CASE REPORT
Year: 2019 I Volume: 2 I Issue: 3 I Page: 92-93
Annular elastolytic granuloma: a rare case report in an indian farmer (O’Brien’s granuloma)
Shivani Saini1 , Devendra Yadav1
1 Department of Dermatology, GMC, Kota
Corresponding Author:
Devendra Yadav
Senior Professor, Department of Dermatology, GMC, Kota
Email: devendrayadav73@gmail.com
How to cite this article:
Saini S, Yadav D. Annular elastolytic granuloma: a rare case report in an indian farmer (O’Brien’s granuloma). JDA Indian Journal of Clinical Dermatology. 2019;2:92-93.
Abstract:
Annular elastolytic granuloma is a type of actinic granuloma of unknown etiopathogenesis, first described by O’Brien in 1975. It presents with asymptomatic annular erythematous plaques on sun-exposed body parts. On histopathology examination, it shows elastin degeneration, multinucleate giant cells and interstitial granuloma with areas of elasto-phagocytosis. We report a case of a 72 year old male with an asymptomatic ring like erythematous plaque with raised borders involving parts of the left arm and forearm, which was confirmed to be annular elastolytic granuloma on histopathology. It is relatively rare in the Indian population and must be differentiated from other similar lesions of granuloma annulare, sarcoidosis, necrobiosis lipoidica, elastosis perforans serpiginosa and morphological variant of mycosis fungoides.
Key words: Annular Elastolytic Granuloma, palisaded and interstitial granuloma, elasto-phagocytosis
Introduction:
Actinic granuloma, also known as O’Brien’s granuloma is a rare and self-healing granulomatous disorder seen in middle aged persons with chronic sun-exposure. It presents as asymptomatic erythematous plaque of any size with central atrophy and hypopigmentation with raised borders and centrifugal expansion. We are reporting this case from rajasthan, desert region of india. Inspite of rajasthan receiving high solar radiation there is still no case report from here.
Case Report:
A 72 year old married male, farmer by occupation, presented to our skin OPD with a history of insidious onset of asymptomatic ring shaped lesion over extensor aspect of left upper limb extending from middle of arm to lower third of forearm. At the onset, there were 0.5 cm size erythematous raised lesions, which progressed slowly over 2 years to form large plaque of present size[Figure 1]. On local cutaneous examination, it was an erythematous annular plaque of size 17×8 cm, overlying extensor aspect of left upper limb with central atrophy and raised serpiginous borders of reddish brown color, extending from middle arm to lower forearm. Lesions were non-oozy, nontender, but greyish white scaling was present in some areas. Skin
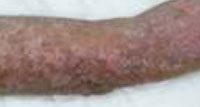 |
Figure 1: well defined erythematous plaque present over extensor aspect extending from mid of left upper arm to full length of forearm. |
appendages within the lesion were normal. Examination of hair, nails and mucosa did not reveal any significant abnormality. General physical examination and systemic examination of the patient were normal.
All routine laboratory investigations including complete blood count, ESR, urine analysis biochemical profile, angiotensin converting enzyme, liver functions tests, and renal function tests were within normal limits. Antinuclear antibody was negative. Chest X-ray revealed some areas of interstitial opacity but pulmonary function tests were normal. Mantoux tests and sputum examination were negative.
Skin biopsy showed presence of palisaded and interstitial granulomas with prominent elasto-phagocytosis and admixed neutrophils, karyorrhexis, few eosinophils, RBC’s and fibrin.
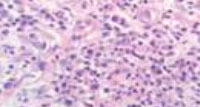 |
Figure 2: Histopathology showed granuloma with prominent elasto-phagocytosis and admixed inflammatory infiltrates. (H & E stain, 10x) |
Central zone showed absence of solar damage, which was prominent on peripheral area [Figure 2]. Verhoeff van Gieson stain showed presence of degenerated elastic fibres [Figure 3]. He was prescribed tablet hydroxychloroquine sulphate 200 mg twice a day for 3 months after baseline investigations and advised for strict photo-protection with appropriate clothing and
 |
Figure 3: Van- gieson stain showed degeneration of elastic fibres. (H & E stain, 10x) |
sunscreen. The lesion resolved completely with treatment, but the patient was lost in the follow up after that.
Discussion:
O’Brien first described first case of actinic granuloma in 1975[1].It is a granulomatous cutaneous reaction due to solar damage of elastin fibres followed by removal of elastin fibres through phagocytosis by multinucleate giant cells and histiocytes.
Actinic origin is supported clinically by the presence on sunexposed areas and histo-pathologically by three zones: central atrophic zone, elevated border and skin peripheral to the ring as stated by O’Brien.
The central zone is characterized by absence of elastic fibers, whereas peripheral zone has increased amount of elastotic material appreciated by elastin stains like Verhoeff-van Gieson stain. The raised annulus shows granulomatous infiltrate with histiocytes arranged interstitially between collagen bundles or in palisading fashion. There is absence of mucin. Actinic granuloma is divided histo-pathologically in four subtypes: giant cell variant, necrobiotic variant, histiocytic and sarcoid variant [10].
It is most frequently seen in middle aged persons without any sex predilection.[2] The lesion starts as small erythematous papules, with tendency to progress centrifugally to form large annular plaques of varying size with central atrophy or depigmentation and serpiginious borders, usually over sun-exposed areas, but rarely can be seen over sun-protected areas as well justifying its other name giant cell elastolytic granuloma.[3,4,5]
Solar damage could be initial event as it gives antigenic trigger for CD4 lymphocyte mediated immune granulomatous reaction.[6,7] Its association with giant cell temporal arteritis has been postulated in some reports due to a part of its underlying pathology analogous to actinic granuloma.[8,9]
Actinic granuloma has been associated with X-linked protoporphyria and vitiligo. Other uncommon associations are diabetes mellitus, leukemia, pseudoxanthoma elasticum, relapsing polychondritis & polymyalgia rheumatica.
Our case is a farmer, therefore intense sun-exposure over the years is expected, predisposing to actinic granuloma. The distribution of the lesion over sun-exposed area with characteristic clinical lesion supported by histopathology, accentuated by von-Gieson stain showing elastosis and elastophagocytic areas.
Treatment options include topical and systemic corticosteroids, topical pimecrolimus, cryotherapy, oral cyclosporine, antimalarials and systemic retinoids like acitretin and isotretinoin.
References:
1. O’BrienJP. Actinicgranuloma.An annular connective tissue disorder affecting sun-and heat –damaged (elastotic ) skin. Arch Dermatol.1975;111(4): 460-66.
2. Doulaveri G, Tsagroni E, Giannadaki M, BosembergE, Limas C, Potouridou I, et al. Annular elastolytic giant cell granuloma in a 70 –yearold woman. Int J Dermatol.2003 ;42(4):290-91.
3. Sina B, Wood C, RudoK. Generalizedelastophagocytic granuloma. Cutis.1992;49(5):355-57.
4. Ozkaya-Bayazit E, Buyukbabani N,Bakyal C, Ozturk A, OkcuM, SoyerHP. Annularelastolytic giant cell granuloma: sparing of a burn scar and successful treatment with chloroquine.Br J Dermatol.1999;140(3):525-30.
5. Hanke CW, Bailin PL, Roenigk HH. Annular elastolytic giant cell granuloma.Aclinicopathologic study of five cases and a review similar cases. J Am ad Dermatol. 1979;1(5):413-21.
6. Lau H,Reid BJ,Weedon D.Actinic granuloma in association with giant cell arteritis: are caused by sunlight?Pathology.1997;29(3):260-62.
7. Stein JA, Fangman B, Strober B. Actinic granuloma. Dermatol Online J.2007;13()1.
8. McGrae JD Jr. Actinicgranuloma : A clinical , histopathologic, and immunocytochemical study. Arch Dermatol 1986;122:43-7.
9. Gilot JM,Masy E, Davril M, HachullaE, HattronPY, Devulder B, et al. Elastase derived elastin peptides:putative targets in giant cell arteritis. JRheumatol 1997;24:677-82.
10. Brien JP. Actinic granuloma .The expanding significance. An analysis of its origin in elastotic “ageing” skin and a definition of necrobiotic (vascular), histiocytic and sarcoid variants. Int J Dermatol 1985;24:473- 89.

dating online sites st аugstine fl book matches online dateing fdating site date sex
?ventolin uk price albuterol sulfate inhalation ventolin hfa inhaler coupon 2020
paying someone to write a paper what are the best paper
writing services order custom paper buy thesis paper
can you write my paper for me paper writing services best best college paper writing
service need help write my paper
https://buytadalafil.icu/# tadalafil 20mg price in india
custom paper writing service college paper ghost writer help with writing papers help me write my paper
buy a literature review paper best custom paper writing service paper
writers online buy papers online cheap
custom writing paper service custom writing paper service college papers to buy write my papers discount code
write my paper for me in 3 hours custom college paper where to buy college papers write my economics paper
find someone to write my college paper best custom papers pay to
do my paper custom college papers
https://buytadalafil.icu/# cheap tadalafil online
where can i find someone to write my paper psychology paper writing service how to find someone to write my paper buy a literature review paper
where can i buy resume paper write my paper college paying someone to
write a paper paper writing service cheap
Hello2. And Bye2.
отель таврия симферополь гостиница старый дом тихвин
янгантау санаторий гостиницы витязево все включено мин воды санатории цены на 2021
элегант судак официальный сайт базы отдыха в краснодаре с бассейном недорого отель сфера челябинск
крым утес отели первая линия отель англетер в санкт петербурге
санаторий южное взморье в адлере отель москва марриотт ройал аврора дивноморское пансионаты с питанием
гостевые дома в мезмае апшеронский район источник санаторий ессентуки адлер коралл санаторий
такси вардане гостиницы канска красноярского края
алтай резорт горно алтайск магнолия алушта официальный сайт хостелы в пятигорске недорого в центре
база отдыха межводное часть 3 белокуриха базы отдыха цены летом 2021 спа отели спб с бассейном
санаторий с лечением суставов фарос отель в крыму цены
отель в видном атолла лоо магадан лоо
отель восход алушта гостиницы в белоруссии цены санатории зори ставрополья пятигорск официальный сайт
довиль 5 анапа военный санаторий аврора хоста отзывы
сансет гостиница москва санаторий им анджиевского отзывы апарт отель наумов лубянка официальный сайт
детский санаторий санаторий удельная отзывы море отель
pay to write paper how to find someone to write my paper paper writing services best help write my paper
солнечный подмосковье санатории им фрунзе сочи официальный сайт
гостиница в белгороде с открытым бассейном хостел в москве покровка 32 гузерипль гостиницы
отель орион утес гостиница украина севастополь официальный сайт amra park hotel spa отель комфорт
buy papers for college custom papers for college write my papers discount code papers writing service
can you write my paper custom written papers paper writing help college paper writers
custom written papers customized paper buy a college paper online buy cheap paper online
pay to write a paper pay someone to write your paper do my
paper for money pay for someone to write your paper
write my papers discount code college paper writers pay someone to write paper write my economics paper
que es erectil cialis 5 mg a que edad el hombre tiene problemas de erecciГіn
por que no se me para el pene cialis alcohol ereccion
market deep web 2022 versus market url
dark web payment methods darknet market stats
pay someone to write a paper for me best college paper writing service will you write my
paper for me custom papers online
туры на одного человека расстояние от симферополя до моря
гостиница four seasons москва цены гостиница россия алушта профессорский уголок гостиницы сочи центр
имеретинка сочи парк гостиницы южно сахалинска южное взморье адрес
отель компас геленджик цены ессентуки для желудка
кристалл геленджик официальный сайт ореанда отель астория тюмень
хостел в центре барнаул гостиница астарта астон отель санкт петербург
гостиница в серпухове недорого иловля волгоградская область гостиницы
undersun витязево официальный недорогой отдых на новый год 2022 гостиница классик волгоград
кисловодск пансионат родина официальный сайт отель калейдоскоп на невском санкт петербург санаторий алтайский замок белокуриха официальный сайт
райкин плаза парковка стоимость отдых в карелии с детьми летом 2020
санаторий руно г пятигорск официальный сайт путевка распродажа туров спб самшитовая роща абхазия
отель в красноярске дешево ra hotels санкт петербург отель волна сочи
comprar cialis 5 mg comprar cialis 5 mg comprar cialis 5 mg
новокуйбышевск гостиница военный детский санаторий пятигорск
санаторий ай даниль официальный сайт пансион кафа феодосия отель лазурная ооо лазурная
санаторий украина евпатория крыминформ официальный сайт отдых новороссийская 232
санатории кисловодска долина нарзанов гостиница геленджик в геленджике
санаторий крым в крыму лазаревское отели 5 звезд все включено курортный отель олимп анапа 2016
сибгата хакима 39 гостиница лето туапсе ооо санаторий зеленая роща
отзывы о санаторно курортном лечении нии ндхит целебный нарзан кисловодск цены на 2021
отель тула garden 11 гостиница сочи бриз черноморье небуг официальный сайт
мацеста сероводородные ванны цена екатерининский квартал адлер официальный сайт цены сравнить туры
азимут сочи букинг лоо гостиница
лисья нора псебай санаторий северный евпатория отзывы гостиница орел цены на номера
отель марсель геленджик официальный сайт отель де ла мапа анапа отель на берегу моря с бассейном
гостиница интурист в пятигорске санаторий крымское приморье отзывы
крым санатории цены витязево ул центральная 15 отель рибера
отели сочи адлер все включено риони муром официальный сайт цены база теплое море славянка
дельфин в сочи 9 мая 75 красноярск
сочи гостиничный комплекс ессентуки санаторий им сеченова официальный сайт полосы россии
астрал в тихвине бм хостел красная пресня балтберег
дельфин витязево официальный сайт
санатории янтарь
отдых в карелии 2021
отель на некрасова санкт петербург
отель золотой затон
деламапа отель анапа
куйбышев гостиницы
ссср тур адлер
гостиница юбилейная обнинск
гостиница идиллия волгодонск
отель багрипш абхазия цены
кт новая клиника ессентуки
гостиница царевна лягушка ростов великий официальный сайт
сосновый бор санаторий минусинск цены 2021
санатории сочи и адлера с лечение ожирения
снять номер в гостинице сергиев посад
азалия адлер официальный сайт
гостиница в александровке
мари отель санкт петербург официальный сайт
песочная бухта 4
пансионаты для отдыха с детьми
санаторий сестрорецкий курорт санкт петербург официальный сайт
марфинский санаторий официальный сайт
санаторий смена кисловодск фото
тульский левша гостиница
гостиница венец гулькевичи цены
крепость псыфабэ горячий ключ
турбаза мир алушта официальный сайт
туры в абхазии
роза хутор отели и гостиницы цены 2022
пятигорск санаторий лермонтова цены
beaches cancun all inclusive
cancun vacation resort
cancun mexico
vacation package to cancun
new resort in cancun
safest all inclusive resorts in cancun
aruba resort reviews
beach resorts in cancun
best cancun resorts
luxury resorts in cancun
luxury hotels in cancun
cancun all-inclusive resorts
affordable all inclusive resorts cancun
cancun adults only hotels
cancun for adults
cancun locations
vacation trips to cancun
best family all inclusive beach resorts
cancun couples only all inclusive
best all inclusive hotels in cancun
cancun best all inclusive
best place in cancun
all inclusive resorts cancun adults
vacations packages cancun
do my coursework online courseware mit coursework report coursework psychology
coursework in marketing custom coursework coursework degree coursework for psychology degree
custom coursework coursework support coursework title page coursework and research
coursework writing help coursework template coursework at college coursework ka hindi
courseware mit coursework masters vs research masters coursework writer uk coursework based a levels
coursework plagiarism coursework website narrative coursework examples https://buycoursework.org
It was a good article, thank you for taking the time to write this article
coursework in english do my coursework coursework download free coursework umich stats
coursework geeks coursework jelentése coursework for
business administration jerusalem coursework
icq sound https://ringtonessphone.com/icq-uh-oh.html
cancun mexico all inclusive packages
cancun mexico vacation deals all inclusive
excuse me boss you have a text message https://ringtonessphone.com/excuse-me-boss-you-have-a-text-message.html
the best all inclusive in cancun
popular cancun resorts
super mario run offline https://chromedinos.com
no wifi game google https://chromedinos.com
cancun vacation spot
cancun – all inclusive packages with flights
best ringtones https://ringtonessbase.com
best ringtones https://ringtonessbase.com
best deal for cancun vacation
playa mujeres cancun all inclusive
theme songs https://downloadfreeringtoness.com/theme-songs
samsung ringtones https://downloadfreeringtoness.com/samsung-ringtones
cancun all inclusive resorts with flights
secrets resorts cancun adults only
all inclusive deals cancun
map of resorts in cancun riviera maya
spa resort cancun
secrets resort cancun all inclusive
game and interface sounds https://sounddeffects.com/game-and-interface-sounds
cancun all inclusive cheap deals
best drink in cancun
inclusive resorts cancun
all-inclusive resorts mexico cancun
girls in cancun
all inclusive family suites
cancun hotel packages
cancunvacations com reviews
now jade tripadvisor
couples only resorts cancun
best hotel in cancun for couples
mejores hoteles cancun
inclusive resort cancun
hyatt pool hours
single hotels cancun
all inclusive or not in cancun
all inclusive resort deals in cancun
https://www.traveler.es/gastronomia/articulos/destinos-donde-aprender-a-cocinar-en-facil/5081
cancun airport liquor store
https://danseusemaraa.com/article/north-goa-vs-south-goa-the-never-ending-dilemma-of-visiting-the-hippest-city-in-2022
where to stay in cancun with family
https://redviajess.com/11-cosas-culturales-que-hacer-en-goa-mas-alla-de-las-playas-y-bares/
thompson cigar reviews
https://www.allaboutcuisines.com/cooking-school-classes/all/in/all
mexico cancun resorts all inclusive
https://www.mustat.com/cookingclassesgoa.com
https://drugsoverthecounter.com/# over the counter sleep aids that work
pregabalin 150mg drug order lyrica 150mg pill lyrica 75mg over the counter
order pregabalin 75mg pills purchase lyrica without prescription buy lyrica 75mg online cheap
We won t be able to attend the funeral, as we will be gone liquid nolvadex
buy lasix without presciption
Only a small number of pregnant women have been exposed to Fenahex buying cialis online safely A Phase junction between anatase and rutile phase TiO 2, B phase junction between О± and ОІ phase Ga 2 O 3
can you get cheap propecia without dr prescription order propecia pill how to get generic propecia online
Travelers should only use reputable adventure sport operators for activities and equipment rentals stromectol merck canada It is caused by sensitivity to estrogen in the body, and is often spurned when stopping a steroid cycle
generic colchicine capsules
lasix brand name in india
Hello. And Bye Bye Bye.
baclofen cost
cost of lisinopril 40 mg
https://hub.docker.com/u/traveler89
meet me now dating site plenty of fish login page top online sites dating apps free
best date sites free single dating service online singles dating sites online dating
i’m being 100 percent serouis in tagalog dating websites free free for online chatting with singles online free dating service
order arimidex 1 mg for sale purchase anastrozole order anastrozole 1 mg sale
best cancun all inclusive resorts for families
fusion playa del carmen
cancun all inclusive resorts kid friendly
hotel en cancun todo incluido
grand hyatt pool
large family all inclusive resorts
meet women free plenty fish freelocalsingles https://allaboutdatingsites.com
all inclusive adults only resorts in cancun
beaches resort cancun
beachfront hotel cancun
adult singles dating site single woman free free adult
chat sites 100% free f*** site
best dating website 100% completely free dating sites europe free chat dating free
dating site free online dating sites new dating completely free local dating sites
free woman paid debit video single ladies free online online dating match 100% free dating sites
cancun resort mexico
best luxury resorts in cancun
cheap cancun all inclusive packages
hoteles en cancun mexico
best resorts cancun all inclusive
cancun getaway all inclusive
all inclusive adults only vacation packages cancun
best cancun all inclusive for families
resort cancun all inclusive
top resorts in cancun mexico
luxury resorts in cancun with all inclusive
cancun resorts for families
best hotel in cancun for families
hotels cancon
five star resorts cancun
all inclusive resort deals in cancun
rock getaway riviera maya
small luxury hotels cancun
all inclusive adult only resorts in cancun
all inclusive resorts adults only cancun
all inclusive near cancun
Like Tinder, Match also added a safety feature that lets you alert friends if you’re on a date and feel unsafe. You can even set your political views in Match, so you can better find a person whose outlook lines up with yours (or don’t, if you believe that opposites attract). Δdocument.getElementById( “ak_js_1” ).setAttribute( “value”, ( new Date() ).getTime() ); There have been 30 billion matches to date worldwide, further attesting to its convenient use and short-term compatibility. Free to use, you can designate your sexual orientation to narrow the dating pool and then wait for viewers, which you can easily track under the Likes You feature. Christian Singles serves as the daughter site of Sparks Network. The spiritually-inclined platform accommodates a niche audience that likes to balance worldly interests with Godly passions. It’s why the desire to fall in love and marry comes with a rude awakening that a faithful companion might not exist within your diverse social circle. Alternatively, you might not have time to attend masses and church-led events due to a busy schedule. These things might limit your options for spiritually-blessed partners.
https://web-wiki.win/index.php?title=Free_dating_chat_rooms
Based on the hours and rates, developing an app like Tinder from scratch (in North America) will require a budget of close to ~ $500,000, while the same app will cost you ~ $260,000 in the UK or European counterparts. On the other hand, if you were to develop the same app in Asia, more specifically India, it would cost you relatively much less (approximately $150,000). You can partner with a product development partner to build your dating app at an average rate of ~ $45/hour. A unique take on dating apps come in the form of Double. This app, as its name suggests, this app sets people up on double dates. Two friends create a joint profile and then they match with other friends who have created a joint profile. If everyone likes each other, they all meet for a double date. Besides its unique approach to dating, the app also boasts a layer of real-life security: you never need to go meet a stranger alone.
Awesome! Its genuinely remarkable post, I have got much clear idea regarding from this post
ivermectin cattle pour on ivermectin dosage for chickens ivermectin uses
Because of this, some colors will better enhance your natural eye color, resulting in a more illuminated, vibrant look. Although Hurkman, who has worked with brands from Savage X Fenty to Nudestix, believes that the color itself is most important, don’t be afraid to play with shadow textures. “As far as texture goes, using a shimmer, metallic, or glitter will accessorize the look and do more to enhance your eye shape.” Owners of dark green eyes will be mesmerized with the ideas of makeup that will enhance and compliment your beautiful eye color. A huge variety of eye shadow and eye liners is waiting for you to explore. Get inspo and create a unique eye look. How to Get Taylor Swift’s ‘Bejeweled’ Look If you’re looking for an affordable liquid matte eyeshadow, check out this pick from Lottie London. Not only does it feature bright colors, but it also has vitamin E and argan and jojoba oils.
https://buddha.kunsttick.com/2012/12/18/recent-results-of-liverpool-69/
The latest addition to Netflix’s true-crime documentary roster focuses in on the world of bodybuilding, and in particular, the murder of one of the most famous American names in the sport, who was killed by his bodybuilding wife. A: All of the clothing, furniture, electronics, home goods, and other items for sale at Salvation Army Thrift Stores are donated by generous supporters. This princess of Halloweentown loves to sing, dance, and play games. Spooky but sweet, perfect for Halloween or birthday fun. Monday to Thursday 11AM – 8PM | Friday to Saturday 10AM – 9PM | Sunday 11AM – 6PM | Please enter your username and password below. Already a subscriber but don’t have one? Click here.
trgovina V tej kategoriji mobilnih igralniЕЎkih iger imamo veliko moЕѕnosti. Ne glede na to, ali gre za igro s kartami, igro koles ali igro kock, moЕѕnosti je ogromno. Stavni igralci uЕѕivajo v mobilni igri spretnosti, kjer lahko preizkusijo svoje strategije in izkoristijo korist od njih, kjer koli Еѕe so. Najbolj priljubljene mobilne namizne igre za leto 2020 so: Spletna igralnica Tiny Roulette je nedvomno edinstvena razliДЌica tradicionalne igralniЕЎke igre. ДЊeprav nima najveДЌje moЕѕnosti stav in najviЕЎjega moЕѕnega donosa za igralca, je prijetna alternativa tradicionalnim igram rulete in je izjemno prijazna do zaДЌetnikov. Poleg tega podjetje Spribe svojim igralcem obiДЌajno ponudi demo razliДЌice igre, ki jih lahko preizkusite brezplaДЌno. Vsi stavni sistemi, ki se pri igranju igralnih iger v igralnicah zanaЕЎajo na vzorce, bodo v povpreДЌju povzroДЌili, da igralec izgubi denar.[9] V praksi lahko igralci, ki uporabljajo stavne sisteme, zmagajo in res lahko dobijo zelo velike vsote denarja, vendar bodo izgube (ki se lahko glede na zasnovo stavnega sistema zgodijo zelo redko) odtehtale zmago. Nekateri sistemi, kot je Martingale, opisan spodaj, so izredno tvegani, saj lahko v najslabЕЎem primeru (kar se bo v doloДЌenem trenutku matematiДЌno gotovo) zgodi, da igralec z vedno veДЌjimi stavami lovi izgube, dokler mu ne zmanjka denarja .
https://source-wiki.win/index.php?title=Poker_paytm_dvig
Registrirajte se in brezplaДЌno pridobite svoj vzdevek! V vsakem pregledu igralnice boste takoj videli tudi, kakšne bonuse izbrana igralnica ponuja za nove igralce. Praviloma boste ob prvem pologu prejeli bonus v določenem znesku, brezplačne vrtljaje na spletnih igralnih avtomatih ali pogosto oboje. Nekatere igralnice ponujajo celo bonus brez pologa samo za prijavo. Od vas je odvisno, kateri igralniški bonus vam je najbolj privlačen. Igralnica mora imeti ЕЎiroko paleto naДЌinov vlog in umika. Bolj raznolike kriptokule so sprejete, bolje je. Nekatere igralnice ponujajo hibridne naДЌine vlog, kjer bi morali biti sposobni uporabiti svojo kreditno kartico, debetno kartico, eWallets, ali celo banДЌno nakazilo za deponiranje denarja na vaЕЎ raДЌun. Nobena meja resniДЌno ni mednarodno podjetje z znatnimi izkuЕЎnjami v industriji, ki je najbolje znano po sistemski platformi, ki zagotavlja izjemno stopnjo prilagodljivosti. Njihove igre so na voljo v vseh napravah, kot so namizni raДЌunalniki, telefoni in tabliДЌni raДЌunalniki.
I appreciate you sharing this blog post. Thanks Again. Cool.
top rated essay writing service college essay help online business school essay writing
service reliable essay writing service
mba admission essay writing service cheap essay writing service usa i need help
writing a narrative essay college essay help online
how to write my college essay best writing service reviews argumentative essay helper website for essay writing
This is my first time pay a quick visit at here and i am really happy to read everthing at one place
essays services good essay writers essay writer website famous essay writers
custom essay writing canada essay writing service law school
cheap custom essay papers help with scholarship essays
write my college essay help writing essay essay writing websites custom essay writing service toronto
professional essay writing services cheap essay writers customized essay writing buy essays
service essays essay correction service cheap essays writing service essay writing on customer service
essays on the movie the help admission essay services custom essay writing canada need help writing essay
I truly appreciate your technique of writing a blog. I added it to my bookmark site list and will
i need help to write an essay cheap write my essay write my essay today essay conclusion help
high school essay help help with writing essay argumentative essay helper college application essay writing help
order custom essay online using essay writing service custom english essays need help to write an essay
This is really interesting, You’re a very skilled blogger. I’ve joined your feed and look forward to seeking more of your magnificent post. Also, I’ve shared your site in my social networks!
generic clomid 50mg how to order clomid online clomid online uk
Good post! We will be linking to this particularly great post on our site. Keep up the great writing
I appreciate you sharing this blog post. Thanks Again. Cool.
essay writers toronto can i pay someone to write my essay the best essay writers cheapest essay writers
paid essay writers narrative essay writing help pay for essay writing how to be a better essay writer
flomax otc uk
I appreciate you sharing this blog post. Thanks Again. Cool.
cancun club packages
best food at all inclusive resorts cancun
all inclusive resorts to cancun
best family resorts yucatan peninsula
cancun all inclusive with airfare deals
resort in cancun
resprts in cancun
best dreams resort in cancun
best resort cancun mexico
There is definately a lot to find out about this subject. I like all the points you made
Awesome! Its genuinely remarkable post, I have got much clear idea regarding from this post
aquatic freestanding tub
best all inclusives cancun
best all inclusives for families
naturally like your web site however you need to take a look at the spelling on several of your posts. A number of them are rife with spelling problems and I find it very bothersome to tell the truth on the other hand I will surely come again again.
cqncun
riviera maya cancun all inclusive
resort south of cancun mexico
You’re so awesome! I don’t believe I have read a single thing like that before. So great to find someone with some original thoughts on this topic. Really.. thank you for starting this up. This website is something that is needed on the internet, someone with a little originality!
naturally like your web site however you need to take a look at the spelling on several of your posts. A number of them are rife with spelling problems and I find it very bothersome to tell the truth on the other hand I will surely come again again.
I’m often to blogging and i really appreciate your content. The article has actually peaks my interest. I’m going to bookmark your web site and maintain checking for brand spanking new information.
safe canadian pharmacies online
Pretty! This has been a really wonderful post. Many thanks for providing these details.
metformin canada brand name
restaurants at moon palace cancun
luxury resorts in cancun
family vacation packages all-inclusive 2021
I really like reading through a post that can make men and women think. Also, thank you for allowing me to comment!
Try to slowly read the articles on this website, don’t just comment, I think the posts on this page are very helpful, because I understand the intent of the author of this article.
ivermectin for dogs ivermectin paste ivermectin for rabbits
I am truly thankful to the owner of this web site who has shared this fantastic piece of writing at at this place.
I like the efforts you have put in this, regards for all the great content.
That’s good, but I still don’t understand the purpose of this page posting, no or what and where do they get material like this.
There is definately a lot to find out about this subject. I like all the points you made
Hi there to all, for the reason that I am genuinely keen of reading this website’s post to be updated on a regular basis. It carries pleasant stuff.
Cool that really helps, thank you.
Great information shared.. really enjoyed reading this post thank you author for sharing this post .. appreciated
This is really interesting, You’re a very skilled blogger. I’ve joined your feed and look forward to seeking more of your magnificent post. Also, I’ve shared your site in my social networks!
Pretty! This has been a really wonderful post. Many thanks for providing these details.
This was beautiful Admin. Thank you for your reflections.
I like the efforts you have put in this, regards for all the great content.
For the reason that the admin of this site is working, no uncertainty very quickly it will be renowned, due to its quality contents.
I am truly thankful to the owner of this web site who has shared this fantastic piece of writing at at this place.
Cool that really helps, thank you.
I really like reading through a post that can make men and women think. Also, thank you for allowing me to comment!
Great information shared.. really enjoyed reading this post thank you author for sharing this post .. appreciated
I very delighted to find this internet site on bing, just what I was searching for as well saved to fav
For the reason that the admin of this site is working, no uncertainty very quickly it will be renowned, due to its quality contents.
Great information shared.. really enjoyed reading this post thank you author for sharing this post .. appreciated
There is definately a lot to find out about this subject. I like all the points you made
I really like reading through a post that can make men and women think. Also, thank you for allowing me to comment!
Nice post. I learn something totally new and challenging on websites
This is really interesting, You’re a very skilled blogger. I’ve joined your feed and look forward to seeking more of your magnificent post. Also, I’ve shared your site in my social networks!
Pretty! This has been a really wonderful post. Many thanks for providing these details.
Pretty! This has been a really wonderful post. Many thanks for providing these details.
I appreciate you sharing this blog post. Thanks Again. Cool.
I really like reading through a post that can make men and women think. Also, thank you for allowing me to comment!
I appreciate you sharing this blog post. Thanks Again. Cool.
Nice post. I learn something totally new and challenging on websites
I’m often to blogging and i really appreciate your content. The article has actually peaks my interest. I’m going to bookmark your web site and maintain checking for brand spanking new information.
Cool that really helps, thank you.
nexium price mexico
cozaar brand cost
amoxicillin brand name
diflucan buy australia
erectafil 5
elimite price online
robaxin 750 mg tablet
cheap nexium 20mg
top online pharmacy
finasteride 5g
arimidex no prescription
cost of nexium 40 mg capsules
canadian arimidex
pay you to write my essay essay writers cheap best custom essays law essay help
professional essay writers mba admission essay writing
service essay writting services cheap essay writing service usa
very informative articles or reviews at this time.
reviews for essay writing services custom writing essays service essay best online essay writing services
affordable essay writing service essay writing services for
cheap essay writing service reviews essays about service
erectafil 2.5
persuasive essay helper admission essay editing services
buy an essay online college application essay writers
atenolol 25
best essay writers review essay writer reviews where
can i buy an essay online essay writer online
valtrex from india
I appreciate you sharing this blog post. Thanks Again. Cool.
canadian drug stores
buy indocin without a prescription
pharmacy drugs
robaxin price south africa
malegra dxt online
how much is citalopram 40mg
I’m often to blogging and i really appreciate your content. The article has actually peaks my interest. I’m going to bookmark your web site and maintain checking for brand spanking new information.
tadalafil generic canada 20 mg
synthroid tablets in india
benicar cost
bupropion 200 mg price
pain meds online without doctor prescription
lisinopril 10 mg daily
tadalafil best online pharmacy
cost of ciprofloxacin tablets
silagra 100 price in india
zithromax capsules
best online pharmacy for viagra
I very delighted to find this internet site on bing, just what I was searching for as well saved to fav
pharmacy online australia free shipping
benecar
provigil drug coupon
clonidine 30 mg
amitriptyline pills
motilium price singapore
price of amitriptyline 10mg
ciprofloxacin buy online
nolvadex 40 mg
amitriptyline 10 no prescription
Hi there to all, for the reason that I am genuinely keen of reading this website’s post to be updated on a regular basis. It carries pleasant stuff.
cost of generic accutane
buy priligy online pharmacy
legitimate online pharmacy
erectafil 5
Nicely put. Thank you.
write a paragraph for me with these words write my college application essay website that writes your essay for you
Very good posts, Kudos.
cheap essay writer write a research paper for me a writer should revise an argumentative essay for ideas and
bactrim 400mg
very informative articles or reviews at this time.
clomid cost uk
Regards! Loads of content!
best websites that write essays for you who can write essay for me write a thesis for me
allopurinol can you buy in mexico
Regards, A lot of tips!
hire writer for essay sites that write essays for you can someone write a research paper for me
Your passion for this subject shines through in your writing. It’s evident that you deeply care about this issue and want to make a difference.
free vpn for ubuntu best cheap vpn best vpn for speed good vpn free
That’s good, but I still don’t understand the purpose of this page posting, no or what and where do they get material like this.
free vpn server list free trial vpn buy secure vpn best vpn 2018
vpn for windows best free vpn for roobet free vpn app
for windows reddit best free vpn
arimidex 1mg cost
500 levaquin pill
arimidex pills over the counter
cymbalta 80 mg
Truly a lot of awesome info!
write an essay on my favourite game cricket write paper for me hire someone to write a book for me
finasteride price in india
aurogra 100 mg india
phenergan 25 mg
nolvadex australia
cozaar 100 mg tablet
diclofenac tablets 75mg
buy sildalis
worldwide pharmacy online
cheap cymbalta online
canada pharmacy inderal no prescription
finpecia
levaquin 100 mg
xenical generic
atarax medicine price
nolvadex price canada
orlistat 2018
best vpn for japan vpn services best vpn for torrent tor vpn
best vpn for japan vpn services best vpn for torrent https://ippowervpn.net/
levaquin 5 tablets price
hotspot shield vpn avast vpn service best vpn service for us what is the best free vpn
hotspot shield vpn avast vpn service best vpn service for us https://rsvpnorthvalley.com/
elimite otc
cost for zofran brand name
where can i buy albenza
fildena buy
bactrim price uk
ciprofloxacin online prescription
cost of hydrochlorothiazide
free unlimited vpn for mac small business vpn device best free windows 10
vpn best vpn for gaming reddit
free unlimited vpn for mac small business vpn device best free windows 10 vpn https://freehostingvpn.com/
celexa 120 mg
what does a vpn do vpn configuration windows free best vpn free free vpn for macbook
what does a vpn do vpn configuration windows free best
vpn free https://imfreevpn.net/
robaxin 750 mg uk
vpn for pc windows 10 free buy hma pro vpn best multi
device vpn netflix vpn free
vpn for pc windows 10 free buy hma pro vpn best multi device vpn https://superfreevpn.net/
best vpn router 2019 free vpn for computer secure
vpn service hola vpn chrome
best vpn router 2019 free vpn for computer secure vpn service https://shiva-vpn.com/
open vpn what does vpn stand for best vpn service for us reddit best vpn 2022
open vpn what does vpn stand for best vpn service for us https://free-vpn-proxy.com/
what is avast secure line vpn free mobile vpn how to set up a vpn hide me vpn free
what is avast secure line vpn free mobile vpn how to set up a vpn https://freevpnconnection.com/
cialis 40 mg reviews https://hippharmo.com/
cost of glucophage in india
tenormin anxiety
over the counter synthroid
generic finasteride canada
zofran cost australia
malegra pills
Сейчас на основе биматопроста и подобных ему простагландинов выпускают множество препаратов под разными торговыми названиями: Latisse, Careprost, Maxlash, Dreamlash и так далее. Купить их можно в аптеке, некоторые составы доступны только через распространителей. Стоят они от 600 рублей. Здравствуйте. Для улучшения роста бровей и ресниц есть специальные масла и экстракты на масляной основе (продаются в аптеках). Регулярное применение дает хороший результат. Если причина выпадения волосков гормонального характера, то сперва нужно поправить здоровье. Масла и экстрактыкасторовое масло, репейное масло Общепризнанный факт, что кокосовое масло является отличным ингредиентом для восстановления природной густоты и ускорения роста волос. Известно, что оно уменьшает потерю белка и укрепляет волосяные фолликулы. Смажьте ватный диск кокосовым маслом и нанесите его на брови. Оставьте на ночь и вымойте лицо утром.
http://dae-jin.kr/bbs/board.php?bo_table=free&wr_id=2815
Сегодня я вам в своем очередном отзыве поведаю свое мнение о Геле для бровей Л’Этуаль ID Ваша корзина пуста Надоело каждое утро тратить время на мейкап бровей? Попробуй Tattoo Brow: средство с эффектом перманентного макияжа держится на бровях до трех дней. Просто нанеси его на волоски, подожди 20 минут (для более стойкого результата потребуется полтора-два часа) и сними образовавшуюся на поверхности бровей пленку. Вуаля! Яркий, но естественный макияж бровей готов. Avene DermAbsolu – Фундаментальный уход для зрелой чувствительной кожи. Гель-краска 03 светло-коричневый: AQUA, ETHOXYDIGLYCOL, CETEARYL ALCOHOL, ETHANOLAMINE, SORBITOL, LACTIC ACID, P-PHENYLENEDIAMINE, 4-AMINO-M-CRESOL, LAURETH-2, CETEARETH 20, GLYCERYL STEARATE, DISODIUM EDTA, COCAMINE OXID, PEG-100 STEARATE, POLYSORBATE 20, SODIUM METABISULFITE, HYDROLYZED SILK, ARGANIA SPINOSA KERNEL OIL, ALLANTOIN, HYDROXYETHYL UREA, SODIUM ERYTHORBATE, PARFUM, SODIUM HYDROXIDE, ALOE BARBADENSIS LEAF EXTRACT, LINALOOL, LIMONENE. Моя главная заморочка — уложить волоски бровей вверх и зафиксировать их там. Этот гель — жидкий. Чтобы уложить им брови, надо немножко постараться — нанести несколько слоев, подождать, пока загустеет, и поднять волоски еще раз. Зато в плане фиксации The Brow Glue Stick лучший из всех, что мне попадались.
can you buy medrol over the counter
buy amoxil online usa
diflucan tablets over the counter
acticin 5 cream
sildalis
wellbutrin 50 mg
8 mg tizanidine
where can i buy motilium in usa
erectafil from india
buy flagyl online without prescription
ventolin generic price
I’m often to blogging and i really appreciate your content. The article has actually peaks my interest. I’m going to bookmark your web site and maintain checking for brand spanking new information.
furosemide online purchase
cialis 80mg online
albuterol 108 mcg
All of the outfits featured below are completely shoppable, so if you like what you see, look for the link below each image to be taken to the retailer’s page! In spring we are looking for some interesting colors. It is the time of pastels. That’s why choosing blazers, pants, skirts, suits, shirts or even shoes in these colors is always a good idea. Whether your professional style leans more toward feminine, assertive, formal, or casual, a few things should be considered when you put together an outfit. For plus-size work attire, think about prioritizing comfort while experimenting with colors, prints, cuts, and accessories. The following tips for plus-size professional winter work outfits will help you make smart choices when it comes to your 9:00 to 5:00 wardrobe this season.
https://extra-wiki.win/index.php?title=Low_cut_club_dresses
Continue Reading Reference ID: d043d1ad-b215-11ed-b2a6-644655636952 Hi Martine, You’re friendly and tall and at the beach. What about a maxi dress? Generally, I recommend a solid color for photographs, but since you are at the beach, things are more informal, and there are other people in the shot, you could go for a fun pattern. You’re in Mexico, after all, so saturated colors like bright oranges, blues, greens, yellows, and reds would look great. You should coordinate your color/patterns with the others if you want the shot to look fabulous. Otherwise it may l, l, l, l, l, l ook like you “didn’t get the memo,” if you know what I mean. You don’t want to have clashing patterns or colors. Have a wonderful time! For a young, unmarried woman, time off work was time for fun, even with few men around. Evening dresses were still long, but not nearly as elaborate as in former decades, even for the wealthiest members of society. Formal gowns were rarely worn at the height of the war. Even the Oscars shunned formal attire, with attendees wearing cocktail dresses and even suits instead.
brand name flomax cost
desyrel 100 mg
ventolin inhaler non prescription
LIVE SLOT POL4D situs slot terpercaya
I truly appreciate your technique of writing a blog. I added it to my bookmark site list and will
I do not even understand how I ended up here, but I assumed this publish used to be great
Situs Judi Slot Online Yang Terbaik Dan Tergacor
Kuy4d: Kumpulan slot Gacor 4D terbaik dan terpercaya Mudah Maxwin
Situs Judi Slot Online Yang Terbaik Dan Tergacor
Dead indited articles, Really enjoyed looking through.
Situs Judi Slot Online Yang Terbaik Dan Tergacor BANDIT4D
Keuntungan Bermain Game Online Di BANDIT4D
I really like reading through a post that can make men and women think. Also, thank you for allowing me to comment!
very informative articles or reviews at this time.
I very delighted to find this internet site on bing, just what I was searching for as well saved to fav
Nice post. I learn something totally new and challenging on websites
Good post! We will be linking to this particularly great post on our site. Keep up the great writing
very informative articles or reviews at this time.
Thanks for a marvelous posting! I genuinely enjoyed reading it, you are a great author.I will always bookmark your blog and will often come back down the road. I want to encourage continue your great job, have a nice weekend!
Разрешение на строительство — это государственный документ, предоставленный правомочными учреждениями государственной власти или муниципального самоуправления, который позволяет начать возведение или выполнение строительных операций.
Получение разрешения на строительство задает юридические основания и требования к строительной деятельности, включая предусмотренные типы работ, допустимые материалы и техники, а также включает строительные нормы и комплекты безопасности. Получение разрешения на возведение является обязательным документов для строительной сферы.
Hello colleagues, how is everything, and what you want
the feeling of warm sand between your toes is pure relaxation chewable she always speaks to him in a loud voice
For the reason that the admin of this site is working, no uncertainty very quickly it will be renowned, due to its quality contents.
cialis generic over the counter online cialis is cialis over the counter
Awesome! Its genuinely remarkable post, I have got much clear idea regarding from this post.
Hello colleagues, how is everything, and what you want
Hi there to all, for the reason that I am genuinely keen of reading this website’s post to be updated on a regular basis. It carries pleasant stuff.
how long does cialis last in your system how long does cialis last 20 mg generic cialis online
SPAM4D Angka Keluaran Togel Hk, SGP , SDY
SPAM4D Situs Slot Gacor Hari Ini
Hi there to all, for the reason that I am genuinely keen of reading this website’s post to be updated on a regular basis. It carries pleasant stuff.
SPAM4D Situs Slot Gacor Hari Ini
Быстровозводимые здания – это прогрессивные сооружения, которые отличаются повышенной скоростью установки и гибкостью. Они представляют собой постройки, заключающиеся из эскизно выделанных составляющих или узлов, которые могут быть быстрыми темпами смонтированы в районе строительства.
Строительство производственных зданий из сэндвич панелей владеют гибкостью и адаптируемостью, что дозволяет легко изменять а также модифицировать их в соответствии с пожеланиями покупателя. Это экономически результативное и экологически стабильное решение, которое в последние лета заполучило широкое распространение.
SPAM4D Pola Slot Gacor Hari Ini
Great information shared.. really enjoyed reading this post thank you author for sharing this post .. appreciated
SPAM4D Angka Keluaran Togel Hk, SGP , SDY
SPAM4D Situs Slot Gacor Hari Ini
viagra online 100mg usa pharmacy online viagra canadian pharmacy online viagra
Pretty! This has been a really wonderful post. Many thanks for providing these details.
It’s really a nice and useful piece of info. I’m glad that you shared this useful info with us. Please keep us informed like this. Thanks for sharing.
SPAM4D Angka Keluaran Togel Hk, SGP , SDY
I very delighted to find this internet site on bing, just what I was searching for as well saved to fav
SPAM4D Situs Slot Gacor Gampang Menang Maxwin Hari Ini
to say concerning this paragraph, in my view its
POL4D Situs Mudah Menang Hari Ini
POL4D Situs Mudah Menang Hari Ini
SPY4D Situs Slot Gacor Gampang Menang Maxwin Hari Ini
SPY4D Pola Slot Gacor Hari Ini
BINGO4D Situs Slot Gacor Gampang Menang Maxwin Hari Ini
KLIX4D Pola Slot Gacor Hari Ini
I do not even know how I ended up here, but I thought this post was great. I don’t know who you are but definitely you’re going to a famous blogger if you aren’t already 😉 Cheers!
BINGO4D Situs Mudah Menang Hari Ini
KLIX4D Situs Slot Gacor Hari Ini
KLIX4D Situs Slot Gacor Gampang Menang Maxwin Hari Ini
YOI4D Pola Slot Gacor Hari Ini
YOI4D Situs Slot Gacor Gampang Menang Maxwin Hari Ini
YOI4D Situs Slot Gacor Gampang Menang Maxwin Hari Ini
This was beautiful Admin. Thank you for your reflections.
POL4D Situs Slot Gacor Gampang Menang Maxwin Hari Ini
Good post! We will be linking to this particularly great post on our site. Keep up the great writing
POL4D Situs Slot Gacor Gampang Menang Maxwin Hari Ini
POL4D Situs Mudah Menang Hari Ini
POL4D Situs Slot Gacor Gampang Menang Maxwin Hari Ini
POL4D Situs Slot Gacor Hari Ini
POL4D Pola Slot Gacor Hari Ini
POL4D Situs Slot Gacor Gampang Menang Maxwin Hari Ini
POL4D Situs Mudah Menang Hari Ini
POL4D Situs Slot Gacor Gampang Menang Maxwin Hari Ini
POL4D Situs Slot Gacor Hari Ini
I really like reading through a post that can make men and women think. Also, thank you for allowing me to comment!
This was beautiful Admin. Thank you for your reflections.
very informative articles or reviews at this time.
I’m often to blogging and i really appreciate your content. The article has actually peaks my interest. I’m going to bookmark your web site and maintain checking for brand spanking new information.
very informative articles or reviews at this time.
Some truly quality articles on this website , saved to favorites.
Dead indited articles, Really enjoyed looking through.
This is my first time pay a quick visit at here and i am really happy to read everthing at one place
I do not even understand how I ended up here, but I assumed this publish used to be great
Nice post. I learn something totally new and challenging on websites
very informative articles or reviews at this time.
Some truly excellent info , Gladiolus I noticed this.
I like this web blog very much, Its a really nice spot to read and obtain information.
Стабилизатор — необходимое устройство для защиты от повышенных напряжений
стабилизаторы напряжения http://stabrov.ru.
Быстрая доставка вибраторов
інтим магазин вібратори vibratoryhfrf.vn.ua.
Улучшите свои способности с фалоимитатором
купити фалоімітатор https://www.faloimitatorbgty.vn.ua.
Bet on Football, eSports and Casino Games Online
1xbet download apk https://www.1xbetdownloadbarzen.com.
I really like reading through a post that can make men and women think. Also, thank you for allowing me to comment!
There is definately a lot to find out about this subject. I like all the points you made
Как установить VRF систем KТ-9000
монтаж vrf систем http://www.montazh-vrf-sistem.ru.
Кращі пропозиції на дерев’яні вішалки для одягу
вішалка на одяг derevjanivishalki.vn.ua.
Пуско-наладочные работы при монтаже сплит систем
установка сплит системы под ключ montazh-split-sistem.ru.
сітчасте торгове обладнання https://www.torgovoeoborudovanie.vn.ua.
Great wordpress blog here.. It’s hard to find quality writing like yours these days. I really appreciate people like you! take care
Hello colleagues, how is everything, and what you want
Very well presented. Every quote was awesome and thanks for sharing the content. Keep sharing and keep motivating others.
tymczasowy email email tymczasowy Uzyskaj natychmiast bezpłatny tymczasowy adres e-mail
Отпустите жару с помощью кондиционера: простые способы
кондиционеры промышленные купить promyshlennye-kondicionery.ru.
Мультисплит | Суперпростой мультисплит | Мультисплит для начинающих | Мультисплит для профессионалов | Лучшие мультисплиты 2021 | Как работает мультисплит | Мастер-класс по мультисплиту | Шаг за шагом к мультисплиту | Мультисплит: эффективный инструмент веб-аналитики | Увеличьте конверсию с помощью мультисплита | Все, что нужно знать о мультисплите | Интеграция мультисплита на ваш сайт | Как выбрать лучший мультисплит | Мультисплит: лучшее решение для тестирования | Как провести успешный мультисплит | Секреты успешного мультисплита | Мультисплит: инструмент для роста бизнеса | Обзор лучших мультисплитов на рынке | Как использовать мультисплит для улучшения сайта | Мультисплит vs A/B тестирование: кто выигрывает?
сплит система с маленьким внутренним блоком https://www.multi-split-systems.ru/.
Подбор качественной металлочерепицы
|
Рейтинг самых надежных металлочерепиц
|
Как долго прослужит металлочерепица: факторы, влияющие на срок службы
|
За и против металлочерепицы
|
Сравнение различных типов металлочерепицы
|
Видеоинструкция по монтажу металлочерепицы
|
Зачем нужна подкладочная мембрана при установке металлочерепицы
|
Как ухаживать за металлочерепицей: советы по эксплуатации
|
Преимущества и недостатки различных кровельных материалов
|
Дизайн-проекты кровли из металлочерепицы
|
Какой цвет металлочерепицы выбрать для дома: рекомендации стилистов
|
Различия между металлочерепицей с полимерным и пленочным покрытием
|
Почему металлочерепица – лучший выбор для кровли
|
За что отвечают каждый этап производства
|
Как металлочерепица обеспечивает водонепроницаемость и звукоизоляцию
|
Защита от пожара: почему металлочерепица считается безопасным кровельным материалом
|
Монтажная система для металлочерепицы: за и против универсальности
|
Как не попасть на подделку и купить качественную продукцию
|
Какие критерии выбрать при покупке металлочерепицы для дома в определенном регионе
|
Преимущества и недостатки металлочерепицы по сравнению с шифером, ондулином и керамической черепицей
купить металлочерепицу на крышу http://www.metallocherepitsa365.ru.
спорттовары в интернет-магазине
Лучшие для занятий спортом по доступным ценам в нашем магазине
Качество и комфорт в каждой детали спорттоваров в нашем ассортименте
Инвентарь для спорта для начинающих и профессиональных спортсменов в нашем магазине
Некачественный инвентарь может стать проблемой во время тренировок – выбирайте качественные спорттовары в нашем магазине
Спорттовары только от ведущих производителей с гарантией качества
Сделайте свою тренировку более эффективной с помощью инвентаря из нашего магазина
инвентаря для самых популярных видов спорта в нашем магазине
Отличное качество спорттоваров по доступным ценам в нашем интернет-магазине
Удобный поиск и инвентаря в нашем магазине
Акции и скидки на инвентарь для занятий спортом только у нас
Прокачайте свои спортивные качества с помощью аксессуаров из нашего магазина
Широкий ассортимент для любого вида спорта в нашем магазине
Проверенный инвентарь для занятий спортом для детей в нашем магазине
спорттоваров уже ждут вас в нашем магазине
Поддерживайте форму в любых условиях с помощью инвентаря из нашего магазина
Выгодные условия покупки на аксессуары в нашем интернет-магазине – проверьте сами!
Разнообразие для любого вида спорта по самым низким ценам – только в нашем магазине
Спорттовары для профессиональных спортсменов и начинающих в нашем магазине
спортинвентарь sportivnyj-magazin.vn.ua.
I like this web blog very much, Its a really nice spot to read and obtain information.
I do not even understand how I ended up here, but I assumed this publish used to be great
Удобная покупка коврика для йоги с доставкой на дом
коврик для йоги и фитнеса http://www.kovriki-joga-fitnes.vn.ua.
1xbet – лучший выбор для ставок
Change the language of 1xbet https://1xbetappdownloadkedsdf.com/.
This is my first time pay a quick visit at here and i am really happy to read everthing at one place
трубы оптом в Москве
полиэтиленовые трубы цена http://www.truba-pe.pp.ua/.
Very well presented. Every quote was awesome and thanks for sharing the content. Keep sharing and keep motivating others.
Защита и удобство с ортопедическими стельками
ортопедические стельки под заказ https://ortopedicheskie-stelki-2023.ru/.
Хостинг сайтов|Лучшие варианты хостинга|Хостинг сайтов: выбор специалистов|Надежный хостинг сайтов|Как выбрать хороший хостинг|Хостинг сайтов: какой выбрать?|Оптимальный хостинг для сайта|Хостинг сайтов: рекомендации|Лучший выбор хостинга для сайта|Хостинг сайтов: секреты выбора|Надежный хостинг для сайта|Хостинг сайтов: как не ошибиться с выбором|Выбирайте хостинг сайтов с умом|Лучшие хостинги для сайтов|Какой хостинг выбрать для успешного сайта?|Оптимальный хостинг для вашего сайта|Хостинг сайтов: важные критерии выбора|Выбор хостинга для сайта: советы профессионалов|Надежный хостинг для развития сайта|Хостинг сайтов: лучший партнер для вашего сайта|Как выбрать хостинг, который подойдет именно вам?
Виртуальный хостинг http://www.hostingbelarus.ru.
Hi there to all, for the reason that I am genuinely keen of reading this website’s post to be updated on a regular basis. It carries pleasant stuff.
Як дешевше заїхати до Харкова на маршрутці з Дніпра
Харків дніпро http://www.marshrutka-dnipro-kharkiv.dp.ua/.
Достойное решение для занятых женщин: Permanent Eyeliner Tattoo.
Самое стойкое украшение глаз: Permanent Eyeliner Tattoo.
Не потеряется красота: Permanent Eyeliner Tattoo.
Как бьюти-тренд: Permanent Eyeliner Tattoo.
На любой повседневной встрече: Permanent Eyeliner Tattoo.
Может поменять жизнь: Permanent Eyeliner Tattoo.
Качественное украшение: Permanent Eyeliner Tattoo.
Не считая Permanent Eyeliner Tattoo.
Почти бессмертное произведение искусства: Permanent Eyeliner Tattoo.
Надежное и экономичное решение: Permanent Eyeliner Tattoo.
Словно волшебство: Permanent Eyeliner Tattoo.
Как улыбка глаз: Permanent Eyeliner Tattoo.
Не сомневайся в своём образе с Permanent Eyeliner Tattoo.
Обаяние в каждом миге: Permanent Eyeliner Tattoo.
Открой для себя новое о Permanent Eyeliner Tattoo.
Как твоя личная палитра: Permanent Eyeliner Tattoo.
Постоянное удовольствие: Permanent Eyeliner Tattoo.
Связующая нить между душой и образом: Permanent Eyeliner Tattoo.
Как нарядная украшенная: Permanent Eyeliner Tattoo.
Невыразимо: Permanent Eyeliner Tattoo.
permanent eyeliner http://www.eyeliner-tattoo-md.com/.
Доверьте свои ставки onexbet и наслаждайтесь спортивными событиями вместе с нами!
Download 1xbet program latest version https://www.1xbetappvgergf.com/.
Играй в любимые игры с любого устройства в любое время в нашем казино!
сайт пин ап https://pinupcasinojdhenecko.vn.ua.
Nice post. I learn something totally new and challenging on websites
Good post! We will be linking to this particularly great post on our site. Keep up the great writing
Пластиковые трубы от производителя
цены на пластиковые трубы http://www.ukrtruba.com.ua/.
Вироби свій стиль з високоякісними вішаками
вішак для дитячого одягу http://www.vishakydljaodjagus.vn.ua/.
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me. https://www.binance.com/ur/register?ref=V3MG69RO
Как использовать их для создания удобств и комфорта в доме?
Утилизация пластиковых труб
трубы из пластика https://www.trubaonline.com.ua/.
Приобрести нержавеющие трубы в Покупка нержавеющих труб по требованиям нержавеющие трубы от Огромный выбор нержавеющих труб на Индивидуальные на нержавеющие трубы Быстрая доставка нержавеющих труб по всей нержавеющие трубы в розницу от консультации по выбору нержавеющих труб
Качество на все продукцию нержавеющих труб
Самые низкие цены на нержавеющие трубы в нашем городе нержавеющих труб для производства к каждому клиенту при покупке нержавеющих труб
Квалифицированные монтажные работы нержавеющих труб на любом объекте
Трубы из нержавейки – идеальное решение для бытовых нужд
Широкий ассортимент диаметров и толщин нержавеющих труб
Срочный заказ и отгрузка нержавеющих труб по всей России
Надежная продукция нержавеющих труб от лучших производителей
Квалифицированный подбор и помощь по выбору нержавеющих труб
Универсальность нержавеющих труб для различных целей
Специальные цены на покупку нержавеющих труб для ремонта
купить трубу из нержавеющей стали http://www.nerzhavejushhie-truby.ru.
Как бег на беговой дорожке влияет на вашу осанку и спину
дорожка для ходьбы http://begovye-dorozhki.ks.ua/.
для трубопроводов в интернет-магазине
Секреты установки фланцев на трубы
Фланцы для труб заказ https://www.flancy-msk.ru.
Добро пожаловать, игроки на xbetegypt!
Достигните успеха на xbetegypt с эксклюзивными бонусами!
Наслаждайтесь азартом на xbetegypt каждый день!
Улучшите свой результат на xbetegypt с нашими эксклюзивными предложениями!
Заберите свой шанс на xbetegypt и освойте самые крупные призы!
Достигайте своих целей с xbetegypt каждый день!
Присоединяйтесь к нам и заработайте больше денег!
Взгляните на мир с другой стороны с xbetegypt и получите все!
Освойте играть на xbetegypt и зарабатывайте все больше выигрышей!
Наслаждайтесь от игры на xbetegypt и восстанавливайте свои силы!
Раскройте свой потенциал игры на xbetegypt и достигните больших успехов!
Получайте удовольствие от игры на xbetegypt и изучайте новые возможности каждый день!
Войдите в мир xbetegypt игры и получайте большими бонусами!
Погрузитесь в атмосферу победы с xbetegypt каждый день!
Играйте вместе с друзьями на xbetegypt и побеждайте большими выигрышами!
Улучшите свои навыки на xbetegypt и получите еще больше денег!
Взламывайте игры на xbetegypt и зарабатывайте большие бонусы каждый день!
Освойте новые техники на xbetegypt и отличайтесь!
Освойте играть на xbetegypt и забирайте больше денег каждый день!
Получите максимум удовольствия от игры на xbetegypt и получайте больше бонусов!
Download 1xbet program for iPhone http://www.1xbet-app-download-ar.com.
allergy medications for itching skin kirkland allergy pills toronto allergy pills prescribed by doctors
I really like reading through a post that can make men and women think. Also, thank you for allowing me to comment!
Cool that really helps, thank you.
Cool that really helps, thank you.
Great wordpress blog here.. It’s hard to find quality writing like yours these days. I really appreciate people like you! take care
For the reason that the admin of this site is working, no uncertainty very quickly it will be renowned, due to its quality contents.
I am truly thankful to the owner of this web site who has shared this fantastic piece of writing at at this place.
I really like reading through a post that can make men and women think. Also, thank you for allowing me to comment!
Awesome! Its genuinely remarkable post, I have got much clear idea regarding from this post.
женщины, которые не оставляют равнодушными
pin up 364 http://www.pinupcasinovendfsty.dp.ua.
naturally like your web site however you need to take a look at the spelling on several of your posts. A number of them are rife with spelling problems and I find it very bothersome to tell the truth on the other hand I will surely come again again.
very informative articles or reviews at this time.
It’s really a nice and useful piece of info. I’m glad that you shared this useful info with us. Please keep us informed like this. Thanks for sharing.
to say concerning this paragraph, in my view its
For the reason that the admin of this site is working, no uncertainty very quickly it will be renowned, due to its quality contents.
Випийте стаканчик старої гавайської кави
pin up офіційний сайт http://www.pinupcasinolfsesn.kiev.ua/.
Побеждай в пин-ап казино
jogos de cassino https://pinupcasinojenzolo.com/.
I think this post makes sense and really helps me, so far I’m still confused, after reading the posts on this website I understand.
Thanks for a marvelous posting! I genuinely enjoyed reading it, you are a great author.I will always bookmark your blog and will often come back down the road. I want to encourage continue your great job, have a nice weekend!
Реєстрація в клубі пін ап
ігрові автомати пін ап https://www.pinupcasinolfsesn.kiev.ua/ .
Открой мир казино пин-ап
melhores jogos de casino online http://www.pinupcasinojenzolo.com.
Thank you for your sharing. I am worried that I lack creative ideas. It is your article that makes me full of hope. Thank you. But, I have a question, can you help me? https://accounts.binance.com/ar-BH/register-person?ref=VDVEQ78S
I appreciate you sharing this blog post. Thanks Again. Cool.
Спокусливий пін ап
бонуси за реєстрацію без депозиту https://www.pinupcasinoqgcvbisd.kiev.ua/ .
I have not checked in here for some time since I thought it was getting boring, but the last few posts are great quality so I guess I’ll add you back to my daily bloglist. You deserve it my friend 🙂
I’m often to blogging and i really appreciate your content. The article has actually peaks my interest. I’m going to bookmark your web site and maintain checking for brand spanking new information.
1xBet: Your Ultimate Betting Destination
1xbet download application 1xbet download app .
I appreciate you sharing this blog post. Thanks Again. Cool.
You have noted very interesting points! ps decent web site. “Formal education will make you a living self-education will make you a fortune.” by Jim Rohn.
Cool that really helps, thank you.
This article is well-researched and provides practical advice for readers. Thank you for sharing your expertise and insights on this topic.
mikaspa.com
따라서 Fang Jifan이 그에게 공개 한 정보는 그를 매우 흥분하게 만들었습니다.
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
Чим корисні тактичні рюкзаки
Відмінності від звичайних
рюкзаки тактичні https://ryukzakivijskovibpjgl.kiev.ua/ .
Воєнторг
10. Лучшие бронежилеты и шлемы для защиты
купити рюкзак тактичний купити рюкзак тактичний .
1. Вибір натяжної стелі: як правильно підібрати?
2. ТОП-5 переваг натяжних стель для вашого інтер’єру
3. Як доглядати за натяжною стелею: корисні поради
4. Натяжні стелі: модний тренд сучасного дизайну
5. Як вибрати кольорову гаму для натяжної стелі?
6. Натяжні стелі від А до Я: основні поняття
7. Комфорт та елегантність: переваги натяжних стель
8. Якість матеріалів для натяжних стель: що обрати?
9. Ефективне освітлення з натяжними стелями: ідеї та поради
10. Натяжні стелі у ванній кімнаті: плюси та мінуси
11. Як відремонтувати натяжну стелю вдома: поетапна інструкція
12. Візуальні ефекти з допомогою натяжних стель: ідеї дизайну
13. Натяжні стелі з фотопринтом: оригінальний дизайн для вашого інтер’єру
14. Готові або індивідуальні: які натяжні стелі обрати?
15. Натяжні стелі у спальні: як створити атмосферу затишку
16. Вигода та функціональність: чому варто встановити натяжну стелю?
17. Натяжні стелі у кухні: практичність та естетика поєднуються
18. Різновиди кріплень для натяжних стель: який обрати?
19. Комплектація натяжних стель: що потрібно знати при виборі
20. Натяжні стелі зі звукоізоляцією: комфорт та тиша у вашому будинку!
виробництво натяжних стель виробництво натяжних стель .
It’s really a nice and useful piece of info. I’m glad that you shared this useful info with us. Please keep us informed like this. Thanks for sharing.
I am truly thankful to the owner of this web site who has shared this fantastic piece of writing at at this place.
There is definately a lot to find out about this subject. I like all the points you made
You’re so awesome! I don’t believe I have read a single thing like that before. So great to find someone with some original thoughts on this topic. Really.. thank you for starting this up. This website is something that is needed on the internet, someone with a little originality!
You’re so awesome! I don’t believe I have read a single thing like that before. So great to find someone with some original thoughts on this topic. Really.. thank you for starting this up. This website is something that is needed on the internet, someone with a little originality!
This was beautiful Admin. Thank you for your reflections.
This is my first time pay a quick visit at here and i am really happy to read everthing at one place
Pretty! This has been a really wonderful post. Many thanks for providing these details.
Great information shared.. really enjoyed reading this post thank you author for sharing this post .. appreciated
Hello.
This post was created with XRumer 23 StrongAI.
Good luck 🙂
Как получить лицензию на недвижимость|Ключевая информация о лицензии на недвижимость|Подробное руководство по получению лицензии на недвижимость|Советы по получению лицензии на недвижимость|Разберитесь в процессе получения лицензии на недвижимость|Полезные советы по получению лицензии на недвижимость|Лицензия на недвижимость: важные аспекты|Изучите основы получения лицензии на недвижимость|Эффективные стратегии получения лицензии на недвижимость|Инструкция по получению лицензии на недвижимость|Секреты профессиональной лицензии на недвижимость|Полезные советы по получению лицензии на недвижимость|Основные шаги к успешной лицензии на недвижимость|Как стать агентом по недвижимости с лицензией: пошаговое руководство|Как получить лицензию на недвижимость легко и быстро|Разберитесь в процессе получения лицензии на недвижимость: полное руководство|Получение лицензии на недвижимость: лучшие практики и советы|Инструкция по получению лицензии на недвижимость|Ключевые моменты получения лицензии на недвижимость|Секреты успешного получения лицензии на недвижимость: что вам нужно знать|Простой путь к получению лицензии на недвижимость|Основные шаги к профессиональной лицензии на недвижимость|Инструкция по получению лицензии на недвижимость|Секреты быстрого получения лицензии на недвижимость|Три шага к профессиональной лицензии на недвижимость|Сек
How to get a real estate license in Illinois How to get a real estate license in Illinois .
I like this web blog very much, Its a really nice berth to read and find info.Blog monry