mg price
sildenafil oral jelly 100mg kamagra: Sildenafil Oral Jelly – Kamagra tablets
Cialis without a doctor prescription cialis without a doctor prescription Buy Cialis online
http://tadalafiliq.shop/# Cialis over the counter
Viagra online price: cheapest viagra – Viagra tablet online
https://kamagraiq.com/# Kamagra 100mg price
buy Viagra online viagra canada sildenafil 50 mg price
https://sildenafiliq.com/# Viagra tablet online
Buy Tadalafil 20mg: cialis best price – Cialis 20mg price
kamagra: Kamagra Oral Jelly Price – Kamagra 100mg price
https://kamagraiq.shop/# Kamagra 100mg price
Cialis 20mg price tadalafil iq Tadalafil Tablet
generic sildenafil: buy viagra online – Buy generic 100mg Viagra online
http://tadalafiliq.shop/# Tadalafil price
Buy Tadalafil 5mg: cialis best price – Tadalafil Tablet
buy cialis pill Buy Cialis online п»їcialis generic
Buy Cialis online: tadalafil iq – п»їcialis generic
https://tadalafiliq.shop/# Cialis over the counter
Cialis 20mg price in USA: tadalafil iq – Buy Tadalafil 5mg
http://tadalafiliq.shop/# Buy Cialis online
https://tadalafiliq.com/# Buy Cialis online
Generic Cialis price cialis best price Cialis without a doctor prescription
Sildenafil Citrate Tablets 100mg: cheapest viagra – Viagra without a doctor prescription Canada
https://sildenafiliq.com/# Viagra Tablet price
https://tadalafiliq.shop/# Cheap Cialis
Buy Cialis online: Tadalafil Tablet – Buy Tadalafil 20mg
sildenafil 50 mg price best price on viagra Viagra Tablet price
http://mexicanpharmgrx.com/# mexico pharmacies prescription drugs
onlinepharmaciescanada com Cheapest drug prices Canada recommended canadian pharmacies
purple pharmacy mexico price list: mexican pharmacy – pharmacies in mexico that ship to usa
buy prescription drugs from india: Healthcare and medicines from India – Online medicine home delivery
http://canadianpharmgrx.com/# online canadian pharmacy
canadian drug stores: Best Canadian online pharmacy – escrow pharmacy canada
canadian pharmacy CIPA approved pharmacies precription drugs from canada
http://indianpharmgrx.shop/# indian pharmacy paypal
Online medicine home delivery Healthcare and medicines from India online shopping pharmacy india
http://canadianpharmgrx.com/# canadian neighbor pharmacy
reputable mexican pharmacies online: buying from online mexican pharmacy – mexico pharmacy
http://indianpharmgrx.shop/# top 10 pharmacies in india
mexican drugstore online mexican pharmacy mexican mail order pharmacies
indian pharmacy: Generic Medicine India to USA – indian pharmacy online
http://indianpharmgrx.com/# india pharmacy
Online medicine order: Generic Medicine India to USA – buy prescription drugs from india
online shopping pharmacy india indian pharmacy online Online medicine order
http://indianpharmgrx.com/# indianpharmacy com
reputable mexican pharmacies online: Pills from Mexican Pharmacy – mexican drugstore online
canadian pharmacy online store My Canadian pharmacy northwest canadian pharmacy
http://mexicanpharmgrx.shop/# buying prescription drugs in mexico online
best online pharmacy india indian pharmacy top 10 pharmacies in india
http://canadianpharmgrx.com/# canada pharmacy 24h
п»їbest mexican online pharmacies: Mexico drugstore – reputable mexican pharmacies online
reputable indian pharmacies: india pharmacy – Online medicine home delivery
https://canadianpharmgrx.com/# canadian drugs
buying from online mexican pharmacy pharmacies in mexico that ship to usa mexican drugstore online
cheapest online pharmacy india: indian pharmacy – world pharmacy india
http://mexicanpharmgrx.shop/# mexico drug stores pharmacies
http://canadianpharmgrx.xyz/# canadian 24 hour pharmacy
rate canadian pharmacies Pharmacies in Canada that ship to the US canadian pharmacy
legitimate canadian pharmacies: Cheapest drug prices Canada – canadian pharmacy prices
https://mexicanpharmgrx.shop/# mexican mail order pharmacies
reputable indian pharmacies: indian pharmacy delivery – india pharmacy
online pharmacy india Healthcare and medicines from India reputable indian pharmacies
https://canadianpharmgrx.com/# best canadian pharmacy online
https://canadianpharmgrx.com/# canadian discount pharmacy
india online pharmacy: Healthcare and medicines from India – reputable indian online pharmacy
mexican drugstore online: mexican pharmacy – mexican rx online
buy cytotec online: buy cytotec online – cytotec buy online usa
doxycycline tetracycline buy doxycycline online without prescription doxycycline 100mg dogs
ciprofloxacin: cipro online no prescription in the usa – cipro for sale
http://doxycyclinest.pro/# doxy
buy cytotec pills Cytotec 200mcg price Misoprostol 200 mg buy online
doxycycline monohydrate: how to order doxycycline – doxycycline prices
diflucan tablets buy online: diflucan 150 mg price in india – diflucan generic costs
cytotec abortion pill cytotec buy online usa buy cytotec
buy cytotec in usa: cytotec pills buy online – cytotec pills buy online
doxycycline 50mg: doxycycline without prescription – 200 mg doxycycline
cytotec buy online usa: buy cytotec pills – Abortion pills online
nolvadex steroids tamoxifen bone density what is tamoxifen used for
cipro online no prescription in the usa: ciprofloxacin order online – cipro for sale
ciprofloxacin: buy ciprofloxacin – ciprofloxacin order online
buy misoprostol over the counter Cytotec 200mcg price buy cytotec pills online cheap
http://misoprostol.top/# order cytotec online
Abortion pills online: cytotec buy online usa – purchase cytotec
Abortion pills online: buy cytotec – cytotec abortion pill
buy generic ciprofloxacin: cipro 500mg best prices – buy ciprofloxacin over the counter
effexor and tamoxifen nolvadex during cycle nolvadex only pct
buy cytotec: buy cytotec over the counter – Abortion pills online
nolvadex generic: tamoxifen cyp2d6 – benefits of tamoxifen
buy ciprofloxacin tablets: buy cipro online canada – buy cipro online canada
doxycycline 100mg doxy 200 order doxycycline 100mg without prescription
buy cytotec online fast delivery: buy cytotec in usa – Abortion pills online
https://doxycyclinest.pro/# doxycycline tetracycline
doxycycline online: buy doxycycline without prescription uk – doxycycline without a prescription
doxycycline doxycycline hyc 100mg buy generic doxycycline
buy cytotec over the counter: buy cytotec over the counter – Cytotec 200mcg price
cytotec online: cytotec online – cytotec abortion pill
tamoxifen rash tamoxifen cyp2d6 tamoxifen and osteoporosis
cytotec buy online usa: buy cytotec over the counter – Misoprostol 200 mg buy online
generic doxycycline: buy doxycycline online uk – buy doxycycline without prescription
buy cheap doxycycline: doxycycline – how to buy doxycycline online
buy cytotec pills online cheap: order cytotec online – cytotec pills buy online
http://diflucan.icu/# can i buy diflucan in mexico
diflucan gel: buy diflucan online – diflucan 200 mg price
can i purchase generic clomid tablets: can you buy clomid now – order clomid tablets
generic clomid without prescription how to buy generic clomid without prescription how can i get generic clomid price
rexall pharmacy amoxicillin 500mg: amoxicillin without a doctors prescription – amoxicillin 825 mg
buy amoxicillin online mexico: amoxicillin medicine – amoxicillin 1000 mg capsule
how to get zithromax online: where can you buy zithromax – zithromax 600 mg tablets
purchase zithromax online zithromax 250 mg tablet price zithromax 500
https://stromectola.top/# minocycline 100mg over the counter
prednisone oral: prednisone otc uk – prednisone cream over the counter
amoxicillin without rx how to buy amoxicillin online cost of amoxicillin prescription
prednisone 100 mg: prednisone 20mg tablets where to buy – 20 mg prednisone
can you buy zithromax over the counter in australia: zithromax 250 mg tablet price – generic zithromax over the counter
https://clomida.pro/# can i buy cheap clomid without prescription
amoxicillin 750 mg price: amoxicillin without rx – where to buy amoxicillin pharmacy
prednisone 20mg price prednisone no rx online prednisone 5mg
https://clomida.pro/# buy generic clomid without prescription
where to buy prednisone in canada: buy prednisone 1 mg mexico – prednisone 50
https://prednisonea.store/# 20 mg prednisone
ivermectin australia: ivermectin topical – ivermectin 6mg tablet for lice
where can i buy clomid: where can i buy cheap clomid without a prescription – where can i get cheap clomid pill
https://azithromycina.pro/# zithromax for sale online
where can i buy zithromax in canada: zithromax 600 mg tablets – zithromax 1000 mg pills
ivermectin 9mg: stromectol price usa – ivermectin tablet 1mg
https://amoxicillina.top/# amoxicillin 500 mg without a prescription
how to get a prescription in canada canadian pharmacy without a prescription online no prescription pharmacy
https://onlinepharmacyworld.shop/# canadian pharmacy discount coupon
https://onlinepharmacyworld.shop/# cheapest pharmacy for prescriptions without insurance
mexico online pharmacy prescription drugs: canadian pharmacy online no prescription needed – canadian pharmacy online no prescription needed
no prescription required pharmacy: online pharmacy no prescription – prescription drugs online
http://onlinepharmacyworld.shop/# cheapest pharmacy prescription drugs
canadian pharmacy world coupon cheapest pharmacy for prescriptions online pharmacy no prescription
https://medicationnoprescription.pro/# best online pharmacy that does not require a prescription in india
http://medicationnoprescription.pro/# canadian prescription drugstore review
online pharmacy without a prescription: no prescription drugs online – indian pharmacy no prescription
cheap erection pills ed medications cost buying erectile dysfunction pills online
http://onlinepharmacyworld.shop/# legit non prescription pharmacies
http://medicationnoprescription.pro/# buy medication online with prescription
no prescription pharmacy online: no prescription canadian pharmacies – online meds without prescription
http://edpill.top/# erectile dysfunction medications online
mexican pharmacy no prescription buy drugs online without a prescription buy drugs online without a prescription
ed medication online: online ed medication – cost of ed meds
http://onlinepharmacyworld.shop/# canadian pharmacy world coupons
buy prescription online: mexican pharmacies no prescription – canada pharmacy without prescription
https://onlinepharmacyworld.shop/# rxpharmacycoupons
http://medicationnoprescription.pro/# no prescription medicines
buy erectile dysfunction pills online online erectile dysfunction prescription online ed medications
http://edpill.top/# ed treatments online
canada pharmacy no prescription: buying drugs without prescription – canada drugs without prescription
https://edpill.top/# ed medicine online
casino online uy tín: dánh bài tr?c tuy?n – choi casino tr?c tuy?n trên di?n tho?i
danh bai tr?c tuy?n casino tr?c tuy?n uy tin danh bai tr?c tuy?n
http://casinvietnam.shop/# casino online uy tin
https://casinvietnam.com/# casino tr?c tuy?n vi?t nam
http://casinvietnam.com/# casino tr?c tuy?n vi?t nam
choi casino tr?c tuy?n tren di?n tho?i danh bai tr?c tuy?n choi casino tr?c tuy?n tren di?n tho?i
https://casinvietnam.shop/# choi casino tr?c tuy?n tren di?n tho?i
casino tr?c tuy?n vi?t nam: game c? b?c online uy tín – casino tr?c tuy?n uy tín
http://casinvietnam.shop/# danh bai tr?c tuy?n
casino tr?c tuy?n uy tín: dánh bài tr?c tuy?n – casino online uy tín
https://casinvietnam.com/# casino tr?c tuy?n vi?t nam
dánh bài tr?c tuy?n: web c? b?c online uy tín – game c? b?c online uy tín
casino tr?c tuy?n: dánh bài tr?c tuy?n – choi casino tr?c tuy?n trên di?n tho?i
https://casinvietnam.shop/# casino online uy tin
casino tr?c tuy?n vi?t nam: casino tr?c tuy?n vi?t nam – casino tr?c tuy?n uy tín
https://casinvietnam.shop/# casino tr?c tuy?n vi?t nam
https://casinvietnam.com/# choi casino tr?c tuy?n tren di?n tho?i
casino tr?c tuy?n vi?t nam: choi casino tr?c tuy?n trên di?n tho?i – dánh bài tr?c tuy?n
casino tr?c tuy?n casino tr?c tuy?n uy tin casino tr?c tuy?n vi?t nam
http://casinvietnam.shop/# web c? b?c online uy tin
danh bai tr?c tuy?n casino tr?c tuy?n choi casino tr?c tuy?n tren di?n tho?i
web c? b?c online uy tín: choi casino tr?c tuy?n trên di?n tho?i – choi casino tr?c tuy?n trên di?n tho?i
http://casinvietnam.com/# choi casino tr?c tuy?n tren di?n tho?i
danh bai tr?c tuy?n web c? b?c online uy tin danh bai tr?c tuy?n
casino tr?c tuy?n vi?t nam: web c? b?c online uy tín – choi casino tr?c tuy?n trên di?n tho?i
casino online uy tin casino tr?c tuy?n uy tin choi casino tr?c tuy?n tren di?n tho?i
casino tr?c tuy?n: web c? b?c online uy tín – casino online uy tín
casino tr?c tuy?n uy tin danh bai tr?c tuy?n choi casino tr?c tuy?n tren di?n tho?i
http://casinvietnam.shop/# casino tr?c tuy?n vi?t nam
https://canadaph24.pro/# best online canadian pharmacy
reputable indian pharmacies online shopping pharmacy india indian pharmacy online
п»їbest mexican online pharmacies cheapest mexico drugs best online pharmacies in mexico
https://canadaph24.pro/# canadian pharmacy world
mexico pharmacy cheapest mexico drugs medicine in mexico pharmacies
http://canadaph24.pro/# pharmacy in canada
canadian king pharmacy Prescription Drugs from Canada best canadian pharmacy online
http://indiaph24.store/# indian pharmacy paypal
cheapest online pharmacy india Cheapest online pharmacy Online medicine order
http://canadaph24.pro/# vipps approved canadian online pharmacy
https://canadaph24.pro/# my canadian pharmacy reviews
world pharmacy india indian pharmacy buy medicines online in india
http://mexicoph24.life/# best online pharmacies in mexico
india pharmacy Cheapest online pharmacy indian pharmacy online
https://indiaph24.store/# pharmacy website india
mexican mail order pharmacies Online Pharmacies in Mexico mexico pharmacies prescription drugs
http://canadaph24.pro/# canadian online pharmacy
canada pharmacy reviews Certified Canadian Pharmacies canada online pharmacy
http://canadaph24.pro/# canadian pharmacy king reviews
purple pharmacy mexico price list Online Pharmacies in Mexico reputable mexican pharmacies online
buy drugs from canada Licensed Canadian Pharmacy canadian pharmacy review
http://mexicoph24.life/# mexico drug stores pharmacies
canadian neighbor pharmacy Licensed Canadian Pharmacy canadian drugs
https://mexicoph24.life/# mexican drugstore online
http://mexicoph24.life/# purple pharmacy mexico price list
reputable indian online pharmacy indian pharmacy fast delivery cheapest online pharmacy india
https://mexicoph24.life/# medication from mexico pharmacy
mexican drugstore online mexican pharmacy buying prescription drugs in mexico online
http://mexicoph24.life/# pharmacies in mexico that ship to usa
pharmacy website india indian pharmacy fast delivery online pharmacy india
http://indiaph24.store/# buy prescription drugs from india
reputable indian online pharmacy indian pharmacy online reputable indian online pharmacy
http://canadaph24.pro/# canada drug pharmacy
Online medicine order Generic Medicine India to USA india pharmacy
mexican drugstore online mexico pharmacy mexico pharmacy
mexico pharmacy cheapest mexico drugs purple pharmacy mexico price list
http://indiaph24.store/# top 10 pharmacies in india
mexican mail order pharmacies Online Pharmacies in Mexico buying prescription drugs in mexico
https://mexicoph24.life/# mexican border pharmacies shipping to usa
http://indiaph24.store/# reputable indian pharmacies
buy prescription drugs from india indian pharmacy top 10 online pharmacy in india
http://indiaph24.store/# legitimate online pharmacies india
buying prescription drugs in mexico buying prescription drugs in mexico mexican mail order pharmacies
http://canadaph24.pro/# canadian pharmacy ed medications
mexican border pharmacies shipping to usa Online Pharmacies in Mexico mexican rx online
http://mexicoph24.life/# medicine in mexico pharmacies
canadian pharmacy victoza canadian pharmacies canada drug pharmacy
aap zofran
http://indiaph24.store/# buy medicines online in india
indian pharmacy online indian pharmacy fast delivery indian pharmacy
http://mexicoph24.life/# pharmacies in mexico that ship to usa
canadian pharmacy price checker Licensed Canadian Pharmacy canadianpharmacymeds com
http://indiaph24.store/# buy medicines online in india
medicine in mexico pharmacies mexico pharmacy medication from mexico pharmacy
https://mexicoph24.life/# buying from online mexican pharmacy
indian pharmacies safe Cheapest online pharmacy best online pharmacy india
https://mexicoph24.life/# mexican pharmaceuticals online
https://mexicoph24.life/# buying prescription drugs in mexico online
п»їlegitimate online pharmacies india buy medicines from India top 10 online pharmacy in india
https://mexicoph24.life/# purple pharmacy mexico price list
mexican pharmaceuticals online Mexican Pharmacy Online mexican online pharmacies prescription drugs
https://canadaph24.pro/# legitimate canadian online pharmacies
mexico pharmacy Online Pharmacies in Mexico п»їbest mexican online pharmacies
http://mexicoph24.life/# buying prescription drugs in mexico online
cheapest online pharmacy india indian pharmacy indian pharmacy
https://mexicoph24.life/# mexican pharmaceuticals online
mexican pharmaceuticals online Online Pharmacies in Mexico reputable mexican pharmacies online
http://indiaph24.store/# cheapest online pharmacy india
best mail order pharmacy canada Prescription Drugs from Canada canadian pharmacy prices
https://mexicoph24.life/# mexico pharmacies prescription drugs
http://mexicoph24.life/# mexican pharmaceuticals online
medication from mexico pharmacy Online Pharmacies in Mexico pharmacies in mexico that ship to usa
http://canadaph24.pro/# canadian pharmacy meds
buying prescription drugs in mexico online cheapest mexico drugs mexico drug stores pharmacies
http://indiaph24.store/# indian pharmacy
mexican drugstore online Online Pharmacies in Mexico mexican rx online
https://indiaph24.store/# top 10 online pharmacy in india
buy prescription drugs from india Generic Medicine India to USA buy medicines online in india
https://mexicoph24.life/# mexico drug stores pharmacies
mexican online pharmacies prescription drugs Mexican Pharmacy Online mexico drug stores pharmacies
http://indiaph24.store/# buy prescription drugs from india
п»їlegitimate online pharmacies india indian pharmacy india online pharmacy
https://canadaph24.pro/# ed meds online canada
canadian pharmacy victoza Certified Canadian Pharmacies pharmacies in canada that ship to the us
http://canadaph24.pro/# www canadianonlinepharmacy
buying prescription drugs in mexico cheapest mexico drugs mexican drugstore online
indianpharmacy com https://indiaph24.store/# mail order pharmacy india
indian pharmacy
https://mexicoph24.life/# medication from mexico pharmacy
mexican mail order pharmacies: mexican pharmacy – mexican online pharmacies prescription drugs
best online pharmacies in mexico mexican pharmacy mexican pharmacy
http://cytotec.club/# buy cytotec in usa
cipro buy cipro cheap ciprofloxacin 500mg buy online
cytotec buy online usa: cytotec online – Misoprostol 200 mg buy online
http://ciprofloxacin.tech/# cipro for sale
buy zestoretic lisinopril 5mg buy lisinopril pharmacy online
buy prinivil: buy lisinopril online no prescription india – zestril 40
https://cytotec.club/# Misoprostol 200 mg buy online
buy cheap propecia prices cost propecia without rx buy cheap propecia without rx
http://finasteride.store/# cheap propecia without rx
lisinopril canada lisinopril 40 mg tablets prinivil 10 mg tab
purchase cytotec: buy cytotec – buy cytotec online
https://lisinopril.network/# lisinopril 4214
antibiotics cipro cipro ciprofloxacin cipro pharmacy
ciprofloxacin: antibiotics cipro – buy cipro online
https://finasteride.store/# cost of propecia for sale
order propecia without insurance buying cheap propecia price get cheap propecia without insurance
https://lisinopril.network/# can you buy lisinopril over the counter
https://ciprofloxacin.tech/# ciprofloxacin generic price
order generic propecia without prescription: cheap propecia pill – cost of propecia online
lisinopril 1 mg lisinopril 40 mg brand name in india lisinopril 240
https://lisinopril.network/# lisinopril pill
buy cytotec pills: buy cytotec in usa – buy cytotec pills
buy cytotec over the counter purchase cytotec buy cytotec online
http://finasteride.store/# cheap propecia without dr prescription
tamoxifen pill: nolvadex half life – nolvadex for pct
generic propecia pill cost cheap propecia cost propecia online
https://cytotec.club/# cytotec online
cipro ciprofloxacin ciprofloxacin mail online buy ciprofloxacin
https://nolvadex.life/# tamoxifen warning
order lisinopril: lisinopril 10 mg daily – price of lisinopril 30 mg
ciprofloxacin 500 mg tablet price cipro 500mg best prices ciprofloxacin over the counter
https://ciprofloxacin.tech/# buy generic ciprofloxacin
cost cheap propecia price: cost generic propecia no prescription – order generic propecia without prescription
http://cytotec.club/# buy cytotec over the counter
generic propecia prices propecia order buy propecia online
https://nolvadex.life/# nolvadex price
buy propecia pill: order generic propecia no prescription – cost of generic propecia
cipro pharmacy ciprofloxacin generic ciprofloxacin 500mg buy online
Generic Levitra 20mg Levitra generic price Levitra 20 mg for sale
https://kamagra.win/# buy Kamagra
cialis for sale: Generic Tadalafil 20mg price – Cialis 20mg price
https://viagras.online/# sildenafil online
Levitra 10 mg best price levitrav.store Vardenafil buy online
Cheap Viagra 100mg: Cheap Viagra 100mg – Buy Viagra online cheap
Buy Tadalafil 5mg: cialist.pro – Buy Tadalafil 5mg
https://viagras.online/# Viagra tablet online
http://cialist.pro/# Generic Cialis price
п»їcialis generic Generic Cialis without a doctor prescription Cialis 20mg price
Buy Vardenafil 20mg online: Levitra generic price – Levitra online USA fast
Viagra without a doctor prescription Canada Buy generic 100mg Viagra online order viagra
https://levitrav.store/# Levitra online USA fast
http://cialist.pro/# Buy Cialis online
Cialis without a doctor prescription: Generic Cialis without a doctor prescription – Generic Tadalafil 20mg price
Cheap Levitra online Vardenafil online prescription Buy Levitra 20mg online
Generic Cialis price: cialist.pro – Cheap Cialis
https://levitrav.store/# Vardenafil buy online
Kamagra 100mg price super kamagra Kamagra Oral Jelly
Kamagra tablets: kamagra – sildenafil oral jelly 100mg kamagra
https://levitrav.store/# Buy generic Levitra online
Cheap generic Viagra buy viagra here cheap viagra
non prescription canadian pharmacy: canada online prescription – no prescription pharmacy online
https://pharmcanada.shop/# best canadian pharmacy
online shopping pharmacy india indian pharmacy paypal mail order pharmacy india
online shopping pharmacy india: online pharmacy india – world pharmacy india
https://pharmindia.online/# top online pharmacy india
meds online no prescription no prescription canadian pharmacies medicine with no prescription
mexican online pharmacies prescription drugs: best online pharmacies in mexico – mexican pharmaceuticals online
Online medicine home delivery: top 10 pharmacies in india – online pharmacy india
https://pharmnoprescription.icu/# quality prescription drugs canada
legit non prescription pharmacies cheapest pharmacy no prescription required pharmacy
buy medications online no prescription: canada mail order prescription – mail order prescriptions from canada
http://pharmmexico.online/# buying prescription drugs in mexico
medication from mexico pharmacy п»їbest mexican online pharmacies п»їbest mexican online pharmacies
77 canadian pharmacy: canada rx pharmacy – canadian pharmacy 365
mexican border pharmacies shipping to usa: mexico pharmacies prescription drugs – purple pharmacy mexico price list
online canadian pharmacy: canadian drug – canadianpharmacy com
http://pharmcanada.shop/# best rated canadian pharmacy
buying drugs without prescription online pharmacy with prescription buy pills without prescription
http://pharmnoprescription.icu/# canada drugs no prescription
buying from online mexican pharmacy: mexico drug stores pharmacies – buying prescription drugs in mexico
https://pharmcanada.shop/# canadian pharmacy meds
international pharmacy no prescription pharm world store cheapest pharmacy for prescriptions without insurance
buy prednisone online uk: prednisone 10mg cost – 1 mg prednisone cost
doxycycline tablets doxycycline online order doxycycline online
https://doxycyclinea.online/# buy doxycycline hyclate 100mg without a rx
amoxicillin 500 coupon: amoxicillin 200 mg tablet – amoxicillin 875 mg tablet
prednisone brand name in usa: prednisone 50 mg for sale – canine prednisone 5mg no prescription
cost of amoxicillin 30 capsules amoxil pharmacy amoxicillin 200 mg tablet
online doxycycline: buy doxycycline online uk – where to purchase doxycycline
https://amoxila.pro/# can you buy amoxicillin over the counter in canada
cost of amoxicillin prescription: generic amoxicillin online – medicine amoxicillin 500mg
where to get doxycycline: doxy 200 – buy doxycycline hyclate 100mg without a rx
SightCare formula aims to maintain 20/20 vision without the need for any surgical process. This supplement is a perfect solution for people facing issues as they grow older. https://sightcare-web.com/
purchase doxycycline online: buy doxycycline online – doxy
zithromax pill: order zithromax over the counter – where can i buy zithromax in canada
medicine neurontin capsules neurontin mexico order neurontin
http://doxycyclinea.online/# buy doxycycline without prescription uk
prednisone 40 mg rx: how much is prednisone 5mg – prednisone 10mg for sale
prednisone 50 mg tablet canada: buy prednisone 1 mg mexico – prednisone 300mg
average cost of generic zithromax purchase zithromax z-pak buy zithromax
http://doxycyclinea.online/# doxycycline monohydrate
neurontin capsules: buy neurontin online no prescription – neurontin 600 mg tablet
doxycycline 100mg tablets doxycycline 500mg buy doxycycline online
PCWer is here to help you with all questions in tech. Whether that
Find the latest technology news and expert tech product reviews. Learn about the latest gadgets and consumer tech products for entertainment, gaming, lifestyle and more. https://axget.com/
Easier WWW is a leading technology site that is dedicated to produce great how-to, tips and tricks and cool software review. https://easierwww.com/
Testosil is a natural polyherbal testosterone booster designed to help men increase their testosterone levels safely and effectively. https://testosil-web.com/
prednisone 60 mg price: prednisone tablets canada – prednisone for cheap
online viagra levitra
http://prednisoned.online/# prednisone 60 mg
prednisone 2.5 mg daily: 54 prednisone – how can i get prednisone
Nagano Lean Body Tonic is a groundbreaking powdered supplement crafted to support your weight loss journey effortlessly. https://naganotonic-try.com/
– Shoot MASSIVE Loads For An Amazing Finish! https://semenax-try.com/
ZenCortex Research’s contains only the natural ingredients that are effective in supporting incredible hearing naturally.A unique team of health and industry professionals dedicated to unlocking the secrets of happier living through a healthier body. https://zencortex-try.com/
Serolean, a revolutionary weight loss supplement, zeroes in on serotonin—the key neurotransmitter governing mood, appetite, and fat storage. https://serolean-web.com/
Tonic Greens is a ready-made greens shake designed to support the entire body and wellness of the mind. It is filled with over 50 individual vitamins https://tonicgreens-try.com/
MenoPhix is a menopause relief supplement featuring a blend of plant extracts to target the root cause of menopause symptoms. https://menophix-web.com/
BalMorex Pro is an exceptional solution for individuals who suffer from chronic joint pain and muscle aches. With its 27-in-1 formula comprised entirely of potent and natural ingredients, it provides unparalleled support for the health of your joints, back, and muscles. https://balmorex-try.com/
Support the health of your ears with 100% natural ingredients, finally being able to enjoy your favorite songs and movies https://quietumplus-try.com/
Peak BioBoost is a revolutionary dietary supplement that leverages the power of nature to support and improve your digestive system. https://peakbioboost-web.com/
GutOptim is a digestive health supplement designed to support your gut and stomach. It restore balance in gut flora and reduce the symptoms of digestive disorders. https://gutoptim-try.com/
amoxicillin 800 mg price where to buy amoxicillin 500mg without prescription amoxicillin cost australia
Burn Boost Powder™ is a proven weight loss powder drink that helps to lose weight and boosts the overall metabolism in the body. https://burnboost-web.com
NanoDefense Pro utilizes a potent blend of meticulously chosen components aimed at enhancing the wellness of both your nails and skin. https://nanodefense-web.com/
amoxicillin 500mg no prescription: amoxicillin azithromycin – buy amoxicillin online cheap
http://prednisoned.online/# prednisone 20mg prices
doxycycline mono: buy doxycycline without prescription uk – where to get doxycycline
prednisone capsules prednisone capsules prednisone 1 tablet
FlowForce Max is an innovative, natural and effective way to address your prostate problems, while addressing your energy, libido, and vitality. https://flowforcemax-web.com/
CLINICALLY PROVEN* To Increase Semen Volume And Intensity https://semenax-try.com/
TestRX™ is a bodybuilding supplement. It’s formulated with high-quality natural ingredients proven to boost natural testosterone and stimulate muscle growth. https://testrx-web.com/
DuoTrim is an innovative weight loss supplement that utilizes the power of natural plants and nutrients to create CSM bacteria https://duotrim-us.com/
BioFit is a Nutritional Supplement That Uses Probiotics To Help You Lose Weight https://biofit-web.com/
doxycycline monohydrate: where to purchase doxycycline – doxycycline 100mg price
https://doxycyclinea.online/# buy doxycycline
Sugar Balance is an ultra-potent blood sugar supplement that you can use to help control glucose levels, melt away fat and improve your overall health. https://sugarbalance-us.com/
GlucoFlush is an advanced formula specially designed for pancreas support that will let you promote healthy weight by effectively maintaining the blood sugar level and cleansing and strengthening your gut. https://glucoflush-us.com/
Alpha Tonic is a powder-based supplement that uses multiple natural herbs and essential vitamins and minerals to help optimize your body’s natural testosterone levels. https://alphatonic-web.com
Vivo Tonic is a remarkable blood sugar support nutritional supplement that offers a wide range of benefits. https://vivotonic-web.com/
buy amoxicillin 500mg online amoxicillin 500mg capsules uk amoxicillin online purchase
purchase doxycycline online: buy doxycycline – generic doxycycline
Nervogen Pro is an effective dietary supplement designed to help patients with neuropathic pain. When you combine exotic herbs, spices, and other organic substances, your immune system will be strengthened. https://nervogenpro-web.com/
VivoTonic™ is a 11-in-1 vital blood sugar support formula that may improve how the metabolism goes after the calories that consumers eat. https://vivotonic-web.com/
Progenifix is designed to help maximize weight loss results using a mixture of natural, science-backed ingredients. The formula also has secondary benefits, including promoting overall wellness and vitality and assisting your immune system. https://progenifix-web.com/
AquaPeace is an all-natural nutritional formula that uses a proprietary and potent blend of ingredients and nutrients to improve overall ear and hearing health and alleviate the symptoms of tinnitus. https://aquapeace-web.com
FoliPrime is a simple serum containing a blend of vitamins designed to boost hair health. FoliPrime has 100 percent natural substances that enhance and supplement the vitamins in the scalp to promote hair growth. https://foliprime-web.com/
zithromax 250 mg: can i buy zithromax online – can you buy zithromax over the counter in australia
Gut Vita™ is a daily supplement that helps consumers to improve the balance in their gut microbiome, which supports the health of their immune system. It supports healthy digestion, even for consumers who have maintained an unhealthy diet for a long time. https://gutvita-us.com/
http://zithromaxa.store/# zithromax without prescription
Neuro-Thrive is a brain health supplement that claims to promote good memory and thinking skills and better quality sleep. This nootropic supplement achieves its cause with its potent blend of natural compounds and extracts that are proven to be effective in sharpening mental acuity. https://neurothrive-web.com/
Fast Lean Pro is a herbal supplement that tricks your brain into imagining that you’re fasting and helps you maintain a healthy weight no matter when or what you eat. It offers a novel approach to reducing fat accumulation and promoting long-term weight management. https://fastleanpro-web.com/
Erectin is a clinically-proven dietary supplement designed to enhance male https://erectin-web.com/
amoxicillin 800 mg price buy amoxicillin 250mg amoxicillin without a doctors prescription
100% Natural Formula Expressly Designed to Help Control Blood Sugar Levels, Improve Insulin Response And Support Overall Health https://glucotrusttry.com/
PowerBite stands as an innovative dental candy, dedicated to nurturing healthy teeth and gums. Infused with a potent formula, it champions the cause of a robust and radiant smile. Crafted meticulously https://powerbite-web.com/
Protoflow is a prostate health supplement featuring a blend of plant extracts, vitamins, minerals, fruit extracts, and more. https://protoflow-web.com/
Boostaro is a dietary supplement designed specifically for men who suffer from health issues. https://boostaro-try.com/
Unlock the incredible potential of Puravive! Supercharge your metabolism and incinerate calories like never before with our unique fusion of 8 exotic components. Bid farewell to those stubborn pounds and welcome a reinvigorated metabolism and boundless vitality. Grab your bottle today and seize this golden opportunity! https://puravive-web.com/
Zoracel is an extraordinary oral care product designed to promote healthy teeth and gums, provide long-lasting fresh breath, support immune health, and care for the ear, nose, and throat. https://zoracel-web.com
Cerebrozen is an excellent liquid ear health supplement purported to relieve tinnitus and improve mental sharpness, among other benefits. The Cerebrozen supplement is made from a combination of natural ingredients, and customers say they have seen results in their hearing, focus, and memory after taking one or two droppers of the liquid solution daily for a week. https://cerebrozen-try.com/
doxycycline hyclate 100 mg cap: doxycycline hyclate – doxycycline pills
buy generic neurontin online: neurontin 1200 mg – drug neurontin
http://amoxila.pro/# purchase amoxicillin online without prescription
doxy how to buy doxycycline online buy cheap doxycycline online
The human body can continue to live thanks to the correct functioning of certain systems. If even one of these systems does not work properly, it can cause problems in human life. https://calmlean-web.com/
amoxicillin 30 capsules price: medicine amoxicillin 500mg – purchase amoxicillin online without prescription
Zeneara is marketed as an expert-formulated health supplement that can improve hearing and alleviate tinnitus, among other hearing issues. https://zeneara-web.com/
http://doxycyclinea.online/# doxycycline 100mg price
GlucoBerry is one of the biggest all-natural dietary and biggest scientific breakthrough formulas ever in the health industry today. This is all because of its amazing high-quality cutting-edge formula that helps treat high blood sugar levels very naturally and effectively. https://glucoberry-web.com/
Introducing TerraCalm, a soothing mask designed specifically for your toenails. Unlike serums and lotions that can be sticky and challenging to include in your daily routine, TerraCalm can be easily washed off after just a minute. https://terracalm-web.com/
neurontin rx: neurontin 200 mg – buy generic neurontin
VidaCalm is an all-natural blend of herbs and plant extracts that treat tinnitus and help you live a peaceful life. https://vidacalm-web.com/
Are you tired of looking in the mirror and noticing saggy skin? Is saggy skin making you feel like you are trapped in a losing battle against aging? Do you still long for the days when your complexion radiated youth and confidence? https://refirmance-web.com/
Gorilla Flow prostate is an all-natural dietary supplement for men which aims to decrease inflammation in the prostate to decrease common urinary tract issues such as frequent and night-time urination, leakage, or blocked urine stream. https://gorillaflow-web.com
zithromax generic cost zithromax prescription in canada zithromax over the counter canada
amoxicillin tablets in india: amoxicillin 500 mg – buying amoxicillin online
Volca Burn is a weight loss supplement that uses a “red tingle hack” to help you rapidly lose weight without dieting or exercising. https://volcaburn-web.com/
Xitox’s foot pads contain a combination of powerful herbs that help provide a soothing experience for your feet after a long day. https://xitox-web.com/
http://prednisoned.online/# buy prednisone 20mg
Hydrossential is actually a skincare serum or you can say a skincare supplement created by Emma Smith to help women keep their skin looking beautiful and flawless. https://hydrossential-web.com/
Carbofix is the revolutionary dietary formula that promises to activate weight loss without all the extra hard work. https://carbofix-try.com
Reliver Pro is a dietary supplement formulated with a blend of natural ingredients aimed at supporting liver health
buy amoxicillin 250mg amoxicillin order online buy amoxicillin online mexico
where to get doxycycline: buy doxycycline online uk – doxycycline mono
buy cheap amoxicillin: amoxicillin 500mg pill – over the counter amoxicillin canada
http://gabapentinneurontin.pro/# gabapentin 100mg
zithromax 500 mg zithromax online usa buy zithromax without presc
vibramycin 100 mg: buy cheap doxycycline – buy doxycycline monohydrate
generic zithromax india: zithromax online pharmacy canada – zithromax pill
http://prednisoned.online/# prednisone cream over the counter
neurontin 300 mg buy neurontin online pharmacy neurontin brand name in india
PotentStream is designed to address prostate health by targeting the toxic, hard water minerals that can create a dangerous buildup inside your urinary system It’s the only dropper that contains nine powerful natural ingredients that work in perfect synergy to keep your prostate healthy and mineral-free well into old age. https://potentstream-web.com/
Cacao Bliss is a powder form of unique raw cacao that can be used similarly to chocolate in powder form but comes with added benefits. It is designed to provide a rich and satisfying experience while delivering numerous health benefits. https://cacaobliss-web.com/
neurontin prices: buy gabapentin online – neurontin price uk
prednisone in india: can i order prednisone – prednisone 20mg by mail order
https://zithromaxa.store/# zithromax for sale 500 mg
price of doxycycline doxycycline monohydrate doxycycline online
9 da auto news – https://9-da.com/
scshlj banking finance news – https://scshlj.com
prednisone 4mg: prednisone 10 mg brand name – prednisone 5 mg
no prescription online prednisone: 10 mg prednisone tablets – prednisone online for sale
http://zithromaxa.store/# buy cheap zithromax online
doxycycline pills doxycycline 200 mg doxycycline prices
Lasixiv provides news and analysis for IT executives. We cover big data, IT strategy, cloud computing, security, mobile technology, infrastructure, software and more. https://lasixiv.com
https://mexicanpharmacy1st.online/# mexico pharmacy
mexican rx online buying from online mexican pharmacy medicine in mexico pharmacies
Wedstraunt has the latest news in the restaurant industry, covering topics like consumer trends, technology, marketing and branding, operations, mergers https://wedstraunt.com
mexico pharmacy: mexico pharmacies prescription drugs – mexican border pharmacies shipping to usa
http://mexicanpharmacy1st.com/# buying from online mexican pharmacy
Cneche provides in-depth journalism and insight into the most impactful news and trends shaping the finance industry. https://cneche.com/
medicine in mexico pharmacies: mexican drugstore online – buying prescription drugs in mexico
Huzad delivers the latest news in the grocery industry, with articles covering grocery delivery, online food shopping, shopper behavior, store formats, technology, and more. https://huzad.com/
mexican border pharmacies shipping to usa mexican rx online mexican border pharmacies shipping to usa
Susibu provides in-depth journalism and insight into the news and trends impacting the hotel https://susibu.com/
mexico pharmacy: best mexican online pharmacies – mexico pharmacies prescription drugs
https://mexicanpharmacy1st.com/# mexican mail order pharmacies
Christside provides news and analysis for retail executives. We cover topics like retail tech, marketing, e-commerce, logistics, in-store operations, corporate retail news, and more. https://christside.com/
https://mexicanpharmacy1st.online/# mexican rx online
Mscherrybomb provides in-depth journalism and insight into the most impactful news and trends shaping the trucking industry. https://mscherrybomb.com/
mexican pharmacy buying from online mexican pharmacy mexican border pharmacies shipping to usa
mexican rx online: best online pharmacies in mexico – mexico drug stores pharmacies
https://mexicanpharmacy1st.online/# mexican rx online
Janmckinley provides news and analysis for waste and recycling executives. We cover topics like landfills, collections, regulation, waste-to-energy, corporate news, fleet management, and more. https://janmckinley.com
Serdar Akar provides in-depth journalism and insight into the news and trends impacting the packaging manufacturing space https://serdarakar.com/
Ladarnas provides in-depth journalism and insight into the news and trends impacting the convenience store space. https://ladarnas.com
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://omiyabigan.com/
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://mimsbrook.com
buying prescription drugs in mexico mexican pharmacy buying from online mexican pharmacy
mexico drug stores pharmacies: mexico pharmacy – best mexican online pharmacies
https://mexicanpharmacy1st.online/# buying from online mexican pharmacy
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://smithsis.com
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://bxbinc.com/
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://hostalmindanao.com
mexican online pharmacies prescription drugs mexican drugstore online best online pharmacies in mexico
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://manciniproductions.com/
buying prescription drugs in mexico online: medication from mexico pharmacy – mexico pharmacies prescription drugs
Sugar Defender is a revolutionary blood sugar support formula designed to support healthy glucose levels and promote natural weight loss. https://blackboxvending.com/
http://mexicanpharmacy1st.com/# purple pharmacy mexico price list
mexican border pharmacies shipping to usa: mexican rx online – purple pharmacy mexico price list
https://mexicanpharmacy1st.com/# medicine in mexico pharmacies
Sugar Defender is a revolutionary blood sugar support formula designed to support healthy glucose levels and promote natural weight loss. https://mineryuta.com
mexican pharmaceuticals online: best online pharmacies in mexico – mexico drug stores pharmacies
mexico pharmacy buying prescription drugs in mexico purple pharmacy mexico price list
pharmacies in mexico that ship to usa: mexico drug stores pharmacies – mexico drug stores pharmacies
https://mexicanpharmacy1st.shop/# mexico drug stores pharmacies
Sugar Defender is the rated blood sugar formula with an advanced blend of 24 proven ingredients that support healthy glucose levels and natural weight loss. https://ibcbellows.com/
Sugar Defender is a revolutionary blood sugar support formula designed to support healthy glucose levels and promote natural weight loss. https://acmesignz.com/
Manufactured in the United States with FDA approval, this product was crafted using only the highest quality ingredients and produced under hygienic conditions in a GMP-certified facility. https://mystylefiles.com/
mexico drug stores pharmacies: buying prescription drugs in mexico – mexican border pharmacies shipping to usa
sugar defender: https://orchidsites.com/
mexico drug stores pharmacies best online pharmacies in mexico buying prescription drugs in mexico
https://mexicanpharmacy1st.shop/# mexican mail order pharmacies
sugar defender: https://novabeaute.com/
sugar defender: https://abmdds.com/
buying prescription drugs in mexico online: mexico drug stores pharmacies – buying from online mexican pharmacy
https://mexicanpharmacy1st.shop/# reputable mexican pharmacies online
best online pharmacies in mexico mexican border pharmacies shipping to usa best online pharmacies in mexico
http://mexicanpharmacy1st.com/# mexican drugstore online
sugar defender: https://peyfon.com/
sugar defender: https://nilayoram.com/
sugar defender: https://seahorsesoap.com/
sugar defender: https://kandicandles.com/
sugar defender: https://sourceprousa.com/
cost cheap clomid without dr prescription cheap clomid without rx where can i buy cheap clomid pill
https://gabapentin.club/# neurontin 800
neurontin 400 mg price: neurontin 150 mg – neurontin 30 mg
lisinopril 25 mg tablet: lisinopril 80 – lisinopril 20 mg discount
neurontin drug where to buy neurontin neurontin 300 mg pill
buy propecia pills: cost of propecia without dr prescription – cost propecia tablets
sugar defender: https://royalforestlaundry.com/
sugar defender: https://flamebustersofkansas.com/
sugar defender: https://lindadicesare.com/
http://propeciaf.online/# buy propecia tablets
sugar defender: https://drdenisemichele.com/
sugar defender: https://alchemyfashiongroup.com/
cost cheap clomid online can i purchase clomid clomid without dr prescription
lisinopril brand name canada: lisinopril 3.5 mg – buy lisinopril mexico
https://cytotec.xyz/# purchase cytotec
lisinopril 2018 zestril 5 mg prices lisinopril drug
lipinpril: lisinopril 5 mg buy – lisinopril 102
http://propeciaf.online/# cost generic propecia prices
where buy cheap clomid pill can you buy clomid without insurance can i order generic clomid without rx
buy generic propecia without insurance: get cheap propecia tablets – propecia sale
http://propeciaf.online/# propecia tablets
neurontin 600 mg cost: neurontin 800 mg tablets – neurontin 800 mg
https://cytotec.xyz/# Abortion pills online
cost generic propecia no prescription cost cheap propecia without a prescription buying propecia
lisinopril 20mg 37.5mg: zestril canada – generic drug for lisinopril
https://propeciaf.online/# get generic propecia without a prescription
lisinopril online without a prescription lisinopril 40 mg for sale buy lisinopril 20 mg without a prescription
neurontin 1200 mg: neurontin 500 mg – neurontin 200 mg capsules
http://gabapentin.club/# neurontin
lisinopril 10 mg canada prescription drug lisinopril lisinopril 5 mg buy online
lisinopril 40 mg price: lisinopril 40 mg cost – lisinopril 5 mg for sale
cost of generic clomid pills: clomid sale – can you buy clomid without dr prescription
lisinopril mexico how much is lisinopril 10 mg lisinopril 20mg coupon
https://cheapestindia.shop/# reputable indian online pharmacy
http://cheapestcanada.com/# legal to buy prescription drugs from canada
canadian mail order pharmacy: cheapestcanada.com – canadian pharmacy king
https://36and6health.com/# cheapest prescription pharmacy
mexico drug stores pharmacies medicine in mexico pharmacies buying prescription drugs in mexico online
http://cheapestmexico.com/# mexico drug stores pharmacies
https://36and6health.com/# canada pharmacy not requiring prescription
https://cheapestcanada.com/# is canadian pharmacy legit
cheapest online pharmacy india india pharmacy pharmacy website india
medication from mexico pharmacy: mexican mail order pharmacies – buying prescription drugs in mexico online
http://cheapestcanada.com/# global pharmacy canada
https://cheapestandfast.com/# buy pain meds online without prescription
https://cheapestindia.com/# indian pharmacies safe
http://cheapestmexico.com/# best online pharmacies in mexico
https://36and6health.com/# canada online pharmacy no prescription
best india pharmacy: indian pharmacy online – indian pharmacy online
https://cheapestmexico.com/# best online pharmacies in mexico
farmacia online barcelona: farmacia online madrid – п»їfarmacia online espaГ±a
farmacie online autorizzate elenco: Farmacie online sicure – Farmacia online miglior prezzo
beste online-apotheke ohne rezept online apotheke deutschland online apotheke deutschland
https://eumedicamentenligne.shop/# pharmacie en ligne fiable
pharmacie en ligne avec ordonnance: Pharmacie Internationale en ligne – pharmacie en ligne
pharmacie en ligne france fiable: pharmacie en ligne avec ordonnance – pharmacie en ligne france fiable
pharmacie en ligne pas cher: pharmacie en ligne france livraison belgique Рvente de m̩dicament en ligne
farmacia online envГo gratis farmacias online seguras en espaГ±a farmacias online seguras
farmacias direct: farmacia online madrid – п»їfarmacia online espaГ±a
pharmacie en ligne france livraison internationale: Pharmacie Internationale en ligne – pharmacie en ligne fiable
online apotheke rezept: eu apotheke ohne rezept – shop apotheke gutschein
beste online-apotheke ohne rezept beste online-apotheke ohne rezept medikament ohne rezept notfall
http://eumedicamentenligne.com/# pharmacie en ligne france pas cher
acheter mГ©dicament en ligne sans ordonnance: pharmacie en ligne france livraison belgique – pharmacie en ligne france fiable
pharmacie en ligne avec ordonnance: pharmacies en ligne certifi̩es Рpharmacie en ligne pas cher
farmacie online affidabili farmacie online sicure farmacie online affidabili
apotheke online: online apotheke deutschland – п»їshop apotheke gutschein
Farmacie online sicure: farmaci senza ricetta elenco – farmacia online
farmacia en casa online descuento: farmacia en casa online descuento – farmacias online seguras
pharmacie en ligne france pas cher Achat mГ©dicament en ligne fiable acheter mГ©dicament en ligne sans ordonnance
pharmacie en ligne france livraison internationale: pharmacie en ligne sans ordonnance – pharmacie en ligne
farmacia online più conveniente: Farmacia online miglior prezzo – acquistare farmaci senza ricetta
beste online-apotheke ohne rezept apotheke online eu apotheke ohne rezept
https://eufarmaciaonline.shop/# farmacias online seguras en espaГ±a
beste online-apotheke ohne rezept: online apotheke – online apotheke deutschland
acquistare farmaci senza ricetta: farmacie online autorizzate elenco – Farmacia online piГ№ conveniente
Achat mГ©dicament en ligne fiable: trouver un mГ©dicament en pharmacie – trouver un mГ©dicament en pharmacie
п»їFarmacia online migliore Farmacie on line spedizione gratuita farmacie online sicure
shop apotheke gutschein: günstigste online apotheke – europa apotheke
online apotheke preisvergleich: europa apotheke – medikamente rezeptfrei
pharmacies en ligne certifi̩es: pharmacie en ligne france livraison belgique Рpharmacie en ligne
farmacia online espaГ±a envГo internacional: farmacias online seguras en espaГ±a – farmacias online baratas
https://eumedicamentenligne.shop/# Pharmacie Internationale en ligne
Farmacie on line spedizione gratuita: farmaci senza ricetta elenco – farmacia online piГ№ conveniente
farmacia barata farmacia en casa online descuento farmacia online espaГ±a envГo internacional
Farmacia online miglior prezzo: farmaci senza ricetta elenco – farmacie online autorizzate elenco
farmacia online: migliori farmacie online 2024 – farmacia online piГ№ conveniente
Pharmacie sans ordonnance: pharmacie en ligne fiable – pharmacie en ligne france fiable
Viagra sans ordonnance livraison 24h: Viagra prix pharmacie paris – Viagra en france livraison rapide
geinoutime.com
Zhu Houzhao는 흠뻑 젖어 땀을 많이 흘렸습니다.
Achat mГ©dicament en ligne fiable pharmacie en ligne sans ordonnance pharmacie en ligne france livraison belgique
п»їpharmacie en ligne france: cialis generique – acheter mГ©dicament en ligne sans ordonnance
trouver un mГ©dicament en pharmacie: pharmacie en ligne pas cher – Achat mГ©dicament en ligne fiable
https://phenligne.com/# pharmacie en ligne avec ordonnance
pharmacie en ligne avec ordonnance: Pharmacies en ligne certifiees – trouver un mГ©dicament en pharmacie
pharmacie en ligne france pas cher: pharmacie en ligne pas cher – п»їpharmacie en ligne france
Hello.
This post was created with XRumer 23 StrongAI.
Good luck 🙂
pharmacie en ligne sans ordonnance: Pharmacies en ligne certifiees – Achat mГ©dicament en ligne fiable
acheter mГ©dicament en ligne sans ordonnance: Pharmacie sans ordonnance – п»їpharmacie en ligne france
Viagra pas cher paris: viagra en ligne – Viagra sans ordonnance 24h suisse
Hello!
This post was created with XRumer 23 StrongAI.
Good luck 🙂
pharmacie en ligne sans ordonnance: pharmacie en ligne sans ordonnance – pharmacie en ligne pas cher
trouver un mГ©dicament en pharmacie: Levitra acheter – acheter mГ©dicament en ligne sans ordonnance
pharmacie en ligne france fiable: Levitra 20mg prix en pharmacie – pharmacie en ligne france pas cher
pharmacie en ligne fiable: kamagra pas cher – pharmacie en ligne france livraison internationale
geinoutime.com
Chenla는 좋은 예이자 나쁜 예입니다.
Achat mГ©dicament en ligne fiable: Levitra pharmacie en ligne – acheter mГ©dicament en ligne sans ordonnance
vente de mГ©dicament en ligne: Levitra 20mg prix en pharmacie – Achat mГ©dicament en ligne fiable
http://phenligne.com/# Achat médicament en ligne fiable
pharmacie en ligne fiable: levitra en ligne – pharmacie en ligne
pharmacies en ligne certifiГ©es: Acheter Cialis – pharmacie en ligne france pas cher
pharmacie en ligne livraison europe: levitra generique sites surs – pharmacie en ligne france pas cher
pharmacie en ligne livraison europe: Acheter Cialis – Achat mГ©dicament en ligne fiable
pharmacies en ligne certifiГ©es: Cialis sans ordonnance 24h – pharmacie en ligne avec ordonnance
п»їpharmacie en ligne france: acheter kamagra site fiable – pharmacie en ligne france pas cher
vente de mГ©dicament en ligne: pharmacie en ligne sans ordonnance – pharmacie en ligne france livraison belgique
pharmacie en ligne france fiable: Levitra 20mg prix en pharmacie – Pharmacie sans ordonnance
pharmacie en ligne avec ordonnance: pharmacies en ligne certifiГ©es – pharmacie en ligne sans ordonnance
pharmacie en ligne france livraison belgique: pharmacie en ligne sans ordonnance – trouver un mГ©dicament en pharmacie
Pharmacie sans ordonnance: Medicaments en ligne livres en 24h – vente de mГ©dicament en ligne
pharmacie en ligne sans ordonnance: Acheter Cialis – vente de mГ©dicament en ligne
SildГ©nafil Teva 100 mg acheter: Viagra sans ordonnance 24h suisse – Viagra homme prix en pharmacie sans ordonnance
pharmacie en ligne sans ordonnance: achat kamagra – pharmacies en ligne certifiГ©es
Pharmacie en ligne livraison Europe: pharmacie en ligne sans ordonnance – pharmacie en ligne
acheter mГ©dicament en ligne sans ordonnance: pharmacie en ligne pas cher – п»їpharmacie en ligne france
п»їpharmacie en ligne france: levitra generique – pharmacie en ligne france pas cher
vente de mГ©dicament en ligne: levitra en ligne – pharmacies en ligne certifiГ©es
acheter mГ©dicament en ligne sans ordonnance: levitra generique prix en pharmacie – pharmacie en ligne pas cher
Viagra pas cher inde: viagra sans ordonnance – Viagra pas cher livraison rapide france
Le gГ©nГ©rique de Viagra: viagra sans ordonnance – Viagra prix pharmacie paris
Pharmacie sans ordonnance: Acheter Cialis – pharmacies en ligne certifiГ©es
pharmacie en ligne pas cher: cialis sans ordonnance – Pharmacie Internationale en ligne
pharmacie en ligne france livraison belgique: Medicaments en ligne livres en 24h – pharmacies en ligne certifiГ©es
Pharmacie Internationale en ligne: Levitra acheter – pharmacie en ligne france pas cher
pharmacie en ligne pas cher: Acheter Cialis – pharmacies en ligne certifiГ©es
pharmacies en ligne certifiГ©es: levitra en ligne – pharmacie en ligne
vente de mГ©dicament en ligne: cialis prix – п»їpharmacie en ligne france
pharmacie en ligne france fiable: cialis generique – trouver un mГ©dicament en pharmacie
pharmacies en ligne certifiГ©es: Achat mГ©dicament en ligne fiable – vente de mГ©dicament en ligne
pharmacie en ligne fiable: pharmacie en ligne sans ordonnance – pharmacie en ligne sans ordonnance
trouver un mГ©dicament en pharmacie: Levitra sans ordonnance 24h – trouver un mГ©dicament en pharmacie
pharmacie en ligne pas cher: Acheter Cialis – acheter mГ©dicament en ligne sans ordonnance
geinoutime.com
“하지만 삼촌은 당신이 납득이 가지 않는다는 것을 알고 있습니다…” Fang Jifan이 천천히 말했습니다.
geinoutime.com
Zhu Houzhao는 아버지의 말이 풍자인지 칭찬인지 알지 못했기 때문에 당황했습니다.
프라그마틱 슬롯
Hongzhi 황제는 Liu Jian을보고 “Liu Qing은 어떻게 생각합니까? “라고 말했습니다.
pin-up kazino: Pin Up Azerbaycan ?Onlayn Kazino – Pin-Up Casino
pin-up 141 casino: pin-up360 – Pin-Up Casino
https://autolux-azerbaijan.com/# ?Onlayn Kazino
Pin Up Azerbaycan ?Onlayn Kazino: Pin-up Giris – Pin-up Giris
https://autolux-azerbaijan.com/# Pin Up Azerbaycan
Pin-up Giris: pin-up 141 casino – Pin up 306 casino
https://autolux-azerbaijan.com/# Pin-Up Casino
발라테일 바이킹즈
아버지는 왜 라오팡의 무력함에 공감하기보다 라오팡의 연기력을 믿는 걸까?
탑 슬롯
Fang Jifan이 어제 그런 말을했다면 모두가 그를 비웃을 것입니다.