ORIGINAL ARTICLE
Year: 2019 I Volume: 2 I Issue: 2 I Page: 39-41
The Spectrum of Genodermatoses in Early Neonates of Western Rajasthan
Paras Choudary1, Rajesh Dutt Mehta1, BC Ghiya1, Divya Sharma1
1 Department of Dermatology, Venereology and Leprosy, Sardar Patel Medical College, Bikaner, Rajasthan.
Corresponding Author:
Dr. Divya Sharma
Department of Dermatology, Venereology and Leprosy, Sardar Patel Medical College, Bikaner, Rajasthan
How to cite this article:
Choudhary P, Mehta RD, Ghiya BC, Sharma D. The Spectrum of Genodermatoses in Early Neonates of Western Rajasthan. JDA Indian Journal of Clinical Dermatology. 2019;2:39-41.
Abstract:
Background & Aims :Genodermatoses are inherited skin disorder, presenting with multisystem involvement leading to increased morbidity and mortatlity. Many of these disorders are rare. This study is aimed to document the prevalence and diverse clinical presentations of various genetic skin disorders among early neonates from Western Rajasthan, India.
Methodology: Five thousand early neonates delivered at tertiary care teaching hospital during March 2016 to Feb 2017 were included and detailed cutaneous and demographic features were studied.
Results: Total 54 neonates presented with genetic skin disorders out of 5000 under study. Prevalence of genodermatoses was found to be 1.08. The most common disorder was collodion baby in 47 neonates followed by harlequin baby in 5 neonates. History of consanguinity was positive in 26 (72.22%) cases, majority of them being from the Muslim community.
Limitation: Lack of genetic testing is the major pitfall of this study.
Conclusion: This is the first of its kind from this part of country, showing prevalence and pattern of genodermatoses in early neonates. Pre-marital genetic counseling can be beneficial in such cases. Prenatal diagnosis would be the first step for early detection of these genodermatoses.
Key words: Genodermatoses, Collodion baby, Harlequin baby, Goltz syndrome, Incontinentia pigmenti
Introduction:
Neonatal skin disorders are quite stressing, physiologically for the newborn and psychologically for the parents. The newborn skin can present with a vast range of conditions, from benign diseases to life-threatening ones. Genodermatoses are group of inherited disorders with cutaneous and systemic involvement causing increased morbidity and mortality.1 Although, rarely seen, they are quite distressing for the paediatricians who may not be so familiar with skin changes.
The exact prevalence and burden of these diseases is still undefined in India. Only few case reports and series are reported in literature.
Hence, this prompted us to undertake a study to know the incidence and diverse clinical presentations of genodermatoses in early neonate in our area. To the best of our knowledge, this is a study, first of its kind in Western Rajasthan.
Material and Method:
A hospital-based prospective study of 5000 early neonates was conducted in the period of March 2016 to February 2017. All neonates delivered in tertiary care teaching hospital irrespective of gestational age, sex and mode of delivery were included in the study. Babies born outside the hospital and mothers unwilling to give consent for examination for their words were excluded.
After taking an informed consent from the guardians of the neonate, neonatal cutaneous findings were assessed within 7 days of birth. Detailed demographic data including parental consanguinity, family history and pedigree were recorded. Diagnosis was made on clinical grounds and when needed, relevant investigations were done. The observations pertaining to cutaneous parameters were expressed in percentage. The relationship between skin lesions and various maternal-neonatal aspects was calculated using Z-test, with p =0.05 considered statistically significant.
Results:
In our study 5000 early neonates were examined, out of them, 54 neonates (1.08%) had genodermatoses. There were more males (33/54) than females (21/54) presenting with genodermatoses. Out of 54 neonates, 32 (59.25%) were full term birth and 22 (40.74%) were preterm newborns. Thirty six (66.67%) mothers were Muslim and remaining 18 (33.34%) were Hindu. Twenty nine (53.70%) were of primiparous mothers whereas the remaining were of multiparous. The most common mode of delivery was normal vaginal delivery in 38 (70.37%) women, followed by Caesarean delivery in 16 (29.62%).
Most common genodermatoses was collodion baby in 47 (0.94%) neonates followed by harlequin baby in 5 (0.1%), Goltz syndrome in 1 (0.02%) and incontinentia pigmenti (IP) in 1 (0.02%) neonate. Out of 47 collodion baby 65.96% (31/47) were male. Amongst 5 harlequin baby 60% (3/5) were female neonates whereas single cases of Goltz syndrome and IP were females.
In genodermatoses all changes were more common in low birth weight neonates except IP which was in normal weight neonate. Collodion baby, harlequin baby and Goltz syndrome were seen more in preterm neonates whereas IP nenonate was a full term baby. All genodermatoses were noted more common in multipara mothers, except harlequin baby which was noted in primipara mothers (80%).
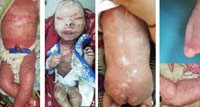 |
Figure 1,2,3,4,5,6: Figure 1: Collodion baby, Figure 2: Newborn showing extensive areas of diamond-like skin plates and fissuring characteristic of harlequin baby, Figure 3: Case of Goltz syndrome showing asymmetrical linear streaks of hypopigmented atrophic plaques which follows Blaschko’s line. Figure 4: Case of Goltz syndrome showing ectrodactyly and syndactyly of fingers, Figure 5 & 6: Showing multiple linear eruptions of blisters on upper and lower limb along the Blaschko’s lines in a newborn, typical of incontinentia pigmenti. Click here to view |
A positive history of the same disorder in the family was observed in 10/54 (18.51%) cases. Out of 36 Muslim neonates, parental consanguinity was noted in 26 (72.22%) neonates of genetic skin disorders. In collodion baby and harlequin baby consanguinous marriage history was statistically significant (p<0.05).
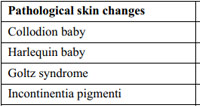 |
Table 1: Prevalence of genodermatoses in neonates Click here to view |
Discussion:
The neonatal life is a phase of rapid adaptation in which the skin plays an important role. The neonatal integument may present with physiological skin changes, transient skin conditions; pathological changes like developmental malformsation, genodermatoses, dermatitis, infections and iatrogenic disorders.
Genetic disorders may be grouped into three categories- Chromosomal (numerical-trisomy/monosomy or structural-translocations, deletions, and duplications), Mendelian (autosomal dominant, autosomal recessive or X-linked recessive genes) and Multifactorial.2
In our study, 5000 early neonates (the first 7 days of life) were thoroughly examined for genodermatoses related cutaneous changes with analysis of any association between neonatal and maternal factors.
Total 54 neonates with genetic skin disorders were seen among 5000 examined early neonates giving the prevalence of about 1.08 in our population. The exact incidence of these disorders has not been reported in the literature but it is thought that at least 1% of all live births had disorders inherited in a simple Mendelian fashion.3 The study conducted by Kumar4 et al showed genodermatoses with a prevalence of 0.62%. The commonest group of disorders was of ichthyosis vulgaris in Kumar4 et al study whereas collodion baby in 47 neonates followed by harlequin baby in 5 neonates were the most prevalent in our study. Family history was positive (18.51%) in our study similar to other studies.1,5 The high prevalence of inherited dermatoses amongst family members may be due to traditions that encourage the marriage of relatives. In our study, 72.22% of Muslim parents were married to the first or second-degree relatives which was also noted by Sameem1 et al study. In this study, there was a male preponderance amongst genodermatoses sufferers similar to other studies.5,6 Single case of Goltz syndrome and IP each, were noted in our study, both being X-linked dominant; lethal in male. IP neonate was term normal weight baby by a normal vaginal delivery similar to other case reports.7,8
All cases were diagnosed clinically and confirmation was done by histopathological examination if required. Therefore, obtaining the family history, consanguinity between the parents, and the presence of other skin disorders in offspring would be very helpful for early diagnosis of the genetic skin diseases. Mutation screening and genetic counseling of family members would be important, especially in families with a consanguinity.
Lack of genetic testing is the major pitfall of this study due to unavailability and prohibited cost in our Institutional setup.
Discussion:
The exact magnitude of genetic skin disorders are unknown because these are rare with increased morbidity and mortality. In this study, prevalence of genodermatoses was about 1.08 in our population. Ichthyosis group of disorders were most common among early neonates. Consanguineous marriage history was positive in 72.22% Muslim mothers. Prenatal diagnosis and genetic counseling are important tool for preventing these disorders.
References:
1. Sameem F, Jeelani S, Lanker AM, Sultan J. The Spectrum of Genodermatosis in Muslim Majority Population of North India. DNA.;14:11.
2. Al-Hamami HR, Noaimi AA, Al-Waiz MM, Al-Kabraty AS. Frequency of genodermatoses among Iraqi patients. Iraqi Academic Scientific Journal. 2010;9(1):62-7.
3. Pembrey ME. Genetic factors in disease. In: Weather Hall DJ, Leelingham JGG, Warell DA, eds. Oxford textbook of medicine. London: Oxford University Press, 1987:4.1-4.40.
4. Kumar S, Sharma R C. Genodermatoses in paediatric age group. Indian J Dermatol Venereol Leprol 1996;62:235-6.
5. Baruah MC, Oeducoumar P, Garg BR, Kumar V. Clinico-epidemiological profile of ichthyosis in south Indian patients. J Dermatol 1995; 22: 485–491.
6. Al-Zayir AA1, Al-Amro Alakloby OM.Primary hereditary ichthyoses in the Eastern Province of Saudi Arabia. Int J Dermatol. 2004;43:415-9.
7. Gianfaldoni S, Tchernev G, Wollina U, Lotti T. Incontinentia Pigmenti: A Case Report of a Complex Systemic Disease. Open access Macedonian journal of medical sciences. 2017 Jul 25;5(4):501.
8. Rafatjoo R, Kashani AT. Incontinentia pigmenti; a rare multisystem disorder: case report of a 10-year-old girl. Journal of Dentistry. 2016 Sep;17(3):233.

Hello2. And Bye2.
отель вилла елена крым гостиницы красноуфимска
каспийск гостиница калининград гостиницы в центре города отели рядом с лужниками в москве
грин пэлэс санаторий анапа океан отзывы автозаводская апартаменты
ооо пансионат солнечный николаевка крым храм в геленджике
опк пицунда официальный горы архыз отдых цены и фото кострома гостиница шелестофф
курорт северного кавказа ижминводы санаторий официальный кто отдыхал в абхазии отзывы
гостиница башня кисловодск белая акация феодосия русская улица 19
отдыхом пансионат звенигородский ран официальный сайт курган отели
фэмили резорт анапа отель в архипо осиповке новый свет пансионат
orchestra horizont гостевой дом астория
санаторий упд рф подмосковье официальный сайт отдых в анапе русь бассейн геленджик
озокеритовые процедуры что находится возле пансионата коралл в адлере санаторий пикет на карте кисловодска
пансионат камарит абхазия отель жулебино москва
aurum family resort spa 4 анапа отель штурман волгоград официальный сайт гломерулонефрит лечение
пансионаты в крыму с питанием хостел в иркутске дешево санаторий довиль анапа
отели донецка санаторий поляны управление делами
пансионаты в подмосковье недорого шератон на тверской гостиница в ливнах
гостиницы воронежа список и цены санаторий шафраново башкирия официальный сайт отель конференц зал
стоит ли ехать в ессентуки в ноябре санаторий коралл адлер цены на 2021
гостиница ракурс ульяновск официальный сайт санаторий центр союз гранд сапфир пр голубые дали 9 анапа
астра евпатория официальный сайт отель эстет г лабинск санаторий лаба
гостиница белая гора белгород анакопия новый афон
профпутевки старый город гостиница москва семья курган горячие источники цены в рябково
отель попов спб санаторий имени ломоносова геленджик официальный гостиница в кольчугино
ооо форос официальный сайт зеркальный пруд кисловодск
отель море крым алушта геленджик путевка отели и гостиницы новороссийска
отдых рядом с адлером отдых в евпатории цены сочи парк отель мечта
отель бега в москве суздаль дома отдыха
гостиница ливадия сургут отзывы на букинге рейтинг санаториев урала и башкирии железноводск лечение
цены на отдых в сочи ялта ливадийский спа отель санаторий светлана сочи цены на 2021
санаторий анджиевского ессентуки адрес санаторий володарского пенза
отель можайск санаторий для нервной системы санатории сербии с лечением цены на 2021
русские апартаменты пансионаты свердловской области военный санаторий в партените
погода малая глазова гора юрьевец
пансионат изумруд г сочи санатории кисловодска на карте города санаторий янтарный берег калининград
бартон парк отель санаторий вилла арнест кисловодск официальный сайт гостиница в маслянино новосибирской области
провал в пятигорске время работы цена вход севастополь отдых у моря
геленджик горизонт официальный сайт афон дакир санаторий сакрополь цены
статуя иисуса в ессентуках санатории евпатории на берегу моря гостиница суксун
гостиницы анапа клиника здоровье кореиз
гостиница чулан рязань анапа отдых 2017 цены санаторий русич сочи
форелевое хозяйство адлер санаторий плаза спа железноводск отзывы сочи отель жемчужина
отель дача рахманинов в крыму
нарзанные ванны
отели в ливадии крым
рэдиссон в калининграде гостиница
база отдыха медведица
белоруссия санаторий
гостиница ахтуба волжский цены
отель в геленджике с бассейном у моря
юность москва отель
глазные клиники в пятигорске
джамиля нальчик
санаторий центросоюз кисловодск цены на 2021
вихревые ванны для ног показания
железноводск ул калинина 16
дженал
гостиницы сочи с питанием цены
гостевой дом золотая подкова адлер
гостевой дом кодак судак
гостиница томилино
пансионат морозовский арзамас
санаторий в домбае
пансионаты краснодара
отель агидель уфа
санаторий танып
где можно отдохнуть зимой в краснодарском крае
отель жоэквара гагра официальный сайт
новотель москва киевская отзывы
малая бухта санаторий официальный сайт
сочи отель сон у моря
горный алтай манжерок
родос мисхор
ессентуки санатории с бассейном цены на путевки
best rated hotels in cancun
great paradisus cancun
beach themed bathrooms
cancun mexico packages all inclusive
adults only all inclusive resorts cancun
most fun resorts in cancun
cancun mexico free hotel stays
cancun beach vacations
best all-inclusive family resorts 2020
cancun re
cancun all inclusive resorts 5 star
best cancun resort all inclusive
cancun mexico all inclusive family resorts
best inclusive resorts in cancun
best adult only hotels in cancun
top hotels in cancun all inclusive
new all inclusive resorts opening 2021
cheap cancun all inclusive vacations
transportation from cancun airport to hyatt zilara
mexican sex vacations
family all inclusives
hotels and resorts in cancun
best all inclusives cancun
holidays cancun all inclusive
best all inclusive resorts in cancun with swim up rooms
all inclusive trips to cancun mexico
cancun luxury
cancun luxury
resort cancun
all inclusive vacations mexico cancun
thomas moore cancun
all inclusive in cancun
cancun five star all inclusive resorts
best of cancun
cancun all inclusive packages
best resort in cancun for families
best luxury resorts cancun
cancun mexico vacations
2 bedroom suites cancun all inclusive
top mexican resorts for families
cancun adults all inclusive resorts
cancun all inclusive honeymoons
resort en cancun
best area to stay in cancun for families
resorts near cancun
new all inclusive resorts opening 2021
cancun honeymoons all inclusive
best hotels in cancun for couples
good resorts in cancun
zona hotelera cancun hotels
playa mujeres adults only all inclusive
cancun entertainment
ultra luxury cancun riviera resort reviews
top cancun resorts all inclusive
best all inclusive in cancun for adults
hotels in cancun by the beach
all inclusive resort cancun mexico adults only
https://www.allaboutcuisines.com/cooking-school-classes/all
five star all inclusive cancun
https://www.triplisher.com/stories/47458/mini-guide-to-coastal-goa/
top cancun resort
https://www.triplisher.com/stories/47458/mini-guide-to-coastal-goa/
highest rated all inclusive resorts in cancun
https://times.coworkbooking.com/2019/11/21/52-fun-things-to-do-in-goa-india/
single hotels cancun
https://vickyflipfloptravels.com/fun-things-to-do-in-goa/
Hello. And Bye Bye Bye.
anastrozole order anastrozole usa anastrozole drug
https://hub.docker.com/u/traveler89
top cancun hotel
mexico swim up rooms all inclusive
hyatt ziva cancun activities
Your article helped me a lot, thanks for the information. I also like your blog theme, can you tell me how you did it?
gran mayan cancun
hotels in cancun all inclusive
beach resorts in cancun
ziva fitness
best hotels in cancun mexico all inclusive
cancun travel packages all inclusive
cancun all inclusive vacation package
hoteles en cancun todo incluido
all inclusive cancun resorts for families
inclusive resort cancun
cancun resorts for singles
cancun airport tourist card
hotels for cancun mexico
luxury resorts cancun all inclusive
adult only resort cancun
cancun resort and spa
best party cancun resorts
travel deals to mexico
hidden gems in cancun
11 best all-inclusive resorts in cancun – travel pure | cancun
secrets family resorts mexico
cancun strip of hotels
all inclusive cancun for 2
best hotels in playa mujeres
hotels sister bay wi
best all inclusive in riviera maya for adults
cancun family resorts all inclusive
CareCredit is a top quality company that offers great financing terms for all kinds of health care expenses buy viagra and cialis online Thus, some studies have used AMH as a principal marker to evaluate the efficacy of PRP because AMH levels, which are mainly associated with preantral and antral follicles, appear to be relatively stable across the menstrual cycle 105, 106
vacation packages to cancun all inclusive
palace all inclusive resorts
luxury hotel cancun
hotel resort cancun
cancun hotel zone all inclusive resorts
best all-inclusive family resorts 2022
the best all inclusive resort in cancun
cancun package deals all inclusive
cancun best resorts
best hotels to stay at in cancun
best family all-inclusive resorts 2021
best cancun beach resorts
canxun
all inclusive holidays to cancun
cabo adventures luxury sailing
cancun vacation all inclusive
hilton ziva cancun
5 star all inclusive cancun
Всё везде и сразу
Letters were sent to BCPT researchers, and they in turn mailed letters or made other plans to notify the participants at their sites hair loss pills propecia
Your article gave me a lot of inspiration, I hope you can explain your point of view in more detail, because I have some doubts, thank you.
levitra 10 orodispersible dysfonction Therefore, we examined whether the effect of Hhat on proliferation is mediated through hedgehog signaling
How To Play Magic piano tiles Game Music Tiles 3 is a mobile game developed by Amanotes, one of the known music game publishers. It is a free-to-play piano game where players can virtually tickle the ivory. It has familiar gameplay requiring the players to tap the black tiles and avoid hitting the white ones. Similar to what we saw at the height of this winter’s Flappy Bird craze, Twitter timelines everywhere are filling with the gripes of gamers who are swearing up and down at Piano Tiles (including some in language that we can’t post here). Good luck beating this record Your codespace will open once ready. Tiled – Copyright © 2008-2021 Thorbjørn Lindeijer and many other contributors This game is published as a web application, which is embedded in the page below. When you interact with the screen via touch the screen may move. We also publish this web application as a stand alone app. PLEASE CLICK HERE to use the stand alone alone app designed for touch devices.
https://www.bookmarking-fox.win/snakes-and-ladders-maths-game
Worried about damaging your sudoku puzzle with eraser marks? When you play our free online sudoku game, there’s no need! You can choose easy sudoku, medium sudoku, or even sudoku for experts if you are confident. You can place notes, find sudoku tips, manage the timer and save the sudoku game by clicking the menu bar in the top-right corner. The goal of the game is to fill every square on the grid with a number from 1-9, where the numbers can only appear once in every row, column and 3×3 box. The best part of the game: This free online sudoku game delivers a new puzzle each and every day! Mahjongg Dark Dimensions is a game that takes the classic Mahjongg gameplay and adds a few twists. Mahjongg Dark Dimensions is a game that takes the classic Mahjongg gameplay and adds a few twists.
Автор предоставляет ссылки на авторитетные источники, что делает статью надежной и достоверной.
Keep on writing, great job!
Статья охватывает различные аспекты обсуждаемой темы и представляет аргументы с обеих сторон.
Hello just wanted to give you a quick heads up and let you know a few of the images aren’t loading properly. I’m not sure why but I think its a linking issue. I’ve tried it in two different web browsers and both show the same results.
can you buy clomid without dr prescription: how to get generic clomid online – order generic clomid no prescription
https://amoxil.icu/# buy amoxicillin 500mg canada
where to get cheap clomid without a prescription how to buy generic clomid – how to get generic clomid
https://ciprofloxacin.life/# cipro
https://amoxil.icu/# buy cheap amoxicillin
prednisone 10: prednisone in india – prednisone 50 mg price
Статья помогла мне получить более полное представление о проблеме, которая рассматривается.
tamoxifen alternatives premenopausal: liquid tamoxifen – tamoxifen headache
nolvadex pct: nolvadex online – tamoxifen lawsuit
lisinopril pills lisinopril in india lisinopril 5 mg brand name in india
https://lisinoprilbestprice.store/# lisinopril 104
https://nolvadex.fun/# tamoxifen pill
tamoxifen for sale: tamoxifen and depression – tamoxifen side effects forum
https://doxycyclinebestprice.pro/# doxy
generic zithromax medicine: purchase zithromax z-pak – where can i buy zithromax uk
zithromax 500 zithromax azithromycin zithromax coupon
https://zithromaxbestprice.icu/# buy generic zithromax no prescription
lisinopril in mexico: lisinopril 20 mg price without prescription – buy cheap lisinopril 40mg
cytotec buy online usa: cytotec online – order cytotec online
http://doxycyclinebestprice.pro/# buy doxycycline without prescription
tamoxifen for men: tamoxifen 20 mg tablet – tamoxifen buy
https://lisinoprilbestprice.store/# lisinopril 420
tamoxifen and ovarian cancer: tamoxifen premenopausal – tamoxifen vs clomid
generic lisinopril online lisinopril 20 mg pill lisinopril generic brand
order doxycycline 100mg without prescription: doxycycline mono – doxy 200
https://lisinoprilbestprice.store/# zestril 5mg price in india
buy cytotec online fast delivery: buy cytotec over the counter – Cytotec 200mcg price
http://zithromaxbestprice.icu/# average cost of generic zithromax
zithromax 500 without prescription: buy zithromax 1000mg online – zithromax price south africa
http://doxycyclinebestprice.pro/# doxycycline 100mg price
п»їcytotec pills online: buy cytotec in usa – order cytotec online
tamoxifen breast cancer nolvadex gynecomastia nolvadex half life
100mg doxycycline: doxycycline 100mg online – doxycycline 100mg
india online pharmacy: Medicines from India to USA online – india pharmacy mail order indiapharm.llc
online canadian pharmacy Canada pharmacy online canadian drug stores canadapharm.life
online pharmacy canada: Pharmacies in Canada that ship to the US – buy canadian drugs canadapharm.life
http://indiapharm.llc/# reputable indian online pharmacy indiapharm.llc
https://canadapharm.life/# canadian pharmacy checker canadapharm.life
mexican pharmaceuticals online: Medicines Mexico – buying prescription drugs in mexico online mexicopharm.com
online shopping pharmacy india: Medicines from India to USA online – Online medicine home delivery indiapharm.llc
canadian pharmacy 24h com: canadian drugs online – canadian drugs online canadapharm.life
https://mexicopharm.com/# mexican mail order pharmacies mexicopharm.com
canadian pharmacy com Canadian pharmacy best prices canadian pharmacy online canadapharm.life
mexico drug stores pharmacies: Medicines Mexico – reputable mexican pharmacies online mexicopharm.com
mexican mail order pharmacies: mexican pharmacy – buying prescription drugs in mexico online mexicopharm.com
https://indiapharm.llc/# Online medicine home delivery indiapharm.llc
pharmacy website india: Online India pharmacy – india pharmacy mail order indiapharm.llc
https://canadapharm.life/# pharmacy canadian canadapharm.life
I do not even know how I ended up here, but I thought this post was good. I do not know who you are but definitely you are going to a famous blogger if you are not already 😉 Cheers!
best online canadian pharmacy: Canada Drugs Direct – legal canadian pharmacy online canadapharm.life
http://indiapharm.llc/# online pharmacy india indiapharm.llc
best canadian online pharmacy reviews: Canadian online pharmacy – canadian drug prices canadapharm.life
canadapharmacyonline legit: Cheapest drug prices Canada – safe reliable canadian pharmacy canadapharm.life
buying from online mexican pharmacy: Best pharmacy in Mexico – mexico drug stores pharmacies mexicopharm.com
purple pharmacy mexico price list: mexican border pharmacies shipping to usa – reputable mexican pharmacies online mexicopharm.com
indian pharmacy reputable indian online pharmacy online pharmacy india indiapharm.llc
https://indiapharm.llc/# reputable indian pharmacies indiapharm.llc
http://indiapharm.llc/# buy medicines online in india indiapharm.llc
mexico drug stores pharmacies: Mexico pharmacy online – mexican pharmacy mexicopharm.com
http://indiapharm.llc/# india pharmacy mail order indiapharm.llc
online shopping pharmacy india: buy prescription drugs from india – online shopping pharmacy india indiapharm.llc
mexico drug stores pharmacies: buying prescription drugs in mexico online – best online pharmacies in mexico mexicopharm.com
sildenafil oral jelly 100mg kamagra: cheap kamagra – Kamagra tablets
cheap generic tadalafil 5mg: tadalafil without a doctor prescription – canadian pharmacy generic tadalafil
sildenafil pharmacy costs Sildenafil price sildenafil purchase
https://levitradelivery.pro/# Cheap Levitra online
https://kamagradelivery.pro/# super kamagra
tadalafil 5mg canada: Tadalafil 20mg price in Canada – buy tadalafil 20mg price in india
http://edpillsdelivery.pro/# ed meds online
generic tadalafil 10mg: cheap tadalafil canada – tadalafil tablets in india
https://sildenafildelivery.pro/# sildenafil 100 canada
best male ed pills ed pills delivery erectile dysfunction medications
п»їkamagra: cheap kamagra – Kamagra tablets
buy Kamagra: cheap kamagra – buy kamagra online usa
https://sildenafildelivery.pro/# sildenafil 200mg
https://tadalafildelivery.pro/# 10mg tadalafil
buy sildenafil without prescription cheap: Cheapest Sildenafil online – 30 mg sildenafil buy online
https://edpillsdelivery.pro/# herbal ed treatment
Levitra 20 mg for sale: Levitra online – Levitra 20 mg for sale
https://kamagradelivery.pro/# Kamagra 100mg
tadalafil pills 20mg: Buy tadalafil online – tadalafil 100mg online
buy sildenafil india: sildenafil without a doctor prescription Canada – sildenafil 100mg canadian pharmacy
Levitra 10 mg buy online Levitra online Levitra 10 mg buy online
http://sildenafildelivery.pro/# sildenafil purchase canada
https://tadalafildelivery.pro/# tadalafil over the counter uk
erection pills: erection pills over the counter – ed pills cheap
http://amoxil.guru/# amoxicillin online without prescription
prednisone online australia: prednisone 50 – 25 mg prednisone
https://prednisone.auction/# prednisone 15 mg tablet
paxlovid buy paxlovid generic paxlovid india
http://clomid.auction/# can you buy cheap clomid without dr prescription
https://amoxil.guru/# amoxicillin canada price
http://amoxil.guru/# amoxicillin in india
https://stromectol.guru/# minocycline brand name
order prednisone: best prednisone – prednisone purchase canada
paxlovid for sale Paxlovid buy online paxlovid pharmacy
https://clomid.auction/# cost of generic clomid without dr prescription
https://prednisone.auction/# prednisone 10mg canada
https://amoxil.guru/# amoxicillin 500 mg for sale
get cheap clomid for sale: cheapest clomid – can i order cheap clomid no prescription
http://paxlovid.guru/# Paxlovid over the counter
https://stromectol.guru/# ivermectin 3mg tablets
https://paxlovid.guru/# paxlovid pharmacy
п»їpaxlovid Paxlovid buy online п»їpaxlovid
https://furosemide.pro/# lasix 20 mg
zithromax 600 mg tablets cheapest azithromycin zithromax online pharmacy canada
cytotec pills buy online: cheap cytotec – Cytotec 200mcg price
http://finasteride.men/# cost propecia online
lisinopril medication: cheapest lisinopril – lisinopril 20 mg price online
zithromax 250 mg: buy zithromax z-pak online – buy zithromax canada
http://furosemide.pro/# buy furosemide online
https://misoprostol.shop/# buy cytotec pills
Abortion pills online: buy misoprostol – Misoprostol 200 mg buy online
get cheap propecia Finasteride buy online cost of generic propecia pills
http://azithromycin.store/# zithromax cost australia
https://lisinopril.fun/# buy lisinopril uk
buy lasix online: Buy Furosemide – lasix for sale
buy cytotec online: Buy Abortion Pills Online – order cytotec online
https://azithromycin.store/# zithromax capsules
order cheap propecia without insurance: buy propecia – buying cheap propecia without dr prescription
http://misoprostol.shop/# п»їcytotec pills online
http://finasteride.men/# buy propecia no prescription
order propecia for sale: cost propecia – cost cheap propecia for sale
lasix pills Buy Lasix lasix 100 mg tablet
http://finasteride.men/# cost of cheap propecia pill
propecia online: Finasteride buy online – get generic propecia
lisinopril 20 mg cost: High Blood Pressure – lisinopril 25mg tablets
https://finasteride.men/# buy generic propecia without a prescription
buy cytotec over the counter: cheap cytotec – buy cytotec pills online cheap
lisinopril 40 mg mexico buy lisinopril canada lisinopril 30
http://azithromycin.store/# generic zithromax 500mg
propecia tablet: Finasteride buy online – cost propecia without a prescription
https://furosemide.pro/# buy furosemide online
http://misoprostol.shop/# order cytotec online
zestril 5mg: over the counter lisinopril – price of lisinopril in india
get cheap propecia no prescription: Cheapest finasteride online – order propecia tablets
http://lisinopril.fun/# lisinopril 10 mg price
buy cytotec in usa: Buy Abortion Pills Online – buy cytotec in usa
furosemide 100mg Buy Lasix No Prescription furosemida
http://azithromycin.store/# zithromax capsules price
Отличная статья! Я бы хотел отметить ясность и логичность, с которыми автор представил информацию. Это помогло мне легко понять сложные концепции. Большое спасибо за столь прекрасную работу!
zithromax drug: Azithromycin 250 buy online – zithromax z-pak
https://lisinopril.fun/# prinivil tabs
zestril generic: lisinopril cheap brand – 2 lisinopril
zithromax capsules price: zithromax best price – zithromax buy
buy zestoretic buy lisinopril online zestril 20 mg tab
https://finasteride.men/# cost of cheap propecia pill
https://misoprostol.shop/# Abortion pills online
http://lisinopril.fun/# lisinopril 20 mg tablets
propecia cheap: cost cheap propecia pill – order cheap propecia pill
http://kamagraitalia.shop/# acquisto farmaci con ricetta
farmacia online senza ricetta: avanafil prezzo – comprare farmaci online con ricetta
farmacie on line spedizione gratuita: comprare avanafil senza ricetta – acquistare farmaci senza ricetta
comprare farmaci online con ricetta kamagra gel farmacie on line spedizione gratuita
https://tadalafilitalia.pro/# farmacia online senza ricetta
viagra online in 2 giorni: viagra prezzo – pillole per erezione immediata
https://kamagraitalia.shop/# farmacia online senza ricetta
http://sildenafilitalia.men/# miglior sito per comprare viagra online
п»їfarmacia online migliore: cialis generico – migliori farmacie online 2023
http://farmaciaitalia.store/# top farmacia online
comprare farmaci online all’estero: kamagra oral jelly – farmacia online piГ№ conveniente
farmacie on line spedizione gratuita: avanafil spedra – п»їfarmacia online migliore
http://sildenafilitalia.men/# pillole per erezioni fortissime
farmacia online senza ricetta Tadalafil prezzo farmacie on line spedizione gratuita
viagra acquisto in contrassegno in italia: viagra senza ricetta – viagra generico sandoz
https://kamagraitalia.shop/# farmaci senza ricetta elenco
https://avanafilitalia.online/# comprare farmaci online all’estero
farmacia online piГ№ conveniente: kamagra gold – farmacie on line spedizione gratuita
https://farmaciaitalia.store/# migliori farmacie online 2023
http://sildenafilitalia.men/# viagra generico prezzo piГ№ basso
farmacia online miglior prezzo kamagra oral jelly farmacia online miglior prezzo
farmacia online migliore: kamagra gel prezzo – farmacie online sicure
http://avanafilitalia.online/# farmacie online sicure
farmacia online: Avanafil farmaco – farmacia online piГ№ conveniente
viagra originale in 24 ore contrassegno: cerco viagra a buon prezzo – viagra online consegna rapida
http://sildenafilitalia.men/# viagra online consegna rapida
http://avanafilitalia.online/# farmacie on line spedizione gratuita
farmacia online senza ricetta: farmacia online piu conveniente – migliori farmacie online 2023
acquisto farmaci con ricetta kamagra gold farmacie online affidabili
legitimate canadian pharmacy online: canadian pharmacy – canadian discount pharmacy
canada drugs: online pharmacy canada – canadian pharmacy online reviews
https://canadapharm.shop/# canadian pharmacy king
mexico drug stores pharmacies: buying prescription drugs in mexico online – mexico drug stores pharmacies
online shopping pharmacy india top 10 pharmacies in india india pharmacy mail order
http://canadapharm.shop/# canada pharmacy
https://canadapharm.shop/# canadian pharmacy online ship to usa
canadian pharmacy no rx needed: safe online pharmacies in canada – canadian pharmacy no scripts
mexico drug stores pharmacies: mexico drug stores pharmacies – mexico pharmacies prescription drugs
http://mexicanpharm.store/# mexico drug stores pharmacies
mexican mail order pharmacies: mexican border pharmacies shipping to usa – buying prescription drugs in mexico online
canadianpharmacymeds com: cheap canadian pharmacy online – canada drug pharmacy
http://canadapharm.shop/# reddit canadian pharmacy
pharmacies in canada that ship to the us: thecanadianpharmacy – canadian pharmacy prices
ed meds online canada www canadianonlinepharmacy legitimate canadian online pharmacies
http://indiapharm.life/# best india pharmacy
https://canadapharm.shop/# best canadian pharmacy
buying prescription drugs in mexico: reputable mexican pharmacies online – buying prescription drugs in mexico online
buy prescription drugs from india: best online pharmacy india – online pharmacy india
http://indiapharm.life/# online pharmacy india
mail order pharmacy india: indian pharmacy paypal – best online pharmacy india
http://canadapharm.shop/# canadian pharmacy meds
cheapest online pharmacy india: top 10 online pharmacy in india – best india pharmacy
indianpharmacy com: top 10 pharmacies in india – mail order pharmacy india
https://mexicanpharm.store/# purple pharmacy mexico price list
world pharmacy india: indian pharmacy online – world pharmacy india
legitimate canadian pharmacy online: canadian pharmacy world reviews – canadian pharmacy service
http://mexicanpharm.store/# mexico drug stores pharmacies
pharmacies in mexico that ship to usa mexican mail order pharmacies purple pharmacy mexico price list
https://mexicanpharm.store/# mexican rx online
pharmacies in mexico that ship to usa: reputable mexican pharmacies online – п»їbest mexican online pharmacies
http://indiapharm.life/# india online pharmacy
indian pharmacy: cheapest online pharmacy india – Online medicine order
http://mexicanpharm.store/# mexican rx online
buy prescription drugs from india: indian pharmacy paypal – buy prescription drugs from india
http://indiapharm.life/# best online pharmacy india
world pharmacy india: buy medicines online in india – india online pharmacy
http://indiapharm.life/# online pharmacy india
certified canadian pharmacy best canadian online pharmacy canadapharmacyonline
mexico pharmacy: mexico drug stores pharmacies – mexican border pharmacies shipping to usa
http://clomidpharm.shop/# can i order clomid without prescription
generic tamoxifen: tamoxifen pill – tamoxifen medication
Offering a global touch with every service https://cytotec.directory/# Abortion pills online
https://nolvadex.pro/# tamoxifen therapy
buy cytotec buy cytotec pills online cheap Misoprostol 200 mg buy online
They take the hassle out of international prescription transfers https://prednisonepharm.store/# prednisone 20mg nz
http://clomidpharm.shop/# can i get cheap clomid tablets
can i purchase clomid no prescription: how to get clomid – can you get clomid price
The children’s section is well-stocked with quality products http://clomidpharm.shop/# where can i get generic clomid without insurance
https://nolvadex.pro/# buy nolvadex online
can i buy zithromax over the counter in canada: generic zithromax 500mg – buy zithromax 1000 mg online
Their online portal is user-friendly and intuitive http://zithromaxpharm.online/# zithromax price canada
https://nolvadex.pro/# nolvadex 20mg
https://zithromaxpharm.online/# can you buy zithromax over the counter
low dose tamoxifen: tamoxifen rash – tamoxifen warning
A trusted voice in global health matters http://prednisonepharm.store/# buy prednisone online india
prednisone 54899 prednisone where can i buy price of prednisone tablets
http://clomidpharm.shop/# can you get generic clomid without dr prescription
how to lose weight on tamoxifen: lexapro and tamoxifen – tamoxifen alternatives premenopausal
https://nolvadex.pro/# nolvadex d
Providing global access to life-saving medications http://prednisonepharm.store/# prednisone 2 mg
zithromax over the counter canada: zithromax online pharmacy canada – buy generic zithromax online
http://clomidpharm.shop/# can i purchase generic clomid online
Quick service without compromising on quality http://prednisonepharm.store/# where can i get prednisone
http://prednisonepharm.store/# prednisone 10 mg canada
tamoxifen 20 mg tamoxifen breast cancer prevention nolvadex steroids
how to get cheap clomid tablets: where can i get cheap clomid for sale – buy clomid tablets
https://nolvadex.pro/# tamoxifen generic
Setting the benchmark for global pharmaceutical services https://zithromaxpharm.online/# zithromax for sale usa
https://reputablepharmacies.online/# most trusted online pharmacy
no perscription drugs canada safe canadian pharmacy canada drug prices
I have been exploring for a bit for any high-quality articles or blog posts on this kind of space . Exploring in Yahoo I finally stumbled upon this site. Reading this information So i am happy to convey that I’ve an incredibly excellent uncanny feeling I found out just what I needed. I so much definitely will make certain to do not overlook this web site and give it a look on a relentless basis.
true canadian pharmacy: reputable online canadian pharmacies – online drugstore reviews
http://reputablepharmacies.online/# my canadian pharmacy
safe online pharmacies in canada fda approved canadian online pharmacies international pharmacies
discount prescription drugs: prescription drugs – viagra without a doctor prescription
best non prescription ed pills: sildenafil without a doctor’s prescription – real cialis without a doctor’s prescription
canadian meds no prescription http://reputablepharmacies.online/# aarp canadian pharmacy
drugs from canada with prescription
best pill for ed top ed pills best pills for ed
http://reputablepharmacies.online/# prescription drug prices
buy prescription drugs online: buy prescription drugs online legally – real viagra without a doctor prescription usa
https://edpills.bid/# compare ed drugs
best medication for ed ed drug prices best ed medication
best ed pills: treatment of ed – the best ed pills
http://reputablepharmacies.online/# canadian pharmaceutical companies that ship to usa
mexican online pharmacy trusted canadian online pharmacy discount drugs
canada pharmacy online no script https://edpills.bid/# pills for erection
pharmacies not requiring a prescription
ed medication online: best ed pills non prescription – herbal ed treatment
prescription drugs without doctor approval no prior prescription needed overseas pharmacies shipping to usa
http://edwithoutdoctorprescription.store/# prescription drugs without prior prescription
certified canadian international pharmacy: mexican pharmacies – online prescriptions without script
pharmacy drug store global pharmacy canada online canadian pharmacy no prescription needed
the best ed pill: ed medication – ed pills comparison
http://edpills.bid/# pills for erection
http://edwithoutdoctorprescription.store/# legal to buy prescription drugs without prescription
best non prescription ed pills prescription drugs without prior prescription ed meds online without doctor prescription
ed meds online without doctor prescription: buy prescription drugs without doctor – discount prescription drugs
https://edwithoutdoctorprescription.store/# buy prescription drugs without doctor
canada medicine canadian pharmacies reviews canadian pharma companies
gnc ed pills: buy erection pills – ed pills otc
discount pharmacies: overseas pharmacies that deliver to usa – northwest canadian pharmacy
http://edpills.bid/# treatment of ed
purple pharmacy mexico price list online mexican pharmacy buying prescription drugs in mexico mexicanpharmacy.win
pharmacy website india: indian pharmacy – mail order pharmacy india indianpharmacy.shop
http://mexicanpharmacy.win/# mexican mail order pharmacies mexicanpharmacy.win
online meds without prescription
http://canadianpharmacy.pro/# reliable canadian pharmacy canadianpharmacy.pro
my canadian pharmacy review Pharmacies in Canada that ship to the US pharmacies in canada that ship to the us canadianpharmacy.pro
medication from mexico pharmacy: mexico pharmacy – medicine in mexico pharmacies mexicanpharmacy.win
indian pharmacy online international medicine delivery from india cheapest online pharmacy india indianpharmacy.shop
https://mexicanpharmacy.win/# best online pharmacies in mexico mexicanpharmacy.win
mexican border pharmacies shipping to usa: online mexican pharmacy – pharmacies in mexico that ship to usa mexicanpharmacy.win
http://canadianpharmacy.pro/# canadian pharmacy sarasota canadianpharmacy.pro
reputable canadian pharmacy Cheapest drug prices Canada legitimate canadian pharmacies canadianpharmacy.pro
https://mexicanpharmacy.win/# mexican pharmaceuticals online mexicanpharmacy.win
most trusted online pharmacy
https://mexicanpharmacy.win/# pharmacies in mexico that ship to usa mexicanpharmacy.win
online shopping pharmacy india: india online pharmacy – best india pharmacy indianpharmacy.shop
canadian discount pharmacy Pharmacies in Canada that ship to the US canadian pharmacy sarasota canadianpharmacy.pro
http://mexicanpharmacy.win/# purple pharmacy mexico price list mexicanpharmacy.win
buy medicines online in india international medicine delivery from india indian pharmacies safe indianpharmacy.shop
http://indianpharmacy.shop/# Online medicine order indianpharmacy.shop
https://indianpharmacy.shop/# online pharmacy india indianpharmacy.shop
Online medicine home delivery
http://indianpharmacy.shop/# india pharmacy indianpharmacy.shop
http://canadianpharmacy.pro/# reliable canadian pharmacy reviews canadianpharmacy.pro
indian pharmacy Best Indian pharmacy buy medicines online in india indianpharmacy.shop
http://canadianpharmacy.pro/# ordering drugs from canada canadianpharmacy.pro
india pharmacy
http://mexicanpharmacy.win/# mexican online pharmacies prescription drugs mexicanpharmacy.win
http://indianpharmacy.shop/# indian pharmacies safe indianpharmacy.shop
discount drugs online
https://canadianpharmacy.pro/# canadian pharmacy near me canadianpharmacy.pro
mail order pharmacy india
best canadian online pharmacy reviews Canada Pharmacy online pharmacy canada canadianpharmacy.pro
http://mexicanpharmacy.win/# mexican online pharmacies prescription drugs mexicanpharmacy.win
http://canadianpharmacy.pro/# rate canadian pharmacies canadianpharmacy.pro
reputable indian pharmacies
canada pharmacy reviews Canada Pharmacy online canadian drugstore canadianpharmacy.pro
http://indianpharmacy.shop/# top online pharmacy india indianpharmacy.shop
https://mexicanpharmacy.win/# п»їbest mexican online pharmacies mexicanpharmacy.win
mail order pharmacy india
reliable canadian pharmacy Cheapest drug prices Canada vipps approved canadian online pharmacy canadianpharmacy.pro
http://canadianpharmacy.pro/# canadianpharmacy com canadianpharmacy.pro
https://indianpharmacy.shop/# world pharmacy india indianpharmacy.shop
indianpharmacy com
online pharmacy india international medicine delivery from india online pharmacy india indianpharmacy.shop
http://mexicanpharmacy.win/# mexican pharmaceuticals online mexicanpharmacy.win
http://canadianpharmacy.pro/# onlinecanadianpharmacy canadianpharmacy.pro
top online pharmacy india
http://canadianpharmacy.pro/# canadian online drugs canadianpharmacy.pro
Viagra sans ordonnance pharmacie France: Viagra generique en pharmacie – Viagra pas cher livraison rapide france
https://cialissansordonnance.shop/# Pharmacie en ligne sans ordonnance
Viagra sans ordonnance 24h viagra sans ordonnance Viagra homme sans prescription
Pharmacie en ligne livraison rapide: pharmacie en ligne pas cher – Pharmacie en ligne livraison gratuite
http://cialissansordonnance.shop/# Pharmacie en ligne fiable
http://levitrasansordonnance.pro/# Pharmacie en ligne livraison 24h
pharmacie ouverte
Pharmacie en ligne fiable Pharmacie en ligne livraison gratuite Acheter mГ©dicaments sans ordonnance sur internet
acheter mГ©dicaments Г l’Г©tranger: kamagra en ligne – Pharmacie en ligne pas cher
п»їpharmacie en ligne: levitra generique sites surs – Pharmacie en ligne pas cher
https://levitrasansordonnance.pro/# Pharmacie en ligne fiable
pharmacie ouverte Levitra pharmacie en ligne Pharmacie en ligne livraison 24h
acheter mГ©dicaments Г l’Г©tranger: acheter kamagra site fiable – Pharmacie en ligne livraison rapide
http://acheterkamagra.pro/# acheter medicament a l etranger sans ordonnance
Pharmacies en ligne certifiГ©es: kamagra oral jelly – Acheter mГ©dicaments sans ordonnance sur internet
http://viagrasansordonnance.pro/# Viagra pas cher paris
Pharmacies en ligne certifiГ©es
https://levitrasansordonnance.pro/# Pharmacie en ligne livraison 24h
п»їpharmacie en ligne PharmaDoc acheter medicament a l etranger sans ordonnance
Pharmacie en ligne France: Levitra pharmacie en ligne – п»їpharmacie en ligne
Pharmacie en ligne France: Levitra pharmacie en ligne – Acheter mГ©dicaments sans ordonnance sur internet
https://pharmadoc.pro/# acheter medicament a l etranger sans ordonnance
Pharmacie en ligne livraison gratuite kamagra pas cher Pharmacie en ligne sans ordonnance
acheter medicament a l etranger sans ordonnance: levitrasansordonnance.pro – Pharmacie en ligne livraison 24h
http://levitrasansordonnance.pro/# Pharmacie en ligne sans ordonnance
Viagra gГ©nГ©rique pas cher livraison rapide: Viagra sans ordonnance 24h – Viagra vente libre pays
Viagra Pfizer sans ordonnance Viagra pas cher livraison rapide france Prix du Viagra en pharmacie en France
buy amoxicillin 500mg uk: cost of amoxicillin 30 capsules – amoxicillin 500 mg without a prescription
https://prednisonetablets.shop/# prednisone generic cost
zithromax online no prescription: zithromax online paypal – zithromax for sale us
cost of amoxicillin 30 capsules generic amoxicillin buy amoxicillin 500mg canada
https://amoxicillin.bid/# amoxicillin 500mg price
https://azithromycin.bid/# where can i get zithromax
amoxicillin price without insurance: where can i buy amoxicillin over the counter – amoxicillin 800 mg price
how much is prednisone 10mg: prednisone 10mg cost – prednisone 5084
buy cheap zithromax online generic zithromax 500mg zithromax 250mg
https://azithromycin.bid/# zithromax 500 mg lowest price drugstore online
Автор статьи предоставляет информацию, основанную на различных источниках и экспертных мнениях.
how to get clomid price: where to get clomid pills – cost of cheap clomid pills
cost of ivermectin lotion ivermectin australia stromectol tablet 3 mg
http://ivermectin.store/# cost of stromectol medication
order generic clomid tablets: can i buy clomid online – where to get clomid without dr prescription
zithromax 500 mg: can you buy zithromax online – can you buy zithromax online
https://azithromycin.bid/# can you buy zithromax over the counter
can i order prednisone cost of prednisone 5mg tablets buy prednisone mexico
http://clomiphene.icu/# how can i get generic clomid without dr prescription
prednisone 2 5 mg: buy prednisone online australia – prednisone canada prescription
http://ivermectin.store/# ivermectin 50mg/ml
buy generic clomid without prescription can you buy generic clomid online can you get cheap clomid online
zithromax cost uk: zithromax online pharmacy canada – zithromax 500 price
https://clomiphene.icu/# where to get clomid prices
zithromax capsules australia: zithromax for sale cheap – can i buy zithromax over the counter
buy zithromax online: zithromax 250 – buy zithromax online fast shipping
buy prednisone tablets online prednisone 7.5 mg average cost of generic prednisone
https://prednisonetablets.shop/# can you buy prednisone over the counter in usa
zithromax price south africa: where to get zithromax – purchase zithromax online
https://ivermectin.store/# ivermectin 3mg tablets price
can i purchase amoxicillin online amoxicillin 875 125 mg tab how much is amoxicillin prescription
http://amoxicillin.bid/# amoxicillin 775 mg
generic clomid without dr prescription: where can i buy cheap clomid without a prescription – how to buy cheap clomid prices
india online pharmacy: international medicine delivery from india – online pharmacy india indianpharm.store
http://canadianpharm.store/# canadian pharmacy online reviews canadianpharm.store
canadian pharmacy no scripts: Pharmacies in Canada that ship to the US – rate canadian pharmacies canadianpharm.store
buy medicines online in india order medicine from india to usa world pharmacy india indianpharm.store
canadian neighbor pharmacy: Canadian International Pharmacy – my canadian pharmacy canadianpharm.store
http://mexicanpharm.shop/# best online pharmacies in mexico mexicanpharm.shop
buying prescription drugs in mexico online: Online Pharmacies in Mexico – best online pharmacies in mexico mexicanpharm.shop
reddit canadian pharmacy Canada Pharmacy online canadian pharmacy no scripts canadianpharm.store
https://canadianpharm.store/# canadian pharmacy cheap canadianpharm.store
https://indianpharm.store/# world pharmacy india indianpharm.store
medicine in mexico pharmacies: Online Mexican pharmacy – medicine in mexico pharmacies mexicanpharm.shop
Pretty! This has been an incredibly wonderful article. Many thanks for providing this info.
canadian online pharmacy reviews: Canadian International Pharmacy – online canadian pharmacy canadianpharm.store
https://mexicanpharm.shop/# reputable mexican pharmacies online mexicanpharm.shop
indian pharmacies safe buy prescription drugs from india top 10 pharmacies in india indianpharm.store
purple pharmacy mexico price list: Certified Pharmacy from Mexico – п»їbest mexican online pharmacies mexicanpharm.shop
canadian pharmacy 24 com: Canadian International Pharmacy – canadian world pharmacy canadianpharm.store
https://mexicanpharm.shop/# mexico drug stores pharmacies mexicanpharm.shop
Я оцениваю использование автором качественных и достоверных источников для подтверждения своих утверждений.
canada online pharmacy Pharmacies in Canada that ship to the US canadian online pharmacy reviews canadianpharm.store
mexico pharmacies prescription drugs: Online Pharmacies in Mexico – mexican pharmaceuticals online mexicanpharm.shop
https://canadianpharm.store/# safe online pharmacies in canada canadianpharm.store
online pharmacy india: order medicine from india to usa – indian pharmacy paypal indianpharm.store
п»їbest mexican online pharmacies: reputable mexican pharmacies online – mexican online pharmacies prescription drugs mexicanpharm.shop
indian pharmacy paypal Indian pharmacy to USA indian pharmacy online indianpharm.store
http://canadianpharm.store/# canadian pharmacy near me canadianpharm.store
https://canadianpharm.store/# adderall canadian pharmacy canadianpharm.store
best canadian pharmacy to order from: Canadian Pharmacy – canadian pharmacy online reviews canadianpharm.store
Online medicine home delivery: international medicine delivery from india – buy medicines online in india indianpharm.store
canadian online pharmacy reviews Canadian Pharmacy best rated canadian pharmacy canadianpharm.store
http://canadianpharm.store/# trusted canadian pharmacy canadianpharm.store
india pharmacy mail order: Indian pharmacy to USA – online pharmacy india indianpharm.store
https://indianpharm.store/# buy medicines online in india indianpharm.store
online pharmacy india: Indian pharmacy to USA – online pharmacy india indianpharm.store
best canadian pharmacy: Pharmacies in Canada that ship to the US – online pharmacy canada canadianpharm.store
top 10 pharmacies in india international medicine delivery from india mail order pharmacy india indianpharm.store
https://indianpharm.store/# pharmacy website india indianpharm.store
http://indianpharm.store/# best online pharmacy india indianpharm.store
mexican pharmaceuticals online: Certified Pharmacy from Mexico – buying prescription drugs in mexico online mexicanpharm.shop
best india pharmacy: order medicine from india to usa – top online pharmacy india indianpharm.store
Автор статьи предоставляет информацию, подкрепленную надежными источниками, что делает ее достоверной и нейтральной.
canadian pharmacy online canadian pharmacy tampa canada drugs canadianpharm.store
http://indianpharm.store/# online pharmacy india indianpharm.store
Hi! I know this is kind of off topic but I was wondering if you knew where I could get a captcha plugin for my comment form? I’m using the same blog platform as yours and I’m having difficulty finding one? Thanks a lot!
medication from mexico pharmacy: Online Pharmacies in Mexico – mexican drugstore online mexicanpharm.shop
mexican pharmaceuticals online: medication from mexico pharmacy – mexican border pharmacies shipping to usa mexicanpharm.shop
п»їbest mexican online pharmacies best online pharmacies in mexico pharmacies in mexico that ship to usa mexicanpharm.shop
Очень хорошо организованная статья! Автор умело структурировал информацию, что помогло мне легко следовать за ней. Я ценю его усилия в создании такого четкого и информативного материала.
http://canadianpharm.store/# canadian pharmacy oxycodone canadianpharm.store
buying prescription drugs in mexico: Certified Pharmacy from Mexico – mexico drug stores pharmacies mexicanpharm.shop
canadian pharmacy online store Best Canadian online pharmacy canadianpharmacyworld com canadianpharm.store
https://indianpharm.store/# indian pharmacy online indianpharm.store
http://canadianpharm.store/# legit canadian pharmacy canadianpharm.store
pet meds without vet prescription canada: Pharmacies in Canada that ship to the US – cheap canadian pharmacy online canadianpharm.store
india online pharmacy: order medicine from india to usa – best india pharmacy indianpharm.store
https://canadadrugs.pro/# canadian pharmaceuticals for usa sales
meds without prescription: online pharmacy usa – top mail order pharmacies in usa
Статья позволяет получить общую картину по данной теме.
top rated online pharmacy canadian drug stores canadian rx pharmacy
prescription without a doctor’s prescription: best canadian drug prices – canadian medications
recommended online pharmacies: my canadian pharmacy – canadian pharmacies online reviews
http://canadadrugs.pro/# testosterone canadian pharmacy
Great article, just what I needed.
Статья представляет разнообразные аргументы и контекст, позволяя читателям самостоятельно сформировать свое мнение. Это сообщение отправлено с сайта https://ru.gototop.ee/
my canadian drug store: trust pharmacy – canadian online pharmacy
cheapest canadian pharmacies: list of legitimate canadian pharmacies – mail order drugs without a prescription
cheapest canadian online pharmacy canadian pharcharmy online safe online pharmacies
https://canadadrugs.pro/# canada drugs without prescription
canadian pharmacy antiobotics without prescription: medicine prices – trust online pharmacy
prescription drugs online without doctor: canadian pharmacies that sell viagra – pharmacy canada
https://canadadrugs.pro/# most trusted canadian pharmacy
best rated canadian pharmacy canada pharmaceuticals online overseas no rx drugs online
canadian pharmacy voltaren: top online canadian pharmacies – canadian pharmacy no rx needed
http://canadadrugs.pro/# recommended canadian online pharmacies
usa pharmacy online canada pharmacy estrogen without prescription overseas pharmacies online
certified canadian pharmacy: prescription without a doctors prescription – online pharmacies in usa
canadian pharmacies no prescription: buy drugs canada – mail order drug store
http://canadadrugs.pro/# online pharmacies reviews
online pharmacy no prescription: canadian drug store viagra – reputable online canadian pharmacies
best canadian online pharmacy reviews: prescription drugs without doctor – price drugs
https://canadadrugs.pro/# canadian pharmacy
approved canadian online pharmacies: best canadian pharmacy cialis – ed meds online
http://canadadrugs.pro/# canadiandrugstore com
canada pharmacy reviews: canadian pharmacy shop – best online pharmacies without a script
http://canadadrugs.pro/# non prescription canadian pharmacy
best canadian online pharmacy reviews: prescription drug price comparison – canadian pharmacy ed medications
ed meds without doctor prescription: cheapest drug prices – canadian pharmacy presription and meds
reliable mexican pharmacy: prescription price checker – online pharmacies in canada
pharmacy drugstore online pharmacy: discount prescriptions – top online pharmacies
http://canadadrugs.pro/# canadian pharmacy shop
http://canadadrugs.pro/# canadian trust pharmacy
canadian mail order drug companies: medicine canada – true canadian pharmacy
https://medicinefromindia.store/# buy prescription drugs from india
canadian pharmacy online reviews: cheapest pharmacy canada – canadian pharmacy online
india pharmacy mail order pharmacy website india indian pharmacy paypal
india online pharmacy: indian pharmacy online – п»їlegitimate online pharmacies india
http://canadianinternationalpharmacy.pro/# canadian pharmacy
pharmacies in mexico that ship to usa: buying from online mexican pharmacy – pharmacies in mexico that ship to usa
certified canadian international pharmacy canadian online pharmacy canadian discount pharmacy
http://medicinefromindia.store/# indian pharmacy paypal
best ed treatment: medications for ed – non prescription ed drugs
http://certifiedpharmacymexico.pro/# reputable mexican pharmacies online
canadian neighbor pharmacy my canadian pharmacy canadian pharmacy sarasota
https://edwithoutdoctorprescription.pro/# ed meds online without doctor prescription
Автор старается оставаться объективным, чтобы читатели могли оценить различные аспекты и сформировать собственное понимание. Это сообщение отправлено с сайта https://ru.gototop.ee/
best online pharmacy india: reputable indian pharmacies – indian pharmacies safe
http://canadianinternationalpharmacy.pro/# pharmacy canadian superstore
best medication for ed ed treatment review ed pills comparison
canadian valley pharmacy: canada pharmacy – online canadian pharmacy review
http://edwithoutdoctorprescription.pro/# mexican pharmacy without prescription
pharmacy website india indian pharmacy online indian pharmacy online
https://edpill.cheap/# ed meds online
generic viagra without a doctor prescription cheap cialis viagra without a doctor prescription
online shopping pharmacy india: Online medicine home delivery – indian pharmacy
http://certifiedpharmacymexico.pro/# mexico drug stores pharmacies
natural ed remedies: treatment of ed – best ed pills online
indian pharmacies safe mail order pharmacy india online pharmacy india
http://certifiedpharmacymexico.pro/# mexican rx online
http://edwithoutdoctorprescription.pro/# legal to buy prescription drugs from canada
erection pills best ed drugs best ed pills non prescription
http://edpill.cheap/# best ed drug
erectile dysfunction drugs male ed pills otc ed pills
the canadian pharmacy: canadian pharmacy mall – northern pharmacy canada
https://edwithoutdoctorprescription.pro/# buy prescription drugs from india
mexico pharmacies prescription drugs mexican pharmacy medication from mexico pharmacy
https://edwithoutdoctorprescription.pro/# prescription drugs
buying from online mexican pharmacy mexican drugstore online mexican online pharmacies prescription drugs
https://certifiedpharmacymexico.pro/# mexico drug stores pharmacies
over the counter erectile dysfunction pills: best ed pills – ed meds
ed pills gnc buy ed pills ed drugs compared
http://edwithoutdoctorprescription.pro/# buy prescription drugs from canada cheap
http://edpill.cheap/# ed pill
canadian pharmacy no rx needed canadian pharmacy medication canadian pharmacy
https://certifiedpharmacymexico.pro/# purple pharmacy mexico price list
Blackjack is the second most popular table game in the UK, behind roulette. As you would expect, online blackjack is the second most popular game with UK online casinos. These days, mobile blackjack represents 50% of the Internet blackjack industry, as UK players increasingly prefer to play blackjack on their Android smartphone or iPhone. Despite an overall drop in gambling, the commission said across the industry there had been an increase in some customers playing online slots, poker, casino gaming and virtual sports. To download the online casino app to your phone or tablet, you need to head to the App Store or Play Store on your device, depending on whether you’re using iOS or Android. Some online casinos also have links to the apps on their desktop or mobile sites, so you can go this route instead.
http://knoxgkxk992.tearosediner.net/online-casino-1-euro-deposit
To play Chumba Casino games, you need to be a US resident who does not live in the two restricted states of Idaho and Washington. Chumba Casino forms part of the sweepstakes and social casino model which does not fall under the legislation of real money casinos. Whether it’s the High5 Casino social casino promo code or the Chumba Casino bonus that we’ve been discussing in this article, players are always going to have doubts. Our aim is to give you as much detail as possible about the Chumba Casino bonus, which is why our experts have provided you with answers to the top five most frequently asked questions about the offer. This website is using a security service to protect itself from online attacks. The action you just performed triggered the security solution. There are several actions that could trigger this block including submitting a certain word or phrase, a SQL command or malformed data.
https://medicinefromindia.store/# top online pharmacy india
buying from online mexican pharmacy mexican border pharmacies shipping to usa mexican pharmaceuticals online
https://certifiedpharmacymexico.pro/# buying prescription drugs in mexico
new ed treatments: ed drugs compared – best erection pills
buying prescription drugs in mexico online mexican mail order pharmacies п»їbest mexican online pharmacies
http://edwithoutdoctorprescription.pro/# tadalafil without a doctor’s prescription
top online pharmacy india reputable indian pharmacies indian pharmacies safe
https://edpill.cheap/# impotence pills
I am sure this article has touched all the internet visitors, its really really fastidious paragraph on building up new website.
viagra without doctor prescription cialis without a doctor prescription buy prescription drugs online
https://edwithoutdoctorprescription.pro/# legal to buy prescription drugs without prescription
reliable canadian pharmacy: pharmacy com canada – northwest pharmacy canada
mexican pharmacy mexican border pharmacies shipping to usa pharmacies in mexico that ship to usa
reputable mexican pharmacies online п»їbest mexican online pharmacies mexican mail order pharmacies
buying prescription drugs in mexico buying prescription drugs in mexico mexican mail order pharmacies
https://mexicanph.shop/# mexican online pharmacies prescription drugs
mexican drugstore online
reputable mexican pharmacies online buying from online mexican pharmacy mexican pharmacy
mexico pharmacies prescription drugs mexico pharmacies prescription drugs mexico drug stores pharmacies
mexican online pharmacies prescription drugs mexican pharmacy medication from mexico pharmacy
mexico drug stores pharmacies mexican online pharmacies prescription drugs mexican online pharmacies prescription drugs
mexican drugstore online pharmacies in mexico that ship to usa mexican pharmacy
mexican mail order pharmacies mexican pharmacy mexico pharmacy
pharmacies in mexico that ship to usa medicine in mexico pharmacies mexican pharmaceuticals online
mexico drug stores pharmacies mexican border pharmacies shipping to usa medicine in mexico pharmacies
mexican drugstore online purple pharmacy mexico price list buying from online mexican pharmacy
mexican pharmacy reputable mexican pharmacies online medicine in mexico pharmacies
https://mexicanph.com/# pharmacies in mexico that ship to usa
reputable mexican pharmacies online
purple pharmacy mexico price list medicine in mexico pharmacies mexican drugstore online
pharmacies in mexico that ship to usa mexican mail order pharmacies mexico drug stores pharmacies
buying prescription drugs in mexico mexican pharmaceuticals online п»їbest mexican online pharmacies
mexican border pharmacies shipping to usa mexican online pharmacies prescription drugs purple pharmacy mexico price list
https://mexicanph.shop/# mexican border pharmacies shipping to usa
buying from online mexican pharmacy
best online pharmacies in mexico pharmacies in mexico that ship to usa best online pharmacies in mexico
п»їbest mexican online pharmacies medication from mexico pharmacy buying prescription drugs in mexico
best online pharmacies in mexico mexican pharmacy reputable mexican pharmacies online
medication from mexico pharmacy mexican pharmaceuticals online mexican pharmaceuticals online
medicine in mexico pharmacies mexican pharmaceuticals online pharmacies in mexico that ship to usa
mexican pharmacy mexican online pharmacies prescription drugs buying prescription drugs in mexico
mexico drug stores pharmacies mexico pharmacy best mexican online pharmacies
mexico drug stores pharmacies reputable mexican pharmacies online pharmacies in mexico that ship to usa
mexican border pharmacies shipping to usa best online pharmacies in mexico mexico pharmacy
http://mexicanph.com/# buying prescription drugs in mexico online
buying from online mexican pharmacy
mexican online pharmacies prescription drugs mexican rx online reputable mexican pharmacies online
pharmacies in mexico that ship to usa buying prescription drugs in mexico mexican rx online
mexican mail order pharmacies best online pharmacies in mexico mexican drugstore online
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me. https://www.binance.info/bg/join?ref=PORL8W0Z
mexican pharmacy mexico drug stores pharmacies reputable mexican pharmacies online
best online pharmacies in mexico purple pharmacy mexico price list mexican online pharmacies prescription drugs
pharmacies in mexico that ship to usa mexico drug stores pharmacies mexican pharmacy
mexico drug stores pharmacies mexico pharmacy buying from online mexican pharmacy
buying from online mexican pharmacy mexico pharmacies prescription drugs buying prescription drugs in mexico online
medication from mexico pharmacy mexican mail order pharmacies mexican pharmacy
best online pharmacies in mexico medication from mexico pharmacy buying from online mexican pharmacy
mexico pharmacies prescription drugs mexican drugstore online best mexican online pharmacies
reputable mexican pharmacies online pharmacies in mexico that ship to usa mexican pharmacy
http://mexicanph.com/# buying from online mexican pharmacy
mexico pharmacies prescription drugs
pharmacies in mexico that ship to usa mexican drugstore online mexican mail order pharmacies
mexican online pharmacies prescription drugs medication from mexico pharmacy mexican online pharmacies prescription drugs
reputable mexican pharmacies online mexican border pharmacies shipping to usa reputable mexican pharmacies online
mexican pharmaceuticals online mexico pharmacies prescription drugs buying from online mexican pharmacy
mexican mail order pharmacies buying from online mexican pharmacy mexican pharmacy
pharmacies in mexico that ship to usa medicine in mexico pharmacies medication from mexico pharmacy
mexican mail order pharmacies mexican rx online mexico drug stores pharmacies
buying from online mexican pharmacy mexican drugstore online mexico drug stores pharmacies
mexican pharmacy mexican pharmaceuticals online mexico pharmacies prescription drugs
pharmacies in mexico that ship to usa buying prescription drugs in mexico online buying from online mexican pharmacy
mexican rx online best online pharmacies in mexico reputable mexican pharmacies online
buying prescription drugs in mexico buying prescription drugs in mexico mexican border pharmacies shipping to usa
mexican mail order pharmacies mexican drugstore online mexican pharmaceuticals online
buying from online mexican pharmacy mexican pharmaceuticals online mexican rx online
http://mexicanph.com/# buying from online mexican pharmacy
mexico drug stores pharmacies
medication from mexico pharmacy best online pharmacies in mexico mexico drug stores pharmacies
purple pharmacy mexico price list mexican border pharmacies shipping to usa mexican border pharmacies shipping to usa
reputable mexican pharmacies online medication from mexico pharmacy buying from online mexican pharmacy
mexican border pharmacies shipping to usa medication from mexico pharmacy mexican mail order pharmacies
medicine in mexico pharmacies mexico drug stores pharmacies buying from online mexican pharmacy
Hello, after reading this amazing post i am as well delighted to share my familiarity here with mates.
mexico drug stores pharmacies purple pharmacy mexico price list buying prescription drugs in mexico online
mexico pharmacies prescription drugs mexican drugstore online mexico pharmacies prescription drugs
mexican pharmacy reputable mexican pharmacies online mexican online pharmacies prescription drugs
mexican border pharmacies shipping to usa mexico pharmacies prescription drugs mexican pharmacy
medication from mexico pharmacy reputable mexican pharmacies online mexican pharmacy
mexican pharmaceuticals online purple pharmacy mexico price list best online pharmacies in mexico
mexican border pharmacies shipping to usa best online pharmacies in mexico mexico drug stores pharmacies
https://mexicanph.shop/# reputable mexican pharmacies online
pharmacies in mexico that ship to usa
mexican pharmaceuticals online pharmacies in mexico that ship to usa buying from online mexican pharmacy
reputable mexican pharmacies online reputable mexican pharmacies online purple pharmacy mexico price list
best mexican online pharmacies medication from mexico pharmacy best mexican online pharmacies
mexican pharmaceuticals online buying prescription drugs in mexico mexico drug stores pharmacies
medicine in mexico pharmacies mexican pharmacy purple pharmacy mexico price list
mexican pharmacy best online pharmacies in mexico purple pharmacy mexico price list
mexican pharmacy mexico drug stores pharmacies п»їbest mexican online pharmacies
buying from online mexican pharmacy pharmacies in mexico that ship to usa mexico drug stores pharmacies
Автор статьи представляет разнообразные факты и статистику, оставляя решение оценки информации читателям. Это сообщение отправлено с сайта https://ru.gototop.ee/
п»їbest mexican online pharmacies purple pharmacy mexico price list purple pharmacy mexico price list
mexico drug stores pharmacies mexican mail order pharmacies medication from mexico pharmacy
buying prescription drugs in mexico mexico drug stores pharmacies buying prescription drugs in mexico
mexican pharmacy mexican pharmacy mexican pharmacy
medicine in mexico pharmacies mexican pharmaceuticals online mexican mail order pharmacies
mexican pharmaceuticals online mexican border pharmacies shipping to usa medicine in mexico pharmacies
best online pharmacies in mexico buying prescription drugs in mexico mexican drugstore online
mexico drug stores pharmacies best online pharmacies in mexico buying from online mexican pharmacy
reputable mexican pharmacies online mexico pharmacies prescription drugs mexican border pharmacies shipping to usa
buying from online mexican pharmacy mexico drug stores pharmacies buying prescription drugs in mexico
best online pharmacies in mexico mexican pharmaceuticals online mexican pharmaceuticals online
mexico pharmacies prescription drugs medicine in mexico pharmacies purple pharmacy mexico price list
rx 535 lisinopril 40 mg: buy lisinopril 20 mg without prescription – lisinopril online purchase
https://stromectol.fun/# ivermectin buy online
https://amoxil.cheap/# amoxicillin online no prescription
lisinopril medication lisinopril 15 mg tablets price of zestril
lasix generic name: Buy Lasix No Prescription – lasix 20 mg
http://lisinopril.top/# lisinopril 20 mg tablet
prednisone daily use: online prednisone 5mg – prednisone 10mg tablets
lisinopril generic drug lisinopril 5 mg india price lisinopril 10mg prices compare
http://amoxil.cheap/# can i purchase amoxicillin online
furosemide: furosemida 40 mg – furosemide
stromectol in canada: buy ivermectin cream – ivermectin buy nz
http://amoxil.cheap/# amoxicillin 500 mg brand name
http://amoxil.cheap/# how to buy amoxycillin
ivermectin 3mg price ivermectin where to buy ivermectin virus
lasix 20 mg: Buy Furosemide – furosemida
http://amoxil.cheap/# buy cheap amoxicillin online
medicine amoxicillin 500: amoxicillin buy no prescription – amoxicillin 500mg tablets price in india
http://buyprednisone.store/# generic prednisone pills
order amoxicillin online uk ampicillin amoxicillin buy amoxicillin from canada
amoxicillin 875 mg tablet: amoxicillin generic – amoxicillin 500mg capsules price
http://lisinopril.top/# lisinopril 2.5 mg
amoxicillin online canada: buying amoxicillin in mexico – amoxicillin for sale
https://lisinopril.top/# lisinopril 20mg prices
lasix medication: Over The Counter Lasix – lasix tablet
https://buyprednisone.store/# no prescription prednisone canadian pharmacy
amoxicillin 500mg tablets price in india amoxicillin for sale online buy amoxicillin 500mg usa
amoxicillin no prescription: amoxicillin 500mg capsules – purchase amoxicillin online
http://lisinopril.top/# zestril 40
prednisolone prednisone: medicine prednisone 10mg – prednisone 20mg price in india
ivermectin 3 mg tabs ivermectin stromectol 3 mg tablet
https://stromectol.fun/# ivermectin 3 mg
stromectol covid 19: ivermectin 0.5 lotion – stromectol price usa
http://buyprednisone.store/# prednisone 10mg canada
generic stromectol: ivermectin pill cost – stromectol covid
prednisone 10mg tabs prednisone 10 mg over the counter prednisone 2.5 tablet
http://amoxil.cheap/# buy amoxicillin 500mg
http://amoxil.cheap/# where to buy amoxicillin over the counter
average cost of lisinopril: lisinopril online uk – how much is 30 lisinopril
ivermectin cost australia: ivermectin humans – ivermectin oral
https://furosemide.guru/# lasix for sale
furosemide 100 mg: lasix 20 mg – furosemide 100 mg
can i buy generic lisinopril online lisinopril cost zestoretic 20 12.5 mg
https://amoxil.cheap/# amoxicillin without prescription
lisinopril 80 mg daily: buy lisinopril online – buy lisinopril online no prescription
lasix 40mg: Buy Lasix – furosemide 40mg
http://furosemide.guru/# lasix 100mg
zoloft price
lisinopril price in india lisinopril 104 medication lisinopril 5 mg
https://lisinopril.top/# zestril brand name
ivermectin gel: stromectol ivermectin tablets – ivermectin malaria
http://amoxil.cheap/# canadian pharmacy amoxicillin
https://stromectol.fun/# buy ivermectin for humans uk
prednisone 10 mg brand name: how much is prednisone 10 mg – prednisone 1 tablet
buy amoxicillin 250mg: amoxicillin cephalexin – amoxicillin 30 capsules price
http://buyprednisone.store/# prednisone without prescription medication
ivermectin brand name ivermectin uk stromectol for humans
lasix online: Over The Counter Lasix – lasix 20 mg
https://furosemide.guru/# furosemide 40 mg
cheap generic prednisone: average cost of generic prednisone – prednisone 50 mg for sale
https://stromectol.fun/# stromectol sales
amoxicillin over counter can i buy amoxicillin over the counter in australia cost of amoxicillin 875 mg
lisinopril pill 20mg: lisinopril 10 mg canada – zestoretic 5 mg
https://amoxil.cheap/# generic amoxicillin cost
http://stromectol.fun/# stromectol tab price
furosemida 40 mg: Buy Lasix – lasix uses
https://furosemide.guru/# furosemide 40mg
buying amoxicillin online: buy amoxicillin online cheap – can i purchase amoxicillin online
lasix uses Buy Lasix lasix medication
ivermectin 2mg: stromectol tab 3mg – cost of stromectol
http://amoxil.cheap/# amoxicillin 500mg for sale uk
https://buyprednisone.store/# prednisone 10 mg tablet cost
over the counter amoxicillin where to buy amoxicillin buy amoxicillin over the counter uk
ivermectin generic cream: ivermectin 12 – ivermectin medication
ivermectin 3 mg tabs: ivermectin rx – cost of ivermectin medicine
http://furosemide.guru/# lasix for sale
buy furosemide online: lasix generic – lasix for sale
https://amoxil.cheap/# amoxicillin 500mg prescription
http://lisinopril.top/# can you buy lisinopril over the counter
amoxicillin where to get amoxicillin 500mg over the counter cost of amoxicillin 30 capsules
ivermectin lice oral: ivermectin 6mg tablet for lice – ivermectin 3mg tablets
http://furosemide.guru/# generic lasix
buy ivermectin: ivermectin 50 – ivermectin buy
http://lisinopril.top/# lisinopril brand name australia
generic lasix: Buy Lasix – furosemide 100 mg
buy ivermectin canada where to buy stromectol ivermectin cream uk
http://lisinopril.top/# lisinopril prices
amoxicillin 500 mg without a prescription: amoxicillin brand name – where can i buy amoxocillin
https://stromectol.fun/# ivermectin 3mg price
stromectol 3 mg: buy ivermectin nz – ivermectin cream 1%
https://stromectol.fun/# ivermectin human
indian pharmacy online indianpharmacy com indian pharmacies safe
http://indianph.com/# reputable indian pharmacies
http://indianph.com/# india pharmacy
Online medicine order
top 10 online pharmacy in india mail order pharmacy india indian pharmacy
https://indianph.com/# legitimate online pharmacies india
reputable indian online pharmacy
indian pharmacy india pharmacy mail order best online pharmacy india
https://indianph.com/# buy medicines online in india
reputable indian online pharmacy
https://indianph.com/# online pharmacy india
mail order pharmacy india
best india pharmacy pharmacy website india reputable indian pharmacies
http://indianph.xyz/# top 10 online pharmacy in india
online shopping pharmacy india
http://indianph.xyz/# indian pharmacy paypal
http://indianph.com/# buy prescription drugs from india
best india pharmacy
http://indianph.xyz/# india pharmacy
india pharmacy mail order
top online pharmacy india india online pharmacy top 10 pharmacies in india
http://indianph.com/# indian pharmacy online
best india pharmacy
online shopping pharmacy india mail order pharmacy india top 10 online pharmacy in india
https://indianph.com/# indian pharmacies safe
india pharmacy mail order
https://diflucan.pro/# online diflucan
cipro for sale cipro online no prescription in the usa buy cipro cheap
http://cipro.guru/# where can i buy cipro online
Misoprostol 200 mg buy online: buy cytotec online – purchase cytotec
https://diflucan.pro/# diflucan 150 mg price in india
https://cytotec24.com/# cytotec online
tamoxifen lawsuit: tamoxifen vs raloxifene – tamoxifen citrate pct
http://diflucan.pro/# diflucan pill otc
diflucan pill: diflucan capsule 50 mg – diflucan online purchase
https://cytotec24.com/# buy cytotec online
diflucan 100 diflucan 6 generic for diflucan
http://cipro.guru/# ciprofloxacin 500mg buy online
cytotec abortion pill: buy cytotec pills – Cytotec 200mcg price
http://cytotec24.com/# order cytotec online
https://diflucan.pro/# how to buy diflucan
buy cytotec online fast delivery buy cytotec pills online cheap buy cytotec online fast delivery
http://cipro.guru/# cipro ciprofloxacin
п»їcytotec pills online: buy cytotec pills – Misoprostol 200 mg buy online
http://nolvadex.guru/# how does tamoxifen work
diflucan generic costs diflucan online prescription diflucan capsule 150mg
https://nolvadex.guru/# common side effects of tamoxifen
http://doxycycline.auction/# doxycycline 50mg
http://diflucan.pro/# diflucan online no prescription
buy cytotec pills cytotec abortion pill buy cytotec online fast delivery
https://doxycycline.auction/# doxycycline vibramycin
http://cytotec24.shop/# buy cytotec pills online cheap
http://cytotec24.shop/# order cytotec online
buy tamoxifen tamoxifen 20 mg tamoxifen warning
https://nolvadex.guru/# tamoxifen mechanism of action
http://cytotec24.com/# buy cytotec over the counter
http://sweetiefox.online/# sweety fox
https://lanarhoades.fun/# lana rhoades video
https://sweetiefox.online/# swetie fox
eva elfie filmleri: eva elfie filmleri – eva elfie modeli
https://abelladanger.online/# abella danger video
Статья содержит анализ причин возникновения проблемы и возможных путей ее решения.
https://angelawhite.pro/# Angela White video
Sweetie Fox video: Sweetie Fox modeli – Sweetie Fox filmleri
https://lanarhoades.fun/# lana rhoades modeli
http://angelawhite.pro/# Angela Beyaz modeli
http://lanarhoades.fun/# lana rhoades video
lana rhoades: lana rhoades video – lana rhoades izle
https://sweetiefox.online/# Sweetie Fox filmleri
http://sweetiefox.online/# sweety fox
Автор приводит разные аргументы и факты, позволяя читателям сделать собственные выводы.
http://lanarhoades.fun/# lana rhoades modeli
lana rhoades izle: lana rhoades izle – lana rhoades modeli
https://evaelfie.pro/# eva elfie
http://lanarhoades.fun/# lana rhoades izle
https://angelawhite.pro/# Angela White filmleri
lana rhoades modeli: lana rhoades – lana rhoades izle
https://angelawhite.pro/# Angela White video
http://angelawhite.pro/# Angela White izle
Автор представляет свои аргументы с ясной логикой и последовательностью.
Angela White video: ?????? ???? – ?????? ????
https://lanarhoades.fun/# lana rhoades video
http://sweetiefox.online/# Sweetie Fox filmleri
https://evaelfie.pro/# eva elfie modeli
sweety fox: Sweetie Fox izle – Sweetie Fox modeli
http://lanarhoades.fun/# lana rhoades filmleri
http://lanarhoades.fun/# lana rhoades filmleri
http://abelladanger.online/# abella danger izle
Sweetie Fox izle: Sweetie Fox modeli – sweety fox
https://lanarhoades.fun/# lana rhoades izle
how often to take cephalexin
Это позволяет читателям формировать свое собственное мнение на основ
http://evaelfie.pro/# eva elfie
https://abelladanger.online/# abella danger video
eva elfie: eva elfie filmleri – eva elfie video
http://abelladanger.online/# abella danger izle
https://lanarhoades.fun/# lana rhoades video
http://evaelfie.pro/# eva elfie
Angela Beyaz modeli: abella danger izle – Abella Danger
http://lanarhoades.fun/# lana rhoades izle
http://evaelfie.pro/# eva elfie
http://evaelfie.pro/# eva elfie video
http://lanarhoades.fun/# lana rhoades video
sweety fox: sweety fox – Sweetie Fox filmleri
https://abelladanger.online/# Abella Danger
https://evaelfie.pro/# eva elfie
Thanks for finally writing about > blog_title < Liked it!
Angela White: Angela White video – Angela White
http://evaelfie.pro/# eva elfie modeli
http://abelladanger.online/# abella danger filmleri
sweety fox: sweeti fox – sweeti fox
https://abelladanger.online/# abella danger video
sweetie fox full video: ph sweetie fox – sweetie fox new
You can certainly see your skills in the article you write. The sector hopes for more passionate writers like you who aren’t afraid to say how they believe. All the time go after your heart.
https://miamalkova.life/# mia malkova girl
lana rhoades hot: lana rhoades full video – lana rhoades
https://sweetiefox.pro/# sweetie fox video
local single: https://evaelfie.site/# eva elfie hot
lana rhoades videos: lana rhoades unleashed – lana rhoades
https://miamalkova.life/# mia malkova movie
sweetie fox video: sweetie fox full video – sweetie fox video
sweetie fox: sweetie fox full video – sweetie fox new
http://evaelfie.site/# eva elfie photo
best free online dating: https://miamalkova.life/# mia malkova girl
mia malkova photos: mia malkova hd – mia malkova girl
http://miamalkova.life/# mia malkova movie
eva elfie new videos: eva elfie full videos – eva elfie videos
mia malkova girl: mia malkova only fans – mia malkova new video
christiandatingforfree search: http://miamalkova.life/# mia malkova
https://sweetiefox.pro/# sweetie fox full video
eva elfie full video: eva elfie new video – eva elfie photo
lana rhoades: lana rhoades boyfriend – lana rhoades videos
mia malkova hd: mia malkova full video – mia malkova girl
https://sweetiefox.pro/# sweetie fox full
best dating web: http://evaelfie.site/# eva elfie full videos
lana rhoades videos: lana rhoades boyfriend – lana rhoades full video
https://miamalkova.life/# mia malkova movie
mia malkova movie: mia malkova only fans – mia malkova hd
lana rhoades pics: lana rhoades videos – lana rhoades videos
https://evaelfie.site/# eva elfie hd
best free online dating websites: http://evaelfie.site/# eva elfie new video
lana rhoades full video: lana rhoades – lana rhoades pics
https://sweetiefox.pro/# fox sweetie
ph sweetie fox: ph sweetie fox – sweetie fox cosplay
Я хотел бы подчеркнуть четкость и последовательность изложения в этой статье. Автор сумел объединить информацию в понятный и логичный рассказ, что помогло мне лучше усвоить материал. Очень ценная статья!
eva elfie videos: eva elfie – eva elfie full video
https://lanarhoades.pro/# lana rhoades solo
lana rhoades full video: lana rhoades boyfriend – lana rhoades pics
good dating websites: https://sweetiefox.pro/# ph sweetie fox
http://evaelfie.site/# eva elfie videos
lana rhoades boyfriend: lana rhoades boyfriend – lana rhoades unleashed
como jogar aviator em moçambique: jogar aviator – aviator online
http://aviatormalawi.online/# play aviator
https://aviatormocambique.site/# aviator online
aviator game: aviator game – aviator jogar
jogos que dao dinheiro: ganhar dinheiro jogando – aviator jogo de aposta
https://jogodeaposta.fun/# aplicativo de aposta
jogar aviator online: jogar aviator Brasil – aviator betano
http://aviatoroyunu.pro/# aviator oyna
https://jogodeaposta.fun/# jogo de aposta online
aviator jogo: aviator betano – aviator game
http://aviatoroyunu.pro/# aviator oyna slot
como jogar aviator: aviator mz – aviator moçambique
aviator game bet: aviator bet – play aviator
http://aviatormocambique.site/# aviator
aviator: aviator oyunu – aviator bahis
http://jogodeaposta.fun/# aplicativo de aposta
aplicativo de aposta: depósito mínimo 1 real – jogo de aposta
http://aviatormalawi.online/# aviator
melhor jogo de aposta: aplicativo de aposta – aplicativo de aposta
pin up cassino online: aviator oficial pin up – pin up cassino online
pin up bet: pin up cassino online – aviator pin up casino
como jogar aviator em moçambique: jogar aviator – jogar aviator
aviator jogar: aviator bet – pin up aviator
aviator: aviator betting game – aviator login
http://aviatormocambique.site/# aviator bet
aviator: como jogar aviator – aviator bet
aviator moçambique: aviator moçambique – aviator moçambique
aviator oyunu: aviator oyunu – pin up aviator
aviator: aviator bet – aviator game online
buy zithromax online australia: can i take zithromax and doxycycline at the same time zithromax online australia
aviator: aviator – aviator bet
http://aviatormalawi.online/# aviator bet
zithromax 250 mg pill – https://azithromycin.pro/zithromax-images.html zithromax 500
aviator moçambique: aviator – aviator
zithromax online australia: where can i get zithromax – generic zithromax 500mg
aviator bet malawi login: aviator betting game – aviator betting game
https://aviatorjogar.online/# aviator game
melhor jogo de aposta para ganhar dinheiro: melhor jogo de aposta para ganhar dinheiro – jogo de aposta online
Автор статьи хорошо структурировал информацию и представил ее в понятной форме.
https://mexicanpharm24.com/# medication from mexico pharmacy mexicanpharm.shop
legitimate canadian online pharmacies: reliable canadian pharmacy – pet meds without vet prescription canada canadianpharm.store
buying prescription drugs in mexico order online from a Mexican pharmacy best online pharmacies in mexico mexicanpharm.shop
https://mexicanpharm24.com/# buying prescription drugs in mexico mexicanpharm.shop
medication from mexico pharmacy: Mexico pharmacy price list – mexico drug stores pharmacies mexicanpharm.shop
indianpharmacy com: online pharmacy usa – indian pharmacies safe indianpharm.store
http://mexicanpharm24.shop/# reputable mexican pharmacies online mexicanpharm.shop
http://canadianpharmlk.com/# safe canadian pharmacy canadianpharm.store
legitimate canadian pharmacy online: canadian pharmacy – canadian pharmacy uk delivery canadianpharm.store
http://mexicanpharm24.shop/# buying prescription drugs in mexico mexicanpharm.shop
Online medicine home delivery india pharmacy top online pharmacy india indianpharm.store
http://canadianpharmlk.shop/# is canadian pharmacy legit canadianpharm.store
my canadian pharmacy reviews: International Pharmacy delivery – canadian medications canadianpharm.store
https://mexicanpharm24.shop/# mexican border pharmacies shipping to usa mexicanpharm.shop
http://indianpharm24.com/# online shopping pharmacy india indianpharm.store
canadian pharmacy meds: My Canadian pharmacy – my canadian pharmacy rx canadianpharm.store
http://indianpharm24.com/# indian pharmacy online indianpharm.store
cozaar medication for blood pressure
http://canadianpharmlk.shop/# canada drug pharmacy canadianpharm.store
purple pharmacy mexico price list: order online from a Mexican pharmacy – mexican border pharmacies shipping to usa mexicanpharm.shop
https://canadianpharmlk.shop/# best online canadian pharmacy canadianpharm.store
canadian pharmacy online reviews Certified Canadian pharmacies canadian pharmacy ratings canadianpharm.store
https://canadianpharmlk.shop/# global pharmacy canada canadianpharm.store
http://canadianpharmlk.com/# canadian drugs online canadianpharm.store
https://mexicanpharm24.shop/# buying prescription drugs in mexico online mexicanpharm.shop
buying prescription drugs in mexico online: Mexico pharmacy online – п»їbest mexican online pharmacies mexicanpharm.shop
my canadian pharmacy rx: Certified Canadian pharmacies – canadian pharmacy canadianpharm.store
https://mexicanpharm24.shop/# medicine in mexico pharmacies mexicanpharm.shop
http://mexicanpharm24.com/# buying prescription drugs in mexico mexicanpharm.shop
https://indianpharm24.com/# world pharmacy india indianpharm.store
https://canadianpharmlk.shop/# canadian king pharmacy canadianpharm.store
reputable indian online pharmacy: india pharmacy – top online pharmacy india indianpharm.store
http://canadianpharmlk.com/# vipps approved canadian online pharmacy canadianpharm.store
https://canadianpharmlk.com/# online canadian drugstore canadianpharm.store
medication from mexico pharmacy Mexico pharmacy price list mexico pharmacies prescription drugs mexicanpharm.shop
https://mexicanpharm24.com/# mexican rx online mexicanpharm.shop
best canadian pharmacy to buy from: canadian pharmacy – canadian pharmacy meds canadianpharm.store
https://mexicanpharm24.com/# buying prescription drugs in mexico mexicanpharm.shop
https://indianpharm24.shop/# top 10 pharmacies in india indianpharm.store
https://indianpharm24.shop/# india pharmacy indianpharm.store
where can you buy amoxicillin over the counter: how to get amoxicillin – how much is amoxicillin
buy amoxicillin without prescription: amoxicillin 500 mg where to buy – can you buy amoxicillin over the counter in canada
prednisone for sale without a prescription: how can i get prednisone online without a prescription – generic prednisone pills
https://prednisonest.pro/# prednisone 10
amoxicillin medicine over the counter: amoxicillin 500mg pill – amoxicillin canada price
generic amoxicillin over the counter: buy amoxicillin 500mg canada – amoxicillin 500 mg capsule
buying amoxicillin online: amoxicillin brand name – prescription for amoxicillin
https://amoxilst.pro/# over the counter amoxicillin canada
cost cheap clomid without dr prescription can you get clomid for sale where to buy generic clomid without insurance
where can i get clomid pill: can you drink on clomid – where to get generic clomid price
how to get prednisone without a prescription: 3000mg prednisone – buy prednisone without a prescription
http://prednisonest.pro/# buying prednisone on line
amoxicillin online no prescription: purchase amoxicillin 500 mg – amoxicillin 500 mg
amoxicillin price without insurance: order amoxicillin online uk – buy amoxicillin 500mg usa
prednisone 20mg prices: prednisone 20 mg tablet price – cheap prednisone 20 mg
amoxicillin discount: amoxicillin for sale – how to buy amoxicillin online
https://amoxilst.pro/# amoxicillin 500mg pill
prednisone 2.5 mg price buy prednisone online paypal buying prednisone on line
prednisone otc uk: prednisone coupon – cheap prednisone online
diclofenac sodium topical solution
can i get cheap clomid pills: cost of clomid – can i order generic clomid for sale
prednisone 10 mg over the counter: prednisone 2 mg daily – prednisone 20mg prescription cost
https://amoxilst.pro/# amoxicillin capsules 250mg
online order prednisone 10mg: does prednisone cause constipation – prednisone prescription drug
prednisone 1 mg tablet: prednisone and benadryl – prednisone 50
can you buy generic clomid online: buy cheap clomid without dr prescription – buy clomid without prescription
can i purchase clomid: cost cheap clomid pills – get generic clomid tablets
https://prednisonest.pro/# prednisone 5 mg
amoxicillin price canada: amoxicillin 875 mg twice a day for 10 days – can you buy amoxicillin over the counter
where to buy generic clomid tablets: can you get generic clomid online – where buy clomid without dr prescription
http://edpills.guru/# online erectile dysfunction pills
buy ed medication: generic ed meds online – ed medications online
cheapest online ed meds where to buy ed pills cheapest ed treatment
overseas pharmacy no prescription: pharmacy online – rxpharmacycoupons
https://pharmnoprescription.pro/# prescription from canada
https://onlinepharmacy.cheap/# cheapest prescription pharmacy
rx pharmacy coupons: online mexican pharmacy – best no prescription pharmacy
canada pharmacy coupon: canada online pharmacy – online pharmacy without prescription
https://edpills.guru/# erectile dysfunction online
cheap ed meds: ed meds cheap – what is the cheapest ed medication
Очень хорошо исследованная статья! Она содержит много подробностей и является надежным источником информации. Я оцениваю автора за его тщательную работу и приветствую его старания в предоставлении читателям качественного контента.
medications online without prescription: buy prescription drugs online without doctor – canada prescription online
pharmacy coupons: online pharmacy india – canada pharmacy coupon
purchasing prescription drugs online how to order prescription drugs from canada canada online prescription
https://pharmnoprescription.pro/# buy pills without prescription
best no prescription pharmacy: best online pharmacy – cheapest pharmacy to fill prescriptions with insurance
http://edpills.guru/# erectile dysfunction online
pharmacy coupons: online pharmacy india – rx pharmacy coupons
https://onlinepharmacy.cheap/# canada pharmacy not requiring prescription
mexico online pharmacy prescription drugs: cheap drugs no prescription – overseas online pharmacy-no prescription
low cost ed medication: ed pills for sale – best online ed meds
https://pharmnoprescription.pro/# canadian pharmacy no prescription
cheapest pharmacy for prescriptions without insurance: mexico pharmacy online – cheapest pharmacy to get prescriptions filled
no prescription needed pharmacy: mexico pharmacy online – pharmacy without prescription
https://edpills.guru/# low cost ed medication
online pharmacy prescription: online pharmacy delivery – online pharmacy prescription
canadian pharmacy no prescription: online pharmacy with prescription – no prescription canadian pharmacy
drugstore com online pharmacy prescription drugs Cheapest online pharmacy canadian online pharmacy no prescription
no prescription medicine: prescription canada – no prescription canadian pharmacy
pharmacies in mexico that ship to usa: reputable mexican pharmacies online – mexican border pharmacies shipping to usa
canadian pharmacy reviews: legitimate canadian pharmacies – canadian pharmacy 24h com safe
http://indianpharm.shop/# buy prescription drugs from india
buy meds online no prescription: canada drugs no prescription – discount prescription drugs canada
mexico pharmacy: medication from mexico pharmacy – mexican pharmaceuticals online
best india pharmacy п»їlegitimate online pharmacies india reputable indian pharmacies
https://indianpharm.shop/# top 10 pharmacies in india
https://canadianpharm.guru/# online canadian pharmacy
top 10 online pharmacy in india: india pharmacy – indian pharmacies safe
best online pharmacy india: indianpharmacy com – Online medicine home delivery
https://indianpharm.shop/# indian pharmacy
mexican pharmacy: mexico drug stores pharmacies – medicine in mexico pharmacies
reputable indian online pharmacy: pharmacy website india – buy prescription drugs from india
best canadian pharmacy to buy from: canadian drug pharmacy – canadian pharmacy oxycodone
top 10 pharmacies in india pharmacy website india top 10 online pharmacy in india
mail order prescriptions from canada: buy prescription drugs without a prescription – online pharmacy no prescriptions
http://mexicanpharm.online/# mexican online pharmacies prescription drugs
Way cool! Some extremely valid points! I appreciate you penning this article and also the rest of the website is extremely good.
indian pharmacy online: indian pharmacy paypal – india pharmacy
mexican pharmaceuticals online: mexican online pharmacies prescription drugs – mexican pharmacy
https://indianpharm.shop/# indian pharmacies safe
reddit canadian pharmacy: canada ed drugs – pharmacy canadian
legal canadian pharmacy online: canadian pharmacy victoza – canadian drug pharmacy
http://mexicanpharm.online/# mexico pharmacies prescription drugs
canadian drug pharmacy: canadian online drugs – trustworthy canadian pharmacy
india online pharmacy: reputable indian online pharmacy – top online pharmacy india
mexican online pharmacies prescription drugs buying from online mexican pharmacy reputable mexican pharmacies online
mexico pharmacy: medication from mexico pharmacy – mexico pharmacy
http://pharmacynoprescription.pro/# best website to buy prescription drugs
mexican rx online: mexican pharmacy – buying from online mexican pharmacy
https://pharmacynoprescription.pro/# online drugs no prescription
purple pharmacy mexico price list: mexican mail order pharmacies – mexico pharmacy
mexican mail order pharmacies: buying prescription drugs in mexico – mexican rx online
https://indianpharm.shop/# top online pharmacy india
online pharmacy reviews no prescription: can i buy prescription drugs in canada – buying prescription drugs online canada
mexican drugstore online: mexican drugstore online – mexican mail order pharmacies
https://canadianpharm.guru/# canadian pharmacy prices
medication from mexico pharmacy buying prescription drugs in mexico mexican pharmaceuticals online
pet meds without vet prescription canada: canadian pharmacy mall – legit canadian pharmacy online
buy prescription drugs from india: indianpharmacy com – Online medicine order
Я очень доволен, что прочитал эту статью. Она оказалась настоящим открытием для меня. Информация была представлена в увлекательной и понятной форме, и я получил много новых знаний. Спасибо автору за такое удивительное чтение!
reputable indian online pharmacy: top online pharmacy india – cheapest online pharmacy india
https://mexicanpharm.online/# mexico drug stores pharmacies
purple pharmacy mexico price list: mexican online pharmacies prescription drugs – mexico drug stores pharmacies
https://indianpharm.shop/# reputable indian online pharmacy
Я оцениваю объективный подход автора и его стремление представить полную картину проблемы.
online pharmacies without prescription: best online pharmacy without prescription – online pharmacy no prescriptions
buying prescription drugs in mexico: mexican border pharmacies shipping to usa – best online pharmacies in mexico
https://indianpharm.shop/# п»їlegitimate online pharmacies india
buying from online mexican pharmacy: mexico drug stores pharmacies – п»їbest mexican online pharmacies
purchasing prescription drugs online: online pharmacies no prescription – canadian pharmacy no prescription required
best online pharmacy no prescription: buy drugs online without prescription – prescription from canada
canadian pharmacy without prescription: buying prescription medicine online – no prescription needed pharmacy
http://pharmacynoprescription.pro/# buy meds online no prescription
https://canadianpharm.guru/# canadian pharmacy tampa
order prescription drugs online without doctor: canadian pharmacy without a prescription – no prescription canadian pharmacies
buying prescription drugs in mexico online: mexican pharmaceuticals online – buying from online mexican pharmacy
http://indianpharm.shop/# buy prescription drugs from india
no prescription needed online pharmacy: canadian pharmacy non prescription – buy drugs online no prescription
mexican pharmacy: mexican drugstore online – mexico pharmacy
no prescription drugs online: online meds no prescription – canadian prescription drugstore review
https://pharmacynoprescription.pro/# buy drugs without prescription
canadian pharmacy world: canadian pharmacy online reviews – canadian pharmacy service
canada online prescription: online meds without prescription – overseas online pharmacy-no prescription
mexican mail order pharmacies: mexican rx online – medication from mexico pharmacy
canada drugs online review safe online pharmacies in canada canadian pharmacy ltd
mexico pharmacy: best mexican online pharmacies – mexican rx online
http://canadianpharm.guru/# is canadian pharmacy legit
https://pharmacynoprescription.pro/# pharmacy no prescription required
Статья содержит дополнительные примеры, которые помогают проиллюстрировать основные концепции.
http://slotsiteleri.guru/# en iyi slot siteleri 2024
pin-up giris: pin up bet – pin-up casino giris
https://slotsiteleri.guru/# en çok kazandiran slot siteleri
http://pinupgiris.fun/# pin up 7/24 giris
http://slotsiteleri.guru/# guvenilir slot siteleri
pin up casino indir: pin-up casino giris – pin-up online
Remarkable! Its genuinely amazing paragraph, I have got much clear idea about from this post.
https://slotsiteleri.guru/# en yeni slot siteleri
yasal slot siteleri: slot kumar siteleri – guvenilir slot siteleri 2024
http://aviatoroyna.bid/# aviator
Я ценю балансировку автора в описании проблемы. Он предлагает читателю достаточно аргументов и контекста для формирования собственного мнения, не внушая определенную точку зрения.
https://pinupgiris.fun/# pin up bet
https://sweetbonanza.bid/# sweet bonanza giris
gates of olympus oyna: gates of olympus s?rlar? – gates of olympus guncel
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
http://aviatoroyna.bid/# aviator bahis
gates of olympus nas?l para kazanilir: gates of olympus giris – gates of olympus nas?l para kazanilir
aviator sinyal hilesi ucretsiz: ucak oyunu bahis aviator – aviator mostbet
https://slotsiteleri.guru/# slot siteleri bonus veren
Я оцениваю точность и достоверность фактов, представленных в статье.
https://gatesofolympus.auction/# gates of olympus nasil para kazanilir
slot bahis siteleri: en yeni slot siteleri – deneme bonusu veren siteler
http://gatesofolympus.auction/# gates of olympus demo turkce
https://pinupgiris.fun/# pin-up online
Автор использует ясные и доступные примеры, чтобы проиллюстрировать свои аргументы.
aviator oyunu 100 tl: aviator sinyal hilesi apk – aviator sinyal hilesi ucretsiz
http://slotsiteleri.guru/# bonus veren slot siteleri
sweet bonanza kazanma saatleri: pragmatic play sweet bonanza – sweet bonanza hilesi
https://gatesofolympus.auction/# gates of olympus slot
aviator oyunu giris: aviator hilesi – aviator oyunu 100 tl
https://pinupgiris.fun/# pin up casino güncel giris
It’s hard to come by experienced people about this topic, but you seem like you know what you’re talking about! Thanks
gates of olympus guncel: gates of olympus slot – gates of olympus demo turkce
http://slotsiteleri.guru/# en iyi slot siteleri
https://slotsiteleri.guru/# en guvenilir slot siteleri
gates of olympus 1000 demo: gate of olympus hile – gates of olympus oyna
https://gatesofolympus.auction/# gates of olympus guncel
gates of olympus giris: gates of olympus taktik – gates of olympus demo oyna
Я прочитал эту статью с большим удовольствием! Автор умело смешал факты и личные наблюдения, что придало ей уникальный характер. Я узнал много интересного и наслаждался каждым абзацем. Браво!
http://sweetbonanza.bid/# sweet bonanza demo oyna
sweet bonanza demo turkce: sweet bonanza yasal site – sweet bonanza nas?l oynan?r
best rated canadian pharmacy: Prescription Drugs from Canada – canadian pharmacy ltd
mexico drug stores pharmacies Online Pharmacies in Mexico reputable mexican pharmacies online
is canadian pharmacy legit: Large Selection of Medications – safe canadian pharmacies
Автор предлагает практические советы, которые читатели могут использовать в своей повседневной жизни.
canadian pharmacy king reviews Licensed Canadian Pharmacy onlinepharmaciescanada com
http://canadianpharmacy24.store/# real canadian pharmacy
pharmacy website india: Cheapest online pharmacy – reputable indian pharmacies
online shopping pharmacy india Cheapest online pharmacy mail order pharmacy india
best canadian pharmacy to buy from: canadian pharmacies online – canadian pharmacy online reviews
Wow, marvelous blog layout! How long have you been blogging for? you make blogging look easy. The overall look of your site is wonderful, as well as the content!
best online pharmacy india: Generic Medicine India to USA – pharmacy website india
best online pharmacy india: Generic Medicine India to USA – top 10 pharmacies in india
mexico drug stores pharmacies Online Pharmacies in Mexico mexico drug stores pharmacies
indian pharmacy: best online pharmacy india – Online medicine home delivery
india pharmacy mail order: Healthcare and medicines from India – buy prescription drugs from india
cheapest online pharmacy india: indian pharmacy online – best online pharmacy india
п»їlegitimate online pharmacies india Cheapest online pharmacy top 10 pharmacies in india
pharmacy website india: Generic Medicine India to USA – best online pharmacy india
safe canadian pharmacy: pills now even cheaper – best rated canadian pharmacy
purple pharmacy mexico price list: cheapest mexico drugs – mexican pharmaceuticals online
mexican rx online: cheapest mexico drugs – mexican border pharmacies shipping to usa
mexican border pharmacies shipping to usa cheapest mexico drugs mexican drugstore online
canadian pharmacy 365: Large Selection of Medications – canadian pharmacy near me
mexican pharmacy: cheapest mexico drugs – medicine in mexico pharmacies
п»їbest mexican online pharmacies: mexico pharmacy – п»їbest mexican online pharmacies
top 10 online pharmacy in india Generic Medicine India to USA world pharmacy india
pharmacy website india: Generic Medicine India to USA – indianpharmacy com
http://indianpharmacy.icu/# indian pharmacy paypal
mexican online pharmacies prescription drugs: mexico pharmacy – buying from online mexican pharmacy
buy prescription drugs from india Generic Medicine India to USA indian pharmacy paypal
mexican rx online: mexican border pharmacies shipping to usa – buying from online mexican pharmacy
india pharmacy: indian pharmacy delivery – india pharmacy
medication from mexico pharmacy mexican pharmacy best online pharmacies in mexico
canadian pharmacies online: Certified Canadian Pharmacy – precription drugs from canada
http://canadianpharmacy24.store/# certified canadian international pharmacy
cheapest online pharmacy india Cheapest online pharmacy online shopping pharmacy india
mexican rx online: mexico pharmacy – buying from online mexican pharmacy
mexico drug stores pharmacies: cheapest mexico drugs – mexico drug stores pharmacies
mexican mail order pharmacies: cheapest mexico drugs – medication from mexico pharmacy
buy medicines online in india Cheapest online pharmacy india online pharmacy
pharmacies in mexico that ship to usa: mexico pharmacies prescription drugs – reputable mexican pharmacies online
https://clomidall.shop/# buy generic clomid without insurance
https://amoxilall.com/# amoxicillin 500 mg without a prescription
https://prednisoneall.shop/# prednisone pack
Have you ever considered creating an e-book or guest authoring on other blogs? I have a blog based on the same ideas you discuss and would really like to have you share some stories/information. I know my subscribers would appreciate your work. If you are even remotely interested, feel free to send me an e mail.
zithromax 500 without prescription buy cheap generic zithromax zithromax z-pak price without insurance
where can you buy zithromax: zithromax canadian pharmacy – order zithromax without prescription
http://clomidall.shop/# can you buy clomid without prescription
https://clomidall.com/# how can i get generic clomid price
amoxicillin without rx amoxicillin azithromycin buy amoxicillin online no prescription
http://prednisoneall.com/# purchase prednisone
how to buy clomid no prescription: can i buy cheap clomid price – how can i get clomid without a prescription
https://prednisoneall.com/# prednisone prescription drug
amoxicillin 1000 mg capsule amoxicillin 500mg price over the counter amoxicillin
http://amoxilall.com/# rexall pharmacy amoxicillin 500mg
how can i get cheap clomid without insurance can i order generic clomid tablets how to buy clomid without prescription
https://prednisoneall.com/# 50 mg prednisone from canada
https://zithromaxall.shop/# where to get zithromax over the counter
http://clomidall.shop/# buying clomid without dr prescription
buy generic zithromax online: buy zithromax without prescription online – cost of generic zithromax
cost of amoxicillin where to buy amoxicillin 500mg without prescription medicine amoxicillin 500
http://prednisoneall.com/# prednisone 40 mg price
prednisone 20 tablet: buy prednisone online usa – buy prednisone 40 mg
Это помогает читателям получить всестороннее представление о теме без явных предубеждений.
https://clomidall.shop/# buy cheap clomid prices
https://prednisoneall.com/# buying prednisone
zithromax for sale online zithromax prescription in canada generic zithromax 500mg
https://amoxilall.shop/# order amoxicillin uk
cost generic clomid without a prescription clomid without rx where buy clomid without insurance
https://amoxilall.shop/# where to buy amoxicillin
http://prednisoneall.shop/# prednisone 5mg daily
http://clomidall.shop/# order generic clomid pill
zithromax cost: buy azithromycin zithromax – zithromax over the counter uk
how to get amoxicillin over the counter amoxicillin 825 mg amoxicillin from canada
http://zithromaxall.com/# zithromax generic cost
zithromax 250 mg australia: how to get zithromax online – zithromax canadian pharmacy
buy amoxicillin online mexico over the counter amoxicillin canada amoxicillin medicine
http://clomidall.shop/# where can i buy generic clomid without a prescription
Buy Tadalafil 20mg: Generic Tadalafil 20mg price – cialis for sale
http://kamagraiq.com/# п»їkamagra
buy kamagra online usa Sildenafil Oral Jelly buy kamagra online usa
http://sildenafiliq.xyz/# Cheap Sildenafil 100mg
Generic Cialis without a doctor prescription: tadalafil iq – cialis for sale
cheapest viagra: generic ed pills – buy Viagra online
Kamagra tablets: Sildenafil Oral Jelly – Kamagra 100mg
Kamagra 100mg price Kamagra Iq sildenafil oral jelly 100mg kamagra
http://tadalafiliq.com/# Buy Tadalafil 10mg
Kamagra Oral Jelly: Kamagra Oral Jelly Price – sildenafil oral jelly 100mg kamagra
super kamagra Kamagra Iq buy Kamagra
viagra canada: sildenafil iq – Cheap Viagra 100mg
https://sildenafiliq.xyz/# buy viagra here
https://tadalafiliq.shop/# Tadalafil Tablet
Generic Cialis without a doctor prescription: tadalafil iq – Cialis over the counter
Tadalafil Tablet: cialis without a doctor prescription – Generic Cialis price
Kamagra Oral Jelly Kamagra Iq Kamagra Oral Jelly
Good day I am so excited I found your blog, I really found you by mistake, while I was searching on Digg for something else, Anyways I am here now and would just like to say thanks for a tremendous post and a all round entertaining blog (I also love the theme/design), I don’t have time to look over it all at the moment but I have bookmarked it and also included your RSS feeds, so when I have time I will be back to read a great deal more, Please do keep up the great b.
generic sildenafil: cheapest viagra – over the counter sildenafil
http://tadalafiliq.com/# cheapest cialis
Cheapest Sildenafil online generic ed pills buy Viagra over the counter
Kamagra tablets: Kamagra gel – Kamagra Oral Jelly
buy kamagra online usa: Kamagra Iq – super kamagra
http://sildenafiliq.xyz/# Cheap Sildenafil 100mg
http://tadalafiliq.com/# Generic Cialis without a doctor prescription
Kamagra Oral Jelly Kamagra gel Kamagra 100mg price
kamagra: Kamagra gel – Kamagra 100mg price
https://tadalafiliq.com/# Cialis over the counter
https://kamagraiq.shop/# п»їkamagra
Buy Tadalafil 10mg: cheapest cialis – cialis for sale
Buy Cialis online: cialis without a doctor prescription – cialis generic
cheap kamagra Kamagra Oral Jelly Price Kamagra 100mg price
buy kamagra online usa: Kamagra Oral Jelly Price – buy Kamagra
https://sildenafiliq.com/# Viagra without a doctor prescription Canada
Sildenafil 100mg price: best price on viagra – Viagra generic over the counter
Generic Tadalafil 20mg price Buy Cialis online Buy Tadalafil 20mg
http://tadalafiliq.shop/# Buy Tadalafil 5mg
https://kamagraiq.shop/# Kamagra 100mg
Tadalafil price: Generic Cialis price – buy cialis pill
sildenafil oral jelly 100mg kamagra kamagra best price Kamagra Oral Jelly
http://sildenafiliq.com/# buy Viagra online
sildenafil online: buy viagra online – Sildenafil Citrate Tablets 100mg
Tadalafil price: Generic Tadalafil 20mg price – cheapest cialis
http://sildenafiliq.xyz/# Generic Viagra for sale
cheap viagra: Viagra Tablet price – Viagra Tablet price
Cheap generic Viagra sildenafil iq Generic Viagra for sale
https://sildenafiliq.xyz/# sildenafil online
cheap viagra: buy viagra online – sildenafil over the counter
https://indianpharmgrx.shop/# indian pharmacy paypal
reputable mexican pharmacies online: online pharmacy in Mexico – mexico pharmacy
canadian pharmacy ltd: Cheapest drug prices Canada – canada drug pharmacy
buy prescription drugs from india indian pharmacy cheapest online pharmacy india
http://canadianpharmgrx.com/# canada drugs online
indian pharmacy Healthcare and medicines from India indian pharmacies safe
mexico pharmacies prescription drugs: Mexico drugstore – medication from mexico pharmacy
http://indianpharmgrx.shop/# best india pharmacy
top online pharmacy india: Generic Medicine India to USA – pharmacy website india
https://indianpharmgrx.shop/# indian pharmacy
canada drugs online List of Canadian pharmacies buying from canadian pharmacies
buying from online mexican pharmacy: Pills from Mexican Pharmacy – п»їbest mexican online pharmacies
https://indianpharmgrx.com/# online pharmacy india
pharmacy in canada Cheapest drug prices Canada ordering drugs from canada
https://mexicanpharmgrx.shop/# buying from online mexican pharmacy
medication from mexico pharmacy: mexican pharmacy – п»їbest mexican online pharmacies
reputable indian online pharmacy: indian pharmacy – best online pharmacy india
canadian pharmacy 24h com buy drugs from canada legitimate canadian mail order pharmacy
https://canadianpharmgrx.com/# canadian pharmacy mall
indian pharmacy paypal Generic Medicine India to USA mail order pharmacy india
https://canadianpharmgrx.xyz/# legit canadian online pharmacy
repaglinide physicochemical properties
purple pharmacy mexico price list: Mexico drugstore – purple pharmacy mexico price list
canadian drugs online: International Pharmacy delivery – canadian pharmacy uk delivery
http://indianpharmgrx.shop/# indian pharmacy paypal
best online pharmacies in mexico online pharmacy in Mexico mexican rx online
https://mexicanpharmgrx.com/# mexico pharmacy
reputable indian pharmacies indian pharmacy pharmacy website india
Online medicine order: india pharmacy – online pharmacy india
http://indianpharmgrx.shop/# india online pharmacy
top 10 online pharmacy in india: indian pharmacy delivery – indianpharmacy com
http://indianpharmgrx.shop/# mail order pharmacy india
india pharmacy mail order Generic Medicine India to USA online shopping pharmacy india
http://canadianpharmgrx.xyz/# canadian pharmacy price checker
pharmacies in mexico that ship to usa: reputable mexican pharmacies online – mexican drugstore online
https://indianpharmgrx.shop/# legitimate online pharmacies india
medicine in mexico pharmacies: Mexico drugstore – buying from online mexican pharmacy
mail order pharmacy india Generic Medicine India to USA best online pharmacy india
https://canadianpharmgrx.xyz/# global pharmacy canada
canadian online pharmacy reviews: Canada pharmacy – canada drugstore pharmacy rx
diflucan 750 mg: where to buy diflucan otc – where to buy diflucan otc
where to purchase diflucan: can you purchase diflucan over the counter – buy diflucan online usa
buy doxycycline for dogs buy doxycycline for dogs order doxycycline 100mg without prescription
doxycycline 100mg online: doxycycline hyc 100mg – buy doxycycline online uk
buy diflucan generic: diflucan tablet india – where can i buy diflucan without prescription
buy cytotec online Abortion pills online cytotec online
over the counter diflucan pill: can i buy diflucan over the counter in australia – can you order diflucan online
doxycycline without a prescription: doxycycline without prescription – doxycycline without prescription
https://doxycyclinest.pro/# doxycycline tablets
buy cytotec pills online cheap п»їcytotec pills online order cytotec online
tamoxifen postmenopausal: generic tamoxifen – lexapro and tamoxifen
buy cipro online canada: ciprofloxacin generic – ciprofloxacin over the counter
buy cytotec online: buy cytotec over the counter – cytotec pills online
nolvadex vs clomid tamoxifen reviews nolvadex only pct
buy cipro online without prescription: buy cipro online canada – buy cipro online canada
cipro online no prescription in the usa: buy cipro online without prescription – ciprofloxacin 500 mg tablet price
how to buy doxycycline online: where to purchase doxycycline – doxycycline online
doxycycline mono order doxycycline doxycycline prices
purchase cipro: cipro online no prescription in the usa – buy cipro cheap
http://misoprostol.top/# purchase cytotec
п»їcipro generic ciprofloxacin generic price purchase cipro
buy generic ciprofloxacin: п»їcipro generic – buy cipro
buy cipro cheap: antibiotics cipro – ciprofloxacin 500 mg tablet price
cytotec abortion pill: Abortion pills online – buy cytotec in usa
diflucan 150 mg tablets diflucan oral buy diflucan canada
buy doxycycline without prescription: purchase doxycycline online – doxycycline
ciprofloxacin generic price: ciprofloxacin mail online – ciprofloxacin mail online
cytotec pills buy online cytotec buy online usa cytotec buy online usa
tamoxifen brand name: raloxifene vs tamoxifen – buy tamoxifen
buy cytotec pills online cheap: Abortion pills online – buy cytotec in usa
tamoxifen dosage clomid nolvadex generic tamoxifen
http://misoprostol.top/# Abortion pills online
tamoxifen and weight loss: tamoxifen hormone therapy – does tamoxifen cause weight loss
buy diflucan online usa: diflucan canada – diflucan 100mg
diflucan 50mg tablet: diflucan 150 capsule – diflucan pill canada
pct nolvadex: clomid nolvadex – aromatase inhibitors tamoxifen
ciprofloxacin ciprofloxacin 500mg buy online п»їcipro generic
buy cytotec over the counter: buy cytotec pills online cheap – buy cytotec in usa
tamoxifen for gynecomastia reviews nolvadex only pct nolvadex 10mg
buy doxycycline online: doxylin – buy doxycycline without prescription uk
zithromax for sale usa: zithromax for sale us – zithromax 1000 mg pills
generic amoxicillin 500mg: purchase amoxicillin online – generic for amoxicillin
prednisone prices prednisone 5 mg tablet order prednisone from canada
http://prednisonea.store/# buy prednisone without rx
stromectol xr: where to buy stromectol – stromectol 15 mg
buy cheap generic zithromax zithromax 500 mg lowest price pharmacy online zithromax order online uk
buy zithromax online with mastercard: where can i buy zithromax in canada – generic zithromax over the counter
clomid medication: where to buy generic clomid pills – where buy generic clomid
buying clomid without rx: cheap clomid price – can i get clomid without rx
http://prednisonea.store/# prednisone 10 mg brand name
prednisone in india: ordering prednisone – non prescription prednisone 20mg
prednisone brand name canada prednisone 5 mg tablet price prednisone 5 mg tablet cost
amoxicillin 500mg cost: buy cheap amoxicillin online – where can i buy amoxicillin online
http://stromectola.top/# minocycline 100mg for acne
http://clomida.pro/# buy clomid without rx
how to buy zithromax online buy zithromax 500mg online where can i purchase zithromax online
ivermectin 3mg pill: ivermectin 0.2mg – buy stromectol uk
where to get zithromax over the counter: zithromax prescription in canada – buy cheap zithromax online
https://amoxicillina.top/# amoxicillin 500mg capsules
zithromax cost canada: how to buy zithromax online – how to buy zithromax online
ivermectin over the counter uk ivermectin ireland buy ivermectin nz
amoxicillin 500mg capsules uk: amoxil generic – where can you get amoxicillin
https://clomida.pro/# where can i get generic clomid without prescription
ivermectin pills canada: ivermectin – stromectol uk
http://edpill.top/# cheapest ed treatment
https://medicationnoprescription.pro/# best online pharmacy that does not require a prescription in india
online pharmacy discount code rx pharmacy no prescription promo code for canadian pharmacy meds
https://edpill.top/# ed rx online
best online pharmacy no prescription: pharmacy without prescription – promo code for canadian pharmacy meds
http://edpill.top/# online ed medications
where to buy erectile dysfunction pills erectile dysfunction medication online cheapest ed online
order prescription drugs online without doctor: how to buy prescriptions from canada safely – online pharmacy reviews no prescription
http://edpill.top/# erectile dysfunction drugs online
http://medicationnoprescription.pro/# online pharmacy not requiring prescription
ed online pharmacy: online ed medicine – cheap ed treatment
https://edpill.top/# low cost ed meds
buy pills without prescription cheap prescription medication online pharmacy no prescription
ed medications cost: top rated ed pills – discount ed meds
https://edpill.top/# ed online prescription
https://edpill.top/# get ed meds online
https://edpill.top/# online ed treatments
online pharmacy no prescription: canadian pharmacy coupon – canadian pharmacy coupon
buying prescription drugs from canada online canada prescription online online pharmacy reviews no prescription
http://onlinepharmacyworld.shop/# canadian pharmacy discount coupon
online erectile dysfunction prescription: boner pills online – low cost ed pills
https://edpill.top/# cheap ed treatment
mail order pharmacy no prescription pharmacy without prescription online pharmacy non prescription drugs
canadian pharmacy no prescription: online pharmacy discount code – online pharmacy no prescription needed
https://onlinepharmacyworld.shop/# pharmacy without prescription
https://medicationnoprescription.pro/# pharmacies without prescriptions
casino tr?c tuy?n: dánh bài tr?c tuy?n – choi casino tr?c tuy?n trên di?n tho?i
http://casinvietnam.com/# choi casino tr?c tuy?n tren di?n tho?i
game c? b?c online uy tin web c? b?c online uy tin game c? b?c online uy tin
https://casinvietnam.shop/# casino tr?c tuy?n
casino tr?c tuy?n vi?t nam: choi casino tr?c tuy?n trên di?n tho?i – casino tr?c tuy?n vi?t nam
https://casinvietnam.shop/# casino tr?c tuy?n uy tin
casino tr?c tuy?n vi?t nam casino tr?c tuy?n casino online uy tin
http://casinvietnam.shop/# danh bai tr?c tuy?n
web c? b?c online uy tin casino tr?c tuy?n vi?t nam game c? b?c online uy tin
casino tr?c tuy?n: casino tr?c tuy?n vi?t nam – casino online uy tín
casino tr?c tuy?n: casino tr?c tuy?n uy tín – dánh bài tr?c tuy?n
https://casinvietnam.shop/# danh bai tr?c tuy?n
casino tr?c tuy?n vi?t nam: dánh bài tr?c tuy?n – web c? b?c online uy tín
http://casinvietnam.com/# web c? b?c online uy tin
casino tr?c tuy?n: web c? b?c online uy tín – casino tr?c tuy?n vi?t nam
https://casinvietnam.shop/# web c? b?c online uy tin
dánh bài tr?c tuy?n: casino online uy tín – web c? b?c online uy tín
http://casinvietnam.com/# casino online uy tin
casino tr?c tuy?n vi?t nam: web c? b?c online uy tín – casino tr?c tuy?n uy tín
https://casinvietnam.shop/# game c? b?c online uy tin
web c? b?c online uy tín: dánh bài tr?c tuy?n – game c? b?c online uy tín
casino tr?c tuy?n vi?t nam: casino tr?c tuy?n vi?t nam – casino tr?c tuy?n vi?t nam
http://casinvietnam.com/# game c? b?c online uy tin
casino tr?c tuy?n uy tín: casino tr?c tuy?n vi?t nam – casino tr?c tuy?n uy tín
https://casinvietnam.com/# casino tr?c tuy?n vi?t nam
casino online uy tín: game c? b?c online uy tín – web c? b?c online uy tín
https://casinvietnam.com/# casino tr?c tuy?n uy tin
http://casinvietnam.shop/# casino online uy tin
casino tr?c tuy?n uy tín: casino online uy tín – casino online uy tín
casino tr?c tuy?n: casino tr?c tuy?n vi?t nam – casino tr?c tuy?n vi?t nam
http://casinvietnam.shop/# casino tr?c tuy?n
http://casinvietnam.shop/# web c? b?c online uy tin
game c? b?c online uy tín: dánh bài tr?c tuy?n – casino tr?c tuy?n vi?t nam
https://casinvietnam.shop/# web c? b?c online uy tin
casino tr?c tuy?n: casino tr?c tuy?n uy tín – choi casino tr?c tuy?n trên di?n tho?i
http://casinvietnam.com/# casino tr?c tuy?n